Abstract
Background
The short synacthen test (SST) is used to investigate patients with suspected hypothalamus–pituitary–adrenal (HPA) axis pathology. A rise of serum total cortisol (total cortisol) above 550 nmol/L is accepted as sufficient adrenal reserve. In total, 80% of cortisol is bound to cortisol-binding globulin (CBG) and 10% to albumin. In the acute phase responses CBG concentrations decrease and can influence the interpretation of SST. The free cortisol index (FCI) is a surrogate marker for free cortisol and is defined as total cortisol (nmol/L)/CBG (mg/L) with an FCI > 12 representing sufficient adrenal reserve. The aim of this study was to compare total cortisol and FCI in the interpretation of SST in patients with liver impairment.
Method
SST was done on 26 patients with liver impairment. Total cortisol was measured on Advia Centaur; serum CBG by radioimmunoassay and FCI calculated.
Results
Eleven (42%) patients had a total cortisol >550 nmol/L (range 555–2070) and FCI > 12 (12.0–68.9) suggesting sufficient cortisol reserve. Three patients (13%) had total cortisol <550 nmol/L (268–413) and FCI < 12 (3.5–11.6) consistent with cortisol deficiency. Twelve patients (46%) had a total cortisol <550 nmol/L (144–529), but an FCI > 12 (12.0–52.9). None of the patients had a total cortisol >550 nmol/L and FCI < 12.
Conclusion
When total cortisol alone is used to interpret SST in patients with liver impairment, 46% may have been classified as having adrenal insufficiency because of low CBG. FCI may be better for the evaluation of HPA axis insufficiency in patients with liver impairment.
Introduction
The short synacthen test (SST) is used to investigate patients with suspected hypothalamic–pituitary–adrenal (HPA) axis pathology. A rise of total cortisol above 550 nmol/L at 30 min postsynacthen is accepted as sufficient adrenal reserve. 1 An incremental increase in total cortisol, calculated as the difference between the maximum response and baseline concentrations following SST, is generally used for evaluation of adrenal response in the critical care setting. An increment of >250 nmol/L at 30 min postsynacthen is used to indicate sufficient adrenal reserve. 2
Cortisol-binding globulin (CBG) is a plasma glycoprotein that is primarily synthesized in the liver. Approximately 80% of cortisol is bound to CBG and 10% to albumin. 3,4 A decreased CBG-binding activity, seen in the acute phase responses, 5,6 can reduce total cortisol and may affect the interpretation of an SST. Furthermore, CBG concentrations have been reported to decline following synacthen administration. 7 Total cortisol measurement may underestimate cortisol production when CBG levels are low. Furthermore, binding capacity of CBG is significantly lower in liver cirrhosis compared with normal subjects and those with fatty liver or toxic fibrosis. 8 Adrenal dysfunction is very common in acute liver disease and may contribute to haemodynamic instability and mortality. 2 Failure to identify secondary causes for adrenal insufficiency can lead to mortality and needless long-term glucocorticoid replacement can cause significant morbidity. 5
There are a number of methods to measure serum free cortisol, such as ultrafiltration, 4 gel filtration 9 and equilibrium dialysis. 10 However, these techniques are time consuming and expensive, making them currently unsuitable for routine laboratory use. The free cortisol index (FCI) has been shown to be a surrogate marker for serum free cortisol 11 and is defined as total cortisol (nmol/L)/CBG (mg/L). An FCI > 12 at 30 min postsynacthen is representative of sufficient adrenal reserve. 5 An incremental increase in total cortisol, calculated as the difference between the maximum response and baseline concentrations following SST, is generally used for the evaluation of adrenal response in the critical care setting. Increment of >250 nmol/L is used to indicate sufficient adrenal reserve. 2 The aim of our study was to compare the use of total cortisol and FCI in the interpretation of SST in patients with liver impairment.
Methods
Data were collected retrospectively on 26 patients (17 men and 9 women) with liver impairment, who had undergone a 250 μg SST. Total cortisol was measured on Advia Centaur (coefficient of variation: 4.22–4.98%) and serum CBG by radioimmunoassay (DRG Diagnostics, Marburg, Germany). Albumin and bilirubin were measured on Advia 2400.
