Abstract
Background
Myofascial pain dysfunction syndrome (MPDS) is a common musculoskeletal cause of orofacial pain and may occasionally mimic early neuropathic or neurological conditions, posing a diagnostic challenge for dental practitioners.
Case Presentation
A 70-year-old edentulous female presented with right-sided orofacial pain and was initially diagnosed with MPDS based on clinical findings. Despite conservative management, she subsequently developed acute unilateral facial paralysis consistent with Bell’s palsy. Temporomandibular joint imaging was unremarkable; however, further evaluation with magnetic resonance imaging (MRI) and computed tomography (CT) of the brain revealed a well-defined calcified extra-axial lesion measuring 1.7 × 1.4 cm at the planum sphenoidale and left olfactory groove, suggestive of a calcified meningioma.
Conclusion
This case highlights the diagnostic challenge posed by overlapping musculoskeletal and neurological symptoms in orofacial pain conditions. The presence of neurological red flag signs such as progressive facial weakness, persistent or worsening pain, sensory disturbances, or inadequate response to conventional therapy should alert dental practitioners to the need for prompt neurological referral and advanced neuroimaging to exclude underlying intracranial pathology.
Keywords
Introduction
Orofacial pain encompasses a wide spectrum of conditions, ranging from odontogenic and musculoskeletal disorders to neuropathic and central nervous system pathologies. Myofascial pain dysfunction syndrome (MPDS) is one of the most common non-odontogenic causes of facial pain and constitutes a major subset of temporomandibular disorders (TMDs). It is characterized by pain arising from the masticatory muscles, often associated with trigger points, muscle tenderness, and functional discomfort during mandibular movements.1–3
Bell’s palsy is an acute idiopathic lower motor neuron facial nerve paralysis and remains a diagnosis of exclusion. Although facial weakness is its hallmark feature, a subset of patients experience prodromal orofacial or periauricular pain prior to the onset of paralysis, which may lead to diagnostic confusion.4, 5 The coexistence or sequential presentation of MPDS-like symptoms followed by Bell’s palsy is uncommon and may delay appropriate diagnosis and management.
The incidental detection of intracranial lesions such as meningiomas during neuroimaging further complicates clinical interpretation. While most incidental meningiomas are asymptomatic and slow-growing, their presence necessitates careful clinico-radiological correlation to establish clinical relevance.6, 7 This case report describes an unusual diagnostic sequence of MPDS preceding Bell’s palsy with an incidental calcified meningioma, and highlights the importance of vigilance and multidisciplinary evaluation.
Case Report
A 70-year-old completely edentulous female presented to the Department of Oral Medicine and Radiology in May 2025 with a chief complaint of continuous, moderate-intensity pain localized to the right mandibular and preauricular regions. The pain was rated seven on the visual analog scale and radiated to the temporal and auricular areas. There was no history of trauma, fever, vesicular eruptions, or previous neurological illness.
Clinical examination revealed localized tenderness of the right masticatory muscles, particularly the masseter and temporalis, with identifiable trigger points. Mandibular movements were within functional limits but elicited discomfort. There was no deviation in mouth opening, joint sounds, or restriction of movement. Cranial nerve examination was normal at this stage. Based on these findings, a provisional diagnosis of MPDS was made. Differential diagnoses such as trigeminal neuralgia (absence of paroxysmal lancinating pain and trigger zones), temporomandibular joint degenerative disease (no crepitus, limitation, or radiographic changes), and cerebrovascular accident (absence of focal neurological deficits) were considered unlikely at presentation.
The patient was prescribed Flexon-MR (Ibuprofen 400 mg + Chlorzoxazone 250 mg) thrice daily for 7 days, along with conservative measures, including warm compresses, jaw exercises, physiotherapy, a soft diet, and reassurance. The patient did not report for the scheduled follow-up and returned after 2 weeks with worsening symptoms. On re-evaluation, pain severity was reassessed using the visual analog scale, and progression of symptoms was noted.
On re-evaluation, she exhibited acute right-sided facial weakness with facial drooping, loss of the nasolabial fold, lagophthalmos, and inability to raise the right eyebrow or smile symmetrically (Figure 1). Based on clinical findings, the facial paralysis was graded as House–Brackmann grade IV. She also reported tinnitus, diminished hearing on the right side, intermittent imbalance, and a change in pain quality to sharp, electric shock-like sensations, triggered by minimal tactile stimuli, suggestive of neuropathic involvement. These findings represented neurological red flag features, including progressive facial weakness, sensory disturbances, otological symptoms, imbalance, and changes in pain quality, warranting prompt neurological evaluation.
