Abstract
Background
Cervical cancer disproportionally burdens Hispanic immigrant communities in the United States, despite its preventable nature and curability when detected early. These persistent disparities represent a “wicked problem,” characterized by contested evidence, fragmented data, and a politicized health policy environment.
Methods
This study uses Tarrant County, Texas—a high-disparity urban region—as a case study to explore how multilevel governance structures shape immigrant health inequities. Drawing on the concept of wicked problems and the political determinants of health (PDoH) framework, we analyze archival data through a policy science lens to examine how electoral, legal, and institutional forces perpetuate barriers to life-saving care for immigrant women.
Results
Four key themes emerged from our analysis: (1) a reactive political environment that amplifies exclusion, (2) decision-making shaped by legal ambiguity, (3) passive enforcement of immigration policies through institutional design, and (4) blame-shifting between public and private healthcare systems. These dynamics collectively sustain health disparities by limiting access to preventive care and delaying treatment among immigrant populations.
Conclusion
Findings demonstrate that cervical cancer disparities are not solely the result of individual health behaviors but are produced and sustained by structural and political forces. Addressing these disparities requires interdisciplinary partnerships and place-based strategies that confront the institutional barriers embedded in local governance. We call for strategic alliances among researchers, community stakeholders, and policymakers to foster shared accountability and develop responsive, equity-driven policies for addressing cervical cancer and other preventable conditions in immigrant communities.
Keywords
Background
In 2018, the World Health Organization issued a call for action to eliminate cervical cancer as a public health problem. 1 A highly preventable and treatable disease, cervical cancer is the fourth most prevalent cancer among women worldwide. 2 More than 99% of cervical cancer diagnoses are linked to the human papillomavirus (HPV), a common viral infection transmitted through sexual contact. 3 Because cervical cancer progresses slowly—often taking up to 20 years to develop—early detection and prevention critical.4,5 Public health initiatives, such as HPV vaccination and Papanicolaou smear screening tests (Pap tests), have significantly reduced cervical cancer incidence in the U.S. and other high-income countries. 6
Despite these advances, disparities persist. 7 Hispanic women in the US are over 32% more likely to be diagnosed with cervical cancer than non-Hispanic white women. 8 Early detection drastically improves survival rates, with a relative survival rate exceeding 91% when cervical cancer is diagnosed at an early stage. 9 However, once the disease progresses, survival rates drop below 20%. 10 Hispanic women also experience greater delays in treatment initiation, 11 exacerbating existing inequities. These disparities are even more pronounced among immigrant women, particularly those with irregular political status, who are more likely to present with advanced disease and face higher mortality rates compared to their U.S.-born Hispanic counterparts.12–15
It is essential to recognize the practical limitations of socio-political categories for understanding the root causes of cervical cancer disparities. Cancer surveillance systems typically rely on the term “Hispanic” as a bureaucratic label to describe individuals with origins in one or more Latin American and Caribbean countries. 16 As Martínez and Rhodes note, however, terms like “Hispanic” and “Latino” are rooted in colonial practices that obscure meaningful within-group differences among the 65 million individuals in the US (19% of the US population) who fall under these labels.17,18 These broad ethnic categorizations effectively homogenize multilingual, multinational, and multiracial subgroups with distinct histories of colonization, migration, and racial formation.19,20
This is further evidenced by the so-called “Hispanic paradox,” an epidemiologic phenomenon characterized by persistent findings of similar or improved survival outcomes among Hispanics relative to non-Hispanic Whites. 21 A closer examination of Hispanic subgroups reveals significant intergroup variation between US-born and foreign-born Hispanics, as well as among groups from different global regions (e.g., Mexicans, Dominicans, Central Americans).22–24 However, neither nativity status nor national origin are systematically collected in cancer registries or national health surveys, limiting the availability of comprehensive data and reinforcing evidentiary gaps. 25
Unlike race and ethnicity, relatively static characteristics generally captured through self-identification, 26 immigration status is a fluid and externally imposed legal-political classification. 25 This is a critical distinction requiring an analytic approach that moves beyond individual behaviors or cultural factors and instead examines how health disparities are actively shaped and sustained by policy decisions. By shifting the focus from individual-level attributes to structural conditions and political context, we can better understand how exclusionary healthcare policies, immigration enforcement mechanisms, and multilevel governance structures contribute to cervical cancer disparities.27–29
Policy Instability and the Accumulation of Health Disparities
Unlike acute conditions that require immediate intervention, cervical cancer’s long latency period makes it particularly vulnerable to political and economic instability.30,31 This instability can manifest through changes in Medicaid eligibility,32,33 shifting public health funding priorities, 34 and variable enforcement of immigration policy. 35 For example, in states that expanded Medicaid under the Affordable Care Act (ACA), cervical cancer screening rates among low-income women improved, whereas access remained limited in states that opted out of expansion.36,37 Resource-strained health systems in regions with large numbers of uninsured patients must often make difficult decisions to ration treatment services or identify alternative pathways for care.38,39 At the same time, restrictive immigration policies—such as expanded public charge rules or increased cooperation between local law enforcement and federal immigration authorities—have deterred immigrant women from seeking care, even when they remain technically eligible for services.40,41
Public health officials have advanced various strategies to promote cervical cancer screening and detection among Hispanic women,42,43 including interventions delivered by community health workers (CHWs) that are culturally and linguistically tailored.44–46 However, a shifting policy landscape can alter healthcare access during a woman’s adolescence, reproductive years, or menopause--critical points when HPV vaccination, routine screening, and follow-up care are most necessary. 47 This can result in disruptions along the continuum of care, such as gaps in preventive care, delayed screenings, missed vaccinations, and lapses in treatment adherence. Each missed opportunity for prevention or early detection increases the likelihood that immigrant women will be diagnosed at later stages, when survival rates are significantly lower. 11
Cervical cancer screening campaigns have demonstrated promise in increasing awareness and early detection, 6 but they risk unintended harm in settings where access to treatment is limited. 48 In regions with restrictive health coverage policies, expanding screening without ensuring follow-up care may lead to a rise in diagnoses among women who face significant structural barriers to treatment—underscoring the need for policy change alongside behavioral interventions. 49 These dynamics underscore the contested nature of both causes and potential solutions to cervical cancer disparities, hallmarks of a public health dilemma that resists straightforward resolution. 50
A Case Study of Cervical Cancer Disparities as a “Wicked Problem”
Geographic variations in cervical cancer disparities among Hispanic women can serve as an indicator of broader systemic inequities,49,51–53 pointing to regions where the intersection of immigration policy and healthcare governance systematically shape access to care and delay early detection and treatment.54,55 In a multi-year study launched in 2017, the American Cancer Society (ACS) Cervical Cancer Mortality Disparities in U.S. Hispanic Women Study identified Tarrant County, Texas as a “high disparity” region due to elevated cervical cancer mortality rates among Hispanic women. 56 Researchers applied a previously-tested mixed method approach 57 to study modifiable barriers and facilitators contributing to this issue. Findings revealed that political conditions and restrictive health policies contribute significantly to disparities among immigrant families in the region (see Figure 1).
