Abstract
The finding of a splenic abscess is rare, with only 500 to 600 cases ever having been reported internationally. Prior to the advent of sonography and computed tomography, the survival rate for an individual with a splenic abscess was 0%. Present-day real-time imaging with sonography allows for accurate diagnosis of an abscess in the spleen versus rupture, hematoma, splenomegaly, or cyst within the spleen or left kidney. Until recently, the prescribed treatment was splenectomy. The increased understanding of splenic abscess etiology and advancements in pharmacology have allowed the treatment to progress from surgical removal of the entire spleen to draining the abscess using fine-needle aspiration with the use of strong broad-spectrum intravenous antibiotics.
Abscess of the spleen is not a routinely seen finding. A review of the literature shows that only 500 to 600 cases have ever been reported internationally. 1 The pathogenesis of splenic infections responsible for splenic abscess is typically defined by five categories: (1) metastatic hematogenous infection, including intravenous (IV) drug use; (2) hemoglobinopathy; (3) immune system suppression secondary to chemotherapy or human immunodeficiency virus; (4) trauma; and (5) contiguous site of infection.2–5 The most frequent agent of splenic abscess is an infection with gram-positive cocci dominated by Enterobacteriaceae. When gram-negative bacilli are the causative agent of the infection, the most frequently represented are Klebsiella pneumoniae and Escherichia coli. 6 Most splenic abscesses are caused by a source of infection originating from outside of the affected organ. Sengupta and Mukhergi 7 determined that 70% of splenic abscesses were caused by infectious sources external to the spleen such as amoebic dysentery, peritonsillar abscess, bacterial endocarditis, lung abscess, appendicitis, or pneumonia. An additional 15% were related to direct trauma to the spleen, and 10% were a result of sepsis.
We present a case of splenic abscess secondary to urosepsis, an infection of the urogenital tract that occurs when bacteria are introduced, which was detected and monitored by sonography. In this case, a prior medical procedure, a transrectal sonography-guided prostate biopsy, allowed E coli to travel to the spleen via the bloodstream.
Case Report
A man in his mid-50s underwent a transrectal sonography-guided prostate biopsy due to elevated prostate-specific antigen (PSA). Bactrim, a preparation of sulfamethoxazole and trimethoprim, had been given for perioperative prophylaxis. Four days after the procedure, the patient returned to the emergency room (ER) with a high-grade fever and abdominal pain. The urinalysis was positive for E coli, and urosepsis was determined to be secondary to the transrectal sonography-guided prostate biopsy. Antibiotic therapy using IV vancomycin (a drug choice usually reserved for treatment of bacterial infections resistant to other drugs) was administered. Nineteen days after the procedure, the patient presented a second time to the ER with a moderate-grade fever, chills, rigors, and increased abdominal pain in the left upper quadrant. A complete abdominal sonographic examination was done using a Philips IU22 system (Koninklijke, The Netherlands) with a curved linear-array 6-MHz transducer that showed an abscess in the spleen. The abscess was noted to be located in the posterior spleen. Abscess volume of 90.4; mL was calculated using the splenic volume calculation package based on measurements of the abscess length (6.40 cm), height (6.26 cm), and width (4.30 cm) (Figures 1 and 2). The abscess had an oval, anechoic appearance with well-defined borders and strong posterior enhancement. No inflammatory rim or isoechoic infiltrations were detected. A peripherally inserted central catheter line was established for the administration of ceftriaxone, a third-generation cephalosporin antibiotic with broad-spectrum activity against gram-positive and gram-negative bacteria. After 14 days of 2 mg IV ceftriaxone daily, a 91% reduction of the abscess volume was visualized on a follow-up sonogram (Figures 3 and 4). In addition to its smaller size (3.30 × 2.81 × 1.70 cm; 8.07 mL), the abscess had also lost its anechoic appearance. The shape was more round than oval, the borders were not as well defined, and most of the abscess was isoechoic to slightly hypoechoic compared with the spleen. The location of the abscess was isolated to the most posterior section of the spleen with only moderate posterior enhancement. The patient continued ceftriaxone antibiotic therapy for another 14 days, at which time a repeat sonogram showed an additional 1% reduction in volume. The abscess was measured as 2.92 × 2.23 × 2.14 cm (7.30 mL), with only a slight posterior enhancement (Figures 5 and 6). An additional antibiotic treatment with augmentin, twice a day, for 28 days was prescribed. The abscess was noted to be further reduced in size to 1.96 × 2.19 × 1.67 cm (3.73 mL), a 96% reduction of the original abscess. It’s appearance was isoechoic to the spleen with no posterior enhancement (Figures 7 and 8). The remaining slightly echogenic borders were the only detectable evidence of the abscess.
