Abstract
Introduction
Individuals with traumatic spinal cord injury (TSCI) are dissatisfied with their chronic pain management. A biopsychosocial approach has been proven to improve chronic pain. Guidelines are required to holistically manage chronic pain in the TSCI population.
Methods
A Delphi study was conducted to gain consensus on design principles for chronic pain in the TSCI population, for the Western Cape of South Africa. Purposive sampling was used to recruit first-line primary health care providers from primary health care settings in the Cape Metropolitan region. Participants were asked for consent on principles pertaining to the assessment, education and planning for chronic pain management, pharmacological and non-pharmacological therapy for neuropathic and nociceptive pain, as well as the monitoring of chronic pain and referral of resistant pain. For consensus analysis, a median of 3.24 or higher was considered in addition to two categories of consensus, namely weak consensus (50%–70%) and strong consensus (>70%).
Results
The first-line primary health care providers agreed on eighteen principles to guide chronic pain management in the TSCI population. Consensus could not be reached on the second to fourth line pharmacological management of neuropathic pain.
Conclusion
The agreed upon design principles may be considered as starting points for implementation at the primary health care level in the Western Cape of South Africa.
Keywords
Introduction
Chronic pain has high prevalence rates in the TSCI population, surfacing within the first few years following the traumatic incident.1-3 Chronic pain in this study population consists of nociceptive pain (NP) and neuropathic pain (NeuP).
The focus of chronic pain management in the TSCI population, in South Africa leans towards a pharmacological approach, which may be evident in two studies depicting opioid misuse amongst TSCI survivors and individuals expressing the lack of non-pharmacological referrals from the primary health care setting.4,5 Persons with TSCI (PWTSCI), locally and abroad, have voiced their dissatisfaction with the current medical approach to chronic pain management, accentuating its temporary pain relief and undesirable side-effects.5-8
A recent study has demonstrated the physiotherapist use of non-pharmacological management strategies for chronic pain in the SCI population and these include cognitive behavioural therapy, electrotherapy/TENS, desensitisation, graded activity, joint mobilisation, myofascial release pain neuroscience education, exercises, neural tissue mobilisation and self-management techniques. 9 The efficacy of these management strategies amongst various types of chronic pain are demonstrated in the literature.10-13 However, its consideration for use in the local setting remains unknown.
Various factors may influence the optimal management of chronic pain in general and in the SCI population. These include poor knowledge and frustrations by health care providers, disregarding the patient’s perspective, affordability of care, time constraints on health care providers and lack of support for patients.14-17 One study reported that health care providers expressed their lack of knowledge and expertise in managing chronic pain. 14 Furthermore, the patient-healthcare provider relationship is essential to the optimal care of chronic pain. Health care providers have highlighted the importance of developing this relationship into one of mutual understanding and goal planning.15,16 Further challenges to optimal chronic pain management specifically in the SCI population include affordability of care, particularly for non-pharmacological therapies; time constraints which limit health care providers ability to adequately educate patients on chronic pain and the management thereof. 17
A holistic approach to chronic pain management had been suggested as early as 1977, with George Engel 18 introducing the biopsychosocial model to pain management. More recently, the World Health Organization (WHO) has advocated for interprofessional and collaborative practice in order to address the complex needs of patients. 19 In South Africa, challenges exist which influence the holistic management of care. These include, but are not limited to staff shortages, inadequate resources, time constraints, ineffective referral system and poor knowledge by health care providers of holistic management.20,21 Therefore, high-quality guidelines are needed to adopt a systematic biopsychosocial approach to chronic pain management, 22 particularly for the TSCI population and in the South African context. In a recent scoping review, guidelines for chronic pain in the SCI population, in Germany, were identified and critically appraised. 23 The guideline was appraised as a high-quality guideline according to the AGREEII tool. The guideline includes recommendations for assessment and classification of chronic pain and its sub-types; pharmacological and non-pharmacological recommendations for NP and NeuP as well as the recommendations for the monitoring of chronic pain and management of resistant chronic pain. Contextualisation of these guidelines for the South African context is required, as a developed country (Germany) will make provision for a larger distribution of resources such as professional services and medication, etc.
Methodology
Research Design
Developed in 1963 24 , the Delphi study technique aims to gather and combine opinions from participants on a certain topic, based on their experience. The process should be repeated until consensus is reached or until it becomes clear that no consensus is possible. 25 In this study, a modified Delphi technique was used to gather health care provider opinions and consensus on a set of principles which should be included, at the primary health care level, to guide the management of chronic pain amongst the TSCI population. The traditional technique consists of a first round of idea/theme construction, a second round of consensus building and a final round of prioritisation. 26 The authors made use of a modified Delphi study as an initial round of idea/theme construction was not required since a list of guiding principles was already sought through a scoping review and rated with good methodological rigor as per the AGREEII tool, 27 as well as themes from previous qualitative interviews conducted with health care providers at the primary health care level 28 and PWTSCI, 5 in the Cape Metropolitan region.
