Abstract
Lymphomas were reported to be induced in rats in bioassays of aspartame, methyl-tertiary-butyl ether (MTBE), and other chemicals conducted by a nonprofit cancer research organization. European regulatory authorities concluded that lymphomas in the aspartame study were caused by Mycoplasma pulmonis and suggested that this also was the case for the MTBE bioassay. To assess the role of M. pulmonis in these bioassays, we reviewed the tumor data for the aspartame and MTBE bioassays and, additionally, the organization's bioassay of methanol. For all 3 studies, the most frequently reported hematopoietic neoplasm was lympho-immunoblastic lymphoma, the most frequently affected organ was the lung, and, in almost half of the rats with this diagnosis, the lung was the only affected organ. Lesions diagnosed as lymphoma in published illustrations had pleomorphic cellular morphology and appeared to contain neutrophils. Information from these reports and other sources indicated that lesions typical of M. pulmonis disease were prevalent among the aspartame and MTBE study rats and that the rats were not specific-pathogen-free. Because the lymphoma type, cellular morphology, and organ distribution reported in these studies are atypical of lymphoma in rats, because lymphocyte and plasma cell accumulation in the lung is characteristic of M. pulmonis disease, and because M. pulmonis disease can be exacerbated by experimental manipulations, including chemical treatment, we suggest that a plausible alternative explanation for the reported results of these bioassays is that the studies were confounded by M. pulmonis disease and that lesions of the disease were interpreted as lymphoma.
Introduction
Hematopoietic neoplasms, chiefly lymphomas, were reported to be induced in rats in lifetime bioassays of aspartame, 40,41 methyl-tertiary-butyl ether (MTBE), 2,3 and other chemicals 1,2,4,39 conducted by a nonprofit cancer research organization. The European Food Safety Authority (EFSA) concluded in its review of the aspartame study that such neoplasms were caused by Mycoplasma pulmonis disease and suggested that this also was the case in the MTBE study (http://www.efsa.europa.eu/EFSA/Scientific_Opinion/afc_op_ej356_aspartame_en1,0.pdf). The UK Department of Health Committee on Carcinogenicity also did not consider the aspartame bioassay results valid (http://www.advisorybodies.doh.gov.uk/pdfs/cc066.pdf), and questions have been raised concerning the organization's methods of conducting bioassays and analyzing and communicating results. 20 A review by Caldwell et al. 10 disputes the EFSA findings but does not take into account important features of M. pulmonis disease and lymphoma in rats. 37 To assess the role of M. pulmonis disease in these bioassays, we tabulated the leukemia and lymphoma diagnoses and their organ distribution from the data available online for the aspartame and MBTE studies (http://www.ramazzini.it/fondazione/studyUpload/APM_P04(1).pdf, http://www.ramazzini.it/fondazione/studyUpload/MTBE_P04(1).pdf), and an additional bioassay of methanol (http://www.ramazzini.it/fondazione/studyUpload/Methanol_P04(1).pdf). Based on these data and information from the published reports of these studies, the EFSA review of the aspartame study (http://www.efsa.europa.eu/EFSA/Scientific_Opinion/afc_op_ej356_aspartame_en1,0.pdf), and other sources, we believe it likely that the rats in these bioassays had M. pulmonis disease, which is characterized by accumulation of lymphocytes and plasma cells in the lung, 19,31,33,35,46 and which can be exacerbated by experimental manipulations, including chemical treatment. 7,19,29,31,33–35,46 We also consider the mixed cellular pattern and predominantly pulmonary distribution of the lymphoma type most frequently diagnosed in these bioassays to be uncharacteristic of lymphoma in rats (http://www.toxpath.org/ssdnc/HemolyphaticProliferativeR.pdf). 6,11–14,23,32,44,45 For these reasons, we consider it likely that these bioassays were confounded by M. pulmonis disease and suggest that a plausible alternative explanation for the reported results is that M. pulmonis disease interfered with accurate diagnosis and that lesions of the disease were interpreted as lymphoma.
