Abstract
Turner syndrome is the most common sex chromosome abnormality in female fetuses, in which all or part of one of the X chromosomes is absent or has some other abnormality. The syndrome has a number of characteristic sonographic findings such as diffuse fetal edema, cystic hygroma with septations, renal and cardiac anomalies, increased nuchal translucency, and growth retardation. A case is presented of Turner syndrome diagnosed by cytogenic testing after a number of anatomic anomalies, including diffuse edema, cystic hygroma and growth retardation, were found by sonography.
Keywords
Introduction
Turner syndrome is the most common sex chromosome abnormality in female fetuses, in which all or part of one of the X chromosomes is absent or has some other abnormality; it may affect all or only some cells of the fetus. It is named after Henry Turner, who first described the syndrome in 1938. 1 Turner syndrome affects 1 in 2000 live births, but over 90% of Turner cases result in miscarriage, making its in utero incidence much higher.2,3 Fetuses with monosomy X, also known as Ullrich-Turner syndrome 45, X, 4 account for the majority of cases and are the cause of approximately 10% of all spontaneous abortions.5–8 The missing sex chromosome is more likely to be from paternal contribution, and unlike the common trisomies, there is no correlation with maternal age.5,6 The following case presents a pregnancy with many of the characteristic sonographic findings of Turner syndrome.
Case Report
A 28-year-old female presented to her obstetrician’s office for a routine check-up regarding a singleton pregnancy. The patient was G1P0 and 17 weeks gestational age as determined by last menstrual period. The obstetrician performed a sonogram on the patient in his office and noted fluid around the fetal liver. He sent the patient to a maternal fetal medicine practice for a complete anatomic survey of the fetus—fetal lie, presentation, environment, all anatomy, and complete measurements.
The patient was seen at the maternal fetal medicine practice at 17 weeks and 3 days gestation, and a comprehensive fetal detail sonogram was done using a Philips iU22 system (Philips Ultrasound, Bothel, WA) with a 4 MHz curvilinear array transducer. The sonogram showed a number of fetal abnormalities. The fetal heart rate was 172 beats per minute (bpm). Because of anatomic abnormalities, normal measurements of the head and abdomen could not be taken precisely. Based on the sonographic measurements, obtained as accurately as possible, the fetus was determined to be at 16 weeks and 1 day gestation, about 1 week and 2 days behind. The deepest vertical pocket of amniotic fluid measured 4.4 cm. The placenta appeared to be posterior, and the fetal gender was not well visualized due to the fetus being in the breech position. There was an extremely large septated cystic hygroma measuring 5.06 cm in anterior-posterior diameter (Figure 1). Massive generalized subcutaneous edema, bilateral pleural effusions, and abdominal ascites consistent with fetal hydrops were also noted (Figure 2). Severe edema of the scalp and limbs was seen (Figures 3 and 4). Pericardial effusion was also noted (Figure 5). The anatomic survey was limited due to the massive edema and distortion of the usual anatomic relationships, but based on sonographic measurements, there was a 1-week lag in long bone and head measurements. The patient had a negative antibody screen, and sonographic blood flow studies were within normal limits. The overall impression and diagnosis was nonimmune hydrops fetalis.
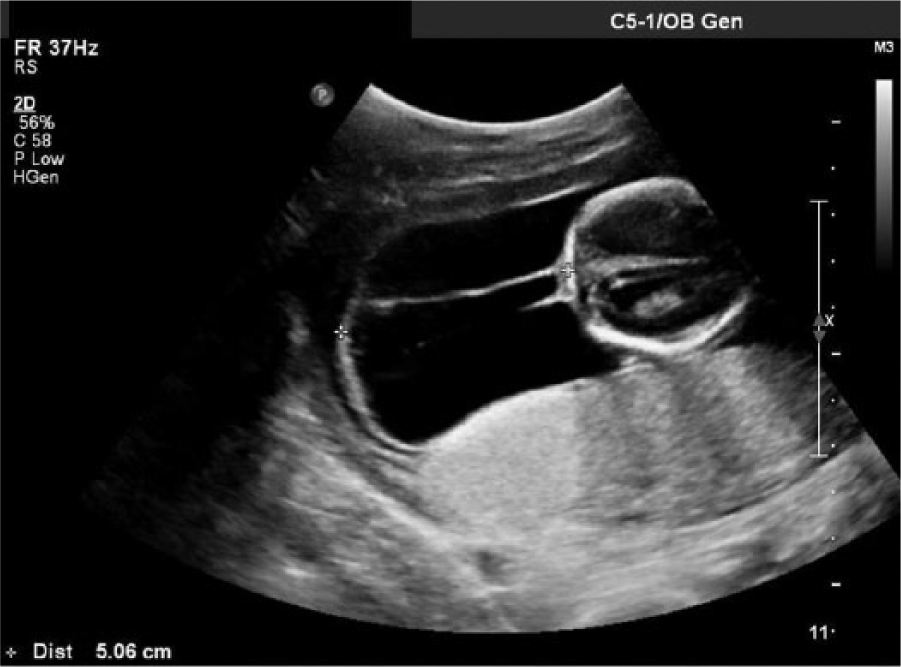
Cross-sectional gray scale fetal sonogram showing a 5.06 cm septated cystic hygroma.
