Abstract
Motor interventions are commonplace for children with neurodevelopmental disabilities, as motor skills such as walking, balancing and using one's hands functionally are instrumental for early exploration and developing a sense of agency and independence in later life. This review explores the use of non-pharmacological interventions for motor delays in children with neurodevelopmental disabilities, specifically looking at the characteristics of effective and ineffective interventions, what skills were targeted, and the transferability of interventions to non-clinical settings. From the 119 reports included in the final sample, the findings demonstrated that gross motor skills were most frequently targeted for intervention. These skills were most often assessed using standardised measures. Characteristics of effective interventions involved twice weekly implementation and unfamiliar environments. Transferability of interventions varied drastically from home-based yoga and parent-implemented massage therapy to interventions requiring virtual reality, treadmills and specialised interventionists.
Lay Abstract
Many children with neurodevelopmental disabilities receive motor interventions for delays with skills such as walking, crawling and using one's hands functionally. This is important for children to explore their environment and develop skills for independence later in life. This review worked to understand behavioural and psychological interventions for motor delays in these children. This article specifically examined what characteristics make an intervention effective or ineffective, what skills were targeted, and the transferability of these interventions beyond a research or medical setting. From the 119 reports included in the final review, findings showed that gross motor skills, including walking and coordination, were most often targeted for intervention. Motor skills were most often assessed using standardised measures. Characteristics of effective interventions involved twice weekly sessions and unfamiliar environments. Some interventions were transferable, including home-based yoga and massage therapy done by parents. Other interventions were not transferable as they required virtual reality, treadmills and specialised professionals to conduct the intervention.
Keywords
Proficient motor skills are critical for early childhood development as they allow young children to actively explore and engage with the world around them (Oudgenoeg-Paz, 2014). In addition, motor development is related to other developmental domains such as social and cognitive abilities (DeLuca et al., 2013), and academic success (Murrah, 2010). For children with neurodevelopmental disabilities including autism, attention deficit hyperactivity disorder (ADHD) and Down syndrome, motor skill development can be challenging and can greatly benefit from early intervention. While motor delays are not a diagnostic criterion for autism and ADHD, these difficulties have been reported in nearly 80% of autistic children (Green et al., 2009) and 50% of children with ADHD (Gillberg, 1998; Goulardins et al., 2016). This exemplifies both the need for appropriate motor intervention and a better understanding of the populations from which we can understand the standards of current interventions. For rarer neurodevelopmental disabilities such as Pitt–Hopkins syndrome, Fragile X syndrome and Williams syndrome, motor delays frequently present in early childhood (Kau et al., 2002; Mayall et al., 2021; Van Balkom et al., 2012). For some diagnoses, motor delays are primary characteristics of the presentation, as in the case of Rett syndrome (Brunetti & Lumdsen, 2020) and Angelman syndrome (Duca et al., 2013), although these diagnoses are rare, making it challenging to draw conclusions about the broader populations. Given the inextricable link between developmental domains, specifically in more plastic periods of early childhood, non-pharmacological motor interventions have led to positive outcomes in areas such as executive function (Schurink et al., 2012; Westendorp et al., 2014), academic success (Flores et al., 2023; Jelle Veijk et al., 2011) and language development (Duncan et al., 2019; Odeh et al., 2020) while potentially minimising the risks associated with some pharmaceutical interventions (Catalá-López et al., 2017). While pharmaceuticals can be incredibly effective for children with ADHD (van der Oord et al., 2008), there are high rates of discontinuation (Habel et al., 2005; Toomey et al., 2012) which can impact their long-term efficacy. Parents and their children have mixed opinions on medication use (Charach et al., 2014) with some feeling positive (McElearney et al., 2005) while others do not (Hart et al., 2018). As such, it is beneficial to understand the non-pharmacological options to give families the opportunity to explore what best suits their respective needs. Pharmacological interventions can vary from stimulant medication for ADHD (Carolan, 2021) to psychotropic medication for children with Down syndrome (Weas et al., 2024) which impact the chemical balance in the brain. Alternatively, non-pharmacological interventions can include occupational therapy, physical therapy and many others which address developmental domains behaviourally. Additionally, there is a wealth of literature that exemplifies the efficacy of motor interventions for children with Down syndrome (Ku & Sung, 2022; Rodríguez-Grande et al., 2022), ADHD (Kleeren et al., 2023, Xie et al., 2021) and autism (Colombo-Dougovito & Block, 2019; Ruggeri et al., 2020) from which researchers can deduce features of effective interventions. While neurodiversity ranges broadly from those with a unique chromosomal difference to those with an unclear genetic underpinning, by looking across diagnoses rather than investigating them independently, we can determine potential effective interventions that can benefit children who were not in the respective sample.
