Abstract
Objective:
Fatty liver disease (FLD) affects hepatic hemodynamics, which can be assessed using Doppler indices. Understanding variations in these indices can enhance noninvasive diagnostic and monitoring tools for FLD. The aim of this review was to assess and analyze variations in hepatic artery resistive index (HARI), portal vein pulsatility index (PVPI), and portal vein velocity (PVV) in patients with FLD.
Materials and Methods:
This study reviewed variations in hepatic Doppler indices in patients with fatty liver disease (FLD) by analyzing peer-reviewed studies published between 2000 and 2024. A total of 52 articles were identified across several scientific databases, using Boolean operators and relevant search phrases. The meta-analysis utilized a random-effects model to account for heterogeneity, which was further assessed using chi-square tests (
Results:
The procured data revealed that FLD patients exhibited significantly lower HARI (15% reduction), VPI (10% reduction), and PVV (25% reduction) than healthy controls (
Conclusion:
This literature review was focused on FLD, which has been consistently associated with reduced portal vein indices and compensatory increases in hepatic artery flow. Variations in HARI, PVPI, and PVV reflected both the hemodynamic consequences of fatty infiltration and the liver’s compensatory adaptations. It may be clinically valuable to further explore these parameters, as noninvasive biomarkers for the diagnosis, staging, and monitoring of FLD.
The liver plays a critical role in overall health, performing essential functions such as detoxification, metabolism, and protein synthesis.1,2 However, abnormalities in liver function can lead to serious conditions, including fatty liver disease (FLD) or steatotic liver disease, which has emerged as a global health concern. 3 FLD is characterized by excess fat accumulation in liver cells and is broadly categorized into metabolic dysfunction-associated steatotic liver disease (MASLD), also known as nonalcoholic fatty liver disease (NAFLD), and alcoholic fatty liver disease (AFLD). NAFLD, the more prevalent form, ranges from simple steatosis to metabolic dysfunction-associated steatohepatitis (MASH), also called nonalcoholic steatohepatitis (NASH), which can progress to cirrhosis and liver cancer. 4 AFLD, caused by chronic alcohol consumption, shares similar pathophysiological changes with NAFLD, including inflammation, oxidative stress, and vascular changes.5,6
Doppler has become an invaluable noninvasive tool for evaluating blood flow dynamics.7,8 Hepatic Doppler indices (hepatic artery resistive index [HARI], portal vein pulsatility index [PVPI], and portal vein velocity [PVV]) can be assessed quantitatively to determine intrahepatic vascular flow and integrity. These indices are essential for diagnosing and monitoring liver diseases, including FLD, portal hypertension, and cirrhosis, 9 as elevated values of HARI suggest cirrhosis or fibrosis, 9 the PVPI assists with identifying vascular abnormalities, 9 and abnormal PVV values raise suspicion of portal hypertension and/or advanced liver disease.7,10
Recent evidence indicates that changes in Doppler indices may occur in patients with fatty liver disease due to structural, physiologic and hemodynamic changes in the liver, as the disease progresses.11,12 In FLD, HARI may decrease due to compensatory vasodilation from fat-induced inflammation (i.e., if FLD progresses to fibrosis or cirrhosis, the HARI will increase), PVPI reduces because of increased portal venous pressure, reduced vascular compliance within the liver, due to parenchymal stiffening, and diminished right atrial compliance, and PVV reduces, due to progressive increased intrahepatic resistance. However, findings are heterogeneous across published studies, and there appears to be no standardized reference for interpreting these variations observed during different stages of FLD. In addition, a variety of conflicting outcomes are due to differences in Doppler protocols, disease classification, and patient demographics.
The purpose of this systematic review was to synthesize current evidence concerning variations in hepatic Doppler indices in patients with FLD, compare findings between disease severity and healthy controls, and to review whether Doppler can serve as a diagnostic staging tool for MASLD/MASH.
Materials and Methods
Research Design
This study used a systematic review, and a meta-analysis based on the PRISMA 2020 guidelines, to synthesize evidence regarding the diagnostic utility of hepatic Doppler indices for FLD patients. The goal of this review was to quantify differences in Doppler parameters between individuals with FLD and a healthy control group, using HARI, PVV, and PVPI, as examples of such parameters.
