Abstract
A case of skeletal dysplasia was sonographically evaluated in the fetus of a 21-year-old patient. The diagnosis of osteogenesis imperfecta type II was suggested during a routine morphological examination at 17 weeks’ gestation, based on visualization of rhizomelia, bowed long bones, and decreased thoracic cavity size. Sonographically, this dysplasia was well visualized and contributed to a final diagnosis, highlighting the diagnostic value of prenatal sonography. The use of routine sonographic examinations continues to prove crucial for early detection of fetal abnormalities such as skeletal dysplasias.
Skeletal dysplasias are rare abnormal developments involving the growth and formation of bone and connective tissues. These conditions can affect any area of the musculoskeletal system and range from minor to lethal. The cause of these conditions is thought to be genetic factors such as the transmission or mutations of genes. Osteogenesis imperfecta (OI) is a rare subgroup of these disorders, affecting approximately 1 in 12,000 births. 1 Four groups of OI (types I–IV) can share similarities in appearance but have critical differences in genetic qualities that assist in diagnosis. Sonography is an excellent diagnostic tool in visualizing these conditions prenatally and is often the first modality to discover these conditions.
Case Report
A 21-year-old G1P0 Hispanic woman presented for routine morphologic evaluation at 20 weeks, 2 days’ gestation based on the last menstrual period (LMP). A previous dating sonogram was performed at 7 weeks, 3 days and showed an intrauterine pregnancy (IUP) with no visible abnormalities. The morphologic examination demonstrated a single IUP in the breech position. The heart rate and cervical length both measured within normal limits. Intracranial anatomy appeared normal. Biparietal diameter measured 42 mm (18 weeks, 5 days), and head circumference measured 162 mm (19 weeks, 0 days). Transcerebellar diameter measured 17.8 mm (18 weeks, 4 days). The spine, umbilical cord, and nose/lips were unremarkable. Cardiac anatomy, diaphragm, stomach, kidneys, bladder, and cord insertion were also within normal limits. Abdomen circumference measured 126 mm (18 weeks, 2 days). Thoracic circumference measured 11.09 cm, which is the 24th percentile for thoracic circumference based on the patient’s LMP (Figure 1). 2 A shortening of the upper (Figures 2 and 3) and lower (Figures 4 and 5) limbs was noted. Femur length measured 12.9 mm (13 weeks, 6 days), which demonstrated significant discrepancy for the estimated gestational age. The femurs exhibited a classic “telephone receiver” sign. Bowing was identified in all limbs. The hands and feet were not well visualized. In addition to these abnormalities, the thoracic cavity size was markedly decreased compared to the abdominal cavity size (Figure 6). Sex was reported postexamination by the scanning sonographer as female.
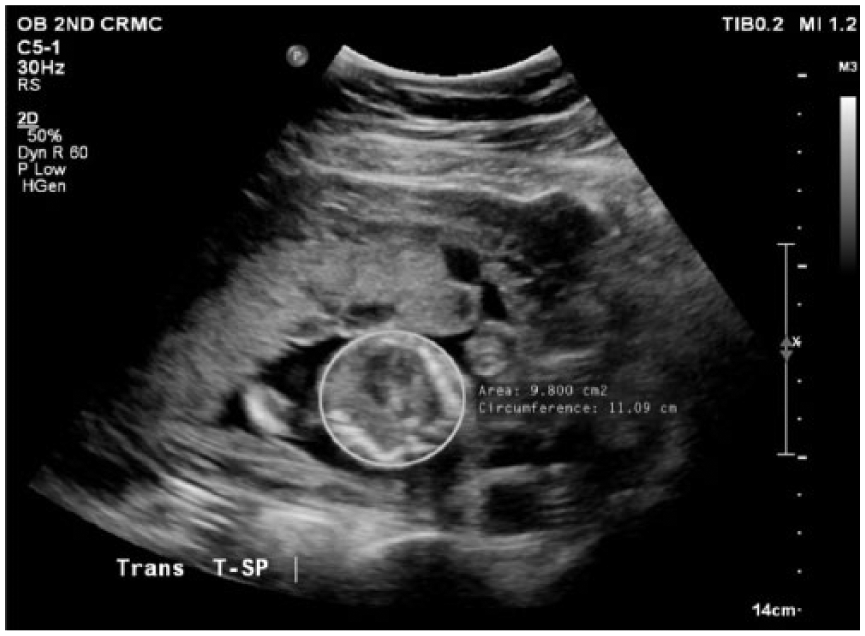
Gray-scale cross-sectional sonogram showing measurement of the thoracic cavity, small for gestational age.