Other reviews have explored the use of interventions for motor delays in the past, ranging from autistic children (Ruggeri et al., 2020) to children with Down syndrome (Maïano et al., 2019), though they are diagnosis-specific. Although the experiences of children with neurodevelopmental disabilities differ broadly, consolidating these findings is beneficial to determine what interventions could benefit children across populations. As autism and ADHD are more common, research within these groups can provide a broader sample from which one can inform motor interventions for other populations with similar presentations. Phenotypes differ for syndromes with a genetic basis, but these reports can be used as a jumping-off point for researchers and practitioners. While there have been efforts to consolidate input from those with lived experience through institutions such as the James Lind Alliance (James Lind Alliance, 2017), it would be beneficial to present intervention research as a parallel to understanding disability intervention experience holistically and transdiagnostically (Astle et al., 2022).
Early intervention has been shown to improve motor skills, in addition to adaptive functioning (Connolly et al., 1993). The options for interventions range from aquatic physical therapy (Milligan et al., 2022) and animal-assisted therapies (Zoccante et al., 2021) to traditional physical therapy (Guivarch et al., 2021; Young, 2017) and virtual reality (Mraz et al., 2016), making it difficult for both parents and clinicians to decide what intervention is best and what makes it so. This systematic review aims to provide a detailed account of current non-pharmacological motor interventions for children with neurodevelopmental disabilities including how their progress is operationalised, the characteristics of effective and ineffective interventions and the transferability of these interventions to non-clinical settings in an effort to enable accessibility and agency for families of children with neurodevelopmental disabilities. We specifically explored non-pharmacological interventions in this report as pharmacological interventions function differently (Cope & Mohn-Johnsen, 2017; Gomathi et al., 2020) compared to behavioural interventions such as occupational and physical therapies. Similarly, we explored how interventions may be transferable to non-clinical settings which would not be possible with pharmacological methods.
Objectives
Before beginning this systematic review, research questions were laid out and refined to ensure that only the relevant studies were included and assessed. Additional information was included beneath each question to ensure transparency and clarity of what the research questions were asking. The research questions asked are as follows:
a) What are the common characteristics of effective interventions? And those of ineffective interventions?

b) What skills are targeted in interventions?
We defined skills as motor skills broadly divided into three categories including fine motor skills, gross motor skills, or both fine and gross motor skills. Skills were kept broad as some studies focused more specifically on skills such as balance, handwriting, sports-related skills and motor control. Other studies explored motor skills more broadly using standardised measures, and this categorisation allowed us to group studies with varying targeted skills together.
c) How is motor delay assessed prior to intervention?
We have defined motor delay broadly as any reference to a delay in one's ability to complete motor-related tasks or reach motor milestones later than the typical age expected.
d) Which skills demonstrate improvement?
As per research question b), motor skills were categorised as fine motor skills, gross motor skills, or both. Given the broad scope of studies that were included in this review, we did not look into specific skills such as walking, bimanual coordination and handwriting. Additionally, we did not require a certain effect size given the variability in sample sizes. Rather, skills were classified as ‘improved’ if the results section of a paper mentioned a distinct improvement in skills, compared to either a control group or participants at an earlier time point while ‘declined’ was a distinct decline in motor skills. Motor improvements were classified as ‘mixed’ if some skills showed improvement while others showed a decline. Skills were classified as having ‘no change’ if the intervention resulted in no reported change in outcome. Additionally, skills were classified as ‘similar’ if different groups showed similar outcomes, including groups receiving interventions for different amounts of time.
e) Are these interventions transferrable for non-clinical persons to use outside of a laboratory setting, if effective?
This question was answered by contextualising the features of effective interventions to determine if they would be transferrable to settings outside of a hospital, clinic, or therapy centre. This included understanding the potential specialised training needed for the therapy, associated costs and the equipment needed for implementation.