To provide context to the Doppler findings, normative standards of the studies that were included were analyzed. The values of PVV and PVPI are substantially decreased in NAFLD patients when compared with healthy individuals.12–15 It is also reported that NAFLD patients have HARI that is reduced,13,14 and the reduction of PVV, PVPI, and HARI tends to confirm the diagnosis of FLD.4,16 Other reports indicate specific cutoff values in the identification of advanced liver disease: PVV < 13 cm/s and HARI > 1.1. 15 Also, it has been proposed that a PVPI < 0.26 will indicate the presence of steatosis. 17 These values form a noninvasive way to grade the NAFLD severity and confirm the diagnosis. 18
Eligibility Criteria
Studies were included if they met the following criteria:
Published in English between January 2000 and January 2024.
Peer-reviewed, human clinical studies (observational or experimental).
Involved patients diagnosed with NAFLD/NASH or FLD, confirmed via clinical or imaging criteria.
Reported quantitative values for at least one of the following Doppler indices: HARI, PVV, or VPI.
Included a comparative group of healthy individuals.
Exclusion Criteria
Studies involving other chronic liver diseases (e.g., hepatitis B/C and autoimmune liver disease).
Case reports, reviews, editorials, or studies without original data.
Studies that did not use Doppler as the primary diagnostic tool.
Search Strategy
A comprehensive literature search was conducted across PubMed, Google Scholar, ResearchGate, and Semantic Scholar. The search was carried out between November 2024 and January 2025. A representative search string used in PubMed was (“fatty liver disease” OR “FLD” OR “NAFLD” OR “non-alcoholic steatohepatitis”) AND (“hepatic Doppler indices” OR “resistive index” OR “pulsatility index” OR “portal vein velocity” OR “Doppler ultrasound”)