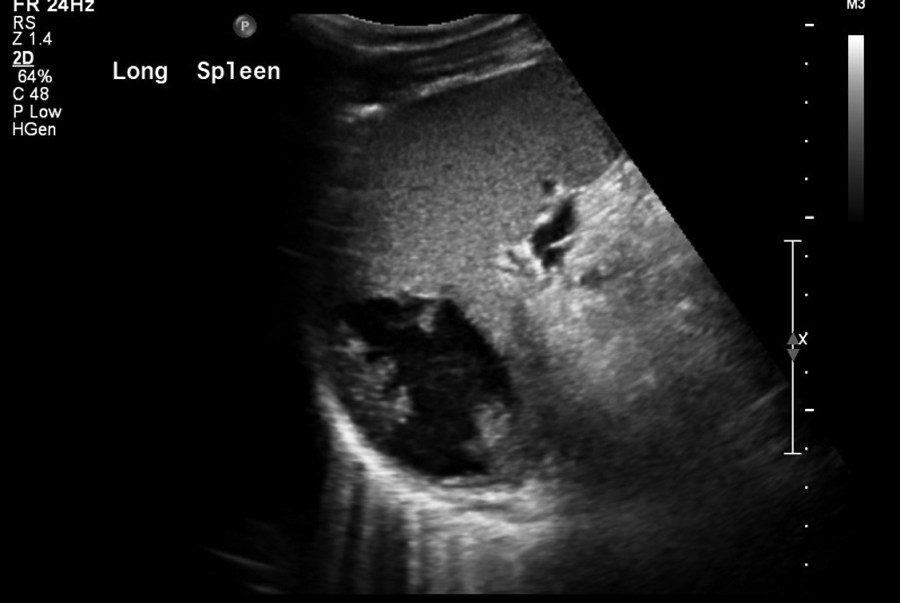
Long view of splenic abscess, 6.40 cm length and 4.30 cm height, 15 days after diagnosis of Escherichia coli and urosepsis secondary to a transrectal sonography-guided prostate biopsy that was done 19 days prior.
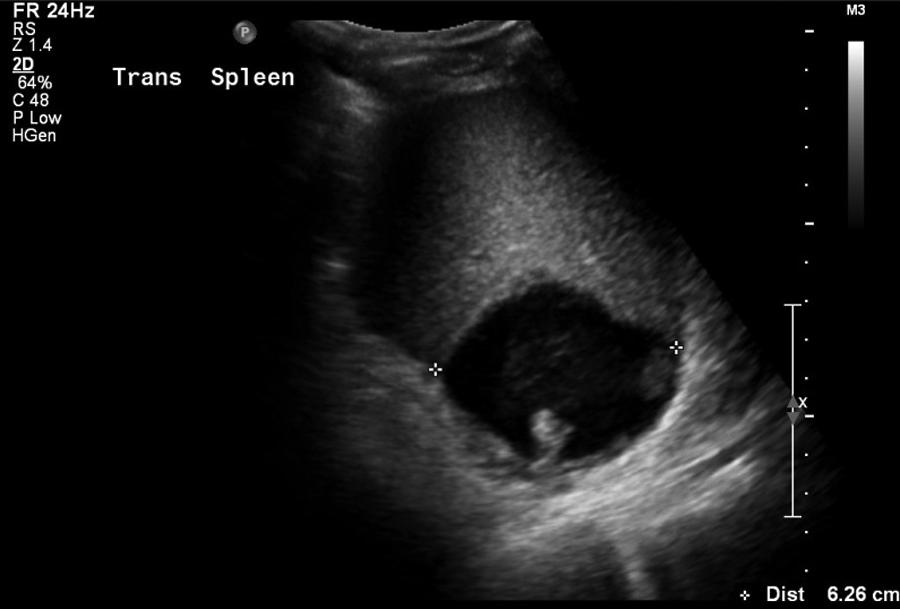
Transverse view of splenic abscess, 6.26 cm width, 15 days after diagnosis of Escherichia coli and urosepsis secondary to a transrectal sonography-guided prostate biopsy that was done 19 days prior.
