Abstract
Objective:
To determine the correlation of umbilical venous flow rate (UV-Q) and fetal abdominal subcutaneous tissue thickness (FASTT) with estimated fetal weight (EFW), and explore the possibility of utilizing UV-Q and FASTT to predict EFW.
Materials and Methods:
A total of 110 singleton pregnancies between 27 and 37 weeks were enrolled into this study. UV-Q and FASTT were measured at the sonographic imaging plane where the abdominal circumference is measured. Estimated gestational age (EGA) and EFW were determined according to the standard sonographic measurement protocol.
Results:
UV-Q and FASTT ranged between 29.10 and 387.01 mL/min, and between 0.40 and 1.10 cm, respectively, and both correlated positively with EGA and EFW (p = .000). Mean UV-Q and mean FASTT increased in a linear fashion from 27 to 37 weeks of gestation. An EFW prediction equation was established using UV-Q and FASTT; EFW = 0.561 + 0.005 (UV-Q) + 1.165 (FASTT).
Conclusion:
The proposed equation derived from measuring UV-Q, at the intra-abdominal site, and FASTT, may be a diagnostic tool that could be adopted for the determination of EFW, in the third trimester. Further studies are needed to replicate this work and assess the potential clinical application of the equation for fetal monitoring during pregnancy.
Keywords
A reliable estimated fetal weight (EFW), obtained using sonography, is essential for a favorable management of pregnancies because it is an important determinant of perinatal and neonatal survival.1,2 A combination of sonographic derived biometric parameters is commonly used to ascertain EFW.3,4 However, it has been reported that a percentage error as high as 25% occurs when this method is utilized. This measurement error is even higher with fetal growth abnormalities.3–5 Consequently, delays in the initiation of interventional measures during pregnancy or parturition commonly ensue due to the absence of a warning or notification for both small and large for gestational age fetus.4,5
The sonographic measurement of fetal abdominal subcutaneous tissue thickness (FASTT), in utero, has been reported to be an important means of determining EFW.1,3,4 FASTT is reduced with intra-uterine growth restriction (IUGR) and increased with macrosomia. It is important to assess FASTT of fetuses in diabetic mothers, since they are at increased risk of macrosomia and its associated complications such as labor dystocia, instrumental delivery, shoulder dystocia, and perineal tears.3,6,7
Conversely, umbilical venous flow rate (UV-Q) mirrors the volume and rate at which nutrients and oxygen in blood are conveyed to a developing fetus, through the umbilical vein. 8 UV-Q increases in geometric proportion throughout the course of pregnancy from 65 mL/min at the 20th week of gestation to 373 mL/min at the 38th week of gestation.8,9 Essentially, UV-Q has to be sufficient to meet with fetal demands for proper growth and to ensure that the fetal weight in utero is appropriate for gestational age.8,9
Fat in the fetus is stored in the subcutaneous tissue of the abdomen and liver, as glycogen contributing to the determination of the girth or circumference of the fetal abdomen.2,10,11 Umbilical venous flow rates significantly correlate with fetal abdominal circumference (AC) measurements. 12 In the setting of a normal fetus, UV-Q potentially determines fat accumulation in the abdomen. 12
The evaluation of umbilical venous flow rate is regarded as a more precise physiological assessment of vascular placental function than umbilical arterial velocimetric indices because it reflects the efficiency of the placenta at coordinating the exact amount of oxygen, nutrient and blood volume necessary for the appropriate development of a fetus. 13 Several studies have demonstrated that in growth-restricted fetuses, where the fetal weight in utero is reduced for gestational age, the umbilical venous flow rate is reduced.14,15 UV-Q is a parameter in which the importance to the fetus is similar to that of cardiac output and lung perfusion evaluation to adults. 16
It is pertinent to identify other techniques, which might be equally or more reliable, to determine fetal weight in utero and identify fetuses at risk of intra-partum compromise, such as the evaluation of UV-Q and FASTT. This could promote more targeted methods at antenatal and intra-partum fetal monitoring, and allow more certainty in effecting interventional measures, such as the optimal time and safest mode of delivery. 14
The aim of the study was to determine the correlation of UV-Q and FASTT with EFW in apparently normal pregnancy and explore the possibility of utilizing UV-Q and FASTT to predict EFW.
Materials and Methods
This prospective cross-sectional study was done in the radiology department of a tertiary health facility. The study was conducted over 6 months from October 2024 to March 2025. Ethical approval for this study was obtained from the host institution’s Institutional Review Board (UCTH/HREC/33/Vol.111/079).
