Abstract
Aims and Objectives
3d-printed models (bio-models) have become a useful tool in the armamentarium of surgeons for improved surgical planning in the recent past. This study directs at reinforcing the incorporation of these bio-models as a handy tool in treatment planning, resident training, patient education and record maintenance. The aim of this empirical study was to compare the outcome in reconstructive maxillofacial surgery when planned using 3d-printed model and without 3d-printed model (conventional). The objectives were to assess and compare the intraoperative time taken during reconstruction, the immediate post-operative experience (pain, mouth opening and incidence of infection) and the quality of life using University of Washington (UW-QOL) questionnaire during follow up.
Methods
This retrospective comparative study was conducted in Department of Oral & Maxillofacial Surgery, from March 2018 to March 2020. It included 50 cases consisting variety of pathologic and traumatic maxillofacial defects and they were grouped into with 3d-printed model (Group A) and without 3d-printed model (Group B). The groups were further subclassified based on maxillary (MR) and mandibular reconstruction [vascularized flaps (VFFF), non-vascularised grafts (NVG), reconstruction plate alone (RP)]. We compared intra operative time taken along with immediate post-operative parameters (pain, mouth opening and presence of infection) and patient’s quality of life using UW-QOL questionnaire. These values were taken for comparison and statistical analysis was done by unpaired t-test.
Result
There was 14.75% (35.26 minutes) mean reduction in operative time (
Conclusion
Use of 3d-printed model to guide and assist in surgical procedures have provided promising results. Based on this study, we found that there is decreased intraoperative time and post-operative pain score when 3d-printed model were used. The patient’s quality of life was also found to be better in terms of reduction in pain, salivary secretion and mood elevation. With increased success rate, the authors are of the strong opinion that it is time to revisit the surgical protocol used for reconstruction and include 3d-printed model as a primary tool or technology across the board for all patients notwithstanding the comparative cost, as the results offset the financial aspect.
Keywords
Introduction
Reconstruction of the face after trauma or surgical tumor extirpation is an integral part of Oral and Maxillofacial surgical procedures to provide desirable functional and aesthetic results. The main goal is to attain preoperative form and function with minimum operative and postoperative morbidities. The literature shows successful use of both vascularized and non-vascularized bone grafts for reconstruction of defects and deformities of midface and mandible with the ultimate aim of providing adequate bone for dental rehabilitation, more recently by insertion of osseointegrated dental implants.1,2
It is difficult to replicate the complex three-dimensional conformation of the face. Any deviation from structural alignment may likely lead to functional disturbances like malocclusion and temporomandibular joint disorders. Furthermore, cases involving extensive bony resection, TMJ involvement, insufficient teeth for dental guidance, severely distorted bony contour and dilemma of primary or secondary reconstruction have definitely added to the difficulties in the reconstructive task.
The advent of newer technologies and surgical techniques has enabled modern Oral & Maxillofacial Surgeons to effectively accomplish the goals of reconstruction. Most recently the use of 3-Dimensional (3D) bio-models to guide and assist in surgical procedures have provided promising results.
3d-printed model (Bio model) have been utilized for variety of different purposes since their introduction by Charles Hull in 1986. 3 With advances in radiology and computer aided design and computer aided manufacturing (CAD-CAM) along with improved material and accuracy, 3d-printed model have become a useful tool in the armamentarium of surgeons by improving surgical planning and reducing the operating time.3,4
The treatment of head and neck pathology has profound and long-term effects on a patient’s overall health, appearance, speech, ability to breathe, communicate, eat, and swallow. Quality of life (QOL) is a measure that encompasses many of these variables and can be used as an outcome measure, along with such factors as mortality, morbidity, survival, and recurrence. 5 Successful use of 3d-printed model in improving the predictability of treatment of maxillofacial defects secondary to traumatic or pathologic conditions has already been described in the literature.6-8 The aim of this article is to present 50 cases demonstrating the versatile use of 3d-printed model for maxillofacial reconstruction and to compare the performance of the pre-bent plates with conventional intra operatively adapted plates in terms of time taken for surgery, immediate postoperative pain, mouth opening and presence of infection along with analysis and comparison of quality of life (QOL) during follow up. With this study, we intend to further reinforce the incorporation of 3d-printed model as a handy tool in treatment planning, resident training, patient education and record maintenance.
Patients & Study Design
Our study design included 50 patients with racial origin from South Asia; treated in our department of oral and maxillofacial surgery from March 2018 to March 2020. Pathology and defects including either maxilla or mandible were included in the study. Initial investigations included plain radiographs and routine blood tests. The final diagnosis for all the pathologies was reached after histopathologic examination.
The patients were categorized into group A (with 3d-printed model) and group B (without the use of 3d-printed model). They were subgrouped according to maxillary (MR) and mandibular reconstruction [vascularized flaps (VFFF), non-vascularised grafts (NVG), reconstruction plate alone (RP)]. We compared the performance of these procedure in terms of time taken for surgery, immediate postoperative experience (pain, mouth opening and presence of infection) and QOL during follow up.
Classification of Surgical Site Infections, Summarized From the Control and Prevention/National Healthcare Safety Network Surveillance Definitions for Specific Types of Infections.
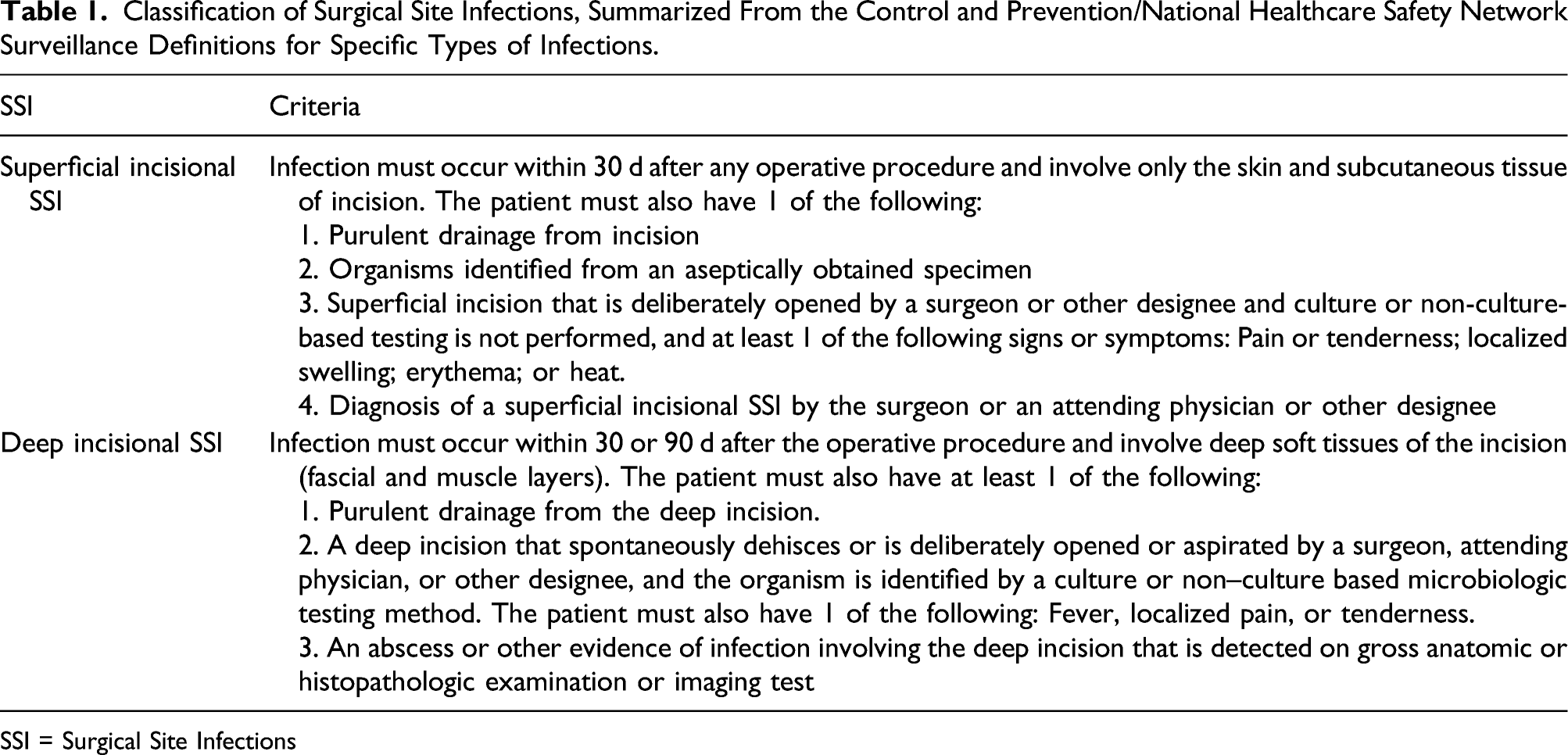

SSI = Surgical Site Infections
Postoperative follow up was done by personal or telephonic interview to assess the quality of life using University of Washington’s Quality of Life Questionnaire version 4(UW-QOL v4) as modified by Young et al. 5 We omitted the domain “Shoulder” as our procedures didn’t involve Neck dissection in any of the cases. The whole questionnaire focused on patient health and quality of life within the past 7 days from the day of assessment. In our study, UW-QOL consisted 11 question domains pertaining to physical and social function. It also included additional 3 global questions assessing the patients feeling before the development of the lesion, their post-operative health and overall health in the past 7 days. The data thus obtained was scaled from 0 (much worse) to 100 (outstanding) to enable ease of presentation and the follow up period was noted in each case.
