Abstract
Factitious Disorder Imposed on Another (FDIA), formerly known as Munchausen Syndrome by Proxy, is a complex psychiatric condition that is underdiagnosed and under-identified in which a caregiver fabricates or induces illness in another person, typically a dependent, to gain attention or sympathy. This article presents a detailed case report that highlights the diagnostic challenges and ethical considerations associated with FDIA. The report discusses the clinical presentation, diagnostic approach, and management strategies while emphasizing the importance of a multidisciplinary approach. Insights into the psychological motives behind FDIA and its impact on victims are also explored. This case aims to contribute to the growing body of literature on FDIA and raise awareness among healthcare professionals about this potentially life-threatening condition.
Introduction
Factitious Disorder Imposed on Another (FDIA) is a complex psychiatric disorder characterized by the deliberate fabrication or induction of illness, symptoms, or conditions in another person, usually by a caregiver. The victim is often a child, making this condition not only a medical concern but also a form of child abuse. FDIA presents significant challenges in clinical practice, as it requires healthcare professionals to distinguish between genuine medical conditions and fabricated illnesses. This process can be further complicated by the caregiver’s manipulation of medical personnel and systems.1 -3 Additionally, FDIA is often underdiagnosed due to the fear of legal repercussions for physicians, the media’s tendency to sympathize with parents, and the fact that it can coexist with organic comorbidities, making it harder to identify.
The first documented cases of FDIA were described by British pediatrician Sir Roy Meadow in 1977, who recognized the deliberate harm inflicted on children by their caregivers. 2 Since then, FDIA has garnered attention from both the medical and legal communities due to its severe consequences for victims. Despite increased awareness, FDIA remains underdiagnosed, partly due to its covert nature and the lack of specific diagnostic criteria until its inclusion in the DSM-5. 1 This case report highlights the importance of institutional support and multidisciplinary collaboration in identifying and managing FDIA, particularly in light of recent trends that have vilified pediatricians for bringing forth such allegations.
This article explores the case of a child victimized by FDIA, detailing the clinical presentation, diagnostic process, and therapeutic strategies. The discussion also examines the psychological underpinnings of the disorder and the ethical dilemmas faced by healthcare providers. By shedding light on the complexities of FDIA, this article aims to enhance recognition and management of this challenging condition.
Materials and Methods
Case Identification
The case discussed in this article was identified through collaboration with pediatric, psychiatric, and legal professionals. The patient, a minor, presented with recurrent hospital admissions for unexplained symptoms.
Diagnostic Criteria
The diagnosis of FDIA was guided by the criteria outlined in the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5). The following elements were considered:
Evidence of falsification of physical or psychological signs or symptoms in another individual.
The deceptive behavior was present in the absence of external rewards.
The behavior was not better explained by another mental disorder.
The perpetrator, rather than the victim, received the diagnosis.1,3
Data Collection
Clinical data were obtained through a thorough review of medical records, direct observations during hospital stays, and interviews with healthcare providers, the caregiver, and extended family members. Patterns of symptom presentation were analyzed, with particular attention to inconsistencies in reported symptoms and clinical findings. Laboratory tests and imaging studies were conducted to exclude organic causes, and a timeline of medical interventions was constructed to identify potentially unnecessary procedures.4,5 As per the APSAC guidelines, it is important to note that FDIA cannot be identified solely through clinical interviews or psychological evaluations of the caregiver, as perpetrators are often sophisticated liars who may appear as diligent caregivers.
Multidisciplinary Approach
A multidisciplinary team consisting of pediatricians, psychiatrists, psychologists, social workers, and legal representatives was assembled to evaluate the case. Team members conducted psychological assessments of the caregiver to explore underlying psychopathology and motivations. Simultaneously, the child’s physical and psychological well-being was closely monitored. Child protective services were involved from the outset to ensure the safety of the victim.6 -8 The key component of identifying the perpetrator in this case was the review of medical data against known patterns of Ehlers-Danlos syndrome (EDS) and the observation of inconsistent wound progression when the mother was the sole caregiver.
Ethical Considerations
Given the sensitive nature of FDIA, strict confidentiality was maintained throughout the investigation. Informed consent was obtained where applicable, and interventions were carried out in collaboration with child protective services to ensure the safety and well-being of the victim.7,9 The APSAC guidelines were followed to ensure an evidence-based approach to evaluation and management.
Results
Case Presentation
The case involves a 3-and-a-half-year-old child who was initially brought to the emergency room (ER) for a wound on his left leg (Figure 1). The wound was sutured, and the child was sent home. The following day, the same child returned to the ER with another wound that required suturing. Upon questioning, the parents claimed that the child was being monitored for Ehlers-Danlos syndrome (EDS), a genetic condition that can cause fragile skin and delayed wound healing. However, EDS is often over-reported and self-diagnosed, particularly with the rise of online support groups, making it a common misdiagnosis in cases of FDIA. 10

The scar of the first wound sutured initially in the OR.