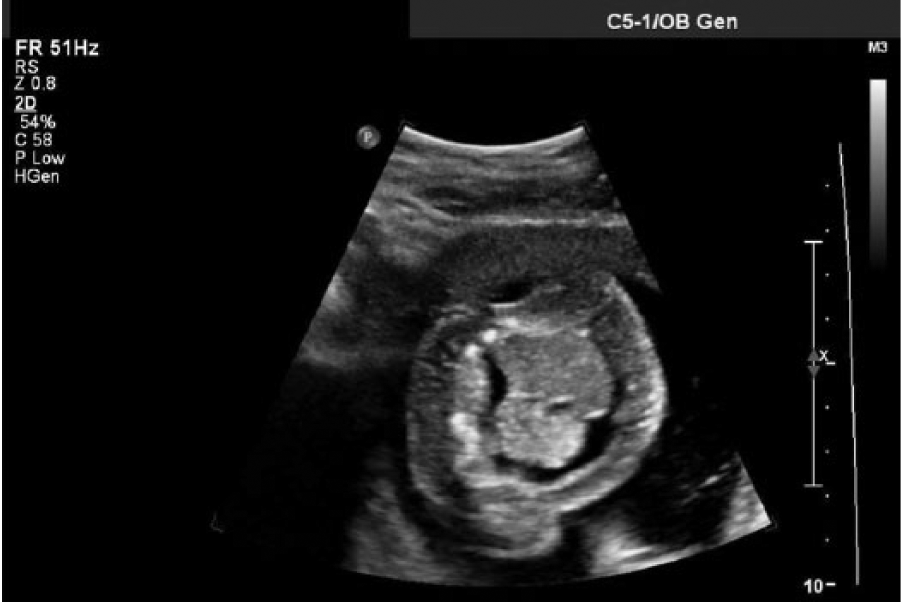
Cross-sectional gray scale midtrunk fetal sonogram showing pleural effusion and ascites.
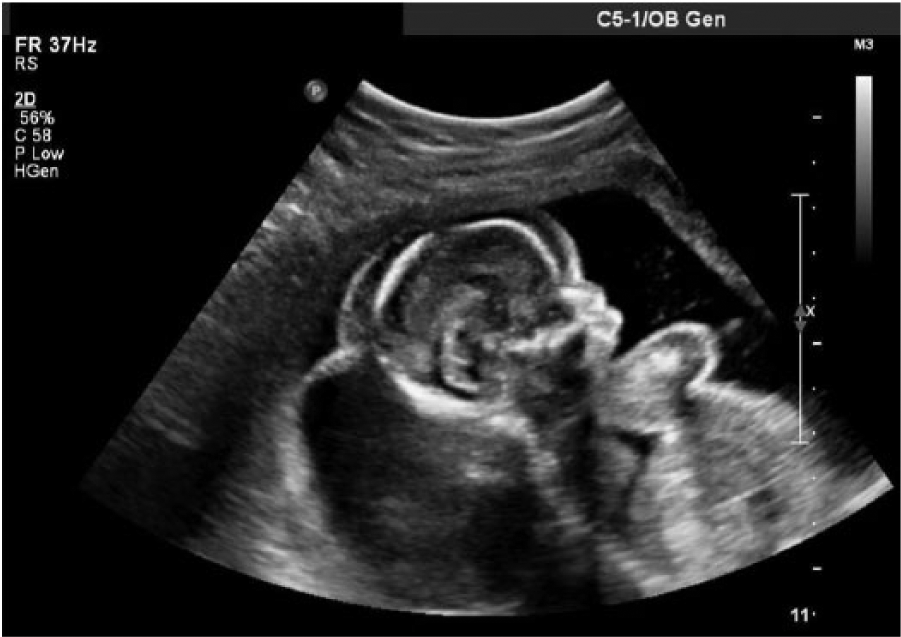
Sagittal gray scale fetal sonogram showing significant scalp edema.
