Abstract
Canine cancer has become more prevalent in recent years because of increased life expectancy and greater attention to the health of pets. The range of cancers seen in dogs is as diverse as that in human patients, and despite more intensive therapeutic interventions, fatality rates remain unacceptably high in both species. Chemoprevention is therefore an important means of confronting this disease. Because domestic pets share our environment, greater cross-application and study of the protumorigenic and antitumorigenic factors in our shared environment will benefit all species, leading to the development of new families of less toxic antitumorigenic compounds based on novel and established molecular targets. Currently, the most interesting cancer preventive agents are nonsteroidal anti-inflammatory drugs, peroxisome proliferator-activated receptor-γ ligands, and dietary compounds. This article provides an overview of what is known about how these agents affect molecular signaling in neoplastic disease, with reference to reported application and/or study in dogs where available.
Carcinogenesis and tumor biologic behavior in dogs have far more features in common with humans than with laboratory rodents. Pet dogs are becoming more widely recognized as valuable in comparative oncology with a broad range of comparable types of cancers, similar tumor genetics and molecular phenotypes, histologic appearances, disease duration, and responses to conventional therapies. 62,80 Importantly, greater variability in environmental and host genetic factors significantly affects disease expression but deters rapid identification of specific tumorigenic and antitumorigenic factors in animals and humans. Cancers found in dogs include melanoma; non-Hodgkin lymphoma; osteosarcoma; soft tissue sarcomas; and prostate, mammary, lung, and colorectal carcinomas, as well as head and neck squamous cell carcinoma and transitional cell carcinoma of the bladder. 81 Approximately 1 in 3 dogs will be diagnosed with cancer during its lifetime, and cancer currently accounts for about half of the deaths of all dogs older than 10 years. Because standard therapy is usually palliative in canine cancer, there is an excellent opportunity to evaluate alternative approaches. Most advanced cancers are incurable; hence, it is important to prolong survival by blocking the process of carcinogenesis through chemoprevention, which is a feasible strategy for cancer prevention or inhibition of tumor growth or metastasis 83 ; greater application and study of this approach in domestic pets will ultimately benefit the health of both the animals and their owners.
Cancer chemoprevention aims to prevent, arrest, or reverse either the initiation phase of carcinogenesis or the progression of neoplastic cells to malignancy. It has been an active area of research for several decades, and chemoprevention is widely used and readily accepted as a strategy that reduces the risk for cancer. It can also be used in some apparently healthy dogs at risk for cancer to prevent or reduce their risk of developing invasive disease. Chemopreventive agents, either alone or in combination with each other, can delay the processes that lead to invasive cancer. Examples of effective chemoprevention agents that have been studied in humans include nonsteroidal anti-inflammatory drugs (NSAIDs), peroxisome proliferator-activated receptor-γ (PPARγ) ligands, and dietary compounds. We will summarize current chemoprevention research in canine cancer, with knowledge gained from human and laboratory animal studies, and look to the future of this research.
NSAIDs in Cancer Chemoprevention and Treatment
NSAIDs have been used for a long time in the treatment of inflammatory diseases and were first recognized for their potential anticancer activity after comparing cancer incidence in individuals that did and did not routinely use these agents. Despite the different structures, these drugs share a central anti-inflammatory therapeutic property in the inactivation of cyclooxygenase (COX, also known as prostaglandin H synthase). Two isoforms of COX have been characterized: COX-1 is constitutively expressed in many tissues, whereas mitogens, tumor promoters, and growth factors upregulate the expression of COX-2. NSAIDs block both COX enzymes, with greater or lesser specificity, resulting in reduced synthesis of prostaglandins, which play a pivotal role in inflammation (Fig. 1). During the last decade, numerous studies have shown that NSAIDs are chemopreventive for colorectal cancer and, to a lesser extent, breast and lung cancer in humans. Similar effects are seen in dogs administered piroxicam for transitional cell carcinoma. 65 The use of NSAIDs to abrogate tumor growth also has been demonstrated extensively in murine models of colorectal cancer, as well as in human clinical cancer cases. 26,37,108 The beneficial effects of NSAIDs in colorectal carcinogenesis have been established by numerous population-based studies and confirmed in 2 large, randomized clinical trials with the prodrug sulindac and the selective COX-2 inhibitor celecoxib. 27,98 The results showed that these drugs inhibit the growth of intestinal polyps and cause regression of existing tumors in patients with familial adenomatous polyposis. Thun et al. 109 reviewed evidence for chemopreventive effects of NSAIDs in colorectal and other cancers based on several population-based studies; however, Jankowski and Hunt 40 recently reported that there is still an increased risk of upper gastrointestinal complications with COX-2 inhibitors, and the risk may increase further in some people when aspirin is also consumed. Overall, a considerable body of data from experimental animal models to in vitro cell culture studies to numerous epidemiologic and clinical trials supports the use of these drugs as effective chemopreventive/therapeutic agents.