Over the subsequent weeks, the child presented multiple times at various healthcare facilities with wounds in different locations, all requiring sutures (Figure 2). Each visit raised more questions, as the wounds seemed unusual and did not fully align with those typically seen in patients with Ehlers-Danlos syndrome. Suspicions escalated when the parents could not provide any medical documentation confirming the child’s EDS diagnosis, stating instead that the documents had been lost.
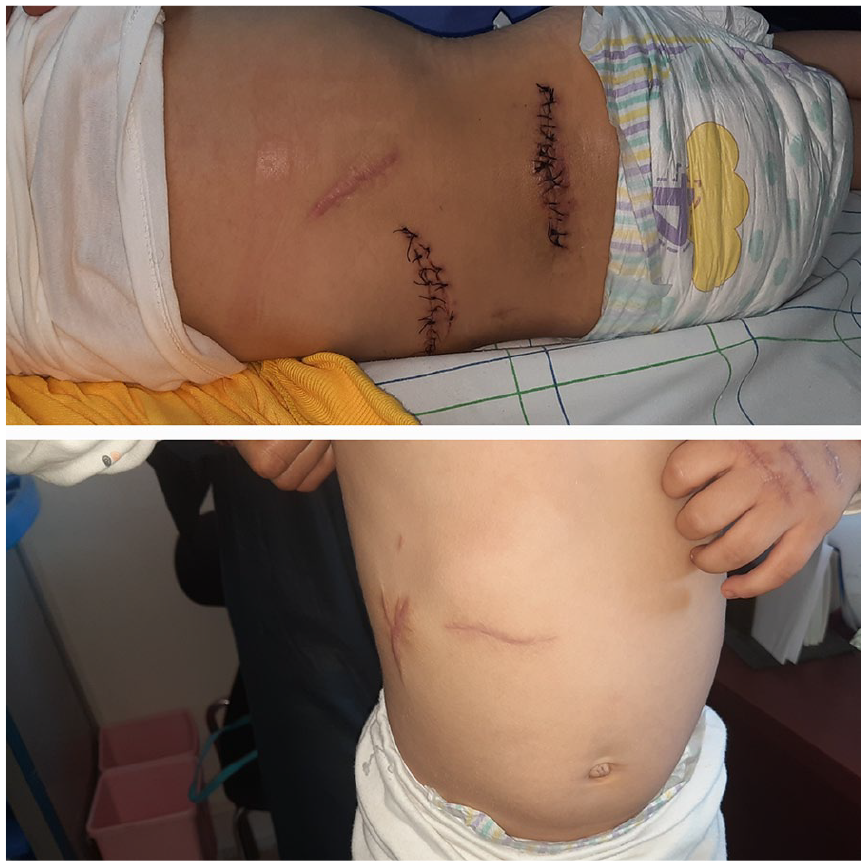
Wounds on differents locations sutured.
The child was hospitalized for further evaluation (Figure 3). A skin biopsy was performed to investigate the possibility of Ehlers-Danlos syndrome, but the results came back negative. During the hospital stay, it was noted that new wounds appeared primarily at night, when the child’s mother was the sole caregiver. This observation ruled out the father’s involvement and narrowed suspicion to the mother. A detailed review of the child’s medical history revealed additional concerning patterns. Between the ages of 3 months and 1 year, the child had experienced episodes of rectal bleeding that were extensively investigated, including a colonoscopy, which yielded negative findings. Later, the child developed gingival bleeding, prompting consideration of Osler-Weber-Rendu disease, which was subsequently ruled out. By the age of 3, the child began presenting with recurrent wounds requiring sutures, which the parents repeatedly attributed to a form of Ehlers-Danlos syndrome, despite a lack of supporting evidence.

Scalp wound that initiated the hospitalization, before and after sutures.
These findings, coupled with inconsistencies in the parents’ accounts and the negative biopsy result, heightened the medical team’s suspicions and prompted the involvement of a social worker, psychologist, and relevant authorities.
Diagnostic Process
To confirm the diagnosis of Factitious Disorder Imposed on Another (FDIA), a meticulous and multidisciplinary investigative process was undertaken. The diagnostic journey began with an extensive review of the child’s medical records, which revealed a pattern of unexplained symptoms and injuries over several years, often reported by the mother. It is important to note that the mother’s admission to her actions was highly unusual, as most perpetrators do not confess. Typically, evidence is gathered through thorough chart reviews and surveillance, which are time-consuming and often not feasible in busy clinical settings.
