Abstract
Objective:
Cardiac sonographers are challenged on a daily basis to provide excellent frontline care for a variety of patients. They face challenges of promoting quality over quantity and continued support for education and training efforts. Echocardiography requires an operator-dependent sonographer with independent judgement and critical thinking skills to obtain and integrate diagnostic information during the echo examination. The growth of echocardiographic procedures has increased the demand for qualified cardiac sonographers to cover the workload.
Materials and Methods:
Occupational employment and wage statistics, educational opportunities, simulation labs and clinical sites, national registries, and ASE standards for a quality echo educational environment are discussed.
Results:
The national curriculum for echocardiography is extensive and requires adequate clinical hands-on training to promote an opportunity for the student to become a competent cardiac sonographer. Credentialing in echocardiography demonstrates to the patients, healthcare professionals, and employers of medical facilities that the cardiac sonographer is a dedicated professional in their respective field.
Conclusions:
Additional accredited cardiovascular programs with active credentialed clinical sites to fulfill this shortage. The skillset has increased with new procedures requiring training in advanced imaging techniques such as three-dimensional imaging, strain, tissue Doppler, and contrast-enhanced imaging.
Keywords
The cardiac sonographer plays an integral role in the diagnostic process with echocardiography. The sonographer should have independent judgment, critical thinking skills, and the ability to obtain and integrate accurate diagnostic information during the performance of the examination. The operator-dependent nature and complexity of practice dictate that the cardiac sonographer functions at a professional level. The American Society of Echocardiography (ASE) Guidelines recommend that individuals who enter the field of cardiac sonography attend education programs that are recognized and supported by the ASE, such as those accredited by Commission on Accreditation of Allied Health Education Programs (CAAHEP), the Joint Review Committee for Cardiovascular Technology (JRC-CVT), and the Joint Review Committee for Diagnostic Medical Sonographers (JRC-DMS), and earn the appropriate cardiac sonographer degree or certificate, in addition to credentialing. 1
The development of the career path for the cardiac sonographer has now extended over five decades. This challenging and exciting field originally began in a few major medical centers with on-the-job training and sharing information of clinical findings with colleagues. Journal articles and white papers were the communication of knowledge available to learn about echocardiography. Commercial ultrasound equipment companies were eager to sell imaging systems and thus provided “Technical Application Specialists” to conduct short courses to provide instruction, for this intriguing new clinical tool. Originally, most sonography labs were located in the Radiology Department, and thus the radiographer was the one chosen to assist the radiologist, during a sonographic procedure. Initially, in many medical centers, cardiology often shared the equipment with radiology, until each field grew so rapidly that cardiology and other specialty areas split away from radiology. to develop their respective clinical programs.
Occupational Employment and Wage Statistics
The median annual wage for individuals with an Associate of Science (AS) degree, in sonography, varied between cardiovascular technologists and diagnostic medical sonographers. In May 2021, the median wage for cardiovascular technologists and technicians was $60 570 (including electrocardiogram [EKG] technicians, telemonitoring technicians, electrophysiology, invasive and noninvasive cardiology), whereas the median annual wage for diagnostic medical sonographers was $77 740.2,3
The US Bureau of Labor and Statistics estimates the occupation of sonography to grow by 14% between 2021 and 2030. 2 These estimates provide sonographers with great job security; however, echocardiography labs now have the challenge of supporting the sonographers’ career growth and continuing education, so they can retain employees, in this current competitive employment environment.
Cardiac Sonographer Shortage
Currently, the available number of qualified candidates for a career in cardiac sonography does not meet the market demand. There are more than 55 000 cardiac sonographers currently employed in the United States. 4 Employment opportunities project an average of more than 10 000 openings for diagnostic medical sonographers and cardiovascular technologists and technicians, each year over the next decade. Many of these openings are a result from the need to replace workers who leave because of the effects of the pandemic, work-related musculoskeletal injury, the transfer to different occupations, or retirement. In addition, orders for echocardiograms are growing with the increasing aging population, as well as the rapid adoption of transcatheter structural heart interventional procedures that require significant echocardiographic assessment and guidance preprocedure, intraprocedure, and postprocedure.