Characteristics of M. pulmonis Disease
M. pulmonis disease is a chronic disease of rats and mice that sucklings acquire from the mother and that persists for the life of the animal. 19,35,46 The organism parasitizes the respiratory mucosal surface, inducing chronic suppurative inflammation, accompanied by epithelial hyperplasia and metaplasia, of the nasal passages, middle ears, larynx, trachea, bronchi, and bronchioles. 19,31,33,35,46 In advanced disease, pulmonary lesions progress to include bronchiectasis, bronchiolectasis, and pneumonia.
Two features of the disease are essential to understanding its potential to complicate diagnosis of hematopoietic neoplasms in the lung. One is that a hallmark characteristic of the inflammation induced by M. pulmonis is accumulation of large numbers of lymphocytes and plasma cells, particularly around the bronchi, bronchioles, and adjacent vessels, where such accumulations can become quite extensive (Fig. 1). Probably in part because components of M. pulmonis cells are highly mitogenic for rat lymphocytes, 25 these accumulations can include many immature and proliferating lymphoid cells (Fig. 2), imparting features to the lesions resembling those of dysplasia or neoplasia. The other key characteristic of M. pulmonis disease is that its expression, particularly that of the pulmonary lesions, can be profoundly influenced by chemical administration, concurrent infections, advancing host age, and other factors. 7,19,29,31,33–35,46 Thus, it is plausible that if lesions of the disease were interpreted as lymphoma, disease progression induced by chemical treatment could result in the conclusion that a treatment or dose-response effect occurred, and exacerbation by concurrent infections and advancing age could lead to a high reported incidence of lymphoma in control rats in lifespan bioassays.

Bronchus of an SPF F344/N rat with experimental M. pulmonis disease exacerbated by Sendai virus infection. Massive accumulation of lymphocytes and plasma cells. HE.
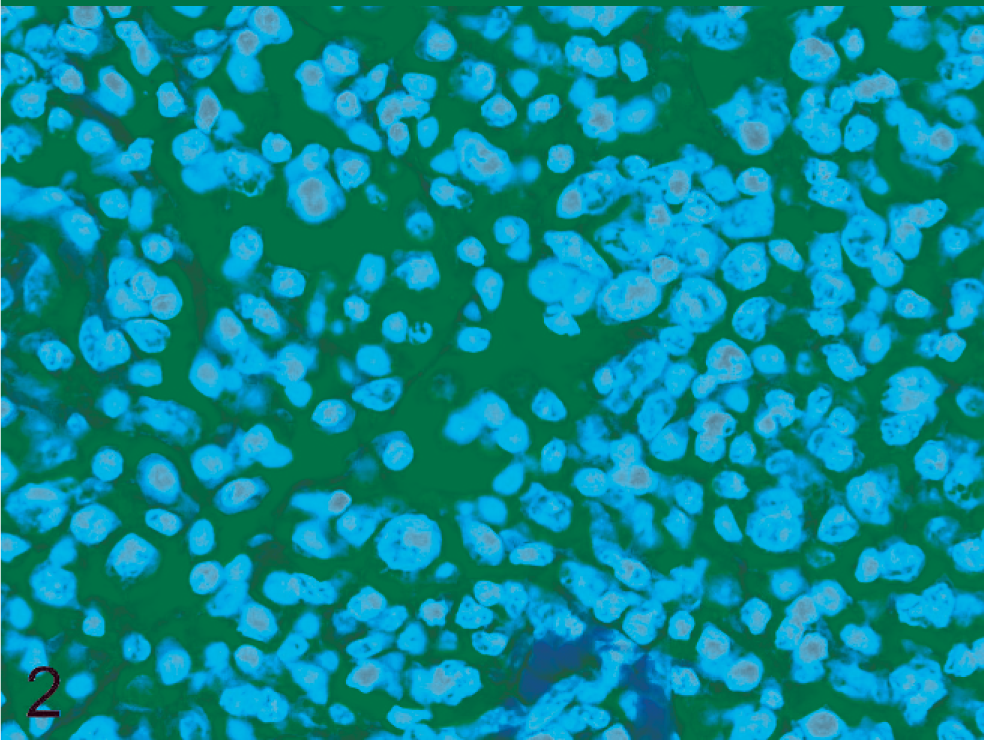
Bronchial inflammatory cell accumulation in a conventionally maintained rat of unspecified strain with natural M. pulmonis disease. Large, immature lymphoid cells, plasma cells, and mitotic figures. HE.
