Abstract
Neonatal and pediatric mortality rates are disproportionally higher in Sub-Saharan Africa, yet data on the rates of healthcare-associated infections (HAIs) in this population are lacking. Using the flexible methodology of a scoping review, we aimed to identify neonatal and pediatric HAI studies not previously included in systematic reviews. We conducted a scoping review to identify studies in the World Health Organization’s Africa region conducted from 2007 to 2021 that reported HAI rates in neonates and/or older children. This scoping review identified 37 studies from 14 countries. The studies confirmed widespread HAIs in children and neonates, however the variability of rate definitions and methodologies did not allow for comparisons between studies or countries. This study illustrates the largely unrecognized efforts across the WHO Africa region to estimate HAI rates in children and highlights the importance of standardizing surveillance methods to implement and monitor impact of preventative strategies.
Keywords
Introduction
Sub-Saharan African countries have disproportionately high rates of deaths in neonates and in children less than 5 years of age. 1 Healthcare-associated infections (HAIs) are increasingly recognized as important causes of neonatal and pediatric morbidity and mortality in this region.2,3 The precise rates are mostly unknown for numerous reasons including lack of electronic medical record systems to support HAI surveillance, variations in ICD 10 codes among nations, and use of different methodologies to collect and report data.3 -5
These factors impede comparisons between studies and drawing conclusions regarding the findings’ generalizability. 6 Most published African HAI surveillance studies include only adult data. 4 However, we theorized that pediatric and neonatal surveillance data may be incorporated into overall hospital data and therefore are not easily discovered with systematic searches. Furthermore, data may be published in local journals and not included in all international research databases.
These limitations may result in systematic reviews that contain few or no African data and underestimate the burden of HAIs in children. 2 Therefore, scoping reviews, with their flexible methodology, are better suited to address these challenges. The primary objective of this scoping review was to review studies presented in a wide range of journals that reported HAI rates in the neonatal and/or pediatric population across the WHO Africa region. Identification of pathogens causing HAIs was also reviewed when available.
Methods
Protocol and Registration
Following the Joanna Briggs Institute (JBI) guidelines for scoping review design, a review protocol was registered in Open Science Forum (osf.io/mb356). 7
Eligibility Criteria
Study designs: Abstracts and published studies in English or French that reported HAI rates (prevalence, incidence, or other frequency) in pediatric and neonatal populations in Africa were reviewed. HAI rates could include neonatal rates or combined neonatal and pediatric rates. Publications that were case reports, did not provide pediatric data, did not provide rate data, or only provided early-onset sepsis rates were excluded.
Population: The population included neonates and children less than 18 years of age in countries of the WHO Africa Region (https://www.afro.who.int/countries).
Outcomes: Outcomes of interest included all neonatal and pediatric HAI and in-hospital mortality. HAI cases were defined by each study and not assessed by the study team for validity. Incidence and prevalence were defined as previously described by the United States Centers for Disease Control and Prevention.8,9
Dates of Search: The search included studies published from January 1, 2007 to November 22, 2021. The start date was selected to coincide with WHO’s 2007 announcement of the resolution to combat antimicrobial resistance and encourage surveillance reporting of infections and antimicrobial resistance.
Search Strategy
The search strategy was developed with a 3-step process as recommended by JBI guidelines (Table 1). The search string (Supplemental Material 1) was run through 9 databases on November 22, 2021, including: PubMed, Embase, Google Scholar, African Index medicus, SCOPUS, MedNar, MEDLINE, Ebsco host, and CINAHL.
Search Strategy Development.

Selecting Studies
Using Covidence (http://covidence.org), duplicates were removed. Two members of the study team independently screened titles and abstracts and removed excluded publications as per the criteria above (Figure 1). Three team members then reviewed full texts and removed further ineligible studies due to lack of rate data. Conflicts for study inclusion were resolved with team members until consensus was reached. The references of included papers were reviewed; none met eligibility criteria for inclusion.

Process of study selection using covidence.
Data Extraction
Data were extracted from eligible studies (Supplemental Material 2) using the Covidence platform. Two team members extracted data from each study. Data extraction fields included country, year of publication, year(s) of study, study design, study population, type of HAIs, HAI rate(s), pathogens, and antimicrobial susceptibility. Specific pathogens were recorded when available. Studies that did not specify specific pathogens were classified as surveying for “all pathogens.” Discrepancies in extracted data were discussed until consensus was reached. We did not obtain additional data nor confirm data with the studies’ investigators.
