Abstract
Study Design
Case series
Objective
By reporting several cases of dislocated foreign bodies, we aim to make dentists/surgeons aware of possible severe and potentially life-threatening complications. In case of dislocation, the appropriate radiological assessment depending on the foreign body is required if direct removal fails.
Material and Methods
Electronic and paper record of patients suffering from various dental foreign bodies were analysed. Analysis included history of dislocation, type of foreign object, anatomical region of dislocation, related dental treatment and approach to surgical removal.
Results
In total, 5 patients with various dental foreign body objects, including fractured root canal instruments (n = 2), a broken dental injection needle (n = 1), a broken Lindemann bur (n = 1) and root filling material (n = 1) are reported. Patient ages ranged from 14 to 54 years. In 4 cases, the foreign body could be salvaged successfully, and one patient refused the surgical therapy. General anaesthesia was required in 4 patients. Intraoperatively, a 3D C-arm was used in 3 cases to ensure the successful recovery of the foreign bodies. In 1 case, the foreign body could be removed with endoscopical assistance.
Conclusion
The management of dental materials and instruments requires diligent care by the practitioner, and prevention techniques should be used at all times to minimise the patients’ risk. In the case of foreign body dislocation, appropriate radiological assessment and determination of further medical treatment (if necessary) should take place. During surgical procedures, intraoperative 3D-imaging, as well as endoscopic techniques, are helpful tools to ensure the recovery of foreign bodies.
Keywords
Introduction
Maxillofacial surgeons are often confronted with foreign bodies in the head and neck area, such as the oral cavity or the anatomically adjacent regions. The main causes for dislocated foreign bodies include violent acts, accidents, self-inflictions by the patient, or as described here, dental treatment.1-3
Common steps in dental/oral surgeon routine, such as the application of local anaesthesia, can be potentially life-threatening.4,5 Dental interventions, which are performed routinely all over the world, take an unexpected turn when an accidental aspiration or ingestion, for example, of an extracted tooth or a root canal instrument, occurs.2,3 Broken instruments bear the risk of being dislocated into the bone or the surrounding soft tissue, with severe consequences. Because of the proximity of the oral cavity to many vulnerable anatomic structures, the effect of a broken bur or a broken root canal instrument might be tremendous.6,7
These foreign bodies may differ in position, density, size and potential for infection, and therefore in the severity and the possible risk for the patient.
A detailed medical history followed by an extensive clinical examination is inevitable and should be the first step in the treatment regime. Efficient imaging is often essential in order to decide on further procedures. Diagnostic procedures including 3D-imaging, intraoperative 3D navigation and endoscopic techniques offer additional information and facilitate the localisation of the foreign object. 8
Dislocated foreign bodies are often hardly accessible without general anaesthesia, as additional surgical accesses are often needed, including the expansion of the existing surgical wound. 9
The following cases provide an overview of the diagnostic and suitable treatment of dental foreign bodies in the head and neck area.
Material and Methods
Ethics Statement
The Ethics Committee of (the Faculty of Medicine Charité, Medical University Berlin), approved this study EA1/175/20.
Study Design
In this case series, we present 5 patients who underwent routine dental/oral surgical treatment in dental practice. All patients suffered from dislocated or remaining foreign bodies in the head and neck area between January 1st 2000 and 31st June 2020 and admitted to our Department of Oral and Maxillofacial Surgery, Campus Virchow-Klinikum, Charité – Universitätsmedizin for further treatment. The mean age was 35.8 years, ranging from 14 to 54 years. Four patients required general anaesthesia and inpatient treatment, ranging between 1 and 5 days in hospital (mean 2.5 days). One patient refused the operation due to a lack of symptoms (Patient No. 4). Intraoperative use of diagnostic 3D-imaging, endoscopic equipment and navigation systems were available as needed.
