Abstract
Patient satisfaction is important to health care facilities because a satisfied customer tends to return for additional services. Identifying the characteristics that increase patient satisfaction can help facilities improve their process. Few studies have directly evaluated imaging departments, but the literature from other health care specialties can be applied when the environment is similar. Having a pleasant waiting experience has shown to have a positive impact on patients’ overall satisfaction and perceived quality of care. Factors that have been linked to improved patient satisfaction include decreased wait time, decreased perceived length of wait time, and increased communication through written information or increased face-to-face time with a provider.
To provide the best services to patients, quality assessment is an ongoing activity. When patients are satisfied with their care, they are more likely to continue using a facility for future services. 1 Factors that affect patient satisfaction ratings include length of wait time, perceived wait time, and communication between the patient and the provider. Studies indicate that extensive wait times can introduce patients to added emotional and psychological stress. 2 Negative consequences can occur as patients choose to avoid waiting room delays by not scheduling initial appointments or follow-up visits. 3 An awareness of which factors affect patient satisfaction is important. Current literature regarding patient satisfaction focuses on interaction with physicians and clinics, but little is written about interaction with sonographers or within imaging departments. This review attempts to assess literature that can apply to an imaging department to increase patient satisfaction and perceived quality of care, thereby improving patient follow-up surveys and rates of return to the facility.
Variables Influencing Patient Satisfaction
Several factors influence how patients recall their satisfaction related to wait time when being seen by a health care provider. Maister developed a formula, S = P – E, to help understand how satisfaction can be calculated. 4 In this equation, S is satisfaction, P is perception, and E is expectation. 4 Perception is how an individual processes and understands sensory information. If a patient enters the environment with a high perception of what should happen, then small amounts of unmet expectation will not decrease the overall satisfaction; however, if a patient enters the environment with low perception, then even a small amount of unmet expectation can significantly affect the patient’s satisfaction. 4 Another way to think of patient satisfaction is the total sum of met versus unmet expectations.5,6 Regardless of how one computes expectations, being cognizant of patient expectations and trying to modify those expectations, when appropriate, can influence patient satisfaction levels. Table 1 provides a summary of research studies that examined factors linked to patient satisfaction.
Most Common Factors Influencing Patient Satisfaction in Regard to Wait Times.
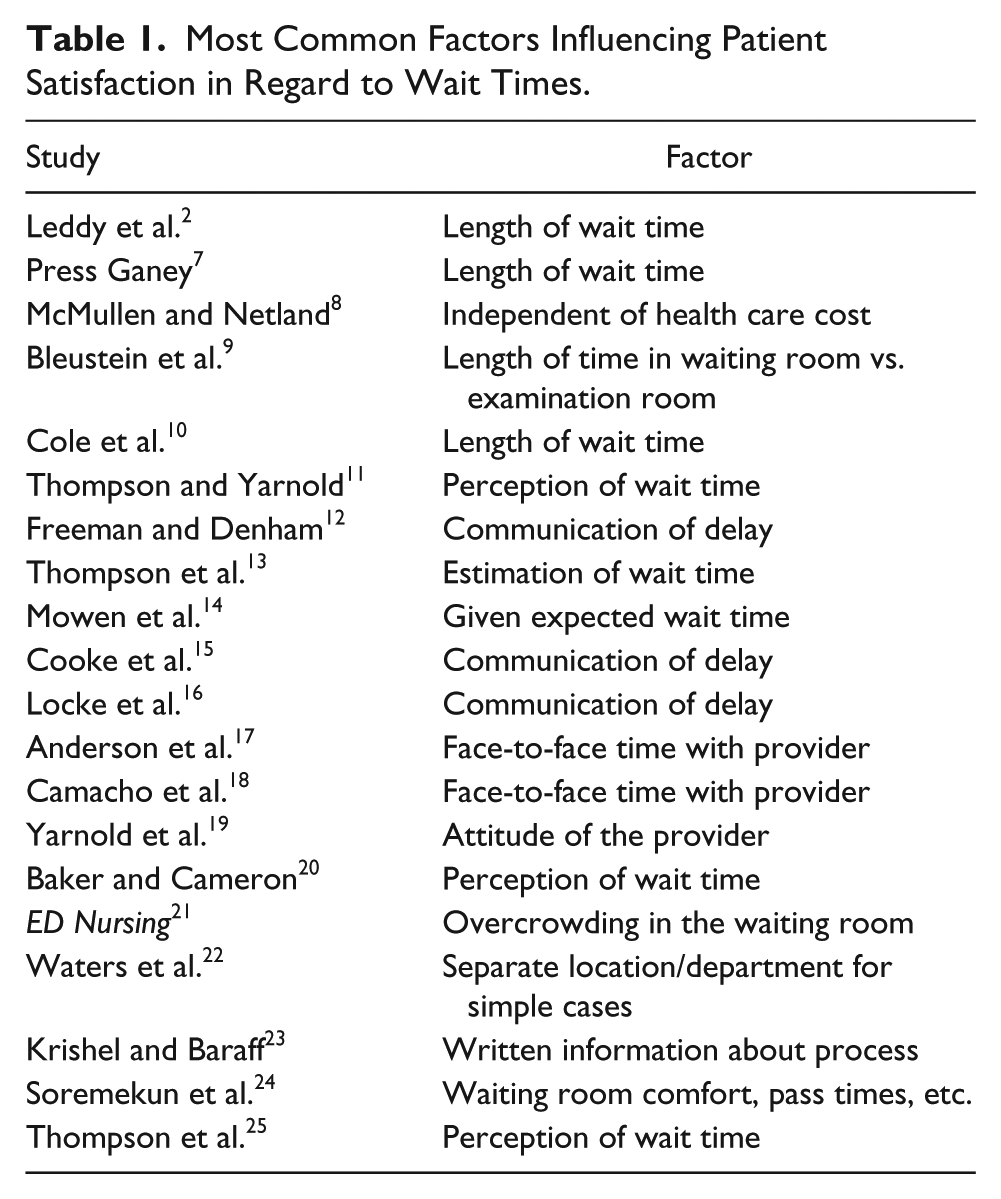