Methodology
Pre-registration
To ensure transparency in conducting our review, our study was preregistered to PROSPERO, the international prospective register of systematic reviews through the National Institute for Health and Care Research. This review was registered under the title ‘Interventions targeting motor delays in neurodivergent children’, with the registration number CRD42022367465. This preregistration detailed the intentions for the review including initial guiding research questions, and inclusion and exclusion criteria. To maximise the quality and reach of this review, adjustments were made to the preregistration criteria, including expanding database searches to include the Cochrane Library and PsycInfo. Additionally, we decided to include interventions from all contexts to expand the scope to include any potentially informative interventions. To focus our attention fully on motor development, we excluded discussions surrounding other developmental domains targeted by the included interventions.
Inclusion criteria and study selection
Following PRISMA guidelines, all studies were required to have a specified population, intervention, comparator and outcome. Participants included in the review consisted of children diagnosed with a neurodevelopmental disability with a genetic component or attention-deficit hyperactivity disorder (ADHD) or autism. ‘Children’ was defined as anyone under the age of 18, excluding studies that investigated prenatal or foetal intervention. ADHD and autism were included in the review as there is extensive literature on motor interventions. Though motor delays are not symptoms required for diagnosis, researchers are seeing more evidence of motor atypicalities that warrant intervention (Johnson et al., 2015). The intervention criterion was specified as any non-pharmaceutical, behavioural intervention focused on improving fine or gross motor skills. The comparator criterion was specified as a point of comparison either with time or population. Studies could meet this criterion if they included pre- and post-intervention measures to fulfil the time comparator or could have a separate control group entirely to fulfil the population comparator. The outcome was defined as any change – or lack thereof – in motor skills measured by standardized assessments, frequency of skill use, or measures specific to an intervention.
We ran searches on the following databases: Medline, Embase, Web of Science, Scopus, ClinicalTrials.gov, Cochrane Library and PsycInfo in November 2022, totalling 19.041 abstracts. The search terms were as follows:
Following deduplication, abstract screening, full-text screening and quality assessment detailed in the PRISMA flow diagram in Figure 1, a total of 119 reports were included in the final review (Page et al., 2021). Initial abstract screening was conducted by three members of the research team. Inter-rater reliability was established by having all three raters screen the same thirty studies, selected at random. These studies were rated, and any discrepancies were discussed in detail prior to further screening. All study abstracts were screened by the principal investigator, and 28% of abstracts were screened by an additional rater. With a total of 143 rating discrepancies, there was an inter-rater reliability of 96.2% when scoring abstracts. A total of 552 studies were included in the full-text screening. During full-text screening, all texts were double-screened to ensure that any potential studies were reviewed in detail. From the 552 studies that were reviewed, a total of 157 studies were included in the final review for critical appraisal with an inter-rater reliability of 93%. An additional 38 studies were excluded further during the study quality assessment informed by the Critical Appraisal Skills Program: Randomised Controlled Trial Checklist (CASP, 2020), as detailed in Figure 1, yielding a final total of 119 studies. For the purposes of this review, the following criteria were used: participant information, intervention details, intervention frequency, findings, data analysis and measures. Of the studies that were excluded, six were excluded for not meeting the participant criterion; 11 were excluded for having insufficient details on the intervention; eight were excluded for insufficient information on the frequency of implementation; two were excluded for not meeting the criterion for findings, eight were excluded for not meeting the criterion for measures; one was excluded for unethical practice. While the final exclusion was not listed under the critical appraisal criteria, the purpose of this systematic review is to better understand the attributes of motor interventions for children with neurodevelopmental disabilities so practitioners can implement those that are most beneficial for these respective populations. If an intervention is unethical and uses methods that cause physical or emotional harm to a child at any point, these will not be considered as these practices will not be tolerated in a research community that aspires towards neurodiversity-affirming care. Any discrepancies between raters were discussed in detail before determining which studies would be included in the final review.

PRISMA Flow Diagram.
