Abstract
International evidence suggests differences in perinatal outcomes between migrant women and their native-born peers, but the intergeneration impact of family migration and interplay with maternal ethnicity remains unclear. This study investigates the relationships between maternal ethnicity, migration status, and perinatal outcomes using secondary analysis of data obtained by an established birth cohort study in the north of England using regression models. Pakistani migrants had higher odds of low birth weight and lower odds of macrosomia compared to white British natives. Pakistani migrants of all generations had higher odds of gestational diabetes, with odds among first-generation migrants almost double that of second-generation migrants. First-generation Pakistani migrants also had lower odds of preterm birth and Apgar score < 7 at 1 min in comparison with other groups. Lower incidence of premature birth in first-generation migrant Pakistani women is of importance. Higher odds of low birth weight and lower odds of macrosomia among Pakistani migrants compared to white British women merits further investigation. It is noteworthy that this is despite higher odds of gestational diabetes overall in this population and generational differences in among Pakistani migrants requiring further attention, with a full consideration of confounding environmental and biological factors, with a view to addressing identified inequalities.
The World Health Organisation (WHO) in its 2018 report on the health of refugees and migrants in the WHO European Region highlights significant differences in pregnancy-related indicators among refugees and migrants compared to native populations. 1 While the nature and magnitude of these differences vary between host countries, a WHO review found that refugee and migrant women were at increased risk of adverse events including induced and spontaneous abortions, caesarean sections, birth complications, and instrumental deliveries across the WHO European Region. 2 Further country-specific evidence has shown specific examples of adverse outcomes, including an 18-fold increased risk of neonatal death among African refugee and migrant mothers in Sweden 3 and increased risk of preterm birth in Italy 4 and Portugal. 5 While these studies provide important context, the majority are of a significant age (10–15 years), meaning that the need for updated evidence in this field is of paramount importance.
In the United Kingdom, analysis of health outcomes related to migration is often based on self-reported ethnicity due to a lack of data relating to migration in health datasets. According to mortality rates in the 2011 census, a slight advantage in terms of life expectancy at birth among first-generation migrants was observed, 6 however further research has highlighted that ethnic minority groups have lower disability-free life expectancy compared to the white British population. 7 Improving recording of ethnicity and migration history in health records is of paramount importance in studying the patterns of health and disease in these populations. 8
Bradford is an ethnically diverse and relatively economically deprived city in the north of England. The population of the city was influenced by large numbers of Pakistani migrants arriving in the 1950s, having been actively recruited to take up employment in the city's wool mills. Most migrants initially were working-aged men; subsequently family reconstitution migration has meant that Bradford is now home to a three-generation population of Pakistani origin. 9
It has been established that an association exists between perinatal outcomes and maternal ethnicity; women of South Asian origin have been found to be more at risk of delivering babies who are of a low birth weight and less at risk of macrosomia, despite higher prevalence of gestational diabetes. It is also important to consider that the concept of ethnicity is a social construct that attempts to convey a sense of shared cultural characteristics which may include elements such as language, religion, dietary practices, norms, and customs in addition to shared nationality or family heritage. While the use of ethnic groupings is useful in identifying and addressing inequalities, it does not account for variation in environment and experience within an ethnic group. 10 The relationship between maternal ethnicity and migration status is less clear in the existing literature. A narrative review of available evidence relating to perinatal outcomes in migrant women highlighted the need for research that attempts to explore the interplay between ethnicity and migration to examine whether migration status influences the established additional risks associated with ethnicity. 11
Given the international importance of improving maternity outcomes and reducing inequalities, as highlighted as a key component of achieving the U.N. Sustainable Development Goals, 12 it is imperative that factors contributing to adverse perinatal events are identified and contextualised to inform preventative strategies. While international evidence of poorer outcomes for refugee and migrant women exists, this evidence tends to focus on recent and/or forced migration, and therefore does not account for intergenerational influences, nor does it assess whether belonging to a largely settled and established migrant community impacts outcomes.
