Abstract
Background
Some practitioner-delivered (eg, acupuncture) and self-directed (eg, yoga) complementary and integrative health (CIH) therapies are evidence-based for chronic pain management. Providers often follow recommendations to encourage patients to take active roles in their health care by using self-directed therapies in addition to CIH therapies they deliver. Doing so might be more effective than using practitioner-delivered CIH therapies alone, however we are unaware of studies qualitatively examining this issue.
Objective
As part of our VA pragmatic study APPROACH (Assessing Pain, Patient-Reported Outcomes and Complementary and Integrative Health) among 6453 veterans with chronic musculoskeletal pain, we qualitatively examined patients’ narrative reports of CIH therapy use to explore how using practitioner-delivered CIH therapies with and without self-directed CIH therapies affected their health and well-being.
Methods
We conducted qualitative telephone interviews with 125 patients at six VA medical centers from March 2022 March 2023, asking if their use of CIH therapies affected several health conditions: depression, anxiety, pain, fatigue, sleep, quality of life, and self-empowerment to take care of one’s own health. We used deductive and inductive thematic analysis.
Results
Half or more of reported CIH therapies helped their pain, quality of life, depression, sleep, and self-empowerment to take care of their own health, but few reported the therapies affected fatigue. Using a combination of practitioner-delivered and self-directed CIH therapies appeared more helpful than using only practitioner-delivered therapies for depression, anxiety, quality of life, fatigue, and self-empowerment. However, for pain or sleep, similar percentages of patients reported using a combination or only practitioner-delivered CIH therapies helped.
Conclusions
Using a combination of practitioner-delivered CIH therapies appear more helpful than using only practitioner-delivered therapies for most examined health conditions, except they appeared similarly helpful for pain and sleep. Chiropractors, acupuncturists and massage therapists might want to encourage patients to participate in self-directed therapies.
Introduction
Some practitioner-delivered complementary and integrative health (CIH) therapies such as acupuncture, chiropractic care and massage therapy are evidence-based for chronic pain management, as are some self-directed CIH therapies (eg, yoga, meditation and Tai Chi).1-8 Providers often follow National Academy of Medicine recommendations 1 to encourage their patients to take more active roles in their health care and use self-directed therapies. Using both self-directed and practitioner-delivered CIH therapies might be more effective than using practitioner-delivered CIH therapies alone if they increase one’s feeling of efficacy over one’s health. 9 For example, feeling a lack of control over one’s pain is related to responding poorly to pain management therapies10,11 whereas patients who feel self-efficacy to control their pain actually do improve their pain.9,12-14 As such, a key question in the CIH therapy field is whether patients using both self-directed and practitioner-delivered CIH therapies have different perspectives on how their health and well-being are affected, relative to the perspectives of patients who use only practitioner-delivered CIH therapies.
As part of its Whole Health transformation from a disease care system to a whole person health care system,15,16 the Veterans Health Administration (VA) has prioritized making evidence-based CIH therapies available for pain and pain-related comorbidities such as anxiety and depression. 16 Given the large numbers of patients using CIH therapies, the VA is an ideal setting in which to explore patients’ experiences with practitioner-delivered and self-directed CIH therapies.
Our large-scale pragmatic study, APPROACH (Assessing Pain, Patient-Reported Outcomes and Complementary and Integrative Health), is quantitively and qualitatively examining patient-reported effects of CIH therapy use on pain and pain-comorbid health conditions among 6453 veterans with chronic musculoskeletal pain at 18 VA medical centers. 17 It addresses the question of the relative effectiveness of practitioner-delivered CIH therapies with and without the addition of self-directed therapies. This paper presents the results of our semi-structured qualitative interviews with a subset of veterans to examine patients’ perspectives how using CIH therapies affected their health and well-being.
Methods
We conducted semi-structured qualitative interviews among 125 VA patients at six of the eighteen VA medical centers in the APPROACH study from March 2022 to March 2023. We asked about the ways in which veterans’ use of six CIH therapies might have affected their health and well-being. Those six therapies were chiropractic care, massage therapy, acupuncture, meditation, Tai Chi/Qigong, and yoga. The VA Central IRB approved this study.