The third most populous county in Texas, Tarrant County is home to a large and diverse population of 2.1 million residents. 58 Hispanics constitute nearly 30% of the population, and the majority of the foreign-born population is of Mexican origin.59,60 Tarrant County is located in the Dallas-Fort Worth-Arlington (DFW) metropolitan area, one of the top five U.S. metropolitan destinations for unauthorized immigrants, 61 further positioning it as a crucial site for examining political determinants of immigrant health.
The Tarrant County Public Hospital District (dba JPS Health Network) is the second-largest public hospital system in the DFW area. Unlike neighboring Dallas County, which has expanded local health programs to include immigrant populations, Tarrant County has historically restricted access to subsidized healthcare for non-citizens.62,63 Over the past two decades, the JPS Health Network has maintained financial assistance policies that exclude individuals without U.S. citizenship or lawful permanent residency from receiving subsidized non-emergency care. These restrictions, adopted by the hospital district’s governing board, remain in place today. While the JPS Health Network does not outright deny healthcare access based on immigration status, restrictive financial assistance policies can discourage immigrant persons from seeking out preventive and routine health care services, particularly in areas with a higher immigrant population density.64,65
Tarrant County serves as an illustrative case study of cervical cancer disparities as a “wicked problem.” This term was coined by Rittel and Webber to describe policy challenges characterized by incomplete knowledge, contested causes, and resistance to straightforward solutions.66,67 As a “wicked problem,” cervical cancer disparities emerge from iterative interactions across systems—healthcare policy, immigration enforcement, and governance structures—and persist despite medical advances.68–70 These interactions complicate clear problem definitions and policy solutions, underscoring the need for interdisciplinary approaches that consider long-term, structural dynamics.
Analyzing Structural Drivers of Cervical Cancer Disparities
While cervical cancer disparities are often framed in public health discourse as a matter of preventive behaviors (i.e., adherence to regular Pap smears and HPV vaccination), they are in fact highly contingent upon policy decisions that are often politically motivated and subject to change. Understanding why cervical cancer disparities persist—despite advances in prevention and treatment—requires analysis beyond empirical data. Bridging the research-to-policy gap of “wicked problems,” such as cervical cancer disparities among Hispanic women, calls for a deeper examination of the structural forces that sustain these inequities.
Drawing on interdisciplinary expertise in health policy and immigrant health, this paper applies the Political Determinants of Health (PDoH) framework to analyze the institutional and governance structures that shape cervical cancer disparities. The PDoH framework refers to the “systematic process of structuring relationships, distributing resources, and administering power, operating simultaneously in ways that reinforce or influence one another to shape opportunities that either advance health equity or exacerbate health inequities.” 71 (p. 44) This model highlights how electoral trends, policy shifts, and governance structures shape access to preventive care and standard cancer treatments for women. 70 By applying this framework, we move beyond individual health behaviors to examine how structural forces—such as restrictive healthcare policies, immigration enforcement mechanisms, and political decision-making—interact to drive disparities in cervical cancer outcomes.
We ground this analysis in the case of Tarrant County, Texas, a “high disparity” region for cervical cancer mortality among Hispanic women. 56 Although the authors of this manuscript did not lead the ACS Cervical Cancer Mortality Disparities Study that conferred this designation, they collaborated with stakeholders involved in its dissemination and used its findings to launch a multi-year academic-community partnership focused on identifying structural barriers and opportunities for policy engagement. This collaboration informed the conceptual framework and policy analysis in this manuscript, drawing on archival data, stakeholder engagement, and applied policy science to extend the study’s relevance to immigrant health equity. This article builds on those findings through an analysis of the local, state, and national policy landscape to illustrate how structural constraints—ranging from county-level hospital policies to federal immigration enforcement—converge to drive disparities in immigrant health. Tarrant County thus serves as an entry point for exploring how governance structures shape access to preventive and life-saving care for politically marginalized women.
The PDoH paradigm has been leveraged to explore the roles of health systems and health providers in reducing health inequities through voting, decision-making, and policy initiatives.70,72–75 While PDoH offers a useful conceptual lens, it draws from longstanding traditions in public health research, including intersectionality-based policy analysis, 76 political economy approaches to health inequities77,78 and global frameworks such as the WHO’s Social Determinants of Health model, 79 which emphasize the critical role of political and socioeconomic context in shaping health outcomes.
Using conceptual frameworks from the policy sciences, we examine the intersection of policy environments, healthcare systems, and immigration governance to illustrate how institutional constraints shape the healthcare landscape for immigrant women. Our approach integrates archival review of local policies and governance structures in Tarrant County with contextual analysis of state and national policy environments. 73 By gaining a deeper understanding of the “upstream” structural forces that shape “downstream” health barriers, we argue that scholars and policymakers can engage in strategic partnerships to drive meaningful action informed by a shared understanding of the local environment.
We began by exploring national, state, and local media coverage and public archives relating to immigrant and immigrant health. This process identified widespread media coverage over controversial hospital district policies, federal and state statutes, legal opinions over Texas county obligations to subsidize healthcare for non-citizens, and hospital board minutes detailing speakers for and against the policy. We then drew on salient policy science frameworks to interpret these materials and identify key patterns. This allowed us to conceptualize the roles, resources, and behavior of federal, state, and local governments, elected officials, health systems, providers, public agencies, and community-based organizations in the context of previous findings. We presented our preliminary findings from archival data for discussion at two national interdisciplinary academic conferences for population health and public policy scholars.