Search terms were combined using Boolean operators (AND, OR). Searches were restricted to titles and abstracts for PubMed, while Google Scholar, ResearchGate, and Semantic Scholar retrieved content using full-text matching, as per their platform default behaviors. The bibliographies of the included studies were also screened manually for additional eligible records. In addition, the bibliographies of included articles were searched manually to identify any other relevant studies.
Study Selection
A total of 52 articles were initially identified for review. Of these, 24 were screened based on title relevance, resulting in the exclusion of 12 articles due to irrelevance. An additional four articles were excluded after abstract and content review for not aligning with the study’s aims. Furthermore, two articles were removed for failing to meet eligibility criteria, such as the absence of quantifiable Doppler parameters or methodological limitations. One additional article was retrieved through manual reference searching. Following this rigorous screening process, seven full-text articles were deemed suitable and included in the final meta-analysis. The screening was conducted in an independent manner by several reviewers, and disagreements were resolved by group consensus. A PRISMA flow diagram illustrating the selection process of the study (See Figure 1).
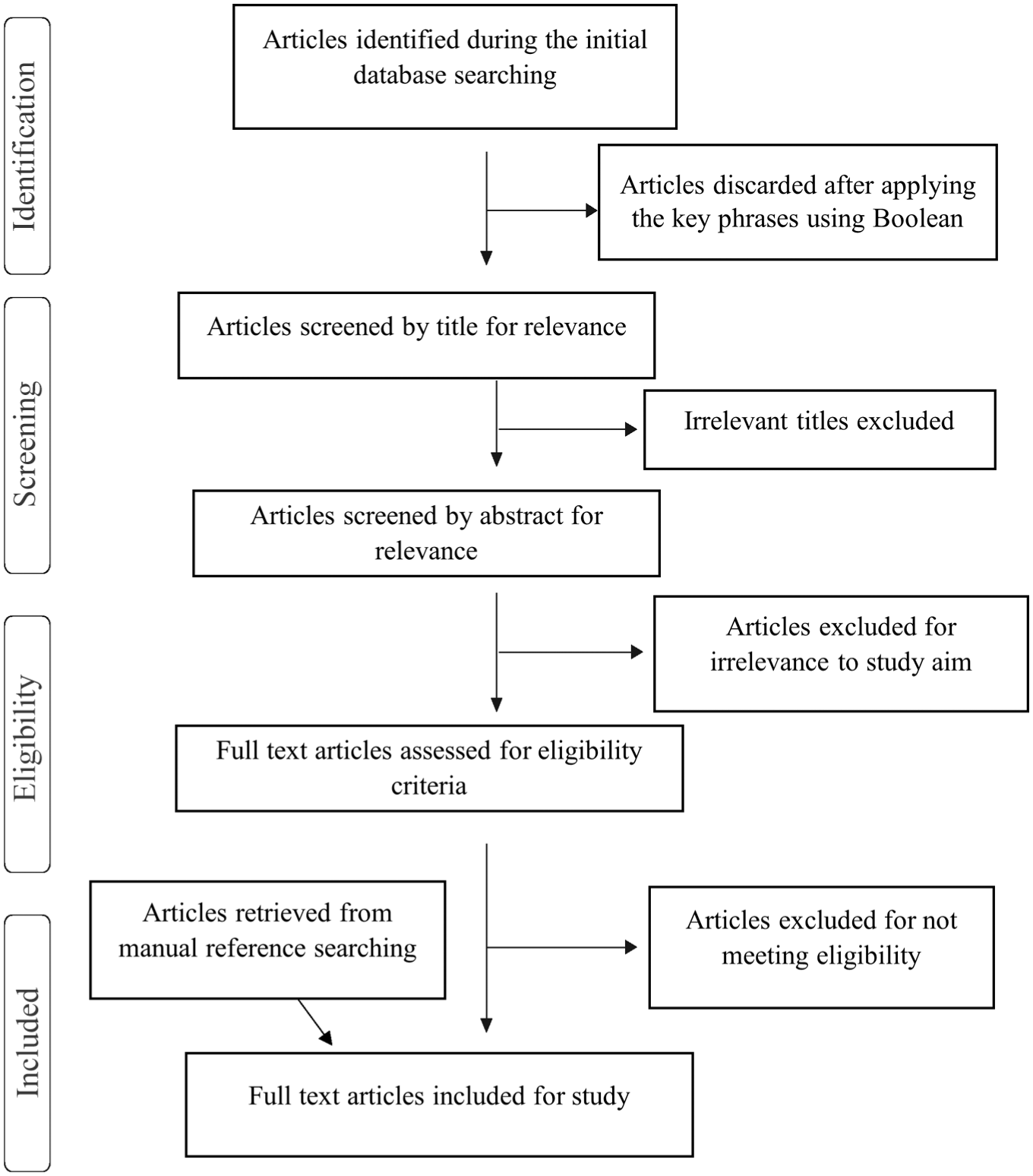
A flowchart that outlines the process of the database search and studies procured.
Data Extraction
A standardized data extraction form was used to retrieve the following information from each included article: Author(s), year of publication, country, study design and sample size, diagnostic criteria for FLD, Doppler indices evaluated: HARI, PVV, and PVPI, mean and standard deviation of indices in FLD patients and the healthy controls groups. Data were extracted independently by two independent review groups and cross-checked for consistency.