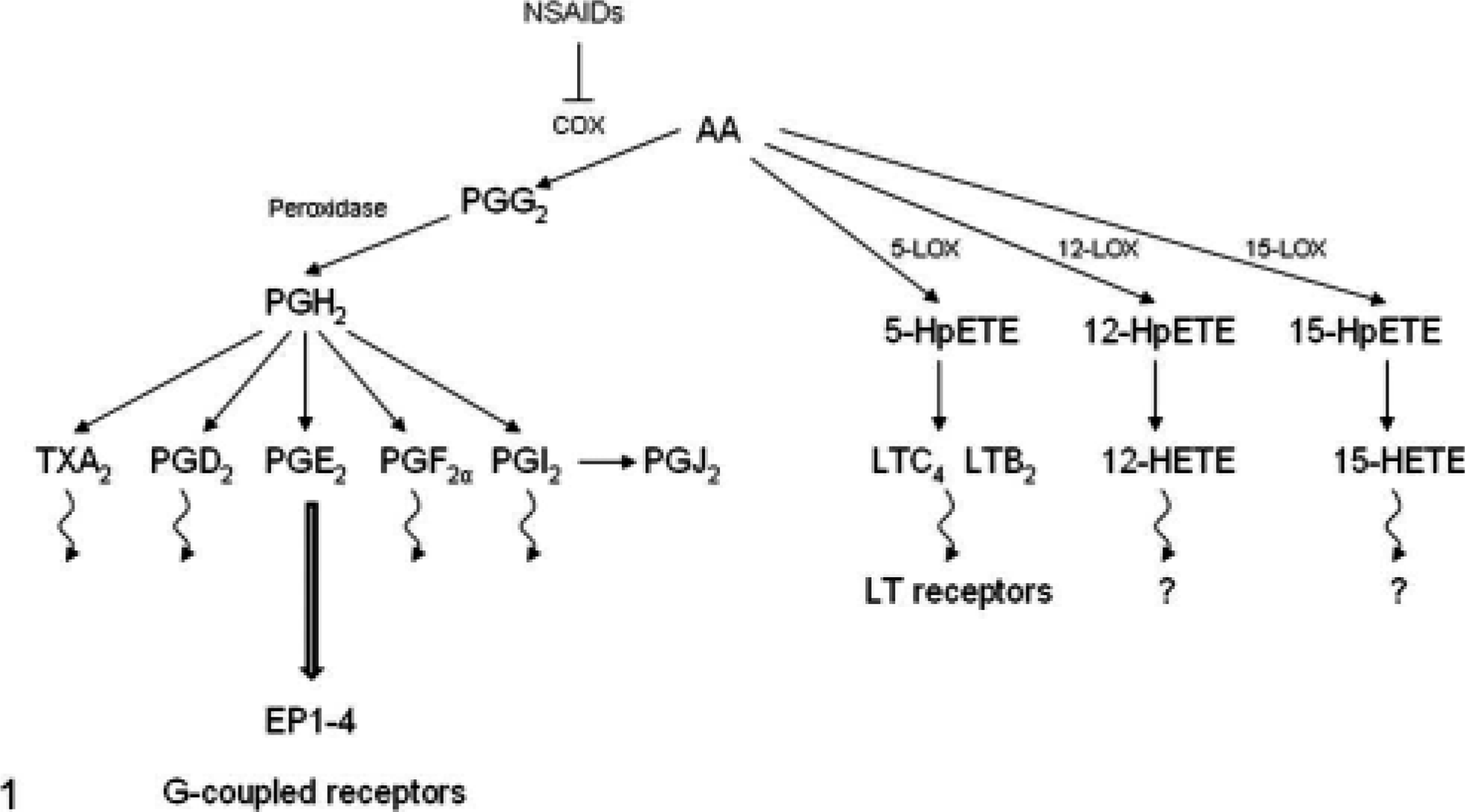
Schematic diagram of AA pathway. PG indicates prostaglandin; LT, leukotriene; TX, thromboxane; HETE, hydroxyeicosatetraenoic acid; and HpETE, hydroperoxyeicosatetraenoic acid.
Although the chemopreventive and antitumorigenic activity of NSAIDs against human and rodent cancers has been characterized extensively, the molecular responses and efficacy in canine cancer have not been elucidated clearly; however, because of the conserved nature of prostaglandin biosynthesis across species, it is entirely logical to expect mechanisms and efficacy in dogs to be similar to those in humans and rodents. Carprofen, piroxicam, and meloxicam are the most common NSAIDs prescribed in dogs (Fig. 2). Both piroxicam and meloxicam inhibit COX-2 activity and induce apoptosis in cell culture, and meloxicam has a greater selectivity for COX-2 in healthy dogs. 100 Administration of piroxicam to human cancer patients with pulmonary metastases induced minor remission in 5 of 31 individuals. 12 Piroxicam was subsequently tested in dogs with naturally occuring, invasive transitional cell carcinoma of the urinary bladder, resulting in remission in 12 of 18 cases. 65 These results were strongly associated with induction of apoptosis and a reduction in urine basic fibroblast growth factor concentration.