M. pulmonis and Other Pathogens in Bioassay Rats
Management of barrier-maintained, specific-pathogen–free (SPF) animal facilities includes rigorous disease control and health assurance measures to exclude M. pulmonis and other pathogens. According to published reviews, 10,22 the rat colony used for the bioassays in question is conventionally maintained, rather than SPF, and the EFSA review of the aspartame study (http://www.efsa.europa.eu/EFSA/Scientific_Opinion/afc_op_ej356_aspartame_en1,0.pdf) states, “no serology was undertaken during the … study to confirm the presence of infection, as would be normal practice.”
According to Caldwell et al., 10 “The primary cause of spontaneous death in geriatric rats” in the colony is “respiratory infection.” The EFSA review of the aspartame study (http://www.efsa.europa.eu/EFSA/Scientific_Opinion/afc_op_ej356_aspartame_en1,0.pdf) states, “The non-tumour pathological findings in the rats indicated a very high incidence of infection, both in treated and untreated rats… The incidences in treated and control groups for brain abscesses ranged from 7–11% in males and from 4–20% in females, for pyelonephritis from 23–62% in males and from 31–83% in females, for pleuritis from 22–71% in males and from 47–94% in females, and for bronchopneumonia from 81–95% in males and from 69–97% in females [emphasis ours]. In addition, a relatively high incidence of peritonitis, liver abscesses and hepatitis, pericarditis and meningitis occurred in all groups.” M. pulmonis is the most likely cause of bronchopneumonia, and is likely to be involved in many cases of “respiratory infection,” in conventional laboratory rats. 19,31,35,46 There also was increased incidence of olfactory epithelial hyperplasia in male and female rats, 40 another lesion characteristic of M. pulmonis disease. However, the other lesions and conditions listed are not typical of M. pulmonis disease, 19,31,35,46 indicating that other pathogens probably also were present.
Data from the MTBE study also strongly suggest that the rats had M. pulmonis disease, inasmuch as 15.0 to 23.3% of control and treated rats had “peribronchial lymphoplasmacellular hyperplasia.” 2 Such lesions are highly characteristic of M. pulmonis disease, and when they are present, M. pulmonis is by far the most likely cause. 19,31,35,46 Based on these observations, we consider it probable that the rats in these bioassays had M. pulmonis as well as other pathogenic and opportunistic microorganisms.
