Abstract
Background
Monolithic zirconia is increasingly used in dental restorations for its high strength and biocompatibility. However, the impact of surface treatments—glazing, polishing, and air abrasion—on its flexural strength remains unclear due to inconsistent findings in existing studies.
Methods
Thirty zirconia specimens (25 × 6 × 3 mm) were milled from SuperfectZir disks using CAD-CAM technology and sintered at 1,350°C–1,500°C. Specimens were randomly assigned to three groups (n = 10). Group A was glazed at 790°C, Group B was subjected to grinding and polishing using diamond burs and ceramic kits, and Group C underwent airborne-particle abrasion with 110 µm alumina at 400 kPa. Flexural strength was tested using a universal testing machine via the three-point bending method.
Results
Group B (Grinding and Polishing) showed the highest mean flexural strength (748.70 ± 79.95 MPa), followed by Group C (Air Abrasion) (689.90 ± 76.95 MPa), and Group A (glazing) (553.30 ± 131.75 MPa). Mann–Whitney U tests showed significant differences between Group A and Groups B (p = .002) and C (p = .041), but not between Groups B and C (p > .05).
Conclusion
Surface treatments significantly influence the flexural strength of monolithic zirconia. Polishing most effectively enhances strength by reducing flaws. Glazing reduced strength, likely due to thermal stress, while air abrasion showed moderate improvement. Clinical choice should balance strength and aesthetics.
Introduction
Ceramic materials have become indispensable in restorative dentistry due to their excellent aesthetics, biocompatibility, and favorable mechanical properties. The term “ceramic” broadly refers to inorganic materials, including glassy and crystalline structures, which can be tailored for specific dental applications based on their translucency, strength, and wear resistance.1, 2 Among these, zirconia-based ceramics—particularly yttria-stabilized tetragonal zirconia polycrystals (Y-TZP)—have emerged as the material of choice for fixed prostheses due to their superior fracture toughness and long-term clinical success.3, 4
Initially, metal-ceramic restorations dominated clinical practice due to their strength and adaptability. However, aesthetic limitations, such as opaque frameworks and marginal discoloration, led to the development of all-ceramic alternatives. 5 The advent of computer-aided design and manufacturing (CAD/CAM) further facilitated the adoption of monolithic zirconia restorations, eliminating the need for veneering porcelain and reducing the risk of chipping. 6 The intrinsic transformation toughening mechanism of zirconia, involving a stress-induced tetragonal-to-monoclinic phase shift, imparts high resistance to crack propagation, making it particularly suitable for both anterior and posterior restorations. 4
Despite these advantages, the clinical performance of zirconia is significantly influenced by post-sintering surface treatments such as grinding, polishing, glazing, and air abrasion. These procedures are often necessary to improve fit, aesthetics, or bonding, but they may also alter surface characteristics and affect flexural strength. 7 Flexural strength refers to a material’s ability to resist deformation or fracture when subjected to bending forces. In dental restorations, especially fixed and cantilever types, high flexural strength is essential to endure the complex stresses of mastication and maintain long-term structural integrity. Monolithic zirconia, with flexural strength ranging from 900 to 1,200 MPa, is particularly suited for such demanding applications due to its exceptional durability under functional loads.8, 9 Zirconia is known for its exceptionally high flexural strength, which is largely attributed to its transformation toughening mechanism and dense microstructure. However, any alterations to its surface—such as those caused by mechanical or chemical treatments—can significantly influence this strength. Surface changes may introduce defects like microcracks or flaws that act as stress concentrators and reduce the material’s strength. Conversely, certain surface modifications can improve mechanical properties by inducing beneficial compressive stresses. 4 Grinding can introduce surface flaws, yet may also enhance strength through compressive stresses generated by phase transformation. Glazing and heat treatments have been shown to improve surface smoothness and reverse deleterious phase changes, although their long-term effects remain controversial. 7
Numerous studies have investigated the impact of surface treatments on zirconia’s mechanical properties, but findings remain inconsistent. Manawi et al. found enhanced flexural strength in glazed zirconia, 10 Ebeid et al. observed that only post-sintering treatments improved strength, whereas pre-sintering treatments increased surface roughness without benefit. 4 Other researchers, including Giti and Abbasi and Elraggal et al., highlighted that surface treatment effects can vary based on zirconia type and translucency.11, 12 Öztürk et al. further emphasized that laser-treated zirconia showed reduced strength, regardless of the timing of the treatment. 13
The null hypothesis tested in this study was that there would be no significant difference in the flexural strength of monolithic zirconia subjected to different surface treatments. The alternative hypothesis proposed that surface treatment type significantly affects zirconia’s flexural strength.