Data was tabulated as means in case of Operative time, VAS score and Mouth opening, while mean number of patients scoring each domain and percentage of patients selecting best score was taken in UW-QOL.
Treatment Planning and Surgical Technique Using 3d-Printed Model (Group A)
For treatment planning using 3d-printed model, high-resolution CT scans of slice thickness ranging from .75 mm to 1.5 mm were taken for all the cases after reaching the final diagnosis. This CT scan data set was then imported in image processing software 3D Slicer (Open-source software, Surgical Planning Lab, Boston, MA) as DICOM data for processing, to generate a virtual three-dimensional image of the patient’s jaw. Following that, a 3D printing machine based on Fused Deposition Modeling (FDM) technology - Anet A8 3D Printer was used. This works by the extrusion of small beads of melted thermoplastic materials, from a small nozzle, that harden afterward to form layers. PLA was the thermoplastic material used. Post processing, the models were sterilized using ETO and used for the surgery. In cases where plate adaptation was anticipated to be difficult due to the extent of pathology or defect, mirror image of the unaffected contralateral side was virtually superimposed on the affected side prior to construction of 3d-printed model (Figure 1Aand B).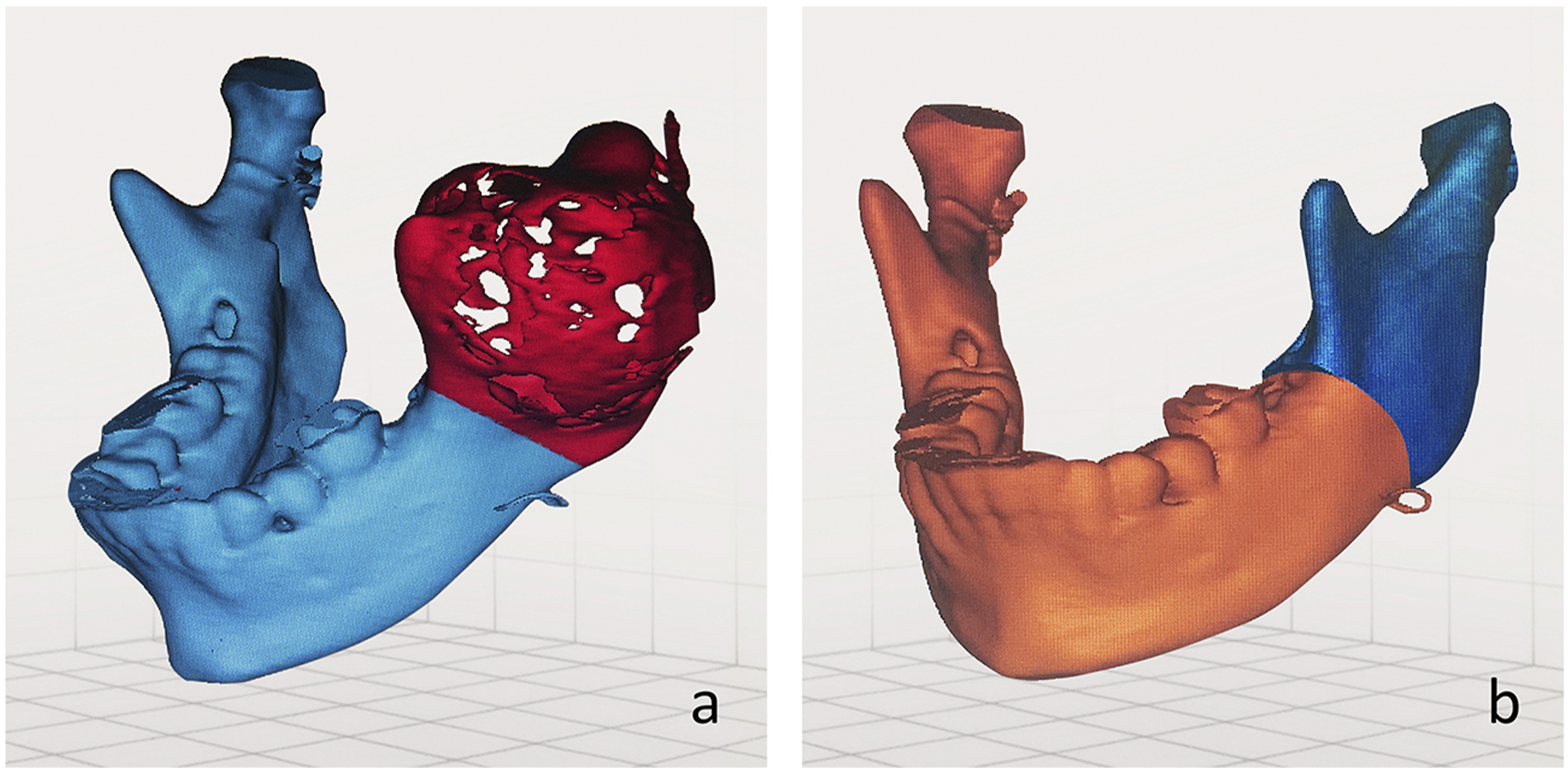
In cases of pathology or defect crossing the midline, sculpting of the model was done manually using carvers after obtaining the 3d-printed model. For 1 patient who was not able to afford construction of 3d-printed model, a stock mandibular model of another patient of the same sex and just about similar dimension verified by using axial view of 3-D CT was selected. The 3d-printed models were used to plan and mark the margins of surgical resection and to obtain the approximate size of graft/flap. The defects were classified according to Boyd’s classification
