Abstract
Objective:
To correlate the prostatic volume (PV) with the participants’ age, body mass index (BMI), clinical symptoms, and renal ultrasonographic findings.
Materials and Methods:
One hundred participants were enrolled in a quantitative prospective study from August 2024 to October 2024. They were selected through a random sample; the inclusion criteria included participants with renal or lower urinary tract symptoms (LUTS). Patients with prostatic tumors or who were unwilling to participate were excluded. All participants underwent a prostate sonogram. The transabdominal ultrasonographic images were obtained with the participant lying supine on an examination table. The prostate was evaluated for volume (PV) and echotexture. A chi-square test, Pearson’s correlations, and univariate regression analysis were conducted to determine statistical correlations.
Results:
The mean age of the participants was 41.8 ± SD 12.1 years, the mean cohort’s PV was 24.37 ± SD 18.1 cm3, and the mean cohort’s body mass index (BMI) was 27.9 ± SD 4.6 kg/m2. There was significant strength of associations found between the PV and clinical findings, renal ultrasonographic findings, age, and BMI (
Conclusion:
Based on the results of this cohort study, PV may have a significant correlation with clinical symptoms, renal ultrasonographic findings, age, and BMI.
The accurate estimation of prostatic volume (PV) is crucial to assess a variety of medical conditions, such as determining urinary outflow obstruction, the degree of hyperplastic enlargement, and in selecting the best surgical treatment. Prostatic volume can also be used to determine which patients, with prostatic cancer, are suitable for brachytherapy, as a PV above 50 mL is typically excluded from this treatment. 1
Expert opinion 2 has been that a normal PV is 20 cm3 (20 milliliters [mL]), while others 3 have indicated that a normal PV ranges from 25 to 30 cm3. 4 Bhat et al 5 has suggested that the upper limit of the normal PV is 30 cm3. An enlarged prostate, also referred to as benign prostatic hyperplasia (BPH) is a histologic diagnosis that refers to the proliferation of smooth muscle and epithelial cells, within the prostatic transition zone. Strand et al 6 indicated that the incidence rates of lower urinary tract symptoms and BPH increases approximately 10%, per decade of life, starting at 40 years of age. Factors such as age, genetics, and geography have been noted to have a significant effect on the etiology of BPH. 7
To estimate PV, various techniques have been employed, including digital rectal examination, which is considered an unreliable method, as well as transrectal ultrasonography (TRUS), and magnetic resonance imaging (MRI). 8 Transabdominal ultrasonography is a valuable diagnostic method for estimating PV.1,9
Prostatic volume assessment has significant clinical value in determining the degree of prostatic BPH, the resultant tendency toward urinary tract outflow obstruction, and in selecting suitable surgical treatment or brachytherapy options. The modifiable factors, such as sex steroid hormones, cardiovascular disease, the metabolic syndrome, obesity, diabetes, diet, physical activity, and inflammation, are clinical risk factors for BPH that, when controlled, can provide opportunities for good treatment and prevention. 7
The objective of this study was to use transabdominal sonography to estimate PV and correlate its mean values with participants’ age, body mass index (BMI), renal ultrasonographic findings, and clinical symptoms. Clinically, BPH may be associated with severe obstructive uropathy and chronic renal insufficiency. 10
Materials and Methods
This prospective cohort study was conducted in selected Saudi Arabian clinics, from August 2024 to October 2024. As part of renal ultrasonographic examination, all participants underwent ultrasonographic PV measurements, based on images captured with a SonoScape S50 (Guangzhou, China) ultrasound equipment system and a 3.5-MHz convex transducer.
The inclusion criteria included participants with renal symptoms or lower urinary tract symptoms, and a random sample selection technique was used to recruit participants. The exclusion criteria were patients with known prostatic tumors or who were unwilling to participate in the study. All participants underwent renal ultrasonographic examination by an expert sonologist, with over 10 years of experience, in sonography. The ultrasonographic images were obtained with the participant lying supine on an examination table and utilizing a transabdominal ultrasonographic examination protocol.
The required participants’ preparation was to arrive after fasting and have a half-full urinary bladder (UB). The examination begins by applying the 3.5-MHz convex transducer sagittally and/or coronally to assess both kidneys for the presence of hydronephrosis or renal parenchymal changes. Additionally, scanning transversely, just above the pubic symphysis, was done to evaluate the UB and the prostate. The renal ultrasonographic findings were correlated with the PV measurements, to determine any statistical strength of association.
To obtain the PV, the transducer is angled approximately 30 degrees caudally, using the UB as an acoustic window. Slight compression was applied to ensure the inferior portion of the prostate was not obscured by a shadowing artifact, from the base of the UB. The required measurements were obtained from the largest section of the prostate gland. The prostatic height (H), width (W), and length (L) were obtained for each participant. Published literature 11 indicates that the PV is calculated using the ellipsoid formula, which involves measurements of H, W, and L. The formula is V (the volume of the prostate gland) = length (L) x width (W) x height (H) x 0.523. Figure 1 is an example of a set of prostatic sample images, demonstrating both the measurement of a normal and an enlarged prostate, using the transabdominal ultrasonographic technique.