Incidence, Organ Distribution, and Morphology of Lymphomas
From the tabulated data for the aspartame, MTBE, and methanol studies (Table 1), the predominant type of hematopoietic neoplasm in these bioassays was lympho-immunoblastic lymphoma, and the organ most frequently affected by this neoplasm type was the lung. Of a total of 507 reported hematopoietic neoplasms affecting the lung among 2,960 rats in these 3 studies, 328 (64.7%) were classified as lympho-immunoblastic lymphoma, and of these 328 neoplasms, 162 (49.4%) affected only the lung and no other organs. Lymphoma in rats characteristically arises in lymph nodes or in the thymus, spleen, and intestine. It can arise occasionally in other sites, including the bronchus-associated lymphoid tissue of the lung, 21 but, aside from lymphoma-like lesions of uncertain nature associated with M. pulmonis and other pathogens (“chronic respiratory disease”) in aged rats,∗ naturally occurring lymphoma in rats does not affect predominantly the lung (http://www.toxpath.org/ssdnc/HemolyphaticProliferativeR.pdf). 6,11–14,23,32,44,45
Hematopoietic neoplasms in the lungs of aspartame, MTBE, and methanol study rats.∗
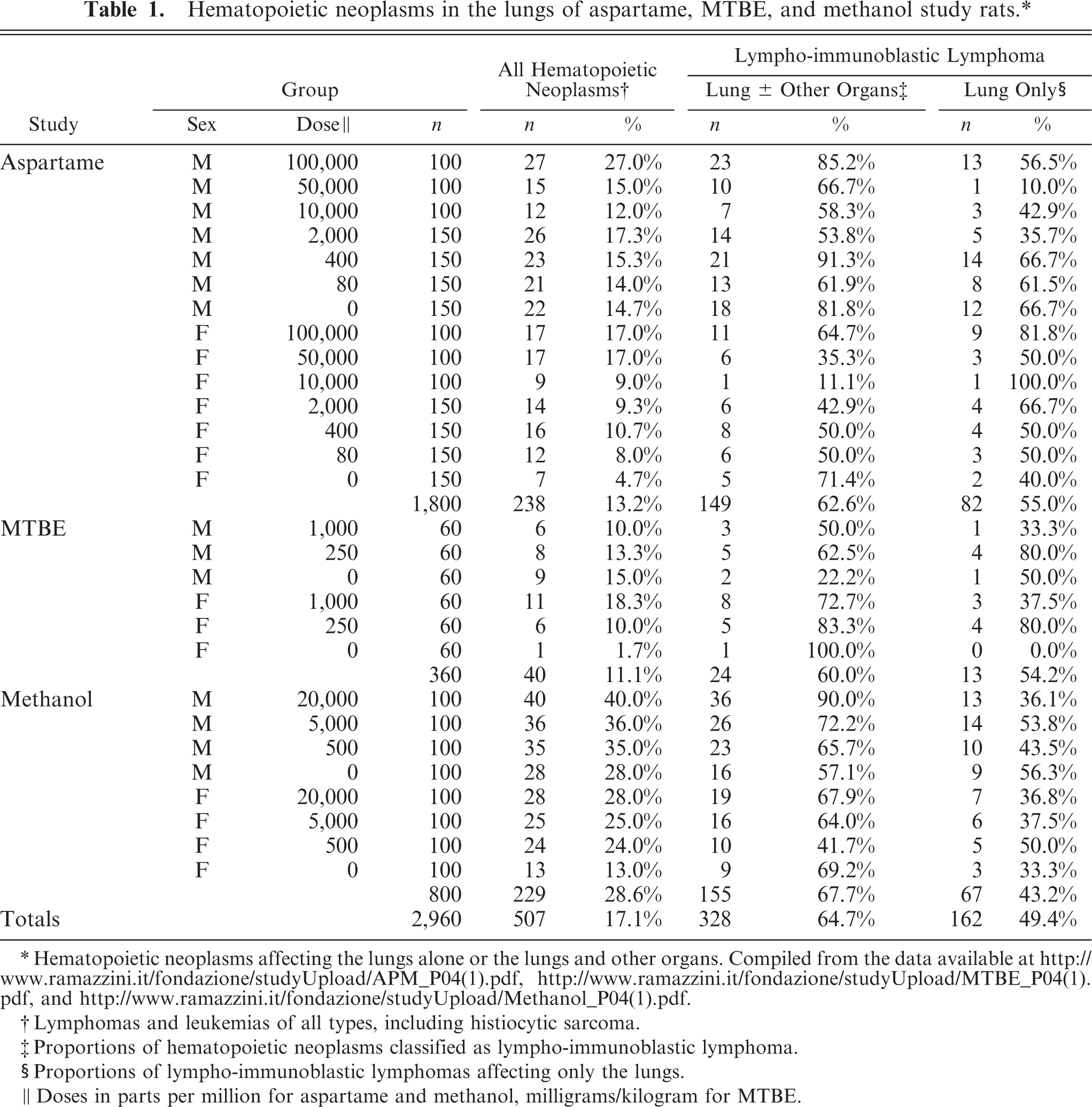
∗ Hematopoietic neoplasms affecting the lungs alone or the lungs and other organs. Compiled from the data available at http://www.ramazzini.it/fondazione/studyUpload/APM_P04(1).pdf, http://www.ramazzini.it/fondazione/studyUpload/MTBE_P04(1).pdf, and http://www.ramazzini.it/fondazione/studyUpload/Methanol_P04(1).pdf.