Results
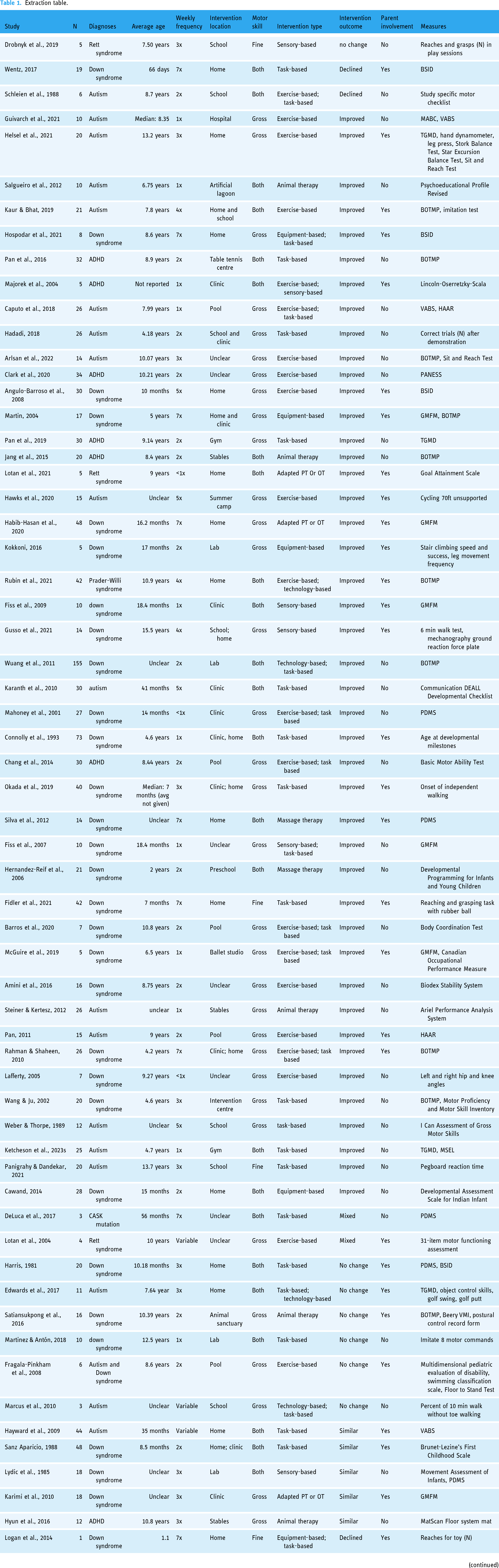
In the final review, there were a total of 60 quasi-experimental studies, 21 case studies and 38 randomized controlled trials. While neurodevelopmental disabilities were broadly represented in this systematic review, Down syndrome (N = 78), autism (N = 49) and ADHD (N = 13) were the most commonly investigated diagnoses. Less common diagnoses included Rett syndrome (N = 4: Drobnyk et al., 2019; Lotan et al., 2004, 2021; Mraz et al., 2016), Prader-Willi syndrome (N = 1; Rubin et al., 2021), Williams syndrome (N = 1; Conklin & Simonds, 2021), Angelman syndrome (N = 1; Han et al., 2022), Joubert syndrome (N = 1; Ipek et al., 2017), Pitt–Hopkins syndrome (N = 1; Casey et al., 2018) and CASK mutation (N = 1; DeLuca et al., 2017). For ease of reference, these included studies are all listed in Table 1, with quasi-experimental studies in pink, case studies in blue and randomized controlled trials in green. Improvements were classified as improved, declined, mixed, no change and similar. ‘Improved’ meant that at least one motor skill showed improvement, even if other skills showed no change. ‘Declined’ meant that at least one motor skill declined, even if other skills showed no change. ‘Mixed’ meant that some skills may have improved while others declined. ‘No change’ meant that there was no significant change in motor skills between the start and end of the intervention. ‘Similar’ meant that motor skills improved for the intervention group, but they were not significantly different from those of the control group.
Extraction table.
Objective 1: What are the common characteristics of effective interventions focused on motor skills? And what are the common characteristics of ineffective interventions?