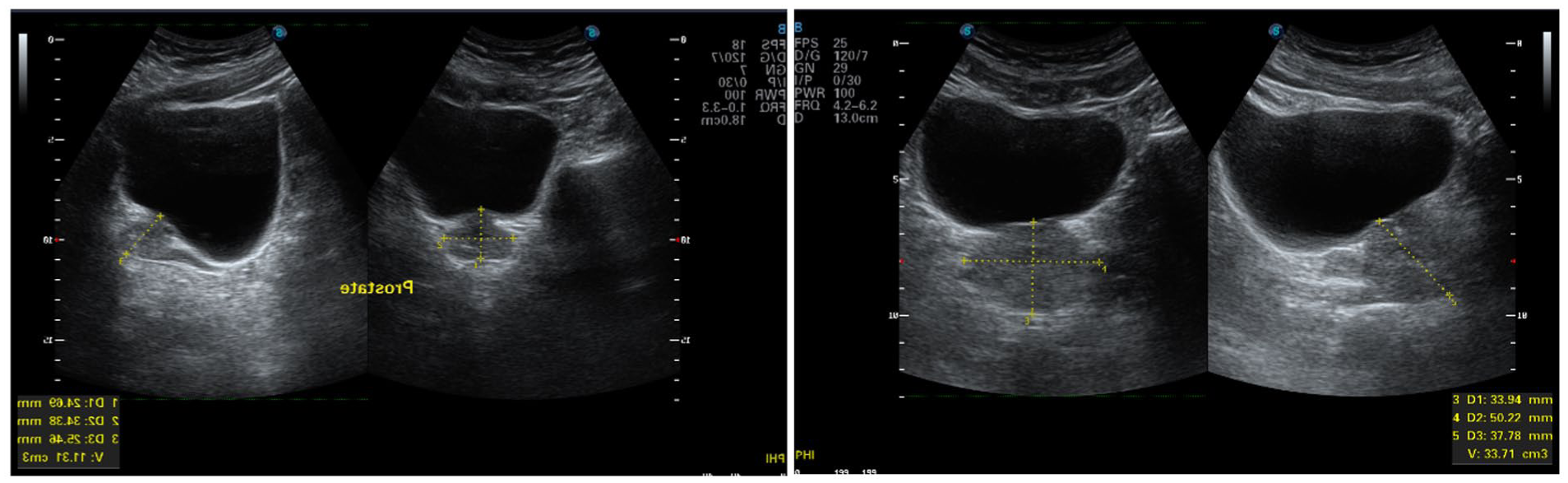
A set of sample sonograms that demonstrate the measurements of both a normal and enlarged prostate, based on the transabdominal sonographic technique.
A structured data sheet was used to record the study data and variables, including age, weight, height, prostatic echo texture, and H, W, and L. The BMI has been calculated using the formula: (BMI = weight (kg)/height (m2)). 12
Statistical Analysis
The data underwent rigorous analysis using industry-standard tools, including Microsoft Excel (2021) and the Statistical Package for the Social Sciences (SPSS) program, Version 26 (IBM, Armonk, New York, USA). Categorical and continuous variables were presented meticulously in percentages, frequencies, and descriptive statistics. The normality of the data distribution was tested by the histogram and the P-P Plot of the regression standardized residuals. The chi-square test, Pearson’s correlations, and univariate regression analysis were used to determine the relationship between the PV and the participants’ age, BMI, renal ultrasonographic results, and patients’ clinical findings. The statistical significance was set at
Results
The normality tests revealed a normal distribution of study data. The mean age of the participants was 41.8 ± SD 12.1 years (ranged between 22 and 80), the mean PV was 24.37 ± SD 18.1 cm3 (ranged between 9 and 118), and the mean BMI was 27.9 ± SD 4.6 kg/m2 (ranged between 17 and 43.8; See Table 1).
The Cohort’s Descriptive Statistics, Based on the Study Variables.
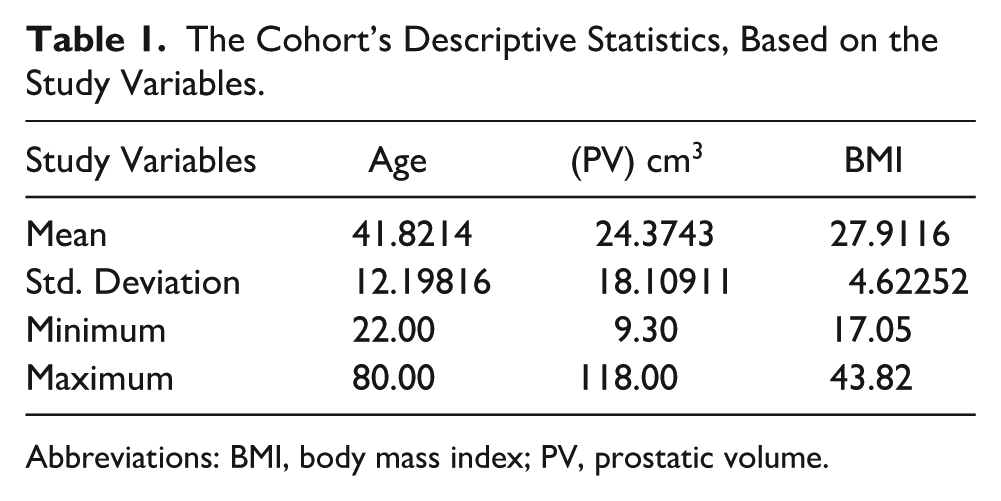
Abbreviations: BMI, body mass index; PV, prostatic volume.