Data Synthesis and Statistical Analysis
A random-effects meta-analysis was done to consider expected heterogeneity between studies. For each Doppler index (HARI, PVV, PVPI), the pooled mean difference between FLD patients and healthy controls, and their corresponding 95% confidence intervals (CIs) were calculated for each. The I² statistics was used to assess heterogeneity, and was considered low: ≤ 25%, moderate: 50%, high: ≥75%
19
and by the chi-square test (significance at
Results
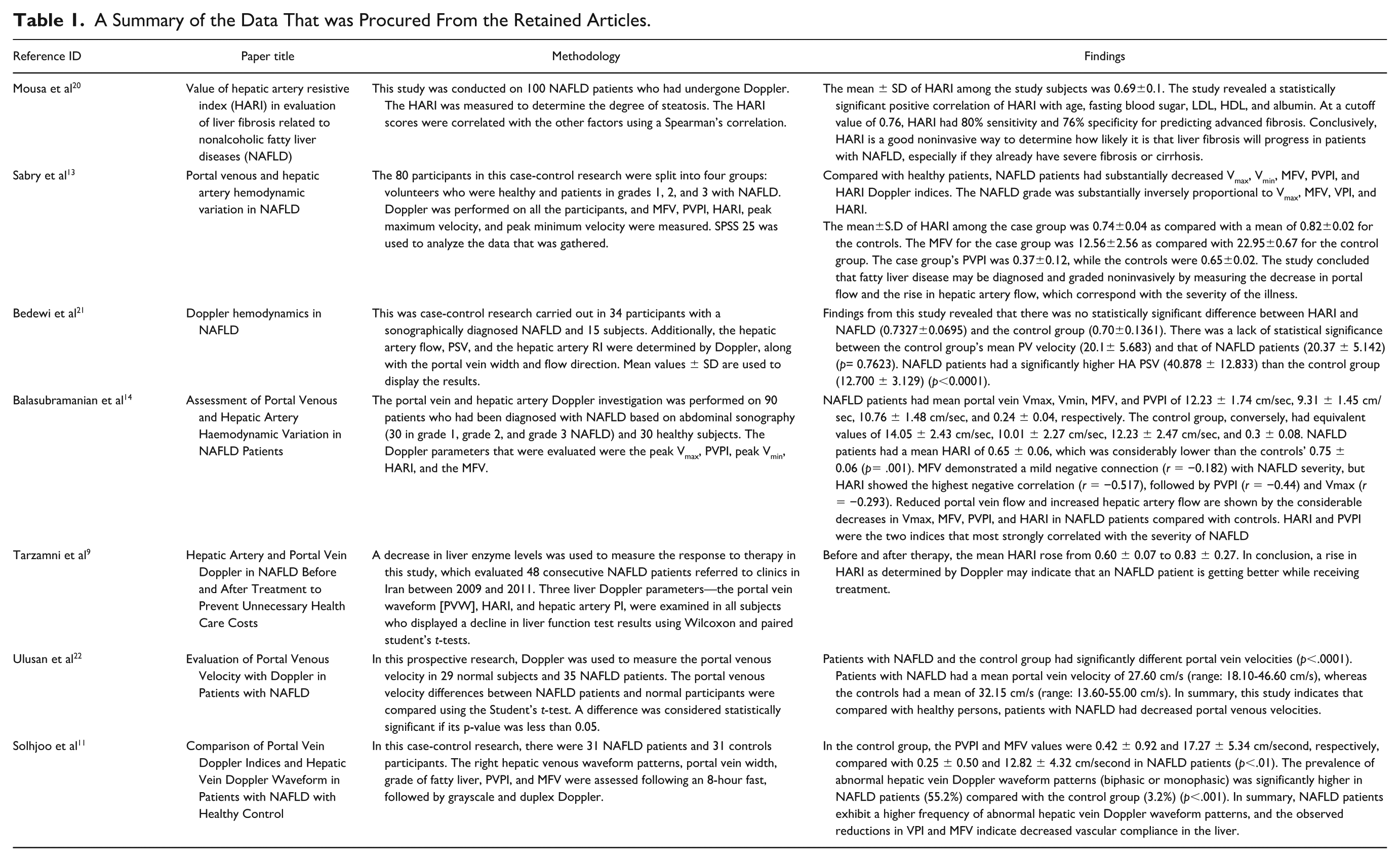
A total of 52 studies were retrieved from PubMed, Google Scholar, Semantic Scholar and ResearchGate. There were 44 studies excluded because they did not meet the inclusion criteria after screening titles and abstracts. Eight full-text articles were reviewed, of which two were excluded due to lack of Doppler index data or irrelevant diagnostic focus. By the manual search of the references of included articles, an extra article was retrieved. Therefore, seven articles were included in both the qualitative synthesis and in the meta-analysis because they met the eligibility criteria. These seven articles included studies that were conducted in Egypt, Saudi Arabia, India, Iran, and Turkey, and all used Doppler for the assessment of hepatic vascular parameters in patients with FLD. HARI, PVV, and PVPI were typically compared between FLD patients and healthy controls in most studies. The summary of the included studies is presented in Table 1.
A Summary of the Data That was Procured From the Retained Articles.
Meta-analysis of Doppler Indices
The mean HARI, PVV, and PVPI are shown in Table 2, indicating significant alterations in hepatic hemodynamics among FLD patients.
Reported Hepatic Doppler Indices in FLD Patients.