Population and Sampling
Purposive sampling was used to recruit nurses and doctors (medical officers) knowledgeable about chronic pain management at the primary health care level. Inclusion criteria included a minimum of two years’ professional experience and currently working at the primary health care level of the public sector.
Setting
Primary health care clinics across the Cape metropolitan region (of the Western Cape) was chosen as the research setting. Primary health care is concerned with essential, evidence-based, affordable, ethical and equitable care provided at a community level, 29 and is the firs-line of care for many people in developing countries. In the Western Cape, 75% of its population depend on public-sector health facilities, especially for chronic conditions. 30 Unfortunately, at the primary health care level in the Western Cape, no specialized pain centres exist. 31
Data Collection
Fourteen City of Cape Town clinics were identified as primary health care settings who attended to PWTSCI. The managers of the health care clinics were emailed to disseminate the invitation to participate, which included the approval letter to conduct the study in the clinic (Reference 1094, from the City of Cape Town, City Health), the ethics approval from the University of the Western Cape’s Biomedical Research and Ethics Committee (Reference 20_8_22), the Google form® which contained the questionnaire, an information sheet as well as the consent form. In addition, in-person recruitment at the various clinics as well as snowballing recruitment techniques were employed.
Data Analysis
In the second round, data coding took place in SPSS V29, for the various pharmacological drugs: Neuropathic pain, opiate (narcotic) analgesic was labelled “1”, anticonvulsants were labelled “2”, tricyclic antidepressants were labelled “3”, Selective serotonin norepinephrine reuptake inhibitors (SNNRIs) were labelled “5” and for nociceptive pain, opioid analgesics were labelled “4” and non-opioid analgesics were labelled “6”. In the first and second rounds the responses from the Likert scale was divided into three categories, with “agree” and “strongly agree” comprising the consensus category; “disagree” and “strongly disagree” comprising the non-consensus category and lastly, “neutral” comprising the unsure category. The consensus category was further divided into weak consensus (50%–70%) and strong consensus (>70%).25,32 Furthermore, a median of 3.24 or higher was also considered as it more appropriately displays consensus amongst a panel, as discussed by Hsu and Sandford. 25
Ethics
Permission to conduct the study at the identified clinics was obtained from the City of Cape Town City Health (Reference 1094). Ethics approval to conduct the study was obtained from The University of the Western Cape’s Biomedical Research and Ethics Committee (Reference 20_8_22). Participants provided informed consent prior to completing the questionnaires.
Results
Participant Characteristics
Twenty-eight participants took part in round one of the Delphi study. Only ten professionals completed the second round of the Delphi study. The results of the Delphi study have therefore been displayed according to each round. Most of the participants were female (round one, n = 28 and round two, n = 9). The ages of the participants ranged from range 27-55 years (round one, SD = 7.9 and round two, SD = 6.7) and their years of experience ranged from range 2-35 years. The cohort included nursing clinical managers, registered nurse, clinical nurse practitioner, enrolled nurse, enrolled nursing assistant and professional nurse and medical officers (doctors).
Main Findings
The participants reached strong consensus (>70%) on most of the guidelines. Weak consensus was attained on two guidelines pertaining to the classification of chronic pain as well as the first-line pharmacological management of neuropathic pain.
Assessment, Education and Planning in Relation to Chronic Pain Management
Assessment, Education and Planning Principles for chronic Pain Management in the TSCI Population Through consensus in Round One.

