Abstract
Background:
Various studies have provided evidence of the impact of COVID-19 and the measures adopted by governments on drug use and its treatment. After 4 years, a more precise assessment of the evolution of patients and addiction treatment services can be made. The objective of this study is to compare different periods during the COVID-19 pandemic to identify changes in patient profiles and the care activity of addiction treatment centres.
Methods:
A retrospective observational study was conducted using data from March 14, 2019 to June 22, 2022, from addiction centres of Andalusia (Spain). Information related to the treatment of each patient was collected during 1 year after the initiation of treatment (until June 22, 2023). Electronic health records of 29 740 outpatients were analysed and divided into 4 periods (pre-pandemic, lockdown, return to normal and post-lockdown).
Results:
Differences were found across the analysed periods. Admissions declined during the lockdown period but subsequently increased, without reaching pre-pandemic levels. Admission to treatment due to opioid dependence increased during the lockdown. In contrast, the percentage of patients with dual pathology decreased. An increase in the dropout rate of patients from treatment was observed compared to the pre-pandemic period.
Conclusions:
The results revealed a similar patient profile across the different analysed periods. The most notable changes are observed in healthcare activity, which appears to have decreased. Therefore, a greater investment is likely required for the reformulation of addiction centres and increased funding to provide adequate assistance to these patients.
Introduction
The COVID-19 pandemic has affected healthcare services worldwide. 1 Since early 2020, many countries have been affected by an unprecedented health crisis with the arrival of the SARS-CoV-2 coronavirus. 2 Most countries were forced to adopt new public health measures to mitigate the spread of the virus. These measures included quarantines, reorganisations of health services, relocations of patients and reductions in patient numbers. 3 This situation has also prompted the implementation of stricter requirements for patient admission to treatment 4 and care activity. 5
People with pre-existing medical conditions, particularly those with mental health issues, were significantly affected by the pandemic. Several studies have suggested that lockdowns increase symptoms of anxiety, depression and suicide attempts. 6 This was particularly concerning for patients with substance use disorders (SUDs), since these individuals represent a vulnerable population due to their dependence on care services and because uncertainty, stress, isolation and economic crises further exacerbate their situation.7,8 Consequently, some authors have reported an increase in drug use,9 -11 along with relapses and overdoses in the clinical population during the pandemic.12 -14
Given these challenges, it is critical to ensure access to treatment for SUD patients during times of crisis, as this can be protective against relapse. 11 However, various studies have shown that support services, particularly outpatient services, experienced a decrease in admissions within the first 2 months of the pandemic.5,15 Many services were forced to close, and those that remained open often faced difficulties in admitting new patients due to the implementation of measures designed to ensure social distancing. 2 Similarly, patients expressed fear of infection 12 and encountered barriers to accessing treatment, especially those living in rural areas affected by mobility restrictions between cities or a lack of resources for online therapy (eg, computers, internet connections). 14
This situation led to a significant reduction in treatment admissions during the initial months of the pandemic. According to the European Monitoring Center for Drug and Drug Addiction’s (EMCDDA) report on the impact of COVID-19 in Europe in 2021, countries such as Bulgaria, Ireland, Lithuania and Portugal experienced a reduction in treatment admissions rates of up to 50%. 2 Regarding care activity, some studies have reported an increase in the number of appointments per patient during this period 8 along with a rise in the number of women accessing treatment. 16 Regarding consumption patterns, research indicates a decline in cannabis use during lockdown, 15 while the odds of testing positive for drug use doubled during the final weeks of the confinement period. 17
Most studies on the impact for COVID-19 on treatment of persons with drug dependence have been carried out in the early stages of the pandemic and on specific patient groups. For example, some studies have focused on the impact of the pandemic on patients with comorbid mental disorders,16,18 in patients diagnosed by opioid use disorder,19,20 or on the first stages of pandemic.21,22 However, there is limited empirical evidence on how the situation has evolved over time in drug addiction centres. In this sense, several studies have emphasised the importance of studying the post-pandemic period to understand how treatment units were functioning after this situation. 5 The lack of evidence on patient characteristics and outcomes during and after the COVID-19 pandemic makes it difficult to provide an overview of whether patients’ needs have changed and how treatment can be adapted. Therefore, our research aims to provide an overview of how the profile of patients with substance use disorders and the care activity of addiction centres have changed at different times during the pandemic. To do this, the present research proposes the following specific objectives: (i) To analyse how the profiles of the patients admitted to treatment changed across the periods: ‘Pre-pandemic’ (14/03/2019-13/03/2020), 2. ‘The first state of alarm and extensions’ (14/03/2020-21/06/2020), and 2 post-COVID-19 periods: 3. ‘Return to normal’ (22/06/2020-21/06/2021) and 4. ‘Post-lockdown’ (22/06/2021-22/06/2022). According to prior research,15 -18 we hypothesise that there will be differences in treatment admissions based on the primary drug of use across different periods. Similarly, we hypothesise that differences will be found in sociodemographic variables and co-occurring mental disorders across these periods; (ii) To compare care activity indicators and treatment outcomes after 1 year of treatment. Based on previous findings,2,5,15 we hypothesise a general reduction in treatment admissions during the confinement period, followed by an increase after this period, returning to previous levels. Also, an increase of drop-out was hypothesised during the lockdown period.