CBG assay
All serum samples were assayed in duplicate. Samples were initially diluted 25 folds in phosphate buffer containing NaCl, NaN3 and bovine serum albumin (BSA). Hundred microlitres of diluted serum samples, standards and quality controls reacted with 100 μL, 125I-labelled CBG and 100 μL antiserum for two hours at room temperature. After two hours, immunoabsorbent (100 μL) was added and incubated for 20 min at room temperature. Tubes were then centrifuged for 15 min at 1500
FCI was calculated from the following equation:
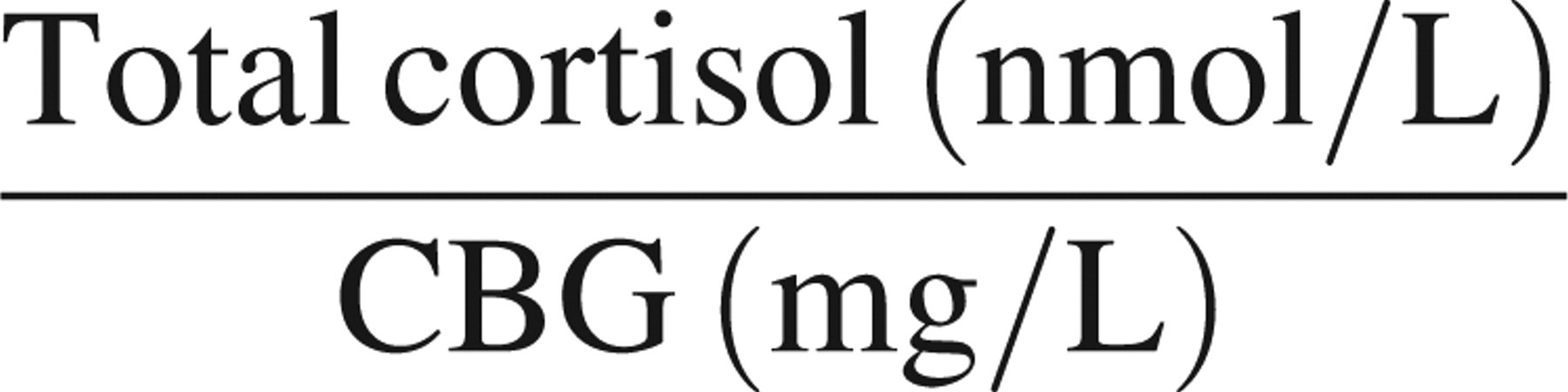
Results
The patients had a mean age of 48 ± 9 yr (mean ± SEM), baseline cortisol 430 ± 86 nmol/L, albumin 21 ± 4 g/L (reference range: 35–50 g/L), total protein 47 ± 10 g/L (60–80 g/L), bilirubin 137 ± 26 μmol/L (2–20 μmol/L), alkaline phosphatase 161 ± 33 IU/L (30–130 IU/L), aspartate aminotransferase 503 ± 103 IU/L (10–50 IU/L), gamma-glutamyl transferase 212 ± 43 IU/L (1–55 IU/L), sodium 140 ± 28 mmol/L (135–145 mmol/L), potassium 4.3 ± 0.9 mmol/L (3.5–5.0 mmol/L), creatinine 195 ± 40 μmol/L (40–120 μmol/L), urea 13 ± 3 mmol/L (3.3–6.7 mmol/L) and CBG 27 ± 5 mg/L (25–50 mg/L).
Underlying liver impairments on admission were alcoholic liver disease, viral hepatitis, autoimmune hepatitis, paracetamol overdose, primary biliary cirrhosis, hepato cellular carcinoma and secondaries. Fifteen patients had chronic liver disease (Child-Pugh score ranging from B8 to C13 and Model for End-Stage Liver Disease [MELD] score of 24 ± 6), 11 had acute liver disease. Five out of the 26 patients had alcoholic liver disease. None were on exogenous cortisol prior to SST. There was no correlation between albumin and CBG concentrations.
Eleven (42%) patients had total cortisol >550 nmol/L (range 555–2070) and FCI > 12 (12.0–68.9) suggesting sufficient cortisol reserve. Three patients (13%) had total cortisol <550 nmol/L (268–413) and FCI < 12 (3.5–11.6) consistent with cortisol deficiency. Twelve patients (46%) had total cortisol <550 nmol/L (144–529), but an FCI > 12 (12.0–52.9) implying a discrepancy. None of the patients had total cortisol >550 nmol/L and FCI < 12 (Table 1). Seven (25%) patients had an increment of >250 nmol/L (252–891), none of them had FCI < 12 (12.0–68.9); however, four (57%) out of the seven had total cortisol <550 nmol/L (391–521).
Sufficient adrenal reserve with total cortisol >550 nmol/L compared with free cortisol index (FCI >12)
Discussion
This is the first study looking at the use of FCI in interpreting SST in patients with liver impairment. Importantly, CBG is not routinely taken into account when interpreting SST based on total cortisol in this group of patients. The current methods available for the measurement of serum free cortisol are cumbersome and not suitable for routine laboratory use. However, the strong correlation between free cortisol and FCI implies that FCI may be a useful surrogate marker of free cortisol.
Salivary cortisol measurement reflects the free and biologically active fraction of cortisol in serum and has the potential for the investigation of possible hypoadrenalism with SST. 12 However, the use of salivary cortisol in the interpretation of SST needs to be validated in patients with liver impairment. In our study, we have demonstrated that 46% of patients may have a diagnosis of adrenal insufficiency due to low CBG when total cortisol alone is used to interpret SST results. The supplementary use of total cortisol increment >250 nmol/L reduced the percentage of diagnosed adrenal insufficiency, although there was still a discrepancy with FCI in 32% of cases. FCI should be considered for the evaluation of HPA axis in patients with liver impairment who have a borderline total cortisol concentration at 30 min postsynacthen.
DECLARATIONS