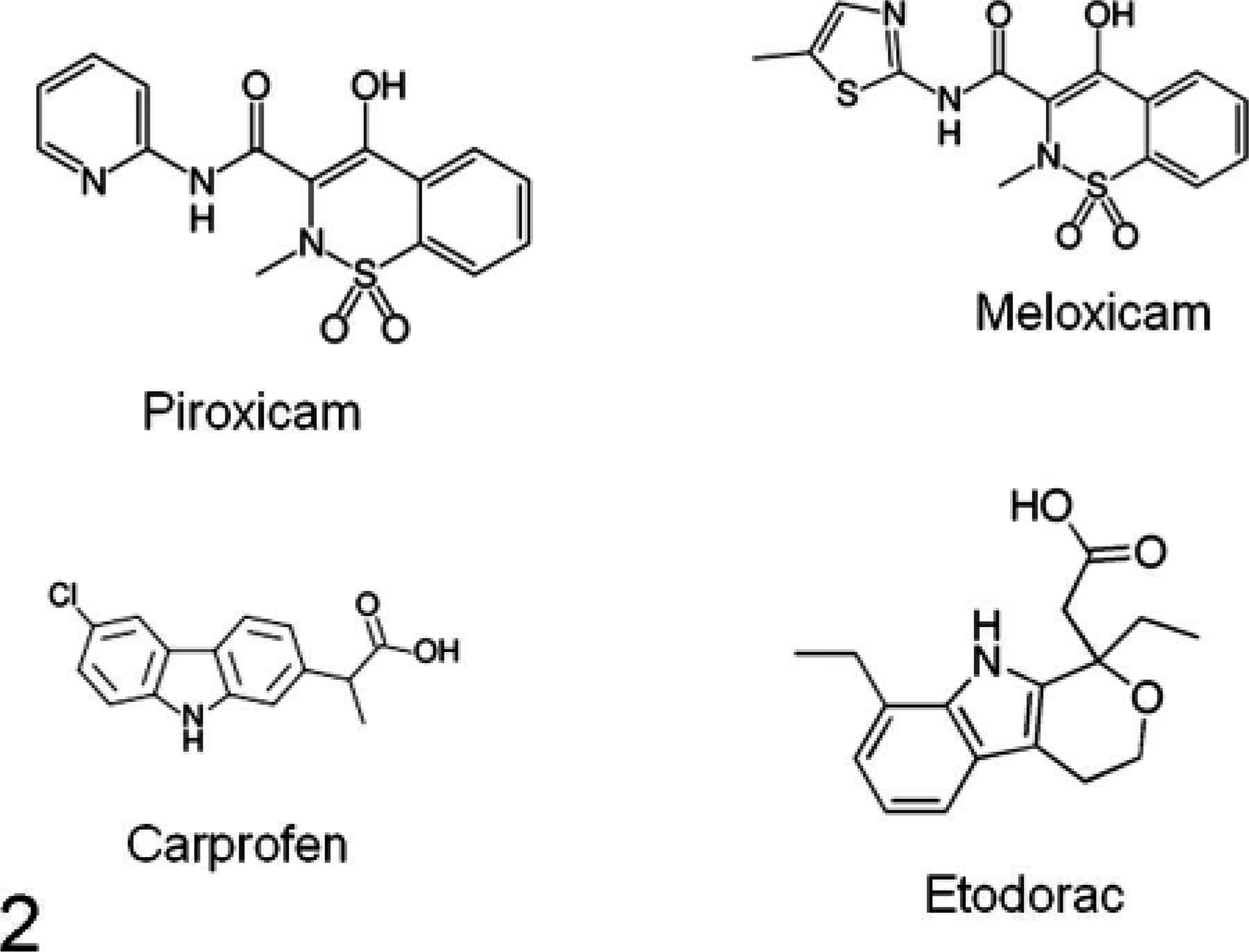
Molecular structure of NSAIDs commonly used in veterinary medicine.
Molecular Targets of NSAIDs in a COX Pathway
A wide range of molecular mechanisms responsible for the antitumorigenic effects of NSAIDs have been implicated in laboratory studies, with the most obvious being the inhibition of COX-2 and reduction of prostaglandin synthesis. As this aspect of NSAID activity was being investigated, it became clear that prostaglandin-independent mechanisms also were involved, particularly with respect to the induction of apoptosis.
COX-1 and COX-2 as molecular targets
Much of the focus on development of NSAIDs as chemopreventive drugs has been on their use as selective COX-2 inhibitors. COX-2 expression is low in most tissues—with some important exceptions—and expression is increased by cytokines and growth factors upregulated during inflammation and within tumors. 97 The importance of COX-2 in tumorigenesis has been demonstrated clearly in studies with COX-2 knockout mice, which are significantly less susceptible to chemically or genetically induced tumors of the skin, intestine, and mammary gland. 110 Although the focus on development of NSAIDs to prevent cancer shifted from conventional NSAIDs to selective COX-2 inhibitors, such as Celebrex and Vioxx, it is important to recognize that experiments using COX-1–deficient mice and COX-1–specific NSAIDs suggest that inhibition of this isoform may also be beneficial. For example, the number of intestinal polyps was reduced by 70 to 80% in the Min mouse model when either COX-1 or COX-2 genes were knocked out. 103 Interestingly, recent studies suggest that COX-1 is a potential target for prevention of ovarian cancer. Expression of COX-1 was found in human epithelial ovarian cancer, and the selective COX-1 inhibitor SC-560 reduced the growth of tumors in a nude mouse model. 19