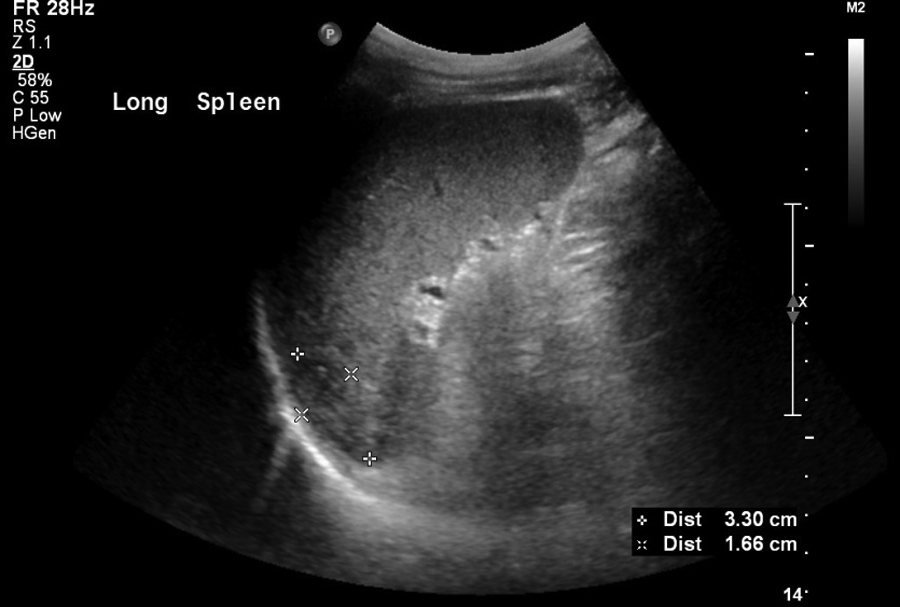
Long view of splenic abscess, 3.30 cm length and 1.66 cm height, 15 days after beginning treatment with intravenous ceftriaxone 2 mg/d.
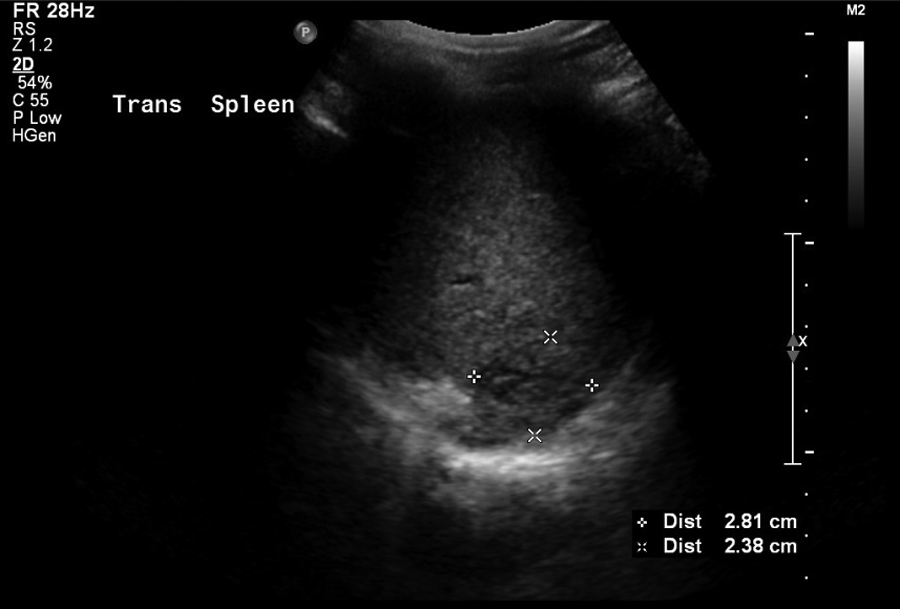
Transverse view of splenic abscess, 2.81 cm width, 15 days after beginning treatment with intravenous ceftriaxone 2 mg/d.