Case Series
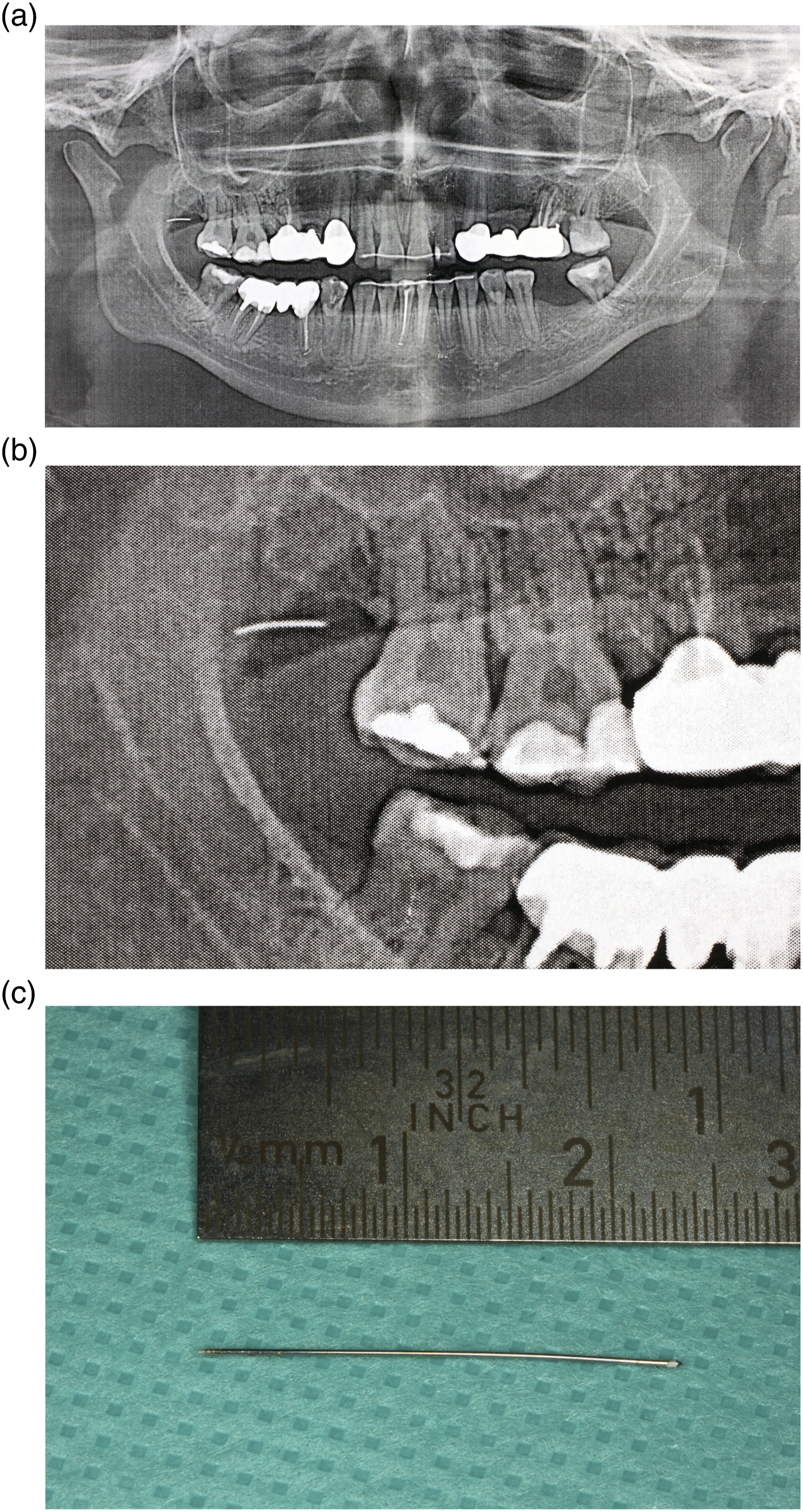
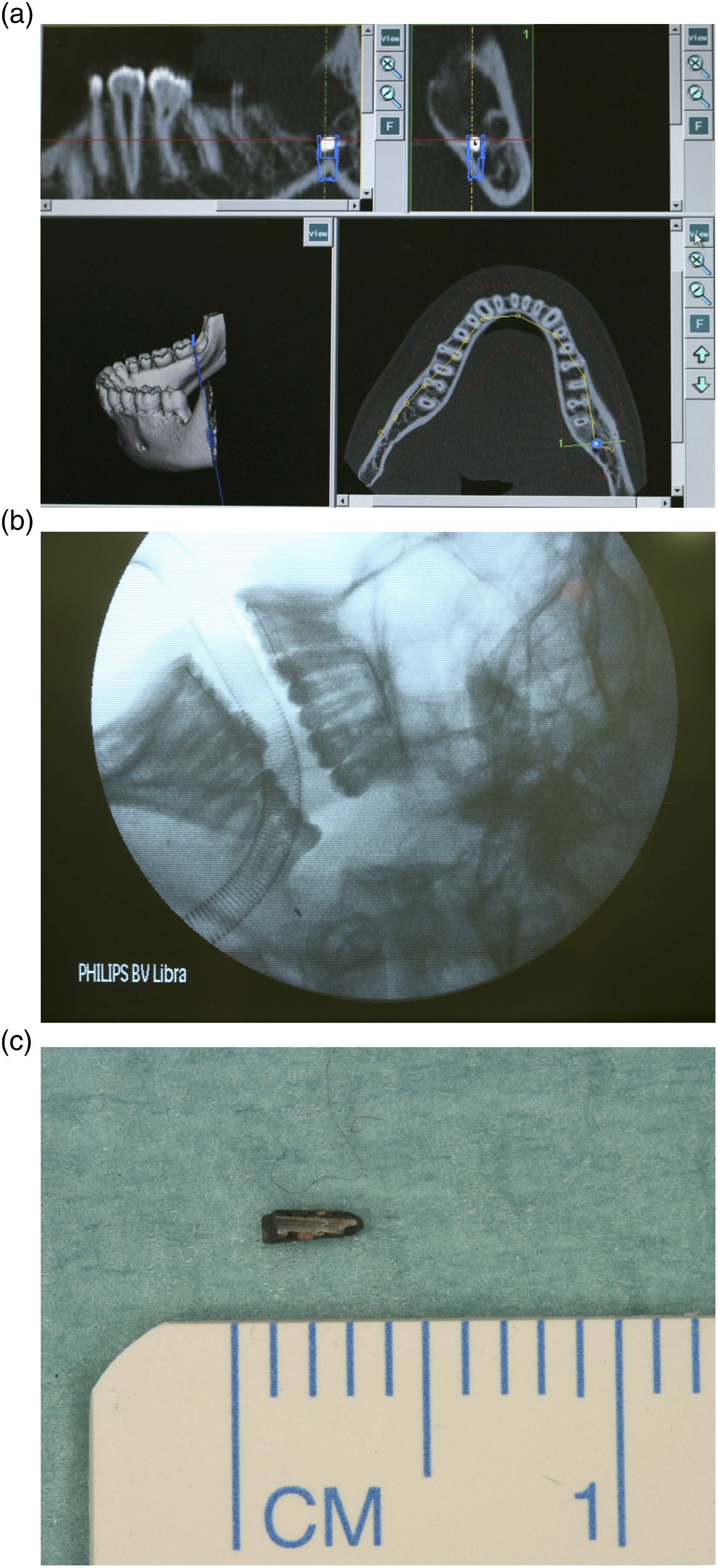
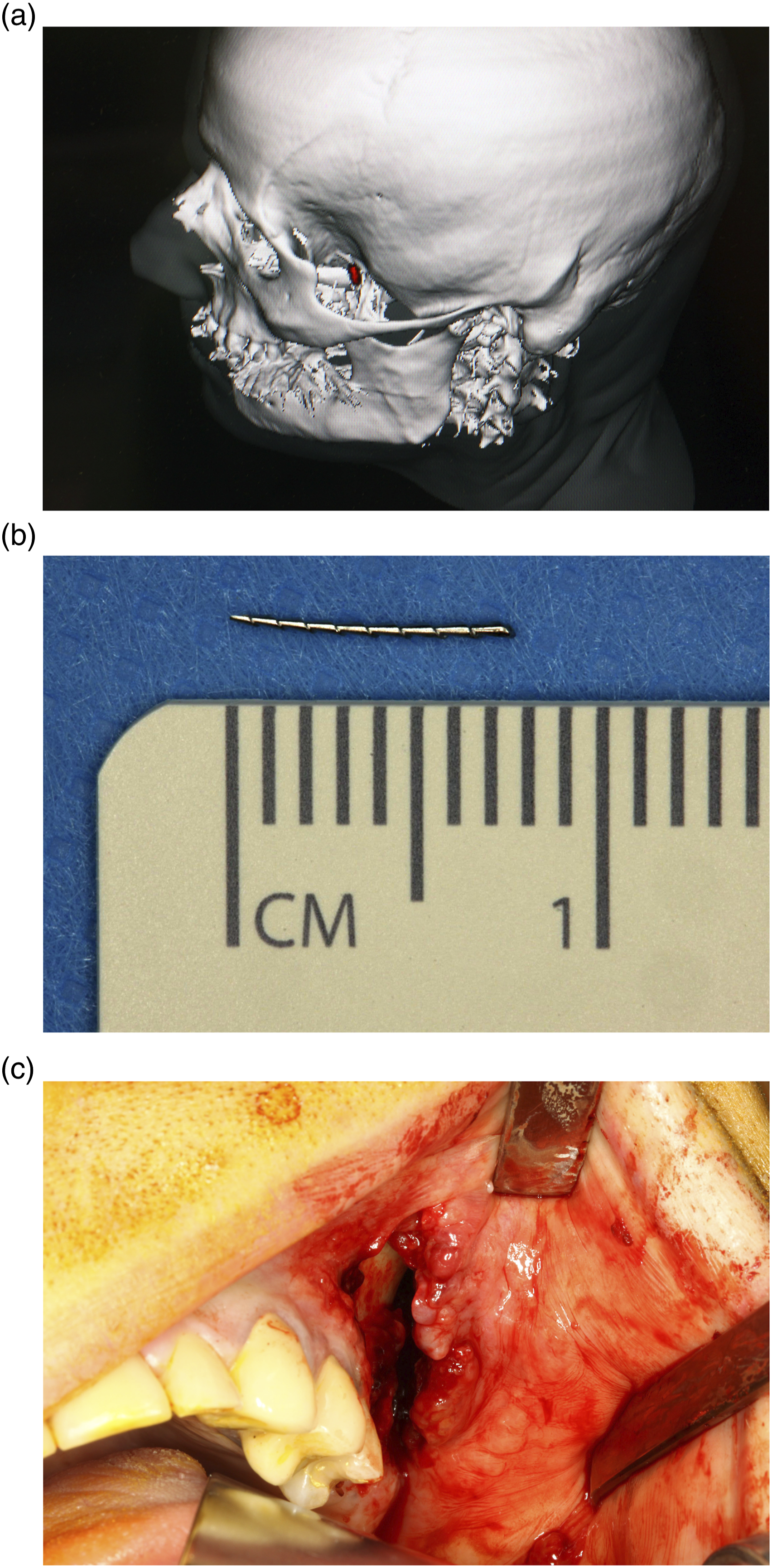
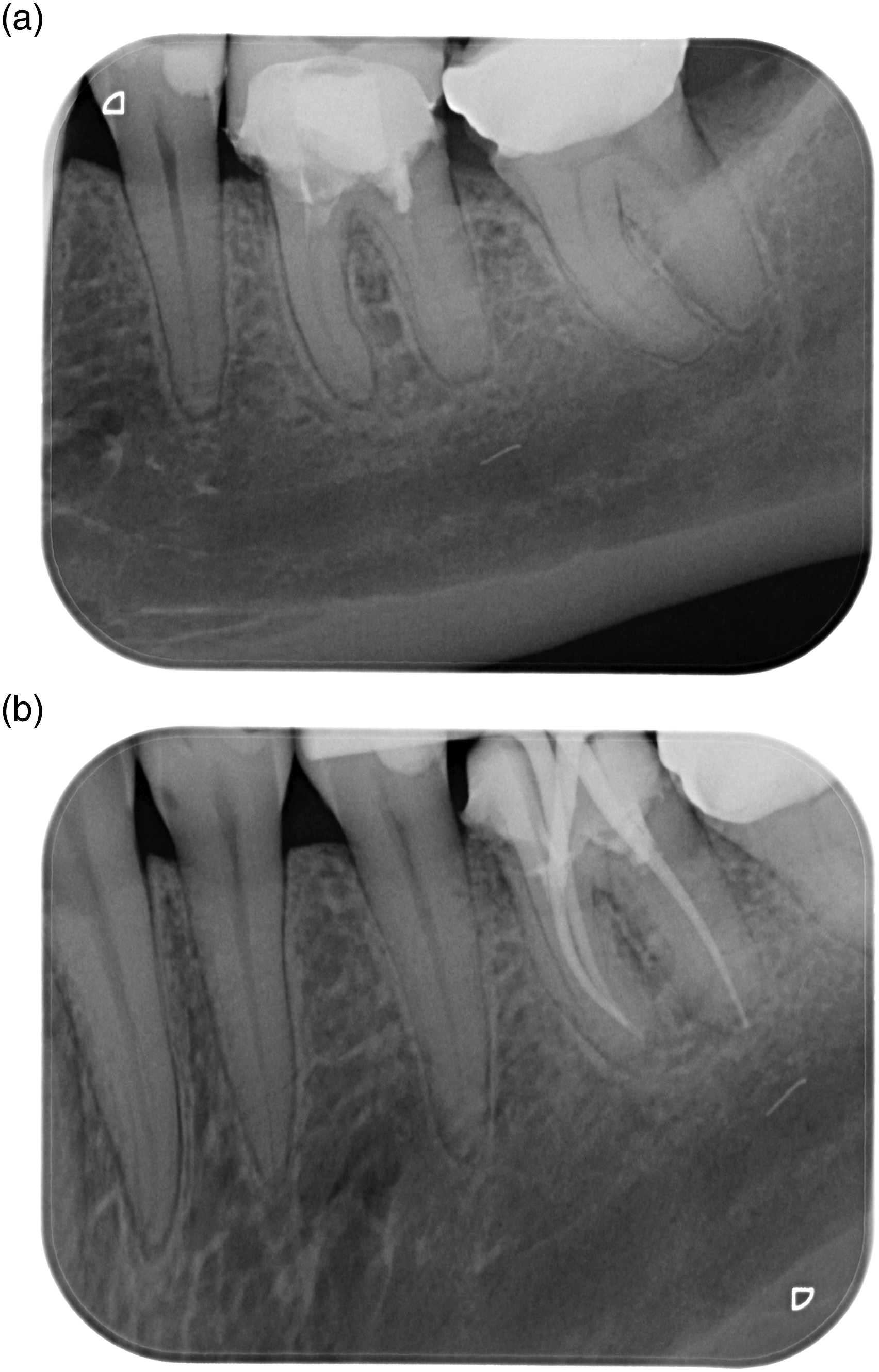
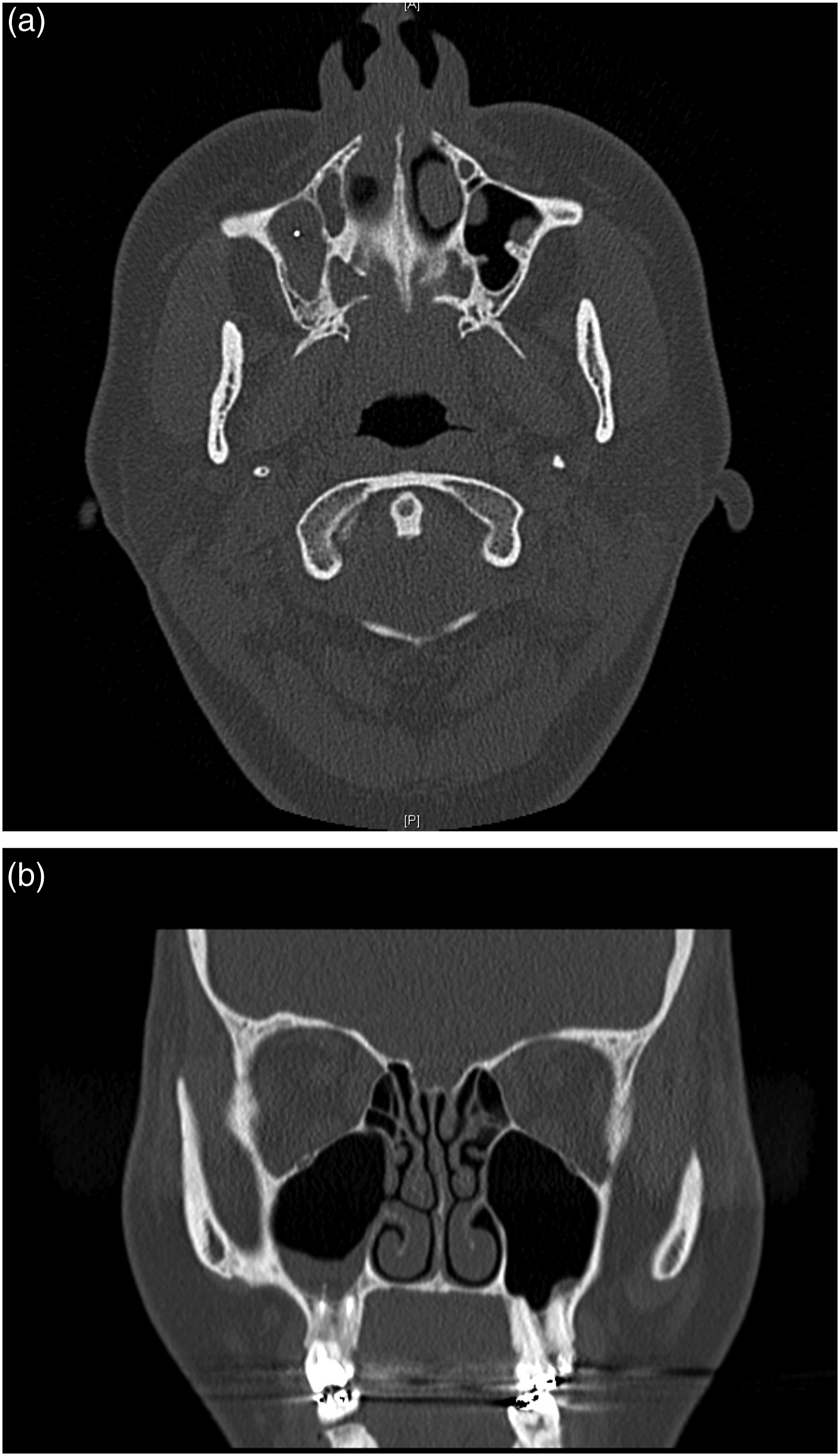
(1) A 37-year-old female patient suffered from a broken syringe cannula during the block of the right inferior alveolar nerve. Even though the missing part could not be recovered by the dentist, no further radiological imaging was performed. A panoramic view displayed the missing part in the right parapharyngeal space (Figures 1A and 1B). Under general anaesthesia and the intraoperative use of a 3D C-arm, the broken syringe cannula, measuring 24 mm, was removed through a small intraoral approach (Figure 1C). The patient could be discharged after 2 days without further complaints. (2) A 14-year-old female patient approached the emergency room after the failed removal of tooth 38 under local