To address the first objective (i.e. to identify the characteristics of successful and ineffective interventions), we examined intervention settings, frequency, parent involvement and the nature of the intervention. With respect to settings, these were divided into two subgroups: familiar (school, home and daycare) and unfamiliar (clinic, lab, intervention-specific i.e. horse stables, swimming pool and ballet studio). There were 50 studies conducted in familiar environments, 63 conducted in unfamiliar environments, seven which were done in both familiar and unfamiliar environments, and 14 where the setting was unclear. Of the interventions implemented in unfamiliar environments, 56 showed some level of improvement in children's motor skills compared to the control, three showed improvements similar to those of the control (Fragala-Pinkham et al., 2008; Ketcheson et al., 2023; Martinez & Antón, 2018) group, and four showed no reported improvement, but no measured decline (Aparicló, 1988; Hyun et al., 2016; Karimi et al., 2010; Lydic et al., 1985). However, there was significant variability in outcomes for interventions implemented in familiar environments. Thirty-eight of the studies showed reported improvements for interventions; four showed improvements equal to those of comparators (Harris, 1981; Hayward et al., 2009; Weerdmeester et al., 2016; Young, 2017); three showed no improvement (Edwards et al., 2017; Gerritsen, 2010; Marcus et al., 2010), six showed mixed results involving some improvement and some regression (Berg et al., 2012; DeLuca et al., 2017; Lotan et al., 2004; Mraz et al., 2016; Wentz, 2017) and only two showed reported reductions in motor abilities (Logan et al., 2014; Schleien et al., 1988). Thus, the familiarity and implied control of an intervention's setting may have an influence on how a child with a neurodevelopmental disability responds to an intervention.
Another element we explored was the frequency of intervention implementation which ranged broadly from less than once per week (N = 4), weekly (N = 20), twice weekly (N = 30), three times a week (N = 27), four times per week (N = 4), five times per week (N = 15), six times per week (N = 0) and daily (N = 10). There were eight studies that had variable frequencies. Of those implemented less than once per week, one article showed both positive and negative results (Columna et al., 2021) while the remaining three showed positive results (Lotan et al., 2021; Mahoney et al., 2001; Lafferty, 2005). Of those implemented once per week, only three showed no improvements while the remaining had positive outcomes (Gabriels et al., 2018; Ketcheson et al., 2023; Martinez & Anton, 2018). Only one intervention that was conducted twice a week had a negative outcome with a minor regression in jumping ability (Schleien et al., 1988). Similarly, only one intervention conducted three times a week had mixed findings (Mraz et al., 2016) and one intervention had a small but not statistically significant impact on motor skills (Drobnyk et al., 2019). One of the studies that was intended to be implemented four times per week (Berg et al., 2012) indicated that the family could not meet the time requirements of the intervention and the child was easily distracted.
Interventions were classified under a number of categories: exercise-based (N = 52), animal therapy (N = 10), technology-based (N = 11), equipment-based (N = 11), sensory stimulation (N = 14), adapted physical or occupational therapies (N = 7), task-based (N = 51) and massage therapy (N = 3). Some interventions fell into multiple categories. Of those task-based interventions that resulted in mixed findings, two of them were also technology-based (Berg et al., 2012; Mraz et al., 2016). One of these technology-based studies (Berg et al., 2012) did indicate that the family was not able to meet the time requirements of the intervention and that the child was easily distracted. Similarly, another study involving technology (Weerdmeester et al., 2016) which showed no significant improvement, noted that the non-significant improvements were likely from the exercise component of the intervention, rather than the virtual reality portion.
The final element we examined as a factor that could influence intervention efficacy was parent involvement. For a total of 71 interventions, there was no parent involvement at all. For the remaining 49 studies, parents were involved in some capacity of either observational, supporting, or implementing the intervention themselves. For some interventions, parent involvement was critical for children to feel comfortable enough for the intervention to be effective, such as massage therapy (Hernandez-Reif et al., 2006; Pinero-Pinto et al., 2020; Silva et al., 2012). For some task-based interventions, parents have the potential to serve as a distractor for the child, rather than an attentional support.
Objective 2: What skills are targeted in these interventions?