† Lymphomas and leukemias of all types, including histiocytic sarcoma.
‡ Proportions of hematopoietic neoplasms classified as lympho-immunoblastic lymphoma.
§ Proportions of lympho-immunoblastic lymphomas affecting only the lungs.
‖ Doses in parts per million for aspartame and methanol, milligrams/kilogram for MTBE.
In the reports of the aspartame study, 40,41 the methanol study, 39 and the 1995 report of the MTBE study, 3 the predominant lymphoma type is classified as lympho-immunoblastic, whereas in the 1999 report of the MTBE study 2 the same neoplasms are classified as immunoblastic. Such designations indicate that the lesions were interpreted to be neoplasms composed of mixtures of lymphocytes and immunoblasts (immature plasma cells), or primarily of immunoblasts. Lympho-immunoblastic lymphoma is not listed as a lymphoma type in rats in available reference sources (http://www.toxpath.org/ssdnc/HemolyphaticProliferativeR.pdf). 6,11–14,23,32,44,45 Immunoblastic lymphoma, the most similar recognized type, is exceedingly rare in Sprague-Dawley rats and rats of other strains, with the sole exception of the LOU/C strain, in which the neoplasm originates in the ileocecal lymph node. 1,4,6,12,44,45
Lymphoma lesions illustrated in aspartame and MTBE study reports (Fig. 10 in Soffritti et al. 41 and Figs. 1–5 of Belpoggi et al., 2 respectively) contain cells of mixed, pleomorphic morphology. Because most types of lymphoma in rats are more uniform in cellular type, 12,45 except possibly the follicular center cell or “reticulum cell” types, which are rare, 12 we consider the cellular pattern in these figures to be uncharacteristic of lymphoma in rats. The lesions shown in Figs. 1–5 of Belpoggi et al. 2 also appear to contain many neutrophils, which is not characteristic of lymphoma. Figure 9 of Soffritti et al. 41 shows peribronchiolar cuffing, which is typical of an inflammatory response, and the focal lesion depicted is discretely demarcated and located in the periphery of the lung lobe, which also is not characteristic of lymphoma. In our view, lesions characterized by accumulation of lymphocytes, plasma cells, and neutrophils in the lungs of conventionally maintained non-SPF rats are more plausibly due to M. pulmonis, possibly with contributions by other pathogens, than to a rare cellular type of lymphoma having an organ distribution uncharacteristic of recognized forms of lymphoma in rats. We therefore believe it plausible that cellular accumulations in response to M. pulmonis could have been interpreted as dysplastic or neoplastic in these bioassays, and that occurrence of true lymphoma or leukemia in the lungs of a few rats could have promoted interpretation of peribronchial lymphoid accumulations of M. pulmonis disease in other rats as earlier stages of lymphoma.