anaesthesia. During the procedure, the drill tip broke and remained adjacent to the left inferior alveolar nerve. After cone beam computed tomography was performed (Figure 2A), the surgical removal of the drill tip under general anaesthesia was planned. Intraoperative 3D navigation was successfully used, and the lost drill tip of 3 mm was removed (Figures 2B and 2C). No hypaesthesia of the inferior alveolar nerve occurred postoperatively. The radiological follow-up showed no remaining foreign bodies, and the patient could be discharged 1 day after. (3) A 54-year-old male outpatient suffered severe chronic pain in the left infratemporal region after the root canal treatment of tooth 26. During the procedure, the root canal instrument fractured and remained in the left infratemporal space. A CT scan revealed a dislocated foreign body of 8 mm (Figures 3A and 3B) in the left infraorbital region. We planned the removal under general anaesthesia, since previous attempts under local anaesthesia had failed. Endoscopically assisted, intraoperative 3D navigation was used to remove the foreign body using an intraoral approach (Figure 3C). The patient could be discharged after 2 days without further complaints. (4) A 40-year-old female patient presented with a broken part of the root canal instrument in the right mandibular canal after the root canal treatment of tooth 46. Unfortunately, the broken part dislocated into the mandibular canal, with no chance of being retrieved without an extended surgical approach. Root canal treatment was completed before the patient was brought to our emergency room. During the dental procedure, single-tooth radiography was performed and showed the missing part (Figures 4A and 4B). However, the surgical removal under general anaesthesia was cancelled by the patient after she was informed about the