12
in mandible and Brown’s classification
13
in maxilla for ease of planning and documentation. According to the defect and its location, 2.4 mm Titanium Reconstruction plates (Stryker, DePuySynthes, OrthoMax®) for mandible and 1.5 mm Titanium Mesh(OrthoMax®) for maxilla was bent and adapted preoperatively to the patient specific 3d-printed model by the same group of surgeons performing the surgery (Figure 2A and B). The pre-bent plates were then packed and sterilized prior to procedure.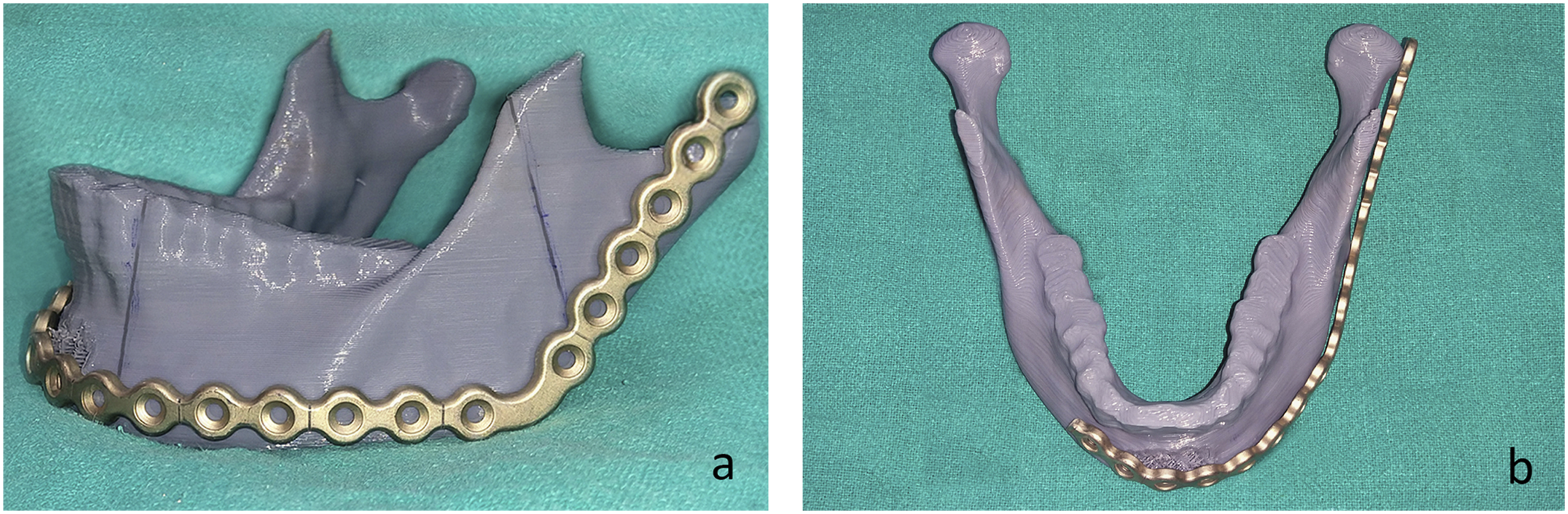
. Characteristics of the Patients, Defects & Surgical Procedure using SLA (Group A).

Combined - Combined Extraoral & Intraoral approach; H - Hemi-mandibulectomy including the condyle; C - Central mandibulectomy defect including bilateral canines; L - Lateral mandibulectomy defects excluding the condyle (Boyd’s HCL classification); Type II - Maxillectomy excluding the orbit; Type III- Maxillectomy involving the orbital adnexae with orbital retention, b - defect involving less than or equal to unilateral palate (Brown’s classification of maxillary defects); VFFF - Vascularized Free Fibular Flap; ICG - Anterior Iliac Crest Graft; CCG - Costochondral grafts; RG - Rib Graft
Characteristics of the Patients, Defects & Surgical Procedure without using SLA (Group B).