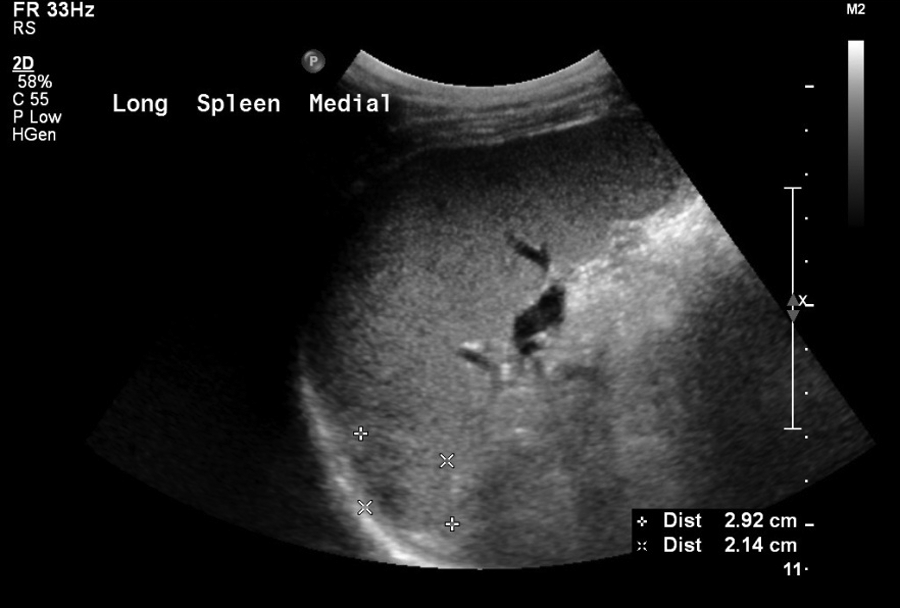
Long view of splenic abscess, 2.92 cm length and 2.14 cm height, 30 days after continued treatment with intravenous ceftriaxone 2 mg/d.
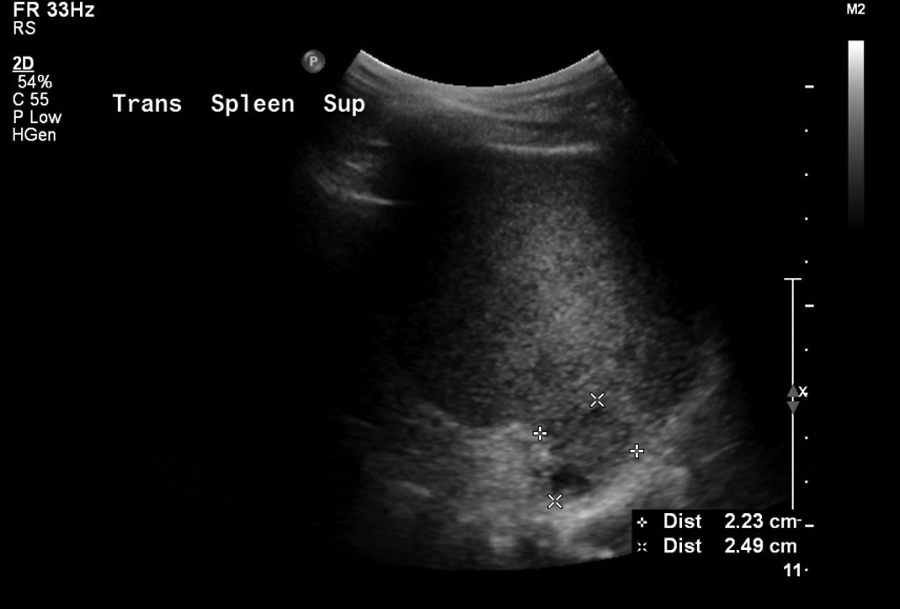
Transverse view of splenic abscess, 2.23 cm width, 30 days after continued treatment with intravenous ceftriaxone 2 mg/d.