Examining skills broadly for the second objective, 70 of the studies examined only gross motor skills, seven examined only fine motor skills, and 38 examined both fine and gross motor skills. Of the studies that measured only gross motor skills, 56 showed improvements generally, six of these demonstrated no significant changes following the intervention, six showed improvements similar to those of controls, and two showed mixed findings (Lotan et al., 2004; Mraz et al., 2016). No studies showed only declines. Of the studies that focused on fine motor skills, six showed improvements, while one resulted in declines (Logan et al., 2014). Of those that measured both fine and gross motor skills, two showed declines (Schleien et al., 1988; Wentz, 2017), three showed improvements similar to controls (Hayward et al., 2009; Lydic et al., 1985; Sanz Aparicló, 1988), seven showed no changes and two showed mixed findings (Berg et al., 2012; DeLuca et al., 2017). As gross motor skills develop first and are critical to exploring one's environment and moving independently, it is understandable that these skills are the primary focus of many interventions. It is also possible that since fine motor skills require the coordination of many small muscles, it may be more difficult for interventions to target these.
Objective 3: How is motor delay assessed prior to intervention?
With respect to the third listed objective, motor skills were assessed in a number of ways, though standardized assessments were used most across all study types. The Bruininks-Oseretsky Test of Motor Proficiency (BOTMP, Bruininks, 1978) was used in 22 of the studies, followed by the Test of Gross Motor Development (TGMD, Ulrich & Sanford, 1985) used in 14 of the studies, the Gross Motor Function Measure (GMFM, Russel et al., 2002) in 12 of the studies, the Bayley Scales of Infant and Toddler Development (BSID, Bayley, 2006) in nine of the studies and Peabody Developmental Motor Scales (PDMS, Folio & Fewell, 2000) in six.
Objective 4: Which skills demonstrate improvement?
As summarized under Objective 2, gross motor skills showed the most improvement with 80% of the interventions reporting overall positive outcomes. With only seven studies focusing on fine motor skills alone, five of these showed significant improvements though these findings do not carry the same weight because of the smaller sample size. For interventions that examined fine and gross motor skills, 63% showed significant improvements. It is possible that interventions that examined both motor skill domains were attempting to address too many delays at a time, which resulted in dampened efficacy.
Objective 5: Are these interventions transferrable for non-clinical persons to use outside of a laboratory setting, if effective?
Many studies conducted in the home were shown to have positive outcomes following the interventions and could then easily be continued following the intervention completion. However, other interventions involved technology or equipment that is not accessible to most families. Studies using virtual reality showed promising results (Wuang et al., 2011), but this equipment may be too expensive to be recommended to families broadly. Similarly, some animal therapies were shown to be effective (Salgueiro et al., 2012; Steiner & Kertesz, 2012), but dolphin-assisted therapy is likely to be expensive, rarely available and inaccessible for most. Other interventions are highly transferrable to a non-clinical environment, such as massage therapy. Of the three massage therapy interventions that were included in the review, all showed improvement and two were implemented by parents (Pinero-Pinto et al., 2020; Silva et al., 2012). This could easily be continued following intervention completion and has no associated cost. Many studies involved physical activity such as yoga programs (Guivarch et al., 2021; Kaur & Bhat, 2019) or aquatic therapy (Chang et al., 2014; Marzouki et al., 2022), they demonstrated improvements and are feasible for many families. Yoga could be carried out within the home through online videos, and many local pools would have options for group classes or free swim if parents wanted to engage in the activity beyond a research setting.
Discussion
Evidence synthesis
There are promising findings resulting from this review paper from the attributes of effective and ineffective interventions, the transferability of interventions to non-clinical settings, and what skills are targeted for improvement. The results show that there is a level of transferability to non-clinical settings for interventions that are affordable, effective and require minimal equipment. Interventions involving yoga, massage, or swimming are accessible for many families and entail a level of adaptability for families to schedule sessions when it suits them best. While some interventions did show positive outcomes, animal-based interventions (Jang et al., 2015; Salguiero et al., 2012; Steiner & Kertesz, 2012) are not easily transferable, typically requiring an intervention-specific space and a trained professional. Similarly, equipment-based interventions that were found to be effective (Hospodar et al., 2021; Kokkoni, 2016; Martin, 2004) require the specific equipment provided by researchers. This means that families not involved in that unique study may not be able to access the same means of intervention. It is helpful to understand what aspects of an intervention made them effective. Similarly, it is beneficial to understand the limitations of transferability. Other interventions showed promising results as well, but the time commitment and location demands can decrease intervention fidelity, thereby decreasing its efficacy. As supporting a child with a disability can include physiotherapy, speech and language pathology appointments, and potential other time commitments, it is important that interventions empower families to work on their unique goals for their child, including operating on their own timelines. Regarding time commitments, the results show that interventions were most effective when implemented twice a week while interventions were less effective if they were too frequent or infrequent. If an intervention requires an unreasonable time commitment, a family is likely unable to attend the number of sessions necessary for the intervention to be fully effective. On the opposite side, therapies that were too short or didn’t occur as often were ineffective. It is possible that there wasn’t sufficient time for the intervention to properly take effect.