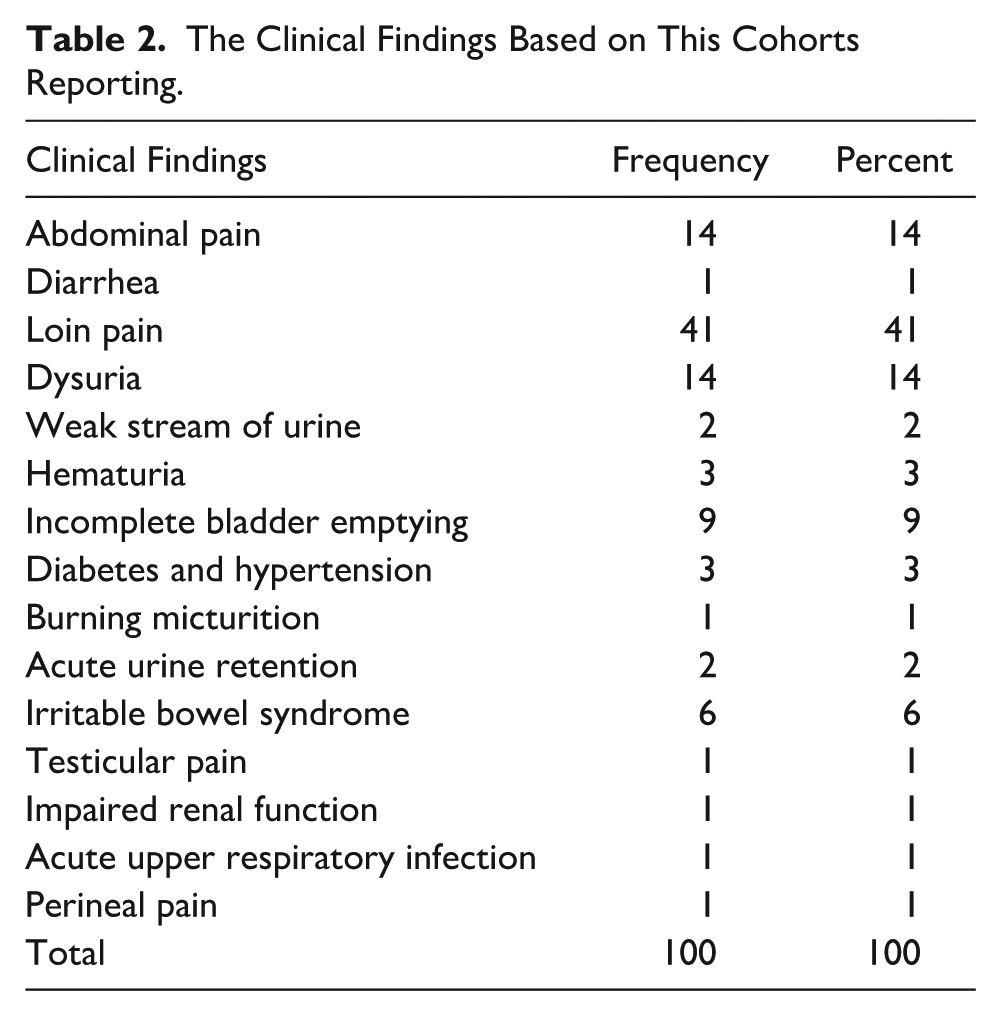
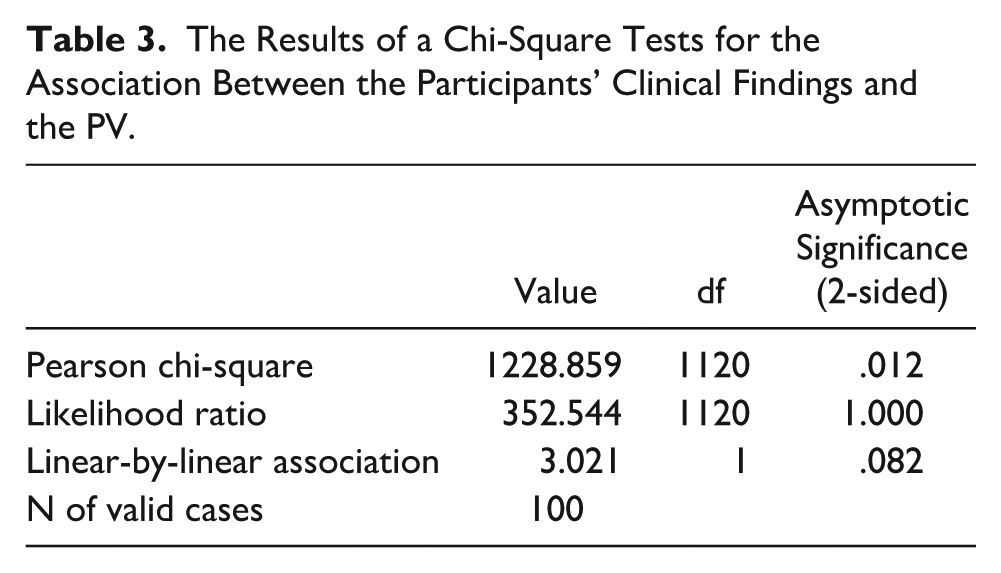
Table 2 provides the participants’ clinical findings, as well as those participants who had more than one finding or symptom. The typical symptoms included lower back pain (41%), dysuria (14%), and incomplete bladder emptying. The results of the chi-square statistical analysis test indicated a significant statistical association between the clinical symptoms of the participants and their PV,
The Clinical Findings Based on This Cohorts Reporting.
The Results of a Chi-Square Tests for the Association Between the Participants’ Clinical Findings and the PV.