We then refined our data into four themes that describe political determinants of immigrant health: (1) a reactive political environment, (2) decision-making legal ambiguity, (3) passive enforcement of immigration policies, and (4) institutional blame-shifting (see Figure 2). These themes build on and echo earlier foundational work by Hagan and Rodriguez, whose concept of “policies of deterrence” helped expose how exclusionary welfare and immigration policies interact to produce layered vulnerabilities for Hispanic/Latine and migrant communities in Texas and beyond.80,81 The following sections describe each theme, integrating evidence from archival research and interweaving relevant concepts from the policy sciences to advance a critical understanding of the forces that shape high cervical cancer disparities in Tarrant County, Texas. Policy implications and key take-aways of Tarrant County results of the American Cancer Society Cervical Cancer Mortality Disparities in US Hispanic Women Study.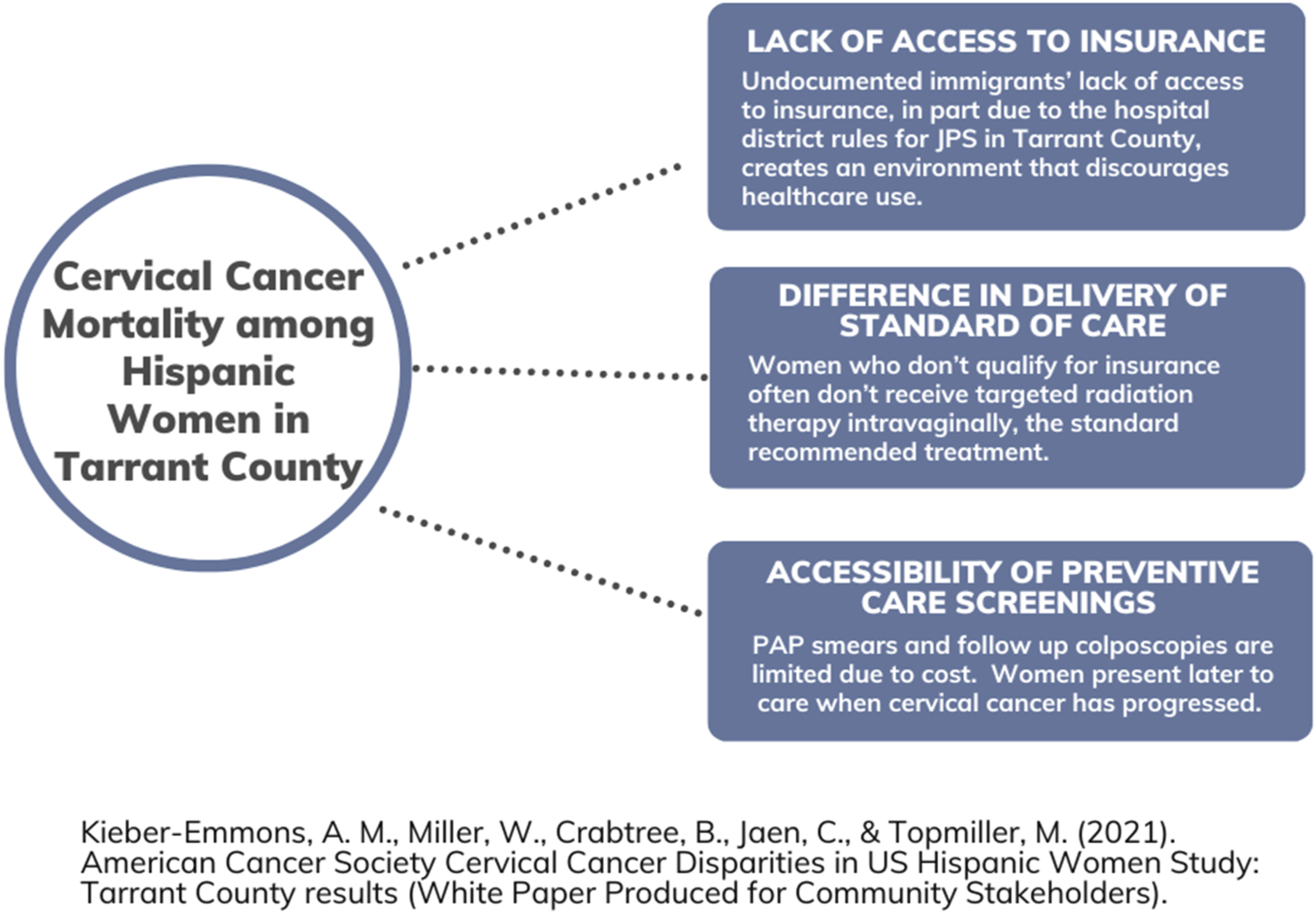
Reactive Political Environment
Tensions over immigration enforcement have long existed between the U.S. federal government and border states like Texas.82,83 This tension escalated in recent years as federal immigration authorities apprehended a record-breaking number of individuals seeking asylum at the US-Mexico border, a common proxy to measure rising rates of undocumented immigration. The COVID-19 pandemic greatly deepened political and economic uncertainty in Latin America, one of the world’s most unequal regions.84,85 Financial insecurity and limited healthcare access contributed to higher infection rates and greater exposure to the COVID-19 virus, 86 political instability, 87 domestic violence, 88 and weakened social protection systems. 89
This policy turbulence is shaped by the United States’ system of federalism, which divides political power between federal and state governments. Gerken discusses the idea of cooperative federalism as one in which states and the federal government both regulate in ways that often overlap. 90 This model, which Gerken dubs the “power of the servant,” rests on the assumption that states draw their power through implementation of federal policy. Cooperative federalism is a helpful lens to understand the structural forces that generate federal and state conflict over immigration enforcement while shaping local political environments. 91
Unlike pre-pandemic migrant flows dominated by immigrants from Mexico and northern Central America, nearly half of recent arrivals are coming from more geographically distant countries such as Venezuela, Cuba, Haiti, and Nicaragua. 92 As a result, recent migrants are less likely to have the resources or connections needed to benefit from sponsorship programs that allow U.S. citizens and permanent residents to sponsor an individual to enter the country as a formal refugee. 93 As the destination for one of the largest immigrant populations in the country, Texas remains one of the most restrictive and reactionary anti-immigrant states, with state leaders frequently contesting federal authority over immigration enforcement. 94
To create a more orderly process, in 2021 the Biden Administration created new immigration enforcement guidelines that prioritized arrests and removals for individuals with particular immigration law violations. 95 This prompted Texas and Louisiana to unsuccessfully file suit against the Biden Administration, claiming that the US government’s “failure to make more arrests or bring more prosecutions” imposed significant costs on state and local governments through their provision of social services and health care for migrants that remain in the US. 96 In December 2023, Governor Greg Abbott signed a bill that allows law enforcement authorities to arrest people for crossing the US-Mexico border without authorization. 97 This law is being actively contested in federal courts at the time of this writing. 98 All trends indicate persons seeking refuge and opportunity in the US will continue to head to top urban destinations, such as the DFW metroplex. Amid unprecedented levels of immigration enforcement that mark the first several months of Trump's second term in office, state officials appear to welcome the opportunity to challenge the previous administration’s decisions before a conservative-leaning Supreme Court. 99
According to Gerken and other scholars, the ability of states to resist or contest federal policies is an important component of cooperative federalism.100,101 In their mission to prevent perceived overreaches by the federal government, state leaders may create an adversarial and even combative environment. This is believed to ensure a balance of power and maintain the stability necessary for cooperation. 102 Cooperative federalism also extends to substate governments, particularly when local officials advance local policies which signal alignment with state and/or federal immigration priorities. 103
Tarrant County is considered the largest Republican stronghold in Texas, a state where no Democrat has been elected to statewide office in 30 years. Local news outlets describe recent changes in county leadership as a transition from one of bipartisan collaboration to the “new front of the culture war.” 104 The reddening of Tarrant County leadership has been accompanied by establishment of the 287(g) program,105,106 a controversial partnership with federal authorities that allows local sheriff’s deputies to function in a similar capacity as agents of U.S. Immigration and Customs Enforcement. 80 This 2017 federal-county partnership was a response to the Trump Administration’s push to expand local immigration enforcement, and Tarrant County is the largest Texas county with an active 287(g) agreement. 81 More recently, in 2022, newly elected county officials established an Election Integrity Task Force to investigate local election complaints. Two years later, county officials have not provided any evidence of punishment that has resulted from its investigations.107,108 These actions fall in line with broader recognition of Tarrant County as a battleground county within the 2024 presidential election. 109
Decision-Making Amid Legal Ambiguity
The Personal Responsibility and Work Opportunity Reconciliation Act (PRWORA) of 1996, intended to reduce incentives for unauthorized immigration, expanded restrictions for federally-funded nonemergency health care services. 110 Under PRWORA, persons lacking US citizenship and those with less than 5 years of lawful permanent residence (LPR) are ineligible for public health insurance programs such as Medicaid, Children’s Health Insurance Program (CHIP), Affordable Care Act (ACA) Marketplace coverage, and Medicare. 111 In line with the logic of cooperative federalism, PRWORA gives states the discretion to use their own funds to extend nonemergency care to certain non-citizens.110,111 Texas—second only to California in total number of persons without lawful authorization— 112 has opted not to extend such coverage, maintaining significant restrictions for both authorized and unauthorized immigrants. 113 By contrast, California has gradually expanded its state-funded Medicaid program to cover all low-income residents regardless of immigration status. 114
However, PRWORA did not specify whether the absence of state legislation prohibited local governments from offering such benefits. This ambiguity led to widespread confusion among Texas counties, especially regarding whether providing locally funded nonemergency care to noncitizens would violate state or federal law. 63 This confusion was compounded by the Emergency Medical Treatment and Labor Act (EMTALA) of 1986, which requires hospitals to provide emergency care regardless of immigration status and ability to pay, but offers only limited reimbursement for uncompensated care. 115 As discussed earlier, while JPS Health Network’s exclusions are not federally mandated, the hospital district has historically aligned its financial assistance policies with restrictive interpretations of federal and state guidelines. This suggests that policy implementation is often guided more by political and legal ambiguity than by statutory obligation.