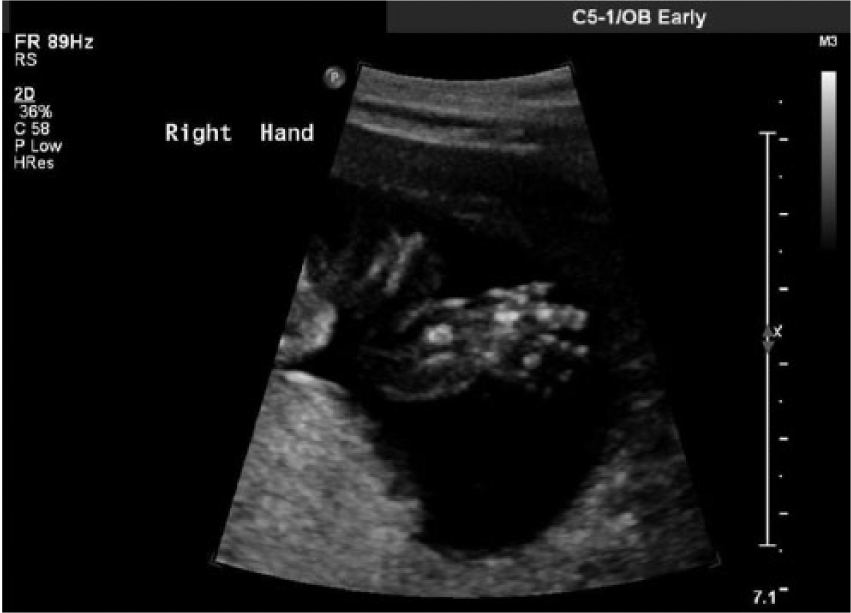
Gray-scale fetal sonogram showing edema of the right hand.
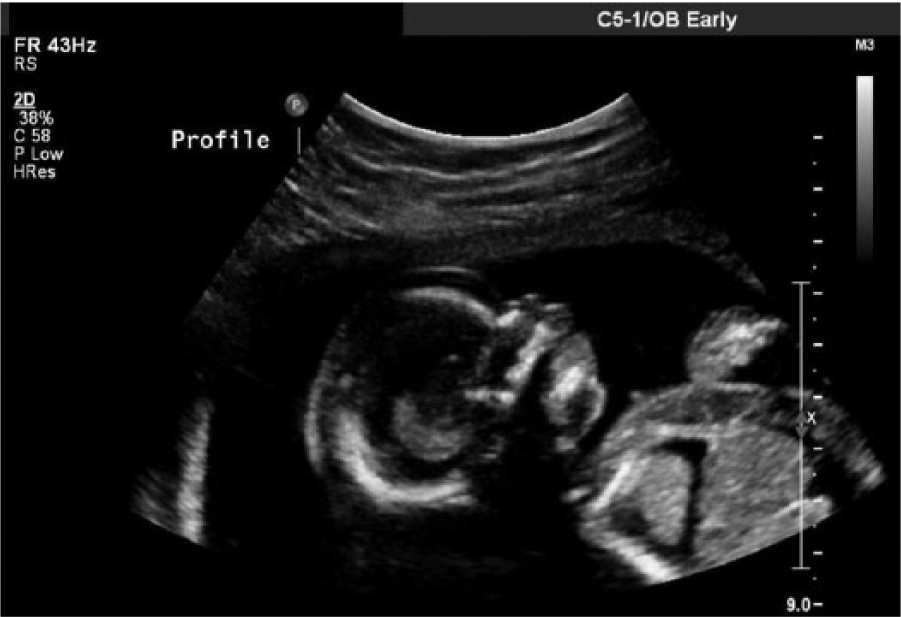
Sagittal gray-scale fetal sonogram showing pericardial effusion in addition to scalp edema.
The findings were explained to the patient and the patient elected to do a genetic ultrasound guided amniocentesis because of the multiple congenital anomalies seen on sonography. The amniocentesis was performed at 18 weeks and 1 day gestation and showed a 45, X–abnormal fetal karyotype. Cytogenic analysis revealed only 1 sex chromosome, the X chromosome (monosomy X), in each metaphase cell examined, consistent with the clinical diagnosis of Turner syndrome. The standard cytogenic methodology utilized in this analysis would not routinely detect subtle rearrangements or low-level mosaicism and cannot detect microdeletions.