Apparently, normal pregnant women attending the antenatal clinic of the health facility, who met the eligibility criteria, were recruited as subjects for the study. The exclusion criteria for this study were: pregnancies below 27 weeks and above 37 weeks of gestation, pregnant women in labor, multiple pregnancy, pregnancy-induced hypertension, gestational diabetes, pre-eclampsia, maternal cardiovascular disease, pregnant women with chronic conditions (such as hypertension, diabetes, auto-immune disease, sickle cell disease, human immune-deficiency virus, tuberculosis, renal disease), placental anomaly, grade 2 and 3 placental calcification, hydrops fetalis, oligohydramnios, umbilical artery abnormalities, cord entanglement, nuchal cord, velamentous cord insertion, and fetal malformation.2,14,15,17,18
Sample Size Determination
An a priori power analysis was done to determine the sample size for the study. The statistical test selected for the analysis was multiple linear regression. The statistical significance level (alpha) was set at p = .05, while the desired power was 0.95. After the calculation, the required sample size for the study using two predictors was shown to be 107 and this was approximated to 110 participants. Following the employment of convenient purposive sampling technique, participants were recruited for the study. Written informed consents were obtained from each of the participants.
Sonographic Examination
Each participant underwent a transabdominal sonographic evaluation where EFW was determined, using the Hadlock method. FASTT and UV-Q, from Doppler studies were obtained. The estimated gestational age (EGA) was determined from the last menstrual period (LMP) of the participants, as documented in their electronic medical record, which had been corroborated by a first trimester sonogram. The participants in the study were evaluated once during the course of their pregnancies. The obstetric sonographic examination and Doppler studies were done using Xario-100 TUS-X100S (Canon Medical Systems Corp., Otawara, Japan) with a 3.5-MHz curvilinear transducer. The obstetric sonographic examination to determine EFW was solely conducted by one of the authors, whereas another author conducted the Doppler studies to determine UV-Q. Both of them are consultant radiologists with more than 15 years experience in sonography. They were both anonymized to the EGA status of the subjects. Two ultrasound equipment systems were kept in separate suites and used for the study. The quality control of these machines is assessed by well-trained biomedical engineers. Routine quality control tests were performed quarterly to ensure proper function and identify potential problems before they affect the diagnostic usefulness of the equipment systems.
For the obstetric sonographic examination, each participant was requested to lie in a left posterior oblique position to avoid prolonged compression of the inferior vena cava. An adequate amount of coupling gel was placed on their abdomen before the sonographic examination commenced. 14
EFW Assessment
Hadlock’s three-parameter formula, for EFW, was generated by the ultrasound equipment software, which utilizes the fetal head circumference (HC), AC, and femur length (FL). It has been proven to be a precise method to determine EFW since it reduces the degree of error to the bare minimum. 19 The acquisition of the HC measurement was based on the sonographic image of the axial plane of the fetal skull. It required the measurement of the HC, including the thalami, separated by the third ventricle, and the echogenic falx cerebri at the midline, which is interrupted anteriorly by the cavum septum pellucidum. Both hemispheres are separated by the midline echogenic falx cerebri and appear symmetrical. The measurement was obtained by placing an ellipse to surround the outer border of the fetal skull. 20 The acquisition of the AC measurement was made from the sonographic image, in the transverse plane, of the fetal abdomen. The fetal abdomen was circular and included the intra-hepatic portion of the umbilical vein, the stomach, and the spine. The measurement was obtained by placing an ellipse around the outer surface of the fetal abdominal skin line. 20 The FL measurement was taken from the sonographic image of the fetal femur. It required that both ends of the ossified diaphysis were visible and kept as horizontal as possible. Each caliper was placed at the ends of the ossified femoral diaphysis and the distance between them is taken as the FL. 20