Methods
Design
This study was a retrospective observational study, analysing data collected from addiction centres in Andalusia (a region of Spain with over 8 000 000 inhabitants) between March 14, 2019, and June 22, 2022.
Participants
The present study included outpatients with a diagnosis of substance use disorder admitted to one of the addiction centres in Andalusia. All patients were followed up for 1 year after onset treatment. Therefore, the data analysed are up to June 22, 2023. The inclusion criteria were: (i) initiate treatment at one of the public or affiliated centres of addiction in Andalusia during the specified period; (ii) having at least one International Classification of Diseases 10 (ICD-10) diagnosis of an addictive disorder (cocaine, opiates, alcohol, cannabis or hypnosedatives); (iii) only patients who were 18 years of age or older were included. The exclusion criteria were: (i) having 1 International Classification of Diseases 10 (ICD-10) diagnosis of another addictive disorder (eg, other stimulants than cocaine, hallucinogens, tobacco, etc.), (ii) patients under 18 years old.
The final sample consisted of 29 740 outpatients from 112 outpatient centres for addictions. It is estimated that 95% of outpatients with addiction problems in Andalusia are treated in 1 of these centres. The main treatment demands were for cocaine-related disorders (45.2%), alcohol-related disorders (40.8%), cannabis-related disorders (22.2%), opiate-related disorders (16.1%) and benzodiazepine-related disorders (3.2%). A total of 22.3% of patients exhibited disorders related to more than 1 drug.
The patients were categorised according to the period during which they were admitted to the addiction centre. During the year prior to the pandemic (March 14, 2019-March 13, 2020) 11 320 patients were admitted for treatment. During the lockdown (March 14, 2020, June 21, 2020) a total of 1135 patients were admitted for treatment. During the period termed as ‘return to normality’ (June 22, 2020-June 21, 2021) a total of 8436 patients were admitted for treatment. Finally, in the ‘post-lockdown’ period (June 21, 2021-June 22, 2022) a total of 8849 patients were admitted to treatment.
Procedure
The data utilised in this study were collected through the Information System of the Andalusian Plan on Drugs (siPASDA). Professionals from each centre had a designated profile that allowed them to code and access information related to individual patients. The information recorded corresponds to the variables of the Treatment Demand Indicator (TDI) Standard Protocol 3.0 of the EMCDDA. 23 The TDI provides basic information about sociodemographic variables, drug use history, previous treatments, and infectious diseases at the start of treatment. In addition, the professionals coded information about the diagnosis of the patients according to the ICD-10 criteria, prescribed pharmacological treatments, psychological evaluation and treatments, results of toxicological tests, social status of the patient, and treatment progress.