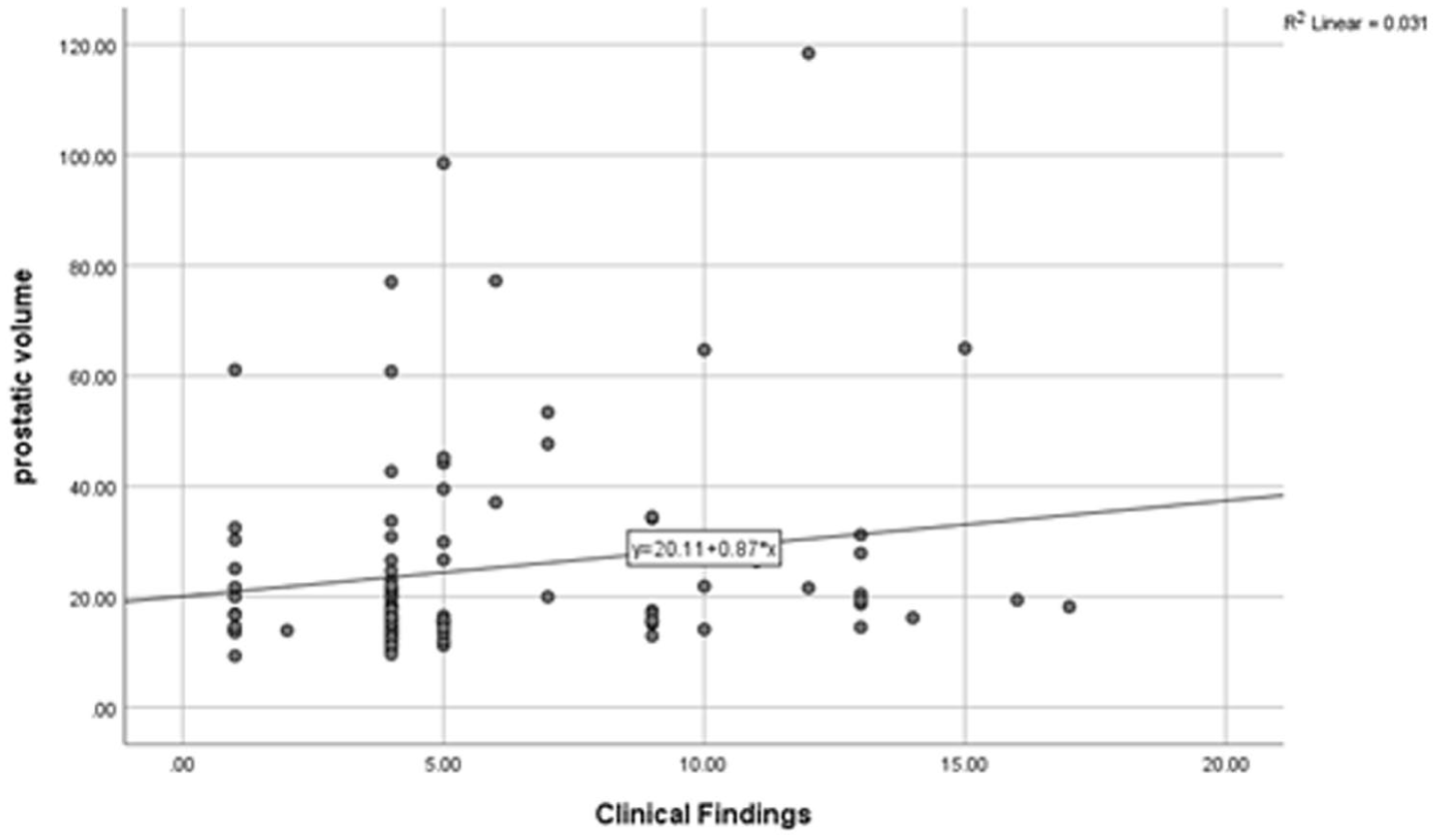
A scatter plot that indicated the association between the study cohorts’ prostatic volume (PV) and their clinical findings.
The Results of an Univariate Regression’s Correlations Between the Prostatic Volume (PV) and the Clinical Findings of the Participants.
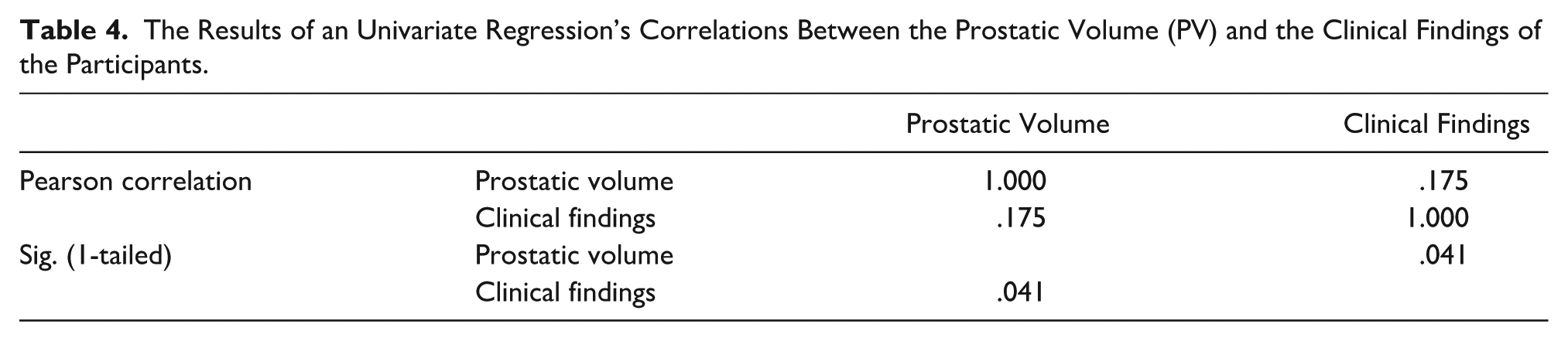

Table 5 presents the associated renal ultrasonographic findings for this cohort of participants. The results showed that 58% had unremarkable renal ultrasonographic findings, with the most common diagnostic finding being renal calculus with hydronephrosis (18%), significant residual urine volume (9%), and renal calculus without hydronephrosis (6%). A significant statistical association was found between the renal ultrasonographic findings and the participants’ PV,
The Reported Renal Sonographic Findings Based on This Study Cohort.