UV-Q Assessment
The umbilical vein was assessed in the intra-abdominal site, at the same plane where the AC is measured with the fetal spine at the 3 o’clock or 9 o’clock position. This was done to ensure optimal visualization of all anatomical landmarks. The major advantage of utilizing this site is because it is immovable, since it is embedded in the fetal liver, and this aids the reproducibility of this measurement.8,20 Color Doppler was used to identify the umbilical vein. The angle of insonation was maintained at 30°, 8 while the Doppler interrogation sample gate was 1.0 mm and placed at the center of the vessel, and about 1.0 cm away from the fetal abdominal surface.8,13 When the velocity profile of the spectral wave display was uniformly flat-fronted the image was frozen and the maximum velocity of the umbilical venous flow was measured in cm/seconds (See Figure 1C). 21
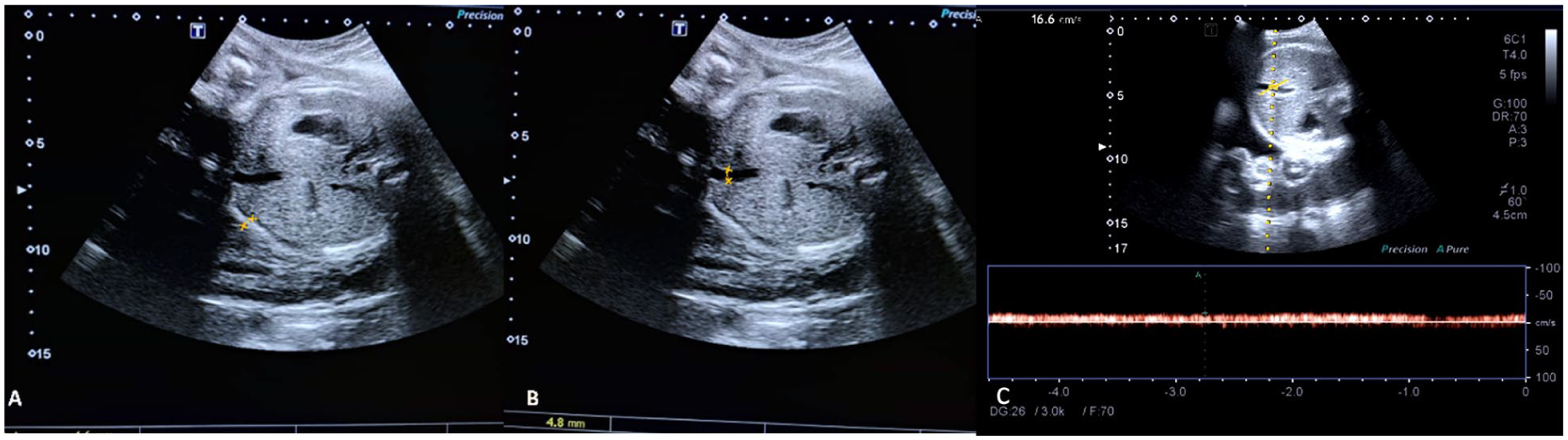
An example greyscale sonogram is provided of a 31-week gestation fetus, captured with a curvilinear transducer. The distance between the cursors that lie at the outer and inner edges of the echogenic subcutaneous fat line measures the FASTT (A). The distance between the cursors placed at the anterior and posterior walls of the umbilical vein, in the intra-abdominal location, measures the umbilical vein diameter (B). The maximum velocity of the umbilical venous flow is obtained by measuring the peak velocity in the spectral wave display of the duplex-mode sonogram (C).
To obtain the umbilical vein diameter, an image showing the vessel at the intra-abdominal site, in the same imaging plane where the AC is measured, was frozen. At a point less than 1 cm away from the fetal abdominal surface, the internal diameter of the umbilical vein was measured, in centimeters (See Figure 1B). All the measurements were done in the absence of uterine contractions and reduced fetal activity, and they were repeated three times with the mean values recorded. The umbilical venous flow maximum velocity and umbilical vein diameter were used to calculate UV-Q.14,15 The following calculation were preformed:
FASTT Assessment
The FASTT was measured in cm along the anterior third of the abdomen, at the same level where the AC was obtained, by measuring from the outer edge to the inner edge of the echogenic subcutaneous fat line, at the point where these edges are clearly delineated (See Figure 1A). Optimal depth was ensured so that the lowest part of the fetal abdominal cross-section was clearly visible and limited transducer pressure was also applied while obtaining the fetal AC. 1 The measurement was done three times and the mean calculated.
Data Analysis
The data obtained (which included relevant demographic features of the subjects) were analyzed using the IBM Statistical Package for Social Sciences (SPSS) for Windows (IBM SPSS Inc., Chicago, IL, USA) version 23. Continuous variables were reported as means (with standard deviation) and range. Spearman’s rank order was used to determine normality of data. Correlations were determined using Pearson’s correlation. Multiple linear regression analysis was done to construct the predictive equation for EFW using the evaluated UV-Q and FASTT. Statistical significance had already been set at p < .05.
Results
The age range of the participants was from 17 to 38 years and the highest parity observed in the participants was 7.0. The mean EFW was 2.20 ± 0.74 kg while the values of the UV-Q and FASTT ranged from 29.10 to 387.01 mL/min and 0.40 to 1.10 cm, respectively (See Table 1).
The Descriptive Characteristics Are Provided for the Cohort of Study Participants (n = 110).