M. pulmonis Disease and Chemical Dose Response Effects
Significant treatment effects on occurrence of hematopoietic neoplasms were reported for these studies, 2,3,39–41 and the tabulated data for lympho-immunoblastic lymphoma separated from other lymphomas and leukemias (Table 1) may suggest some dose-response trends. Appropriate statistical analysis of these trends is neither our focus nor expertise; rather, we emphasize here that diagnosis of increased occurrence of pulmonary lymphoma as a result of interpretation of lesions of M. pulmonis disease as lymphoma is consistent with the potential of the disease to be exacerbated by chemical treatment and other experimental manipulations. 7,19,29,31,33–35,46 Ingestion of hexamethylphosphoramide 29 and inhalation of gaseous ammonia 7,34 have been shown experimentally to promote development of severe M. pulmonis disease; thus, it is plausible that administration of aspartame, MTBE, methanol, and other chemicals could promote progression of M. pulmonis disease, which, if the lesions were diagnosed as lymphomas, could result in apparent treatment- or dose-response effects. Conversely, a lack of such findings in other cases could be because the test chemicals did not exacerbate the disease. Hexamethylphosphoramide 29 and ammonia 7,34 did not affect disease expression differently in male and female rats, but, inasmuch as chemicals commonly differ in metabolism or toxicity between males and females, it is plausible that a chemical more toxic in animals of one sex could exacerbate the disease more strongly in those animals.
Lymphoma in Control Rats
Diagnosis of lesions of M. pulmonis disease as lymphoma also could account for reported incidences of lymphomas and leukemias among the organization's control rats of up to 30.9%, 42 whereas, according to available reference sources, rates of 1 to 2% are typical for spontaneous lymphomas and leukemias in Sprague-Dawley rats in chronic (2-year) studies (http://ntp-server.niehs.nih.gov/index.cfm?objectid=471922A2-F1F6-975E-70CB11D6311782F2). 6,11,12,23,32,44,45 The higher incidence of hematopoietic neoplasms among control rats does not take into account neoplasm type and organ distribution, but, from the data for the aspartame, MTBE, and methanol studies (Table 1), 51/80 (63.8%) of all hematopoietic neoplasms affecting the lung among 620 control rats were classified as lympho-immunoblastic lymphoma, of which 27/51 (52.9%) affected only the lung. These data suggest that lympho-immunoblastic lymphoma is the predominant type diagnosed in the organization's control rats, that the lung is the most frequently affected organ, and that in many rats only the lung is affected; characteristics not typical of lymphoma in rats. If applicable to the organization's control rats in general, such characteristics make the disparity between occurrence of these neoplasms in control rats and that regarded as the norm for the Sprague-Dawley strain considerably greater than if cellular type and organ distribution are not considered.
It can be argued that the longer duration of the bioassays (animals allowed to die rather than being sacrificed after 104 weeks) could contribute to the high incidence of lymphoma in control rats. 10 Another possibility is that rats of the colony are predisposed to lymphoma, as an inbred subline of Sprague-Dawley rats has been developed that has a high rate of spontaneous lymphoma. 28 However, in view of the apparent organ distribution and cellular type of the predominant form of lymphoma reported in the studies in question, we consider it more plausible that lesions of advanced M. pulmonis disease in control rats were interpreted as lymphoma. Such interpretation would be consistent with the potential of M. pulmonis disease to progress with age and to be exacerbated by concurrent infections with other pathogens; 19,31,35,46 which the EFSA review (http://www.efsa.europa.eu/EFSA/Scientific_Opinion/afc_op_ej356_aspartame_en1,0.pdf) shows are likely to be present among the rats.