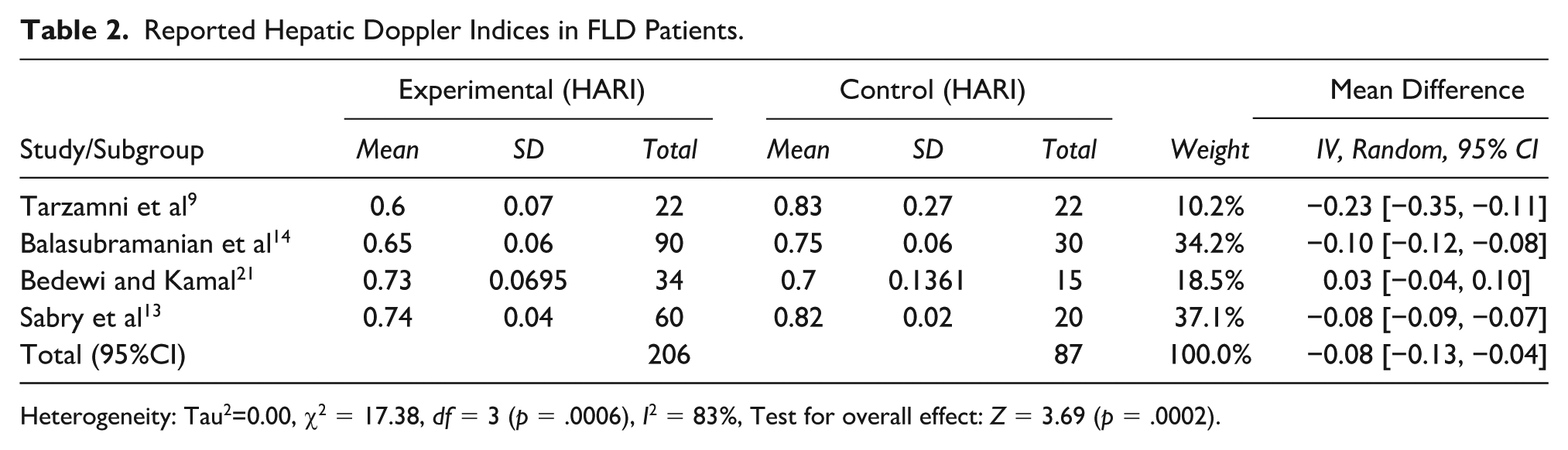
Heterogeneity: Tau2=0.00, χ2 = 17.38,
Four out of the seven studies compared the mean HARI between FLD patients and healthy adults (see Table 3), which was significantly higher in healthy adults (range: 0.75–0.83) than in the FLD patients (range: 0.6–0.74). In the pooled analysis, the HARI was significantly lower in FLD patients than in the control groups, with a mean difference of −0.08 (95% CI: −0.13 to −0.04,
Hepatic Artery Resistive Index (HARI) Between Patients With FLD and Healthy Individuals.
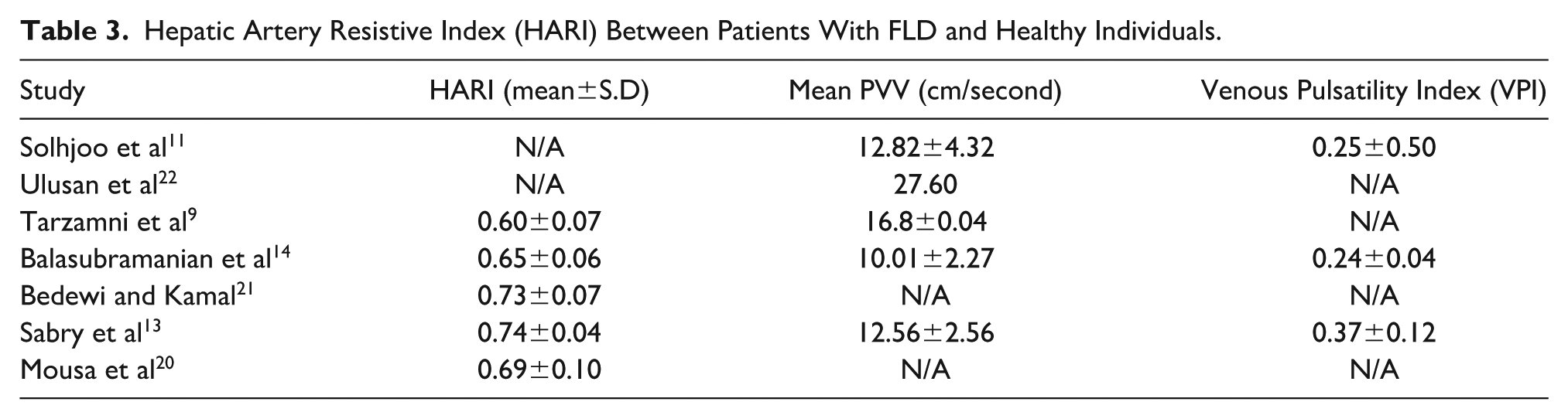
Five studies reported that the mean PVV was significantly higher in healthy participants (12.23–32.15 cm/sec) than in FLD patients (10.01–27.60 cm/sec) (See Table 4). The pooled analysis demonstrated that PVV was significantly lower in FLD patients, with a mean difference of −2.92 cm/s (95% CI: −4.61 to −1.23,
Portal Vein Velocity (PVV) Between Patients With FLD and Healthy Individuals.