Data Presentation
Extracted data for HAI prevalence, incidence, and other rates were presented in separate tables. Studies that included more than 1 type of rate (eg, both prevalence and incidence) were included in more than 1 table. Rates that did not meet prevalence or incidence definitions were classified as “other.” The study population for studies that included both neonates and older children was classified as “all children” and the population for studies that included children but not neonates was classified as “older children.”
Ethical Approval and Informed Consent
Ethics approval was not required as per the local institutional review board for this scoping review.
Results
Included Studies
This scoping review included 37 studies from 14 countries (Figure 2). South Africa most frequently published HAI data (n = 18 studies), followed by Ethiopia (n = 3), Kenya (n = 3), Uganda (n = 2), and Nigeria (n = 2).
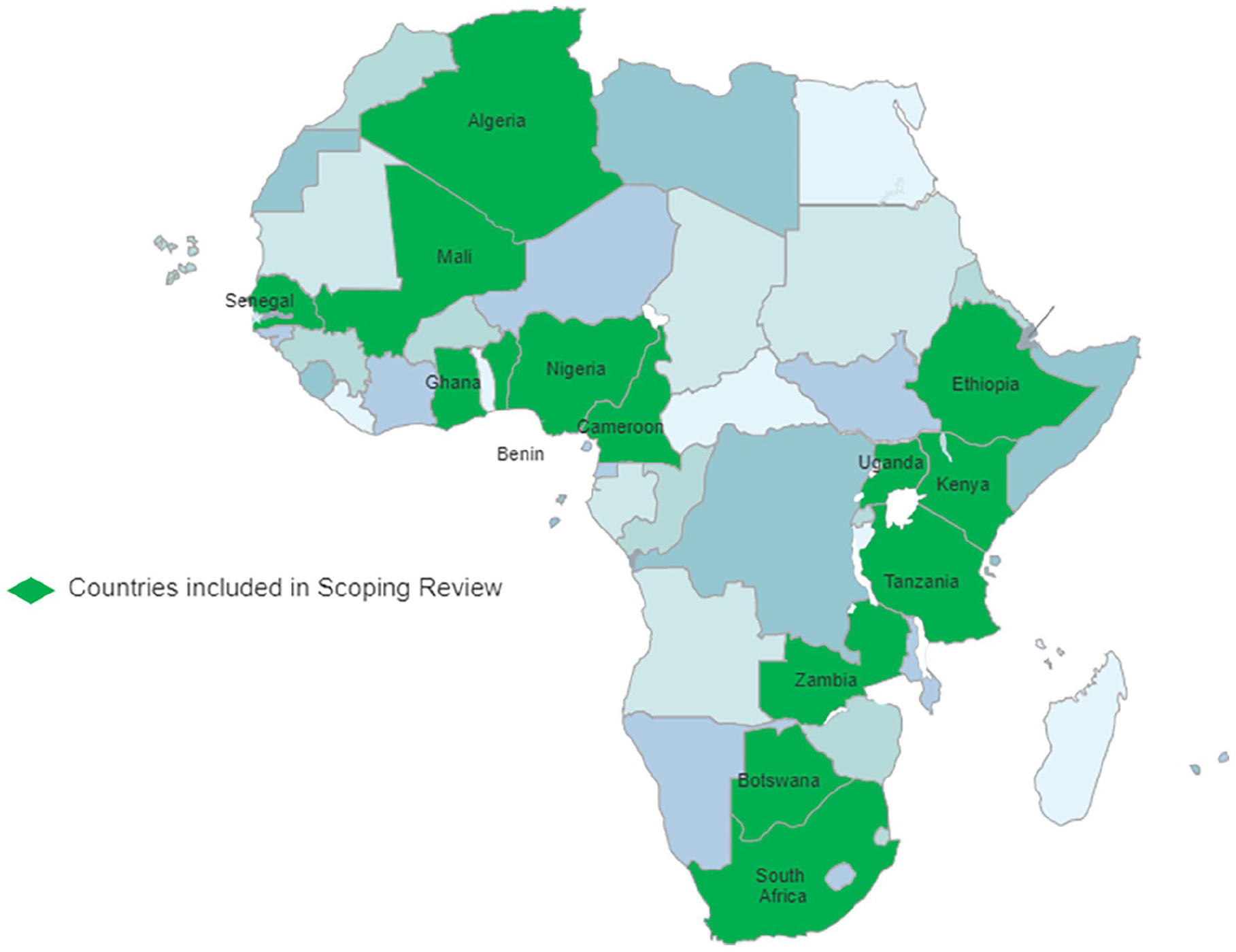
Map of countries of included studies.