To provide evidence-based guidance on how specific post-sintering surface treatments influence the mechanical durability of zirconia, and with the goal of improving material selection and treatment outcomes in restorative dentistry, it is essential to understand the outcome of these surface alterations. This will be critical for optimizing clinical protocols and improving the longevity of zirconia-based restorations, particularly in high-stress environments. Thus, given the variations in the findings of flexural strength and the increasing clinical use of monolithic zirconia, the aim of this study was to compare the Flexural Strength of Monolithic Zirconia after glazing, Grinding, & Polishing and Air-particle abrasion.
Materials and Methods
Study Design
A 3 × 1 × 10 factorial design was employed. A total of 30 monolithic zirconia specimens by SuperfectZir® zirconia disk of A2 shade (Aidite) [Figure 1] of dimension 25 mm × 6 mm × 3 mm, as per ADA Specification No. 69, 1991, were fabricated and distributed into three experimental groups:
Group A: Glazing
Group B: Grinding and Polishing
Group C: Air Abrasion

EXOCAD X5 Dental Plus (VS Lab Pvt. Ltd., Vadodara) software was used for designing the CAD model of the specimens, as shown in Figure 2.
EXOCAD X5 Dental Plus System.

Dental Plus X5, a 5-axis milling machine (Figure 3), was used to mill zirconia specimens at 2,900 RPM, with a feed rate of 2,000 mm/min.
Five Axis Milling Machine.

The milled specimens were sintered at 1,350°C–1,500°C for 7–8 hours to achieve full density before further processing.
Surface Treatments
After sintering, specimens were randomly assigned to the three surface treatment groups (n = 10 per group):
Group A (glazing): A thin coat of zirconia glaze was applied and fired at 790°C for 7–8 minutes using a standard ceramic furnace, as shown in Figure 4.
Group B (Grinding and Polishing): Specimens were ground using a coarse-grit diamond point under 40 lb/in² pressure, followed by polishing with the Shofu Zirconia Polishing Kit CA at 25,000 RPM, as per manufacturer instructions, as shown in Figure 5.
Group C (Air Abrasion): One surface of each specimen was abraded with 110 µm aluminum oxide (Al₂O₃) particles at 400 kPa pressure for 10 seconds, maintaining a 10 mm distance from the surface as shown in Figure 6.
Group A Glazed Samples

Group B Grinding & Polishing.

Group C Air Abrasion.

Flexural Strength Testing
Flexural strength was assessed using a Universal Testing Machine (UTM) via a three-point bending test with a crosshead speed of 1 mm/min, and load was applied centrally until specimen fracture, as shown in Figure 7.
Samples were Placed Under the Universal Testing Machine.

Flexural strength was calculated using the formula:
Flexural strength = 3 Wl/2bd2 Where w = Applied load (N)
I = Test span (mm)
b = Specimen width (mm)
d = Specimen thickness (mm)
The ultimate load that caused the specimen fracture was recorded.
Results
The in vitro study conducted to evaluate the flexural strength of monolithic zirconia after glazing, grinding and polishing, and air abrasion suggested the following results.
Table 1 suggests the mean values of Load and flexural strength for all three groups. Group A had a mean Max Load of 996.20 with a standard deviation of 996.20 ± 237.29. The mean flexural strength of samples of Group A was 553.30, and the standard deviation of 553.30 ± 131.75.
Descriptive Analysis.
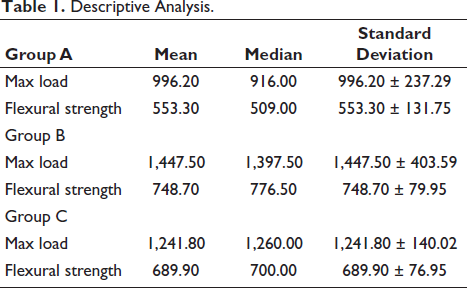
In Group B, the mean Max Load showed a higher average value of 1,447.50 with a larger standard deviation of 1,447.50 ± 403.59. The flexural strength had an average value of 748.70 and a standard deviation of 748.70 ± 79.95.