All professionals underwent training to ensure accurate data recording. Previous research using the same dataset has shown adequate reliability values. 24
Statistical data analysis
Pearson’s chi-square test was used to analyse differences between periods in terms of qualitative variables, and Cramer’s V statistic was used to calculate effect sizes. The association was considered weak if this value was less than 0.2. Quantitative variables, such as age, were analysed with the nonparametric Kruskal‒Wallis’s test and post-hoc analysis was conducted with the Games–Howell test since the data were not normally distributed. A
Ethics
The registration of the data and storage of the information complied with the General Health Law, and ethical approval was granted by the Research Ethics Committee of the Andalusian Ministry of Health, which has certified compliance with the requirements for the ethical handling of the information. Patients provided their consent for their information to be included in the system. The database is completely anonymous to both patients and professionals, and it is not possible to inform participants about the study. The storage and coding of these data comply with the General Health Law of April 25, 1986 (Spain) and Law 41/2002 of November 14 on Regulating Patient Autonomy, Rights, and Obligations regarding Clinical Information and Documentation. Moreover, compliance with the Organic Law 3/2018 of December 5, 2018, on protecting personal data and guaranteeing digital rights, adapted to European regulations, was also ensured.
The study received ethical approval from the Research Ethics Committee of the Ministry of Health in Andalusia (Cod. 0661-N-22), ensuring that it met the ethical standards for data management.
Results
Sociodemographic characteristics, drug use and other mental health disorders
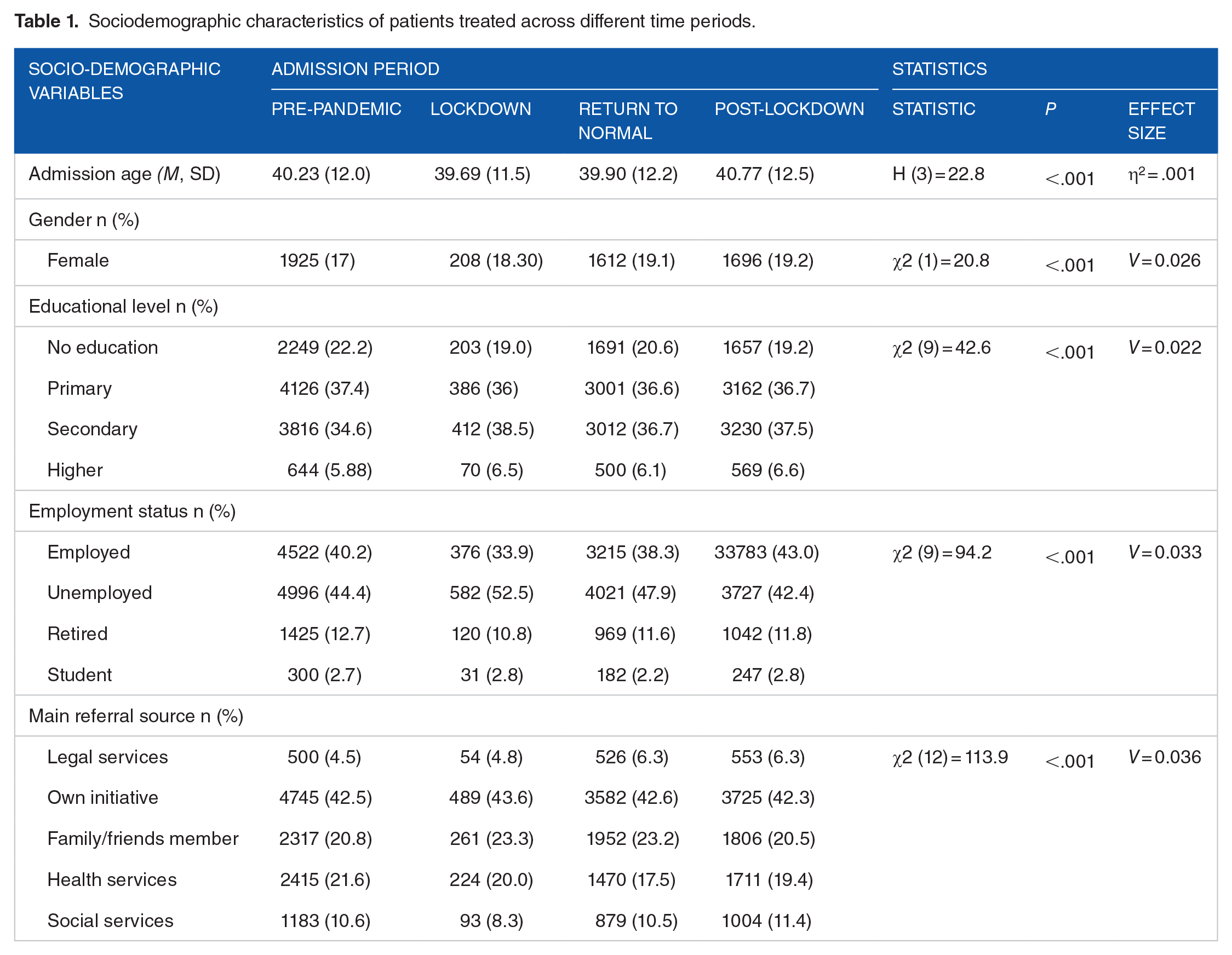