Summary and Discussion
The role of M. pulmonis disease in the studies in question cannot be determined with certainty without examination of the slides and appropriate diagnostic testing of the rats, but we consider it probable that M. pulmonis disease was present among the subject rats because bronchopneumonia, the most likely cause of which in rats is M. pulmonis, was prevalent in the aspartame study rats, because inflammatory lesions characteristic of M. pulmonis disease were present in the lungs of the MTBE study rats, and because the rats used in the studies were conventional rather than SPF (http://www.efsa.europa.eu/EFSA/Scientific_Opinion/afc_op_ej356_aspartame_en1,0.pdf) 10,22 and therefore likely to harbor M. pulmonis. 19,31,35,46
We consider that the weight of available evidence favors the hypothesis that lesions of M. pulmonis disease were interpreted as lymphoma in the aspartame, MTBE, and methanol bioassays, as this would account for the reported occurrence of lympho-immunoblastic lymphoma in the lung, whereas spontaneous tumors of immunoblastic type are rare in Sprague-Dawley rats, and the organ distribution and cellular morphology are uncharacteristic of immunoblastic or other well-characterized types of lymphoma in rats. Such interpretation of lesions of M. pulmonis disease also could account for reported dose-related increases in lymphoma occurrence, due to exacerbation of M. pulmonis disease by the test chemical, which is consistent with known features of the disease. The reported high incidence of lymphoma in control rats also is consistent with interpretation of M. pulmonis–induced lesions as lymphoma, inasmuch as progression with age and exacerbation by other pathogens also are known features of M. pulmonis disease. Finally, such interpretation also would account for lymphoma being reported to be induced by aspartame, MTBE, and methanol in the studies in question but not in studies of the same chemicals by others (http://www.methanol.org/pdfFrame.cfm?pdf=18MonthmouseVolume6.pdf, http://www.methanol.org/pdfFrame.cfm?pdf=18MonthmouseVolume7.pdf, http://www.methanol.org/pdfFrame.cfm?pdf=24MonthRatVolume7.pdf, http://www.methanol.org/pdfFrame.cfm?pdf=24MonthRatVolume8.pdf). 5,8,17,18
We disagree with the EFSA review of the aspartame study (http://www.efsa.europa.eu/EFSA/Scientific_Opinion/afc_op_ej356_aspartame_en1,0.pdf) that lymphoma is “well established” to be associated with M. pulmonis and other pathogens (“chronic respiratory disease”) in aged rats, although we cannot exclude the possibility. Publications in which this is reported† describe or illustrate lesions that could be interpreted as pulmonary lymphoma, but we consider these lesions to be uncharacteristic of recognized forms of lymphoma in rats for the same reasons as the lesions shown in the reports of the aspartame 41 and MTBE 2 studies, including mixed cellular morphology, presence of neutrophils, and atypical organ distribution. Moreover, we know of no definitive evidence that M. pulmonis can induce lymphoma, nor have any of us seen a convincing example, despite having considerable experience with natural and experimental M. pulmonis disease. For these reasons, we consider induction of pulmonary lymphoma by M. pulmonis to be unproven and unlikely.
Questions regarding the role of M. pulmonis disease and the histopathologic diagnosis of the lung lesions in the studies in question could be settled by 2 straightforward measures. First, the histologic slides from the studies in question could be subjected to full and independent review by a qualified Pathology Working Group. Examination of respiratory tract sections in addition to those of lung would be helpful, because suppurative respiratory mucosal inflammation and epithelial hyperplasia and metaplasia would be present in M. pulmonis disease but would not be characteristic of lymphoma. Second, tissues from the studies in question, and samples from animals in studies currently in progress, could be tested for M. pulmonis. Several methods exist for detection of M. pulmonis infection in rodents. 33 For the aspartame, MTBE, methanol, and other completed studies, paraffin-embedded tissues could be tested for M. pulmonis by a polymerase chain reaction (PCR) method. Several such methods have been described, one of which we developed and have used successfully on paraffin-embedded tissues. 36 Paraffin-embedded tissues also could be reprocessed for electron microscopy and examined for organisms consistent with M. pulmonis on the surface of respiratory epithelial cells. In addition, samples from live rats from studies currently in progress could be tested by PCR, serology, and mycoplasmal and bacterial culture for M. pulmonis and other agents, and tissues also could be fixed and processed for immunohistochemical staining 45 to help characterize lymphomatous and indeterminate lesions.
Footnotes
Acknowledgements
We thank Dr. Joseph Haseman and Dr. Robert Maronpot for manuscript review and suggestions.