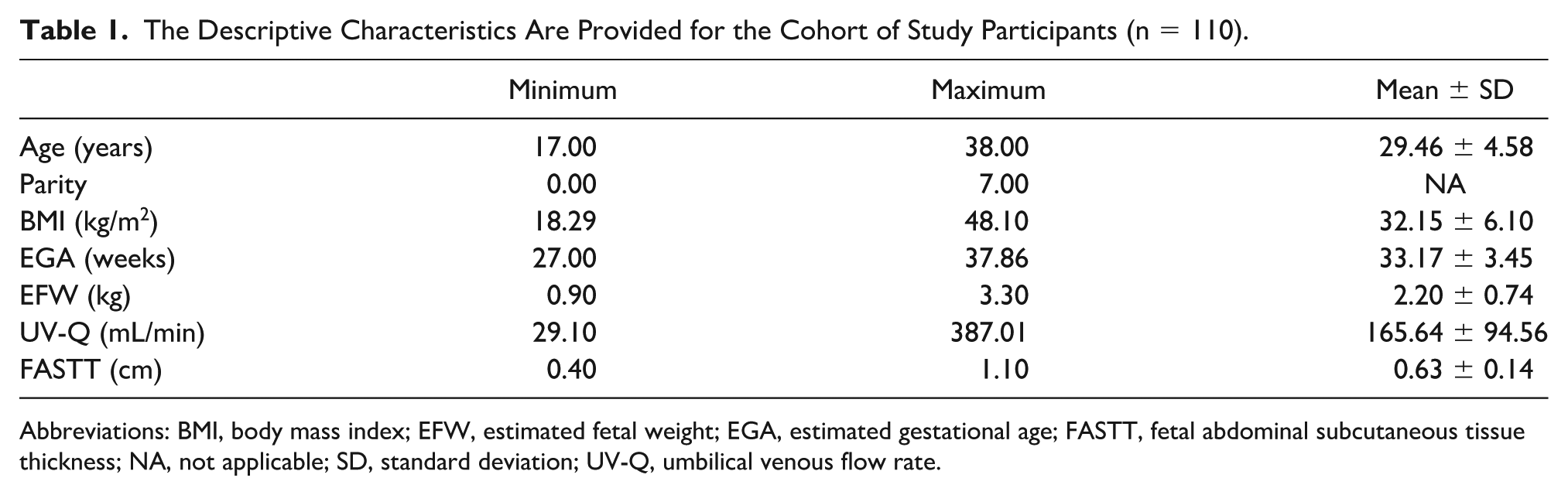
Abbreviations: BMI, body mass index; EFW, estimated fetal weight; EGA, estimated gestational age; FASTT, fetal abdominal subcutaneous tissue thickness; NA, not applicable; SD, standard deviation; UV-Q, umbilical venous flow rate.
While the sociodemographic features of the participants in the study, which were age, parity, and body mass index (BMI), did not attain significant correlation with UV-Q and FASTT, the r value of both EGA and EFW did, in a positive fashion, and the strength of the relationship was strong in both instances (r = .871 and r = .886; r = .817 and r = .834; p < .001). UV-Q significantly correlated with FASTT (p < 0.001) (See Table 2).
The Strength of Association of UV-Q and FASTT With Other Study Variables (n = 110).
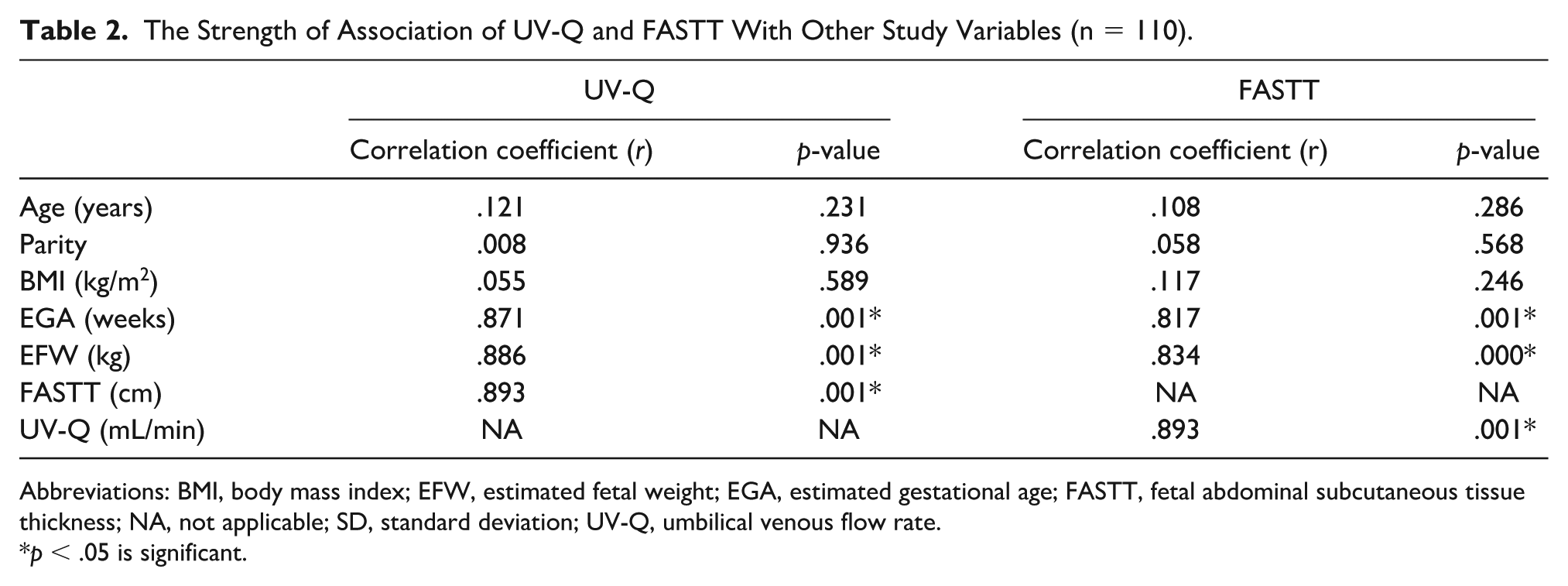
Abbreviations: BMI, body mass index; EFW, estimated fetal weight; EGA, estimated gestational age; FASTT, fetal abdominal subcutaneous tissue thickness; NA, not applicable; SD, standard deviation; UV-Q, umbilical venous flow rate.