The fact that NSAIDs affect antitumorigenesis in humans stimulates cancer research in other species, including dogs. COX-1 has not been studied as a chemopreventive target gene in dogs, but it has been reported that treatment of a canine mammary carcinoma cell line with NS-398 (a specific COX-2 inhibitor) significantly blocked prostaglandin E2 (PGE2) synthesis and reduced cell proliferation. 14 The authors concluded that some neoplastic canine mammary cell lines constitutively overexpress COX-2, and that COX-2 inhibition decreases PGE2 production and cell proliferation, supporting a role for COX-2 and prostaglandins in canine mammary tumorigenesis. A number of studies also have investigated the expression of COX-1 and COX-2 in canine tumor tissues, primarily by immunostaining in mammary, prostate, ovarian, colorectal, nasal, and bladder carcinomas and in osteosarcoma (Table 1, Fig. 3). Although most of these studies demonstrate upregulation of COX-2 protein expression in tumors, this should not be interpreted to directly implicate functional activity in generating any particular bioactive product. The human colorectal cancer cell line HT-29 highly expresses COX-2 protein as determined by immunohistochemistry and Western blot analysis; however, there is no detectable PGE2 in these cells as assessed by high-performance liquid chromatography. 35 Similarly, the clinical response in dogs with transitional cell carcinoma treated with piroxicam therapy was not predicted by intratumoral COX-2 expression before treatment. 72
Summary of COX- 1 and COX-2 expression in canine tumors. Number of dogs with COX expressed over total number of dogs are shown.∗
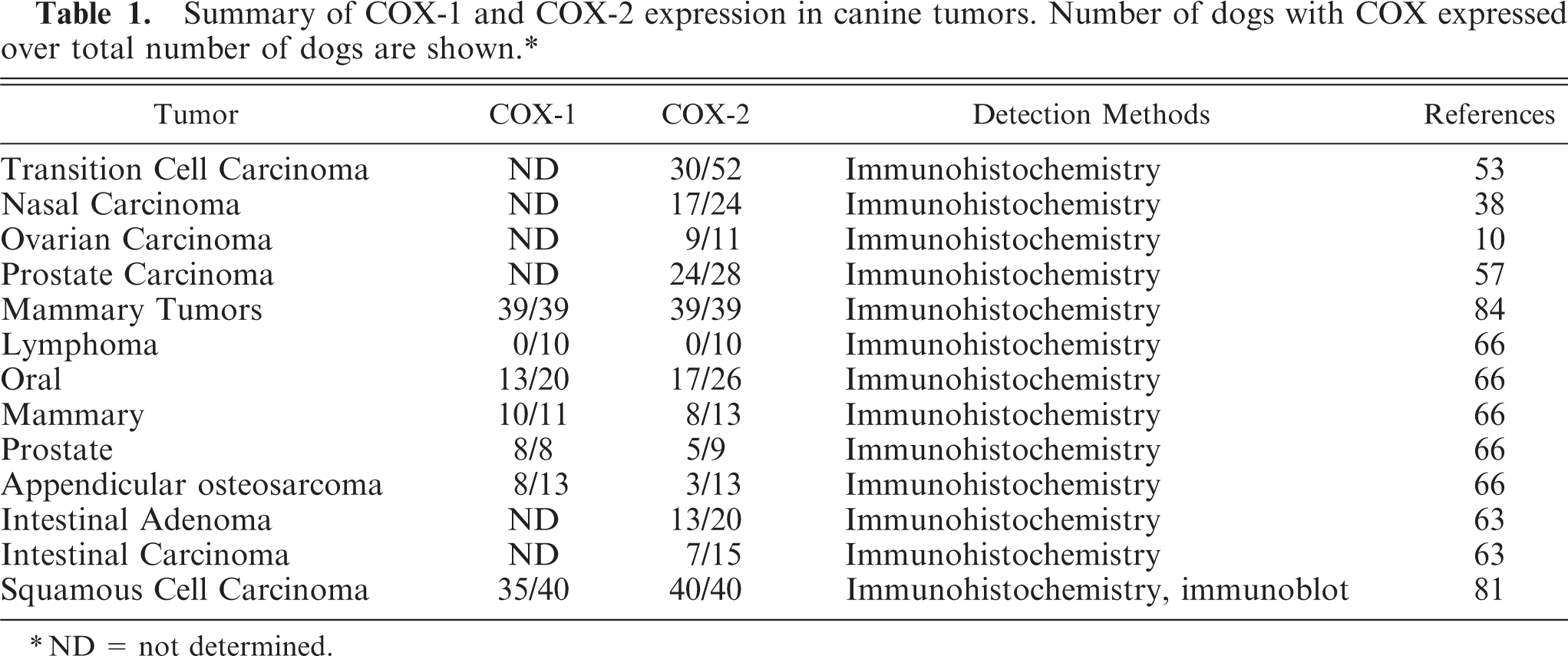
∗ND = not determined.