In Texas, counties are responsible for ensuring healthcare access for medically indigent residents—uninsured individuals who are ineligible for other forms of healthcare assistance. Urban counties typically meet this requirement through public hospital districts. In 2001, Texas Attorney General (AG) John Cornyn issued an opinion that public hospital districts would be violating state and federal law if they provided locally funded nonemergency care to non-citizens otherwise ineligible under PRWORA. 116 Two years later, the state legislature added a statutory provision permitting—but not requiring—local governments to extend such care (Health & Safety Code, Section 285.201).
In January 2004, the JPS Board of Managers voted to provide subsidized nonemergency care to unauthorized immigrants for the first time since PRWORA passage.62,117 In July of the same year, AG Greg Abbott issued a legal opinion affirming that hospital districts were permitted—not obligated—to extend these benefits.
118
In August 2004, the JPS Board reversed course and reinstated its prior policy excluding non-citizens without lawful permanent residency.
117
In 2016, AG Ken Paxton reinforced the authority of restrictive state and federal provisions, interpreting them as justification for maintaining limited access to nonemergency healthcare.
119
These layered legal decisions are visualized in Figure 3 and continue to shape local policies today, 20 years later.
120
Political determinants of immigrant health in an urban county with high cervical cancer disparities among Hispanic women.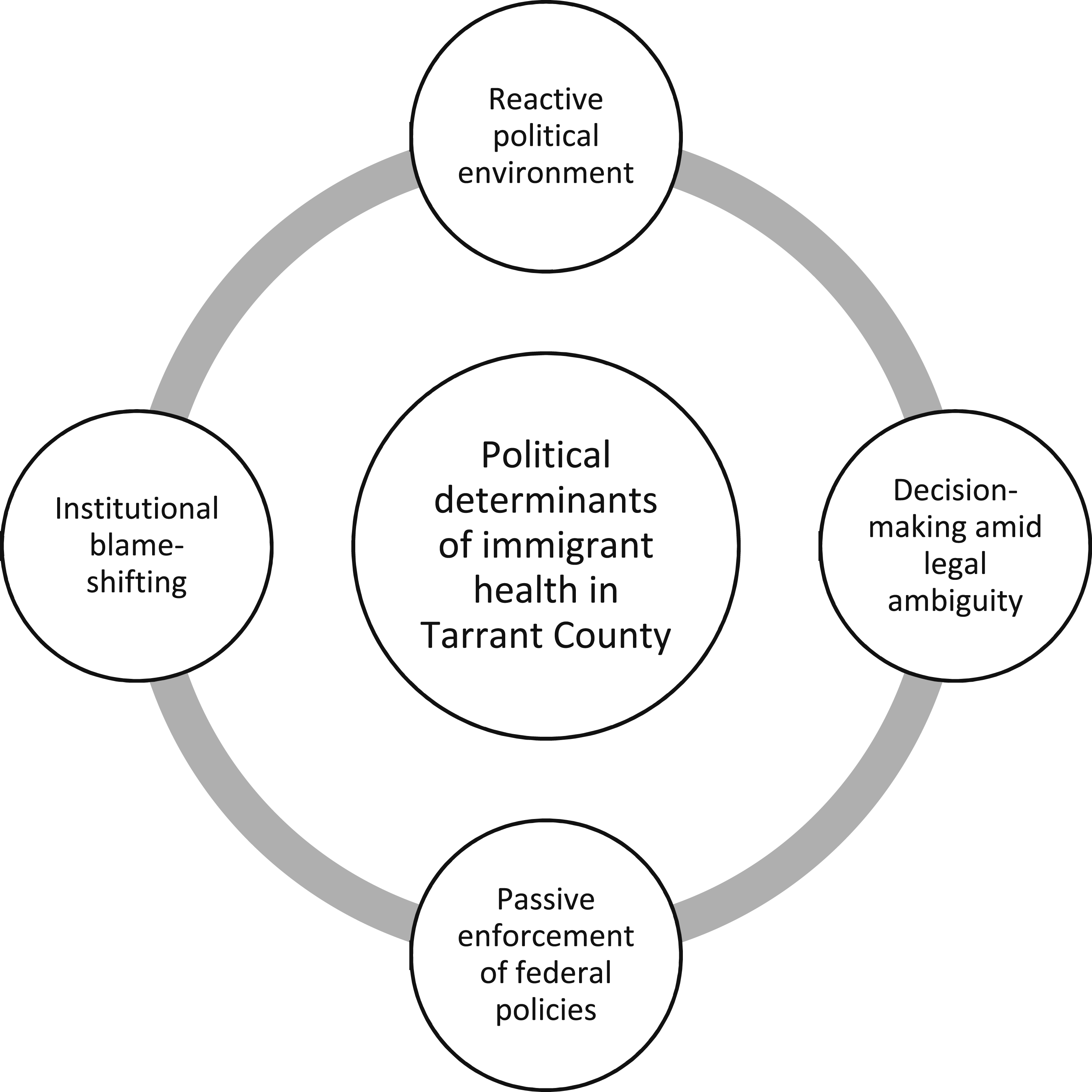
To interpret how these patterns endure, we draw on the multiple streams framework (MSF) of policy analysis, which assumes that policymakers operate under conditions of limited time, information, and political capital. When a policy problem or solution is ambiguous, decision-makers tend to elevate issues that align with their personal ideology, re-election goals, or time constraints (a process called agenda-setting). 121 MSF posits that policy change is most likely during “windows of opportunity” when problem awareness, political will, and feasible solutions converge. 122
Applying MSF to Tarrant County, we interpret restrictive healthcare policies as the product of self-interested decisions made possible by varying definitions of “residency” at different levels of government. At the federal level, residency for non-citizens may refer to visitors, students, business investors, temporary workers, or others with an approved, time-limited purpose for being in the country. Those with lawful permanent residency (green cards) are granted indefinite authorization to establish residence in the US but remain subject to revocation based on legal infractions. 103
Public agencies define residency in ways that reflect their institutional goals. For example, Texas law considers individuals who have lived in the state for at least 30 days to be residents for the purposes of taxation. Local governments and businesses benefit from inclusive definitions of residency, especially when collecting taxes or recruiting a bilingual workforce. In 2001, the Texas legislature even expanded in-state tuition eligibility for students who graduated from a local high school but did not yet possess lawful status under federal law. 123 In June 2025, however, just as this article went to press, this policy was struck down in a strategic alignment of interests between state and federal officials. 124
By contrast, public hospital districts like JPS have drawn on a more restrictive interpretation of residency, limiting access to subsidized healthcare based on immigration status. 63 As MSF suggests, this divergence is not simply legalistic but political. In a hypothetical future where federal funding expanded access to immigrant healthcare, Texas officials could still opt for obstructive implementation. MSF helps explain how institutional actors selectively interpret legal definitions to advance politically expedient goals, especially in conservative states.