Twenty-nine studies (78%) reported only pediatric or neonatal HAIs and 8 studies (22%) reported HAIs for both children and adults. Twenty-eight (76%) studies included HAIs in neonates of which 22 reported separate neonatal rates and 9 reported combined rates for all children.
All 37 studies reported bloodstream infection data. Twelve (32%) also reported other types of HAIs, the most common being respiratory (n = 8/37, 22%), urinary tract infections (n = 8/37, 22%), and surgical site infections (n = 7, 19%). Two (5%) reported central line-associated bloodstream infections.
Most studies defined HAIs as infections that presented 48 hours after admission (n = 26, 70%) or 3 days after admission (n = 4, 11%). The HAI definitions are provided in Supplemental Material 3.
HAI Prevalence
Twelve (32%) of the 37 included studies reported prevalence of HAIs (Table 2), most (n = 8/12, 67%) of which were point-prevalence surveys. Eight (67%) of 12 studies reported prevalence rates for multiple types of HAIs (range 3-7 HAIs) and 4 (33%) reported prevalence rates for BSIs only. All 12 studies reported HAIs caused by all pathogens. Seven (58%) reported HAI prevalence in neonates and 4 (33%) reported prevalence in older children. Most (n = 9/12, 75%) rates were calculated for “surveyed patients.” Prevalence rates for BSIs in neonates were reported as 1.13% of admissions in a prospective cohort study performed in Kenya, 11 24.1% of surveyed patients in a point prevalence study performed in Benin, 12 and 50% of surveyed patients in a point-prevalence study performed in Uganda. 13 A study in Nigeria 14 reported the prevalence of HAIs in the pediatric surgery ward. A study in Uganda 15 showed reduction of HAIs after implementing an infection control program.
Prevalence of Healthcare-associated Infections in the WHO Africa Region, Scoping Review January 2007 to November 2021.

Abbreviations: BSI, bloodstream infections; CLABSI, central-line associated bloodstream infections; CNS, central nervous system; ENT, ear, nose, throat; GI, gastrointestinal infections; HAIs, healthcare-associated infections; MSK, Musculoskeletal; NICU, neonatal intensive care unit; RTI, respiratory tract infection; SSI, surgical site infection; SSTI, skin/soft tissue infection; URI, upper respiratory infections; UTI, urinary tract infections.
ID = identification number for included studies.
Published in 2018.
HAI Incidence
Sixteen (43%) studies reported incidence rates of HAIs of which 10 reported all pathogens (Table 3) and 6 reported select pathogens (Table 4). Three studies assessing neonatal BSIs reported incidence rates for all pathogen which ranged from 3.6 to 6.27 BSIs per 1000 patient-days. Three studies assessing BSIs in all children reported all pathogen incidence rates which ranged from 1.0 to 22.5 BSIs per 1000 patient-days. The highest incidence rates assessing multiple types of HAI were reported in 2 pediatric ICU studies performed in South Africa; both were 94.4 HAIs per 1000 patient-days.16,17
Incidence of Healthcare-Associated Infections in the WHO Africa Region, Scoping Review January 2007-November 2021: All Pathogens.

Abbreviations: BSI, bloodstream Infections; CLABSI, central-line associated bloodstream infections; CNS, central nervous system; ENT, ear, nose, throat; GI, gastrointestinal infections; HAIs, healthcare-associated infections; MSK, musculoskeletal; NICU, neonatal intensive care unit; RTI, respiratory tract infection; SSI, surgical site infection; SSTI, skin/soft tissue infection; URI, upper respiratory infections; UTI, urinary tract infections.
Incidence of Healthcare-associated Bloodstream Infections (BSI) in the WHO Africa Region, Scoping Review January 2007-November 2021: Select Pathogens.