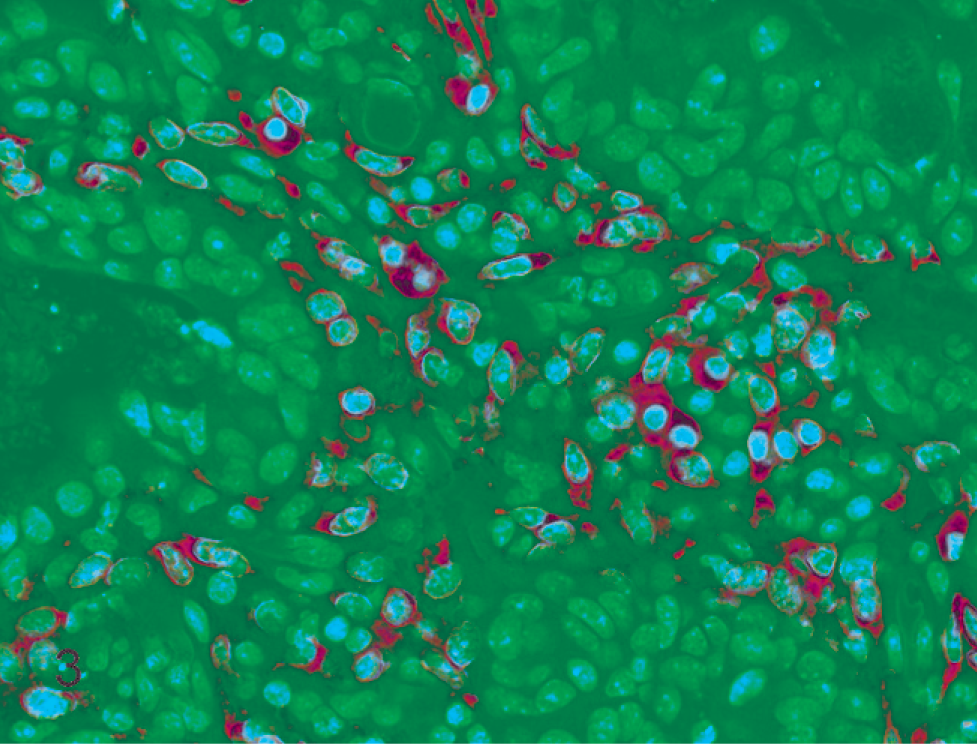
Immunostaining of COX-2 in canine tumors. COX-2 protein expression is commonly increased in neoplastic cells and/or the supporting stroma of epithelial tumors, as in this canine colorectal adenoma. Autocrine and paracrine effects of the prostaglandin metabolites on tumor growth would be similar, regardless of where COX-2 is expressed. Immunohistochemistry, COX-2 polyclonal antibody (Cayman Chemical), Mayer hematoxylin counterstain.
Inhibition of prostaglandin formation and cancer prevention
The major target of NSAIDs is COX activity, with the desired goal of reducing prostaglandin formation. The critical role of prostaglandins in the development of cancer is supported by a considerable body of data, which largely points toward PGE2 as a protumorigenic agent of COX metabolism. Prostaglandins produced by specific enzymes, such as PGE synthase (PGES), exert their biologic activity by binding a family of receptors, such as EP for PGE receptors and FP for PGFα receptors. 111 There are 4 known EP receptors: EP1–EP4. 13 Studies with receptor knockout mice and receptor-specific antagonists and agonists have implicated signaling through EP2 as important in tumorigenesis. Genetic disruption of the EP2 receptor decreased the number and size of intestinal polyps in a mouse model of human familial adenomatous polyposis, whereas disruption of the EP1 and EP3 receptors had no effect. 100 A recent study with MMTV-COX-2 mice, which develop mammary tumors in multiparous females, indicates a requirement for the EP2 receptor. 16 EP2 is a G-protein–coupled receptor that increases cyclic adenosine monophosphate, followed by activation of the protein kinase A (PKA) signaling pathway. The activated PKA pathway leads to an increase in amphiregulin, enhancement of the RAS-MAP kinase pathway, and transactivation of the PPARδ receptor pathway. 117 Furthermore, the PKA pathway phosphorylates GSK-3β, altering the important APC/β-catenin/TCF pathway to regulate cell proliferation, angiogenesis, and apoptosis. 15 In dogs, conjugated linoleic acid (CLA) decreases EP2 expression in mammary cells. 114 This is the first report of EP expression in canine cells. Further, we could speculate that the knowledge obtained from canine studies may also be beneficial to the study of human breast cancer.
The importance of PGE2 in tumorigenesis also has been demonstrated by targeting PGES activity. It has been reported that genetic deletion of mPGES-1 in APC mutant mice results in marked and persistent suppression of intestinal cancer growth by 66%, whereas suppression of large adenomas (>3 mm) was almost 95%. 74
NSAIDs and lipoxygenases
The inhibition of cyclooxygenase activity may increase availability of the substrate, arachidonic acid (AA), for metabolism by other enzymes and may result in a shift of the metabolite profile from prostaglandins to hydroxylated metabolites (Fig. 1). Lipoxygenase (LOX) activity has been implicated in several types of neoplasia, and although COX inhibition may reduce one protumorigenic signaling pathway, shuttling of AA through another metabolic pathway may promote tumor growth. In fact, dual inhibitors of COX and LOX are currently being developed and tested. Licofelone is one such drug in the advanced stages of clinical trials for treatment of inflammatory diseases 68 and colorectal cancer in humans. 106 Encouraging results should prompt further testing of Licofelone as a potential chemopreventive or therapeutic agent in dogs.
COX-Independent Molecular Targets of NSAIDs
The chemopreventive effects of certain NSAIDs appear to be mediated through both COX-dependent and COX-independent pathways, but the latter are not well characterized.