Educational Opportunities
Initially, education and training for the sonographer consisted of on-the-job learning and short-term courses (consisting of one or two-day programs to one week). All areas of sonography continued to expand and grow to such an extent that formalized training was necessary. Hospital programs were located in the radiology department, with a broad coverage of abdominal, cardiac, and obstetrics/gynecology imaging applications. These dedicated sonography educational programs initially were three months that expanded to six months and then one year, as the need for clinical applications developed, within commercial companies.
The first American Society of Ultrasound Technical Specialists (ASUTS) Educational Outlines in Ultrasound were created in 1973 by Sandra Hagen-Ansert, Kathy McDiarmid, Linda London, Laura Schorzman, Judy Alexander, and Joan Korfhagen. This was the initial attempt to provide curriculum unity to the multiple ultrasound programs that were developing throughout the United States.
Diagnostic Medical Sonography was recognized as a separate allied health field by the CAAHEP in the mid-1970s and the Standards and Guidelines for the Accreditation of Educational Programs in Diagnostic Medical Sonography were adopted in 1979. 5 In December 1981, the American Medical Association Council on Medical Education officially recognized Cardiovascular Technology as an allied health profession. 6 Subsequently in 1985, the Standards and Guidelines for the Accreditation of Educational Programs in Cardiovascular Technology were adopted. The most recent Standards and Guidelines were adopted in 2012 for the Advanced Cardiovascular Sonographer. 7 These CAAHEP guidelines were instrumental in providing quality education for those students interested in sonography as a career.
To date, there are now 136 accredited programs for the cardiac sonographer, which includes 45 CAAHEP accredited programs in cardiovascular technology and 91 programs in diagnostic medical sonography, that contain specialized programs in cardiac sonography. In these programs, many offer an introductory course in echocardiography and vascular technology. Most of these programs are associated with a community/technical college or large medical center and grant an AS or bachelor’s degree in diagnostic medical sonography, with a cardiac focus or a degree in cardiovascular technology.
Programs in allied health are very costly, to the institution, as the number of students is limited by the number of active clinical sites available. The CAAHEP states that accredited program resources must be sufficient to ensure the achievement of the program’s goals and outcomes. In our experience, students who complete a minimum of 1500 clinical hours with 40 patients/month are better prepared for an entry-level position in cardiac sonography after graduation. According to CAAHEP, program resources must include, but are not limited to, the following factors: faculty; clerical and support staff; curriculum; finances; offices; classroom, laboratory, and ancillary student facilities; clinical affiliates; equipment; supplies; computer resources; instructional reference materials; and faculty/staff continuing educational opportunities.
National Curriculum for Echocardiography
For programs seeking accreditation in noninvasive cardiology, refer to the “Guidelines for Cardiac Sonographer Education: Recommendations of the ASE Sonographer Training and Education Committee,
1
” and/or echocardiography portion of the ASE approved sonographer core curriculum and/or the National Education Curriculum for Sonography 2008.
6
The comprehensive curriculum includes the following topics: Anatomy and Physiology of the Heart Basic Embryology Physics & Instrumentation Ergonomic Techniques The Echocardiographic Examination Quantitation Principles: M-mode, 2D, Doppler, Calculations Principles of Cardiac Hemodynamics and Cardiac Cycle Ventricular Function Coronary Artery Disease Valvular Heart Disease Cardiomyopathies Systemic and Pulmonary Hypertensive Heart Disease Diastolic Ventricular Function Strain Imaging Endocarditis Pericardial Diseases Cardiac Tumors / Masses Diseases of the Aorta Normal and Altered Electrical Activation Pediatric and Adult Congenital Heart Disease Stress Echocardiography Transesophageal Echocardiography Structural Heart Disease Real-Time 3-D Echocardiography Ultrasound Enhancing Agents (UEAs) Advanced Techniques/Procedures Systemic Disease Miscellaneous Topics: Athlete’s Heart; Heart Failure; Heart Transplant; Cardiac Assist Devices; Multi- Modality Imaging) Quality Control & Improvement Radiation Safety
Use of Simulation in the Clinical Lab
The JRC-CVT recognizes the advancements in simulation technology and thus the importance of simulation as an adjunct to student hands-on training that at one time could only be acquired during the time spent in the clinical site. 8
It is the responsibility of each program to determine the number of hours required for students to develop psychomotor skills and ultimately to demonstrate achievement of terminal learning objectives (final clinical competencies). The program determines how many of these hours are allocated to laboratory sessions and how many are allocated to clinical practice. The use of simulation technology in the program’s comprehensive curriculum design does not, in and of itself, alter the total number of hours dedicated to developing and demonstrating psychomotor learning objectives. The program may discover, however, that some hours previously assigned to the clinical site can be shifted to the program’s laboratory where simulation can be used to develop skills, including those skills that are part of formative competency assessments, before performing the procedure on a patient in the clinical setting (Figure 1).