existing risks regarding the inferior alveolar nerve. (5) A 34-year-old female patient was brought to our emergency room after undergoing root canal treatment of a right upper molar 2 weeks prior. An orthopantomogram and computed tomography were initiated (Figures 5A and 5B), showing almost one centimetre of radiopaque material at the root tip of tooth 16. Obviously, the length of the root canal was calculated incorrectly, and the filling material was too long. Due to reduced general conditions, apicoectomy of tooth 16, the removal of the foreign body and, in this context, a final retrograde root canal filling was performed under general anasthesia. The patient received prolonged systemic antibiotic treatment and could be discharged 5 days later with improved condition. (a) Orthopantomogram showing the missing part of the syringe cannula in the right parapharyngeal space. (b) The missing part of the syringe cannula, displayed in right parapharyngeal space. (c) The broken syringe cannula, measuring 24 mm. (a) Cone beam computed tomography, showing the broken drill tip closed to the left inferior alveolar nerve. (b) Intraoperative radiological imaging, showing the missing drill tip region 38. (c) The recovered drill tip, measuring 3 mm. (a) 3D-CT-scan, showing a dislocated foreign body in the left infraorbital space. (b) The removed broken root canal instrument, measuring 8 mm. (c) Intraoral approach region 23-26. (a) Initial single tooth radiology of tooth 46. (b) Single tooth radiology, showing the fractured and dislocated root canal instrument in the right mandibular canal. (a) Axial view on the computed tomography, showing radiopaque material in the middle of the right, shadowed maxillary sinus. (b) Coronal view on the computed tomography, showing radiopaque material on the floor of the right maxillary sinus.