NSAID-activated gene-1 (NAG-1)
NAG-1 protein has broad activity in inflammation and cancer, as indicated by the diversity of nomenclature (MIC-1, GDF-15, PLAB, and PDF). 2,24 Its biologic activity and molecular mechanisms of action are still being studied, but it is clear that NAG-1 shares some of the common functions inherent in the transforming growth factor-β (TGF-β) superfamily of cytokines. 2 For instance, TGF-β1 induces apoptosis and cell growth arrest in epithelial cells, as also reported for NAG-1, and TGF-β1 knockout mice die of widespread inflammation. 76 Indeed, NAG-1 appears to have some anti-inflammatory activity, because its expression reduces tumor necrosis factor-α secretion in macrophages. 9 In addition, NAG-1 expression inhibits proliferation of primitive hematopoietic progenitors 22 and several epithelial cancer cell lines, 4–7,104 reflecting the activity of a multifunctional cytokine. Ectopic expression of NAG-1 causes cell growth arrest of cancer cells as assessed in soft agar and cloning efficiency assays. 5,6 Further, overexpression of human NAG-1 in human colon and glioblastoma cells inhibits tumor formation in nude mice. 1,5
NAG-1 expression in normal and transformed tissue has been reported. Expression of NAG-1 in surface epithelium of normal human intestinal villi occurs in regions undergoing apoptosis and is downregulated in colon tumors compared with adjacent normal tissue. 46 NAG-1 is expressed in the normal tracheobronchial epithelia but not in areas of squamous metaplasia or lung tumors. 75 Thomas et al. 107 found NAG-1 expression to be downregulated in 8 of 10 primary prostate cancers, although conflicting results also were presented. 45 This apparent dichotomy in NAG-1 expression in normal cells and tumors of the prostate has not been explained adequately and raises the possibility that NAG-1 plays distinctly different roles in different organs or at different stages of tumor progression. Similar to TGF-β1, these observations also provide evidence for a dual role for NAG-1 in cancer progression: the suppression of tumorigenesis in normal tissue at the early stages of cancer development and the promotion of tumor invasiveness and survival at more advanced stages of disease. The NAG-1 receptor and immediate downstream signaling mediators have yet to be identified, but these may provide an answer for this dichotomy. Despite conflicting data on expression in tumors, NAG-1 has been clearly documented to suppress tumor growth in mouse models of cancer. We recently cloned the canine NAG-1 gene and investigated its expression in canine tissues. 119 The predicted canine NAG-1 amino acid sequence has 9 cysteine residues and an RXXR sequence also conserved with human, mouse, rat, and chimpanzee NAG-1, suggesting that canine NAG-1 protein may have a similar biologic activity to other species. In fact, canine NAG-1 is induced by several NSAIDs, with the most robust upregulation by piroxicam in osteosarcoma cells. 119 This observation is consistent with the notion that NAG-1 plays an important role as a mediator for chemopreventive agents in canine cancer.
Early growth response-1 (EGR-1)
EGR-1 is a transcription factor (also known as NGFI-A, Zif268, krox24, and TIS8) that preferentially binds to the GC-rich DNA core sequence to induce gene expression. EGR-1 is also a member of the immediate early gene family and encodes a nuclear phosphoprotein involved in the regulation of cell growth and differentiation. A number of reports indicate that EGR-1 acts as a tumor suppressor gene. EGR-1 is downregulated in tumors and an array of tumor cell lines 36 and is induced by several tumor suppressor proteins. 82,85 We also have identified EGR-1 as another NSAID-induced gene. 4 Thus, NSAIDs may influence the expression of many other genes via their ability to increase the expression of tumor suppressor proteins and thereby inhibit tumorigenesis. The expression of EGR-1 has not been investigated in normal or neoplastic canine tissues.
Other molecular targets of NSAIDs
In addition to NAG-1 and EGR-1, a number of other genes associated with tumor development are altered by physiologic concentrations of NSAIDs. For example, indomethacin suppresses the expression of the extracellular matrix protein laminin-γ1 in human glioblastoma cells, thereby reducing the capacity for invasion by this brain tumor cell. 39 Two genes, TSP-1 and ATF3, are also increased by NSAIDs, 11,67 and both proteins attenuate the invasion of tumor cells. Because gene alteration by NSAIDs has been frequently associated with the effects on NSAID-induced antitumorigenesis, these altered genes may be considered for examination in canine cancer research.
PPARγ Ligands as Chemopreventive Compounds
PPARγ is a ligand-activated transcription factor belonging to the steroid receptor superfamily. 94 Three isoforms (α, β/δ, and γ) have been identified and are encoded by separate genes. All PPAR isotypes form a heterodimeric complex with the retinoid X receptor, and the complex binds to the PPAR response element, which functions as the central regulator of cellular differentiation, 112 apoptosis, 32,120 inflammatory responses, 42,88 lipid metabolism, and metabolic disease. 77 PPARα activation is responsible for the pleiotropic effects of peroxisome proliferator drugs, such as enzyme induction, peroxisome proliferation, liver enlargement, and anti-inflammatory activity, 47 and it plays a critical role in the regulation of cellular uptake and β-oxidation of fatty acids. 61 PPARδ (also known as PPARβ) is expressed at relatively high levels in the brain, colon, and skin, and it has been reported a key regulator with the potential to therapeutically target multiple aspects of the metabolic syndrome. PPARγ is expressed in multiple normal tissues, such as those in the breast, colon, lung, ovary, and placenta. It promotes cell differentiation (particularly in adipocytes) and has anti-inflammatory effects. The ability of PPARγ to regulate cell differentiation and proliferation has inspired a number of researchers to explore the use of PPARγ agonists as chemopreventive/chemotherapeutic agents. 71,89 PPARγ is highly expressed in a wide variety of human cancer cell lines, 17,48,69,92,93 and introduction of PPARγ ligands induces apoptosis and growth inhibition. Troglitazone was voluntarily withdrawn from the market in March 2000 because it caused idiosyncratic liver injury, but a new class of thiazolidinediones, represented by MCC-555 (KRP-297, RWJ-241947), may represent a safe alternative, with antidiabetic activity validated in animal models of type 2 diabetes. Like other thiazolidinediones, MCC-555 binds to PPARγ and affects its transcriptional activities, but it also binds to PPARα and represents a dual PPAR agonist. 118
Defining the physiology of PPARs in dogs is important not only to help us understand the pathophysiology of obesity in dogs, but also to establish the significance of these drugs in treating canine cancer. A canine PPARα sequence has been reported, 73 and canine PPARγ and PPARβ sequences have been identified recently. Canine PPARγ shares greater homology with human PPARγ than with that of other species and is expressed in adipose tissues, spleen, lung, and large intestine 76 similarly to other species. Paciello et al. 79 showed that the pattern of PPARγ expression differed between normal and neoplastic canine nasal epithelium. We also have shown that rosiglitazone (a PPARγ agonist) induced expression of apoptosis-related genes, including NAG-1, in a canine osteosarcoma cell line. These results implied the possibility of the usage of PPARγ ligands in canines with osteosarcoma. These results also will provide the importance of this transcription factor in the pathophysiology of several different tumors and will stimulate further research in this field and open new opportunities for the treatment of canine cancer.