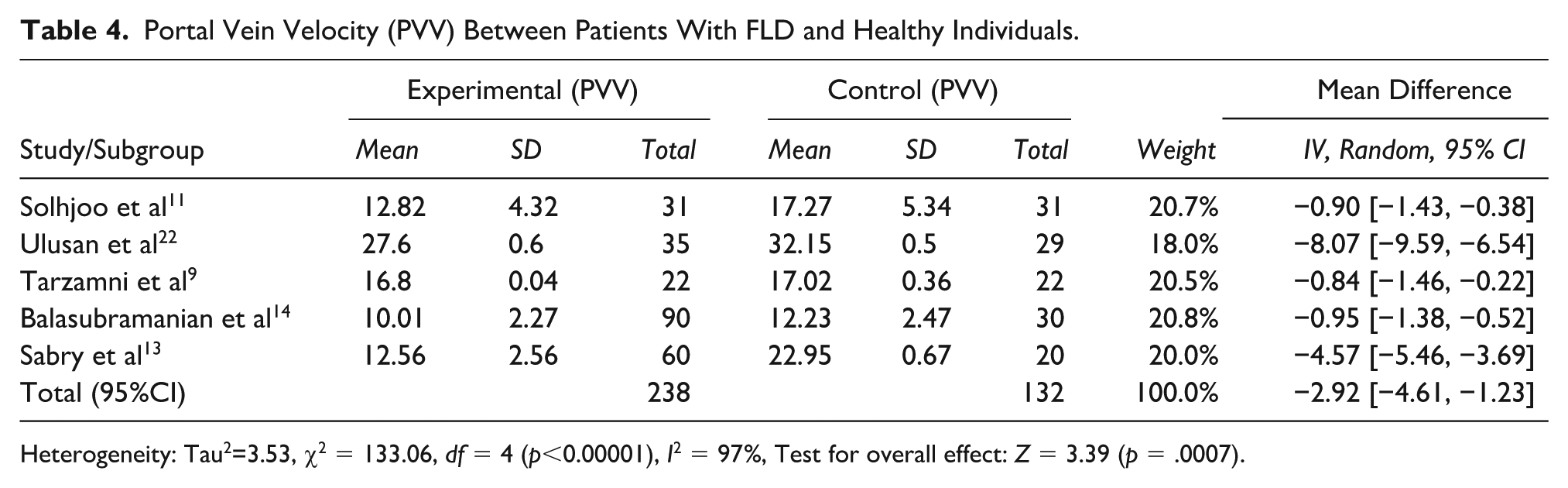
Heterogeneity: Tau2=3.53, χ2 = 133.06,
The three studies assessing VPI found significantly lower values in the FLD patients (See Table 5). The pooled mean difference was −1.32 (95% CI: −2.54 to −0.09,
Portal Vein Pulsatility Index (PVPI) Between Patients With FLD and Healthy Individuals.
