Abstract
Tuberous sclerosis is primarily a neurocutaneous autosomal dominant disorder that affects the skin, kidneys, eyes, heart, lungs, bones, and central nervous system. It encompasses the triad of adenoma sebaceum, mental retardation, and epilepsy. Because of their cosmetic deformity, patients with adenoma sebaceum and normal mental development may experience severe psychological and social issues. Adenoma sebaceum fibroplasias have been treated with a variety of methods, including electrocoagulation, electrodesiccation and curettage, liquid nitrogen freezing, excision, and dermabrasion. There is not a single modality that is particularly effective. In this study, we describe the effectiveness of dermabrasion as a treatment for adenoma sebaceum. This study was conducted in the department of plastic surgery in a tertiary care center in North India. Departmental ethical clearance and consent from the subject were obtained. The process was carried out while under general anesthesia. All of the tuberous lesions on the forehead, cheeks, and chin were abraded using mechanical dermabrasion equipment. Following surgery, the treated areas recovered without skin discoloration or scars. The procedure was both cosmetically pleasing and efficacious. Mechanical dermabrasion is an efficient and safe remedy for treating massive adenoma sebaceum of the face, even though we cannot permanently clear these lesions due to their nature. A recurrence of the angiofibromas may require recurrent dermabrasion. The quality of life can be enhanced with their social perspective and physical appearance.
Introduction
A hereditary condition called tuberous sclerosis primarily presents as cutaneous, visceral and brain tumours. This neurocutaneous autosomal dominant condition affects the kidney, skin and central nervous system, eyes, heart, lungs and bones. Seldom does it affect the endocrine system. It includes the trio of epilepsy, mental retardation and adenoma sebaceum. In 60%–70% of cases, cutaneous lesions manifest as adenoma sebaceum, hypopigmented macules (ash-leaf spots), periungual fibromata and shagreen patches. Because of their cosmetic deformity, patients with normal mental development and adenoma sebaceum may have significant psychological and social issues. For these people, effective therapy is crucial. Adenoma sebaceum fibroplasias have been treated with a variety of methods, including electrocoagulation, electrodesiccation and curettage, liquid nitrogen freezing, excision and dermabrasion. There is not a single modality that is particularly effective. In this study, we describe the effectiveness of dermabrasion as a treatment for adenoma sebaceum.
Case Report
A 25-year-old Indian male presented to the outpatient clinic with a 5-year history of gradually increasing multiple facial papules localised to the central face, predominantly over the nose, malar eminences and chin. The lesions were asymptomatic (non-itchy and non-painful) but were a source of significant cosmetic concern.
The patient first noticed a few small, flesh-coloured papules on the nasal ala approximately 5 years earlier. These lesions gradually increased in both number and size, eventually spreading to involve the nasolabial folds, malar eminences and perioral region. He observed that the lesions became more noticeable following sun exposure. There was no history of bleeding, discharge or tenderness, and he had not sought or received any prior treatment.
On cutaneous examination, multiple symmetrically distributed, firm brown to hyperpigmented papules measuring 1–5 mm were seen, predominantly over the nasolabial folds, cheeks and chin, creating a butterfly-shaped distribution across the mid-face. Unlike the erythematous appearance often described in lighter skin types, in this patient, the lesions were predominantly hyperpigmented with occasional telangiectatic changes. No excoriations, ulcerations or secondary infections were noted (Figure 1). Systemic examination was unremarkable, and there was no significant family history of similar complaints.
Pre-operative Clinical Photographs.