Sampling Methods
We used the VA’s electronic health record data to identify the six VA medical center study sites from which to recruit patients to interview. We purposefully sampled two VA sites with higher volumes of CIH therapy provision, two with average volumes, and two with lower volumes. We then identified veterans receiving any of the following in the previous 6 months: three or more chiropractic care visits, three or more massage therapy visits, five or more acupuncture visits, five or more meditation sessions, five or more Tai Chi or Qigong sessions, or five or more yoga sessions.
Our target sample size was 25 participants in each of three study groups: (1) those using only practitioner-delivered therapies, (2) those using only self-directed therapies (in-person and virtual), and (3) those using a combination of practitioner-delivered and self-directed CIH therapies. We also targeted 25 veterans using only virtual self-directed therapies because the study was conducted in-part during the COVID-19 pandemic when self-directed CIH therapies were predominantly delivered virtually. We examined those using virtual care therapies separately given the likelihood of virtual and in-person CIH therapies having differing perceived effects, 18 although they represented only 8% of veterans who completed the APPROACH 6-month survey. 19
VA CIH Therapies
Chiropractic, acupuncture, therapeutic massage, and in-person Tai Chi, Qigong, yoga, and meditation therapies were delivered by certified practitioners (eg, healthcare provider, therapist, instructor) in one of the six VA medical centers participating in our APPROACH study. Virtual self-directed CIH therapies (eg, meditation, yoga, Tai Chi, or Qigong) were delivered by instructors in synchronous classes via VA video software. Given our APPROACH study is a pragmatic trial, it studied use of therapies as they were given, and did not impose uniformity on therapies. In VA, these therapies differ somewhat in their length and content, a heterogeneity which should increase the generalizability of the results.
Semi-structured Interview Content
We used a semi-structured interview guide containing 18 questions to ask veterans about how the therapies might have affected their health and well-being, if at all. It included probes to ask about pain, anxiety, depression, sleep, fatigue, quality of life, and self-empowerment to take care of their own health (see Supplemental Material 1, Interview guide). Veterans using combinations of practitioner-delivered and self-directed therapies were questioned about their motivations and thoughts about which therapy helped which symptoms. We also asked if they used these virtually or in-person.
Data Collection
A study coordinator (DK) mailed 280 veterans a study information packet containing: (1) an invitation letter informing veterans that a study team member would call, (2) the study coordinator’s phone number and email for veterans to use if they wished to opt out, and (3) a patient information sheet with detailed study information. Approximately 2 weeks after invitations were mailed, if eligible participants did not opt out, the study coordinator phoned patients to inquire about study interest. During the data collection period, we attempted to contact 238 veterans. No more than five telephone attempts were made to any individual. During enrollment calls, the study coordinator provided study details, ensured participants’ informed consent, and asked for consent to record the interview. Of the 238 veterans, 113 were unreachable by phone, declined to be interviewed, or were excluded for having more than a six-month time gap since their last CIH therapy. All interviews were conducted by three authors, one with PhD-level training in qualitative methods (MM) and two research assistants (MMc, DK) with qualitative training took notes. Interviews were recorded on Teams then transcribed by VA transcription services. We successfully completed 125 semi-structured telephone interviews that lasted 20-50 minutes and compensated participants with a gift certificate upon completion.
Analysis
A five-person qualitative team (MM, MMc, DK, and MS) used NVivo 12 to code transcripts using a deductive-inductive approaches based on interview guide domains and emerging content. First, we coded interviews using the health conditions we asked about as domains: pain, anxiety, depression, sleep, fatigue, quality of life, and self-empowerment. Next, we used a rigorous five-stage analysis process (ie, compiling, disassembling, reassembling, interpreting, and concluding) 20 to develop themes and subthemes from grouped coded excerpts within each domain. Through discussion and consensus, our four-person qualitative team analyzed data, and reviewed themes and subthemes to assure patients’ perceptions were accurately captured in the final narrative.