Table 1 shows statistically significant differences in all the socio-demographic variables analysed. However, no clear trend is found for any of the variables except for gender. With respect to this variable, after the lockdown, although fewer number of women were admitted for treatment (n = 1612 in ‘return to normal’ period and n = 1696 in ‘post-lockdown’ period compared to n = 1925 in pre-pandemic period), the proportion of women/men has increased compared to pre-pandemic rates, reaching 19.2% of woman in the post-lockdown period.
Sociodemographic characteristics of patients treated across different time periods.
The analysis of the substance use disorders during the lockdown showed that admissions of patients with opioid dependence increased by more than 7%. Conversely, during this period, admissions of patients with alcohol use disorder decreased by more than 6%. After the lockdown, admissions of patients with opioid dependence decreased to levels below those of the pre-pandemic period (14.7% and 14.4% on ‘return to normal’ and ‘post-lockdown’ period respectively). In contrast, admissions for alcohol dependence increased to pre-pandemic levels (41.5% in the return to normal period; Table 2). It was also observed that the number of patients with poly-dependence admitted for treatment remained stable (24.9%-25.6%) until the ‘post-lockdown’ period. During this period, a decrease of more than 10% was observed. No significant changes were observed in the frequency of drug use.
Pattern of consumption and comorbid mental disorders.
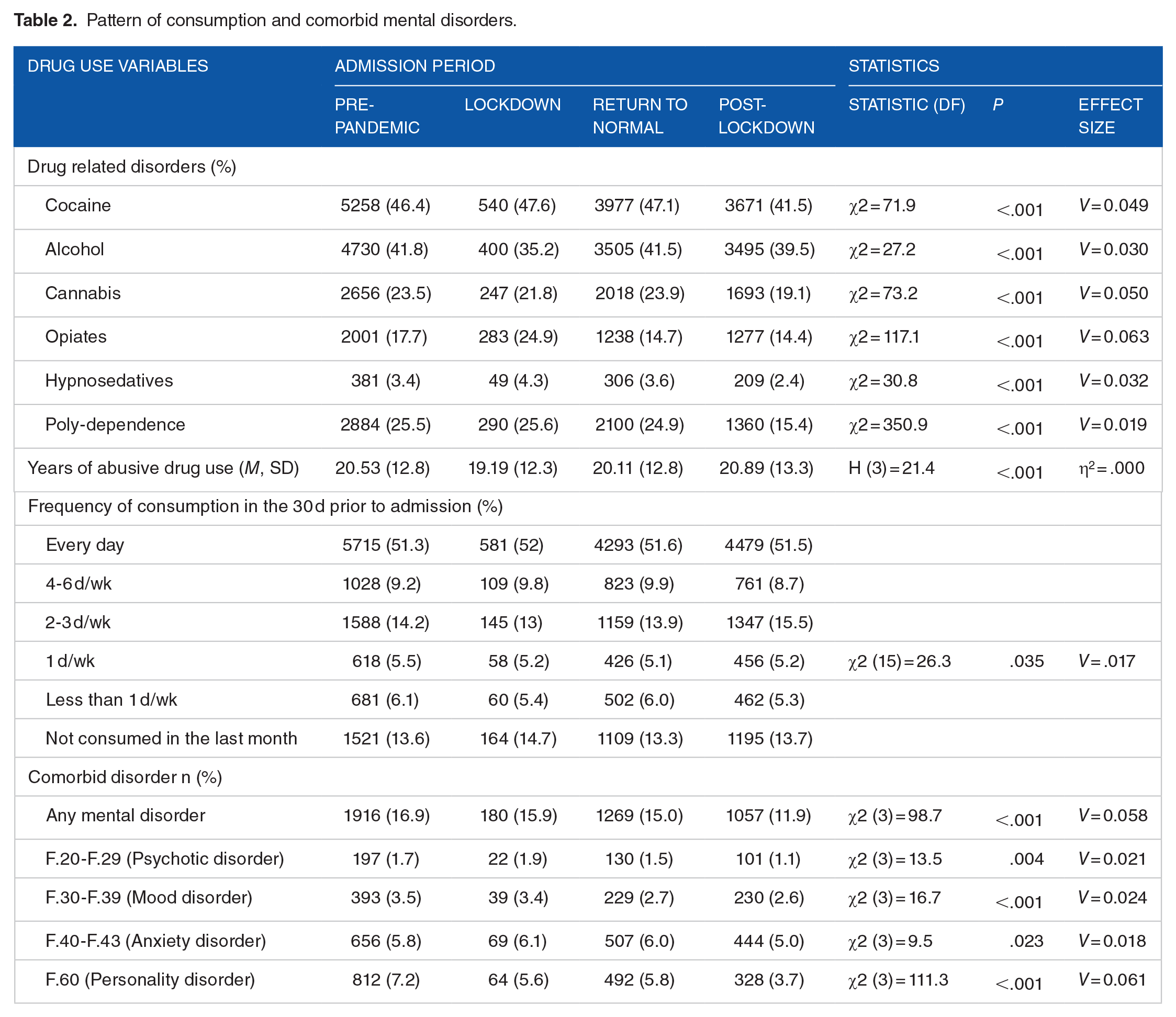
Analysis of the different periods revealed that the number of patients with other primary comorbid mental disorders – not induced by substance use – also decreased in addiction centres. Before the pandemic, dual disorder patients represented nearly 17% of the patients. After that, they decreased to 11.9% (Table 3). This reduction is observed across different diagnostic categories of mental disorders, except for patients with psychotic disorders. The most notable reduction is in personality disorders, where a reduction of nearly 50% is observed.
Care activity across periods.

Trend in treatment admissions