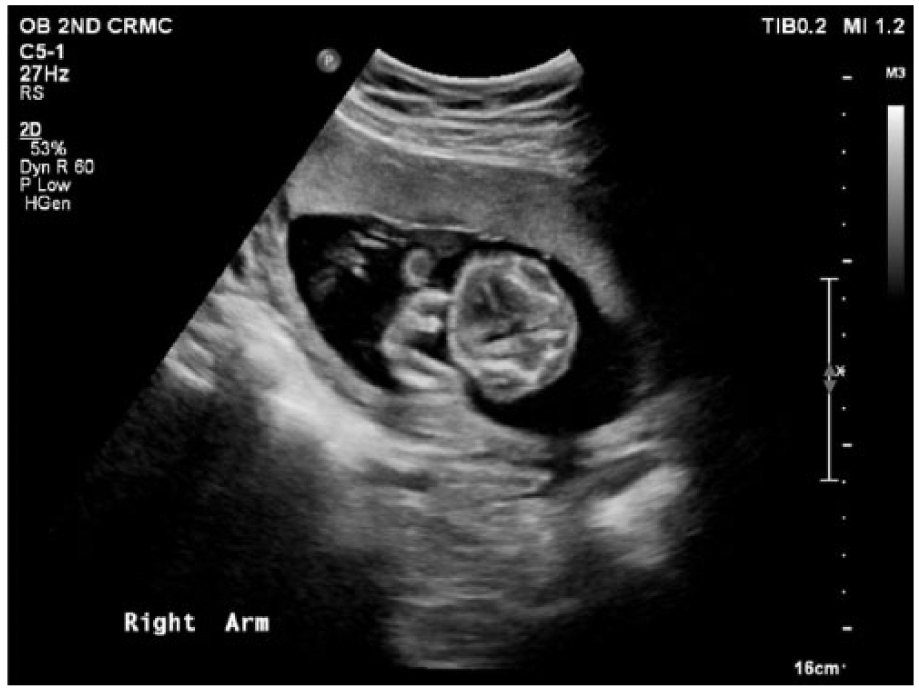
Gray-scale sonogram showing rhizomelia in the right arm.
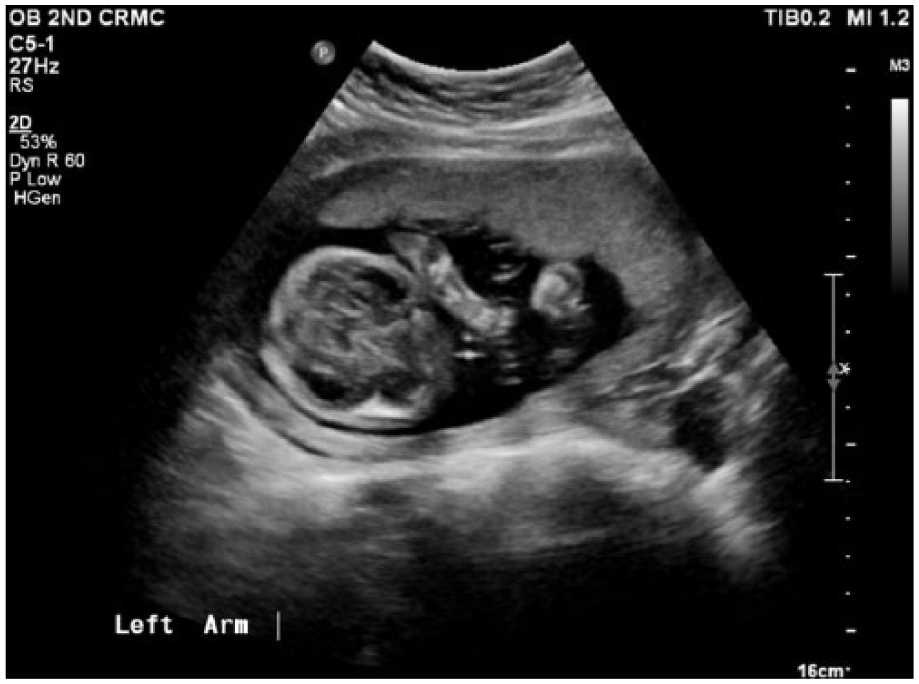
Gray-scale sonogram showing similar rhizomelia in the left arm.
