Abstract
Effective management of diabetes warrants accurate and regular monitoring of glucose levels to prevent serious diabetes-associated complications and long-term health consequences. Hence, achieving target glucose levels and maintaining adequate glycemic control is essential in diabetes to prevent episodes of hypoglycemia. Multiple glucose monitoring tools have been developed over time, each with differing degrees of precision, convenience, and real-time input. The management of diabetes has been considerably improved by using these various glucose monitoring devices, both in terms of treatment outcomes and patient quality of life. However, in India, the lack of awareness, patient education, availability, and affordability of glucose monitoring devices poses a significant concern resulting in poor adherence to glucose monitoring and low medication adherence thereby increasing disease burden. Consequently, there is an urgent need for healthcare professionals and policymakers in India to collaborate and address the challenges associated with glucose monitoring in patients with diabetes, while also providing recommendations to overcome these concerns. This recommendation article offers a comprehensive evaluation of various glucose monitoring tools available for use by patients suffering from different types of diabetes, explores the challenges associated with glucose monitoring in India, and also presents expert panel recommendations to enhance diabetes management effectively.
Keywords
Introduction
Worldwide, there are 537 million individuals (aged 20-79 years) with diabetes and by 2030 and 2045, this number is expected to rise to 643 million and 783 million, respectively. Approximately three out of four adults with diabetes live in low- and middle-income countries. 1 India has approximately 77 million people with diabetes and is ranked second after China in the global diabetes epidemic. There has been an increase in diabetes prevalence in India from 7.1% in 2009 to 8.9% in 2019. 2 Uncontrolled glucose levels in patients with diabetes remain a major concern in India with a burden as high as 76.6%. 3
Regular monitoring of glucose is crucial for diabetes management. Both high or low levels of blood glucose are associated with impairment of cellular function leading to fatal consequences, if not appropriately managed. 4 Uncontrolled diabetes can cause micro- and macro-vascular complications and is the main reason for disease burden. Microvascular complications lead to retinopathy, neuropathy, and nephropathy, whereas macro-vascular complications are responsible for coronary and peripheral artery diseases. 5 Glucose monitoring facilitates early detection of hypoglycemia and glycemic control assessment, thereby helping to provide optimum treatment options for diabetes. 6 Several glucose monitoring methods are available, such as measurement of glycated hemoglobin (HbA1c) level, self-monitoring of blood glucose (SMBG), continuous glucose monitoring (CGM), etc.5-8 Depending on the type of diabetes (such as type 1 diabetes [T1D], type 2 diabetes [T2D], and gestational diabetes [GDM]), the extent of disease severity in the patients, and the availability of monitoring systems, the clinicians need to select appropriate glucose monitoring tools.
Several global (such as theAmerican Diabetes Association [ADA] and National Institute for Health and Care Excellence [NICE]) and country-specific guidelines are available to guide both clinicians and patients in choosing the right glucose monitoring metrics. Similarly, in India, there are national recommendations or guidelines provided by the Research Society for the Study of Diabetes in India (RSSDI) and the Indian Council of Medical Research (ICMR).5,9-13 Low adherence to glucose monitoring guidelines is directly related to poor or suboptimal glycemic control 7 and also low medication adherence in patients with diabetes, thus increasing the disease burden in India. 14
In India, adherence to glucose monitoring guidelines can be challenging due to financial constraints, lack of availability of monitoring devices and free glucose monitoring strips (particularly in remote areas), lack of knowledge about appropriate usage of SMBG devices, and unavailability and unaffordability of newer monitoring devices (e.g., CGM) because of cost and lack of awareness.5,15,16 Furthermore, there is a scarcity of specialists to manage this complex disease, limited access to high-tech diagnostic laboratories, thus patients need to undertake extensive burden for consultation and testing, a situation often not feasible at regular intervals. All these factors hinder appropriate diabetes management in India. There is thus an unmet need for healthcare professionals (HCPs) and policymakers to collaborate to address these issues with regular glucose monitoring in patients with diabetes and develop appropriate strategies for the successful implementation of international and national guidelines on glucose monitoring and maintenance of good glycemic control throughout life.
This article aims to discuss the challenges of using glucose monitoring in patients with diabetes in India and provide recommendations to mitigate those challenges. These recommendations will not just help clinicians guide their patients for appropriate testing at regular intervals but also help the patients achieve better glycemic control, better treatment adherence, and improved quality of life (QoL).