Figure 1 shows the monthly trends in the number of treatment admissions during the periods analysed. Although admissions for treatment increased following the lockdown, they have not yet reached the pre-pandemic average number. The average number of patients admitted per month during the pre-pandemic period was 909.58 (SD = 143.76), with the highest number of admissions occurring in October 2019 (1110). However, during the lockdown period, this average decreased to 454.5 (SD = 257.29). After the lockdown period, there was an increase in the average number of patients per month, reaching 700.67 (SD = 121.40) during the ‘return to normal’ period and 716.58 (SD = 135.02) during the 2 months of the ‘post-lockdown’ period.

Monthly evolution of admissions in addiction treatment centres.
In contrast, during the lockdown, the percentage of patients who had previously received treatment (readmission), slightly increased compared to that in the previous period (20.9% compared to 19.1% on pre-pandemic period), with a notable decrease in the subsequent stages analysed (14.8% and 15.2% respectively). Similarly, the highest percentage of patients receiving coordinated care for other mental disorders in mental health centres was observed during the lockdown (6.4%). This percentage has also decreased since that period.
Treatment drop-out and discharge at 1 year
Regarding the therapeutic situation of patients after 1 year of follow-up, notable changes were observed between the dropout group and the follow-up group. Specifically, the number of dropouts after 1 year of treatment onset increased in the different periods analysed, reaching almost 60% in the post-lockdown period. Conversely, the percentage of patients still in treatment after 1 year decreased by more than 12%. No significant changes were observed in therapeutic discharge.
Discussion
Numerous studies have analysed the impact of the COVID-19 pandemic on the treatment of patients with substance use disorders. However, this is one of the few studies that establishes 4 study periods with different levels of restriction: it uses the year prior to the lockdown as a reference and follows up until all COVID-19-related restrictions were lifted. Additionally, the evolution of patients for 1 year from the initiation of treatment was analysed.
