Abstract
Testicular metastasis from prostate cancer is a rare occurrence. This case report describes a 63-year-old man with a history of metastatic prostate cancer, who presented with right-sided scrotal swelling. Sonography revealed a right hydrocele and an incidental left testicular mass, later confirmed as bilateral testicular metastases, through orchiectomy. Given the nonspecific symptoms and the rarity of testicular involvement, such cases may be overlooked without thorough diagnostic imaging. This report highlights the importance of sonography in evaluating scrotal abnormalities in prostate cancer patients, even in the absence of pain or palpable masses, to ensure timely diagnosis and management of uncommon metastatic sites.
Testicular metastasis from a prostate cancer is a rare occurrence. 1 It has been documented in less than 4% of patients, and often found incidentally, or at autopsy. 2 The most common site of metastasis associated with prostate cancer is bone, followed by lymph nodes, liver, and thorax. 3 The documented patient cases of testicular metastases are typically in older men compared to patients with primary testicular cancer, with both primary and metastatic occurring most often unilaterally. 4 It is common for patients to have testicular swelling with or without pain during the course of treatment of prostate cancer. 5 However, at least one case of testicular metastasis from prostate cancer was incidentally detected in an asymptomatic patient. 6 With the rarity of testicular metastases and nonspecific nature of scrotal swelling, it is possible to overlook the necessity for diagnostic imaging in these patients. This case report reviews a rare case of bilateral testicular metastasis from prostate cancer that was discovered by sonography. The sonogram was ordered for suspected recurrence of a hydrocele and was definitively diagnosed at the time of surgical removal.
Case Report
A 63-year-old man presented for a scrotal sonogram with a right-sided swelling, without pain. A sonogram from an outside facility reported a right hydrocele that was subsequently drained at that facility about 1 month, prior to the current visit. The patient had a history of metastatic prostate cancer diagnosed about 8 years prior, with surgery and chemotherapy as treatment. His tumor metastasis was originally located in the urinary bladder.
The sonographic findings from the current study were a large right hydrocele and heterogenous appearance of the right testicle (See Figure 1). The left testicle was heterogenous with one hypervascular mass seen within the testicle (See Figures 2 and 3). An additional mass with microcalcifications was seen outside of the testicle and adjacent to the epididymis (See Figures 2 and 3). Following a discussion with his physician and considering his prior medical history, the patient elected to undergo a bilateral orchiectomy. No further diagnostic imaging was performed prior to the surgery, approximately 3 weeks after the sonogram.
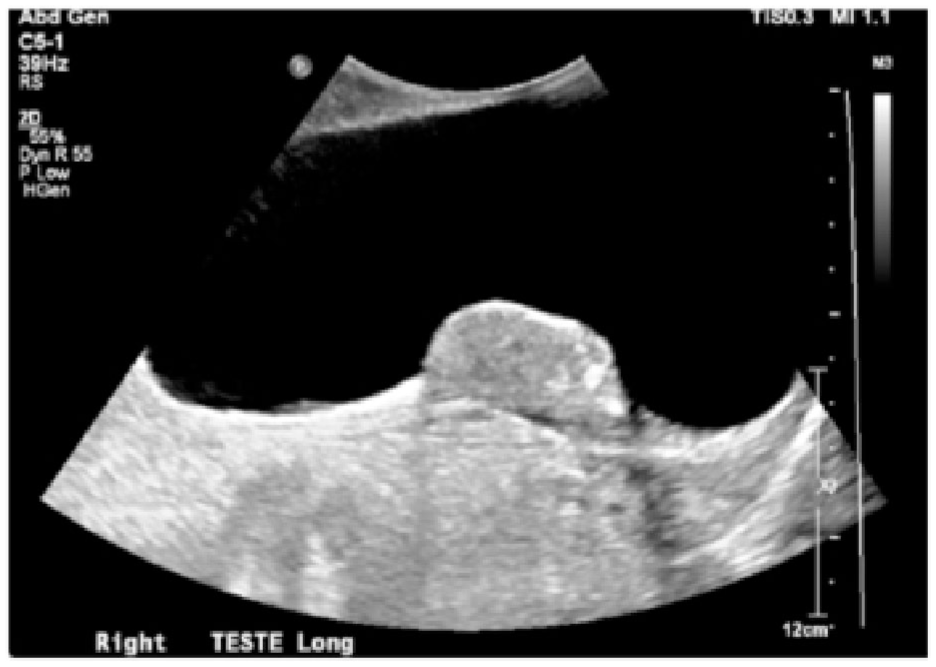
A sonographic longitudinal view of the patient’s right testicle in conjunction with a large hydrocele.