Length of Wait Times Influencing Satisfaction
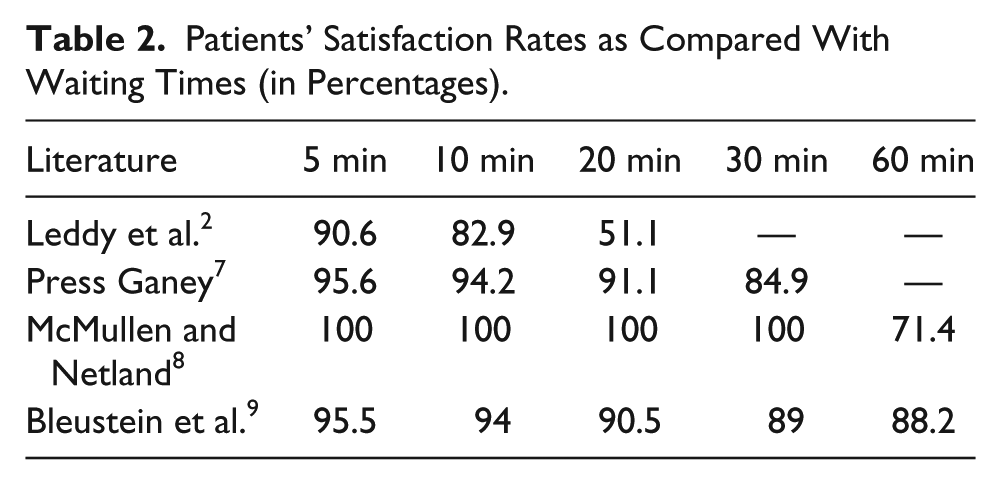
Increased wait times correlate to decreased patient satisfaction scores and decreased perceived quality of care. Leddy et al. noted that patients who waited ≤5 minutes rated their satisfaction at 90.6%, but satisfaction fell to 51.1% for those who waited ≥20 minutes. 2 Likewise, a Press Ganey report 7 compiled 2 million patient surveys, documenting that those who waited <15 minutes had a satisfaction score of 94.3%, whereas the patients who waited >60 minutes had satisfaction scores of 86.1%. McMullen and Netland used a Likert scale from 1 to 7, with 7 being most satisfied, to ask patients to self-identify how satisfied they were with their wait times in an outpatient ambulatory setting where some patients were seen for free. 8 Patients whose wait time was 30 minutes gave a satisfaction score of 7 (100%), whereas it was 5 (71.4%) when the wait time was doubled, regardless of the cost of care. 8 Patients who received free care were just as dissatisfied with an increased wait time as those without financial assistance. 8
The expected wait time length may be more of a factor than the actual wait time. Bleustein et al. reported patient satisfaction using a Likert scale of 1 to 5, with 5 being the highest. 9 A 20-minute wait time was associated with a satisfaction score of 4.51 (90.5%), and a 60-minute wait time had a score of 4.41 (88.2%). 9 This study teased out how time spent in the waiting room and time spent waiting in the examination room correlated. 9 The satisfaction scores decreased quicker when patients waited in the examination room versus the main waiting room. 9 This may be due to the expectation that once a patient is in an examination room, the wait time should be shorter, or it might be that there are not as many activities in there to occupy one’s time. This corresponds with other findings indicating that patients whose wait time was shorter than expected were more likely to recommend a facility to others10,11 and perceived a higher quality of care.9,12
Another distinct factor is the perceived wait time. When the patient perceives a long wait time, the actual wait time becomes irrelevant. 13 Thompson et al. noted that 22% to 36% of patients reported accurate wait times, leaving the majority to overestimate them. 11 An awareness of factors affecting the perception of wait times is important. Maister elaborated on factors that could cause wait times to seem longer, including unoccupied time, anxiety while waiting, and uncertain wait times. 4 Staff communication is a factor that contributes to perceived wait time and patient satisfaction. Mowen et al. found that patients waiting in an emergency department were more satisfied when given an expected wait time. 14 Cooke et al. identified that 21% of emergency department patients thought that there should be “check-in” or “reporting” every 15 minutes while in the waiting area, whereas 55% said every 30 minutes and 20% said every 60 minutes. 15 Locke et al. concluded that the most important factor regarding wait time is being informed of a delay. 16 Communicating delays was shown to be 60% specific, with a positive predictive value of 65% regarding satisfaction. 16 This finding implies that communication alone affects the satisfaction of the patient regardless of wait time length. 16