Clinical Photograph Showing Right-sided Facial Asymmetry with Incomplete Eye Closure (Lagophthalmos) and Loss of Nasolabial Fold, Consistent with Lower Motor Neuron Facial Nerve Palsy.

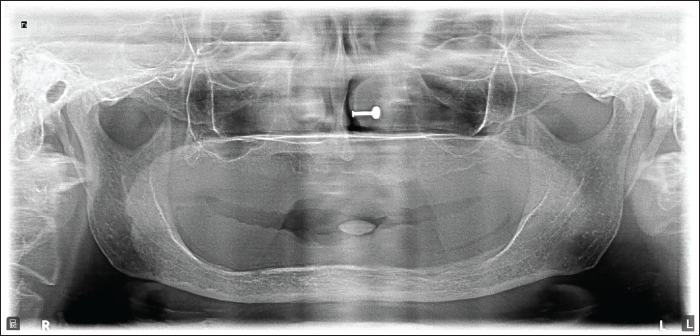
The patient was referred for neurological evaluation. Screening for metabolic causes revealed no history of diabetes mellitus, and random blood glucose levels were within normal limits. There were no clinical features suggestive of active herpes simplex or herpes zoster infection. A panoramic radiograph showed no abnormalities of the maxillofacial bones or temporomandibular joints (Figure 2). Given the evolving neurological signs, advanced neuroimaging was advised.
Panoramic Radiograph (Orthopantomogram (OPG)) Showing No Significant Abnormalities in the Jaws or Temporomandibular Joint (TMJ) Region.
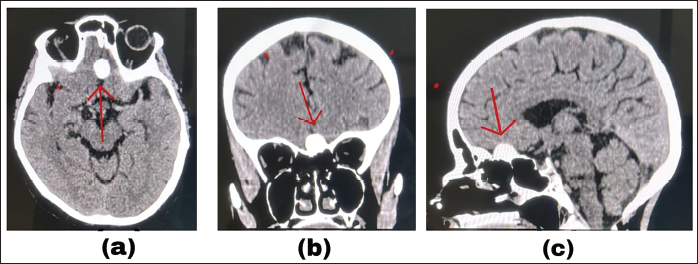
Magnetic resonance imaging (MRI) and computed tomography (CT) of the brain, performed using a stroke protocol with time-of-flight sequences, revealed a well-defined, calcified extra-axial lesion measuring 1.7 × 1.4 cm at the planum sphenoidale and left olfactory groove, radiologically consistent with a calcified meningioma (Figure 3A–3C). There was no perilesional edema or mass effect. Mild cerebral atrophy and punctate fluid-attenuated inversion recovery (FLAIR) hyperintensities were noted in the left frontal lobe. Neurology consultation concluded a diagnosis of Bell’s palsy with an incidental intracranial meningioma. The patient was advised oral corticosteroid therapy along with eye lubrication, protective eye patching, and facial physiotherapy as part of conservative management for Bell’s palsy. Conservative management for facial palsy and periodic radiological surveillance for the meningioma were advised. Clinical timeline: Day 0: The patient presented with right-sided orofacial pain and was diagnosed with MPDS. Day 14: The patient reported worsening pain with the onset of unilateral facial weakness, following which neurological consultation and neuroimaging were undertaken.
Composite Neuroimaging Showing a Well-circumscribed Calcified Extra-axial Lesion at the Planum Sphenoidale and Left Olfactory Groove: (A) Axial Non-contrast Computed Tomography (CT) Image, (B) Coronal T1-weighted Magnetic Resonance Imaging (MRI) View, and (C) Sagittal T1-weighted MRI View.
Discussion
MPDS is a common subtype of TMDs characterized by pain originating from the masticatory muscles rather than the temporomandibular joint itself. It is frequently associated with occlusal imbalance, parafunctional habits, psychological stress, and loss of posterior dental support, particularly in elderly and edentulous individuals.1, 3, 8 Clinically, MPDS presents with dull, aching pain, muscle tenderness, trigger points, and pain aggravated by mandibular movements, with a normal neurological examination. These features supported the initial diagnosis in the present case.