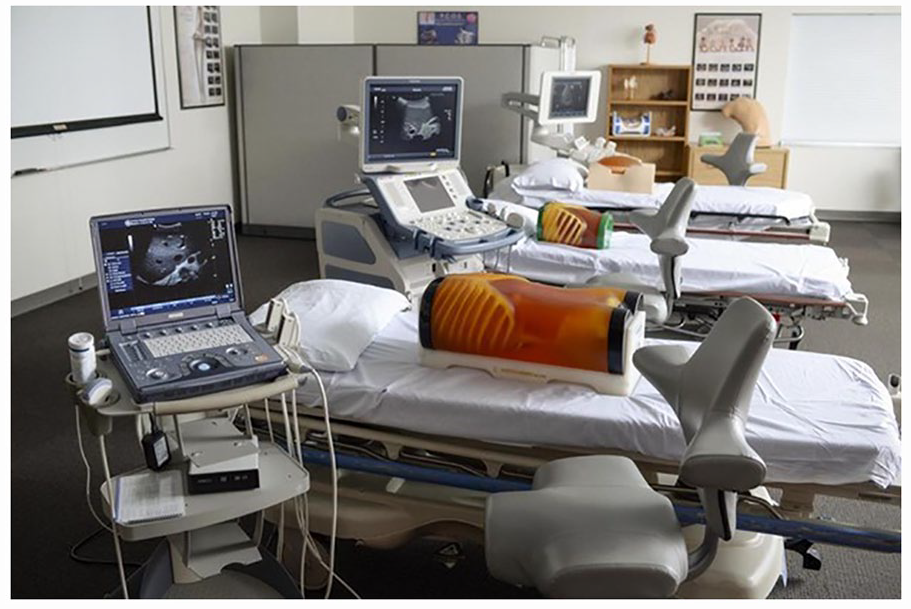
An example of an educational scanning laboratory at the Advent Health University.
The JRC-CVT is not encouraging the elimination of clinical time because that is an integral part of the students’ education. However, the literature supports the use of simulation in nursing and allied health education, and the JRC-CVT believes that the use of simulation can be beneficial during the current time of reduced clinical access by students. While simulation can be used for skill development and formative assessments, the final clinical competency, or learning objective, must be completed on a patient in the clinical setting and documented either by an appropriately credentialed clinical preceptor or by program faculty with the appropriate credentials. The JRC-CVT supports the use of simulation for skill development; however, simulation is not a substitute for documenting clinical competency. 8
Clinical Site Advantages
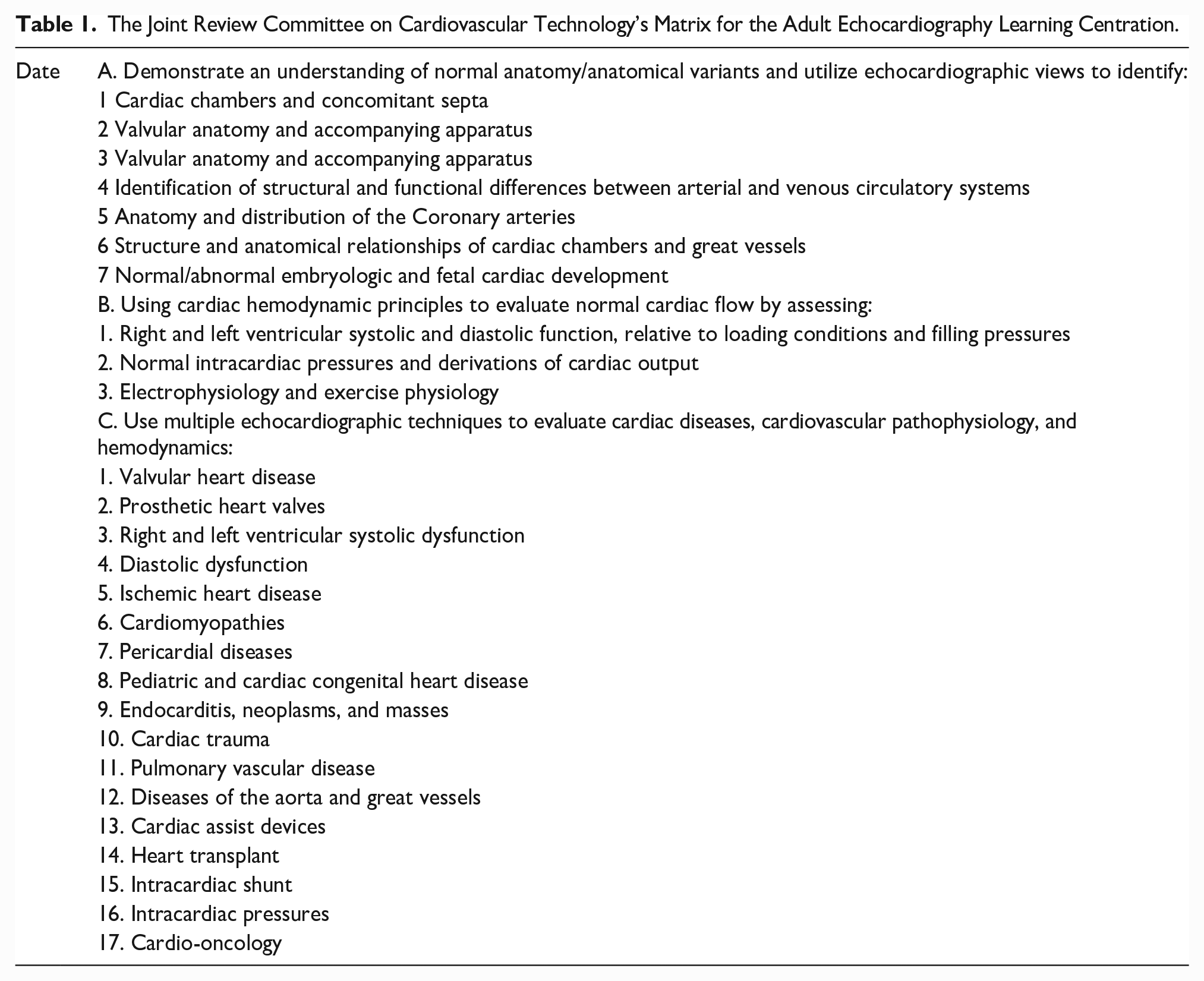
Cardiac sonographers have the opportunity to take an active role in developing the student experience in echocardiography by encouraging their institutions to become clinical sites, for accredited cardiovascular programs. The hands-on instruction is critical for the emerging student to develop the skills and understanding necessary in echocardiography. The credentialed cardiac sonographer serves as a mentor for the student throughout their internship in the clinical laboratory. Documentation of student experience, problem-solving ability, and mastery of skills and knowledge should be documented. The overall program volume of procedures should be representative of the wide range of cardiac procedures. The JRC CVT has constructed a matrix for the Adult Echocardiography learning centration (see Table 1). 8
The Joint Review Committee on Cardiovascular Technology’s Matrix for the Adult Echocardiography Learning Centration.
Becoming a clinical instructor for a well-organized and motivated accredited program can be very rewarding. Mitchell states the advantage of becoming a clinical site is that it provides change to the clinical routine and challenges sonographers to become better communicators to teach echocardiography concepts to a variety of students with different learning styles.
9
In doing so, one can re-evaluate an understanding of the sonographer’s role in the health care team, and how important the work is to try and answer the clinical question of the patient’s problem. The mentor may instill a positive attitude of why it is important to tailor the examination, and how to go about doing such.