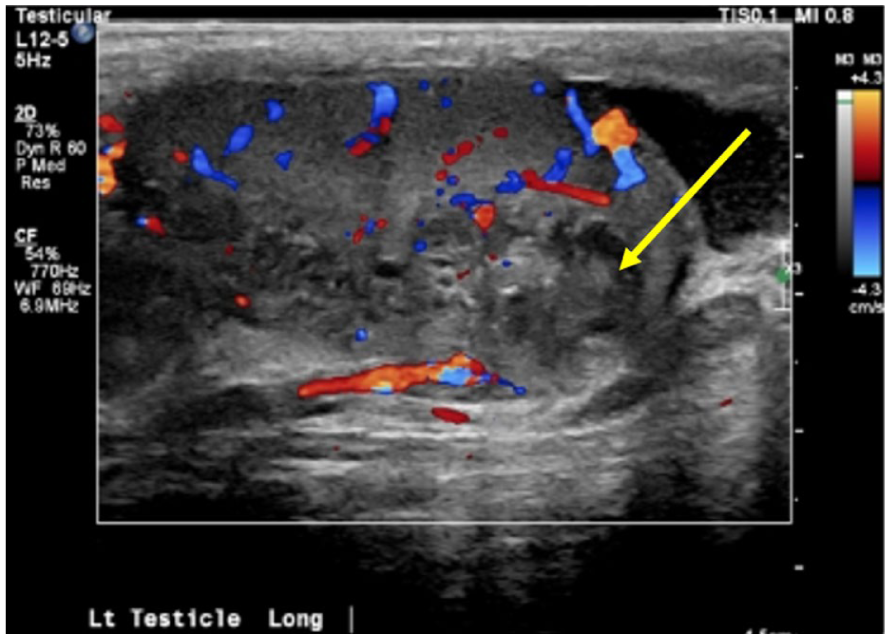
The use of color Doppler helps to demonstrate a mass (indicated by a yellow arrow), contained within the left testicle.
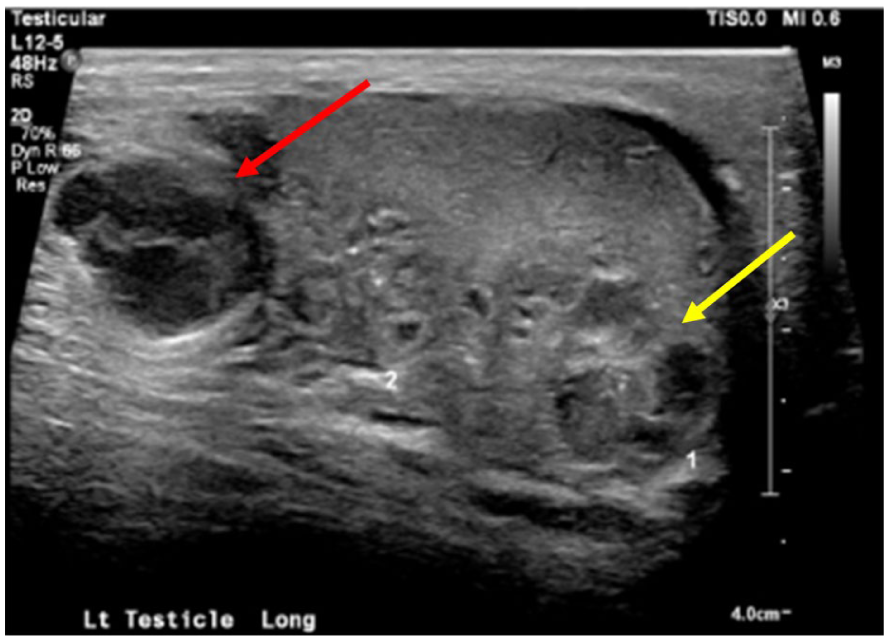
A sonographic longitudinal view demonstrates masses within (indicated by a yellow arrow) and adjacent (indicated by a red arrow) to the left testicle.