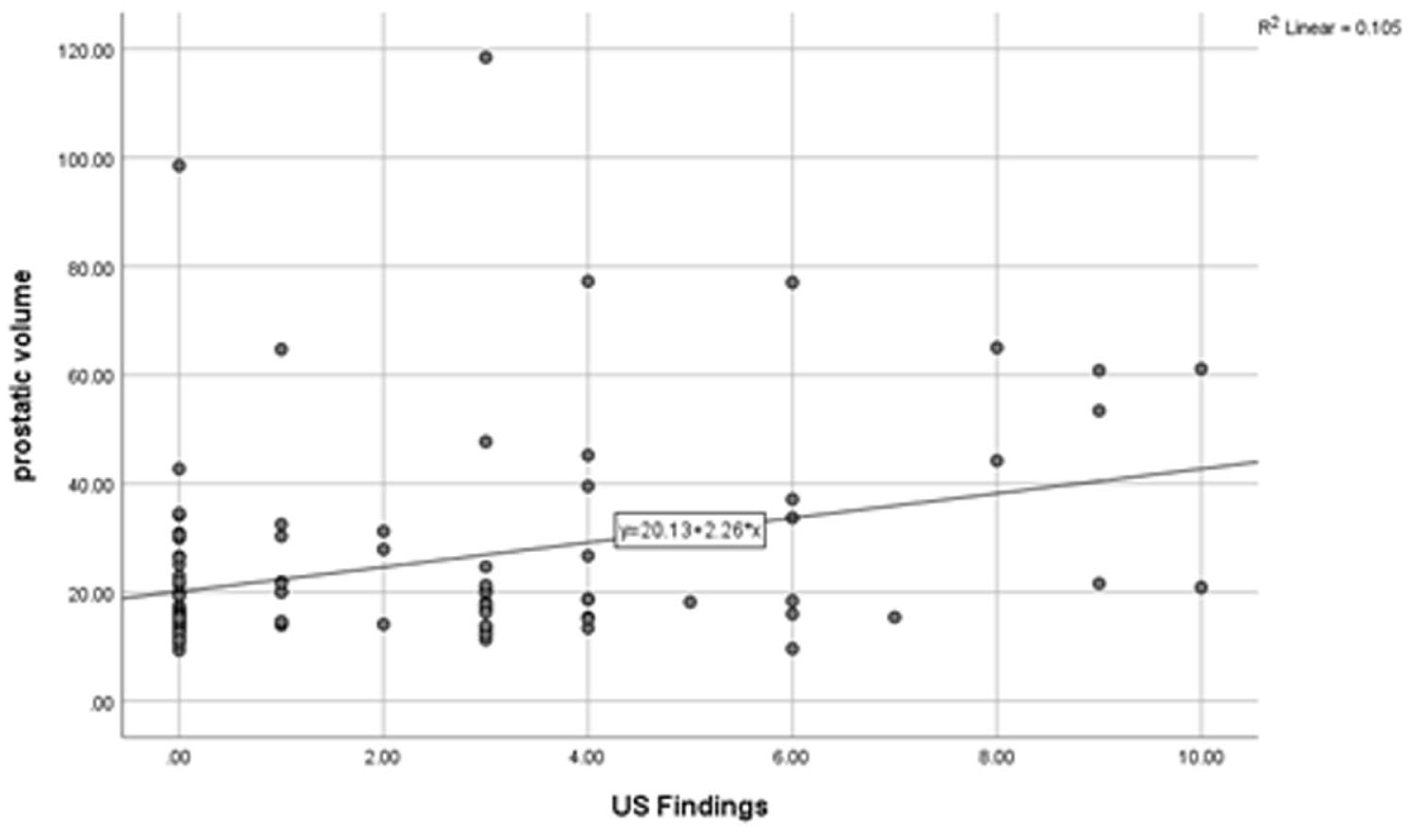
A scatter plot that indicates the association between the study cohorts’ prostatic volume (PV) and renal ultrasonographic findings.
Figure 4 illustrates the distribution of PV greater than 30 mL per age group. PV > 30 was noted in 24% of these participants, and this was more frequent in the age group above 40, with the 60 to 69 age group having the highest frequency. Table 6 summarizes the results of chi-square tests for participants’ age and their PV. It revealed a significant statistical association (
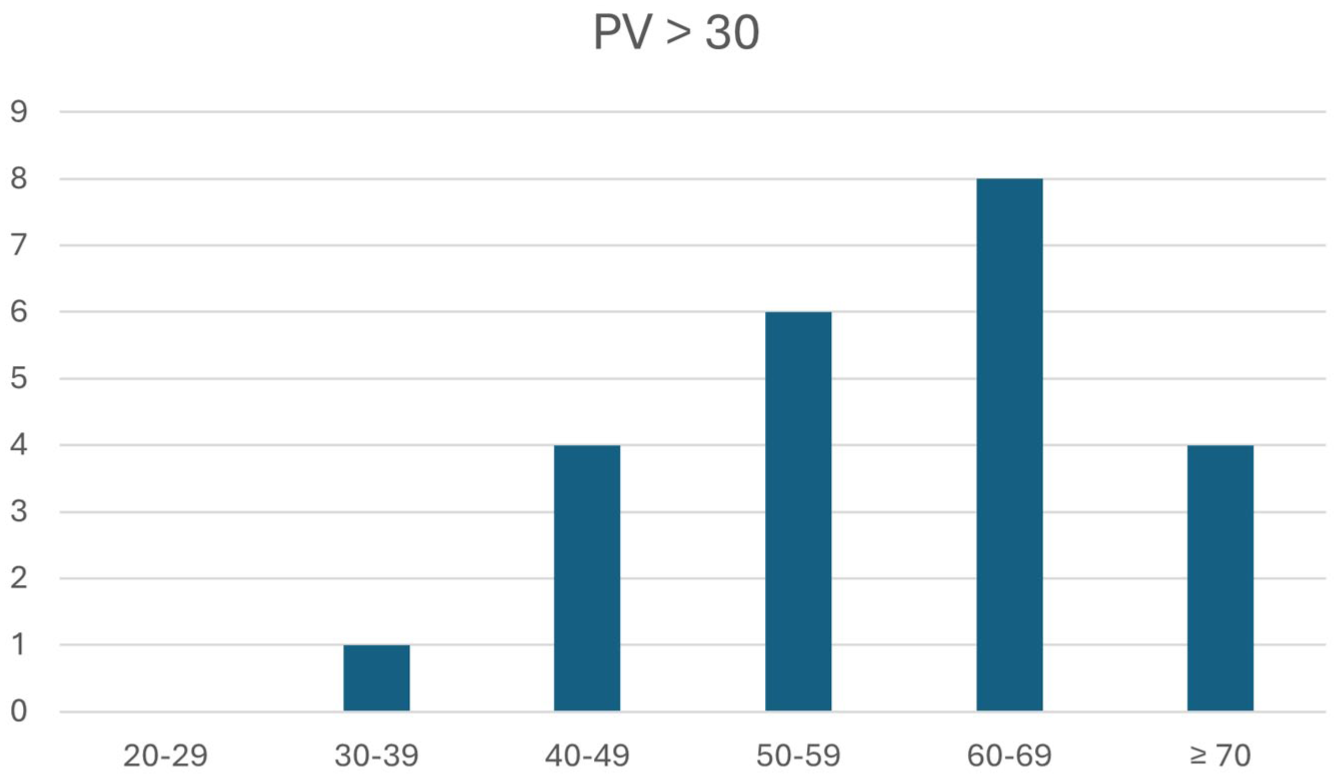
A bar chart shows a distribution of the prostate volume >30 mL, based on the study cohorts’ age distribution.