We coded veterans’ perceptions of the effects of using CIH therapies as “positive” when veterans reported specific symptoms and a perceived benefit (eg, helped with pain, anxiety, etc.) or “negative” when they perceived a worsening effect on a symptom (eg, my pain felt worse). We coded them as “null” when a veteran reported having a symptom, but that the CIH therapy did not improve them (eg, I have depression, but yoga did not help). Given the large size of the qualitative dataset, we also descriptively summarized the findings by counting the number of responses to help discern patterns in our coding. 21 We calculated the percentage of veterans using multiple therapies not only to describe the population, but also because the number of therapies each person used could be associated with effects. For veterans using multiple therapies of the same type, we did not interview representative samples of their health effects.
Results
Demographic Characteristics

Concurrent Therapy Use
Therapies Used Concurrently

Patients’ Perspectives of How Using CIH Therapies Affected Their Health and Well-Being
To simplify the presentation of our qualitative findings, we condensed our study groups into three: (1) veterans using a combination of practitioner-delivered care and self-directed CIH therapies, (2) veterans using only practitioner-delivered CIH therapies and (3) veterans using only self-directed CIH therapies (both in-person and virtual). The quotations shown are ones the project team agreed succinctly articulated health outcomes from the hundreds of quotations we captured.
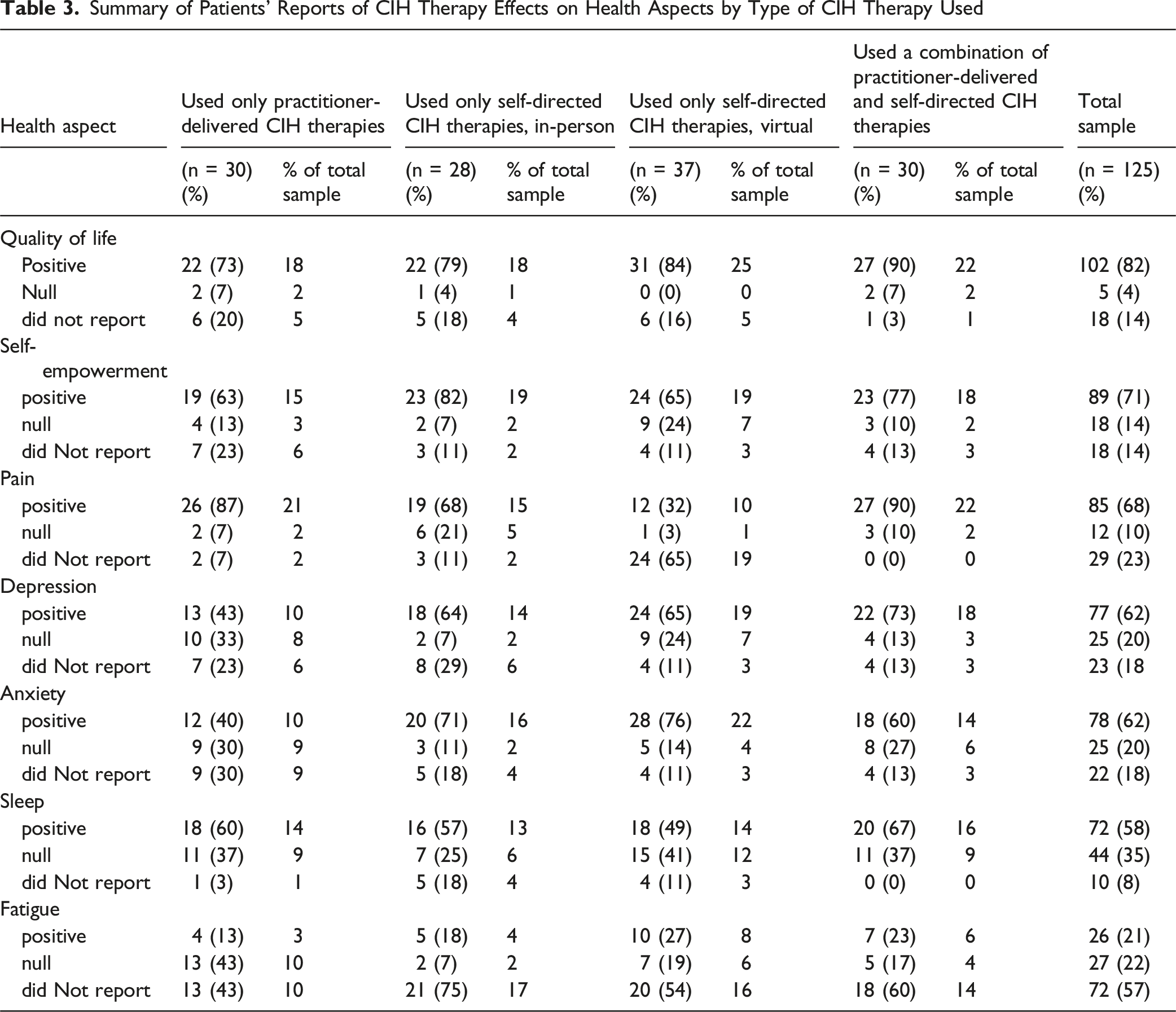
Summary of Patients’ Reports of CIH Therapy Effects on Health Aspects by Type of CIH Therapy Used
Patients’ Perspectives on How Adding Self-Directed CIH Therapies to Practitioner-Delivered CIH Therapies Affected Their Health and Well-Being
Relative to veteran patients using only practitioner-deliver CIH therapies, it appeared higher percentages of veteran patients using a combination of practitioner-delivered care and self-delivered CIH therapies reported therapies helped their quality of life, depression, anxiety, fatigue, and self-empowerment to take care of their own health. (see Table 2). Relatively similar percentages of veteran patients using those 2 categories of CIH therapies helped their pain and sleep.
Pain
Almost all veterans using a combination of practitioner-delivered and self-directed CIH therapies reported positive effects on pain, as did those using only practitioner-delivered CIH therapies. However, more veterans using a combination of CIH therapies reported positive effects than those using only self-directed CIH therapies. Regarding the effects of using a combination of therapies, a veteran using chiropractic care and yoga reported, It has absolutely made a life-changing experience. Before I started doing it, I felt excruciating pain every morning, and that’s all but subsided… there were times I couldn’t leave my house, I was in so much pain… that has definitely gone to rehabilitating my lower back… to be able to function and continue on with every day—normal, everyday things that I couldn’t do before…. chiropractic for the physical, and then the yoga also helps… but I get more mental relief and release from yoga. So it’s both physical and mental. Veteran 106