The Born in Bradford cohort offers a unique opportunity to examine these factors, having collected data relating to the personal and family history of migration of all participants. Assessing pregnancy and birth outcomes, particularly with the inclusion of more objective variables such as migration status, length of stay in the host country (or length of migration), and country of origin, in addition to self-reported ethnicity, could provide substantive information on health inequalities and the extent to which these variables may change over time. The objectives of this study are therefore to:
Investigate the impact of maternal migration status on perinatal outcomes. Explore the influence of family migration history on differences in perinatal outcomes. Assess the extent to which self-reporting ethnic group contributes to differences in perinatal outcomes.
Methods
The Born in Bradford Cohort
Born in Bradford (BiB) is a prospective cohort study that recruited participants during pregnancy. The cohort was established in the city of Bradford, located in northern England, in response to the observation of very high rates of infant mortality in the city. Women were invited to participate in the study when attending a universally offered oral glucose tolerance test appointment at 26–28 weeks’ gestation or when attending other antenatal appointments. Informed consent was obtained, and women were asked to complete a baseline questionnaire providing data on maternal characteristics, including their personal and family migration background. Recruitment took place between March 2007 and December 2010, and over 80 percent of women eligible in this period agreed to take part, which represents approximately 64 percent of the births occurring in Bradford during this period. Data from the baseline questionnaire has been linked with routine maternity data which enables the examination of perinatal outcomes by maternal characteristics. Details of the cohort profile are published elsewhere. 13
Outcome Variables
The neonatal outcome variables studied were low birth weight (below 2,500
Migration Status
Migration status groups were calculated using questionnaire responses regarding the mother's country of birth and that of her parents and grandparents. First-generation migrants are therefore those women who were themselves born outside of the United Kingdom; second generation migrants were those women who were themselves born in the United Kingdom but have at least one parent who was born abroad. Due to small numbers, those with a higher order migrant background (i.e., grandparents born abroad) were combined with second-generation migrants. To account for the impact of ethnicity in differences between groups, each migrant group was stratified based on self-reported ethnicity, White British, Pakistani or Other Ethnicity. While it is acknowledged that ‘Pakistani’ may not commonly be regarded as an ethnicity, rather a nationality, and ‘White British’ an ethnic group and nationality combined, these categorisations were self-reported by the individuals participating in the study when asked to define their ethnic group. These groupings therefore reflect the source data and are analysed with the complexities of defining a socially constructed concept such as ethnicity in mind.
Statistical Analysis
Characteristics of the sample and perinatal outcomes in all other groups were compared with those for white British native women, who were considered as the reference group. Characteristics of the sample were described, presenting categorical variables as percentages and continuous variables as means and standard deviations (SD). Differences between groups were explored using χ2 for categorical data and Student's t-test for continuous data.
Logistic regression analyses were used to compare the rate of each of the binary outcome variables by migration status, with white British women considered as the reference group and differences between groups estimated using odds ratios (ORs). The adjusted regression model included maternal characteristics which may influence the outcome variables. These were informed by the literature and refined by the assessment of multicollinearity. Index of multiple deprivation (IMD) score, maternal age, and parity were therefore included as covariates in the adjusted analysis. Crude and adjusted ORs (OR and aOR) are therefore presented with 95 percent confidence intervals (CI). IMD is the official measure of relative deprivation for small areas in England and combines information from seven domains of deprivation (income, employment, education, health, crime, housing and environment) to give a deprivation score. IMD score is therefore assigned to participants based on their self-reported home address.
In the multivariate logistic regression model for this study, there is no clear logical or theoretical basis for assuming any variable to be prior to any other, either in terms of its relevance to the research goal of explaining phenomena or in terms of a hypothetical causal structure of the data. For this reason, a simultaneous model of including independent variables in the multivariate logistic regression model was most appropriate.
Where significant associations between first-generation migrant status and outcome variables were observed, multiple linear regression was employed to explore the extent to which maternal length of stay in the United Kingdom was associated with changes in outcomes. Statistical analysis was undertaken using SPSS V.24.