Overall, our data did not reveal significant changes in the sociodemographic profiles of individuals admitted to treatment. We consider the most relevant finding to be the observed percentage increase in women. These findings align with existing literature on treatment admissions during crises. 16 As highlighted by other authors, 25 during COVID-19, 44% of women reported an increase in illicit substance use, while 20% experienced symptoms of depression and 23.4% reported symptoms of anxiety. These emotional stressors likely contributed to the rise in substance consumption.
Our findings concerning patterns of drug use are in line with those of other studies,13,16 which found an increase in admissions for opioid use patients during the lockdown period. Various factors could explain this finding. First, several studies have reported an increase in the demand for opioid agonist treatment,13,14 likely resulting from a reduction in the availability of opiates on the illicit market. This scarcity may have led patients to seek pharmacological treatment as an alternative. 26 In addition, the World Health Organization prioritised opioid agonist treatment, 27 recognising the considerable challenges faced by these patients, including marginalisation, stigmatisation, and the risk of withdrawal.28,29 Moreover, healthcare services in many countries, such as Spain, provided flexible treatment options, including ‘take home’ programmes, 5 which were easier for patients to adhere to during the lockdown. After the lockdown, treatment admissions decreased significantly to levels slightly lower than those in the pre-pandemic period.
Regarding the diagnosis of other mental disorders, the authors expected an increase in mental disorders reflecting the observed increases in prevalence in the population following the COVID-19 period, especially in anxiety and mood disorders. 30 However, the results showed a reduction in patients with psychiatric comorbidities. Particularly notable is the observed decrease in mood or anxiety disorders after the lockdown. These findings contrast with those of previous research, which revealed an increase in anxiety and depression due to the fear of contagion, economic crises, job losses and social distancing.1,8,12,31 A possible hypothesis explaining this result is that individuals with comorbid mental disorders are attending mental health centres instead of addiction centres. This might occur because they consider their problematic drug use to be caused by their underlying mental disorders. Therefore, a decrease in patients with dual pathology was observed.
Concerning care activity, the data of the present study show a notable change in the activity of treatment centres, with a significant reduction in the number of admissions. This finding is consistent with those reported by other authors,13,28,32 who also observed a decrease in treatment admissions during and after the COVID-19 pandemic. This decrease might be attributed to the lockdown policies imposed on healthcare units. Most addiction centres were forced to limit new patient admissions by focusing primarily on the most severe cases and implementing more stringent admission criteria.33,34 Additionally, patients expressed concerns about the fear of infection and difficulty accessing treatment centres. Furthermore, the lack of internet access hindered their participation in online meetings, and they were unable to attend treatment centres for in-person appointments.15,31 These results are consistent with other studies, 15 indicating the inability of the healthcare system to return to previous levels of admissions and activity. On the other hand, the increase in the percentage of readmissions to treatment during the lockdown could be attributed to the self-perception of patients at increased risk of relapse, with the possibility that individuals with a history of chronic and excessive substance use may be particularly vulnerable to increased usage. 35 Also, as pointed out by other authors, these findings suggest that individuals with pre-existing addiction problems were more likely to experience adverse effects from the lockdown.7,8
Unlike other studies, this research also included an analysis that extended beyond the lockdown period, covering over a year after admissions, that examined 2 distinct periods: ‘return to normal’ and ‘post-lockdown’. This follow-up revealed that the percentage of patients who discontinued treatment during the first year increased by more than 12%. Consequently, the percentage of patients receiving treatment has decreased. That is, the results reflect that the ability to retain patients in treatment seems to have notably diminished after the lockdown. This aspect is crucial because the duration of treatment and therapeutic adherence are predictors of a favourable prognosis for patients diagnosed with substance use disorder.36 -38 The data available in this study do not allow for hypotheses regarding the causes of these results. However, this finding underscores the urgent need for a reorganisation of existing addiction services to address current unmet needs. 39 The situation is expected to worsen in the post-COVID-19 era due to economic recession and social isolation.40,41 Therefore, there is a need to improve care for patients with substance use disorders. Further studies including data in this post-pandemic stage, would complement present results and better understand current situation.