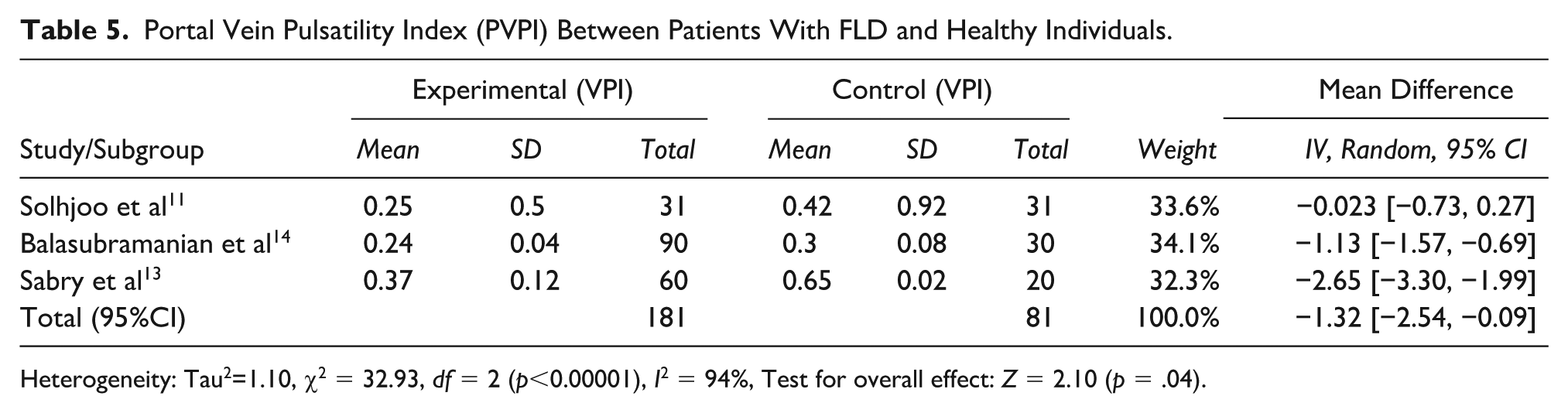
Heterogeneity: Tau2=1.10, χ2 = 32.93,
Heterogeneity and Outlier Analysis
High heterogeneity was observed across all indices (see Tables 3–5). While the direction of effect remained largely consistent (i.e., Doppler indices lower in FLD), variation in sample size, operator technique, disease severity, and Doppler angle likely contributed to the heterogeneity. Bedewi and Kamal 21 was the most prominent outlier, with findings inconsistent with the rest of the dataset.
Discussion
This systematic review and meta-analysis examined variations in hepatic Doppler indices, HARI, PVV, and PVPI in patients with FLD and compared them to healthy individuals. The findings revealed significant alterations in hepatic hemodynamics among FLD patients, with potential implications for diagnosis and monitoring. The reviewed studies reported a wide range of HARI values (0.60–0.74), which may be influenced by geographical and climatic conditions. For example, studies conducted in arid regions (e.g., Egypt, Saudi Arabia) reported higher HARI values,13,21 while other studies conducted in more stable and humid regions reported lower HARI values.9,14,20 Further research is needed to explore the relationship between environmental factors and hepatic Doppler indices. PVV and PVPI also varied significantly across studies, with PVV ranging from 10.01 to 27.60 cm/sec and PVPI ranging from 0.24 to 0.37. These variations were often correlated with FLD severity, consistent with previous findings that fatty infiltrations reduce portal vein flow.
23
However, some studies found no significant correlation, highlighting the need for standardized measurement techniques. The studies by Tarzamni et al,
9
Sabry et al
13
and Balasubramanian et al
14
showed a consistently lower HARI in FLD patients than in healthy controls, with a confidence interval (CI) that does not overlap the line of no effect (i.e., zero) in the forest plot, indicating a statistically significant difference in the compared groups. None of the included studies that compared PVV overlapped the line of no effect (i.e., zero, indicating a significant difference in all the measured PVV across the studies. Three out of the seven included literature compared the PVPI of the two groups but only two studies (e.g., Sabry et al
13
and Balasubramanian et al
14
) had a significant reduction in the PVPI of FLD patients when compared with the healthy control (did not cross the line of no effects on the forest plot). Although Solhjoo et al
11
showed a slight decrease in the PVPI of the two groups, it was statistically significant. The pooled mean difference for HARI was −0.08 (95% CI: −0.13 to −0.04;
The significant differences in HARI, PVV, and PVPI between FLD patients and healthy individuals highlight the potential of Doppler indices as noninvasive biomarkers for FLD diagnosis and monitoring. Two studies (e.g., Sabry et al 13 and Balasubramanian et al 14 ) further demonstrated that these indices correlate with FLD severity, supporting their use in tracking disease progression and treatment response. Doppler, being affordable, readily available, and radiation-free, is a valuable first-line tool for FLD management, particularly in resource-limited settings.