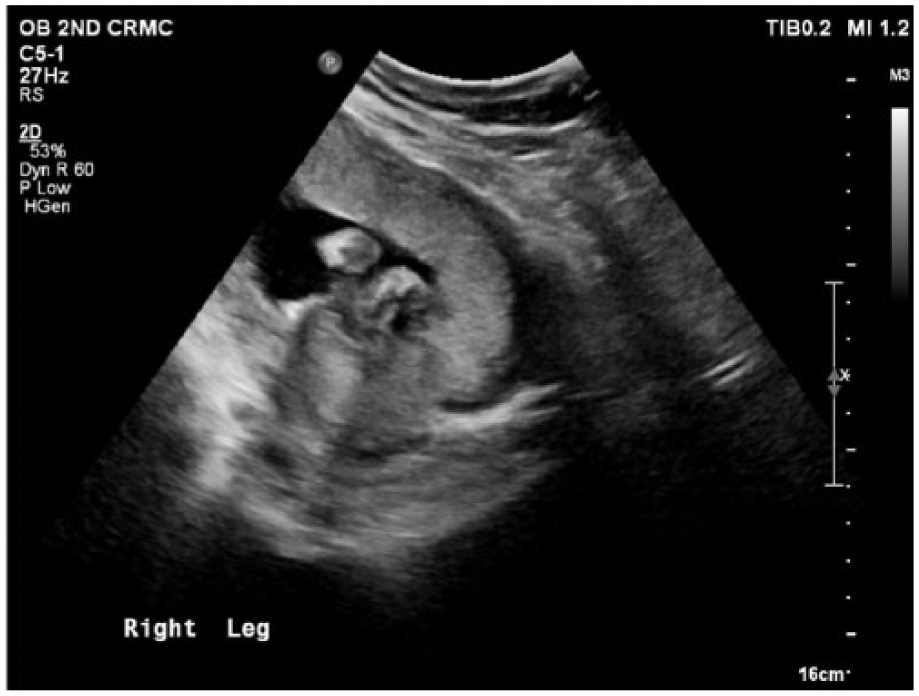
Gray-scale sonogram showing rhizomelia in the right leg.
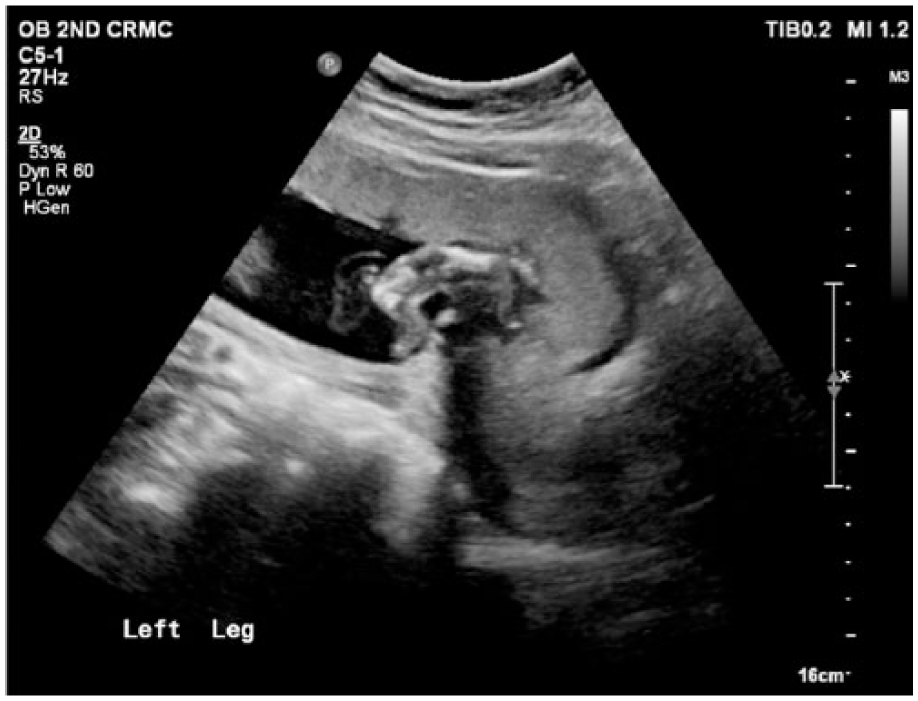
Gray-scale sonogram showing similar rhizomelia in the left leg.