Discussion
Turner syndrome is a chromosomal disorder that is characterized by the absence of part or all of a second sex chromosome in some or all cells. 2 There are two types of Turner syndrome—classic and mosaic. Classic Turner syndrome results in an entire X chromosome missing; mosaic Turner syndrome signifies that the abnormalities only occur in the X chromosome of some of the cells in the body. 2 Turner syndrome is usually not inherited because it occurs during a random event during the formation of reproductive cells in the affected person’s parents. 12
Classic sonographic findings of Turner syndrome include diffuse fetal edema, cystic hygroma with septations, renal and cardiac anomalies such as horseshoe kidney and coarctation of the aorta, nonimmune fetal hydrops, a short cervical spine, increased nuchal translucency, brachycephaly, hydramnios, and growth retardartion.2,5,9,10 While sonography is the best method to prenatally diagnose Turner syndrome, a genetic amniocentesis or chorionic villus sampling should be done to confirm the karyotype and determine a definitive diagnosis.2,9 Laboratory values associated with Turner syndrome include decreased serum alpha-feto protein (AFP) and low unconjugated estriol (uE3), with an elevated maternal beta human chorionic gonadotropin (hCG) and serum inhibin in the presence of nonimmune fetal hydrops; if hydrops is not present, beta hCG is decreased and serum inhibin is absent.11 –15
This case report presented with several markers associated with Turner syndrome including a septated cystic hygroma, limbs measuring a week behind, pleural effusion, scalp edema, edema of the arms and legs, pericardial effusion, and abdominal ascites. These markers indicated nonimmune fetal hydrops, but no chromosomal problems could be determined without an amniocentesis or chorionic villus sampling. Since chorionic villus sampling is best done prior to the twelfth week of gestation, the use of ultrasound guided amniocentesis was essential for a definitive diagnosis and treatment of the chromosomal abnormality. Prenatal diagnosis allowed for appropriate family education and counseling and proper treatment regarding this pregnancy.
Prenatal diagnosis of Turner syndrome can be highly variable depending on the degree of anomalies present and how early the syndrome is diagnosed. Turner syndrome is associated with a high rate of fetal loss, with an estimated greater than 90% of fetuses not surviving to term.2 –4,12 The loss or alteration of the X chromosome occurs randomly, usually due to a problem with the sperm or an egg. Family history has not been shown to be a risk factor, therefore it is unlikely that parents who have had a child with Turner syndrome will have another child with the disorder as well.3,12
The overall prognosis of Turner syndrome is variable and highly dependent on the associated anomalies and the severity of the anomalies. 2 A large majority of fetuses that develop Turner syndrome will abort in the second trimester of pregnancy. 12 If the anomalies are not diagnosed in utero or are not severe, a fetus can persist through pregnancy and be delivered alive and most of these children will have a long life expectancy. 2 If Turner syndrome is diagnosed during childhood, recommendations for extensive medical screening have been developed to search for related anomalies.11,16 Children who live with Turner syndrome will present with a variety of problems throughout their life; most of these children will have a short stature that will become evident by age 5.2,6,9 Standard recommended treatment based on clinical trials now includes the routine use of recombinant growth hormone.17,18 An early loss of ovarian function is also very common; the ovaries develop normally at first but oocytes die prematurely and most ovarian tissue degenerates before birth.19,20 Many girls do not undergo puberty unless they receive hormone therapy. About 30 percent of females with Turner syndrome have extra folds of skin on the neck, lymphedema, skeletal abnormalities, or kidney problems. 6 One-third to one-half of individuals are also born with a heart defect that can be life threatening, most frequently aortic coarctation. 21 Many girls and women with Turner syndrome have normal intelligence, but characteristics can vary among individuals.6,20
Conclusion
Turner syndrome is the most common sex chromosome abnormality that occurs in female fetuses. Turner syndrome can be characterized by a variety of sonographic findings, and prognosis is highly variable depending on severity of these findings. An amniocentesis or chorionic villus sampling is required for a definitive prenatal diagnosis of Turner syndrome and to confirm monosomy of the X chromosome. Sonography has been the most effective tool in diagnosing Turner syndrome prenatally.
Footnotes
Acknowledgements
The author would like to thank Dr Laura Vricella, Jessica Gerhardt, RDMS, and Jessica Gamm, RDMS, RVT, for their assistance and support with this case study.
Declaration of Conflicting Interests
The authors declare no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