p < .05 is significant.
UV-Q, FASTT, and EFW were shown to progressively increase in value from the 27th to the 37th week of gestation. The r value of the model was .891 which indicated a good level of prediction by the independent variables. The r2 value was .794 and demonstrated that the independent variables utilized in the model explained 79.4% of the variability of the dependent variable (EFW). The independent variables (UV-Q and FASTT) were shown to be significant as predictors of the dependent variable (p < .05). The standard error of the estimates from the model summary was 0.339. The equation generated from the multiple linear regression analysis was EFW = 0.561 + 0.005 × UV-Q + 1.165 × FASTT (See Tables 3 and 4).
The Mean Values for UV-Q and FASTT, Based on the Participants at 27 to 37 Weeks of Gestation.
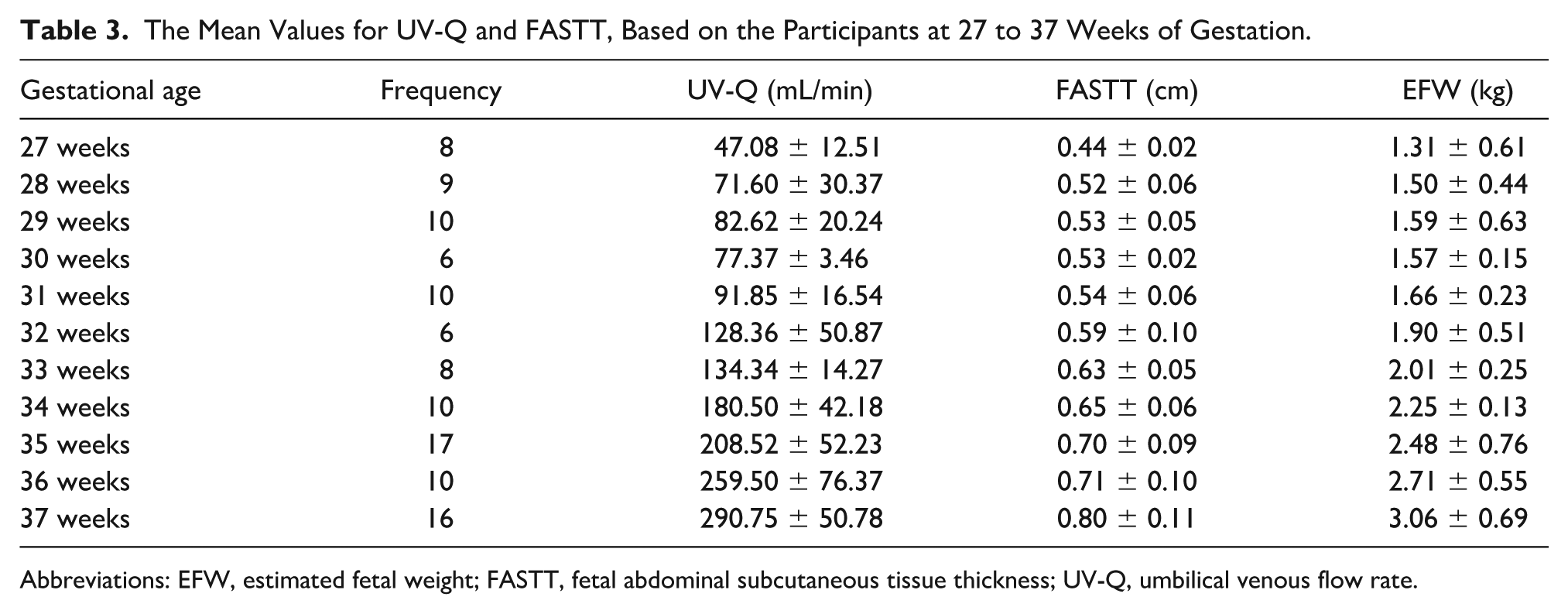
Abbreviations: EFW, estimated fetal weight; FASTT, fetal abdominal subcutaneous tissue thickness; UV-Q, umbilical venous flow rate.
