Abstract
Hemangiopericytoma (HP) is a well-recognized neoplasm arising from vascular pericytes that has been reported only in the dog and man. In this study, we describe a 14-year-old female Arabian horse that was presented for surgical excision of a 2-cm-diameter expansile subcuticular mass in the right lower eyelid. Histologically, the mass consisted of loosely arranged interlacing streams and storiform bundles of spindle cells that often formed distinct whorls around a central capillary and bundles of collagen (Antoni A-like pattern). Immunohistochemical analysis revealed strong diffuse cytoplasmic immunoreactivity for vimentin and focal immunoreactivity for smooth muscle actin, whereas neoplastic cells did not stain for Factor VIII-related antigen, Glial fibrillary acidic protein (GFAP), or S100. On the basis of histomorphology and immunohistochemical reactivity, the present tumor was diagnosed as HP. To our knowledge, this is the first report describing a HP in a horse.
A 14-year-old female Arabian horse was presented for clinical evaluation of a cutaneous mass on the right lower eyelid. The mass had been present for approximately 2 years but had recently increased in size. Clinical examination revealed a well-delineated, 2-cm-diameter, semi-mobile, subcutaneous mass located approximately 1 cm from the palpebral margin. Palpation of the mass did not elicit pain, and no other physical abnormalities were detected. Complete blood count, fibrinogen concentration, and serum chemistry were within normal ranges. The palpebral conjunctiva was diffusely hyperemic with mild vascular congestion. During the ophthalmic examination a visual deficit or other ocular abnormalities were not detected. By ultrasonograph, the mass appeared hypoechoic, was well encapsulated, and partially invaded the orbital cavity. Cytologic evaluation of fine needle aspirates was inconclusive.
The horse was anesthetized with xylazine and ketamine and positioned in left lateral recumbency. Anesthesia was maintained with isofluorane administered through a semiclosed circuit. After preparing an area around the right eye for aseptic surgery, a 4-cm-long, elliptical, cutaneous incision was made around the rostral border of the mass. Using blunt dissection, the mass was carefully undermined, to avoid penetrating the conjunctiva, and freed from the surrounding subcutaneous tissue. The mass was excised in toto, without disrupting its capsule. The mass was soft, well encapsulated, and oblong and extended approximately 3 cm into the orbital cavity. However, it did not invade the orbital bone or the sclera.
The subcutaneous tissue and skin were closed with a simple interrupted pattern using #3–0 polyglactin 910 suture and #2–0 polydioxanone suture, respectively. The mass was submitted for histologic examination.
Six weeks following surgical excision, the horse was readmitted to evaluate a diffuse swelling of the right lower eyelid. Mucopurulent material exuded around unabsorbed sutures. Suture material was removed, and within 4 days the swelling subsided. Twelve months following surgical excision, the horse was reexamined, and an ophthalmic examination was unremarkable, with no evidence of eyelid mass recurrence.
Grossly, the subcutis was expanded by a well-delineated, 20 × 20 × 40 mm, encapsulated soft tissue mass containing engorged blood vessels. The cut surface was multi-lobulated and mottled white to partly red. The mass was fixed by immersion in 10% neutral-buffered formalin, routinely processed, embedded in paraffin and sectioned at 4 to 6 µm for routine histologic examination. All sections were stained with hematoxylin and eosin (HE; Gill's #2) using eosin phloxine counterstain. Additional sections of the mass were examined immunohistochemically with a streptavidin-biotin kit (Dako Cytomation, Carpinteria, CA) and the following antisera: prediluted monoclonal antibodies against vimentin (Dako, catalog number M0725), smooth muscle actin (SMA; DAKO, catalog number M0851), S100 (DAKO, catalog number Z0311), polyclonal antibodies for von Willebrand Factor (Factor VIII-related antigen; Dako, catalog number N1505), and Glial Fibrillary Acidic Protein (GFAP, catalog number N1506; Dako). Positive control slides consisted of tonsil (Vimentin and Factor VIII-related antigen), esophagus (SMA), equine nerve (S100), and cerebrum (GFAP). Immunostaining was performed using a Dako Autostainer universal staining system (Dako). Slides containing the mass and the tissues used for positive control were stained with buffer and served as negative controls. All slides were counterstained with hematoxylin.