Orofacial pain poses a significant diagnostic challenge due to the overlap between musculoskeletal and neurological conditions. The appearance of sharp or electric shock–like pain, sensory disturbances, tinnitus, imbalance, or facial asymmetry is atypical for MPDS and should prompt reconsideration of the diagnosis.2, 9 Bell’s palsy is an acute idiopathic lower motor neuron facial nerve paralysis and remains a diagnosis of exclusion. Prodromal orofacial or periauricular pain preceding facial weakness has been reported in 11%–18% of patients and may mimic temporomandibular or myofascial disorders.4, 5 Recent clinical guidelines emphasize that atypical pain patterns or progressive neurological symptoms warrant prompt reassessment and neuroimaging to avoid misdiagnosis, as routine MRI may reveal underlying abnormalities even in apparently typical cases of Bell’s palsy.10, 11
The differential diagnoses considered included trigeminal neuralgia, temporomandibular joint degenerative disease, and cerebrovascular accident. Trigeminal neuralgia was excluded due to the absence of paroxysmal lancinating pain, trigger zones, and refractory response patterns. Temporomandibular joint degenerative disease was considered unlikely due to the absence of crepitus, joint restriction, deviation, or radiographic changes. Cerebrovascular accident was ruled out based on the lack of upper motor neuron signs, preserved limb function, and the absence of acute ischemic changes on neuroimaging. The subsequent development of unilateral lower motor neuron facial weakness with House–Brackmann grade IV severity supported the diagnosis of Bell’s palsy.
The progression from localized myofascial pain to overt facial nerve paralysis underscores the importance of close follow-up and reassessment when symptoms worsen or fail to respond to conservative therapy. Similar case reports have described patients in whom Bell’s palsy was initially misdiagnosed as temporomandibular or myofascial pain disorders due to prodromal orofacial pain. These reports highlight that early facial nerve involvement may present with pain before overt paralysis, leading to diagnostic delay. The present case aligns with such observations and reinforces the need for vigilance when managing atypical or progressive orofacial pain.12, 13
Neuroimaging in the present case revealed a calcified meningioma located in the anterior cranial fossa. Meningiomas are the most common benign intracranial tumors and are frequently detected incidentally, particularly in elderly individuals undergoing imaging for unrelated neurological complaints.6, 7, 14 The lesion was considered non-causative in this case due to its anterior cranial fossa location, absence of mass effect, perilesional edema, or brainstem compression, and lack of anatomical proximity to the facial nerve nucleus or its intracranial course. Additionally, the facial paralysis occurred contralateral to the lesion, further supporting an incidental rather than an etiological association.15, 16
A neurology consultation was obtained, and after comprehensive clinical–radiological correlation, neurosurgical intervention was deemed unnecessary. The lesion was classified as an incidental, asymptomatic meningioma, and conservative management with periodic radiological surveillance was advised. Current guidelines recommend observation with serial imaging for small, calcified, asymptomatic meningiomas without evidence of growth or neurological compromise, particularly in elderly patients.14–16 Regular follow-up is essential to monitor for interval growth or the emergence of new neurological symptoms, which would warrant reconsideration of surgical or radiosurgical management. 14
This case highlights the limitations of panoramic radiography in evaluating atypical or progressive orofacial pain, as it cannot detect intracranial pathology. Advanced neuroimaging should be considered when neurological features accompany orofacial pain. Overall, the report underscores the importance of multidisciplinary evaluation and vigilant reassessment of evolving symptoms.
Conclusion
This case demonstrates the diagnostic challenge posed by overlapping musculoskeletal and neurological causes of orofacial pain. Prodromal pain in Bell’s palsy may mimic MPDS, particularly in elderly patients, leading to an initial misdiagnosis. Careful clinical assessment, recognition of atypical features, and timely neuroimaging are crucial for accurate diagnosis, while incidental intracranial findings should be interpreted cautiously with multidisciplinary input.
Footnotes
Authors’ Contribution
Dr. Jyoti C: Conceptualized the case, reviewed clinical findings, wrote and edited the manuscript.
Dr. Praveenkumar Ramdurg: Assisted in literature review, contributed to manuscript drafting, formatting, and final review.
Dr. Naveen Srinivas and Dr. Harshita K Arabbi: Read and approved the final manuscript.
All authors read and approved the final manuscript.
Data Availability Statement
The dataset generated and/or analyzed during the current study is available from the corresponding author upon reasonable request.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval Institutional Statement
The patient’s identity has been adequately anonymized, and the study complies with institutional ethical standards and journal guidelines for case reports.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
Written informed consent was obtained from the patient for publication of this case report and associated images.