The Results of the Chi-Square Test for the Association Between the Participants’ Age and Prostatic Volume (PV).
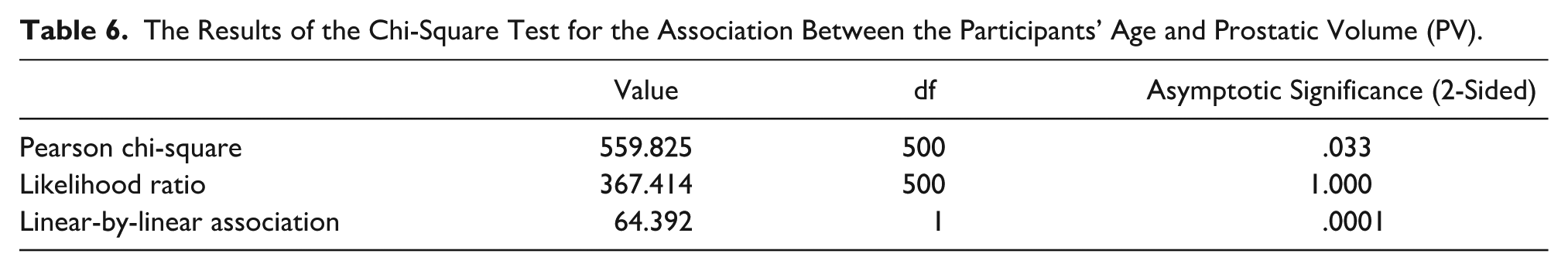
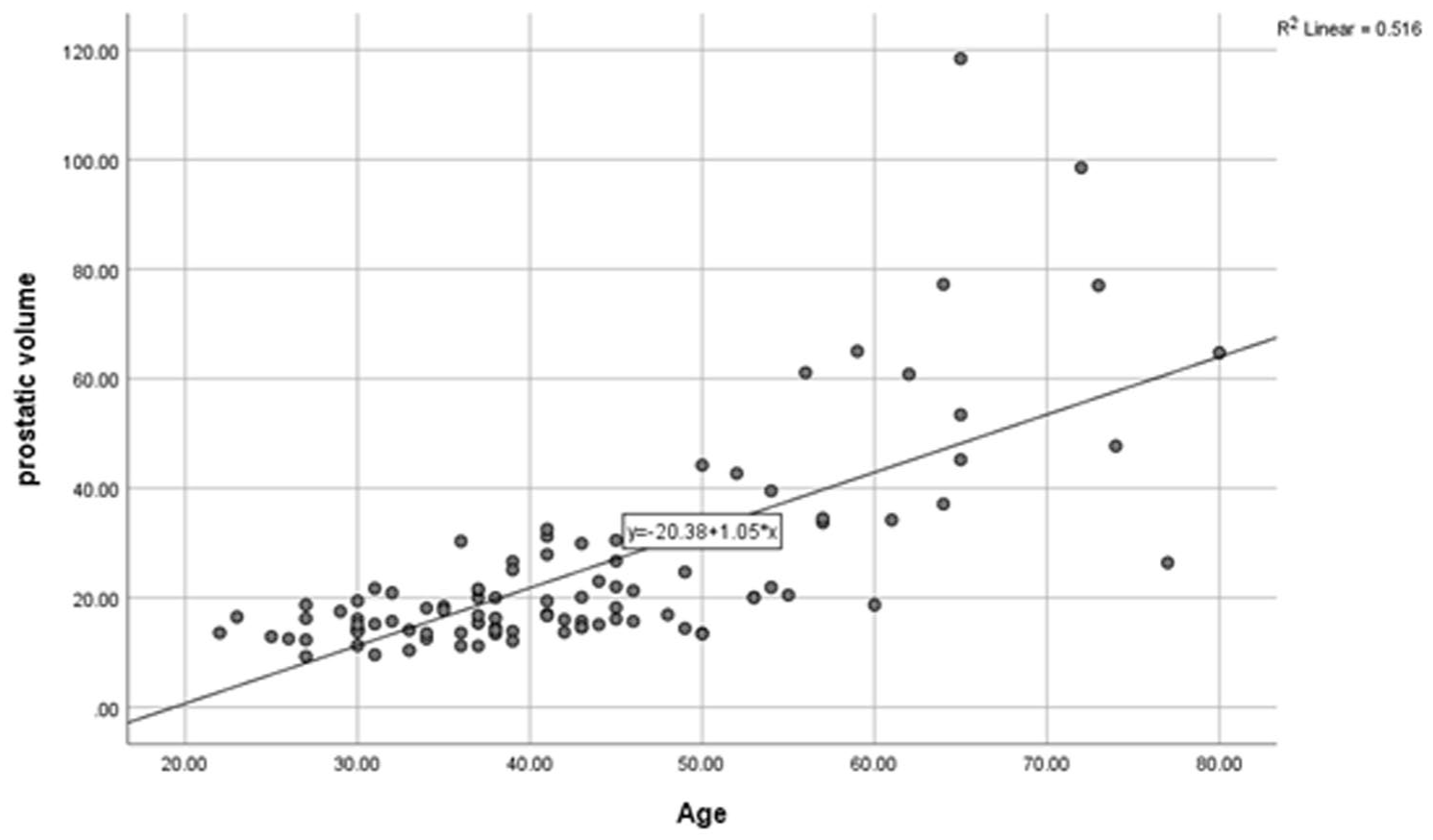
A scatter plot shows the association between the study cohorts’ prostatic volume (PV) and their age.