Provider Interaction Influencing Satisfaction
Patient satisfaction is linked to the amount of time spent with the provider and how the patient perceives the quality of information given to them. Patients have been found to be most satisfied when they experienced decreased wait time accompanied by increased interaction with the provider. 17 Camacho et al. assessed patients who waited <75 minutes with survey questions on a scale of 0 to 10, with 10 being the best care. 18 Increased wait time combined with decreased provider interaction resulted in decreased satisfaction scores. 18 Patients who waited 40 minutes and spent 0 to 5 minutes with the provider had a mean satisfaction score of 7.75 (78%), whereas patients who waited 10 minutes and spent ≥10 minutes with the physician had a mean score of 9.56 (95.6%). 18
Do not negate the importance of being kind and friendly while interacting with the patient. Yarnold et al. linked nurse attitudes and perceived quality of care as the best indicator of satisfaction. 19 The perceived quality of care appears unrelated to the type of information being conveyed. 11 Any positive interaction with nurses and physicians has been noted to improve satisfaction scores from patients. 11
Comfort Level While Waiting Influencing Satisfaction
When patients rate the waiting room as “comfortable and pleasant,” they are willing to wait longer. 20 Medical practice waiting rooms rated as “very poor” by patients who waited 0 to 5 minutes yielded a satisfaction level of 41.3%, whereas waiting periods of 0 to 5 minutes in a “very good” waiting room showed a 96.3% satisfaction score. 2 This same trend was seen in outpatient testing and treatment facilities. 2 Patients waiting 0 to 3 minutes who rated the comfort of the waiting room as “very poor” showed satisfaction of 58.3%, while “very good” waiting rooms had a 96.7% satisfaction rating for the same time frame. 2
Overcrowded waiting rooms can cause patient anxiety, which may negatively affect the perception of wait time. When surveyed, 86% of emergency department nurses stated that they witnessed violence over the course of 3 years when the waiting room was overcrowded. 21 They speculated that the cause was related to increased tension from the overcrowding. 21 To address congested waiting rooms, some facilities have restructured the way that they provide care. One chemotherapy clinic established a short-term treatment area to increase patient satisfaction. 22 Patients with simpler treatments are seen in this clinic, which has shortened wait times because the more complicated cases, which require unexpected delays, are not on the schedule. Patients reported less anxiety and frustration, and the facility reported increased patient satisfaction scores. 22
Ancillary Information Influencing Satisfaction