Certain limitations of this study should be considered to interpret these findings accurately and make valid comparisons. First, the results were obtained through a retrospective observational design. While the clinicians had experience recording the data in a standardised manner, the pressures of providing care during the months studied could have led to minor errors in data registration. Additionally, the retrospective analysis based on real-world data, inherently limits control over sample size. As a result, a formal sample size estimation was not performed prior to data analysis. However, given that the sample exceeds 29 000 patients, the analyses with significant and relevant results surpass the conventional threshold for statistical power (<0.80). Despite this limitation, the use of real-world data offers information of high ecological value. Second, this research encompasses 1 year of follow-up, indicating that there is still a considerable amount of patient information to be analysed. This implies that we are obtaining a ‘snapshot’ at a particular moment in the treatment of patients. A high percentage of patients were ‘undergoing treatment’; thus, the final prognosis of these patients remains unknown.
Despite these limitations, the findings of this study may provide valuable insights for enhancing care activities in substance addiction treatment centres. The pandemic has reshaped society, necessitating a re-evaluation of substance use services to adapt to the ‘post-COVID era’ and to recover the human and economic resources that have been affected. This study is one of the few that examines, from a certain distance, the long-term effects of the crisis, particularly concerning mental health issues. 42 Understanding the collateral damage inflicted by the pandemic is essential for devising new plans and strategies for the ‘post-COVID era’. 43
Conclusions
Initially, many studies were published on the impact of COVID-19 on substance use and addiction treatment. However, there is limited information on how care activity has evolved. In this study, we have observed some changes in patient profiles. Most notably, there has been a significant decrease in the number of patients with psychiatric comorbidities in addiction centres. Additionally, the number of patients discontinuing addiction treatment has increased. These findings underscore the necessity for addiction services to adapt to the needs of the most vulnerable patients without compromising care for others, while increasing flexibility in their treatment options (including diverse treatment delivery methods and improved digital access services). Results emphasise the importance of enhancing staff training for emergency preparedness and ensuring that treatment services remain flexible and responsive to evolving patient needs.
Footnotes
Acknowledgements
This study has been developed thanks to the transfer of data by the Department of Equality, Social Policies and Conciliation of the Junta de Andalucía.
Author Contributions
1. Conceptualisation and Study Design
- Narváez-Camargo, M., Mancheño-Velasco, C., Lozano, O.M.: Conceived and designed the study, outlined objectives and hypotheses.
- Narváez-Camargo, M., Mancheño-Velasco, C., Lozano, O.M., Fernández-Calderón, F.: Contributed to the refinement of the study design and helped define key variables.
2. Data Collection and Acquisition
- Narváez-Camargo, M., Mancheño-Velasco, C., Lozano, O.M.: Organised and verified dataset quality and integrity.
3. Data Analysis and Interpretation
- Narváez-Camargo, M., Mancheño-Velasco, C., Lozano, O.M., Fernández-Calderón, F. and Díaz-Batanero, C.: Conducted the data analysis, including statistical modelling and interpretation of findings.
4. Manuscript Preparation
- Narváez-Camargo, M., Mancheño-Velasco, C., Lozano, O.M., Díaz-Batanero, C.: Drafted the initial manuscript and prepared the figures/tables.
- All authors: Reviewed and edited the manuscript, added critical content, ensured clarity and accuracy, provided comments on the draft, revised specific sections, approved the final version for submission and agreed to be accountable for all aspects of the work.
Funding:
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the grant ‘Evolución de la actividad asistencial y los resultados del tratamiento de pacientes con trastorno por consume de sustancias en Andalucía durante las diferentes fases de la pandemia Covid-19’, project EXP 2022/08882 by Delegación para el Gobierno del Plan Nacional sobre Drogas (Spain) from the European Union’s Recovery, Transformation and Resilicience Mechanism.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical and Approvals
The registration of the data and storage of the information complied with the General Health Law and Ethical approval was granted by the Research Ethics Committee of the Andalusian Ministry of Health, which has certified compliance with the requirements for the ethical handling of the information.