Another using acupuncture and yoga said, I feel like the combination between the acupuncture and the yoga have been the most helpful... The yoga… it’s like a routine, a ritual, and it also helps me to be mindful… the acupuncture… addresses some really deep pains that weren’t able to be addressed with other methods. Veteran 006
Depression
Most veterans using a combination of practitioner-delivered and self-directed CIH therapies reported the combination lifted their mood, even tamed their suicidal ideation, whereas less than half of those using only practitioner-delivered therapies reported similarly. For example, a veteran using chiropractic care and yoga said, I do get depressed… when the chiropractor gets done with me, or I get done with yoga, I can bend better for a while, and I can do things… they keep me from being suicidal, I guess, that’s the best thing…They kind of bring me out of my depression enough to where I don’t do anything stupid. Veteran 011
Anxiety
Over half of the veterans using a combination of practitioner-delivered and self-directed CIH therapies reported positive effects on their anxiety such as feeling more relaxed, put into a better mindset, and feeling like they were taking care of themselves, whereas less than half of those using only practitioner-delivered care reported similarly. One veteran using acupuncture and yoga stated, I do have anxiety. [Yoga] just makes you feel better…As long as I do [yoga], and keep exercising, keep moving, I guess, is what I want to say, [I] feel better. [I] can stay ahead of that anxiety, so to speak…I think [yoga and acupuncture] work in different ways. I would say that yoga probably is the best because, like I said, the movement and that gets [me] moving. But yet, the acupuncture, kind of calms [me] down too…And some of that acupuncture too, it sort of helps [my] mood. Veteran 097
Sleep
More than half of veterans using a combination of therapies reported positive effects on their sleep, such as falling asleep faster, having uninterrupted sleep, longer sleep, or a combination of those. However, similar percentages of veterans using only practitioner-delivered therapies reported these effects. Some veterans reported waking up less frequently due to a decrease in nightmares or flashbacks, with 1 veteran receiving acupuncture, Tai Chi, and yoga stating, I’ll just say I’m relieved, I can maybe focus on what I’m doing at the time, the acupuncture or Tai Chi, or the yoga, and take my mind off of the flashbacks and nightmares which I have. Veteran 104
Fatigue
Few using a combination of practitioner-delivered and self-directed CIH therapies reported having positive effect on their fatigue while others reported no (null) effects, or even negative effects if they had a gap between therapy sessions. However, higher percentages of those using a combination of therapies had positive effects on fatigue. One veteran receiving acupuncture and yoga reported a positive effect saying, If I’m doing yoga twice a week, and the acupuncture one every three weeks, I don’t get as tired through the day… and it may help my sleep at night ‘cuz I don’t lay around during the day. I am active. Veteran 097