Microscopically, the mass was moderately infiltrative and histologic features were consistent with hemangiopericytoma (HP). Neoplastic cells were arranged in short, interlacing bundles and storiform whorls randomly distributed throughout a delicate fibrillar stroma (Fig. 1). The majority of the cells were spindloid to fusiform with indistinct cell borders and homogenous eosinophilic cytoplasm. Cells often had a perivascular distribution forming concentric laminations around a central capillary. The nuclei were round to oval with a vesiculate to finely stippled chromatin pattern and a single prominent nucleolus with an average of two mitotic figures per 400× field. By immunohistochemical examination, tumor cells showed strong cytoplasmic positivity for vimentin (Fig. 2). Occasionally, small groups and whorls of neoplastic cells had focal cytoplasmic positivity for SMA (Fig. 3). Conversely, cells did not stain with S100, Factor VIII-related antigen and GFAP (data not shown).
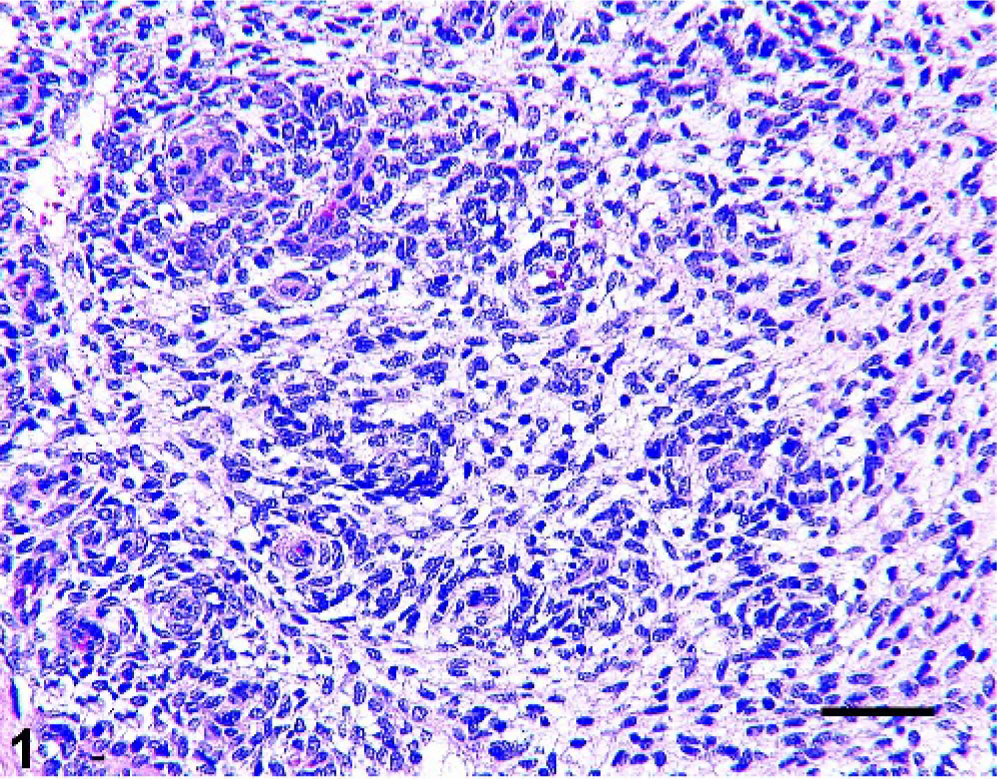
Eyelid; horse. Hemangiopericytoma. Interlacing bundles and whorls of neoplastic cells are loosely arranged in a delicate fibrillar stroma. HE. Bar = 50 µm.