These dynamics reflect not only legal ambiguity, but also political ambition. Legal scholars have noted that attorneys general are especially likely to issue partisan legal opinions on controversial topics when doing so aligns with the pursuit of institutional authority.
125
The Texas AG position is a well-known stepping stone to higher office, as evidenced by John Cornyn and Greg Abbott who respectively went on to long-standing roles as Texas governor and US senator. Notably, these legal opinions often align with the broader agenda of state leadership. This observation is further reinforced by the moderating impact of reduced political sensitivity associated with broader electoral bases and longer term lengths of national office. For example, 2 years into his first 6-year term as US senator, John Cornyn indicated his support for more inclusive health care access while speaking about his previously noted 2001 decision as Texas Attorney General: The law was the Texas legislature had not provided for preventive care for undocumented immigrants. And so I did my job at that time as an attorney general - saying what the law was. But, I think as a legislator, now as a senator - I think a better solution is not to deny people access to preventive care when it costs a whole lot more to treat them when they go to the emergency room.
117
(p. 16)
At a county level, the JPS Board of Managers has the authority to modify eligibility guidelines for its charitable financial assistance program, JPS Connections. While state law permits more inclusive policies, the Board is appointed by members of the Tarrant County Commissioner’s Court, who retain the power to remove them. Even though the Board has formal authority to act independently, appointees face strong incentives to align with their Commissioners’ political agendas—particularly in politically conservative settings. As MSF illustrates, even well-intentioned actors may defer to partisan pressures or maintain the status quo rather than risk political backlash.
Passive Enforcement of Federal Policies
Active immigration enforcement occurs through statutory or executive mandates and formal partnerships to implement immigration law. This is carried out by federal, state, and local law enforcement agencies that actively identify non-citizens who have violated criminal or administrative immigration policies. By contrast, passive enforcement occurs through administrative decisions that indirectly limit access to health and social services by narrowly defining eligibility—such as for subsidized cancer treatment or healthcare navigation. These decisions do not directly target immigrants or seek to apprehend or detain non-citizens. Rather, passive enforcement functions as a form of structural violence, withholding basic services and civic rights through implicit deference to federal laws.39,68 A chronology of restrictive hospital district policies in Tarrant County, Texas.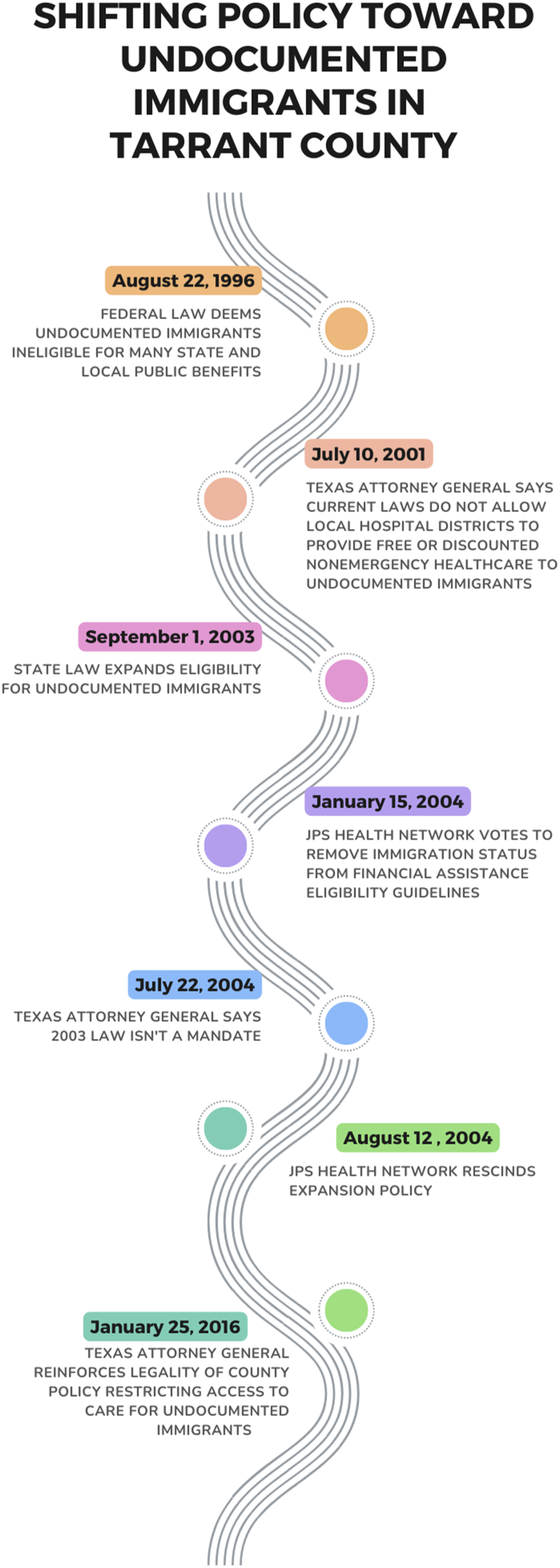
For most of JPS Health Network’s history, Tarrant County officials have limited non-citizen access to locally subsidized healthcare. In the absence of public scrutiny, the rationales and impacts of these policies remain opaque. While not directly engaged in arresting or identifying unauthorized immigrants, the JPS Board of Managers is effectively enforcing federal policies by restricting access to local safety net services for persons lacking federal residency status, even when they meet state or county definitions of residency.