Quality of Life
Most veterans using a combination of practitioner-delivered and self-directed CIH therapies reported positive effects on their overall quality of life, improving their wellbeing, reducing their pain, and giving them the ability to be more active to participate in daily tasks and hobbies. One veteran using acupuncture, Tai Chi, yoga, and meditation recounted, For me it's a combination of all of them. It gives me spiritual, mental, and physical health. I'm back in the driver's seat now of my well-being. Before, I lost… who I was… I’m a medic by trade… always helping others… once… my mission was over it just all caved in on me. And I really lost who I was… mentally, physically, and spiritually… the combination of all these programs… gave me back my identity and really taught me to believe in myself... And more than anything else, I had to have that back because I lost that… I'm still working on it every day… it's a work in progress. But that's what it really gave to me all these programs put together. Veteran 040
Additional Benefits of Using a Combination of Self-Directed and Practitioner-Delivered CIH Therapies
Those using a combination of CIH therapies reported becoming more mindful, having mental relief, having an improved range of motion, and having pain relief and subsequent improvements in sleep. A veteran using chiropractic care, yoga, and Tai Chi said, The chiropractor… puts everything in alignment… I needed that, first…. then I got into… yoga… Qi Gong and Tai Chi class, every day…. for about six weeks, doing chiropractic every month. Within two months, my chiropractor was remarking at how much better toned… my muscles were… she had to do much fewer adjustments. And my range of motion had improved exponentially. My pain level had dropped within about three weeks…. For six months…. I couldn't sleep at night because I couldn't find a comfortable position. It didn't matter what I did. Ice, heat, pillows, lack of pillows it didn't matter. Within three weeks, I could just sleep. Because my body didn't hurt anymore. Veteran 012
Others reported that the effects of a combination of a self-directed and practitioner-delivered CIH therapies build on each other or sustains pain relief that would otherwise not happen. One veteran using chiropractic care and yoga stated, I think that it’s the way that it’s integrated… the adjustment through chiropractor, but the yoga helps sustain it and make it stronger.” (Veteran 106) Another receiving acupuncture, chiropractic care and yoga reported, “I think it’s been a joint effort, so because I think every one of them got a point that they hit on… I think in conjunction they’re great together… Each one of them adds something every time. (Veteran 070)
Veterans Using Only Practitioner-Delivered CIH Therapies
Of the 30 veterans using only practitioner-delivered CIH therapies, most reported the therapies helped their pain and quality of life while over half reported the same for their sleep and self-empowerment to take charge of their health (see Table 2).