A Multiple Linear Regression Analysis of UV-Q and FASTT Used to Predict EFW.
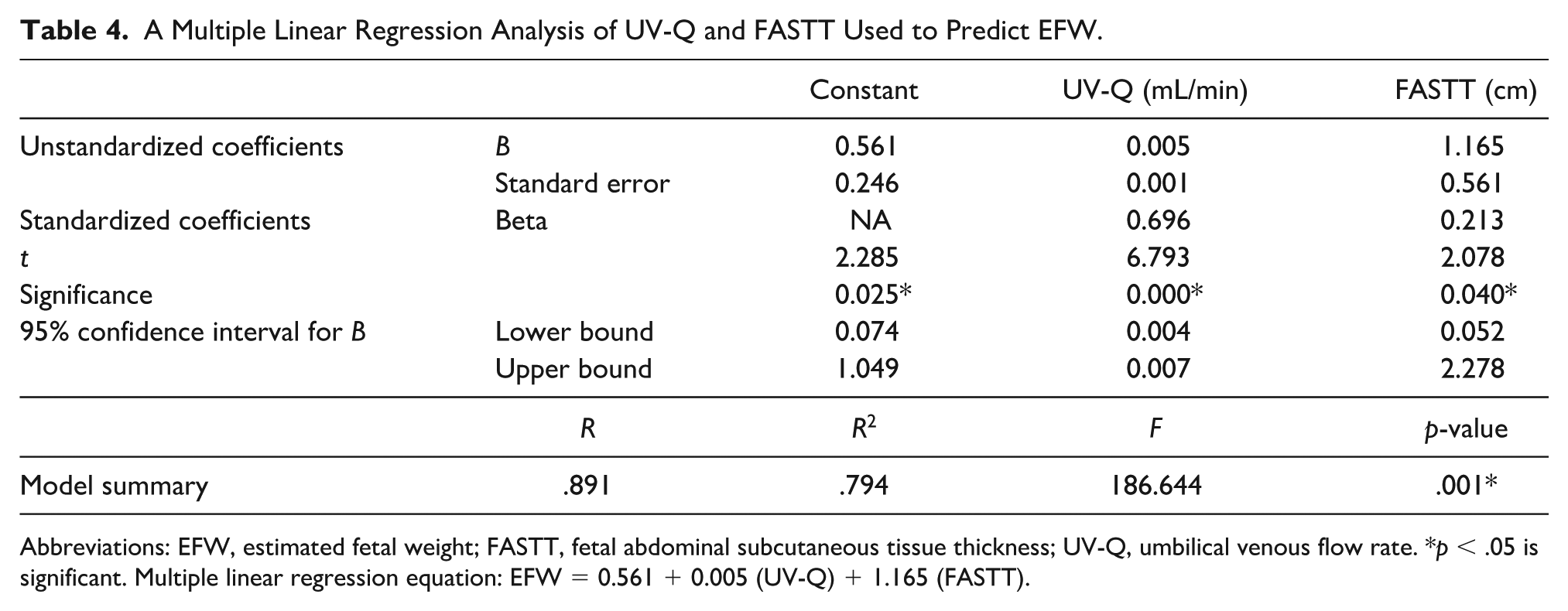
Abbreviations: EFW, estimated fetal weight; FASTT, fetal abdominal subcutaneous tissue thickness; UV-Q, umbilical venous flow rate. *p < .05 is significant. Multiple linear regression equation: EFW = 0.561 + 0.005 (UV-Q) + 1.165 (FASTT).