The clinical instructors may obtain continuing educational credits through the Society for Diagnostic Medical Sonography (SDMS) for their clinical instruction time with the student.
It is advantageous for the clinical site to have the same student for a minimum of 6 to 12 months to provide adequate experience in all areas of echocardiography. This enables the student to become familiar with the protocols necessary to produce quality echocardiograms, as well as understanding the institution’s computer process and policies. In the long run, being a clinical site may produce potential coworkers for recruitment, within the echocardiography lab. Having participated in their education can reduce the orientation time period because they are familiar with the institution’s protocols, billing, and charting. 9
Cardiac Sonography Credentials
Credentialing in echocardiography demonstrates to the patients, health care professionals, and employers of the medical facilities that the cardiac sonographer is a dedicated professional, in the field of sonography. The benefits of credentialing are that it represents the highest standard in the field, increases career opportunities, and provides a commitment to patient care and safety. There are two widely recognized organizations that provide credentialing in echocardiography as discussed below.
American Registry of Diagnostic Medical Sonography
The American Registry of Diagnostic Medical Sonography (ARDMS) administers multiple specific examinations and awards credentials in four specialty areas of ultrasound: Registered Diagnostic Medical Sonographer (RDMS), Registered Diagnostic Cardiac Sonographer (RDCS), Registered Vascular Sonographer (RVT), and Registered Musculoskeletal Sonographer (RMSKS). More than 100 000 credentials have been awarded to medical professionals worldwide. 10
To obtain the RDCS credential, the applicant must meet the specific examination prerequisites and pass the physics and a corresponding specialty examination within five years. There are three specific registries for the cardiac sonographer: Adult Echo (AE), Pediatric Echo (PE), and Fetal Echo (FE). The echocardiography examinations test the requisite echocardiographic knowledge, skills, and abilities essential to sonography professionals. Once credentialed, the cardiac sonographer must obtain a minimum of 30 continuing education units every three years.
Cardiovascular Credentialing International
Cardiovascular Credentialing International (CCI) administers multiple specific examinations and awards credentials in nine specialty fields of cardiovascular technology, five of them being specific to ultrasound: Registered Cardiac Sonographer (RCS), Registered Congenital Cardiac Sonographer (RCCS), Registered Phlebology Sonographer (RPhS), Registered Vascular Sonographer (RVS), and Advanced Cardiac Sonographer (ACS). More than 27 000 credentials have been awarded to medical professionals worldwide (see Table 2). 11
Credentialing Statistics for Cardiovascular Sonography.

Abbreviations: ACS, Advanced Cardiac Sonographer; AE, Adult Echo; ARDMS, American Registry of Diagnostic Medical Sonography; CCI, Cardiovascular Credentialing International; FE, Fetal Echo; PE, Pediatric Echo; RCS, Registered Cardiac Sonographer; RCCS, Registered Congenital Cardiac Sonographer; RDCS, Registered Diagnostic Cardiac Sonographer.
There are three specific registry examinations for individuals in echocardiography: RCS, RCCS, and ACS. To obtain any of these credentials, the applicant must meet the specific examination prerequisites. 11 The echocardiography examinations test the requisite echocardiographic knowledge, skills, and abilities essential to sonography professionals. The most recently created registry is the Advanced Cardiac Sonographer. This examination is designed to build a career pathway for sonographers who practice at an advanced level in the echocardiography laboratory. Once credentialed, the cardiac sonographer must obtain a minimum of 36 continuing education units every three years. 11
ASE Recommended Standards for an Echocardiography Training Environment
The ASE recommends that cardiac sonography students consider entering programs that have been awarded accreditation by the CAAHEP, JRC-CVT, or JRC-DMS. 1 Such an environment should contain
a broad spectrum of cardiovascular medicine to provide the full breath of cardiovascular diagnostic procedures;
comprehensive patient evaluation and care;
a patient population that encompasses the full disease spectrum, from neonatal cardiovascular abnormalities to cardiac abnormalities of the elderly and includes patients who present with a variety of other medical and pediatric illnesses that may or may not influence cardiovascular dynamics;
a variety of echo imaging modalities for use in training, including M-mode, two-dimensional, three-dimensional, Doppler (continuous wave, pulsed wave, color flow, tissue velocity), strain, harmonics, and advanced automated imaging techniques;
competent practitioners in echocardiography, including physicians, credentialed cardiac sonographers, and specialists in the fields of ultrasound physics and instrumentation, anatomy, physiology, and pathology;
an echocardiography laboratory that performs and interprets a minimum of 100 echocardiograms per month.