Different Glucose Monitoring Tools: Uses, Strengths, and Limitations
Glycated HbA1c
HbA1c represents the average blood-glucose level of patients over the last three months. 7
HbA1c Advantages and Disadvantages
HbA1c testing can prevent short- and long-term complication risks in diabetes, thus regular HbA1c testing can facilitate appropriate diabetes care. 17 Other advantages of this assay include the feasibility of performing irrespective of the prandial state and its pre-analytical and analytical stability. 16 HbA1c testing is found to be more efficient when used along with CGM. 18
However, HbA1c measures blood glucose for the previous three months, so it may have a “delayed effect” in guiding medication dose. 7 Moreover, HbA1c testing does not reveal day-to-day fluctuations of blood-glucose level, thus failing to detect the extent of glycemic variability (GV), hypoglycemia, and hyperglycemia. 18 Additionally, because of different rates of glycation and life span of red blood cells, the level of HbA1c may not manifest glycemic control in some populations. 19 Moreover, in patients with hemoglobinopathies, iron deficiency anemia and hematologic disorders like thalassemia, HbA1c may be an unreliable measure resulting in overdiagnosis or underdiagnosis of diabetes/prediabetes. 16 The ICMR guidelines recommend for HbA1c testing bedone via HbA1c analyzers certified by theNational Glycosylation Standardization Program (NGSP). 13 The lack of NGSP-certified laboratories is the main limitation in India. The reports generated by various laboratories using the same assay technique are not comparable in theabsence of this standardization. 20 The cost burden associated with theHbA1c test (approximate cost ranging from Rs 266 to Rs 476 per test) is another constraint.21,22
Self-monitoring of Blood Glucose (SMBG)
SMBG is the most common form of blood glucose monitoring performed by patients or their caregivers using a glucose meter at home. It is an invasive technique that involves finger pricking with a lancet device, taking small blood droplets in the testing strip, and then inserting it into the glucose meter. Glucose reading is exhibited in the glucose meter within a few seconds and recorded manually in the SMBG chart. These readings allow the patients to adjust their lifestyle and the physicians to adjust treatment.5,23 SMBG can be conducted in a structured way, which is a methodical way of measuring glucose levels daily at predefined times to understand apatient’s blood glucose pattern at regular intervals in a whole day based on which the drug dose is adjusted. This structured SMBG is preferred over unstructured SMBG to understand the blood glucose pattern on a regular basis. 5
Advantages and Disadvantages of SMBG
SMBG is important to treat patients who are on insulin, or hypoglycemic drugs, or experiencing glycemic fluctuations, or not achieving targeted glucose levels. It helps to identify acute hypoglycemia or hyperglycemia and thereby take proper action. 5 The affordability, portability, ease of use, and reasonably accurate data are the advantages of SMBG. 24
However, there are some limitations of SMBG, including theinconvenience of use (particularly carrying aglucose meter while traveling and is a cumbersome method) and pain associated with finger pricking, due to which patients find difficulty in using this daily. Moreover, the cost of the test strips (approximately ₹660 to ₹1245 per 50 strips) and lancets (approximate cost from ₹105 to ₹200 per 100 lancets) particularly for patients paying healthcare out-of-pocket, is another major concern, especially in underdeveloped or developing countries.5,24-26 The other limitations are time required for the fingertip wound to heal, risk of infection, reduced shelf life of test strips, and inaccurate blood glucose readings associated with inappropriate storage of test strips or due to user error.5,24 The possible factors leading to this error could be a lack of proper patient training, the use of an un-calibrated glucose meter, contaminated blood strips, and damaged or expired test strips.7,24 This undesirable glucose meter reading can be demotivating for the patients, leading to SMBG result-related anxiety and depression, thereby affecting their QoL. 5 Additionally, in the market, there are different brands of glucose meters with considerable variation in accuracy and precision. The International Standardization Organization (ISO) has issued guidelines for glucose meter use. According to the updates ISO15197:2013 95% values need to be accurate within ±15 mg/dL for glucose values <100 mg/dL and within ±15% for glucose values ≥100 mg/dL. Glucose meters adhering to ISO 2013 standards should be used for SMBG. 27 Although some research has been conducted to compare standard glucose meters,28,29 there is a lack of sufficient data about the comparison of standard glucose meters in the Indian context. Therefore, there is an unmet need to assess the accuracy and reliability of the standard glucose meters accessible in India.