Pain
A majority of the veterans in this group reported a reduction in pain level and that consistent therapy visits helped keep their pain levels down. For example, 1 veteran using chiropractic care and massage therapy said, I couldn’t live without the chiropractic care. I don’t want to live without the massage piece because it’s so much more beneficial... I can’t even put words to it…. Going on a consistent basis helps keep my pain level down. Veteran 105
Depression
Less than half who used only practitioner-delivered CIH therapies reported positive effects on their experiences of depression while some reported no (null) effects. Positive effects on depression most often included a reference to pain and doing daily activities without worry. For example, a veteran using chiropractic care recounted, When you’re in depression and you’re hurting, you’re in a fetal position… wondering what’s going on and why you want to live anymore. And chiropractic can help take a lot of that pain away… because you’re able to get something done during the day, and… act normal, instead of being all hunched up and in pain, and not doing anything but taking aspirin and being in the fetal position. Veteran 079
Anxiety
Less than half of veterans in this group reported positive effects on their experience of anxiety. However, when they did report positive effects, they stated that they were in a better mindset after therapy, with a veteran using chiropractic care and acupuncture recounting, Severe PTSD, 22 combat deployments. I've watched… friends die… people die. I've had to kill people. I was a Green Beret. That tension is centered between my shoulder blades up to the top of my head… if I start thinking about [it], I start locking up. With the acupuncture it puts me in a better mindset. The relaxation comes, and the chiropractor when they release all that, that tension goes away… I don't know why, but my mind automatically starts going towards happier thoughts. Veteran 001
Sleep
Over half of veterans (60%) from this group reported positive results of practitioner-delivered CIH therapies on their sleep, with one using acupuncture saying, Calming me down helps get me to sleep … once I wake up, I would be up for the rest of the night but now I can get up and use the bathroom and go back to sleep... Veteran 029
Fatigue
Using only practitioner-delivered CIH therapies seemed to have little positive effect on patient experiences of fatigue. We found 43% of veterans in this group reported null effects on their fatigue, while 13% of them reported positive effects. A veteran using acupuncture said, Some of the acupuncture… I can get a boost of energy to… my metabolism… it’s given me a lot of energy. Motivation. It’s kind of helped reset my mindset on how I look at things. Veteran 038
Quality of Life
Using only practitioner-delivered CIH therapies seemed to do less for veterans, compared to those using a combination of therapies or only self-directed therapies, in terms of improving in their social relationships, their spiritual health and personal development. Of the 30 veterans in this group, 73% reported a reduction in pain that allowed them to be more active and do the things that they would otherwise not be able to do. One veteran using acupuncture said, Since I've been using acupuncture, I have less pain as I did before. Before, I had so much chronic pain on a daily basis that sometimes it really interfered with me doing things. But since I've been doing acupuncture, I have less pain, I can move more. I can cope more. I actually can be more…active and moving around…along with acupuncture, I actually am able to do some exercises on a daily basis, whereas before I would have to stop because I would be aggravating the nerve systems or whatever. But with acupuncture, I can actually move. I have more movement in my joints and everything. Veteran 038
Self-Empowerment
Over a half of veterans from “the group using only practitioner-delivered therapies” (63%) reported that using these CIH therapies helped them take charge of their health, with one veteran using chiropractic saying, I do feel like I have a lot more control over… what I can do now… I have a sloped backyard; I'm not scared to walk down my yard and come back up it because I might fall. Veteran 001
Veterans Using Only Self-Directed CIH Therapies
We found that similar percentages of veteran patients using only self-directed therapies reported those therapies helped their depression, fatigue, quality of life, and self-empowerment relative to those using a combination of provider-delivered and self-directed CIH therapies. However, many fewer patients using only self-directed CIH therapies reported they helped their pain, and slightly fewer reported they helped their sleep or anxiety. As a minor point, among those using only self-directed CIH therapies, it appeared somewhat higher percentages of veterans using only
Pain
Over half of veterans using only in-person self-directed CIH therapies reported pain relief. They reported learning tools for managing their pain (eg, breathing techniques, taking their mind off their pain). One using in-person yoga said, I would say yoga probably has helped the most because… I do it more frequently… once or twice a week… it either stops or eases the pain to the point to where… If I’m like a 7 in pain… it brings it down to maybe a 2 or 3. And in some cases, it just goes away all together for the day and then tomorrow’s a new day. Veteran 134