During the child’s hospitalization, healthcare staff observed that new wounds appeared predominantly during nighttime hours (Figure 4), when the child’s mother was alone with him. This observation excluded the father as a potential perpetrator and reinforced concerns about the mother’s role. To further investigate, the parents were asked to provide documentation of the purported Ehlers-Danlos syndrome diagnosis. Their inability to produce these records, combined with the negative results of the skin biopsy, cast significant doubt on the validity of the diagnosis.
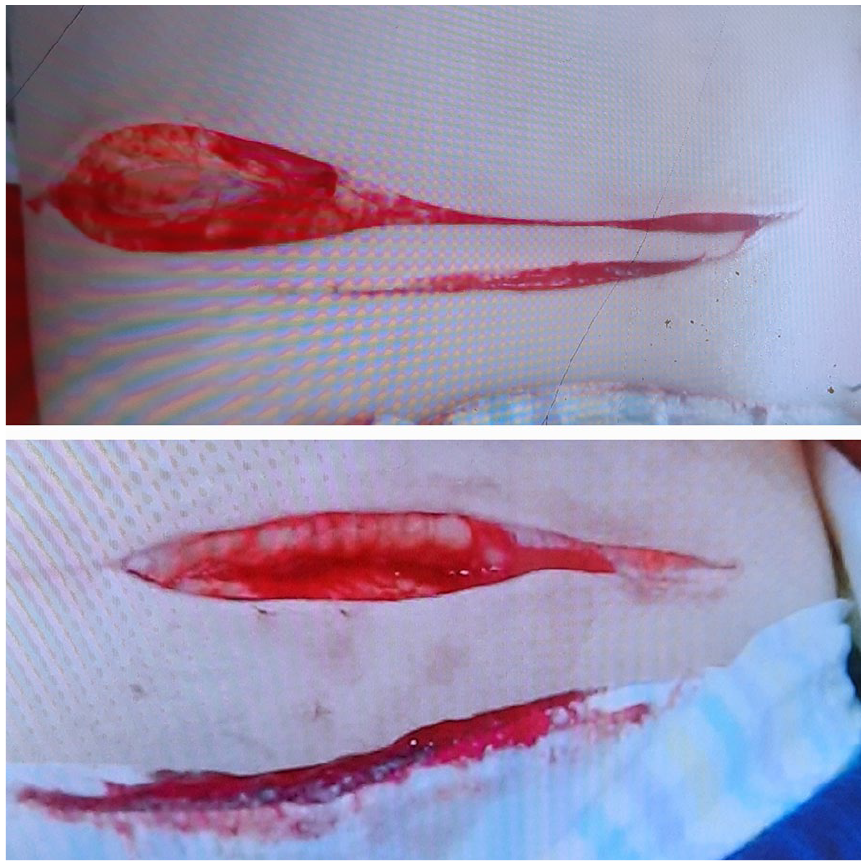
Uncommon wound for Ehlers Danlos disease that raised suspicions.
A thorough interview with the child’s father revealed additional discrepancies and raised further suspicions about the mother’s behavior. The medical team also re-examined earlier episodes of rectal and gingival bleeding, which had been extensively investigated with no organic cause identified. These events were consistent with the possibility of fabricated or induced symptoms.
With the support of psychologists, social workers, and legal authorities, the parents were separated from the child during evening and nighttime hours to monitor the child’s condition without interference. Remarkably, no new wounds occurred during this period of isolation. This absence of symptoms strongly implicated the mother as the source of the child’s injuries. Subsequent psychological evaluations and interviews with the mother revealed that she had been intentionally inflicting wounds on the child. These findings confirmed the diagnosis of FDIA and necessitated immediate intervention to ensure the child’s safety.
Interventions and Outcomes
The primary goal of intervention was to protect the child from further harm while addressing the mother’s behavior and underlying psychopathology. The child’s safety was ensured by isolating him from the mother during critical periods, such as evenings and nights, when the injuries had previously occurred. This immediate action effectively stopped the occurrence of new wounds, providing both physical safety for the child and confirmation of the mother’s involvement.
Social services and legal authorities were promptly engaged to evaluate the family’s situation and implement protective measures. The child was placed under the care of child protective services, ensuring a secure environment free from further harm. The father’s cooperation and willingness to provide information were crucial in piecing together the history of the mother’s behavior and advocating for the child’s safety. However, it is important to consider the father’s role in enabling the mother’s actions, as he may have been complicit in the abuse by failing to intervene earlier.
Psychological interventions were initiated for the mother, including therapy to address her underlying motivations and psychopathology. However, engagement in treatment is often challenging in cases of FDIA, as perpetrators may deny wrongdoing or resist therapeutic efforts. Long-term psychological support was also recommended for the child to address potential emotional and psychological consequences of the abuse, including trust issues and trauma-related symptoms.