Furthermore, SMBG is unable to provide real-time data on blood-glucose levels for an entire day and detecting asymptomatic hypoglycemia; this inefficiency of SMBG has paved the way for the use of CGM. 6 Besides, lack of adiabetes care team to provide appropriate assistance and guidance to patients on the proper use of SMBG and medication dose titration is another challenge. 5
Continuous Glucose Monitoring (CGM)
CGM is a simple, minimally invasive technique in which a sensor is inserted subcutaneously that automatically measures glucose concentrations from the interstitial fluid of the patient and helps to understand dynamic changes in glucose levels. The recorder receives a signal every few seconds, and then converts the average recorded signal into a glucose level every one to five minutes and saves it. This level can vary depending on the type of sensor. Patients need to wear the sensor for 7-14 days based on the type of CGM used. CGM technology provides an ambulatory glucose profile (AGP) of the glycemic pattern, which can be evaluated for formulating treatment modalities or dose adjustments for the patients.6,7,23
Based on the device characteristics, there are real-time CGM (rt-CGM), and intermittently scanned CGM (isCGM). 6 The rt-CGM measures glucose levels continuously in real time and may have an alarm system to avoid hyperglycemic and hypoglycemic events. 7 Blood glucose levels can be monitored through SMBG to identify CGM alarms related to false-negative and false-positive results. 7 The isCGM provides close to real-time data by scanning the sensor intermittently at least once every eight hours. 16
Based on the usage, CGM is further classified as personal CGM and professional CGM. Personal CGM device displays real-time glucose levels to the patients and guides them on insulin dosage adjustments and alerts them of extreme glucose excursions. Personal CGM also aids in comprehending the impact of lifestyle and diet on the levels of blood glucose. However, the glucose values generated by professional CGM devices are masked from the patients and only retrospective data are generated, which are used by the HCPs to formulate treatment strategies based on the glycemic pattern. 30
Advantages and Disadvantages of CGM
Evaluating daily blood glucose variations and identifying hyperglycemic and hypoglycemic events, especially nocturnal hypoglycemia is feasible with aCGM system.7,18 CGM is particularly beneficial for patients with T1D and T2D (receiving insulin therapy) with poor glycemic control and can be used along with SMBG for detecting hypoglycemia. CGM can evaluate intra- and inter-day blood GV. 7 CGM facilitates more frequent monitoring and thus can identify more hypoglycemic episodes, post-prandial hyperglycemia, dawn phenomenon, and the Somogyi effect.7,19 The glucose pattern created by CGM helps patients understand the effect of lifestyle modification and medication adherence in reducing GV, thereby facilitating better management of diabetes in insulin-treated patients.7,19 Moreover, the CGM data is beneficial for clinicians to distinguish between hyperglycemia and rebound from hypoglycemia. 7
However, there are several challenges associated with CGM use. rt-CGM needs to be used continuously, which might lead to anxiety and allergy. In children, localized pain, redness, bleeding, swelling, irritation, hindrance of daily activities, and detachment of sensors during overactivity are the fundamental issues. The awareness about the use of CGM devices in children with T1D is very limited in India. 31 The need for recalibrations, periodic replacement of sensors, inconvenience in uploading data for retrospective analysis, cost and variable reimbursement, and lack of HCP training on CGM result interpretation leading to inaccurate measurement are the other limitations.30,32 Moreover, CGM is expensive and thus not accessed frequently by the general population in underdeveloped or developing countries.18,30
Time-in-range (TIR)
The TIR is considered an innovative metric of CGM for assessing glycemic control in patients with T1D and T2D. TIR is the percentage of time the glucose level is within the preferred glycemic range. 8 Reduced TIR can be a predictor of microvascular complications. Time-above-range (TAR) and time-below-range (TBR) can help in assessing treatment efficacy. 33 A higher level of TIR is associated with a lower level of HbA1c. 19 According to Advanced Technologies and Treatments for Diabetes (ATTD) consensus recommendations, the glucose level should be within the target range (70-180 mg/dL) for more than 70% of the time per day (>16 hours) for T1D, T2D, and non-pregnant adults and >50% for older adults and those having ahigher risk for complications.8,18 The target range during pregnancy is 63-140 mg/dL. The treatment modalities should focus on reducing TBR and increasing TIR. 8
Position of Each Monitoring Method in Various Forms of Diabetes
Type 1 Diabetes
SMBG typically plays a vital role in diabetes treatment and several studies established the effectiveness of SMBG in maintaining better glycemic control in diverse types of diabetes. Historically, glucose monitoring was introduced for T1D. The more the number of times glucose is monitored, the longer the chances of complications-free survival. Typically, in T1D, glucose needs to be monitored four to eight times/day for meaningful modifications in behavior. SMBG with a glucose meter used to be the gold standard for several decades until very recently when modern-day CGM devices started demonstrating their superiority. Patients with T1D experience higher GV and have an increased risk of hypoglycemia and diabetic ketoacidosis. SMBG can be beneficial in themanagement of blood-glucose levels in these patients. 5 Moreover, nocturnal hypoglycemia is frequent in these patients. 34 Several randomized controlled trials (RCTs) were conducted on patients with T1D to determine the efficiency of CGM. The DIAMOND and GOLD trials are the major clinical studies on patients with T1D administering multiple insulin injections.35,36 The relevant studies on the use of different glucose monitoring tools are depicted in Table 1.
Relevant Studies on Use of Different Glucose Monitoring Tools in Patients with T1D, T2D, and GDM.