Combined - Combined Extraoral & Intraoral approach; H - Hemi-mandibulectomy including the condyle; C - Central mandibulectomy defect including bilateral canines; L - Lateral mandibulectomy defects excluding the condyle (Boyd’s HCL classification); Type II - Maxillectomy excluding the orbit; b - defect involving less than or equal to unilateral palate (Brown’s classification of maxillary defects); ICG - Anterior Iliac Crest Graft; CCG - Costochondral grafts
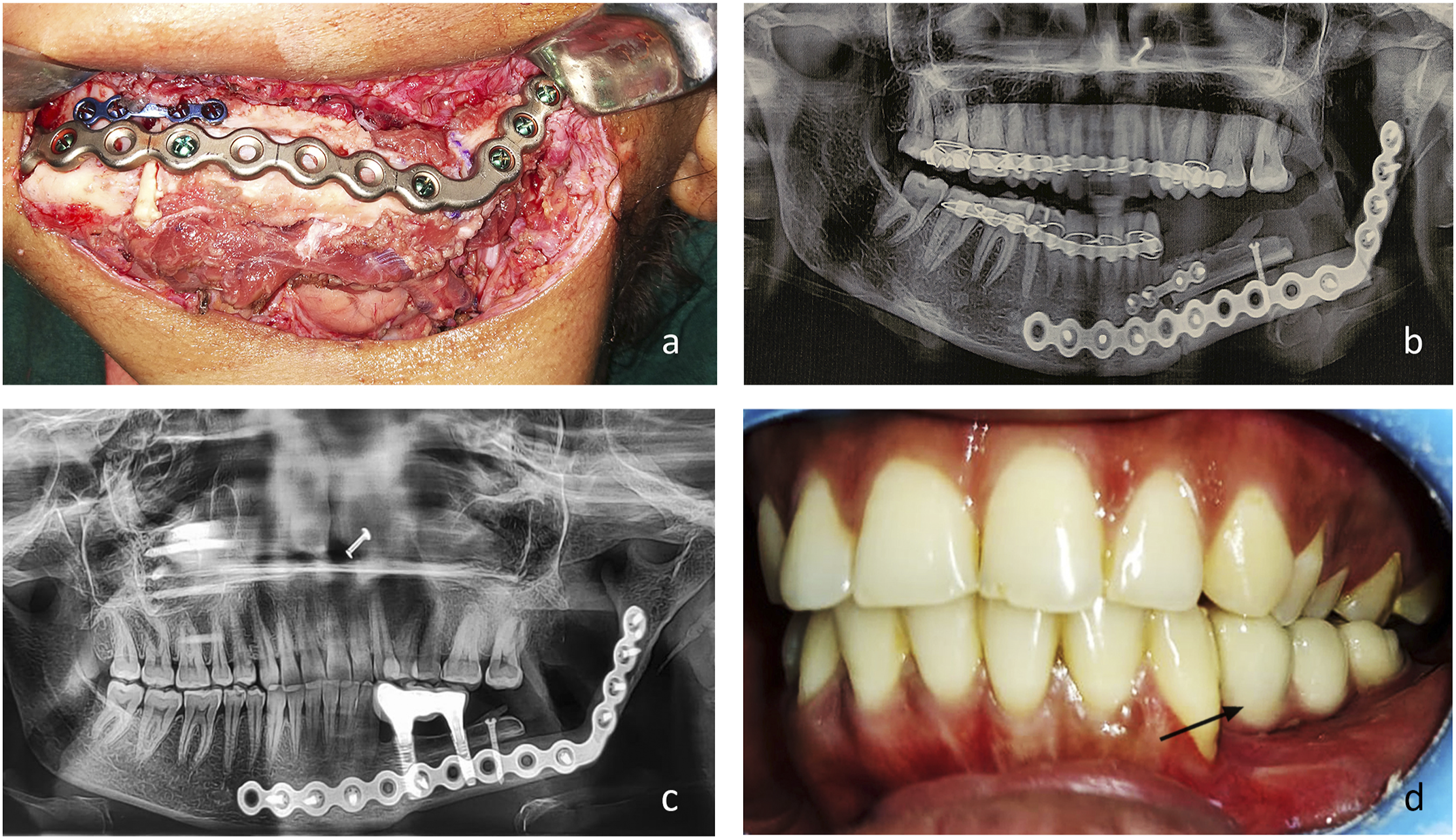
Anterior iliac crest graft (ICG) was used in 5 cases, Costochondral grafts (CCG) in 3 and Rib graft (RG) in 2, with later being the choice for younger patients. In 1 of the cases reconstructed with anterior iliac graft, 4 dental implants were placed immediately (Figure 4A-D).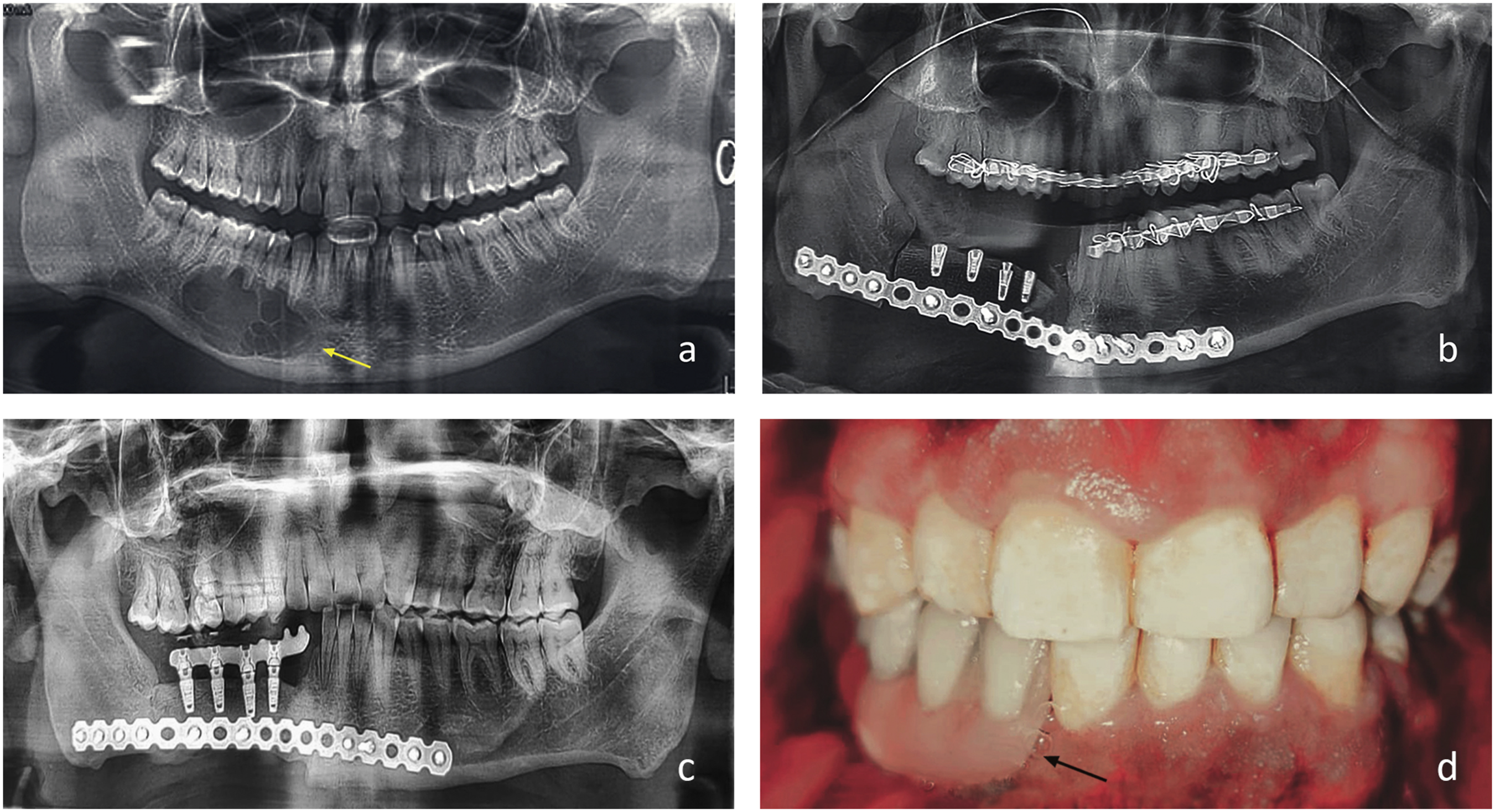
Reconstruction plate (RP) without graft was used in 6 cases of which 2 were plate replacement due to failure. For maxillectomy cases, preadapted titanium mesh was used for reconstruction (Figure 5A-F). Plating was carried out after putting the patient on Intermaxillary fixation (IMF) and done keeping in view that at least 3 - 4 screws were placed on the sound bone adjacent to the continuity defect.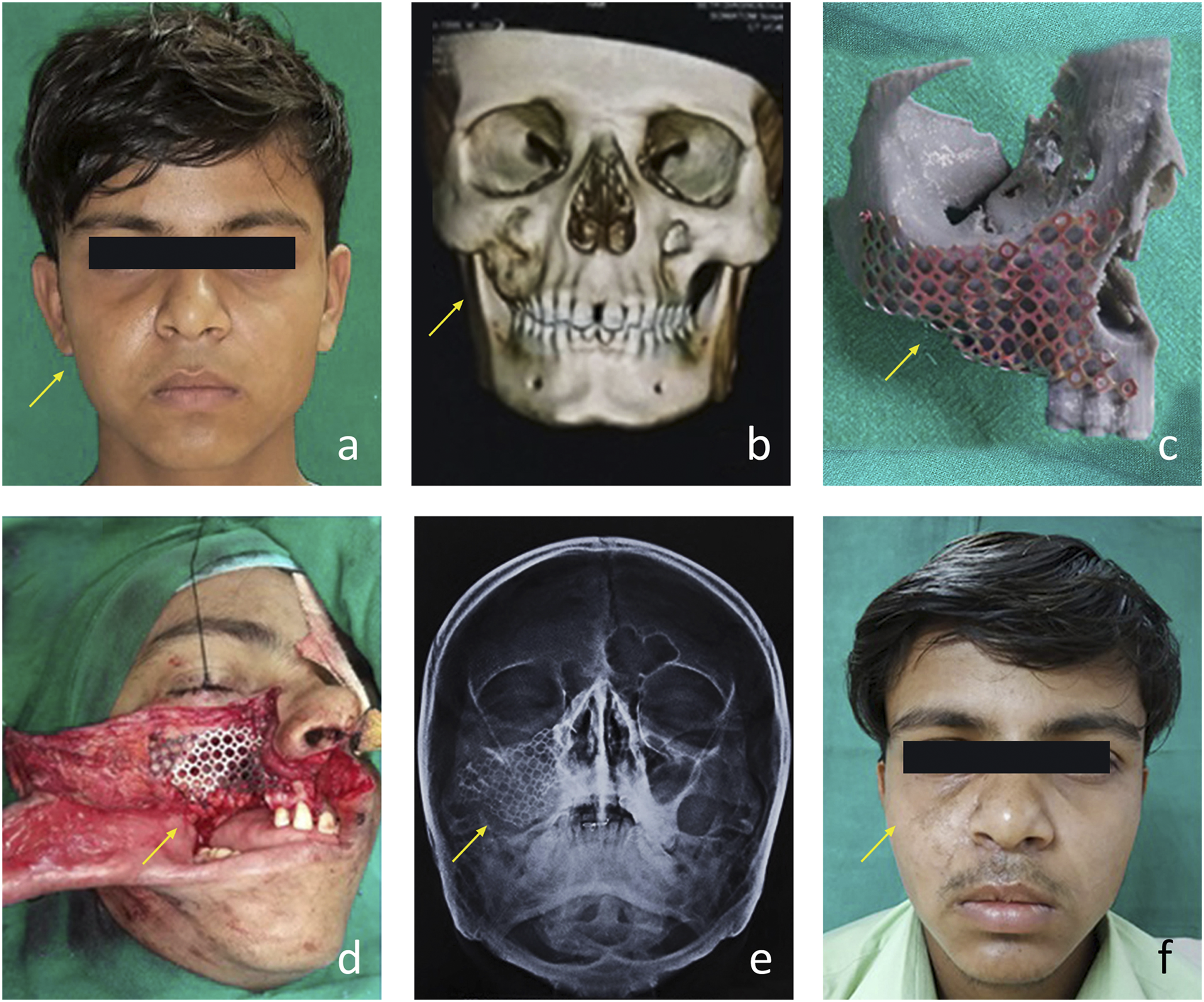
Combined - Combined Extraoral & Intraoral approach; H - Hemi-mandibulectomy including the condyle; C - Central mandibulectomy defect including bilateral canines; L - Lateral mandibulectomy defects excluding the condyle (Boyd’s HCL classification); Type II - Maxillectomy excluding the orbit; Type III- Maxillectomy involving the orbital adnexae with orbital retention, b - defect involving less than or equal to unilateral palate (Brown’s classification of maxillary defects); VFFF - Vascularized Free Fibular Flap; ICG - Anterior Iliac Crest Graft; CCG - Costochondral grafts; RG - Rib Graft