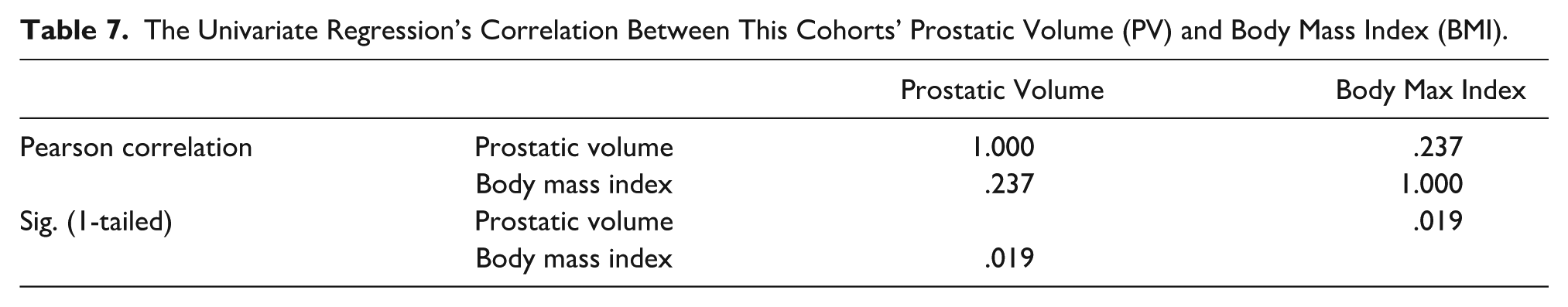
Table 7 shows the univariate regression analysis between the participants’ BMI and their PV. The analysis of variance (ANOVA) revealed a significant statistical association between PV and BMI (
The Univariate Regression’s Correlation Between This Cohorts’ Prostatic Volume (PV) and Body Mass Index (BMI).

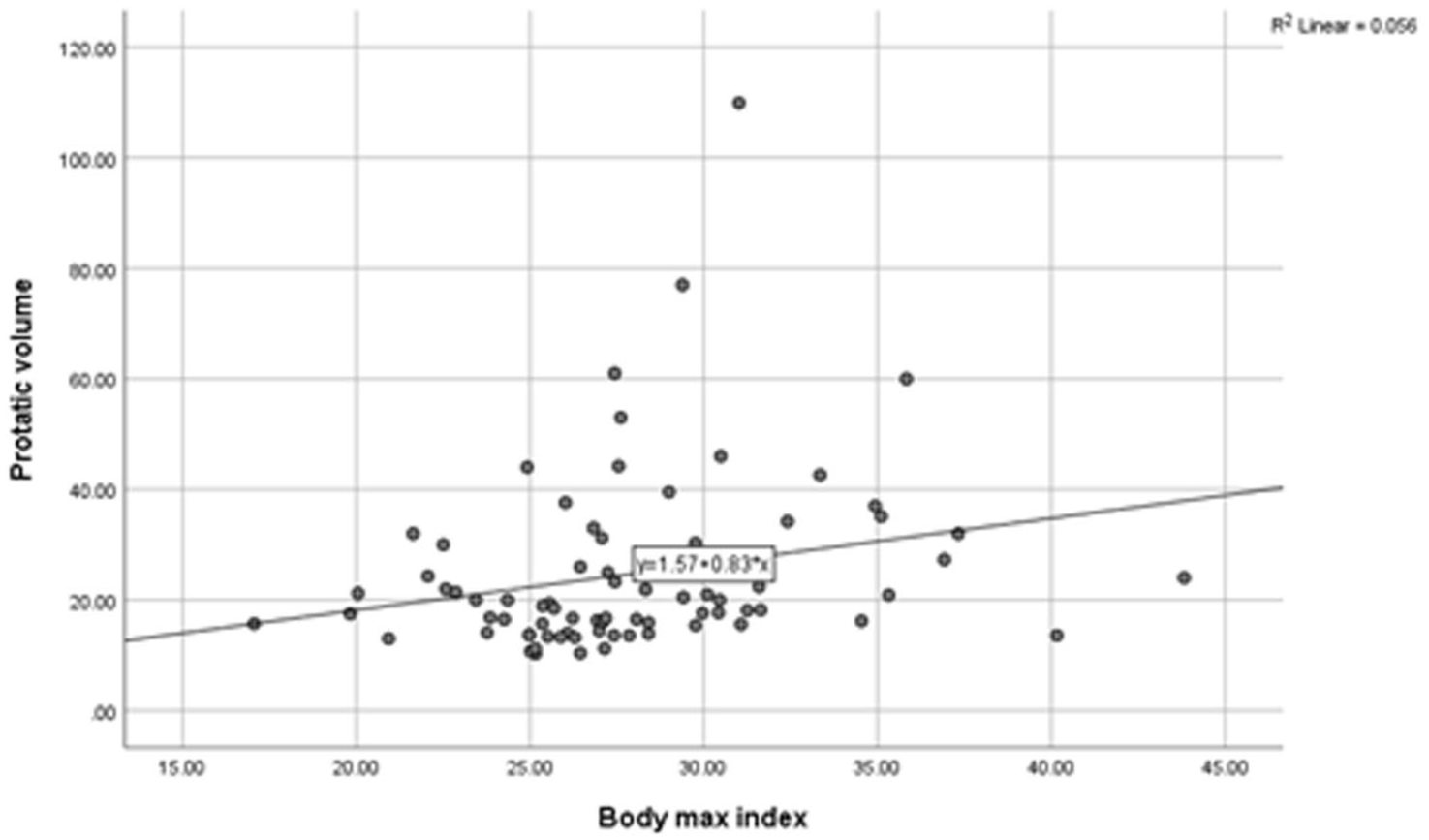
A scatter plot shows the significant association between the study cohorts’ body mass index (BMI) and their prostatic volume (PV).