Pharmacological Management of Chronic Pain
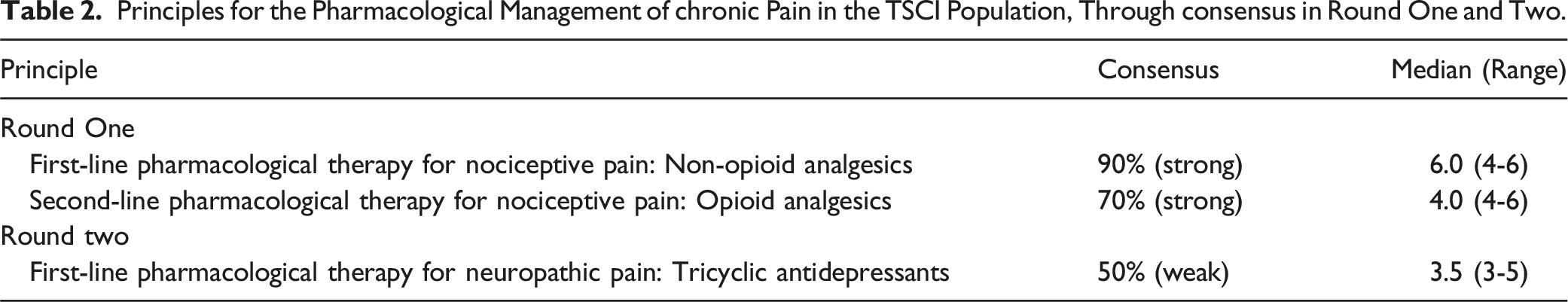
Consensus regarding the pharmacological management of nociceptive pain was obtained in the first round of the study. Regarding neuropathic pain, many participants were unsure regarding the specific drug name in relation to the line of therapy. Therefore, the second round of the Delphi study asked participants to recommend the class of drugs appropriate for the line of therapy, for neuropathic pain. However, as seen in the first round, the participants could only agree on Tricyclic antidepressants (TCA) as first-line therapy for neuropathic pain. A few of the participants commented that many of the drug names listed were not available at the primary health care level and certain drugs could only be prescribed by specialists and not at the primary health care level. No consensus could be reached on the recommendation for second to fourth-line pharmacological therapy, for neuropathic pain. The second-line pharmacotherapy for neuropathic pain was listed as Duloxetine [selective serotonin and norepinephrine reuptake inhibitors (SSNRIs)], thereafter, Amitriptyline [tricyclic antidepressant (TCA)]. The third-line was listed as Oxycodone [opiate (narcotic) analgesics], thereafter Lamotrigine [anticonvulsant]. The fourth-line was listed as Venlafaxine [selective serotonin and norepinephrine reuptake inhibitors (SNRIs)] and thereafter Opioid analgesics: Tramadol.
Principles for the Pharmacological Management of chronic Pain in the TSCI Population, Through consensus in Round One and Two.
Non-pharmacological Management of Chronic Pain
Principles for the Non-pharmacological Management of chronic Pain in the TSCI Population, Through consensus in Round One.

Additional Comments on the Management of Chronic Pain
The first-line primary health care providers were given an opportunity to comment on any additional principles that should be considered in the context of the Western Cape. One participant mentioned that interprofessional approaches to manage chronic pain is problematic as staff scarcity remains an issue at the primary health care level. Furthermore, the participants also commented that at the primary health care level, the only drugs which are available include amitriptyline, paracetamol, ibuprofen and tramadol. Drugs such as pregabalin and gabapentin are only available at the specialist level of care.
Monitoring of Chronic Pain Management and Management of Resistant Chronic Pain
Principles for the Monitoring of chronic Pain and Management of Resistant chronic Pain, Through consensus in Round 2.

Figure 1 illustrates the final compilation of design principles for chronic pain in the TSCI population, which gained consensus in this Delphi study. Design principles for chronic pain management in the TSCI population, in South Africa. The blue section displays the assessment principles for chronic pain. The yellow section indicates principles relating to the education of chronic pain and its management. The green section displays the planning involved in the management of chronic pain. The orange indicates the treatment options for the management of nociceptive pain. The grey displays the treatment options for the management of neuropathic pain. The final block illustrates the principles for monitoring chronic pain as well as management of resistant chronic pain.
Discussion
The aim of the study sought to gain consensus on principles to guide the management of chronic pain in the TSCI population, in the developing context of the Western Cape of South Africa. The principles were based on themes explored in qualitative papers from patients 5 and health care providers’ perspectives. 28 In addition to published German guidelines for chronic pain in the TSCI population, retrieved and assessed with the AGREEII tool by the authors. 27 The first-line primary health care providers agreed on 18 principles pertaining to the assessment of chronic pain. These included the first-line pharmacological management for neuropathic and nociceptive pain, first-line non-pharmacological therapy for nociceptive pain, second-line non-pharmacological therapy for neuropathic pain, second-line pharmacological therapy for nociceptive pain as well as three principles in relation to the monitoring of chronic pain and the management of resistant pain. No consensus could be reached on the appropriate recommendation for the second- to fourth-line pharmacological management of neuropathic pain, which included Duloxetine [selective serotonin and norepinephrine reuptake inhibitors (SSNRIs)], thereafter, Amitriptyline [tricyclic antidepressant (TCA)] (second-line); Oxycodone [opiate (narcotic) analgesics], thereafter Lamotrigine [anticonvulsant] (third-line), and Venlafaxine [selective serotonin and norepinephrine reuptake inhibitors (SNRIs)], thereafter Opioid analgesics: Tramadol (fourth-line).