Only seven veterans using only self-directed CIH therapies reported negative and/or null effects on their pain. For example, one veteran using yoga and meditation stated, I thought my back would get a little stronger, but it keeps on hurting. Veteran 127
Depression
A little over half of veterans using only in-person or virtual self-directed CIH therapies reported the therapies helped alleviate their worry and elevate their mood by taking their mind off negative aspects of life. Others stated that using self-directed CIH therapies provided them a better perspective on life (eg, be present, more insightful, redirect their thoughts, and a more positive focus/thinking). One veteran using meditation recounted, Anyone that knows about depression knows it can take you into some really, really dark places... And if you’re not strong, if you don’t have the right support, it can really just lead you to some areas that for some, it’s hard to come back from. And having that avenue to concentrate and deeply get your mindset where you can focus on nothing but good…reclaim yourself… pinpoint in your head… that you are greater, and you are larger than what depression is…Being able to meditate, concentrate, lean on all of the good, all of the good that you can just think about…that excitement and that good part of your life, that space you’re in at that moment, regardless of how many years it may have been, just think of all the good that you can possibly surround yourself with, to overcome and know that making it another day, taking another step forward, will help you a long way, than to just sit, soak, and allow yourself to fall deeper and deeper into one of the enemy’s strongholds. Veteran 118
Anxiety
The majority of veterans using only in-person or only virtual self-directed CIH therapies reported feeling more relaxed, more positive and at ease from using self-directed CIH therapies. Some said that they learned tools to help them calm their mind and body (eg, stop and listen, be still, take a time out), with 1 veteran using Tai Chi and yoga saying, I would say yoga. It helps with anxiety. I was in treatment for alcoholism, and they offered the class and I do have some anxiety that comes and goes that is very mysterious— I don’t see when it’s coming or going. The yoga seems to help, it just felt like maybe it was the group setting the participation maybe I felt like a sense of kind of beginning to learn how to just put aside these little difficulties and concentrate on the moment and it’s such a challenge to do it but once you get away from it, it’s hard to remember how good it was. It is so calming. Veteran 003
Sleep
Using only self-directed CIH therapies had nominal positive effects on sleep. Slightly more than half of the veterans using in-person therapies and almost half using only virtual self-directed CIH therapies reported benefits, such as waking up less frequently due to a decrease in nightmares or flashbacks with 1 veteran using meditation stating, I call the regular crisis line and they have done guided meditations with me and that has been beneficial [after waking up from very bad nightmares, feeling sick]. Veteran 123
Fatigue
Only a few veterans using only in-person or only virtual self-directed CIH therapies reported positive effects on fatigue. However, a gap in therapy might have negative consequences, as one veteran using Tai Chi stated, When I go to Tai Chi, I don't feel as tired. Now, since I've missed it, I've missed several, quite a few sessions, and it's like I’m tired all the time. Veteran 063
Quality of Life
Proportionally more veterans who used only self-directed CIH therapies reported improvements in their spiritual health and personal development than the other groups. They also reported physical, mental, and emotional improvements as well as an improved sense of self and more control over their body and emotions. One veteran using meditation said, … the state of mind I existed in the military, meditation has helped me escape from that… and go back to normal state of mind where I'm not living in constant fear and threat… all of those things help me to think clearer, manage my life better, and they improve on my relationships with other people. Veteran 117
Self-Empowerment to Take Care of One Own’s Health
Most veterans using only in-person self-directed CIH therapies reported positive effects on their sense of knowledge about themselves and their health. Somewhat fewer patients using only virtual CIH therapies reported similarly. Overall, veterans in the self-directed therapy groups reported more motivation to do exercises or self-directed CIH therapies on their own. One veteran using in-person Tai Chi stated, These new programs have made me feel like I am in charge of my health, because they’re there, and I can do them… I’m a big believer … no one cares more about me than me. Veteran 113
Discussion
Our semi-structured qualitative interviews with 125 VA patients having chronic musculoskeletal pain provided rich detail on patients’ perspectives of how using practitioner-delivered CIH therapies with and without self-directed CIH therapies affected their health and well-being.
Using both self-directed and practitioner-delivered CIH therapies appeared more helpful than using only practitioner-delivered therapies for improving quality of life, depression, fatigue, anxiety, and self-empowerment. However, for both pain and sleep, adding self-care CIH therapy to a practitioner delivered therapy did not appear to be more beneficial.