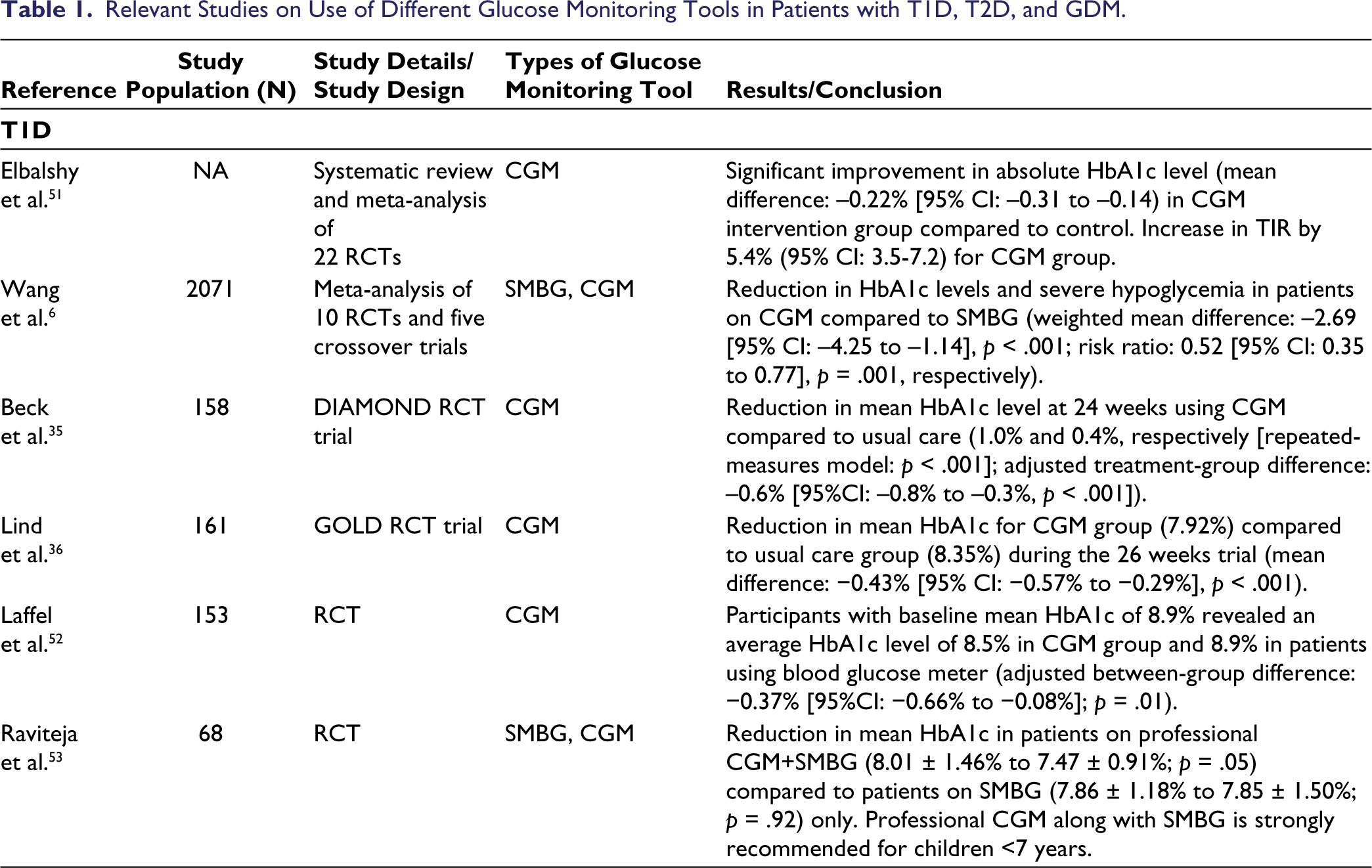
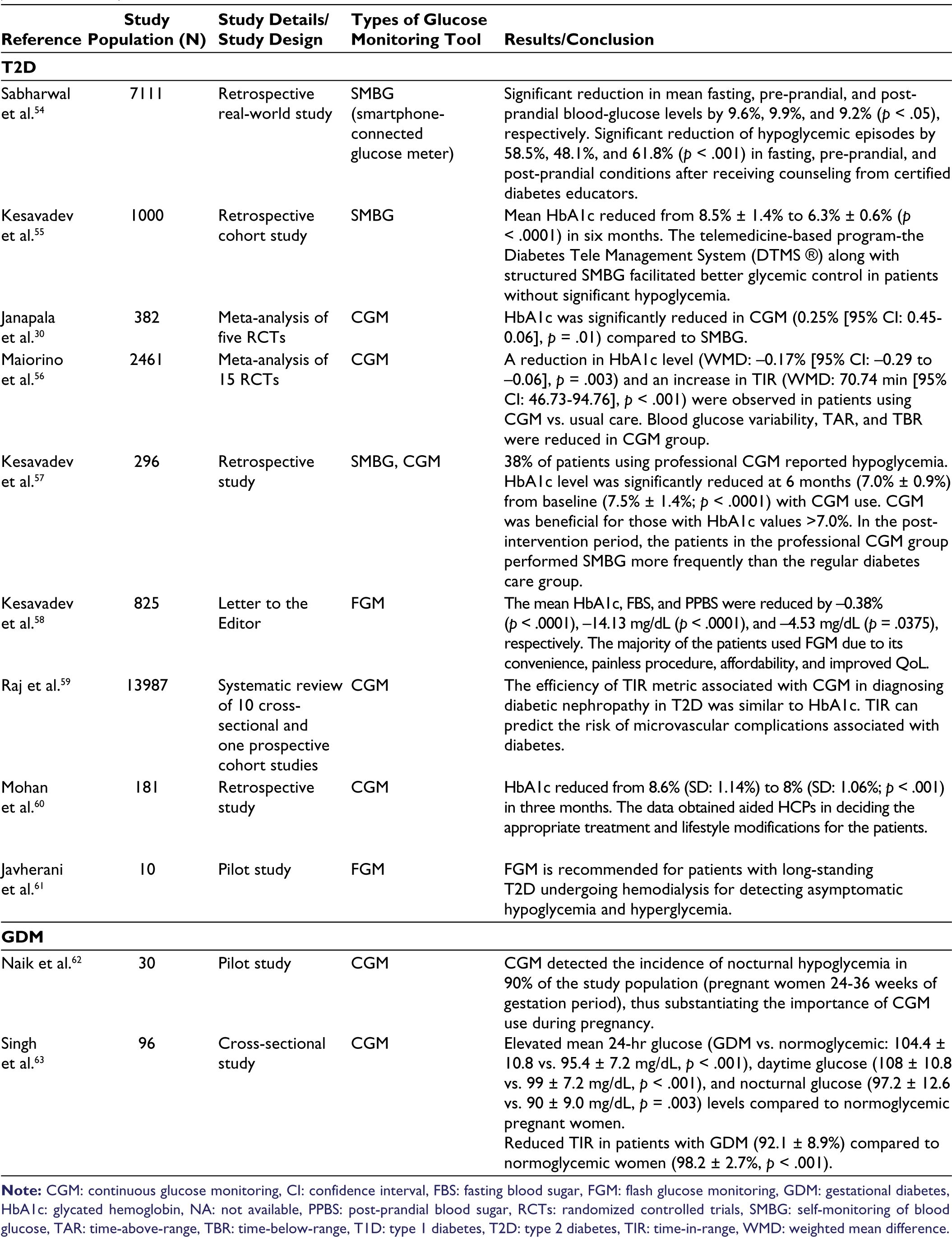
Type 2 Diabetes
SMBG has a crucial role in achieving glycemic control in patients with T2D. 5 Connected glucose meters are gaining popularity by providing a user-friendly display of blood glucose patterns, duration of hypoglycemia, time spent in range, cloud-based storage, capability to send the digital blood glucose logbooks to the doctor’s clinic through email, while also retaining the complete dataset. Additionally, they offer functionalities for users to input information regarding insulin and other medicines, compute insulin-to-carb ratios, and insulin correction factors. As a result, they offer a comprehensive digital resolution for patients with diabetes. 16
CGM serves as a valuable tool in diabetes management for patients with T2D and uncontrolled hyperglycemia. CGM can assess intra-day, inter-day, and post-prandial glucose (PPG) variability (GV), magnitude of glycemic swings, and nocturnal hypoglycemia. Hence, CGM can help lower GV, thereby increasing glycemic control and preventing diabetes-related complications in adult/elderly patients with T2D. Thus, CGM can overcome the key challenge of T2D management, which is GV. 7 Moreover, the advantage of flash glucose monitoring (FGM) in improving glycemic control in patients with T2D (n = 2339) was reported in a multicenter study conducted in the southern and western parts of India (Madurai, Mumbai, Trivandrum, Chennai, Coimbatore, and Belgaum). The patients with T2D had greater reductions in HbA1c values (pre-AGP: 9.2% vs. post-AGP: 8.3%, p < .001) compared to T1D (pre-AGP: 9.6% vs. post-AGP: 8.9%, p < .001). 37 The relevant studies on glucose monitoring tools in patients with T1D and T2D are provided in Table 1. All these studies provide substantial evidence that CGM is beneficial not only in patients with T1D but also in those with T2D.
Gestational Diabetes
CGM (rt-CGM or isCGM) is recommended for all pregnant women with T1D to achieve glycemic targets and enhance neonatal outcomes. In addition, rt-CGM is recommended for pregnant women who are on an insulin regimen but do not have T1D, provided they have reported severe hypoglycemia (with or without impaired hypoglycemia awareness) or unstable glycemic levels. 38 A systematic review of patients with GDM, determined that CGM was more efficient in managing dysglycemia compared to SMBG, as it can detect hyperglycemia (fasting and post-prandial), hypoglycemia, and nocturnal hypoglycemia, thereby concluded that CGM can be considered as a predictor for initiating insulin therapy in pregnant women with GDM. 39
CGM also facilitated the diagnosis of GDM based on clinically relevant glycemic parameters associated with CGM in majority of South Asian pregnant women who were earlier considered normoglycemic. 40 The use of CGM during pregnancy can facilitate the assessment of glucose patterns and insulin dose adjustments.