Discussion
The current study involved estimating PV and correlating this volume with the participants’ clinical symptoms, renal ultrasonographic findings, age, and BMI. As a review, the participants’ mean age was 41.8 ± SD 12.1 years, the mean PV was 24.37 ± SD 18.1 cm3, and the mean BMI was 27.9 ± SD 4.6.
The current study revealed a statistically significant positive association between the participants’ clinical findings, such as hydronephrosis, dysuria, and incomplete bladder emptying, and their PV. Moreover, it indicated a significant positive statistical association between the participants’ renal ultrasonographic findings and their PV. These conclusions align with the published findings provided by Udo et al. 13 Their work suggested a positive and significant correlation between PV and the International Prostate Symptom Score (IPSS). Similarly, Iqbal et al 14 concluded that different urinary tract abnormalities, detected with ultrasonography, may be presented in patients with BPH. Awaisu et al 15 reported a significant correlation between the PV and the maximum flow rate, as well as between the PV and the IPSS. Likewise, Besut et al 16 concluded that a PV greater than 30 mL is one of the most influential factors in the occurrence of chronic kidney disease.
A search of the literature yielded a diverse range of conclusions regarding the correlations between participants’ PV and age. The current study’s findings indicated a significant association between the participants’ age and their PV. This conclusion is strongly supported by Meng et al, 17 who proposed that age, height, and BMI were positive independent risk factors of enlarged PV. Enjela Maysah Situmorang et al 18 concluded that there is a significant association between age and benign prostatic hyperplasia. While E Aigbe et al 19 have suggested a contrasting opinion, they indicated that there is no significant association between the participants’ PV and their age.
Regarding the association between the participants’ PV and their BMI, the current study results revealed a statistically significant association. These findings are in total agreement with those of Kowalczyk et al, 20 whose results indicated a significant statistical association between prostate size and patients’ weight and height. Li et al 21 suggested a significant linear association between BMI and the risk of larger PV, and Negi et al 22 reported a strong statistical correlation between PV and BMI. Clinically, Omran et al 23 indicated that metabolic syndrome usually coexists with obesity and BPH. Although some authors24,25 hold the opposite opinion, concluding that there is no significant association between the participants’ PV and their BMI.
Limitations
The major limitation to this study is research design that has inherent threats to both internal and external validity. In addition, the relatively small sample size, which was selected by convenience affects the generalizability of the findings. In addition, the absence of laboratory investigations, such as urinalysis, creatinine levels, prostate-specific antigen (PSA) levels, and renal function tests, limits the ability to fully characterize participants’ clinical status. Furthermore, the potential influence of undocumented treatments or undetected comorbidities on PV cannot be dismissed and should be acknowledged as a confounding factor.
Conclusion
These study findings may suggest that the mean PV has a significant correlation with patients’ clinical symptoms, renal ultrasonographic findings, age, and BMI. The statistical results from this cohort study indicated that age was the strongest association with the PV. In clinical practice, when assessing BPH patients, the sonographer should evaluate the entire urinary system to record any associated renal findings. Also, managing modifiable factors such as clinical symptoms, renal disorders, and BMI through physician intervention, for example, lifestyle changes, may provide a good opportunity for effective treatment and prevention of BPH. Further studies on the correlation between PV and patients’ clinical symptoms, renal ultrasonographic findings, age, and BMI are suggested, particularly among individuals over 50 years of age. To apply these kinds of results, a large sample size would be required, along with correlations of suitable laboratory tests, such as creatinine, PSA, and fasting blood glucose, due to their clinical association with BPH. Addressing certain current medications and comorbidities is necessary in the data collection step to control for confounding factors. The PV assessment is critical in determining the degree of prostatic hyperplastic enlargement, the resultant tendency toward urinary tract outflow obstruction, and the selection of suitable surgical treatment or brachytherapy options.
Supplemental Material
sj-docx-1-jdm-10.1177_87564793251391196 – Supplemental material for The Correlation of Prostatic Volume With Participants’ Age, Body Mass Index, Renal Ultrasonographic Findings, and Clinical Symptoms
Supplemental material, sj-docx-1-jdm-10.1177_87564793251391196 for The Correlation of Prostatic Volume With Participants’ Age, Body Mass Index, Renal Ultrasonographic Findings, and Clinical Symptoms by Mahmoud S. Babiker and Adil Mohammed in Journal of Diagnostic Medical Sonography
Supplemental Material
sj-docx-2-jdm-10.1177_87564793251391196 – Supplemental material for The Correlation of Prostatic Volume With Participants’ Age, Body Mass Index, Renal Ultrasonographic Findings, and Clinical Symptoms
Supplemental material, sj-docx-2-jdm-10.1177_87564793251391196 for The Correlation of Prostatic Volume With Participants’ Age, Body Mass Index, Renal Ultrasonographic Findings, and Clinical Symptoms by Mahmoud S. Babiker and Adil Mohammed in Journal of Diagnostic Medical Sonography
Supplemental Material
sj-png-3-jdm-10.1177_87564793251391196 – Supplemental material for The Correlation of Prostatic Volume With Participants’ Age, Body Mass Index, Renal Ultrasonographic Findings, and Clinical Symptoms
Supplemental material, sj-png-3-jdm-10.1177_87564793251391196 for The Correlation of Prostatic Volume With Participants’ Age, Body Mass Index, Renal Ultrasonographic Findings, and Clinical Symptoms by Mahmoud S. Babiker and Adil Mohammed in Journal of Diagnostic Medical Sonography
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of the article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethics Approval
Ethical approval was not sought for the present study because the clinical center where the study was conducted did not have an ethics committee for obtaining ethical approval; instead, approval was granted by the center director.
Informed Consent
Written informed consent (verbal assent) was obtained from all subjects before the study.
Animal Welfare
Guidelines for humane animal treatment did not apply to the present study because no animals were used during the study.
Trial Registration
Not applicable.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