In Group C, the Max Load had an average of 1,241.80 and a standard deviation of 1,241.80 ± 140.02. The flexural strength had an average value of 689.90 and a standard deviation of 689.90 ± 76.95.
Further, to compare two independent groups “Mann–Whitney” test is applied, and to compare three independent groups, “Kruskal–Wallis” test is applied.
Table 2 compares the parameters among the three groups using the Kruskal–Wallis test. For maximum load, the mean ranks were 8.80 for Group A, 21.65 for Group B, and 16.05 for Group C. This gave a significant p value of .005.
Kruskal–Wallis Test.
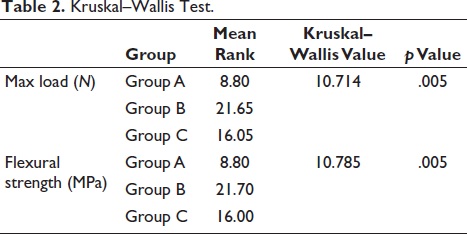
Similarly, for flexural strength, the mean ranks were 8.80 for Group A, 21.70 for Group B, and 16.00 for Group C, yielding a significant p value of .005.
Table 3 shows a comparison of the maximum load and flexural strength between Group A and Group B using the Mann–Whitney test. For maximum load, the mean rank was 6.50 for Group A and 14.50 for Group B with a z-value of −3.024 and a statistically significant p value of .002.
Mann–Whitney Test.
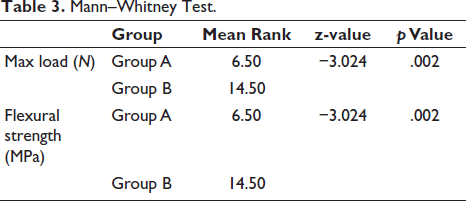
Similarly, for flexural strength, the mean rank was 6.50 for Group A and 14.50 for Group B with a z-value of −3.024 and a p value of .002, indicating a significant difference in both variables.
Table 4 shows a comparison of maximum load and flexural strength between Group A and Group C using the Mann–Whitney test. For maximum load, the mean rank was 7.80 for Group A and 13.20 for Group C, with a z-value of −2.041 and a statistically significant p value of .041.
Mann–Whitney Test.
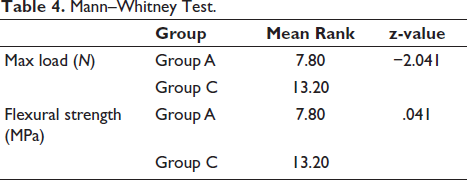
Similarly, for flexural strength, the mean rank was 7.80 for Group A and 13.20 for Group C with a z-value of −2.041 and a p value of .041, indicating a significant difference in both the variables.
Table 5 shows a comparison of the maximum load and flexural strength between B and C using the Mann–Whitney test. For maximum load, the mean rank was 12.65 for Group B and 8.35 for Group C, with a z-value of −1.626 and a p value of .104.
Mann–Whitney Test.
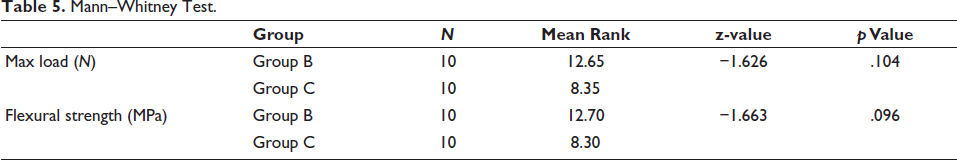
Similarly, for flexural strength, the mean rank was 12.70 for Group B and 8.30 for Group C with a z-value of −1.663 and a p value of .096. It can be noted here that p value for Max Load and flexural strength is >.05. Thus, there is no statistically significant difference between the variables in Group B and Group C.
Discussion
The current study compared the three surface treatments, namely glazing (Group A), grinding and polishing (Group B), and air abrasion (Group C) of zirconia specimens. The findings revealed significant differences in the flexural strength among the groups.