Research Gaps and Unmet Needs Associated with Glucose Monitoring in Diabetes in India
Lack of general awareness on regular monitoring of glucose levels, appropriate resources, and associated complications of diabetes, are the major challenges in diabetes management in India. Although SMBG is an efficient technique to track glycemic trends, only 24.1% of patients were using SMBG regularly and 75.8% were not knowledgeable enough and were not practicing SMBG appropriately as reported by a cross-sectional study from Chennai, India on 153 patients with T2D. In India, the accuracy of the glucose meter is not usually assessed by the patients and diabetes educators. In hospitals, diabetes educators should be a part of the diabetes management team in order to create awareness and help patients understand the importance of practicing SMBG 15 According to a cross-sectional study, the main reasons for patients with T1D and their family members to refrain from performing SMBG were lack of insurance coverage and the cost related to glucose meter and test strips. Moreover, SMBG is a complex technique, which might be a reason for patients’ non-compliance to SMBG. 41 Another cross-sectional study on patients with T2D (n = 400) in rural Mysuru, India also found non-adherence among patients in performing SMBG, physical activity, and diabetic foot care due to alack of knowledge on blood glucose control and available resources. This emphasized the need to identify these patients and counsel them for performing SMBG at their homes. The study also suggested the need for community-based diabetes education programs to promote diabetes self-care practices. 42
CGM is another important glucose monitoring tool. It is essential that patients have knowledge of CGM and are satisfied with its use. 31 Diabetes education programs should be organized for patients and physicians on CGM data analysis with more focus on the interpretation of indices rather than the technical aspects of CGM for effective diabetes management. 8 Improving the accuracy, approvals for using CGM for insulin dose adjustments, and automated interpretation of results can help in wider acceptance of CGM. 32
The first-line therapy for T2D in pregnancy is insulin and its requirement increases from the first trimester till delivery. Pre- and post-meal glucose monitoring helps to achieve glycemic control in these patients. Assessing post-dinner blood-glucose levels is particularly essential due to the diverse dietary habits among Indians. The lack of adequate data on insulin dose, frequency, and the effect of various foods might affect glucose management in pregnant women with T2D. 43
Family support also plays a vital role in motivating the patients to regularly monitor blood glucose and maintain a healthy diet thus obtaining optimal glycemic control. 31 This emphasizes the need for awareness programs or conversations focused on the importance of glucose monitoring in maintaining optimal glycemic control among the family members of patients with diabetes and the HCPs.31,44
The previously published RSSDI recommendations (2018, 2022) for different glucose monitoring techniques are shown in Table 2.
