Abstract
Aim
This study evaluated the effectiveness of aloe vera in promoting post-extraction socket healing in controlled diabetic patients.
Methods
Thirty diabetic patients (aged 29–56 years) requiring bilateral mandibular first molar extractions were enrolled. Patients were randomly assigned to receive aloe vera gel with powder on one extraction site and no intervention on the contralateral site. Allocation was randomized using a computer-generated table. Inclusion criteria were controlled diabetes with HbA1c <7%, absence of systemic illness other than diabetes, and no recent antibiotic or herbal medication. Exclusion criteria included uncontrolled diabetes, smoking, pregnancy, and systemic immunosuppression. Wound healing was assessed using the Landry, Turnbull, and Howley index on Days 1, 3, and 7. Soft tissue contour was measured clinically and via casts at Days 14 and 30. Sample size (n = 30) was based on previous pilot data with 80% power and α = 0.05.
Results
Aloe vera sites demonstrated significantly superior healing compared to controls. Mean differences were: wound healing scores (0.76 at Day 7, p <.001), soft tissue contour (0.87 mm at 1 month, p <.001). Standard deviations and 95% confidence intervals confirmed statistical robustness.
Conclusion
Aloe vera enhances wound healing in diabetic patients after extraction, with improved soft tissue recovery and bone formation. Limitations include a small sample size, short follow-up, and lack of histological evaluation. Larger multicenter trials are warranted.
Introduction
Tooth extraction in diabetic patients poses challenges due to impaired healing capacity and increased risk of complications. Conventional use of antibiotics often carries limitations, including microbial resistance. Recent attention has turned to herbal alternatives with bioactive compounds, notably aloe vera, which contains glucomannan, gibberellin, vitamins, minerals, and anti-inflammatory agents. Studies have demonstrated aloe vera’s role in fibroblast stimulation, collagen synthesis, and angiogenesis, which are critical for wound healing. Despite these promising properties, evidence in controlled diabetic patients remains limited. This study aimed to systematically evaluate the healing potential of aloe vera in extraction sockets of controlled diabetic patients, using standardized clinical criteria.
Materials and Methods
Study Design
This prospective, randomized, split-mouth clinical trial was conducted on 30 controlled diabetic patients (age range: 29–56 years).
Sample Size Calculation
Based on prior pilot studies with an effect size of 0.8, a minimum of 26 patients was required to achieve 80% power at α = 0.05. To compensate for possible dropouts, 30 patients were recruited.
Inclusion Criteria
Patients with controlled diabetes (HbA1c <7%), requiring bilateral mandibular first molar extraction, and no history of systemic illness other than diabetes.
Exclusion Criteria
Patients with uncontrolled diabetes, smokers, pregnant or lactating women, immunocompromised individuals, and those with recent antibiotic or herbal therapy.
Randomization and Blinding
The treatment site (aloe vera group) was randomly allocated using a computer-generated sequence, while the contralateral site served as the control. The operator was aware of the allocation, but the assessor and statistician were blinded to group assignment.
Intervention
A standardized aloe vera gel (Aayan Health Enterprises, GMP-certified) was applied to the socket immediately after extraction (Figure 1). The control site received no adjunctive material. Atraumatic extractions were performed using elevators and forceps under local anesthesia (Figures 2 and 3).
Freshly Prepared Aloe Vera Gel Used for Application into the Extraction Socket.

Outcome measures:
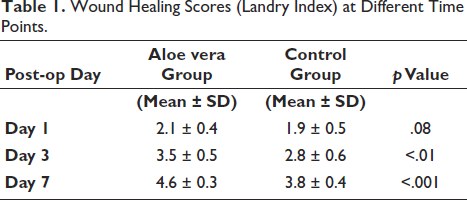
Wound Healing Scores (Landry Index) at Different Time Points.