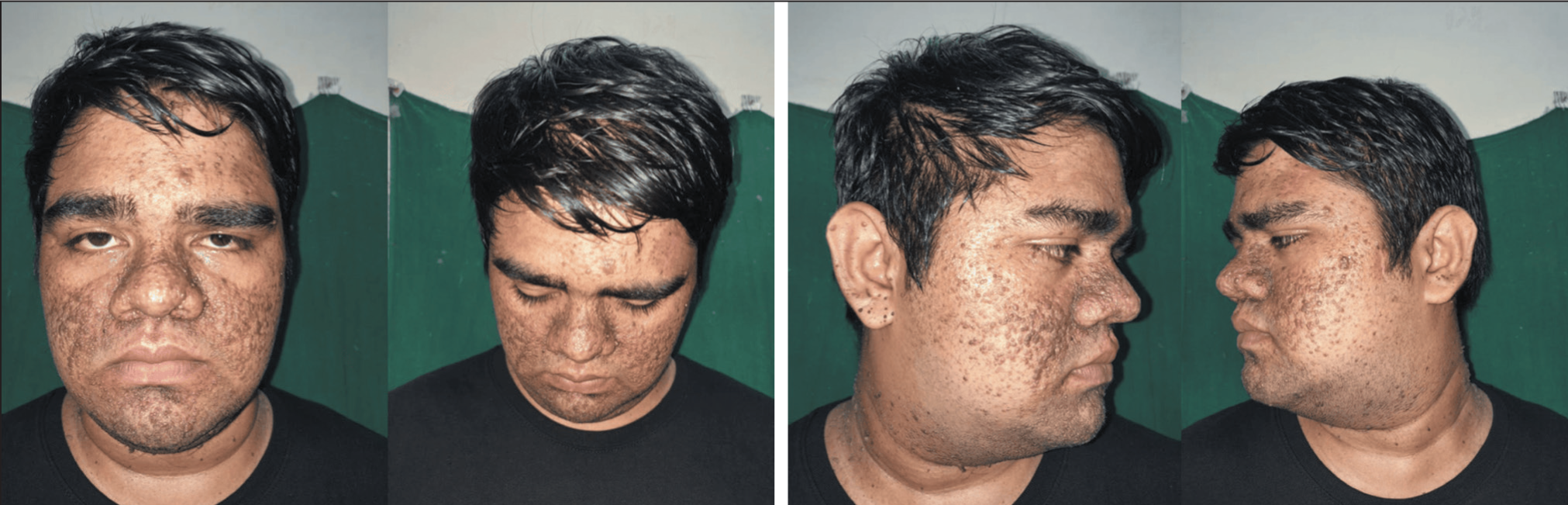
Based on the clinical history and examination, the patient was diagnosed with facial angiofibromas associated with tuberous sclerosis complex. In this Indian patient (Fitzpatrick type IV–V), the lesions demonstrated a brown to hyperpigmented appearance rather than the classical reddish hue typically described in lighter skin types. This variation highlights the importance of recognising differences in presentation in skin of colour, where reduced erythema can make diagnosis less straightforward.
Considering the cosmetic disfigurement and the benign but progressive nature of the lesions, the patient underwent dermabrasion under general anaesthesia. All lesions over the forehead, cheeks and chin were abraded using a hand-held dermabrader with a diamond fraise, down to the superficial dermis (endpoint: pinpoint bleeding). Adequate hemostasis was achieved, and the treated area was dressed with sterile paraffin gauze. The patient was discharged on post-operative day 2 with advice on wound care, emollient use and strict photoprotection. Weekly outpatient reviews were conducted.
By the third post-operative week, as shown in the post-operative clinical photographs (Figure 2), the treated areas had healed well with complete epithelialisation. The facial contour appeared smoother with flattening of the angiofibromas and a marked cosmetic improvement. In this Indian patient (Fitzpatrick type IV–V), the healing phase was notable for post-inflammatory hyperpigmentation, a common outcome in skin of colour following dermabrasion. At the six-week follow-up, pigmentation changes had begun to fade gradually. The patient reported high satisfaction with the aesthetic outcome. At three months, the results remained stable, with no evidence of lesion recurrence. The patient was counselled about the chronic nature of tuberous sclerosis, risk of recurrence and the need for long-term follow-up.
Post-operative Pictures at Three-week Follow-up.
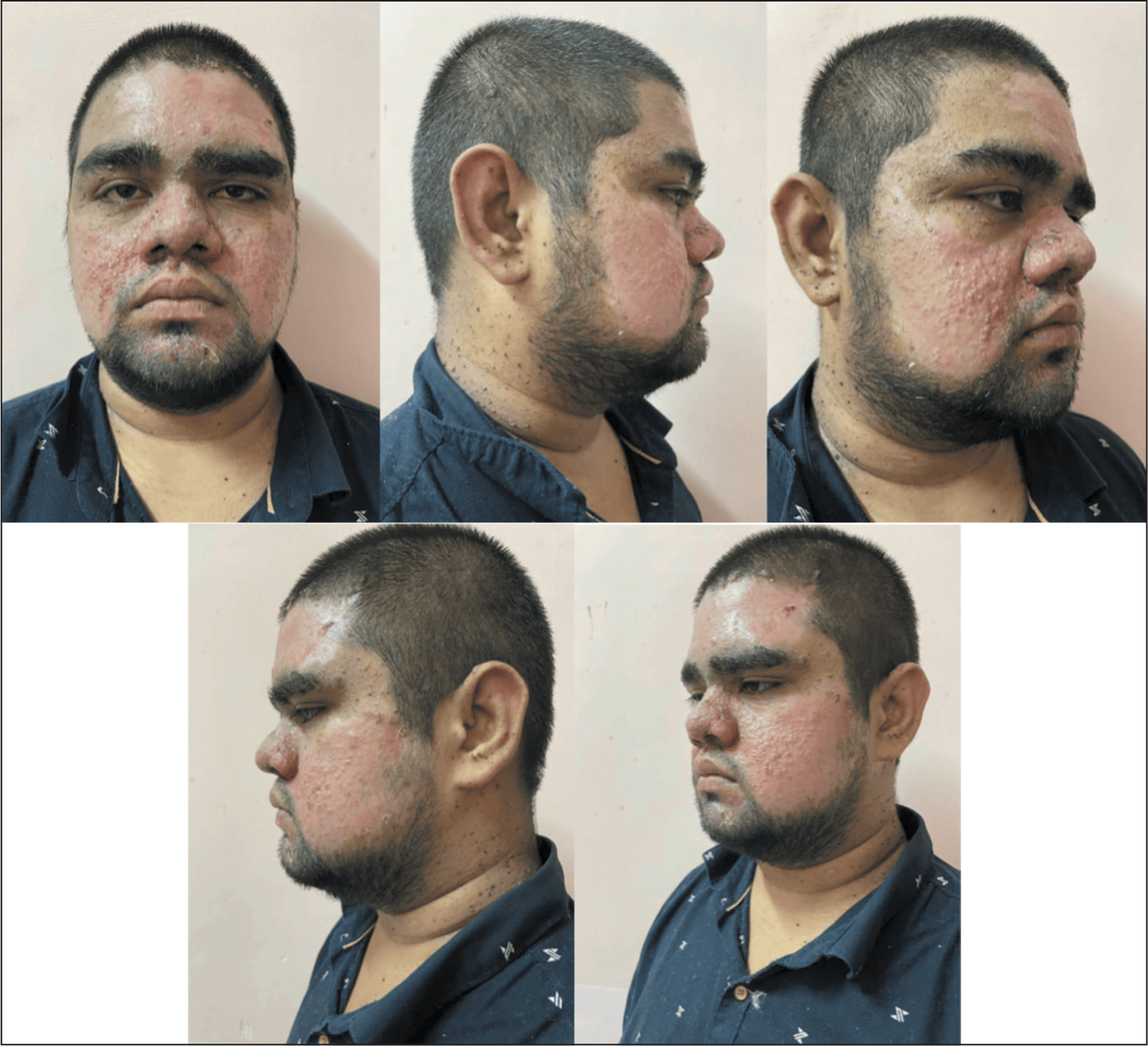
Discussion
Adenoma sebaceum is a misnomer of a term. Adenoma sebaceum always had some degree of vascular hypertrophy, according to Pringle’s 1890 description of the condition. 1 However, he erroneously concluded that this hypertrophy of the sebaceous glands was the essential component of these tumours; these lesions are angiofibromas, which are hamartomas made of fibrous and vascular tissues. 2 These lesions can sometimes be seen at birth and are typically noticeable by early childhood and become conspicuous very quickly during puberty. Adenoma sebaceum can present with a variety of clinical characteristics, including pinpoint papules to nodules, flesh-coloured, pink or bright red, and smooth, shiny surfaces. They affect the butterfly region of the face, primarily the nasolabial folds, and are predominantly symmetrical and bilateral. They tend to spare the upper lip and are less common on the chin and forehead. 3