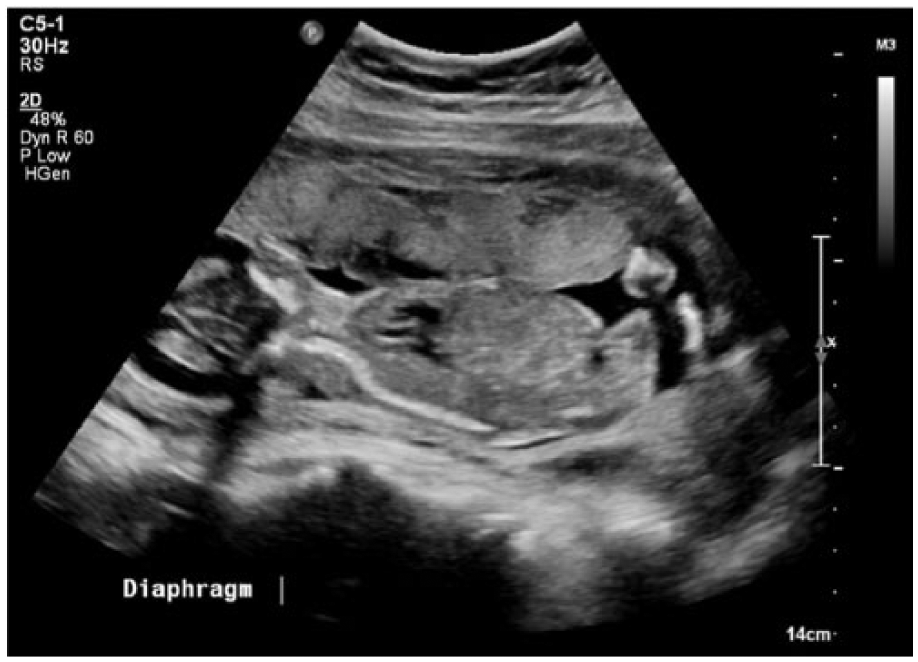
Gray-scale sonogram showing significantly decreased thoracic size compared to abdominal size.
Based on the sonographic findings, an evaluation at a high-risk fetal medicine facility combined with a detailed morphologic examination and genetic testing was recommended. Genetic testing at an outside facility confirmed the diagnosis of osteogenesis imperfecta type II. Differential diagnoses for OI type II include thanatophoric dysplasia, achondrogenesis, and congenital hypophosphatasia. No additional follow-up information was available.
Discussion
Skeletal dysplasias encompass a group of low-prevalence disorders of the musculoskeletal system. They occur in approximately 3.2 in 10,000 live births. 3 Of these dysplasias, thanatophoric dysplasia (TD) is the most common lethal type, and achondrogenesis is the most common nonlethal type. 4 OI is the second most common lethal type, with roughly 22% of all skeletal dysplasia diagnoses. 4 OI is classified into four subgroups based on clinical, genetic, and other diagnostic findings.