In the present study, grinding followed by polishing (Group B) resulted in the highest flexural strength, while glazing (Group A) yielded the lowest values, and air abrasion (Group C) showed intermediate strength. These results support the hypothesis that surface treatments significantly influence the flexural strength of zirconia.
The low flexural strength observed in the glazing group may be attributed to the high viscosity and poor wettability of glaze materials, which limit their ability to effectively seal the microdefects created during prior grinding. Glazing can also give contradictory results due to variations in application method, glaze layer thickness, and post-processing handling, which determine whether the glaze seals flaws or introduces new weaknesses. Thin or uneven layers may fail to cover microdefects, whereas excessively thick layers increase brittleness and susceptibility to chipping. Handling after glazing and the presence of bubbles can further compromise the integrity of the glaze layer. These concerns are consistent with the findings of Lai et al., who reported that glazing may not benefit ground zirconia and could even weaken its structure due to poor bonding and the fragile nature of the glaze. In their study, IPS e.max glaze paste (Ivoclar Vivadent, Liechtenstein) was applied to all specimen surfaces and fired at 500°C for 3 minutes, followed by 830°C for 2 minutes, producing a relatively thick glaze layer of approximately 10 µm with entrapped bubbles of 1–3 µm. 14 In the present study, glazing was carried out by applying a thin coat of zirconia overlay porcelain powder mixed with glaze liquid, followed by a single furnace firing at 790°C for 7–8 minutes. Despite these procedural differences, both studies consistently demonstrated that glazed groups exhibited the lowest flexural strength, suggesting that the intrinsic brittleness of the glaze layer, bubble entrapment, and poor interfacial bonding are the key factors responsible for strength reduction.
Contrary findings were reported by Chougule et al., who demonstrated that glazing could improve strength by filling minor surface flaws. However, they also noted that the weak interface (bi-layer zone) between the glaze and zirconia may act as a stress concentration zone, ultimately compromising long-term durability. These conflicting results suggest that while glazing may offer short-term aesthetic and mechanical benefits, its effectiveness depends on variables like application method, thickness, and post-processing handling. 15
The superior performance of polished specimens in Group B can be attributed to the ability of polishing to remove surface flaws, reduce crack propagation potential, and induce beneficial compressive stresses. According to Mohammadi-Bassir et al., during the polishing process, friction between abrasive tools and the zirconia surface generates localized heat, which may trigger a tetragonal-to-monoclinic (t ↓ m) phase transformation. This transformation causes a volume increase, leading to compressive stresses that help prevent crack propagation and enhance flexural strength. 16 Asli et al. reported that if cooling follows, a partial reverse monoclinic-to-tetragonal (m ↓ t) transformation may occur, restoring the original phase structure and contributing to the material’s mechanical resilience. 17 Polishing also avoids the introduction of additional thermal stresses, unlike glazing, which can compromise structural integrity. These findings are consistent with Aboushelib et al., who reported that polishing strengthens zirconia by eliminating microscopic surface imperfections. Zucuni et al. further confirmed that polishing restores surface smoothness and promotes reverse phase transformation, thereby improving fatigue and flexural strength.18, 19
According to Traini et al., over-polishing with very fine grit may lower hardness and fracture toughness, making the material more brittle. In their study, polishing was performed with diamond silicone wheels (StarGloss system, Edenta AG, Switzerland) in coarse (green) and superfine (yellow) grits, with the fine polishing group receiving an additional 3 µm diamond paste. While the manufacturer does not specify the exact abrasive particle size of the polishing wheels, reporting them only in qualitative terms (coarse, fine, superfine), the use of a superfine grit in combination with the 3 µm paste likely contributed to the reduced fracture toughness observed in the fine-polished specimens. In contrast, rough polishing increased toughness but also raised surface roughness, leading to potential stress concentrators. Thus, an optimal balance is required between surface smoothness and mechanical resistance. 20
The intermediate strength in the air-abraded group (Group C) is indicative of a dual effect. On one hand, air abrasion increases surface roughness, promoting better resin bonding, but on the other, it creates microdefects that weaken the material. Interestingly, Aurelio et al. reported that air-particle abrasion can improve zirconia strength due to tetragonal-to-monoclinic phase transformation, which induces compressive stress and heals microcracks. Moreover, this transformation was shown to enhance aging resistance, especially after a 12-hour period, indicating possible long-term clinical advantages. 21
Conversely, Abi-Rached et al. emphasized the risk of using large particle sizes (250 µm), which introduce deeper microcracks that undermine strength. 22 The stage at which abrasion is performed is critical for its mechanical outcomes. Yilmaz et al. demonstrated that post-sintering air abrasion improves biaxial flexural strength, whereas pre-sintering abrasion reduces it due to weak surface integrity. 23 In the present study, the milling operation was carried out at 2,900 rpm with a feed rate of 2,000 mm/min to achieve the desired dimensions and surface quality of the specimens. The samples were then sintered to full density at 1,350°C–1,500°C for 7–8 hours, and a subsequent surface treatments, including air abrasion, were performed post-sintering, ensuring that the specimens were treated in their fully dense state.