General Recommendations by RSSDI for Different Glucose Monitoring Techniques.
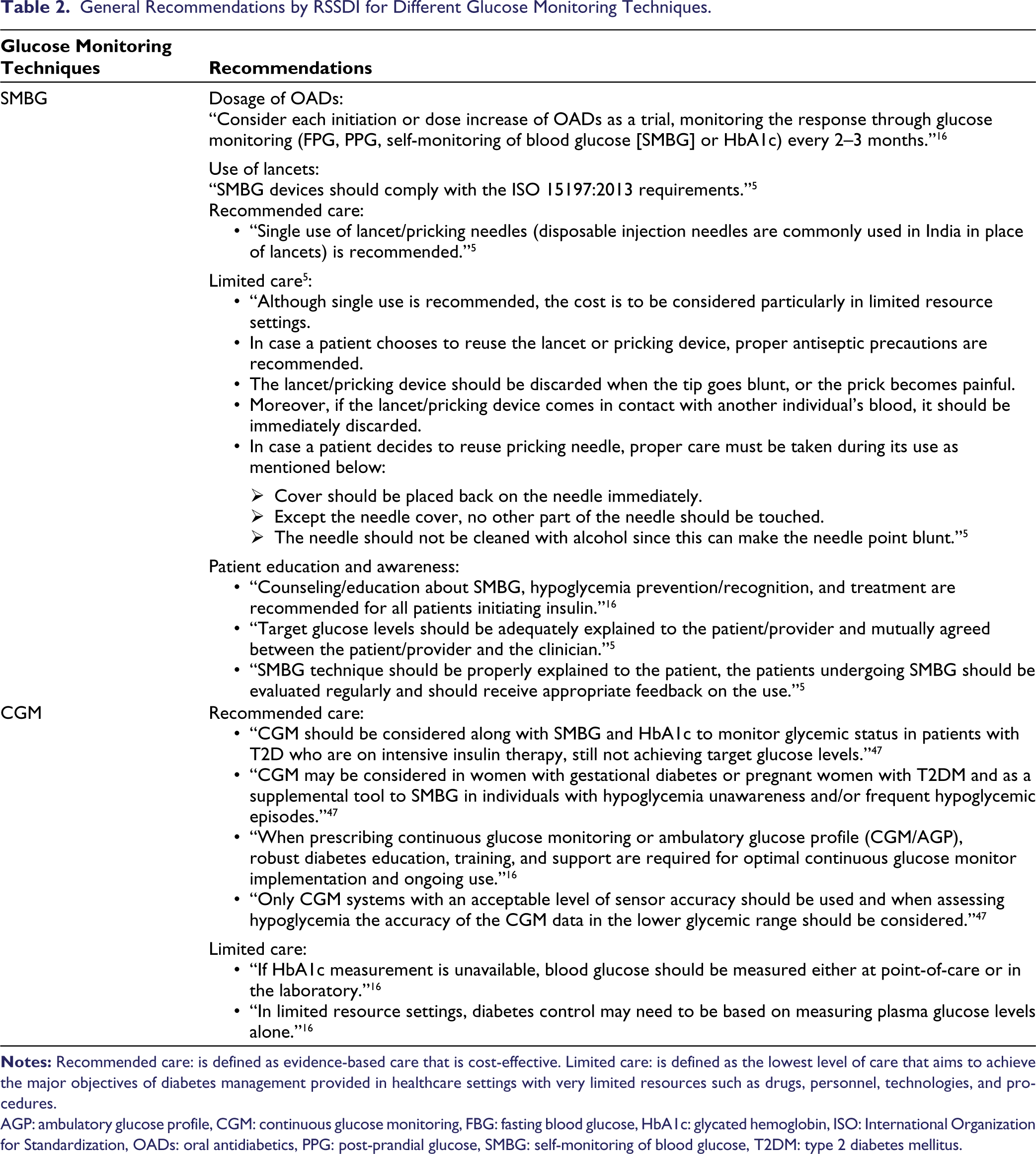

AGP: ambulatory glucose profile, CGM: continuous glucose monitoring, FBG: fasting blood glucose, HbA1c: glycated hemoglobin, ISO: International Organization for Standardization, OADs: oral antidiabetics, PPG: post-prandial glucose, SMBG: self-monitoring of blood glucose, T2DM: type 2 diabetes mellitus.
Ideal Frequency of Each Monitoring Method in Diabetes
As per RSSDI recommendations, the intensity and frequency of SMBG should be tailored on acase-by-case basis. Intensive/regular SMBG should be performed in patients with a history of hypoglycemia unawareness, on multiple insulin injections, GDM on insulin therapy, and with poor glycemic control on multiple oral antidiabetic drugs or basal insulin. For patients on insulin therapy, SMBG should be performed every time insulin is administered. SMBG is recommended ≥3 times/day-during bedtime, pre-meals, post-meals, and before exercise for patients on intensive insulin therapy. 5 In adults and children with T1D who are using an insulin pump and injections, a strong association was observed between higher SMBG frequency and lower HbA1c level, indicating the achievement of improved glycemic control with increased frequency of SMBG. 45 Additionally, an improvement in HbA1c level was observed in obese patients with T2D who frequently performed SMBG (5 times/day for 12 weeks). 46 Pregnant women with diabetes who are on insulin therapy should perform SMBG on a daily or at least weekly basis. Ideally, one should conduct seven tests/day (three before and three after each meal and one test at 3 am). If this is not feasible, one fasting test and three tests after breakfast, lunch, and dinner should be conducted daily. As the pregnancy progresses, the testing frequency can be customized and reduced to twice or thrice a week. 5
The RSSDI recommends that CGM should be used for 14 days to assess the TIR, for which at least 70% data is required. 16 Similarly, the ICMR guidelines also recommend CGM for patients with T1D who are motivated and committed to wear the device for at least 70% of the time as this can evaluate the improvement in glycemic control. CGM can be used in conditions of recurrent hypoglycemia and hypoglycemia unawareness in patients with T1D and T2D. Under such circumstances, CGM for five to seven days or CGM for 14 days is recommended. The guidelines also recommend the use of TIR along with CGM in patients with T1D.12,13
RSSDI recommendations on frequency/timing of different glucose monitoring methods are depicted in Table 3.
Recommended Care and Limited Care Recommendations by RSSDI Experts for Frequency/Timing of Various Glucose Monitoring Techniques.



CGM: continuous glucose monitoring, DCCT: Diabetes Control and Complications Tria, DM: diabetes mellitus, FBG: fasting blood glucose, GDM: gestational diabetes, HbA1c: glycated hemoglobin, OADs: oral antidiabetics, SMBG: self-monitoring of blood glucose, SU: sulphonyl urease, T1D: type 1 diabetes, T2D: type 2 diabetes, TIR: time-in-range.