Results
Characteristics of the Sample
For descriptive analysis, differences between groups were explored using χ2 for categorical data and Student's t-test for continuous data. There were a significantly higher proportion of adolescent mothers in all native groups compared to migrant groups, except for second-generation white migrants (majority Irish immigrants). Approximately, 23.5 percent of first-generation Pakistani migrants had parity of three or more compared to 17.1 percent among second generation Pakistani migrants and 7.2 percent of white British natives. Migrant women of both Pakistani and other ethnicities were significantly more likely to be married compared to native women in the same ethnic groups. Both mothers and fathers in migrant groups were more likely to have educational qualifications equivalent to A level or higher; first-generation Pakistani migrants were twice as likely than any other group to have never been employed, and the highest levels of unemployment among fathers were in the native Pakistani men and native men of other ethnicities. Characteristics of the sample are shown in Table 1. Exploratory analysis of differences in perinatal outcomes between migrant groups is shown in Table 2. The results suggest a higher prevalence of gestational diabetes among migrant groups with the highest rate being among first-generation Pakistani migrants. There was also a higher incidence of low birth weight and a lower rate of macrosomia among these groups. The rate of low birth weight was highest among second-generation migrants of Pakistani or other ethnicities.
Characteristics of the Sample.
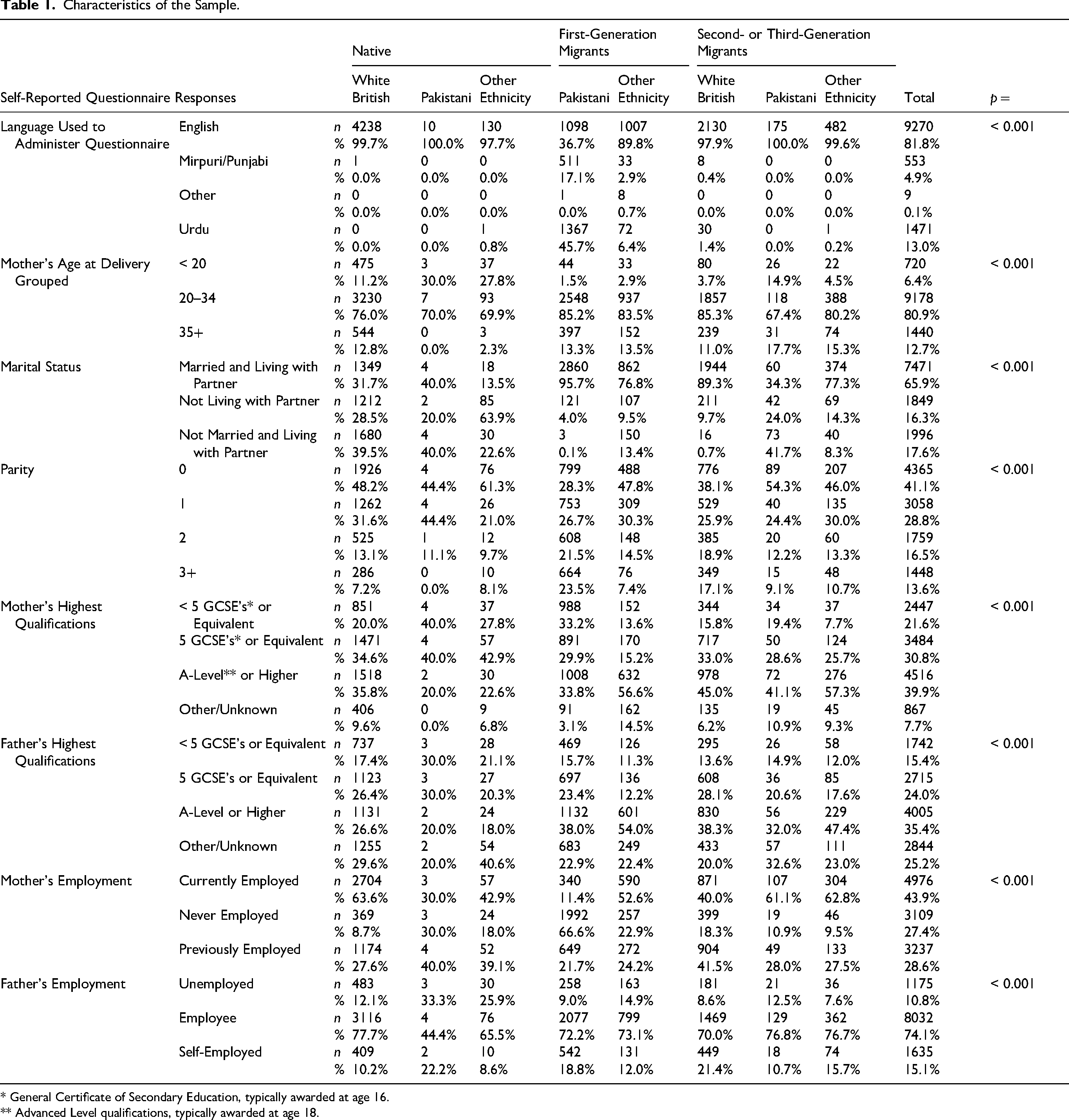
* General Certificate of Secondary Education, typically awarded at age 16.
** Advanced Level qualifications, typically awarded at age 18.
Descriptive Analysis of Differences in Perinatal Outcomes by Migration status.
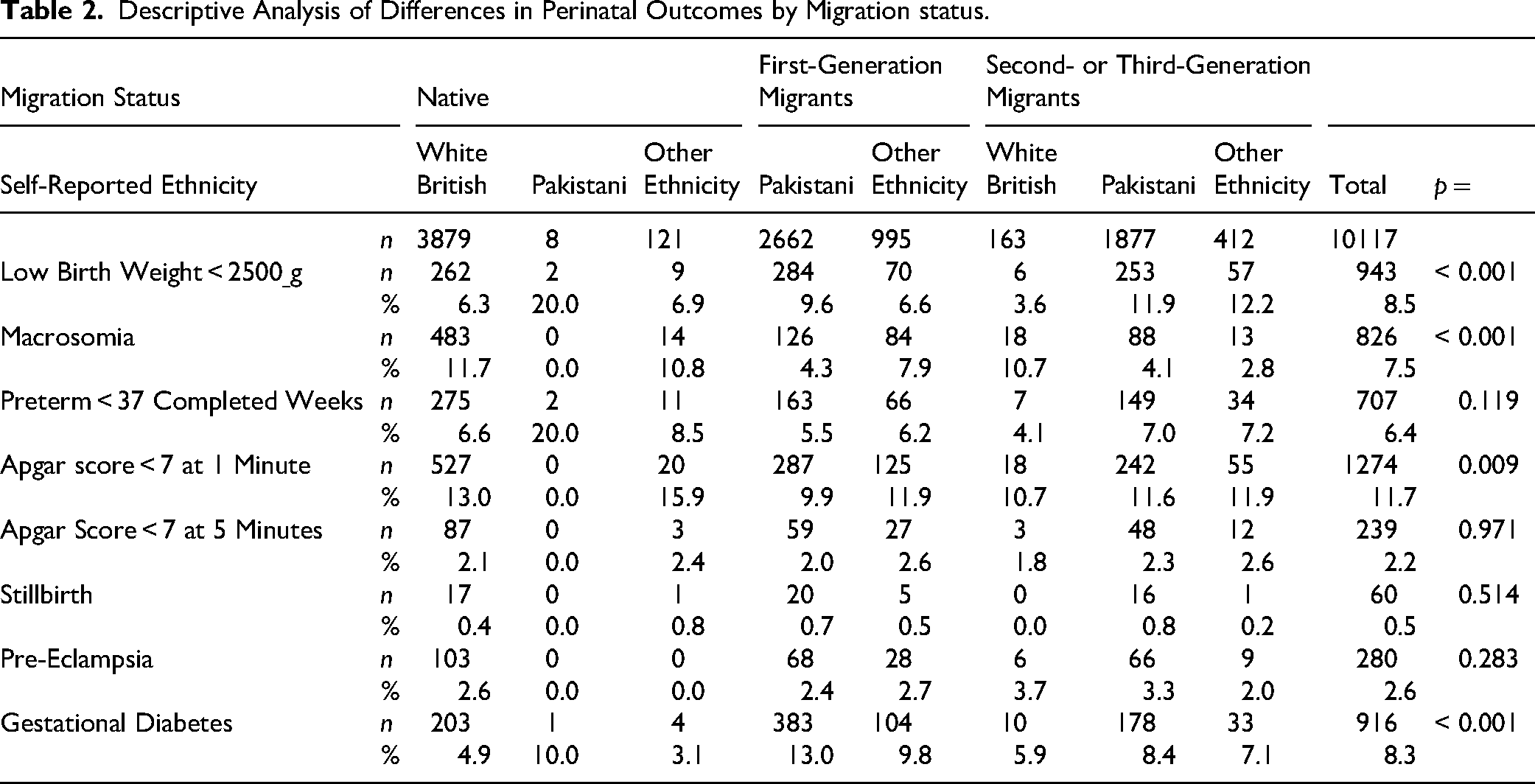
Perinatal Outcomes by Ethnicity and Migration Status
Table 3 presents a comparison of perinatal outcomes by ethnicity and migration status. Native women of Pakistani ethnicity are excluded from this analysis due to small numbers. First- and second-generation migrant Pakistani women and second-generation migrant women of other ethnicities had higher odds of delivering low birth weight babies in the adjusted analysis while lower odds of macrosomia were also observed among these groups. First generation Pakistani migrants had increased odds of stillbirth, but it did not reach statistical significance. However, decreased odds of preterm delivery, Apgar score below 7 at 1 min, and caesarean section were observed in this group of migrant women compare to native mothers.
Perinatal Outcomes by Ethnicity and Migration status.
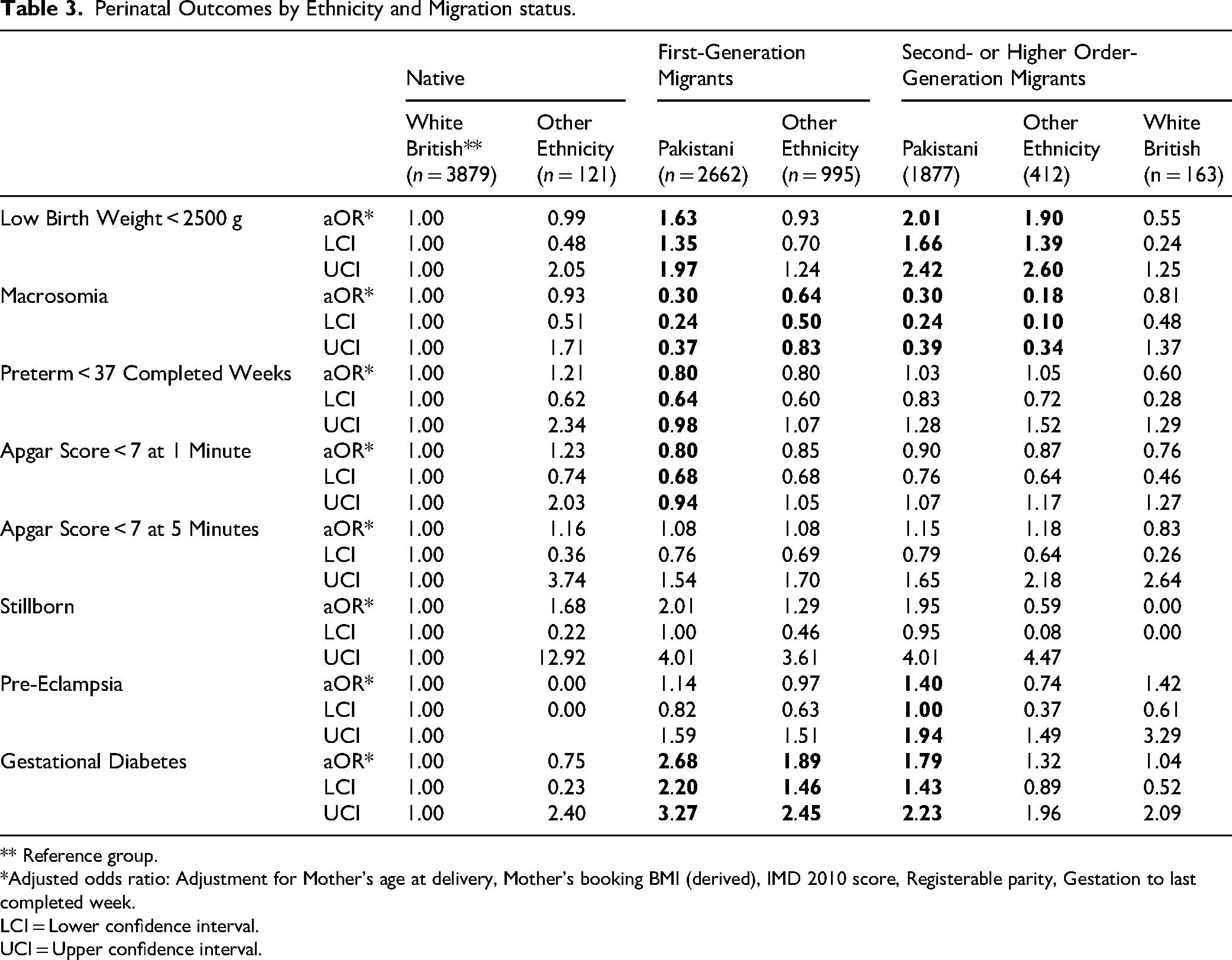
** Reference group.
*Adjusted odds ratio: Adjustment for Mother's age at delivery, Mother's booking BMI (derived), IMD 2010 score, Registerable parity, Gestation to last completed week.