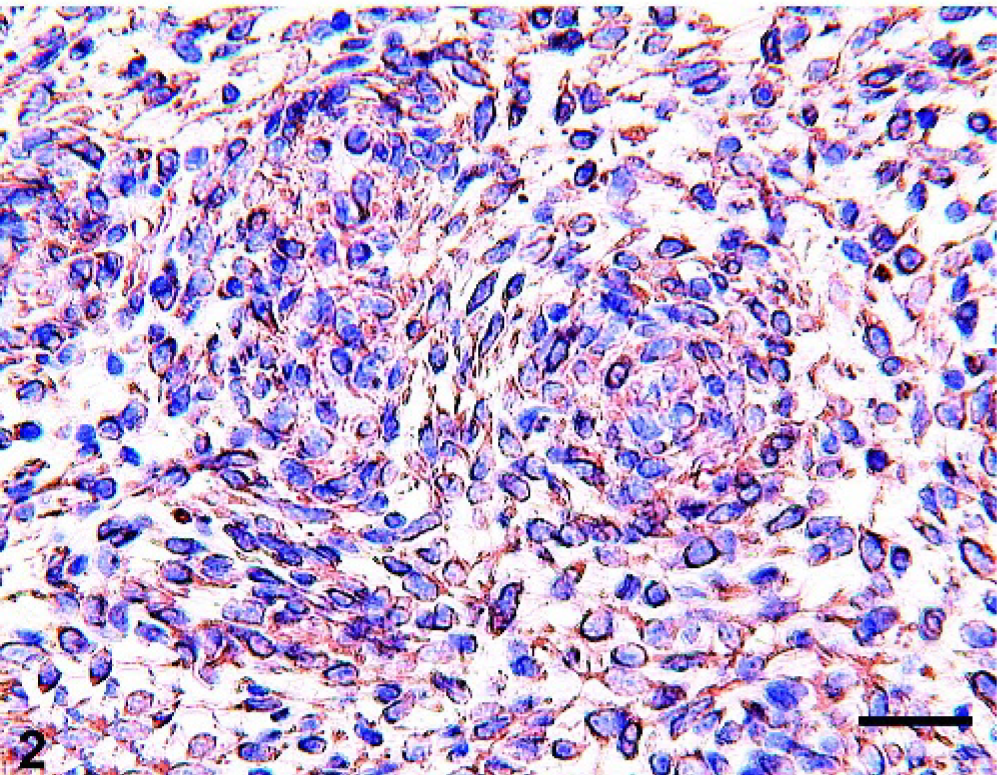
Eyelid; horse. Hemangiopericytoma. Neoplastic cells show marked immunoreactivity for vimentin. Immunoperoxidase stain; hematoxylin counterstain. Bar = 30 µm.
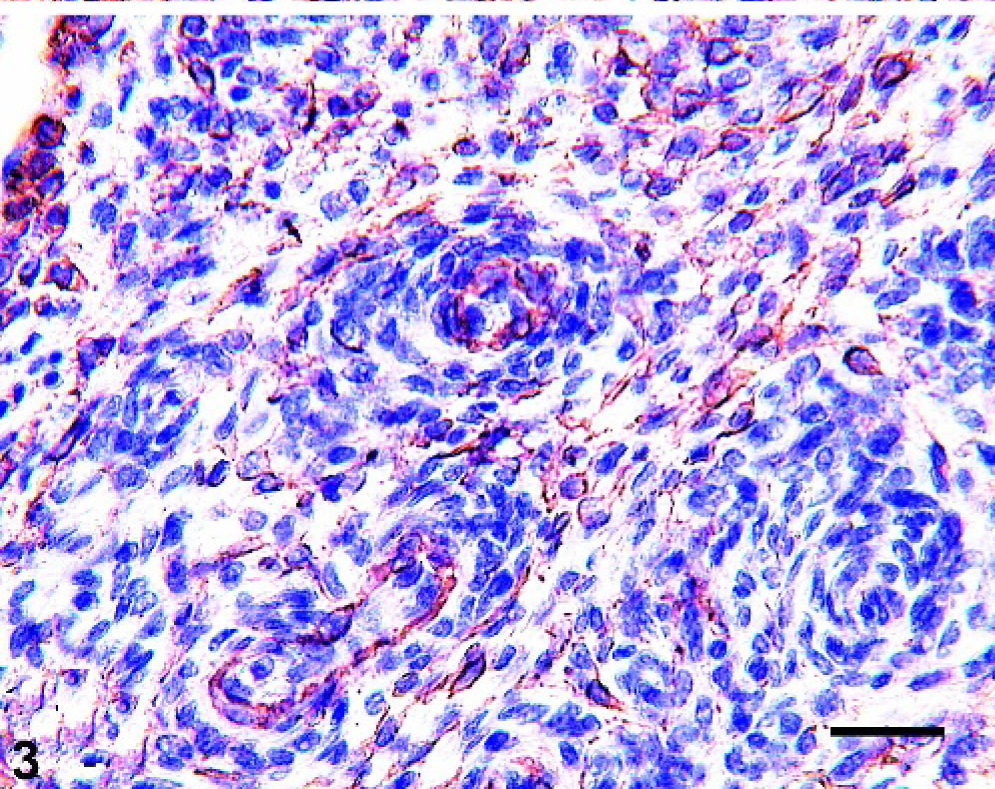
Eyelid; horse. Hemangiopericytoma. Perivascular whorls of neoplastic cells stain strongly for SMA. Immunoperoxidase stain; hematoxylin counterstain. Bar = 30 µm.