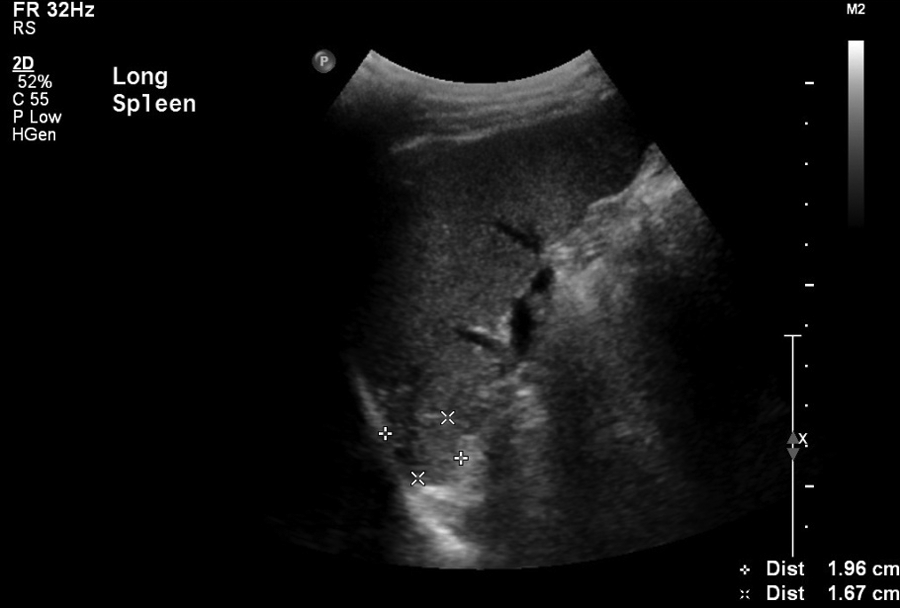
Long view of splenic abscess, 1.96 cm length and 1.67 cm height, 28 days after oral administration of augmentin and 30 days of treatment with intravenous ceftriaxone 2 mg/d.
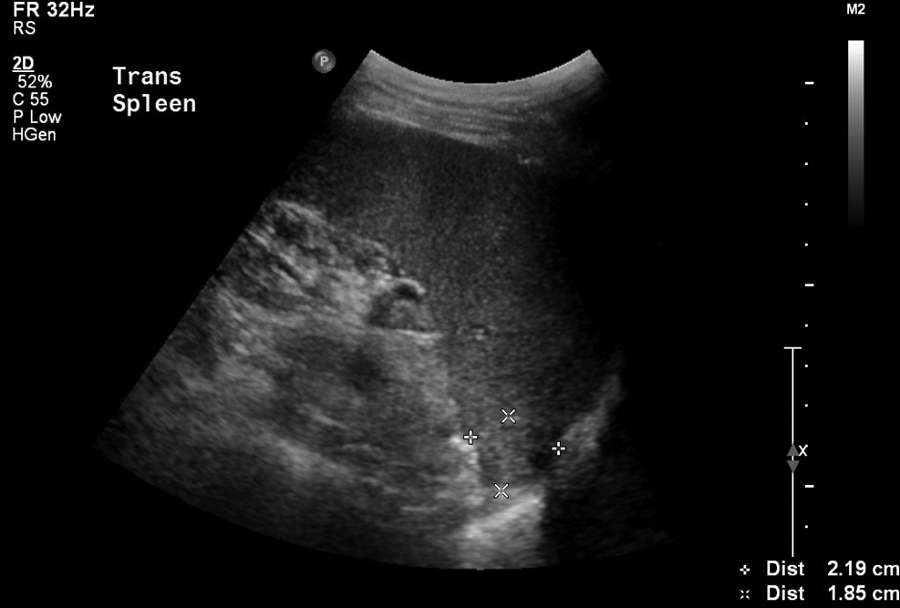
Transverse view of splenic abscess, 2.19 cm width, 28 days after oral administration of augmentin and 30 days of treatment with intravenous ceftriaxone 2 mg/d.