Abbreviations: BSI, bloodstream infections; CLABSI, central-line associated bloodstream infections; CNS, central nervous system; ENT, ear, nose, throat; GI, gastrointestinal infections; HAIs, healthcare-associated infections; MSK, musculoskeletal; NICU, neonatal intensive care unit; RTI, respiratory tract infection; SSI, surgical site infection; SSTI, skin/soft tissue infection; URI, upper respiratory infections; UTI, urinary tract infections.
Other HAI Rates
Seventeen (46%) studies reported rates of HAIs other than prevalence or incidence rates (Table 5). Examples of these other rates included HAIs as a percentage of all infections, percentage of all blood cultures, or proportion of hospitalizations. Study designs included surveillance, retrospective reviews, case control studies, and prospective observational studies. Nine studies reported specific pathogens involved in recent outbreaks or pathogens with antimicrobial resistance.
Other Reported Rates of Healthcare-associated Infections (HAI) in the WHO Africa Region, Scoping Review January 2007-November, 2021.

Abbreviations: HA-BSI, healthcare-associated bloodstream infection; MSSA, methicillin-sensitive Staphylococcus aureus; MRSA, methicillin-resistant Staphylococcus aureus.
Reported Pathogens
Twenty-nine (78%) of the 37 studies provided microbiologic data (Table 6), of which 22 (76%) provided antimicrobial susceptibility data. Twenty-three (79%) studies reported HAIs caused by Gram-negative bacilli, most commonly E. coli (n = 20/23, 87%), K. pneumoniae (n = 14/23, 61%), other Klebsiella spp., (n = 14/23, 61%), or Enterobacter spp. (n = 14, 61%). Twenty-three (79%) studies reported HAIs caused by Gram-positive cocci, most commonly S. aureus (n = 21/23, 91%). Eleven (38%) studies reported HAIs caused by Candida spp.
Pathogen Frequency Reported in Neonatal and Pediatric (HAIs) in the WHO Africa Region, Scoping Review January 2007 to November 2021.

Total number of studies reporting pathogens.
Excluding Klebsiella pneumoniae.
Haemophilus spp. (n = 1), Neisseria meningitidis (n = 1), Stenotrophomonas maltophilia (n = 1), Morganella spp. (n = 1), Burkholderia spp. (n = 1).
Aeromonas spp. (n = 1), Corynebacterium spp. (n = 1).
Discussion
This scoping review identified 37 studies from 14 countries conducted from 2007 to 2021 that reported HAI rates in neonates and/or older children. To our knowledge, only 1 prior systematic review of HAIs conducted in developing countries included Africa and only 3 studies were identified that included children. 4 Other systematic reviews and secondary analyses of severe neonatal bacterial infections included HAIs, but rates were not consistently provided.18,19 We enhanced our yield for publications by including studies that primarily targeted adult patients but included neonatal and pediatric data. With WHO’s recent focus on infection prevention and control (IP&C), 20 more hospitals should be encouraged to systematically evaluate their HAI rates, using methodologies recommended by WHO, particularly in vulnerable populations such as neonates and children.
The studies identified in this scoping review confirm that many African countries experience widespread HAIs in neonates and older children, and have a consistent definition of HAI. However, heterogeneity of included studies hindered our ability to compare rate data across different studies and draw meaningful conclusions. Studies used different study designs and different study populations which were not always precisely defined. Studies reporting incidence rates did not consistently use denominators of 1000 patient-days or 100 admissions. Studies assessing multiple types of HAIs did not report rates for each type of HAI separately and could not be compared to 1 another or to studies reporting BSIs. Studies reporting different select pathogens were useful in outbreak settings, but did not provide estimates of endemic HAI rates.