Discussion
Optimal antenatal care, which ensures a successful maternofetal outcome in peripartum and postpartum, predominantly depends on a consistent determination of accurate EFW. The evaluation of EFW also provides obstetricians the criteria to make crucial decisions on the best route of delivery.1,2,14
In this cohort, UV-Q was shown to significantly correlate with FASTT. The nutrient supplied by the placenta is deposited at the fetal abdomen as a fatty mass which ultimately determines the value of FASTT.1,3 As a result it can be postulated that FASTT could be an objective means of determining the adequacy of UV-Q or that the increment in the values of both variables occur in pari passu.1,3 Concordant with the findings of the present study, Kiridi et al, 9 Barbera et al, 12 and Fang et al 15 and all observed that the estimated fetal AC, whose girth is strongly influenced by the thickness of the abdominal subcutaneous fat, significantly correlated with UV-Q (p < .001), in a positive direction.
To further support this correlation, several publications have reported that the value of UV-Q drops considerably in growth-restricted fetuses, where FASTT is also likely reduced. Ozawa et al 22 suggested that this drop is brought about by the impaired distribution of placental blood flow and systemic circulation that are frequently seen in the condition. Aligning with them, Farsetti et al 23 demonstrated that UV-Q was significantly lower in fetal growth restriction compared with constitutionally small fetuses. The submission was that in growth-restricted fetuses the umbilical venous flow velocity significantly diminishes, whereas the umbilical vein diameter remains unaltered. 24
It was demonstrated in the current study that UV-Q and FASTT increased in a linear fashion as the gestational age of the pregnancies advanced. Same congruity of findings was reported by Fang et al 15 in China, Kiridi et al 9 in Nigeria, Khalifa et al 1 in Egypt, Chen et al 5 also in China, and Jelany et al 25 in Pakistan. The rise in UV-Q and FASTT as pregnancy progresses is basically a result of the increase in the dimensions of the fetal vessels.1,9 Conversely, Ozawa et al 22 stated that the increase in UV-Q in proportion to the gestational age is a consequence of elevated cardiac output which occurs with the advancement of pregnancy. It is pertinent to note that the placental circulation receives about 25% to 30% of the fetal cardiac output. 22 Oriji et al 21 further observed that the increase in UV-Q with the progress of pregnancy continues beyond 40 weeks of gestation. In addition, they found out that the highest mean umbilical venous flow velocities were observed in post-date fetuses. In variance, Prior et al 14 noticed the non-existence of a significant correlation between umbilical venous flow rate and EGA in their United Kingdom cohort study. This deviation was likely because the researchers opted to evaluate the umbilical venous flow rate at the free loop of the umbilical cord.
UV-Q and FASTT were both observed to have a significant positive relationship with EFW in the present study. Similarly, Khalifa et al 1 in a prospective observational study on 100 pregnant women found out that FASTT correlated significantly with EFW. It was further noted that this significant relationship with fetal birth weight still existed 11 days after the FASTT evaluation.3,5 Gardeil et al, 26 in Ireland, observed that fetuses with higher FASTT often had higher birth weights and most were macrosomic babies. Solyman et al, 27 in Egypt, demonstrated that FASTT had a statistical relationship with both EFW and birth weight of significant proportions in a positive direction. Their study had enrolled 72 full-term singleton pregnant women who delivered 48 hours after the ultrasound evaluation.
Assimakopoulos et al 4 reported on a Greek cohort that showed that the correlation between FASTT and birth weight reached statistical significance in a positive fashion (p < .001). Singh et al 11 discovered that FASTT significantly correlated with actual birth weight (p < .001). This re-affirmed the fact that FASTT can be utilized to accurately predict birth weight. Moreover, it is also an appropriate tool to predict fetal growth aberration associated with anomalies in soft tissue thickness. 11
Similar to the findings of the present study, Prior et al 14 observed a significant positive correlation between umbilical venous flow rate and EFW in their study population. Barbera et al, 12 in Italy, also realized that UV-Q increased in an exponential manner from the 20th to the 40th week of gestation. In addition, Kiridi et al 9 , Fang et al, 15 and Jelany et al 25 all observed that UV-Q significantly correlated with EFW (p < .001).
Protein-calorie deprivation culminates to the wasting of fetal soft-tissues but fetal skeletal growth is relatively spared, and consequently, this impoverished state of fetal health is usually not reflected in the EFW obtained using the regular sonographic parameters.24,28 However, the assessment of UV-Q (which determines the rate at which glucose is transported and its excess stored as glycogen at the fetal abdominal subcutaneous region) and FASTT (which mirrors the adequacy of nutrition) are potentially two highly reliable and accurate methods that takes into cognizance fetal soft tissue waste in the course of ascertaining fetal weight in utero.24,28
The importance of the availability of reliable means to accurately determine EFW has led to the development of several predictive models. Fang et al 15 employed a linear regression equation to formulate an EFW predictive model utilizing UV-Q normalized with EFW. The efficacy of this equation demonstrated positive validation results. The model is potentially a means to alert clinicians of fetuses at risk of having abnormally low or high weight during the third trimester.