Combined - Combined Extraoral & Intraoral approach; H - Hemi-mandibulectomy including the condyle; C - Central mandibulectomy defect including bilateral canines; L - Lateral mandibulectomy defects excluding the condyle (Boyd’s HCL classification); Type II - Maxillectomy excluding the orbit; b - defect involving less than or equal to unilateral palate (Brown’s classification of maxillary defects); ICG - Anterior Iliac Crest Graft; CCG - Costochondral grafts
Results
The included patients were 26 males & 24 females with age groups, ranging from 7 to 63 years (Mean age ± Standard deviation = 30.38 ± 13.57 years) with pathologies or defect involving either maxilla or mandible. Of these cases, 1 case was a second surgery for osteonecrosis due to gunshot wound and 2 plate failure cases; others were of pathologic nature in which 3 cases were reconstructed secondarily.
In this study while 21 cases (11 males, 10 females) were included in group A while 29 cases (15 males, 14 females) were included in group B. The immediate postoperative period of patients in group A was uneventful and showed good aesthetic results with satisfactory functional movements.
Details of Cases Included in the Study.
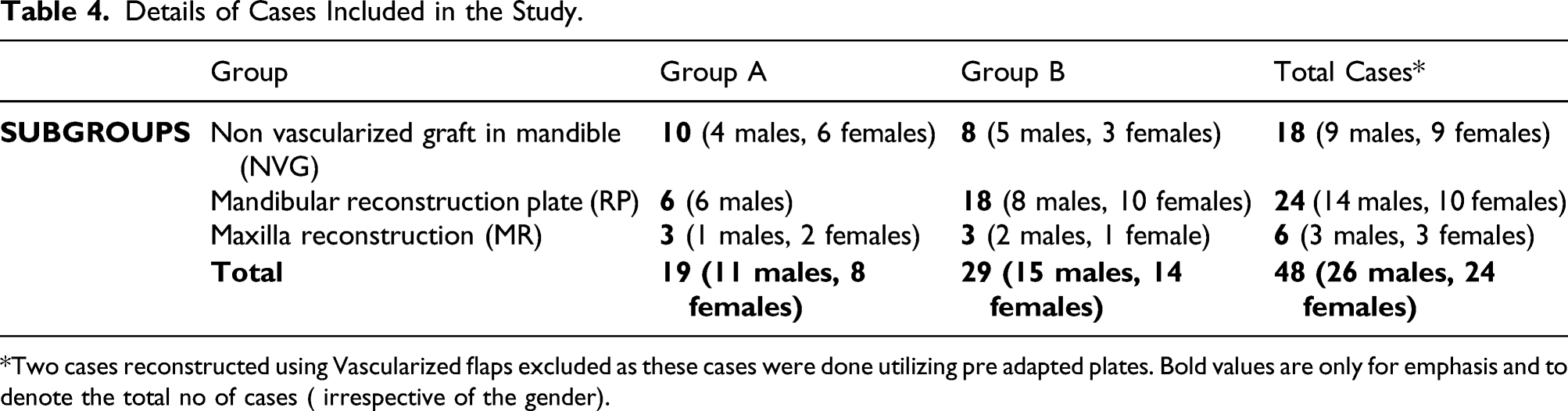
*Two cases reconstructed using Vascularized flaps excluded as these cases were done utilizing pre adapted plates. Bold values are only for emphasis and to denote the total no of cases ( irrespective of the gender).
Comparison of Operative time, Visual Analogue Score Score & Mouth opening
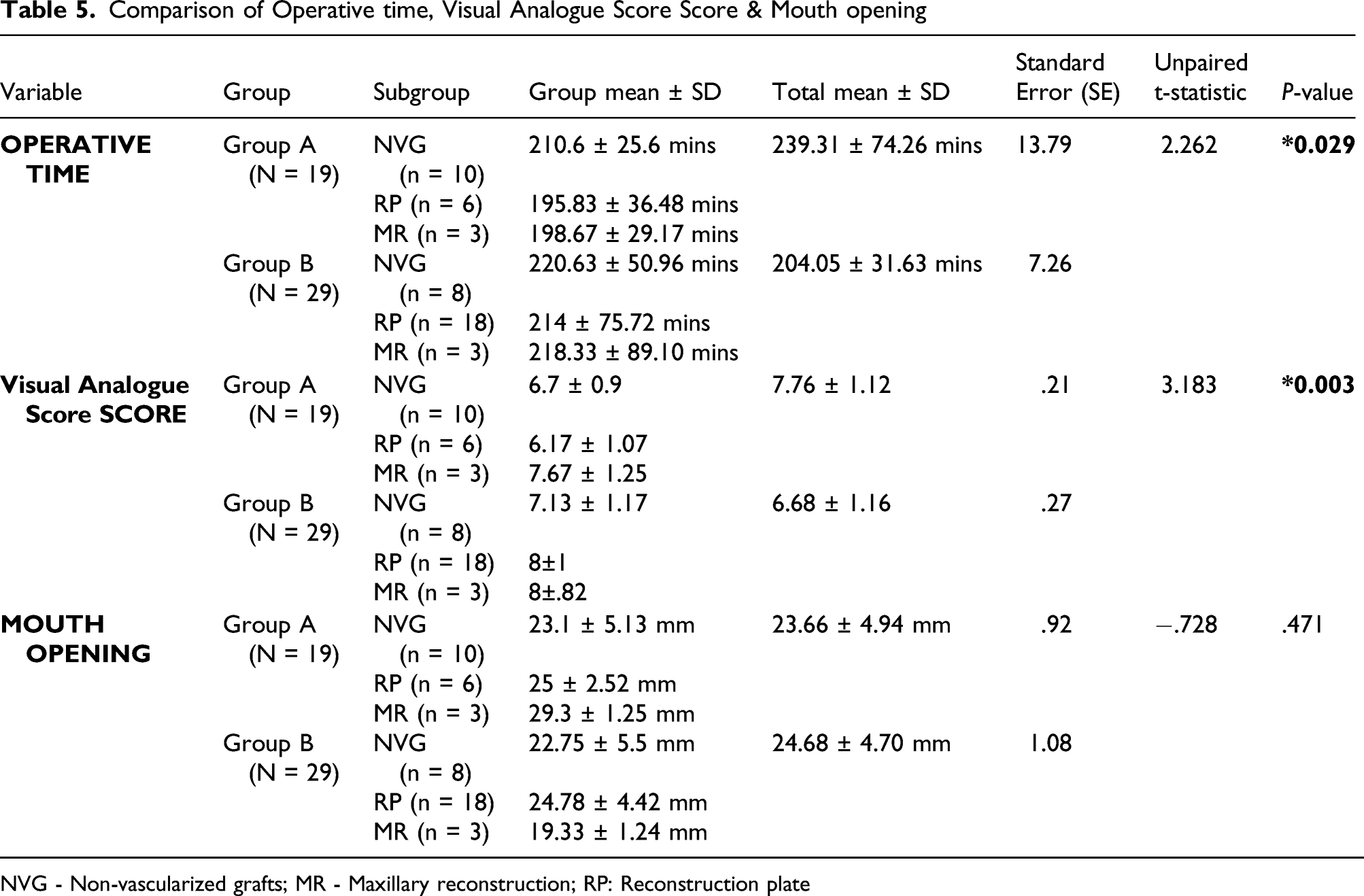
NVG - Non-vascularized grafts; MR - Maxillary reconstruction; RP: Reconstruction plate
Comparison of Presence of Infection.