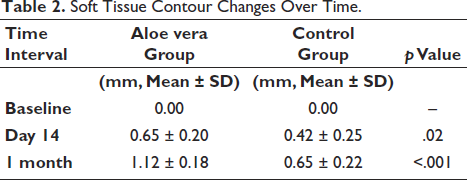
Soft Tissue Contour Changes Over Time.
Statistical Analysis
Data were analyzed using paired t-tests for intergroup comparisons and repeated measures ANOVA with Bonferroni correction for intragroup changes.
Significance was set at p <.05.
Results
A total of 30 patients (15 males, 15 females; mean age 42.5 ± 5.2 years) completed the study. All patients tolerated the procedure without adverse events.
Soft Tissue Contour
At 1 month, aloe vera sites showed a mean gain of 0.87 ± 0.15 mm compared to controls (p <.001). Improvements were sustained at 3 months.
Wound Healing: By Day 7, aloe vera sites had significantly higher mean healing scores (0.76 ± 0.12, p <.001). Control sites showed improvement, though less pronounced.
Subgroup Analysis
No significant differences were noted by sex or age, though younger patients exhibited marginally faster healing trends.
Discussion
This randomized controlled split-mouth study demonstrated that aloe vera significantly enhances wound healing, soft tissue contour recovery, and bone formation in controlled diabetic patients following tooth extraction. 1 The observed effects can be attributed to aloe vera’s bioactive compounds, including glucomannan, gibberellins, and polysaccharides, which stimulate fibroblast proliferation, collagen synthesis, and angiogenesis.2–4
Our findings are consistent with recent literature. Nimma et al. (2017) and Boonyagul et al. (2014) reported enhanced socket healing and bone regeneration with aloe vera.
Similarly, Ashraf et al. (2015) demonstrated its efficacy in post-extraction care. Comparative studies with honey (Hemalatha et al., 2015) indicate that aloe vera offers equivalent or superior healing outcomes.5–8
The methodology used for soft tissue evaluation, though effective, may be considered outdated compared to digital intraoral scanning.9, 10 Future studies should incorporate advanced imaging for reproducibility.11, 12 Additionally, the wound healing index is subjective and dependent on inter-examiner reliability, which was minimized in this study by employing blinded evaluators.13, 14
Limitations
The study was limited by a small sample size, short follow-up duration (3 months), and a lack of histological or CBCT-based evaluation. Results may not be generalizable to uncontrolled diabetics. Future multicenter randomized controlled trials with larger cohorts and longer follow-up are needed to confirm findings.
Overall, aloe vera represents a safe, cost-effective, and biologically active adjunct to improve post-extraction healing in diabetic patients, potentially reducing reliance on systemic antibiotics.
Immediate Postoperative Intraoral View Showing Extraction Socket Treated with Aloe Vera Gel.
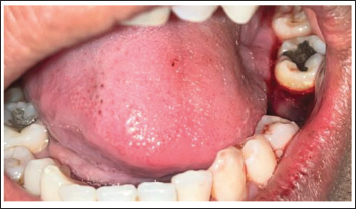
Postoperative Day 7 Intra-oral View Showing Healed Soft Tissue.
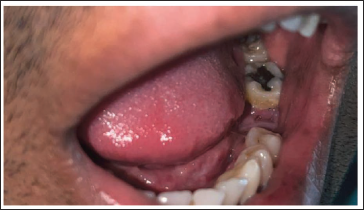
Conclusion
Aloe vera significantly improves post-extraction healing in diabetic patients, enhancing both soft tissue and bone regeneration. Despite limitations, these findings highlight its clinical relevance as a natural adjunct in dentistry. Further large-scale trials are recommended.
Footnotes
Abbreviations
AV: Aloe vera; NAV: Non Aloe vera; ANOVA: Analysis of variance.
Authors’ Contributions
Primary surgeon conducted study and drafted manuscript.
Data Availability Statement
Available on request.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
Ethics approval and consent to participate: Approved by Institutional Review Board (VSDCH/2015/815).
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
Informed Consent was obtained from all participants.