Passive immigration enforcement is further reinforced by structural barriers that limit the capacity of private nonprofit hospitals in Tarrant County to fulfill their statutory mandate to provide “medical care without regard to the beneficiaries’ ability to pay” as outlined in the Texas Tax Code (§ 11.18). Tarrant County is home to several nonprofit hospitals operated by private health systems, which compete with JPS Health Network for privately insured patients. Competition is especially intense in the Dallas-Fort Worth (DFW) metroplex, where local uninsurance rates are the highest in the nation, ranging from 16.8 to 21.4% of the population.126,127
Texas law requires all tax-exempt hospitals to spend at least 5% of their net patient revenue on community benefit activities (Tex. Health & Safety Code § 311.045), which includes uncompensated care. However, providing services for uninsured patients with complex or chronic conditions—such as cervical cancer—can generate substantial unreimbursed costs. This creates tension for nonprofit hospitals that must balance financial viability with legal obligations and ethical standards of care.
In practice, these dynamics often shift the burden of care to JPS. In some cases, private nonprofit hospitals may subtly redirect high-need patients to JPS. In more extreme cases, providers may engage in “medical repatriation,” transferring an immigrant patients to medical facilities in their countries of origin without ensuring they have the means or legal ability to return. 128 While difficult to track, these cases illustrate how health systems may indirectly enforce immigration exclusion through care decisions, further highlighting the structural violence embedded in passive enforcement.
New institutionalism, also known as neo-institutionalism, provides a useful lens for understanding how restrictive hospital policies become established as authoritative guidelines for social behavior. This perspective helps reveal how voters, officials, and institutional actors interpret and reinforce these rules over time. 129 At the intersection of immigration law and health policy, the JPS Health Network has engaged in a form of “boundary work” that establishes who is eligible for care, creating “entry” and “exit” rules that align with broader exclusionary trends. 130 (pp226-227) In the absence of open dialogue or opposing evidence, residents and officials may view the exclusion of non-citizens from subsidized care as fiscally responsible, reinforcing its legitimacy.129,131
The administration of Tarrant County’s 287(g) agreement, a formal partnership between the county and U.S. Immigration and Customs Enforcement (ICE), further illustrates how passive enforcement is embedded in local governance. Through this program, local sheriff’s deputies collaborate with federal immigration agents to identify individuals in custody for potential removal. In the first 4 years of implementation, more than 400 individuals were reported to ICE, resulting in detention, forced removal, or voluntary self-deportation. 132
In 2020, the Tarrant County Commissioner’s Court voted to extend the program’s federal contract indefinitely, which effectively removed it from future agendas and limiting opportunities for public input. 132 Staffing shortages temporarily paused ICE referrals, 133 but public reporting on outcomes such as number and outcomes of ICE encounters remains limited. Even if rarely used, the program contributes to passive enforcement by chilling community engagement with public institutions, including healthcare systems, and suppressing transparency and political contestation. 54
In contrast, some states have adopted laws to ensure transparency and public oversight of immigration enforcement. California passed the Transparent Review of Unjust Transfers and Holds (TRUTH) Act in 2017, requiring local law enforcement to notify immigrants of their rights prior to ICE interviews and mandates annual public forums on program impacts. 134 While such protections are unlikely to be adopted in Texas, they illustrate how policy design can mitigate the chilling effects of immigration enforcement on health access and civic participation while creating a system of checks and balances amid a federalist system of government.135,136
In Tarrant County, however, a lack of transparency further entrenches passive enforcement. Hospital boards are not required to disclose data on immigrant exclusions from financial aid programs or their health outcomes, 137 leaving voters with limited tools to evaluate whether local health systems are fulfilling their mission. A transparency framework—such as reporting the number of patients denied care due to immigration status, the cost of uncompensated care, 138 or instances of medical repatriation 139 —could enable more informed public oversight. These data could also help public health officials and community organizations identify gaps in service delivery, track emerging disparities, and assess the capacity of the safety net to meet the needs of immigrant families.
While the documentation of immigration status is a risky endeavor, posing legal risks for clinicians while exposing patients to potential discrimination, stigmatization, and even deportation, states like Texas and Florida have already made this data collection a requirement.140,141 This reality may present an opportunity to leverage such data for accountability, even while acknowledging the serious concerns surrounding its use. As described in the next section, this lack of transparency also facilitates blame between health systems. Without shared responsibility or clear public metrics, private hospitals may minimize their role in providing safety net services by placing disproportionate pressure on public systems like JPS to absorb the care of politically marginalized populations.
Institutional Blame Shifting
The COVID-19 pandemic underscored how public health crises can rapidly become political crises when outcomes are framed as government failures. 142 Despite significant investments in education and vaccine development, the U.S. pandemic response was weakened by political polarization and public mistrust. These dynamics also affect cervical cancer prevention, where evidence-based strategies may be undermined by institutional inaction or political opposition.
Empirical research on immigrant health disparities is also constrained by evidentiary gaps and political sensitivities. 143 Even rigorous methodologies cannot fully overcome the limitations imposed by reactive political environments. Literature on organizational behavior suggests that institutions frequently delegate decisions to avoid responsibility for negative outcomes. 144 Effective policy analysis in polarized environments must acknowledge this political fragmentation and consider how different types of evidence are used to shift responsibility.
In 2008, a leading executive from the JPS Health Network spoke publicly about the hospital district’s policies.
145
This speech by Robert Earley—a former state legislator who later served a 13-year tenure as hospital CEO—characterized “the undocumented issue” (p. 331) as an emotional and politically-charged arena. In defending JPS’s exclusionary policies, Earley emphasized the institution’s fiscal responsibilities to “legal residents” and suggested that officials were uncomfortable making moral distinctions between patients.
62
This framing reveals how JPS leadership deflected responsibility to state and federal actors, while portraying patients, taxpayers, and even hospital staff as factors in the system’s limited capacity to provide care. Such deflection illustrates a broader pattern of institutional blame shifting that obscures accountability. “I don’t think you should ask the hospital to make moral decisions for the State of Texas or, for that matter, for the United States.”
62
“This is pretty much a federal issue looking for a place to hide.”
145
(p. 335) “It’s hard to deal with those issues because they are emotional issues.”
145
(p. 332) “We are political. It would be naïve and it would be denying the facts to admit that our hospital doesn’t have a strong political element.”
145
(p. 333) “I’ve never met a person that [wanted to pay more taxes]… It’s not going to happen, and it doesn’t happen when it relates to health care either.”
145
(pp. 332-333) “With Parkland [neighboring Dallas County’s public hospital], they are providing that care…They deal with the bills, and…they assume some of those bills and it is very difficult on them. JPS finds itself in another situation.”
145
(p. 333) “Texas should become more involved in federally qualified health centers.”
145
(p. 335) “Increased funding from the level of state government and local government could help.”
145
(p. 335) “There is a reluctance to want to sign up for programs like that for an undocumented population for fear of any retaliation.”