Discussion
Splenic abscess is a rare finding caused by infectious sources external to the spleen, direct trauma to the spleen, or a result of sepsis.3,4,6–9 They are found more often in adults as a singular unilocular abnormality and more often in children as multiple or multilocular abnormalities. Sepsis may be secondary to a variety of sources such as endocarditis, dental infections, or, as in the case presented, urosepsis. Sepsis will occur when an infection leads to systemic inflammatory response syndrome, 10 the dysregulation of the inflammatory response with excessive and uncontrolled release of proinflammatory mediators. It can lead to apnea, abnormal organ function, changes in mental function, decreased urine output, and disseminated intravascular coagulopathy, forming microthrombi or other blood abnormalities. If severe, sepsis can lead to septic shock and hypotension, hypoperfusion of one or more organs, and eventually end-organ ischemia. Early detection is essential for a favorable prognosis, and treatment with antibiotics should be started as soon as possible after diagnosis. For every hour of delay in beginning treatment with the correct antibiotic therapy, there is a correlating 7% rise in mortality. 11
In the case presented, a splenic abscess was a result of a prior medical procedure, a transrectal sonography-guided prostate biopsy, which allowed E coli to become translocated via the bloodstream to the spleen. A potential contributing factor in this particular case was the patient’s prior history of chronic obstructive pulmonary disease (COPD) and osteoarthritis. He was taking albuterol to help manage the COPD, a steroid that reduces the body’s inflammatory response. This may have reduced the ability of the patient’s immune system to respond to the infection resulting from the transrectal sonography-guided prostate biopsy.
Transrectal sonography-guided prostate biopsy is frequently associated with minor complications (60%−79% of cases) but rarely with major complications that require hospitalization (0.4%−3.5% of cases).12–14 Early complications of transrectal sonography-guided prostate biopsy include hematuria (70.8%) and rectal bleeding (8.3%). Delayed complications of transrectal sonography-guided prostate biopsy, at 3 to 7 days postbiopsy, include persistent hematuria (47.1%), vague pelvic discomfort (13.2%), hematochezia (rectal bleeding) (9.1%), dysuria (9.1%), and hematospermia (blood in the semen) (9.1%). Even though complications from transrectal sonography-guided prostate biopsies are fairly common, a study by Paterson et al 12 determined that only 0.23% of 4749 outpatients in whom transrectal sonography-guided prostate biopsies were performed between 2001 and 2006 were positive for urosepsis. A recently tested protocol included obtaining colon swabs from the patient prior to the transrectal sonography procedure to determine the sensitivity of the flora. 14 Antibiotic prophylaxis was then selected to reflect the organisms encountered and their susceptibilities, decreasing the infective complications.
Sonography was an essential element in the diagnosis and surveillance during the course of treatment in this case of splenic abscess. Sonography allowed a noninvasive, rapid accurate diagnosis of an abscess in the spleen versus possible diagnoses of rupture, hematoma, splenomegaly, or cyst. The ability of sonography to monitor the splenic abscess allowed the treatment with strong broad-spectrum IV antibiotics to run its course without the need for splenectomy or other invasive procedures.
Conclusion
The use of imaging modalities such as sonography can confirm or rule out a splenic abscess in a febrile patient with left upper quadrant pain. If such an abscess is not detected and treated with antibiotics early, it may become severe and rapidly life-threatening with a mortality rate up to 47%. 9 The ability of sonography to monitor the effectiveness of the antibiotics being administered has allowed successful pharmacologic treatment of splenic abscesses and avoided invasive procedures and splenectomy with its surgical risks and long-term consequences.
Footnotes
Acknowledgements
The author thanks Sharlette D. Anderson, MHS, RDMS, RVT, RDCS, and Ecaterina M. Hdeib, MA, RDMS, for their encouragement and help in writing and editing this case study.
Declaration of Conflicting Interest
The author declared no potential conflicts of interest with respect to the authorship and/or publication of this article.
Funding
The author received no financial support for the research and/or authorship of this article.