LCI = Lower confidence interval.
UCI = Upper confidence interval.
Given the differing observations relating to preterm delivery and birth weight categories between migrant groups, multiple linear regression analyses were conducted to examine the relationship between both birth weight and gestational age at delivery and length of stay in the United Kingdom for first-generation migrants.
The multiple linear regression calculated to predict birth weight based on length of stay in the United Kingdom and adjusted for maternal age, maternal body mass index (BMI), Index of Multiple Deprivation score, parity and gestational age at delivery found a significant regression equation (F(6,3625) = 418.1, p < 0.001), with an R2 of 0.409 and effect size f2 = 0.692. Predicted birth weight increased 4.4 grams for each additional year of residence in the United Kingdom amongst first-generation migrants. The multiple linear regression calculated to predict gestational age at delivery based on length of stay in the United Kingdom and adjusted for maternal age, maternal BMI, Index of Multiple Deprivation score, and parity found a significant regression equation (F(5,3626) = 8.67, p < 0.001), with an R2 of 0.012 and effect size f2 = 0.012. Predicted gestational age at delivery decreased by 0.014 days for each additional year of residence in the United Kingdom amongst first-generation migrants.
Discussion
Main Findings
The results show some important differences in outcomes both by ethnicity and migration status. The results of this study support the previous literature suggesting higher odds of low birth weight and gestational diabetes in Pakistani women and lower odds of macrosomia.11,15 However, the results show that first-generation Pakistani migrants had decreased odds of preterm delivery and Apgar score below 7 at 1 min, which were not apparent in other groups.
Examination of gestational age at delivery and birth weight for first-generation migrants using multivariate linear regression suggested a statistically significant association between both variables and length of stay in the United Kingdom. This said, the effect size related to gestational age was small, equating to 0.014 days gestation for each additional year of residence suggests this is not a clinically important finding. The effect size related to birth weight was larger, equating to an increase of 4.4
While the odds of gestational diabetes in both first- and second-generation Pakistani women in the present study were significantly higher compared to white British native women, there were also differences between these two groups. Odds of gestational diabetes in first-generation Pakistani migrants were 2.68 (CI 2.20–3.27) compared to 1.79 (CI 1.43–2.23) for second-generation Pakistani migrants, meaning the odds for first-generation migrants were almost double those for second-generation migrants in the same ethnic group.