Expert Panel Recommendations on Glucose Monitoring in Special Settings
For Patients Undergoing Fasting
Monitoring blood-glucose levels regularly during fasting (especially in those who are unwell) using SMBG is essential to avoid hypoglycemia. 16 According to RSSDI recommendations, SMBG should be performed during fasting as it is beneficial in deciding drug dosage and diabetes management. Moreover, individualized education is important during Ramadan so that the patients undergoing Ramadan fasting will be able to modify their diabetes treatment plan, perform SMBG (at least two times/day), and be aware of the hypoglycemic symptoms compared to patients following standard diabetes management strategies.16,47 It has been found that during Navratri and Durga pujas, patients with well-controlled diabetes who continue to take medications and perform SMBG have a lower risk of diabetes-associated complications than those who do not perform SMBG regularly. Patients can maintain an SMBG chart during the fasting period for assessment of GV. Auditing this chart by consulting physicians can be beneficial in developing a treatment plan. 48
For Patients on Basal Insulin and Patients on Premix Insulin or Basal-bolus
Recommended care for patients on basal insulin includes testing of daily fasting glucose levels. In settings with limited healthcare resources (limited access to care), fasting glucose level checks can conducted less frequently, either twice a week or once every three days. Post-prandial glucose levels should be modified only after correcting fasting blood-glucose levels. 5
For patients undergoing premix insulin or basal-bolus therapy, it is advisable to conduct three pre-meal (including fasting) and three post-meal tests on alternate days until the desired HbA1c and blood-glucose levels are achieved. Less frequent testing can be performed after achieving target levels. 5
For Patients with End-stage Organ Disease
Patients with end-stage organ disease usually receive daily multiple insulin doses or remain on insulin infusions. However, the frequency and timing of SMBG should be tailored to the specific needs of these patients and increased monitoring may be necessary depending on patient’s clinical condition. 5
For Elderly Patients
Hypoglycemia is a major concern in elderly patients and should be determined. 47 Pre-prandial glucose values are important in ascertaining hypoglycemia. The RSSDI expert panel suggests that, during the initial phase, patients in this category should perform SMBG once daily (at varying times), and gradually reduce it to two to three times per week. Additionally, it is important to provide education and training on SMBG to family members so that they can effectively support these patients. 5
For Patients in Intensive Care Unit (ICU)/Critical Care Unit/Hospital Settings
The RSSDI recommends using point‑of‑care capillary blood glucose meters for monitoring glycemic levels in hospitalized patients with diabetes. To ensure accuracy of results, it is essential to use glucose meters adhering to the latest ISO standards. For critically ill patients with T2D who are on intravenous insulin infusions, it is advisable to employ point-of-care blood glucose meters at regular intervals (every 30 minutes to two hours) to prevent hypoglycemia. CGM use is recommended in critically ill patients as it measures the extent of GV and blood glucose patterns and thus facilitates safe and precise insulin infusion dosing and reduces hypoglycemic risks. 47
Glucose Monitoring in COVID-19 Scenario
The RSSDI recommends frequent monitoring of blood-glucose levels (at least every four hours including nighttime) in patients with T1D and COVID-19. Ketones need to be checked more than twice in a row if blood-glucose levels are >240 mg/dL. If the patient is experiencing hypoglycemia (blood glucose is <70 mg/dL), 15 g of simple carbohydrates should be consumed, then blood-glucose levels should be checked every 15 minutes and the steps need to be repeated until it is stabilized. 49 A blood glucose meter or alternatively rt-CGM should be used to screen hyperglycemia in patients admitted to hospital with COVID-19. Glucose monitoring must be continued during the entire course of COVID-19 treatment to reduce the risk of hyperglycemia. 16 A virtual COVID inpatient model from India showed thesuccessful treatment of hundreds of patients using telemedicine and remote monitoring of all vitals including glucose.50
Conclusion
Outcomes of diabetes treatment remain poor in India due to uncontrolled glucose levels. This is attributed to the lack of implementation of treatment strategies owing to intense fear of hypoglycemia. The fear of hypoglycemia should be eliminated, and patients can safely reach glycemic targets with proper utilization of monitoring devices. Recommendations for customizing different glucose monitoring tools have been provided by the experts of RSSDI to popularize glucose monitoring techniques among patients with diabetes in India, to improve glycemic control and proper management of diabetes. However, implementation of these recommendations by physicians in their clinical practice requires some essential steps to be undertaken by the government, healthcare policymakers, and pharmaceutical companies. These should include popularizing RSSDI guidelines among general practitioners and diabetes educators, developing a regulatory strategy to ensure that only reliable glucose meters are marketed, introducing certain SMBG devices that can reduce/eliminate pain associated with pricking but at the same time cost-effective, and finally to develop stringent policies to reduce the cost of reliable CGM sensors so that the common people will have access to CGM.
Footnotes
Acknowledgements
Writing assistance was provided by Somdatta Mukherjee from Turacoz Healthcare Solutions (
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Extending Working Committee
Dr Vasanth Kumar, Dr Rakesh Sahay, Dr Sujoy Ghosh, Dr L Sreenivasa Murthy, Dr Pratap Jethwani, Dr Jugal Sharma, Dr J Aravinda, Dr NK Singh, Dr M Shunmugavelu, Dr Amit Gupta, Dr Rakesh Parikh, Dr Anil Virmani, Dr Anuj Maheshwari, Dr Vijay Vishwanathan, Dr Sunil Gupta.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