The role of parents in intervention implementation was variable, highlighting the differences between individual children and disabilities, broadly. While some children improved when their parent was present, which could demonstrate potential scaffolding or emotional support for the child, other studies did not show changes or a decrease in motor skills, potentially resulting from distractibility or an inclination to familiar motor skills rather than new ones.
Regarding the motor skills targeted by interventions, gross motor skills were most frequent. Given that gross motor skills precede fine motor skills in development (Department of Education, n.d.), it is understandable that this developmental domain would be a priority for intervention work. Additionally, this finding exemplifies the importance placed on improving certain motor skills over others. One's ability to walk and balance while standing would have more of an immediate impact on a child's life given that gross motor skills are often a pre-requisite to attaining fine motor milestones.
Additionally, this review provided valuable insights regarding what could make an intervention effective including implementing the intervention in an unfamiliar environment. While previous literature has provided evidence to suggest that placing a child in a novel environment interferes with their ability to learn a new task (Falk et al., 1978), it is possible that learned play routines (Vygotsky, 1967) can be changed when moved to a new environment. This could potentially allow children to engage in motor behaviours they had not engaged in previously. As such, this aspect of intervention work could be explored by future researchers.
Limitations
A limitation of this review is that it is influenced by publication bias because studies had to be published to be included. Most interventions showed improvements, though it is possible that other motor interventions have been investigated and have not been published on the basis of null findings. Additionally, there is a gap in the literature resulting from the rarity of certain diagnoses, such as Rett syndrome and Pitt–Hopkins syndrome. Some studies showed negative outcomes, although they consisted of a single participant, making it difficult to draw conclusions based on intervention rather than diagnosis or individual differences.
Another limitation is that this is a narrative systematic review, meaning that the various studies are not weighted according to sample size or effect size. This is a beneficial first step to developing a transdiagnostic understanding of interventions for neurodevelopmental disabilities, as this review was able to identify characteristics of interventions that may promote or prevent efficacy. While a meta-analysis could be beneficial for future research, some studies did not provide an effect size or the data necessary for calculating effect size. Additionally, this review sought to explore more contextual factors and diverse outcome measures that are not suitable for meta-analysis.
Future directions
Further directions could include exploring the mechanisms of interventions being effective or ineffective within the home, such as distractibility, parent scaffolding and proclivity for established behaviours. It would be beneficial for researchers to understand why familiarity with the environment may be beneficial for some children while it promotes pre-established behaviours for others. In a similar vein, practitioners could focus on providing resources to families that allow them to implement interventions within the home and that do not require professional support. Whilst this review was inclined to avoid precluding the inclusion of small-scale studies with valuable information regarding contextual factors, further research that explores randomised controlled trials with larger sample sizes could be beneficial in making more generalisable claims. However, as our research wanted to include rare aetiologies such as Rett syndrome and Pitt–Hopkins syndrome, some studies did not include effect sizes and sufficient sample sizes necessary for a meta-analysis, though this could be informative in studies to come. Though our review was not designed to target narrower age groups, diagnoses, or intervention methods, it would be beneficial for future research to narrow the focus to explore intervention efficacy within these respective groups. This would be beneficial as it would allow researchers to determine what aspects of an intervention make it effective for some children while it may not be effective for others. As research has been progressing and making great strides with each passing month, new future reviews could include the most recent evidence surrounding motor interventions and include the aforementioned research questions.
As the goal of motor interventions is to optimise outcomes and improve the quality of life for children with neurodevelopmental disabilities, this review provided a better understanding of the characteristics of effective and ineffective interventions, transferability to non-clinical settings and the various measures used to assess motor skills. This will inform practitioners and researchers as they explore motor interventions for their respective populations.
Footnotes
Acknowledgements
We would like to extend our gratitude to Alexandra Hendry for her guidance and support as we prepared this review.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