The results of this study have important clinical implications. While glazing is often selected for aesthetic enhancement, it may be unsuitable for high-stress areas, such as molars or bruxism-prone zones. On the other hand, grinding and polishing not only improve surface finish but also enhance flexural strength, making it a preferable choice for load-bearing restorations. Air abrasion, when applied correctly, can be beneficial for improving bonding but should be carefully managed to avoid excessive damage.
These findings also underscore the need for clinicians and dental laboratories to understand the mechanical effects of routine surface treatments. Choosing an appropriate finishing protocol can influence not only the success of the restoration but also its long-term performance and patient satisfaction.
Limitations of the Study
Despite its strengths, this study has some limitations:
In vitro nature: The experimental setup does not fully replicate intraoral conditions such as temperature fluctuations, humidity, saliva, and occlusal forces.
Lack of thermomechanical aging: No cyclic loading or thermocycling was performed, which could influence flexural strength over time.
Limited sample size: The study utilized a small number of specimens, which may affect the statistical power and generalizability of the results.
Single zirconia system: Only one brand/type of zirconia was tested, which may not reflect the performance of other commercially available materials.
Thus, it can be suggested that to further investigate the flexural strength of zirconia, the following things can be accommodated:
Incorporate thermocycling and cyclic fatigue testing to simulate intraoral aging. Explore combinations of surface treatments (e.g., polishing + thin glaze) for optimal mechanical and aesthetic outcomes. Compare different brands, translucency levels, and grain sizes of zirconia. Evaluate the influence of bonding cements and luting agents on flexural strength in conjunction with surface treatments. Consider long-term clinical trials to validate in vitro results.
Conclusions
Within the limitations of this in vitro study, it can be concluded that surface treatments significantly influence the flexural strength of monolithic zirconia restorations. Among the methods evaluated, grinding followed by polishing proved most effective in enhancing mechanical performance by minimizing surface flaws and microcracks. While glazing offers aesthetic benefits, it may compromise strength due to the formation of a brittle surface layer and thermal stresses. Air abrasion increases surface roughness and bonding potential but may introduce microdefects that weaken long-term durability. Overall, polishing provides the best balance between strength and reliability, making it the preferred option for high-stress clinical applications.
Footnotes
Acknowledgments
The author gratefully acknowledges the support and guidance of Manubhai Patel Dental College and Hospital, Vadodara, for providing the academic framework and resources necessary to carry out this research work. Sincere thanks are extended to VS Dental Lab Pvt. Ltd., Vadodara, and Praj Dental Laboratory, Pune, Maharashtra, for granting permission and providing access to their facilities for the laboratory testing required in this study. Special appreciation is due to Mr. Vivek Suryakant Rao, Director of VS Dental Lab, and Mr. A. M. Bhagat, Proprietor of Praj Dental Laboratory, for their kind cooperation and technical assistance throughout the process.
Authors’ Contribution
All authors contributed to the study design, data collection, analysis, and manuscript preparation. All authors have read and approved the final manuscript.
Consent to Participate
Not applicable.
Consent for Publication
Not applicable.
Data Availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Declaration of Conflict of Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
This research was approved by the Institutional Ethics Committee of Manubhai Patel Dental College & Hospital, Vadodara, Gujarat. Approval No: IEC/MPDC_279/PROSTHO-40/23. Date: November 1, 2023.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