Data from this scoping review support the need for use of standardized case definitions for HAIs, surveillance strategies, and reporting to facilitate our understanding of the HAI burden in African neonates and older children. According to the 2020 to 2021 Tripartite Antimicrobial Resistance Country Self-assessment Survey (TrACSS), few African countries have implemented national IP&C programs. 20 Surveillance of HAIs and antimicrobial resistance are recognized as critical priorities using standardized surveillance protocols such as the European Centre for Disease Prevention and Control Point Prevalence Study (ECDC PPS). 21 However, while the 2021-2022 global survey indicated that though most countries in the African region had plans for HAI surveillance, it was unclear whether these plans were implemented. 20
Delayed implementation of HAI surveillance likely reflects resource constraints in African hospitals. Surveillance measures that require the total number of admissions and patient-days are challenging to collect without electronic medical records. Many hospitals lack the capacity to consistently perform cultures or generate real-time microbiologic data. While data describing specific pathogens were consistent with previous reports describing the predominance of Gram-negative organisms, 22 collection of these data may have reflected concerns for multidrug-resistant organisms and outbreaks, rather than systematic surveillance of HAIs.23 -25 As supported by findings in this scoping review, clinical criteria to identify HAIs can be used. While use of clinical criteria may impact the precision of HAI surveillance, several large point prevalence surveys, including the ECDC PPS, have used clinical identification of HAIs. 21 Thus, resource-limited hospitals, including smaller district hospitals, could be encouraged to use clinical data to develop HAI surveillance reports.
Limitations
Though the methodology of this scoping review allowed for inclusion of more studies, we were not able to compare them due to their different methodologies. Our language search was limited to English and French, which could have missed studies from Arabic- and Portuguese-speaking countries. The search string could have missed publications. Since authors, hospitals, or governments were not contacted, unpublished data from internal HAI surveillance programs or ongoing studies were not captured by our search. Studies were primarily from South Africa, and less resourced countries were not as well represented. We did not conduct a systematic assessment of the quality of evidence, given the study’s design as a scoping review.
Conclusion
This scoping review is an exploratory effort to present a more comprehensive picture of HAIs in children in Africa by identifying neonatal and pediatric HAI studies not previously included in systematic reviews. Our review identified largely unrecognized efforts across the WHO Africa region to estimate the rate of neonatal and pediatric HAIs, supported the view that current data likely under-represent the burden of HAIs, and further highlighted the importance standardizing surveillance methods. Establishing the baseline burden of HAIs is crucial when implementing and monitoring the impact of preventative strategies.3,11,14 The 2022 WHO Global Report on Infection Prevention and Control identified HAI surveillance as a core component of IP&C programs, established minimum requirements for surveillance programs, and recognized lack of expertise and financial investment as common challenges. 14 Worldwide, hospitals are increasingly being encouraged to perform HAI surveillance. Concurrently, the global community should be urged to help provide the framework for this surveillance in the region most affected by child mortality. These efforts to provide standardization of surveillance methods will facilitate benchmarking for HAI prevention, both at the facility level and nationally.
Supplemental Material
sj-docx-1-gph-10.1177_30502225251324279 – Supplemental material for A Scoping Review of Healthcare-associated Infection Rates in Neonatal and Pediatric Populations in Africa
Supplemental material, sj-docx-1-gph-10.1177_30502225251324279 for A Scoping Review of Healthcare-associated Infection Rates in Neonatal and Pediatric Populations in Africa by Irene Frantzis, Jack Huebner, Neetika Ashwani, Julia Johnson, Lawrence R. Stanberry and Lisa Saiman in Sage Open Pediatrics
Supplemental Material
sj-docx-2-gph-10.1177_30502225251324279 – Supplemental material for A Scoping Review of Healthcare-associated Infection Rates in Neonatal and Pediatric Populations in Africa
Supplemental material, sj-docx-2-gph-10.1177_30502225251324279 for A Scoping Review of Healthcare-associated Infection Rates in Neonatal and Pediatric Populations in Africa by Irene Frantzis, Jack Huebner, Neetika Ashwani, Julia Johnson, Lawrence R. Stanberry and Lisa Saiman in Sage Open Pediatrics
Footnotes
Acknowledgements
We would like to acknowledge John Usseglio for his assistance in the study design.
Ethical Considerations
Ethics approval was not required as per the local institutional review board for this scoping review.
Author Contributions
Conception and design: IF, LS; Design: JH, JJ, LRS; Interpretation: LS; Acquisition and analysis: NA, JH; Acquisition, analysis, and interpretation: IF; Drafted manuscript: IF; Critically revised manuscript: JH, NA, JJ, LRS, LS; Final approval: JJ, LRS, LS; Agrees to be accountable for all aspects of work ensuring itegrity and accuracy: IF, LS.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Irene Frantzis supported by NIAID T32 AI007531. Julia Johnson supported by NIH K23HD100594. The sponsors had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