Odthon et al 10 showed that employing FASTT alone as a diagnostic parameter with a cut-off of ≥10 mm to predict macrosomia had an 81.0% sensitivity, 86.8% specificity, 98.4% negative predictive value (NPV), and 86.4% accuracy. Kongsing et al, 29 in Thailand, who recruited singleton pregnant women between 26 and 37 weeks of gestation with clinically suspected IUGR, determined that FASTT at a cutoff of ≤4.5 mm at 35 and 36 weeks of gestation had a diagnostic sensitivity, specificity, NPV, and accuracy of 76%, 75.29%, 91.42%, and 75.74%, respectively, to predict lower birth weight babies.
Wang et al, 30 in China, built a deep neural network predictive model for EFW calculation using 10 parameters and six of them were ultrasound data. They observed that the accuracy of this model was 83.87% and had a root mean square error of 243.80 g. Furthermore, they discovered an excellent area under curve (0.918) for predicting macrosomia. They subsequently inferred that the model was more reliable in determining the EFW in a pregnancy than Hadlock’s formula and multiple linear regression predictive models.
Dulger et al 31 revealed in a study that enrolled 730 pregnant women that the elastic net regressor algorithm was reliable for fetal weight prediction. The result produced by this model was shown to exhibit an average absolute error percentage of 8.87% and an average error of ±284 g. Kumari et al, 32 in India, constructed the Gompertz predictive model in research that involved 774 pregnant women and found that the model accurately EFW with less than 8% error.
In the present study, an equation was produced using FASTT and UV-Q to determine EFW. The technique involved in assessing these potential tools has been reported to be easily reproducible and dependable. In addition, the evaluation can also be conducted during the latent phase of labor when the fetal head is engaged.26,33 This is especially important since it is commonly difficult to obtain the appropriate planes for the measurement of fetal HC and bi-parietal diameter when the fetal head is engaged and similar difficulty may be experienced with fetal AC evaluation in large fetuses. These aberrations usually culminate to the calculations of inaccurate EFW. 34
Limitations
It is important to note that the study results were based on a convenience sampling technique and a pre-experimental study design. This creates threats to both internal and external validity. An additional limitation was that each subgroup of gestational age had an unbalanced proportion of participants. Therefore, result percentiles (5th, 10th, 50th, 90th, and 95th) could not be obtained in each gestational age group during data analysis. It is also important to point out that the participants were recruited from one health facility. An added limitation was that this cross-sectional study only included third trimester pregnant women. This also limited the continuous evaluation of pregnancies throughout their course, which could have revealed patterns of temporal relationships. Importantly, the study mainly evaluated the consequence of UV-Q and FASTT on EFW, without taking into consideration the significant roles of the biological factors (i.e., genetic factor) and chemical factors (i.e., vascular growth factors and umbilical venous blood sugar level) responsible for appropriate growth, which ultimately limits the generalization of the results. 15 Another important limitation was that toward term, when the fetal position is fixed, it was observed that fetal bone shadowing was an undesirable challenge to achieving precise UV-Q values at the fetal intra-abdominal site. 8 Last, FASTT measurement was occasionally challenging in obese pregnant women with anterior placentation. 1
In spite of these limitations, the study provided important data that could be potentially useful in the management of pregnancies. However, future research should be conducted to test the performance of the equation on a larger heterogenous population from the second trimester to term, and also compare with actual birth weight, to validate its clinical relevance.
Conclusion
The measurement of UV-Q, at the intra-abdominal site, and FASTT is a composite diagnostic tool that can be adopted for the determination of EFW, in the third trimester. Further studies on the potential clinical application of the equation for fetal monitoring during pregnancy are necessary.
Footnotes
Acknowledgements
The authors sincerely appreciate the commitment of the staff and heads of Departments of the Radiology Department, and Obstetrics and Gynecology Department of the University of Calabar Teaching Hospital, Calabar toward the accomplishment of this research.
Ethics Approval
Ethical approval for this study was obtained from the hospital’s Institutional Review Board (UCTH/HREC/33/Vol.111/079).
Informed Consent
Written informed consent was obtained from all the subjects before the study.
Animal Welfare
Guidelines for humane animal treatment did not apply to the present study because no animals were used during the study.
Trial Registration
Not applicable.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