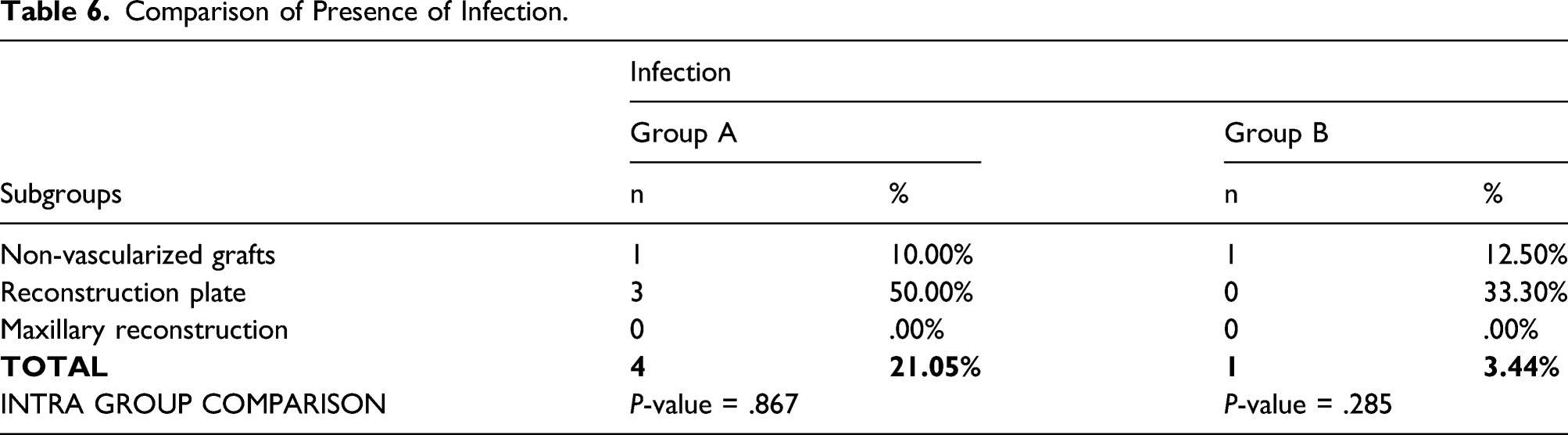
UW-QOL Results
All the 48 patients responded to our interview for assessing UW-QOL either personally or telephonically. The follow up period ranged from 9 months to 2 years.
For comparison, the mean scores of each domain obtained from UW-QOL questionnaire was used in each subgroup. Percentage of patient selecting best score (%Best Score) for physical and social function was taken as the percentage of patients who awarded ‘100’ for that particular domain and that of global questions was percentage scoring 50, 75 or 100 for first question, i.e. Health related QOL compared to month before disease and percentage scoring 60, 80 or 100 for next 2 questions, i.e. Health related QOL during the past 7 days and Overall QOL during the past 7 days.
Comparison of University of Washington - Quality of life Mean Scores and % Best Scores for Patients Treated With Non Vascularized Graft (NVG) for mandibular defects.
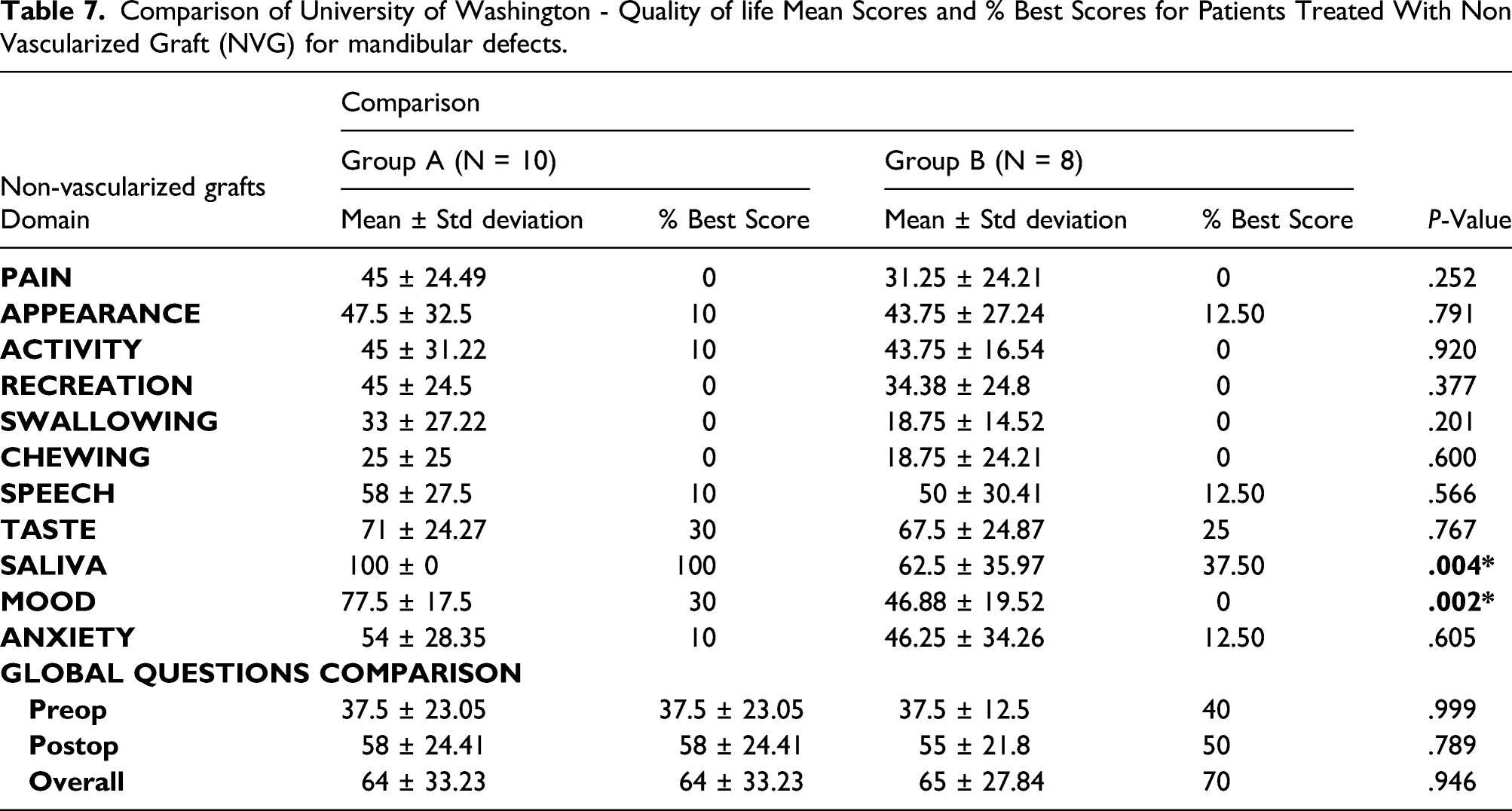
Comparison of University of Washington - Quality of life Mean Scores and % Best Scores for Patients Treated With Reconstruction Plate (RP) Only for Mandibular Defects.