Previous studies examining the relationship between ethnicity and preterm birth have reported mixed results regarding Pakistani populations,16–18 suggesting that factors other than ethnicity may be stronger predictors of preterm birth risk. A previous retrospective study examining the relationships between ethnicity, maternal country of birth and preterm birth in over 4.5 million births in England and Wales found an increased risk of preterm birth in Pakistani mothers; however, this risk was lower in mothers born outside the United Kingdom compared to U.K.-born Pakistanis. 19 This lower rate of preterm birth in mothers who were born outside the United Kingdom is in line with our study findings and raises the importance of considering intergenerational and migration status differences in the analysis of such population-based studies. Family structure and support through lower incidence of single parents, smoking and adolescent pregnancies and higher level of education observed mostly in the first-generation Pakistani families in a previous study may have also played a role in the observed positive outcomes. 20 Additionally, studies have shown that vaginal microecological dysbiosis-related diseases are the most common causes of preterm birth, such as bacterial vaginosis (BV), vulvovaginal candidiasis (VVC), group B streptococcal (GBS) infections, and other infectious diseases. 21 Therefore, the impact of healthy lifestyles in terms of lower incidence of smoking, adolescent pregnancies, maternal family structures (e.g., having higher rates of marriage and stable relationships in mothers), and vaginal infection rates in relation to differences in lower incidence of preterm birth in Pakistani women merits further investigation.
Associations between ethnicity, hyperglycaemia, and perinatal outcomes have previously been investigated in the BiB cohort. 22 In addition to examining birth weight, this study also examined infant adiposity measured using skinfold thickness and cord blood leptin levels. The study found that while babies born to South Asian women were lighter, on average they had a higher body fat percentage when adjusted for birth weight compared to white British infants. These findings suggest that any attempts to address disparities in low birth weight babies must be mindful of the tendency for greater adiposity in South Asian infants, and that the thresholds for classification of low birth weight may need to be revisited to account for ethnic variations in the determinants of adverse outcomes. These findings are expanded upon by the current study by examining migration status of women of Pakistani origin as a strata within women of South Asian ethnicity. While our findings add weight to the need to consider ethnicity-specific thresholds, they also highlight that there are nuances within ethnic groupings which warrant further exploration. This is supported by clear evidence of correlation between incidence of low birth weight and poverty-related measures such as nutrition, health care, and housing that transcend international boundaries. 23 In the present study, Index of Multiple Deprivation and geographic small area-based measures were used to consider this factor in the model, meaning that individual differences between families living within the same area were not captured. This again highlights the need for improved clarity and detail in routine data collection in the United Kingdom.
Ethnicity-specific birth weight distributions have previously been investigated with significant results. A study assessing birth weight distribution of babies with European, Chinese and South Asian heritage reported that on average infants born at 40 weeks’ gestation of European descent weighed 254.6
The observed higher odds of stillbirth among first-generation Pakistani migrants and the higher odds of preeclampsia in the Pakistani second-generation migrants were of a borderline statistical significance, which could be indicative of the need for a larger sample size for these outcomes. Similar patterns by ethnicity have been seen previously, 28 however the higher risk of pre-eclampsia in second-generation Pakistani mothers merits further attention to investigate the potential interplay between ethnicity, acculturation, and environmental influences on birth outcomes.