We found that most patients using only practitioner-delivered therapies reported those therapies alleviated their pain whereas most patients using only self-directed therapies reported those therapies improved their quality of life and self-empowerment over their health. Also, we found that roughly equal percentages used multiple CIH therapies among those using (1) only practitioner-delivered therapies (43%) or (2) only self-directed therapies (50%) and that of those using both practitioner-delivered and self-directed therapies only 17% used combinations of multiple types of therapies concurrently. As such, it does not seem likely that veterans using more self-directed and practitioner-delivered therapies concurrently reported better health benefits.
Veterans using a combination of therapies highlighted that the therapies seem to build on one another, buttressing the effects of each. This finding is consistent with prior studies that highlighted the synergistic effects of combining diverse therapies 22 such as combining practitioner-delivered with self-directed CIH therapies. 23 Veterans also reported that using a combination of types of therapies led to sustained relief of their symptoms better than using only practitioner-delivered CIH therapies. That is, using self-directed therapies (eg, meditation, yoga and Tai Chi) might result in sustained symptom relief by providing patients with tools to modify their mood and anxiety on an ongoing basis through breathing techniques and calming the nervous system.17,19
Our study has limitations. We interviewed a subset (n = 125) of veterans using CIH therapies at VA, which was 53% of the sample we contacted. The respondents might have been those who were eager to convey personal stories of how CIH therapies improved their lives. As such, the results might not be generalizable to the broader veteran population or the general population. Also, we could not directly ask interviewees about the relative effectiveness of using self-directed, practitioner-delivered, or a combination of therapies because pilot interviews revealed interviewees understandably had a difficult time articulating how each therapy was helping them in specific ways. The sample includes patients who used CIH therapies for only 6 months, so the findings do not reflect long-term use.
However, our study demonstrated the synergistic and sustained effects of adding self-directed to practitioner-delivered CIH therapies for particular health conditions. It was able to capitalize on its large sample to select a large number of patients with differing use of CIH therapies to address the research question. It used qualitative methods to provide rich detail of patient experiences and uncover issues that are not asked about in surveys, not to determine effectiveness. Determining effectiveness quantitatively was the goal of our companion paper. 24
Conclusions
Our large-scale qualitative exploration found that patients using self-directed CIH therapies such as yoga, meditation or Tai Chi in addition to practitioner-delivered therapies such as acupuncture, massage therapy or chiropractic care appeared to report improvements in their depression, anxiety, quality of life, fatigue, and self-empowerment more than patients using only practitioner-delivered therapies. Similar percentages of patients in these groups described benefits for pain and sleep, whereas using only a self-directed therapy did not appear to benefit as many people. As such, practitioners delivering CIH therapies might consider recommending self-directed CIH therapies to their patients with these health conditions.
Supplemental Material
Supplemental material - Patient Reports on How Well Combining Provider-Delivered and Self-Directed Complementary and Integrative Health Therapies Help Their Health and Well-Being
Supplemental material for Patient Reports on How Well Combining Provider-Delivered and Self-Directed Complementary and Integrative Health Therapies Help Their Health and Well-Being by Melissa Medich, PhD, MPH, Marlena H. Shin, JD, MPH, Michael G. McGowan, MA, Danna R. Kasom, BS, Briana Lott, MPH, Steven B. Zeliadt, PhD, MPH and Stephanie L. Taylor, PhD, MPHA in Global Advances in Integrative Medicine and Health
Footnotes
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: VA HSR&D, SDR# 17-306. Assessing Pain, Patient Reported Outcomes and Complementary and Integrative Health (APPROACH) study, supported by VA Health Services Research & Development, Service Directed Research 17-306 (Taylor/Zeliadt, PIs). Dr Taylor’s work was supported by a Veteran Health Administration Research Career Scientist Award. RCS 23-082, Office of Patient-Centered Care and Cultural Transformation and Quality Enhancement Research Initiative. PEC 16-354.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Disclaimer
The views expressed in the submitted article are our own and do not reflect those of the Veterans Health Administration.
Supplemental Material
Supplemental material is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