Because no other subcutaneous masses were observed in this horse, this eyelid HP was most likely a primary neoplasm, originating from blood vessels within the subcutis of the lower eyelid.
The equine eye and adnexa are frequent sites of tumors. 1, 3, 8, 12, 15 The eyelid, in particular, has been reported to be affected by squamous cell carcinoma, sarcoid, melanoma, and with much less frequency by papillomas, adenomas, adenocarcinomas, mast cell tumors, basal cell tumor, hemangiomas, hemangiosarcomas, lymphosarcomas, fibromas, and schwannomas. 1, 3, 8, 12, 15 Among these, squamous cell carcinoma and sarcoid are by far the most common tumors of the equine eyelid. Mesenchymal tumors of vascular origin, which affect the eyelid, are rarely reported and include hemangiomas and hemangiosarcomas. 3 Regardless of the anatomical location, HP, a vascular tumor originating from pericytes, has not been previously reported in the horse.
Hemangiopericytomas are uncommon vascular tumors that arise from pericytes, which are mesenchymal cells that surround capillaries. 9 However, there is much uncertainty regarding the origin and differentiation of HPs. Indeed, some investigators broadly designate HPs as “soft tissue sarcomas” or consider HPs as peripheral nerve sheath tumors (e.g., schwannomas). 4, 6 Schwannomas of the eyelid have been observed in horses. 8 Cytoplasmic processes that wrap around collagen bundles and the overall ultrastructural appearance of the neoplastic cellular elements with cytoplasmic processes covered by basal lamina material are characteristic of Schwannian differentiation. These histologic and ultrastructural features are supported by positive S100 immunoreactivity. Hemangiopericytomas may appear histologically similar to schwannomas; however, the absence of staining for GFAP and S100 support a diagnosis of the former.
Although this is the first report of HP in the horse, there are several reports of the tumor occurrence in man and dog. In man, HP occurs most commonly on the limbs, retroperitoneum, and the head and neck. Three percent of primary orbital tumors in man are HPs. 7 Metastasis of this tumor, usually to bone, lung, and the breast, was reported to occur in 12–45% of human cases. 9, 14 Hemangiopericytoma of the eyelid and orbit is reported to be slowly invasive, occasionally metastatic, and to have a tendency to recur. 5, 9 In dogs, HP develops exclusively in the subcutaneous tissue with occasional infiltration of the underlying muscle. 10 In this species, HP usually affects the limbs and trunk and tends to be locally aggressive, but with a low tendency to metastasize. A report of HP of the orbit in a dog, treated with surgical excision, describes no recurrence or metastasis 12 months after surgery. 2
To prevent recurrence, in human surgery, a wide excision without rupture of the capsule, if present, or excisional margins free of neoplastic cells, is considered essential. In our case, the surgical procedure was successful in the excision of the mass in toto, without rupture of the capsule.
Twelve months after surgery there was no evidence of recurrence. A possible therapeutic approach in the event of local recurrence could be in the form of high-dose radiotherapy, which has been reported to be an effective treatment of HP in both man and animals. 11, 13