The increasing trend for risk of stillbirth is in line with previous reports in which Pakistani ethnicity was identified as a significant risk factor for stillbirth alongside factors such as maternal obesity, smoking, pre-existing diabetes, socio-economic inequalities, and foetal growth restriction. 29 Gardosi and colleagues 30 identified unrecognised foetal growth restriction as the single largest risk factor and, along with our findings, this provides a solid evidence base for the need for targeted preventive strategies. Stillbirth may also be associated with higher prevalence of congenital abnormalities particularly considering that consanguineous marriages are also more common in this group. 31 A previous study of the BiB cohort showed the risk of congenital abnormalities in infants of Pakistani origin was almost twice that of white British infants and that 37 percent of babies born in Pakistani families had parents in first-cousin unions. 31 The current study potentially adds a further level of detail to these associations by highlighting the increased odds of stillbirth in first-generation Pakistani migrants, however further investigation into these associations is needed.
There is a significant lack of evidence in the existing literature regarding the relationship between migration status of U.K. residents, country of origin, or migration journey experiences with perinatal health, and the focus is largely on refugees and asylum seekers’ pregnancy and birth outcomes. It is possible that this fact highlights problems in grouping of ‘migrants’ versus ‘non-migrants’ without consideration of the reasons for migration or differences between migrant categories. Economic and family restoration migrants are likely to have very different characteristics compared to refugees and asylum seekers, for example—meaning the grouping of migrants as a homogenous group may be problematic. A recent systematic review evaluating maternal and perinatal outcomes of asylum seekers and undocumented migrants in Europe found evidence of increased risk of adverse outcomes in these groups, largely attributed to lack of access to health care and quality of services. 32 The authors said the study only reviewed eleven eligible papers, highlighting the dearth of research in this area. Data regarding the reason for migration and migration journey was not available in the BiB cohort, which is an important consideration for further research.
Strengths and Limitations
The size and diversity of the Born in Bradford cohort is a significant strength of this study, particularly the availability of detailed information regarding migration histories and country of origin. This analysis utilised this data in a unique way that added important nuance to established patterns of ethnic inequalities by including migration history and intergenerational variations as a contextual measure. Due to significant shortcomings in the collection of routine data relating to ethnicity and migration history in the United Kingdom, all variables related to these characteristics in this study were self-reported. For this reason, it is possible that errors of recollection or knowledge of family history could have impacted groupings. There were also no data available regarding reasons for migration or travel histories before reaching the United Kingdom (for example, time spent in other countries or traumatic experiences while in transit during migration journey). These details could provide further insight into the mechanisms at play resulting in differential outcomes. Similarly, no standardised measure of individual socio-economic status was available to this study. The use of a small geographical area measure as a proxy is legitimate but may, however, lead to individual differences being missed.
Analyses for some outcomes were also limited by small numbers, particularly in relation to rare outcomes such as stillbirth, meaning robust conclusions were difficult to draw.
Conclusion
At the time of writing, this article is the first U.K.-based study to examine the interplay between ethnicity and migration status in reference to perinatal health, and it has uncovered some important differences, particularly between groups of women with shared ethnicity but different migration status. Positive results such as lower incidence of premature birth or lower incidence of macrosomia amongst Pakistani women compared to white British women is noteworthy; however, higher incidence of complications such as gestational diabetes, pre-eclampsia, and low birth weight among these women requires further attention. Of particular note is the finding that odds of gestational diabetes among first-generation Pakistani migrants were almost double that of second-generation migrants, despite shared country of origin. Work to develop appropriate interventions with a full consideration of confounding environmental and biological factors to address the identified inequalities is urgently needed.
Footnotes
Acknowledgements
The Born in Bradford study is only made possible because of the enthusiasm and commitment of the children and parents in BiB. We are grateful to all the participants, practitioners, and researchers who have made Born in Bradford happen.
Ethical Approval and Informed Consent
Ethical approval for the Born in Bradford cohort study was granted by Bradford Research Ethics Committee (ref no. 07/H1302/112), which includes informed consent to share anonymised data for secondary analysis and publication.
Authors’ Contributions
KMD: data analysis, manuscript drafting. HS: review and finalisation of manuscript.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was funded by a grant from The Burdett Trust for Nursing, grant number 472356.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Availability of Data and Material
Requests for access to data should be addressed to the corresponding author or to the Born in Bradford programme manager at rosie.mceachan@bthft.nhs.uk.