OI type I is caused by a decrease in collagen production and is considered the second mildest form of this condition. 5 Diagnostic findings can include femoral bowing in utero and fractures after birth. Other common findings of OI type I are small stature, scoliosis, and multiple fractures before puberty. Hearing loss is also prevalent with OI type I. 6 The rate of occurrence of OI type I is 45% to 50% of all OI cases. 7 The prognosis for OI type I is good, with most patients exhibiting a normal appearance. 8 OI type II is the most severe form of this condition, with several sonographic characteristics that distinguish OI type II from other types of the condition. 9 Rib fractures due to concave ribs, reduced long bone echogenicity, and angulated appearance of the long bones due to fractures are classic signs of OI type II. Another notable characteristic of OI type II is the bell-shaped appearance of the thorax (Figure 6). 9 The prevalence of OI type II is approximately 10% of all cases. 7 The prognosis for OI type II is very poor, with most neonates dying shortly after birth because of respiratory failure secondary to rib fractures. 10 OI type III is less severe than OI type II but can present with similar findings such as limb bowing and bone fractures. 8 OI type III can also lead to abnormal bone development in adolescence. 10 The typical appearances of OI type III include low birth weight, severe physical disability, and long bone deformity. 7 The prevalence of OI type III is approximately 20% of all OI cases. 7
OI type IV is known as moderately severe OI and is a combination of OI types I and III. OI type IV does not present until later in the life of those affected. Because of this delay, it is not likely to be detected in utero. 11 The prevalence of OI type IV is about 20% of all cases of OI. 7 The typical appearance of OI type IV includes long bone deformity, spinal deformity, and dentinogenesis imperfecta (DI). 12 DI is a defect of the dentin in the teeth and is commonly associated with OI types I, III, and IV. 7 The prevalence of this condition in patients who have been diagnosed with OI is about 50%. 12 Additional types of OI exist and are identified in OI patients with variances in their presentations. 6 These types are rare and present similarly to OI types I to IV but with distinct variations. 6
Each subtype of osteogenesis imperfecta has a different method of genetic inheritance. Most occur through an autosomal dominant or recessive pattern. OI types I and IV are inherited in an autosomal dominant pattern, while type II is inherited in an autosomal recessive pattern. 11 OI type III can be inherited in either an autosomal dominant or autosomal recessive pattern. 11 Rhizomelia, as seen in this case (Figures 1–4), is possible in skeletal dysplasias with an autosomal recessive pattern. 11 Genetic panels allow for noninvasive gathering of information for differentiation of similar conditions.
While the prognosis for this case of type II OI is very poor, the use of prenatal sonography in accurately diagnosing the skeletal dysplasia allows for possible treatment. The treatment for OI depends on the type present. Type II is usually fatal at birth, while types I, III, and IV are often survivable. There are several methods for treatment of OI, ranging from pharmaceutical to surgical options. In pharmaceutical treatment, the most common method is the use of bisphosphonates (BPs). This type of therapy prevents the loss of bone mass through inhibition of bone digestion by osteoclasts. 13 This method can be administered orally or intravenously. 14 Another common treatment is surgical intervention. The use of metal rods to splint long bones is often used to manage deformities and repeated fractures. 7 These rods are commonly telescopic to allow for growth throughout development. The second common surgical intervention is spinal fusion. This treatment allows for the management of scoliosis, a common finding in patients with OI. 7 The use of BP therapy and surgical intervention can increase the chance of a better outcome for patients with OI.
The importance of sonography in the diagnosis of this case cannot be overstated. As a first line of evaluation, prenatal sonography discovered the abnormalities in this fetus. The abilities of this technology allowed for rapid diagnosis of the skeletal dysplasia and provided diagnostic information that allowed differentiation between several different types of skeletal dysplasias. In combination with laboratory testing, a final diagnosis of OI type II was reached. The use of sonography in cases like these can also allow expecting parents to prepare for the possibility of poor outcomes that are associated with the more severe abnormalities. 15
Conclusion
The use of prenatal sonography in this case provided significant insight into the anatomical and physiological variants present in the fetus. By detailed sonographic imaging of the fetal skeleton, a diagnosis was identified and differentiated from several other similar diagnoses. This study highlights the importance of sonography in the identification and diagnosis of fetal skeletal abnormalities.
Footnotes
Acknowledgements
The authors thank Karen Hackman, BHS, RDMS, Lesa Langlotz, BHS, RDMS, RVT, and Sharlette Anderson, MHS, RDMS, RVT, RDCS, for their assistance and guidance in preparation of this study.
Declaration of Conflicting Interests
The authors declares no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