Limitations
This review has several limitations that may hamper generalization. Many of the studies conducted were in Asia and Africa, and this fact limits the level of generalizability to other populations. Some lacked control groups, which may have weakened comparative analysis. Also, the search was limited to four databases (PubMed, Google Scholar, ResearchGate, and Semantic Scholar), which may have excluded relevant studies found in Embase, Scopus, or CINAHL. As much as these databases were selected based on their access and coverage of peer-reviewed and gray literature, it is important to underscore this drawback and suggest considering more databases in future systematic reviews. Statistically, the small number and sample sizes of included studies may limit the reliability of heterogeneity measures like I² and Tau². According to Thorlund et al, 24 these estimates can be very different in small meta-analyses, and they are to be interpreted cautiously.
Conclusion
This systematic review and meta-analysis highlight significant variations in hepatic Doppler indices, HARI, PVV, and PVPI, among patients with FLD. Compared with healthy controls, FLD patients exhibited a 0.08 reduction in HARI, a 2.92 cm/sec reduction in PVV, and a 1.32 reduction in PVPI, indicating altered hepatic hemodynamics. These changes are attributed to compensatory mechanisms, such as vasodilation of the hepatic arteries, which increase hepatic artery flow and reduce resistance in response to decreased portal vein flow. The severity of FLD in the study cohorts influenced the range of Doppler indices observed, with more advanced disease associated with greater reductions in PVV and VPI. These findings emphasize the benefit of using Doppler as a nonionizing and low-cost noninvasive tool to diagnose and monitor the FLD, especially in areas having limited access to other diagnostic imaging tools. The application of hepatic Doppler indices for future research to predict disease progression and treatment response, and to standardize measurement techniques to reduce variability between studies should be considered. In summary, this review finds that Doppler plays an important expanding role in the management of FLD as a less invasive approach to diagnostic intervention.
Supplemental Material
sj-png-1-jdm-10.1177_87564793251380858 – Supplemental material for Variations in Hepatic Doppler Indices in Patients Presenting With Fatty Liver Disease: A Meta-Analysis
Supplemental material, sj-png-1-jdm-10.1177_87564793251380858 for Variations in Hepatic Doppler Indices in Patients Presenting With Fatty Liver Disease: A Meta-Analysis by Sobechukwu Warric Iwene Onwuzu, Uchenna Ugbala, Chukwunonso Ugbome, Ebubechi Udeh, Christiana Udeh, Stanley Udeh, Chelfrey Ucheoma and Kasiemobi Udegbunam in Journal of Diagnostic Medical Sonography
Supplemental Material
sj-png-2-jdm-10.1177_87564793251380858 – Supplemental material for Variations in Hepatic Doppler Indices in Patients Presenting With Fatty Liver Disease: A Meta-Analysis
Supplemental material, sj-png-2-jdm-10.1177_87564793251380858 for Variations in Hepatic Doppler Indices in Patients Presenting With Fatty Liver Disease: A Meta-Analysis by Sobechukwu Warric Iwene Onwuzu, Uchenna Ugbala, Chukwunonso Ugbome, Ebubechi Udeh, Christiana Udeh, Stanley Udeh, Chelfrey Ucheoma and Kasiemobi Udegbunam in Journal of Diagnostic Medical Sonography
Supplemental Material
sj-png-3-jdm-10.1177_87564793251380858 – Supplemental material for Variations in Hepatic Doppler Indices in Patients Presenting With Fatty Liver Disease: A Meta-Analysis
Supplemental material, sj-png-3-jdm-10.1177_87564793251380858 for Variations in Hepatic Doppler Indices in Patients Presenting With Fatty Liver Disease: A Meta-Analysis by Sobechukwu Warric Iwene Onwuzu, Uchenna Ugbala, Chukwunonso Ugbome, Ebubechi Udeh, Christiana Udeh, Stanley Udeh, Chelfrey Ucheoma and Kasiemobi Udegbunam in Journal of Diagnostic Medical Sonography
Footnotes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