Transthoracic Echocardiography
The cardiac sonographer must have a broad understanding of cardiovascular disease, noncardiac illnesses that complicate cardiac pathology, and pathophysiologic findings in the adult population. A broad understanding of the manifestations of congenital heart disease in the adult population is also important. The sonographer must have the ability to adapt the transthoracic echocardiography (TTE) examination to optimize imaging when body habitus and/or immobility present technical limitations. The sonographer must also have an understanding of the expected outcomes and potential complications of surgical and nonsurgical cardiac interventions and know the manner in which each affects the anatomy and physiology. 1
In 2011, the ASE stated that each sonographer should achieve and maintain minimum standards in education and credentialing, within 2 years of the start of employment. This includes the initial education required to be eligible for credentialing exams and the continuing education required to ensure competency, maintain credentials, and become familiar with the latest technologies. For sonographers who perform pediatric or fetal echocardiography, the minimum standard includes more specialized credentials. Some sonographers may be required to have a work experience component prior to eligibility for credentialing exams, and so it is recognized that laboratories may employ some sonographers who may not yet have credentials. In this case, a credentialed sonographer should be immediately available to provide supervision.
12
Stress Echocardiography
The cardiac sonographer should have extensive experience in the evaluation of patients with ischemic heart disease and a thorough understanding of segmental wall motion abnormalities to include the corresponding coronary artery perfusion regions. The ASE recommends training on at least 100 stress echo studies with supervision and maintenance of skills on greater than 15 studies per month. A minimum of 100 stress echo studies per year, per laboratory, is required. Training in stress echocardiography (SE) entails exposure to a mix of exercise and pharmacological stress testing, including patient selection, stress modality choice, stress test supervision, and integration of all diagnostic information.
Ultrasound Enhancing Contrast Agents
Ultrasound Enhancing Contrast Agents (UECAs) consist of intravenous (IV) injection of microbubble agents to enhance detection of blood flow within the cardiac chambers and thus improve the definition of cardiac target information, such as the endocardial borders or intracardiac masses. Appropriate training should be obtained to understand UECA administration and technical optimization tips. The Society of Diagnostic Medical Sonographers (SDMS) and the ASE support the sonographer performance of IV insertion and administration of UECAs with proper training and competencies. Some sonography training programs now include IV insertion training into their curriculum.
Transesophageal Echocardiography
The role of the cardiac sonographer in the performance of the transesophageal echocardiography (TEE) examination is usually limited to manipulation of the controls on the ultrasonography system. An understanding of the standard views, the order in which they are obtained, and the potential complications of the examination are important aspects of the sonographer’s participation in the procedure. 1
Three-Dimensional Echocardiography
The sonographer should attend a formal training course in acquisition and postprocessing of three-dimensional echocardiography (3DE) data sets. The sonographer should also obtain mentored experience in the acquisition and postprocessing of at least 50 3DE volumes (both TTE and TEE) of various cardiac pathologies. Knowledge of the cardiac views feasible by 3DE, including en face views of valves and septa, is critical in 3DE understanding.
Conclusion
In summary, cardiac sonography is a challenging and rewarding career that demands individual initiative, clinical judgment, critical thinking, and a commitment to ongoing professional development in the rapidly evolving field of echocardiography. A student planning a career in cardiac sonography must take the opportunity to find the best accredited program that offers an extensive clinical affiliate hands-on training in order to gain a strong comprehensive experience.
The goal of the cardiac sonography student should be to apply to a CAAHEP-accredited program and use the knowledge obtained in the program to actively participate in an Intersocietal Accreditation Commission (IAC) echocardiography–accredited clinical site with hands-on instruction provided by the credentialed clinical site sonographers. Completion of the program should lead to successful credentialing in echocardiography through the ARDMS or CCI.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