145
(p. 336)
In the absence of coordinated public investment in care for uninsured immigrants, responsibility is often redirected to under-resourced entities. Community stakeholders point to a patchwork of local providers—Tarrant County’s public health department, federally qualified health centers (FQHCs), and charitable community clinics—as fallback resources for immigrant patients. 56 Women without lawful status may be eligible for the state’s Breast and Cervical Cancer Services (BCCS) program, which provides screening and diagnostic services. However, these services are limited in capacity and scope, and undocumented women diagnosed with cancer remain ineligible for the state’s Medicaid for Breast and Cervical Cancer program. 146 This creates significant ethical tensions for providers: promoting screening among uninsured women in a county with limited treatment access may increase diagnosis without viable paths to care. 128
Outside of the JPS system, Tarrant County’s private nonprofit hospitals are required by state law to dedicate at least 5% of gross patient revenue to uncompensated care and community benefit activities. 147 In practice, however, private hospitals may shape policies in ways that minimize their financial exposure and shift the burden of high-cost care to public institutions. 148 As a result, the JPS emergency department has become a default provider of routine and complex care for immigrant patients. 149
The hospital district offers an 80% discount for low-income patients who do not qualify for JPS Connections but lack other forms of health coverage, 120 but this still leaves patients responsible for substantial out-of-pocket costs. For context, the Centers for Disease Control and Prevention (CDC) estimates the first-year cost of cervical cancer treatment is approximately $58,700, with continuing care averaging $4,000 annually—and nearly double that in the year before death. 150 Nonprofit and philanthropic organizations have limited ability to offset these costs, making programmatic triage and financial rationing inevitable.
Healthcare economics applies theories of competition to examine how individuals, providers, and insurers interact to influence access to healthcare. 151 At its core, health insurance serves to manage the burden of uncompensated care by regulating access, discouraging unnecessary services, and providing consistent payment for care. Historically, the US health system has resisted government intervention, with providers and institutions often opposing perceived intrusion. 152 Major policies like the Affordable Care Act (ACA) reflect a compromise, grounded in the belief that market-driven solutions, rather than direct government intervention, can improve access to healthcare while balancing cost control and individual choice. 153
This is evident in the design of ACA health insurance marketplaces and state Medicaid expansions implemented through managed care organizations. While the ACA significantly reduced uninsurance rates nationally, Texas did not expand Medicaid, limiting those gains. 114 Even in expansion states, undocumented immigrants remain ineligible for federal subsidies and Medicaid coverage. 111 As a result, safety net hospitals in immigrant-dense, restrictive states face strong pressures to shift care responsibilities to resource-limited faith-based and community-based organizations. 153
Some counties have developed innovative funding strategies to address this gap. In Travis County, home to the Texas state capitol, the public hospital district does not operate a stand-alone facility. Instead, it distributes funding to a network of hospitals to ensure access across the region. 154 A similar model in Tarrant County could equitably distribute the financial burden of uncompensated care among nonprofit hospitals. This structure would also align with conservative ideals of limited government by separating political actors from direct service delivery. 155 For example, while both school districts and hospital districts in Texas are considered taxing entities, hospital districts fall under the direct control of the County Commissioners Court—narrowing the space for independent administrative decision-making. A distributed funding model could allow physician leaders and hospital administrators more autonomy to establish targeted assistance programs for immigrants ineligible for other forms of coverage.
Discussion
Despite global efforts to reduce cervical cancer incidence, Hispanic women in the US—particularly immigrants—continue to experience disproportionately high mortality rates. While early detection and treatment can drastically improve survival, systemic barriers to care contribute to late-stage diagnoses and preventable deaths. These disparities are especially acute in states with restrictive healthcare policies and anti-immigrant political climates, where access to public health services is systematically constrained.
This article illustrates how structural forces, rather than individual behaviors, shape disparities in cervical cancer outcomes. Exclusionary public healthcare policies exacerbate these disparities by shifting financial burdens onto local safety net hospitals, which often lack the funding or capacity to absorb these costs. Without federal or state support, these institutions must navigate the burden of providing life-saving treatment under politically and fiscally constrained conditions. These patterns reflect broader inequities in the US healthcare system, where uninsured and immigrant populations disproportionately bear the consequences of preventable health crises due to fragmented access to care.
While federal policies set broad parameters for immigrant healthcare access, county-level governance plays a critical role in determining how these policies are implemented. In Tarrant County, restrictive hospital financial assistance policies, local immigration enforcement initiatives, and political resistance to healthcare expansion collectively contribute to persistent disparities in cervical cancer outcomes. These findings illustrate how multilevel governance structures—federal, state, and local—can intersect in ways that amplify exclusion, underscoring the importance of place-based research on the political determinants of health.
While not the central focus of this analysis, the conditions described here echo patterns of structural violence—that is, institutional arrangements that systematically constrain access to health and well-being for marginalized communities. This concept, which has been defined as the “disparity between actual and possible abilities to meet fundamental human needs,” 68 (p. 7) is taken up more explicitly in a companion manuscript which examines how researchers working in restrictive political settings must navigate ethical, methodological, and evidentiary constraints when producing data-driven insights on health inequities. In the present article, we focus on how cervical cancer disparities are often framed in public health discourse as a matter of personal responsibility (i.e., adherence to screening guidelines), yet access to preventive care is fundamentally shaped by policy decisions that either facilitate or obstruct healthcare for marginalized populations. The restrictive policies observed in Tarrant County exemplify how governance structures function as key determinants of immigrant health, shaping both care-seeking behavior and survivorship through multilevel institutional barriers.
As public health officials promote community-based interventions to encourage screening and early detection among Hispanic women, these efforts may cause unintended harm if they increase diagnoses among populations without access to follow-up treatment. 47 This paradox reinforces the limits of behavioral interventions when structural barriers remain unaddressed. It underscores the need for policy-based solutions that confront the systemic conditions—such as exclusionary eligibility criteria, restrictive financial assistance policies, and fragmented safety net systems—that shape access to cervical cancer prevention and care.
A key challenge in understanding and addressing these disparities is the fragmented nature of public health data. Immigration status, which can vary over time—is not collected in national health surveys or cancer registries, 31 requiring researchers to rely on inconsistent methodologies to measure disparities.32–35 This omission reflects broader political debates over immigrant inclusion in public policy and reveals how gaps in health data both reflect and reproduce marginalization. Without reliable data, scholars and policymakers struggle to quantify disparities, evaluate policy impacts, and design targeted interventions. In turn, the absence and uneven quality of immigrant health data limit opportunities for responsive policymaking, further widening the research-to-policy gap. Addressing these gaps is essential for developing evidence-informed policies that promote equitable healthcare access.
While considerable work has examined socioeconomic and cultural determinants of immigrant health, fewer studies have explicitly interrogated how political structures shape access to preventive care and life-saving treatment. 156 There remains a gap in applying conceptual frameworks that systematically analyze the broader governance structures and ideological forces that shape immigrant health inequities over time. This results in a disconnect between research on policy impacts and research on broader structural forces that determine how and why such policies are enacted, implemented, or challenged, limiting public health researchers from forward-looking analyses that anticipate emerging disparities rather than react to them retroactively. By integrating a political determinants of health framework, this study contributes to closing this gap by illustrating how local and state political environments shape health inequities, particularly for immigrant communities navigating restrictive policy landscapes.