Discussion
Dislocated and remaining foreign bodies related to dental treatment/oral surgery are well reported in head and neck surgery, but treatment remains challenging due to difficult access, unfavourable location or a combination of both.8,10 Every single step in common dental treatment, and especially in dental surgery, can be, if performed incorrectly, potentially life-threatening,4,10,11 because of the high number of vital structures in the head and neck area.
The diagnosis of dental foreign bodies can be especially challenging when the missing object is not visible during the clinical examination. First, a detailed medical history should be taken, followed by a meticulous clinical examination. Since all of the described dental foreign bodies were found in juvenile/adult patients, a full clinical examination should be practicable.
Diagnostic imaging is an essential tool in detecting foreign bodies in the head and neck area,9,12 and includes ultrasound, 13 X-ray, 14 computed tomography (CT), 14 magnetic resonance imaging (MRI) and cone beam computed tomography (CBCT). 15 The radiological assessment should be adapted to the suspected or missing foreign body by the underlying composition of the object. 14
Previous studies showed that CT is regarded as the gold standard and should be the first-choice modality.14,16 If the missing object is known to be radio-opaque, conventional plain radiography can be used as an initial imaging technique. 14 Abolvardi et al. showed that CBCT can be used with almost equal accuracy as CT for detecting foreign bodies in the head and neck area, 15 which is consistent with our observations concerning dental foreign bodies. Since CBCT is generally easier to implement and involves a lower radiation exposure, the usage of CBCT in detecting (dental) foreign bodies in head and neck is highly recommended.
Commonly, MRI is not used initially in cases with missing dental foreign body, especially when the composition is known to be ferromagnetic.9,14 Additionally, MRI is still expensive, not always available and not susceptible to artefacts caused by metal and even plastic.17,18
Intraoperatively, a C-arm can be used in order to provide excellent additional support for the localisation of the foreign body. 9 In the present study, a C-arm was used in three cases.
If the missing dental foreign body is expected to be located in easily accessible superficial soft tissue in the head/neck-area, ultrasonography is an excellent option. 13 High-resolution ultrasound, in particular, provides a dynamic, inexpensive and portable imaging method, with real-time imaging and no radiation exposure.13,14
Since foreign bodies in the head and neck are well known to cause an acute or chronic infection, and in rare cases even an immune response, 19 immediate retrieval should be planned and carried out.9,19 Further indications such as neurological, mechanical and functional impairment have to be considered as well. 9 Even if the wound healing proceeds uneventfully, the patient has to be informed of possible sequelae, even after years (Case No. 4).19,20
All patients in this study required general anaesthesia because the missing dental foreign bodies were barely accessible and additional surgical accesses were needed. Existing wounds had to be expanded. However, dental foreign bodies are mostly difficult to access and/or directly adjacent to vital structures, which makes us believe that a removal under general anaesthesia should be the first choice, especially if removal was not successful under local anaesthesia in the first place. Endoscopically assisted or intraoperative navigation offer an additional help in the localisation of the missing object (Case No 3). 21
Since local anaesthesia is regularly used in dental treatment, risks such as allergic reactions, flushing and swelling, and, in particular, the risk of needle breakage are given. Needle breakage occurs mostly during the blockage of the inferior alveolar nerve.22,23 In these cases, the remaining needle part(s) are located in the pterygomandibular space, in which many vital structures are found. When local anaesthesia is used, it has to be ensured that the injection needle is in good condition and not weakened, for example, by (pre-) bending, or too thin and short. In addition, the risk of sudden patient movement has to be minimised.22,24 Dental instruments, such as a Lindemann bur, are a potential threat to the patient and the medical staff. In 2016, Matsuzaki et al. 6 reported a rare case in which a broken dental bur penetrated the medial orbital wall of a dental assistant. Rajaran et al. 25 reported a case of a broken bur that dislocated into the mandible, and stated that many comparable iatrogenic complications could be avoided easily with the use of proper equipment and technique. Another rare case was reported by Voss et al., where a dislocated dental bur was discovered accidentaly during an MRI scan years after the removal of a molar in the upper jaw. Here, the loss of the bur was not further investigated by the dentist. 19