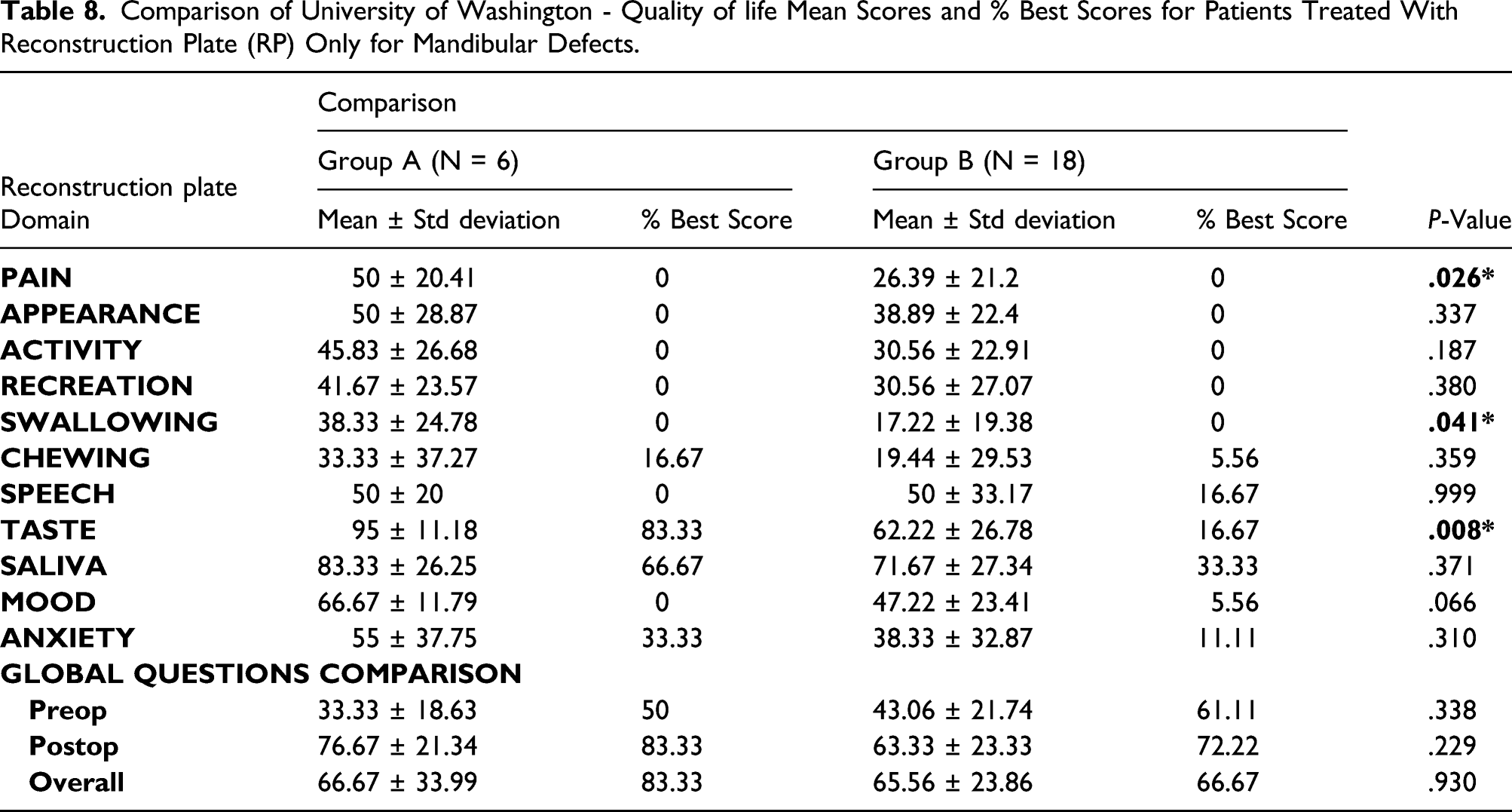
Comparison of University of Washington - Quality of life Mean Scores and % Best Scores for Patients Treated With Maxillary Reconstruction (MR).
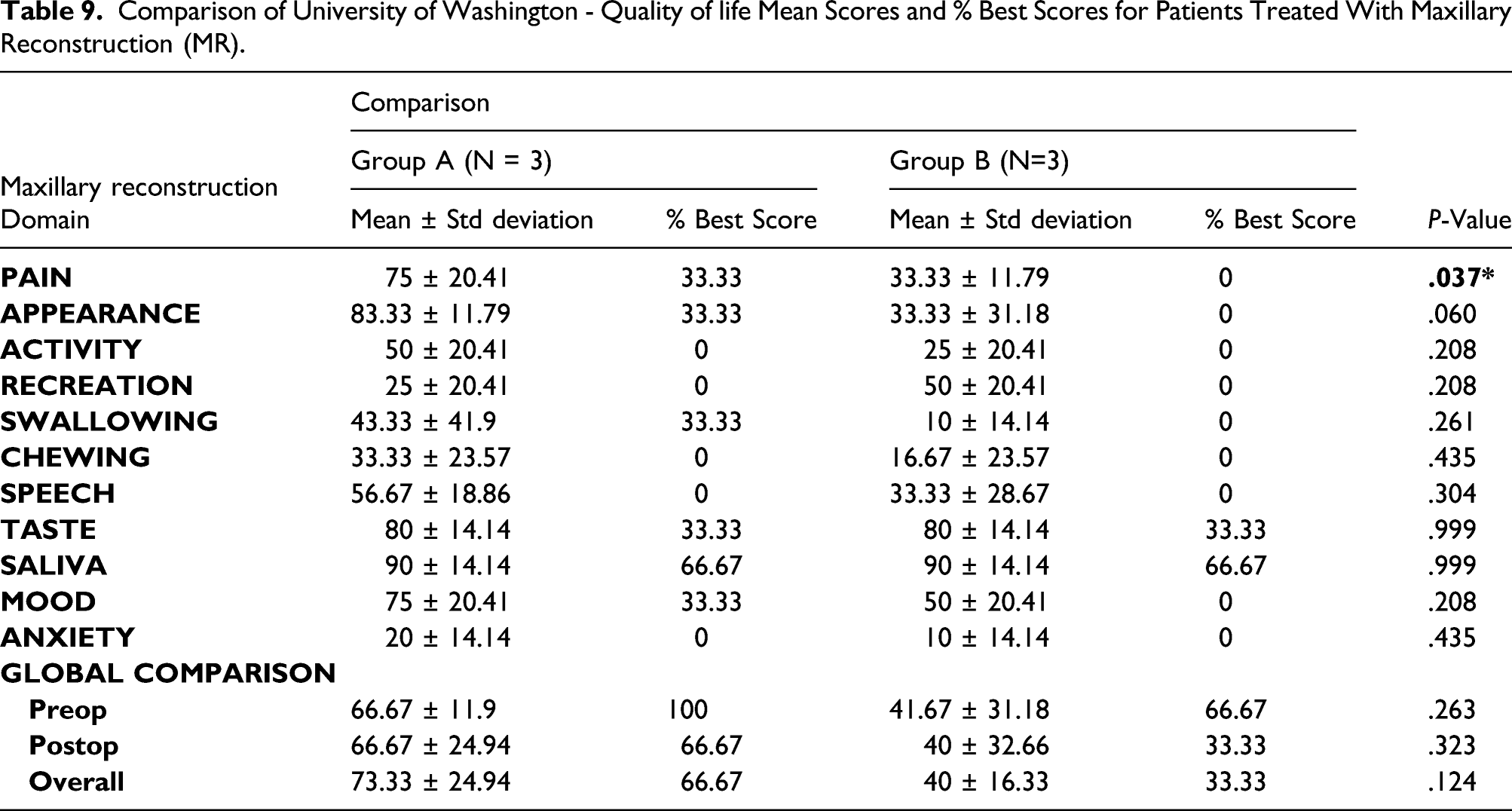
Discussion
The primary goal of a reconstructive surgeon is to ‘restore the form and function’ of an anatomical structure lost due to pathologic or traumatic event. Reconstruction of the maxillofacial region is particularly challenging because of the need to maintain proper aesthetic contour and occlusion. The success rate of maxillofacial reconstruction has increased as a result of advances in plate design and materials. However, inadequate contouring and adaptation of the reconstruction plate to the extant mandible still represents the most common cause of plate failure, malocclusion or condylar malposition.14-17 Adjustive bending of the plates intraoperatively can lead to fracture of the reconstruction plates postoperatively because of generated residual stresses, which affect the mean stress in fatigue loading.7,18,19 Incidence of plate removal due to plate fracture has already been reported to as high as 18%. 20 Our institutional experience with 126 patients from last 10 years suggested a failure rate of 19.8 % (25 patients) when plate was not pre-adapted. To function without failure, the plates should be pre-bent preoperatively, so as to match closely and passively with the three-dimensional shape of the mandible in order to avoid any bending during the surgery. This human error can be to a good extent obviated by use of 3d-printed models, thereby enhancing the qualitative improvement in the end result. Azuma et al reported that the use of reconstruction plates that are pre-bent to fit 3d-printed models in mandibular reconstructive surgery resulted in improved aesthetic outcomes with potential for improved QOL of the patients compared to the use of conventional reconstructive methods. 21 Wilde et al and Naros et al also reported about the superior accuracy of pre-bent plates over intraoperative bending method.22,23
Rapid prototyping using 3d-printed model have also been utilized for variety of other purposes since its introduction. 6 3d-printed model are an effective surgical tool when planning resections and reconstruction in the maxillofacial region as they aid in planning the osteotomy lines, deciding on the graft size, construction of custom-made hardware and determining plate and screw position. Studies suggest that computer assisted surgeries reduces surgical time and ischemia time for maxillofacial reconstructive surgeries.3,4,8,22,24 Erickson et al 25 in their study reported reduction of operating time from 17% to 60%, with an average of 20%. According to Toro et al, the reduction in operative time amounted to almost 1-1.5 hours when using pre-bent reconstruction plates.17,26 In our study we found a reduction of 14.75% in operative time.
In our study, we found that there is significant reduction in post-operative pain and immediate post-operative mouth opening. This could be possibly due to avoidance of unnecessary muscle stripping which could lead to trismus and pain. The same reason could be attributed to the reduction in surgical site infection.
Quality of life was assessed using UW-QOL questionnaire as described by Young et al. Comparison of the social and functional domain showed that the all the group of patients in group A fared better than those without medical prototyping and most of the patients chose the best scores in domain saliva and taste. The burden of symptoms related to swallowing and chewing was selected as poor to worse by most of the patients in each group. In global questions, the overall QOL during the past 7 days of assessment appeared to be similar in NVG group and RP group but in MR group the patients using 3d-printed model fared better. Percentage best scores of UW-QOL revealed that group A patients opted better scores compared to group B. One of the caveats in our QOL assessment was the wide range in follow up period extending from 9 to 2 years.