This is the first study aimed at creating principles for chronic pain management in the TSCI population, in the developing context of the Western Cape of South Africa. A study published in 2012 33 includes guidelines for neuropathic pain in South Africa. However, these guidelines are not specific for the TSCI population nor does it include nociceptive pain management. Our study yielded holistic assessment, management and monitoring principles for chronic pain (neuropathic and nociceptive) in the TSCI population. Chronic pain is multifaceted, defined as pain lasting longer than three months and influenced by a complex interaction of biopsychosocial factors. 34 A holistic approach to chronic pain was recommended as early as 1977,18,35 with the biopsychosocial approach to chronic pain management aimed to address biological, physical, psychological and social ramifications of chronic pain in patients. 34
In the present study, the first-line primary health care providers highlighted staff shortages as a challenge to interprofessional collaboration to holistically manage chronic pain in the TSCI population. This is consistent with other studies conducted in South Africa, where staff shortages are evident in developing contexts.20,21 Furthermore, challenges to holistic management of care in South Africa includes ineffective referral between interdisciplinary teams, such as technical complications and knowledge of referral patterns.20,21 In addition to the challenge of staff shortage in limiting holistic approaches of care, these staff shortages and high patient workload may also explain the 74% drop-out rate in relation to participation in round two of our Delphi Study. Health care providers in South Africa are burdened by a lack of resources, a lack of time, increased hours and a high patient to provider ratio increasing the risk of burnout amongst this population.20,21,36 The lack of psychologists and pain specialists at the primary health care level in the South African context is of great concern as the assessment and management provided by these professionals are part of the holistic approach to chronic pain management.37,38 Furthermore, the intensity of pain as well as pain-related disability has shown improvement through psychotherapeutic techniques, such as CBT, in the SCI population.39-41
Our Delphi study revealed that consensus could not be reached on the second to fourth-line pharmacological management of chronic pain in the TSCI population, in a developing context. There could be several reasons for this non-consensus, ranging from the lack of pain specialists at the primary health care level in the South African context, a lack of resources, such as staff training and skill support in pain management which is evident in the challenges faced by health care providers in relation to holistic care,20,21 the complexity of chronic pain, the issue of high prevalence rates of substance abuse in the TSCI population. 4
Implications for Clinical Practice
These principles (Figure 1) highlight the agreement by first-line primary health care providers that a holistic biopsychosocial approach to chronic pain assessment, management and monitoring should be prioritised, in the TSCI population, in the Western Cape of South Africa. Despite the challenges present in the South African context, health care providers should firstly be aware of the best available contextual evidence and, secondly, work towards incorporating these principles into the management of chronic pain at the primary health care level.
The lack of consensus regarding the second- to fourth-line pharmacological management of neuropathic pain draws attention to the need for the government, to make the appropriate drugs available at the primary health care level and for institutions to provide the necessary staff training for the improvement of chronic pain pharmacological management at the primary health care level.
Limitations of the Study
Eighteen participants did not participate in the second round of the Delphi study despite numerous follow-up emails and in-person recruitment. A limitation of the study therefore is that a larger cohort of first-line primary health care providers may have resulted in a richer data set. Furthermore, the study did not include health care policymakers and pharmacy managers who may understand the economic and regulatory decisions for the lack of availability of certain drug treatment classes at specific levels of care. In addition, the inclusion of psychologists and pain specialists would provide further insights into the necessary care required to manage chronic pain in the TSCI population, however, these are not available at the primary health care level in the Western Cape region of South Africa.
Conclusion
This study, the first of its kind in the developing context of the Western Cape of South Africa, provides agreed upon principles for chronic pain management in the TSCI population, particularly at the primary health care level. Future studies should assess which design principles are currently being implemented at the primary health care level and the factors associated with the implementation. Thereafter, studies should assess the impact of the implementation, which include the challenges and enablers.
Footnotes
Acknowledgements
The authors would like to acknowledge Professor Joliana Phillips for her instrumental role in the research project leading up to this Delphi study. Professor Phillips sadly passed away before she could see this end result of the project. Her support, motivation, dedication, and hard work played a pivotal role in this research project.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The authors received financial support from the Department of Higher education and training in South Africa.
Ethical Statement
Data Availability Statement
The data that support the findings of this study are available on request from the corresponding author, [TW]. The data are not publicly available due to containing information that could compromise the privacy of research participants.