Dietary Compounds and Cancer Chemoprevention
Epidemiologic studies have strongly suggested that nutritional factors play an important role in carcinogenesis and have associated a thin body condition score in 9- to 12-month-old female dogs with a significantly decreased risk of developing mammary carcinoma later in life. 60,96 Obesity increases the risk of developing cancer in people and dogs. For example, obesity was identified as a risk factor in association with pesticides for the development of transitional cell carcinomas in Scottish Terrier dogs. 29 Thus, maintaining ideal body weight may also reduce the risk for the development of a variety of tumors and reduce the incidence of pancreatitis, diabetes mellitus, and bone and joint diseases. Recently, studies of lifelong diet restriction in Labrador Retrievers indicated a 1.8-year longer survival in the leaner dogs. 52 It also has been estimated that, on average, a third of cancer morbidities and mortalities might be prevented by dietary modification. 33,87 Therefore, dietary components may be considered very important in carcinogenesis, and epidemiologic studies indicate that human populations consuming foods rich in specific phytochemicals have lowered incidence of cancer, heart disease, and osteoporosis. However, antitumorigenic efficacy of such dietary factors in dogs has not been adequately addressed.
Dietary phytochemicals are found in plant products, such as fruits, vegetables, beverages, herbs, and spices, and a number of these compounds have been found to inhibit tumorigenesis in experimental animals and/or exhibit potent biologic properties. 115 Absorption, metabolism, and/or degradation of phytochemicals would be of interest in their activity. The bioavailability of many phytochemicals has been studied in detail in humans. 54 When it comes to canine studies, some phytochemicals, like green tea catechin and ipriflavone, showed a similar bioavailability compared with humans. 32,38 However, the bioavailability of most phytochemicals in dogs has not been studied in detail. In contrast to dietary compounds, Dalvie et al. 20 reported that glucuronidation was the primary route of metabolism in humans and dogs when they were administrated the MMP inhibitor CP-544439. Interestingly, drug metabolism with food was different between humans and dogs. In contrast to observations in human studies, metabolism of allopurinol (a drug for gout) in dogs is not influenced by diet 8 ; however, aspartame in dogs and humans is digested in the same way. 86 Thus, the bioavailability of phytochemicals or drugs depends on species and compounds.
We have been studying several phytochemical compounds, including resveratrol, indol compounds, genistein, and 6-gingerol, in the chemoprevention of human and canine cancer. 3,6,54,55,116 Other groups also have examined the antitumor effects of phytochemicals at the cellular level, and it appears that the main effect is induction of apoptosis and cell cycle arrest. Other potential mechanisms may include antioxidative activity, 58 inhibition of enzymes related to tumor promotion, such as COX and LOX, 18 inhibition of activator protein-1, 25 inhibition of vascular endothelial growth factor (VEGF), 95 angiogenesis, 121 and others. 102 Thus, phytochemicals influence many tumor-related signaling pathways, but the mechanisms by which specific phytochemicals induce apoptosis or antitumorigenic effects remain to be elucidated.
In contrast to laboratory and epidemiologic studies in humans, veterinary research addressing anticancer effects of dietary compounds has only just begun in domestic animals. There are a few reports indicating that flavonoids may affect cell growth arrest in canine cancer cell lines, but this has not been evaluated clinically in dogs. The increased marketing of dietary compounds as alternative remedies for canines with cancer currently lacks the mechanistic and clinical studies required to support broad recommendations for use. As noted earlier, neoplastic diseases in humans and dogs are very similar, and greater study of phytochemicals in canine cancer would not only benefit domestic animals, but also their owners.
Green tea
Antitumor effects of green tea catechins (particularly EGCG) include apoptosis and cell cycle arrest. 30,34 It was shown recently that EGCG suppressed the angiogenic factors basic fibroblast growth factor and VEGF, suggesting application not only in chemoprevention but also in therapy. 101 However, there are essentially no studies examining the effects of green tea components in canine cancer.