At our institute, while treating maxillofacial pathologies, traumatic defects and an osteonecrotic defect due to a gunshot wound, 3d-printed model were made using an open source software already approved by institutional ethical committee and were incorporated for treatment planning, patient education and motivation. With our prior experience of intraoperatively adapted plates, it was noted that the imprecision in a few cases had resulted in plate failures, including TMJ pain as a result of a displaced condylar segment. To overcome this debacle the 3d-printed model were used to accurately adapt reconstruction plates preoperatively. They were also used for determining the size of the graft or flap as well as the position of the immediate implant in the graft prior to reconstruction. In cases where the size of the lesion or defect distorted the regional anatomy thereby causing trouble in defining the original contour of the skeleton; mirroring of the healthy contralateral side 27 or sculpting of the bio-model was done for assessment and planning, so as to rebuild the diseased.
Preadapting and contouring of the reconstruction plates and the mesh lead to reduced operative time, better postoperative period and an aesthetic outcome in all the cases. It was also found that the 3d-printed model played an important role in resident training as it offered hands on experience with reconstruction hardware. Another advantage in our experience was that, the 3d-printed model could be kept as a record for future evaluation of patients and could be used again in any case of recurrence of the disease.
As noted by Salgueiro et al and Isler et al, the principal disadvantage of using an 3d-printed model is its high cost, however since preplanning using 3d-printed model leads to a better patient satisfaction and reduced chance of plate failure, additional preoperative costs may be justified.17,28 Since our institution is a tertiary care center, catering to the needs of average to below average, economically weak patient population, it is not uncommon to come across such cases. In 1 such case, we improvised using a stock mandibular model of comparable dimension verified by assessing the dimension of the inferior border of mandible using an axial view of 3-D CT and got good results postoperatively. In our experience, planning with 3d-printed model, is a more affordable option than computer-designed patient specific implants [PSI] even though PSI offers higher accuracy and adaptation compared to pre-bent plates. 29
One limitation of our study was that we opted manual sculpting of 3d-printed model rather than digital sculpting in lesions crossing midline. Also no surgical cutting guides or resection templates were made using the bio-models as it would have caused financial burden on the patients. Another drawback of this study was its confounding factors associated with varied number of patients and pathologies. There still remains a paucity of large-scale, well-controlled clinical studies supporting the use of 3D printing technologies. 30
Conclusion
The versatile usage of 3d-printed models for maxillofacial reconstruction as a very useful tool in treatment planning, resident training, patient education & record maintenance, has been amply explained and demonstrated in the 21 cases discussed in the above article. This further amplifies the successful use of bio-models for improving the predictability of treatment of maxillofacial defects secondary to traumatic or pathologic conditions. With increased success rate, and patients reporting better quality of life, the authors are of the strong opinion that it is time to revisit the surgical protocol used for reconstruction and include 3d-printed models as a primary tool or technology across the board for all patients notwithstanding the comparative cost, as the results offset the financial aspect.
Supplemental Material
Supplemental Material - Analysis of Quality of Life With 3D-Printed Model VIS - À - VIS Conventional Procedure in Oral & Maxillofacial Surgery – An Empirical Study
Supplemental Material for Analysis of Quality of Life With 3D-Printed Model VIS - À - VIS Conventional Procedure in Oral & Maxillofacial Surgery – An Empirical Study by Zainab Chaudhary, Mithilesh Kadanthode, Pankaj Sharma, Sujata Mohanty, Ragavi Vijayaragavan, PS Bhandari, Lalit Maini, and Shekar Grover in Craniomaxillofacial Research & Innovation
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Clearance
This study was exempted by Ethical Committee of Maulana Azad institute of Dental Sciences as it was a retrospective study. Consent was taken from all patients for publication of clinical photographs.
Supplemental Material
Supplemental material for this article is available online.
Appendix
Abbreviations List
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