Krishel and Baraff discovered that when patients were provided written information describing the process of an emergency department, there was a greater degree of satisfaction due to knowing what was going to happen next. 23 Patients who perceived that they received good information at arrival were most satisfied. 23 Likewise, Thompson et al. found that patients who received information, explanations, or instructions were more satisfied with the visit. 11
Discussion
Patient wait times can be described through different parameters. Increased patient satisfaction scores associated with decreased wait times have been well documented (Table 2).3,7–9 Research has noted that longer wait times can actually decrease patients’ perceptions of the quality of care.9,12 Additionally, perceived wait time has been shown to be more predictive of satisfaction than actual wait time. 13 Only 22% of patients are accurate in their perception of wait time, with the majority overestimating it. 11 Having continual interactions, communicating when a delay has occurred, and estimating how long that delay may last can increase satisfaction.4,24 Providing patients with an expected wait time has been shown to be beneficial in easing patient uncertainty.15,16
Patients’ Satisfaction Rates as Compared With Waiting Times (in Percentages).
Because of imaging department dynamics, it is difficult to increase providers’ face-to-face time with patients, but being attentive and portraying oneself as competent and caring may improve satisfaction. 25 Further research showing how behavior may be modified to improve patient satisfaction scores would be beneficial. Providing the patient with additional information has shown to be effective, but what form the communication should take (written, verbal, digital), how often it should be given, and at what time in the process it should be given have not been well documented.11,23
Making the waiting room comfortable improves patients’ willingness to wait.2,20 Having a greeter welcome patients upon arrival to provide early interaction and establish a rapport creates a more positive atmosphere. 24 Perceptions are generally more positive when patients can wait in a group as compared with waiting in isolation. 4 Not calling the patient back until his or her procedure is ready to begin may improve the perceived wait time because remaining with the larger group allows for more activities versus being in an isolated imaging room.
Conclusion
Patients spend a great amount of time waiting to be seen for medical imaging services. Using research data from other medical specialties may help imaging departments pinpoint areas of improvement to increase patient satisfaction scores. The evidence shows that managing patients’ expectations of wait time, along with demonstrating good communication and positive attitudes, improves overall satisfaction. This is not always easy to accomplish given the dynamics of service delivery in an imaging department. In an increasingly competitive health care environment, having a plan to interact with and care for patients when faced with extended wait times can help imaging departments manage the situation. Even small adjustments may make a large impact to keep overall satisfaction high.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