Community-based researchers face a wide range of legal and ethical barriers in soliciting primary data and active research participation within immigrant communities.157,158 Scholars often face limited funding opportunities, institutional support, or career incentives to engage in long-term research collaborations that document and measure the extent of health disparities in high-immigrant communities—particularly in regions with restrictive or polarizing health policies where such work may be politically sensitive or carry professional risk.
The structural barriers identified in Tarrant County—such as restrictive healthcare policies, anti-immigrant rhetoric, and politically driven barriers to accessing care—are not unique to this region. Similar exclusionary policies and governance structures in other conservative states that restrict immigrant access to preventive and routine care. For example, both Texas and Florida recently implemented policies requiring that hospitals request patient immigration status. 159 Hospitals are also required to inform patients that their responses will not affect their right to access emergency care under federal law. Previous studies have documented an increase in hospital collaboration with immigration authorities following enactment of restrictive federal immigration policies,80,81 prompting concerns that such policies will lead to avoidance of the healthcare system and significant delays in care-seeking behavior. 159 High uninsurance rates among immigrant persons can also impact the healthcare quality of their US-born children and other groups dependent on local safety net systems, 160 which weakens overall community resilience to respond to and address the long-term impacts of public health emergencies, such as the COVID-19 pandemic. 161
As illustrated in this case study, even when evidence supports effective interventions—such as community health workers or Medicaid expansion—implementation is often constrained by shifting political climates, legal ambiguity, or institutional resistance. This is exacerbated by the absence of reliable immigration-related health data, limitations in the quality of available data, challenges in communicating findings to policy audiences, and ideological barriers to the acceptance of evidence by key decision-makers. These gaps reinforce each other and constrain the development and implementation of timely, evidence-informed health equity interventions.
Public health scholars generally have limited training and preparation for community-based dissemination and policy analysis, and many struggle to communicate their research findings and identify actionable policy levers to reduce health disparities within immigrant communities. 162 In the absence of evidence-informed partnerships between scholars and local policymakers, nonprofit organizations and grassroots collaborations often take it upon themselves to fill the evidentiary gap and advocate for change. However, knowledge produced outside of academic settings is more likely to be contested as biased or unreliable, especially when it is associated with other forms of political activism. 143 These challenges are particularly acute in conservative states like Texas, where the legislative culture is marked by skepticism toward scientific expertise and limited political appetite for structural health reforms. Unlike states such as Massachusetts, where policymakers actively seek academic partnerships to guide immigrant health equity efforts, 163 states like Texas and Florida are shaped by polarized governance structures and ideological resistance to public investment in safety net systems. This climate can severely limit the uptake of research, even when evidence is strong, and reinforces the need for interdisciplinary strategies that consider not only data gaps but also political dynamics that influence policy receptivity.
By situating health disparities within the broader political determinants of health, we argue that this perspective provides a critical and necessary lens for scholars in restrictive policy environments to engage in timely and actionable research on health inequities. Future studies should explore how shifts in political ideology, legislative decision-making, and state-level policy implementation contribute to long-term disparities in immigrant health. Moreover, interdisciplinary collaborations between public health researchers, social scientists, and policymakers can enhance efforts to translate research into equitable policy interventions. As illustrated in this case, cervical cancer disparities persist not only because of political resistance but also due to overlapping gaps that define it as a “wicked problem.”
To move beyond a state of perceived helplessness in addressing structural barriers to immigrant health, we propose that scholars and community stakeholders engage in strategic alliances premised on the notion of immigrant health disparities as a wicked problem. Academic, policy, and political champions of immigrant health can leverage each other’s knowledge and expertise to co-interpret emerging evidence, develop a shared understanding of the local environment, and identify windows of opportunity for change. Building on this review of the political determinants of immigrant health in an urban Texas county, we are actively extending research, policy, and community engagement strategies that can foster a local environment of shared accountability which protects the health of immigrant women and their families. We call for others to join us in developing academic-community partnerships that can work together to lessen the harms of structural barriers to life-saving treatment and prevention care for cervical cancer and other highly curable diseases.
These findings also have broader relevance beyond Tarrant County. The framework we advance—grounded in the political determinants of health and enriched by policy science concepts—can be applied to other conservative or anti-immigrant state contexts where governance structures limit access to health care for marginalized populations. Similar patterns of restrictive Medicaid eligibility, ambiguous hospital district policies, and local enforcement partnerships with federal immigration authorities have been observed in states such as Florida and Georgia.164,165 Moreover, this framework is adaptable to other forms of health inequity beyond cervical cancer. Similar mechanisms of exclusion have been documented in maternal mortality, 166 COVID-19 disparities, 167 and chronic disease management 75 —conditions that, like cervical cancer, are deeply affected by systemic barriers to care. In states that have not expanded Medicaid—many of which are also anti-immigrant—safety net hospitals often absorb the costs of delayed care and preventable complications. 168 These disparities are not isolated but symptomatic of a broader policy landscape that structurally limits health equity for immigrant and marginalized communities. 168 By illuminating how political and institutional forces structure access to care, this conceptual lens can support more anticipatory, equity-oriented policy research across diverse settings.
Health equity refers to a vision of advancing social justice in health by creating the conditions that allow all individuals to attain their full health potential, regardless of their immigration status and eligibility for healthcare coverage.169,170 To align with this vision and avoid unnecessary harm from well-intended public health initiatives, it is essential for health equity scholars to engage in strategic partnerships with local policymakers and community health advocates. Critically, these partnerships must be premised on a sense of shared accountability for navigating the research-to-policy gap of addressing cervical cancer disparities among Hispanic immigrant women. Academic-community partnerships for shared accountability can be formal or informal, as their main objective is to provide a venue for transparent, direct, and clear communication. These mutually beneficial collaborations can involve the exchange of knowledge and insight to navigate the political environment, interpret emerging evidence, and identify windows of opportunity for policy change.
Footnotes
Acknowledgements
Many ideas expressed in this paper draw on decades of insights gained from interactions with community leaders and advocates committed to improving basic health care access in Tarrant County and beyond. We thank the following individuals for their role in establishing partnerships and lending expertise critical to the ideas in this paper: Jose Aguilar, Ann Sutherland, Richard Scotch, Amanda English, Amanda Arizola, Alexis Allison, Autumn Kieber-Emmons, and Willie Lubka.
Author Contributions
M.N., H.P., and J.E. co-led an academic-community partnership through which they conceptualized the ethical framework underlying this paper. M.N. and M.C. developed the conceptual framework to structure these ideas. L.R. provided critical feedback and helped shape the ethical framework and recommendations.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
AI Disclosure Statement
During the revision of this manuscript, the author(s) used OpenAI’s ChatGPT to assist in refining the structure, improving clarity, and enhancing the flow of the text. The AI tool was not used for content generation, data analysis, or conceptual development. After utilizing this tool, the author(s) thoroughly reviewed, edited, and ensured the accuracy and originality of the final manuscript. The author(s) take full responsibility for the content of this publication.