CLA
Scientific interest in CLA was sparked in 1987, when Dr. Pariza's team at the University of Wisconsin-Madison recognized that it inhibited chemically induced skin tumors in mice. 31 Since then, CLA has been shown to inhibit growth of human colon, breast, and melanoma cancer cells, as well as chemically induced cancer in the colon, mammary gland, and forestomach in animals. CLA may influence LOX and COX metabolic pathways. CLA is incorporated into membrane phospholipids, and therefore competes with AA to alter eicosanoid production. Indeed, CLA has been shown to modulate COX-2 expression and metabolite production in human prostate cancer, 78 as well as in human breast tumor cells. 59 CLA may induce proapoptotic gene expression to modulate tumorigenesis, 56 as well as suppress growth of malignant and nonmalignant canine mammary tumor cells in vitro and suppress EP2 protein expression. 114 The data indicate that the dietary component CLA regulates COX-2 and EP2 protein expression in both malignant mammary cells and cells from the tumor-associated stromal compartment. In turn, this may suppress PGE2 signaling, leading to a better prognosis.
Polyunsaturated Fatty Acids (PUFAs)
PUFAs are essential in the diet and are represented by 2 parallel families of fatty acids distinguished by their unique chemical structure: n-3 (or omega-3) PUFAs have their first double bond 3 carbons from the methyl end, whereas the first double bond is located at the sixth carbon for n-6 PUFAs. The n-3 and n-6 PUFAs are not interconvertible in mammals and are only obtained from the diet. The most abundant PUFA in the human diet is the short-chain n-6 PUFA linoleic acid. This is elongated and desaturated to form the n-6 PUFA AA, which serves as the substrate for generation of diverse bioactive lipids, such as PGE2, through the activity of COX, LOX, and other metabolic enzymes. Tissue AA content and generation of these bioactive lipids can be reduced significantly by inclusion of long-chain n-3 PUFAs, such as eicosapentaenoic acid in the diet. 64 This long-chain n-3 PUFA is currently obtained almost exclusively from fish or fish oil, but work is underway to increase availability in terrestrial/plant sources, such as canola oil. 113 During the past decade or so, the health benefits of dietary omega-3 PUFAs and fish oil in humans have been studied widely, and this has resulted in some commercial pet food manufacturers including these PUFAs in their dietary formulations. 91 The primary beneficial effects of increasing long-chain n-3 PUFA content in tissues is the reduction of AA and its proinflammatory metabolites, but these PUFAs may also act directly in modulating signaling pathways relevant to inflammation and cancer. 43
Vitamin D
The anticarcinogenic properties of vitamin D have been reported extensively. 19,105 The vitamin D receptor (VDR) is a nuclear ligand-activated receptor that is expressed in almost all tissues in the body; this widespread distribution indicates a pivotal role for vitamin D in several physiologic conditions. In fact, experimental studies have shown repeatedly that vitamin D can inhibit cell proliferation, induce differentiation, and promote apoptosis, processes directly involved in the development of human carcinogenesis. Animal and observational data have confirmed consistently that vitamin D protects against colorectal neoplasia. A diversity of scientific literature, including in vitro, animal, ecologic, and epidemiologic studies, supports a role for vitamin D in decreasing colorectal cancer incidence. 62,95 However, despite abundant experimental evidence in support of an inverse association between vitamin D status and breast cancer risk, 90 the available epidemiologic evidence provides, at best, limited support for such an association. 21,28 Similarly, the association between vitamin D status and prostate cancer risk is less clear than that for colorectal cancer, which suggests that not all tissues respond identically to vitamin D. 26,49,70 In veterinary studies, calcitriol (VDR agonist) and other analogs when added to several canine cancer cell lines, including transitional cell carcinoma cells, canine squamous carcinoma cells, and canine adenocarcinoma, inhibited cell growth via induction of cell cycle arrest. 41,44,46–48 These data extend the potential use of VDR agonists to canine cancer and provide a sound rationale for further clinical testing.
Prospective Cancer Chemoprevention Research in Canine Cancer
Naturally developing tumors in client-owned dogs present a unique scientific opportunity to evaluate the benefits of chemopreventive drugs. The findings from such studies would guide tumor prevention in dogs and would provide valuable information for future studies in people. There are breed predilections for certain tumors. Giant breeds of dogs are at increased risk for developing osteosarcomas. Large-scale and double-blinded studies of NSAIDs or dietary supplements in altering the risk of developing osteosarcoma in giant breeds of dogs are feasible. Similar studies with Scottish Terriers that are at a high risk for developing transitional cell carcinomas of the bladder could be done. Because of the increased likelihood of developing tumors in certain breeds and the shorter lifespan of dogs compared with people, meaningful data could be generated more rapidly. In addition to the classic chemoprevention, the role of previously discussed compounds as adjunct therapy to standard of care cancer treatment can be evaluated easily. Most owners would readily accept the addition of low-toxicity agents, such as green tea catechins and conjugated linoleic acid, as adjuncts to chemotherapy. The sale of these compounds has already created a multimillion-dollar industry, with limited studies to justify their supplemental use in chemotherapy or radiation therapy. The value of COX inhibitors, NAG-1 inducers, and other agents that modify inflammatory responses should also be evaluated in an adjuvant setting to determine their value.
Footnotes
Acknowledgements
We thank Misty Bailey for her critical reading of manuscript. This work was supported by grants from the American Cancer Society (CNE-111611), National Institutes of Health (R01CA108975), and the University of Tennessee Center of Excellence in Livestock Diseases and Human Health to S.J.B.