A review of the literature indicated that these tumours can be treated using a variety of techniques.
There have been successful reports of attempts at liquid nitrogen cryosurgery. Although there is a significant chance of scarring and pigmentary issues, electrolysis and cautery have been done. With varying degrees of success, chemical peels and oral 13-cis retinoic acid were used. For these kinds of vascular ectasias, lasers—including argon, carbon dioxide (with or without flash scanning), potassium titanyl phosphate, copper vapour and pulsed-dye—were advised as the preferred method of treatment. There were several problems with lasers: This treatment frequently necessitates general anaesthesia, particularly when large areas are involved; scarring and pigmentation are common complications; multiple sessions and lengthy operating times are required, particularly with the argon laser, which is known to penetrate and vaporise only a few millimetres of tissue at a time; and the additional costs.4–13
Numerous authors have suggested dermabrasion as a therapy option; the results have been excellent, although there are concerns about recurrence. Using dermabrasion to treat adenoma sebaceum lesions is an effective treatment. 14 These are located in the dermis and can be safely abraded without leaving scars or endangering the skin’s regeneration processes. Under general anaesthesia, the method can treat the entire face in a single session, requires little time during surgery and is cost-effective. However, the possibility of disease transmission by aerosol particles is a concern raised by this therapy approach. Few long-term results of this approach have been reported; these indicate a varying frequency of recurrences and the need for additional treatment. 15
A recurrence of the angiofibromas may require repeat dermabrasion. The quality of life can be enhanced in patients with tuberous sclerosis with meticulous dermabrasion of the adenoma sebaceum, as the above cases illustrate. It enhances their social perspective and physical appearance.
Conclusion
Although it is difficult to completely eradicate these lesions because of their nature, mechanical dermabrasion is a safe and effective treatment for large adenoma sebaceum of the face. A recurrence of the angiofibromas may require recurrent dermabrasion. The quality of life can be enhanced with their social perspective and physical appearance.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