The pathology report for the right orchiectomy identified right metastatic high-grade prostate acinar adenocarcinoma involving testicular tissue, epididymal tissue, vas deferens, and extending to the spermatic cord. The pathology report for the left orchiectomy showed metastatic high-grade prostate acinar adenocarcinoma involving testicular tissue only. Surgical removal was the definitive treatment for the testicular metastases; however, new metastatic lesions were discovered in the brain on a contrast magnetic resonance imaging (MRI) examination, a couple months later and radiation treatment was started.
Discussion
Prostate cancer is the most common cancer to be diagnosed among men and when it becomes aggressive and can metastasize directly to skeletal bones.3,7 There have been theories that metastasis to the testicles is rare due to the lower temperature of the testes, within the scrotum. 8 Arterial embolism, retrograde venous, or lymphatic extension, and through the lumen of the vas deferens are the four ways prostate cancer is thought to spread to the testes. 7
One factor that makes this case interesting is that the patient presented with complaints of recurrent swelling in his right scrotum without pain or palpable lump in either testicle. He had no complaints or concerns about the left side of his scrotum upon initial evaluation. The patient ultimately was diagnosed with bilateral testicular metastases based on pathology after surgical excision. A case report published by Connelly et al 9 also reported on a case of bilateral testicular metastases. In that case, the patient did present with bilateral palpable testicular masses a year after initial diagnosis of high-grade prostate adenocarcinoma. It is also extraordinary that the current patient had bladder metastasis at the time of original diagnosis of prostate cancer, bilateral testicular metastases years later, and finally a third metastatic site of the brain, all of which are rare, based on available literature. 8
Prostatic cancer metastasis to the testicles is difficult to treat without performing an orchiectomy. Some believe that this could be due to the blood-testis barrier (BTB) that is formed by seminiferous epithelium cells compartmentalizing into basal and apical layers to protect the testicles from paracellular flow of substances that could be potentially harmful. 10 This barrier works very similarly to the blood-brain barrier (BBB) that is found in the brain and has the same basic function. These barriers regulate the entrance of substances through the bloodstream, whether they are nutritional or toxicants. Both the BTB and the BBB work as immunological barriers to protect the body. 10 There is currently no standard treatment for metastatic prostate cancer, but the National Comprehensive Cancer Network has guidance that includes definitive therapies such as surgery and radiation, non-definitive therapies including monitoring, or a combination of these treatments. 11 While the prognosis for localized prostate cancer is good with a 5-year survival rate of almost 100%, the 5-year survival rate with metastatic, or stage IV prostate cancer, is only 30.6%. 12
The use of different diagnostic imaging techniques in the screening, diagnosis, and surveillance of prostate cancer can vary. According to a review of imaging used in prostate cancer by Gravestock et al, 13 a combination of prostate specific antigen levels, transrectal sonography-guided biopsy, various types of MRI, and positron emission tomography/computed tomography are utilized. The American College of Radiology appropriate use criteria for the detection, surveillance, and staging of prostate cancer is complex and dependent on the timing of investigation and risk-stratification. 14 The recommendations include various combinations of the imaging listed above without the use of sonography, for diagnosis or follow-up. 14 Targeted imaging of symptomatic areas is the main role of sonography, as demonstrated in the current patient case. Following standard sonography protocols can also lead to imaging of asymptomatic areas. For instance, in this case the left side of the scrotum was also imaged despite lack of symptoms due to standard protocols.
Conclusion
Metastasis of prostate cancer to the testicles, especially bilaterally, is considered to be rare. Prostate cancer is more likely to spread to other areas of the body. Scrotal swelling is often accepted as a common symptom in a patient that has had surgery or undergoing treatment for a known cancer, especially in the prostate. A recurrent documented hydrocele can further complicate the patient’s “clinical picture” and possibly falsely assure the physician no further imaging is needed. It is also vital for the sonographer to obtain a complete history from the patient, especially identifying any prior history of cancer and follow standard sonography protocols. In this patient case, if the left side had not imaged, per the standard imaging protocol, the diseased portion of the left testicle may have progressed causing delayed treatment and a worse outcome.
Footnotes
Acknowledgements
We acknowledge the use of AI-assisted tools, including ChatGPT, in the drafting and refinement of the abstract portion of this article only.
Ethics Approval
Ethical approval was not sought for the present study because all case data were de-identified.
Informed Consent
Informed consent was not sought for the present study because all case data was de-identified and/or aggregated and followed ethics committee or IRB guidelines (also referred to as the Honest Broker System).
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