The case highlights the importance of a multidisciplinary approach in managing FDIA. Collaboration between pediatric surgeons, psychologists, social workers, and legal authorities ensured a comprehensive response to the situation. While the immediate outcome—protection of the child—was achieved, ongoing monitoring and support for both the child and family were emphasized to prevent recurrence and promote recovery.
Discussion
Diagnostic Challenges
FDIA poses significant diagnostic challenges due to its insidious and deceptive nature. The caregiver’s ability to manipulate medical professionals and systems often delays recognition of the disorder. Misdiagnosis or delayed diagnosis can lead to unnecessary medical procedures, prolonged suffering for the victim, and potential harm. This case underscores the importance of maintaining a high index of suspicion and systematically evaluating inconsistencies in the caregiver’s narratives.2,4,11 Another challenge is that 90% of medical care relies on parents’ verbal reports of symptoms, which can lead to iatrogenic harm when those reports are fabricated.
One key challenge is distinguishing FDIA from genuine medical conditions, particularly when the caregiver provides convincing accounts of symptoms. In this case, meticulous documentation and collaboration among specialists were crucial for uncovering the truth. Children with developmental delays or complex medical conditions are at higher risk of FDIA, as it can be harder to distinguish between real and fabricated symptoms.
Psychological Motives and Dynamics
The psychological motives behind FDIA remain poorly understood but are thought to involve a need for attention, validation, or control. Caregivers with FDIA often display traits of personality disorders, such as borderline or narcissistic tendencies. In this case, the caregiver’s behavior appeared to stem from a profound need for sympathy and recognition, leading to the intentional harm of the victim. Understanding these dynamics is crucial for developing effective therapeutic strategies.8,12,13 Perpetrators are often resistant to treatment, and long-term separation from the victim is usually necessary to ensure safety.
Victims of FDIA often suffer long-term psychological consequences, including post-traumatic stress disorder (PTSD) and difficulties forming trusting relationships. Early intervention is essential to mitigate these effects and provide the child with a supportive environment for recovery. 14
Ethical and Legal Considerations
Healthcare providers face numerous ethical and legal dilemmas when managing FDIA. Balancing the duty to protect the victim with the need to respect the caregiver’s autonomy requires careful judgment. In this case, multidisciplinary collaboration was essential for ensuring the child’s safety while adhering to ethical principles. The involvement of child protective services and legal authorities highlights the importance of a coordinated response to FDIA.6,7,9 The APSAC guidelines provide a framework for managing these cases, emphasizing the need for institutional support and thorough documentation.
FDIA cases also raise questions about the boundaries of physician-patient confidentiality. Reporting suspected cases to child protective services is not only a legal obligation but also an ethical imperative to prevent further harm to the victim. 4 In cases where the perpetrator denies involvement, hidden cameras or other surveillance strategies may be necessary to gather evidence, though these methods must be used ethically and legally.
Management Strategies
Effective management of FDIA involves addressing the immediate safety of the victim, providing psychological support for the affected child, and implementing therapeutic interventions for the caregiver.3,15 In most cases, separation from the perpetrator is necessary to prevent further harm. This case illustrates the value of a multidisciplinary approach, including input from pediatricians, psychiatrists, social workers, and legal professionals.7,16,17 Perpetrators are often resistant to treatment, and long-term monitoring of the victim is critical to prevent recurrence.
Therapeutic interventions for the caregiver may include psychotherapy to address underlying psychopathology, although engagement in treatment is often limited. Long-term monitoring of the victim’s well-being is also critical to ensure sustained recovery and prevent recurrence of abuse.
Implications for Practice
FDIA remains a challenging and underrecognized condition that requires heightened awareness among healthcare professionals. This case highlights the need for improved training and guidelines to facilitate early detection and intervention. Future research should focus on elucidating the underlying psychological mechanisms of FDIA and developing evidence-based treatment protocols.12,13,18 Institutional support for healthcare teams is crucial, as cases of FDIA often require extensive time and resources to investigate.
Conclusion
Factitious Disorder Imposed on Another is a complex and underdiagnosed psychiatric condition with significant implications for victims and healthcare systems. This case report underscores the importance of early recognition, multidisciplinary collaboration, and ethical decision-making in the management of FDIA. 3 By increasing awareness and understanding of this disorder, healthcare professionals can better protect vulnerable individuals and improve outcomes for affected families. Continued research and education are essential to advancing the diagnosis and treatment of FDIA. The APSAC guidelines provide a valuable framework for managing these cases, and institutional support is critical for ensuring the safety of victims.
Footnotes
Ethical Considerations
No ethical approval is required for de-identified case reports and case series based on our institutional policies.
Consent for Publication
Written informed consent was obtained from the patient’s legally authorized representatives.
Author Contributions
All the authors contributed equally to the conception, acquisition, analysis, interpretation of data, and drafted and approved the manuscript.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