Any dental instrument can in principle fracture or dislocate totally, whether due to stress, microcracks, poor manufacturing, fatigue or misuse.19,25 That indicates the importance of intraoperative inspection of the returned instrument and, if necessary, the replacement of the used instrument by the medical staff. Furthermore, the selection of patients treated under general anaesthesia is of particular importance, to assure that the risk of potential complications is as low as possible. It is essential for the dentist/dental surgeon to have anatomical knowledge, and the anatomic structures should be protected by any means.
Fractured root canal instruments represent a foreign body, which can be dislocated in different anatomic regions. Mostly, a breakage in the root canal occurs. In this case, the prevalence of the fractured root canal instrument differs from 0.5% to 5% and depends on the system being used.26-29 Besides infection and a poor prognosis for the preservation of the tooth, a fractured root canal instrument can cause severe injury of the vital structures. Such complications appear in the case of migration beyond the tooth apex in the jaw, and in the worst case, damage to the inferior alveolar nerve may occur.27,28 In case of fractured endodontic instruments in the canal, non-surgical removal, such as ultrasound, is possible and represents an effective way in recovering fractured root canal instruments. 30 On the one hand, ultrasonic removal is mostly successful, even if the fractured file is located deep in the canal. 31 On the other hand, it can cause new microcracks that can weaken the tooth. 31 If migration beyond the tooth apex takes place, a surgical approach may be indicated. 26
The presented cases showed a variety of dislocated files, which were located in the temporal region, the floor of the maxillary sinus and the mandibular canal. On the latter occasion, a surgical approach was defined by the position of the foreign body. The remaining foreign bodies, regardless of their origin, can possibly migrate, especially through repetitive muscle contraction such as swallowing and chewing, and should therefore be removed immediately. 10
Besides foreign bodies that can be found in the head and neck, aspiration and ingestion of dental instruments, materials or the tooth is a potential risk, but is quite uncommon in dental treatment. 32 If aspiration occurs, the foreign body might be removed immediately by reflexive coughing; otherwise it should be removed within 24 hours by bronchoscopy or surgery. 33 Alternatively, acute airway obstruction could appear. 33 In contrast, most cases of ingestion do not require the immediate recovery of the dental foreign body because foreign objects often pass through the gastrointestinal tract uneventfully. 34
All cases emphasise how important the risk-minimisation of dental foreign bodies is and that prevention should be carried out, if possible, by any means. The patients’ medical and mental condition should always be considered in the selection of the right treatment. In order to reduce the risk of aspiration or ingestion, a rubber dam, ligation or even a throat pack can be used. 35
Conclusion
The presented variety of cases outline a selection of severe complications in the daily routine of dental treatment/oral surgery and demonstrate that the management of dental materials and instruments requires particular care. Possible prevention techniques should also be used at any time to minimise the patients’ risk, and the patients’ medical and mental condition should be considered in the selection of the suitable treatment. If the missing foreign body cannot be located, 3D-imaging such as a CT scan or cone beam computed tomography is imperative. This allows the intraoperative use of a 3D image converter as well as intraoperative navigation, which represents a successful tool to ensure the recovery of foreign bodies. If the foreign body is located in the maxillary sinus, endoscopic interventions enable a minimally invasive and reliable method of removal.
Footnotes
Acknowledgements
We thank (Franz Hafner) for his photographic documentation.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Dr. Dr. Jan Voss is a participant in the BIH-Charité Clinician Scientist Program funded by the Charité-Universitätsmedizin Berlin and the Berlin Institute of Health.
