Abstract
Objective:
The primary objective was to determine age-related changes in perceived nasal resonance of young children with repaired cleft palate with or without cleft lip (CP ± L). A secondary objective was to explore associated changes in vowel segment duration, speaking rate, and fundamental frequency (F0) of the children.
Design:
Prospective, longitudinal observational.
Setting and Participants:
Twenty children with non-syndromic CP ± L followed at 3 facilities.
Materials and Methods:
All participants were audio recorded repeating identical speech samples at 3 time points corresponding to mean ages of 6, 7, and 8 years. Sixty audio files were created with counterbalanced pairs of recordings from the 3 time points. Five blinded speech-language pathologists judged which sample of a pair sounded more nasal.
Main Outcome Measures:
Paired-comparison judgments of nasality at each age; vowel duration, speaking rate, and F0 at each age derived from acoustic analysis.
Results:
Speech samples from the youngest age were judged as more nasal more often than samples from the older ages (P < .001). There were decreases in vowel duration (P = .021) and F0 (P = .006) along with an increase in speaking rate (P < .001) as function of age.
Conclusions:
Children with repaired CP ± L are perceived to be more nasal at younger ages during production of phonetically identical speech samples. Clinicians need to be cognizant of age-related changes in other aspects of speech production that may influence judgments of nasal resonance.
Introduction
Some young children with repaired cleft palate may require additional surgery to correct persisting velopharyngeal inadequacy and hyper nasal resonance. Although estimates vary, approximately 5% to 30% of children will require additional surgery. 1 Often, these surgeries are recommended before the start of school, by 5 or 6 years of age, to eliminate stigma of hypernasality.
Perceptual evaluation is the gold standard for assessing hypernasality of young children with repaired cleft palate.2-4 Given its importance, it is surprising that there is little longitudinal data describing how nasal resonance might change during the early school-age years. Hardin et al 5 retrospectively studied 49 children with repaired cleft palate who were diagnosed with marginal velopharyngeal competency from approximately 4 to 18 years of age. They reported that nasality ratings decreased from age 4 to 10 for a subset of the children who were diagnosed as velopharyngeal competent at their last assessment. Nasality ratings also decreased over time for children who continued to be diagnosed with marginal velopharyngeal competency but ratings appeared to plateau at approximately 7 years of age. This study was limited by its retrospective nature and the use of clinical ratings of hypernasality. Zajac et al 6 retrospectively studied 23 children with repaired CP ± L aged 4 to 7 years across a span of 2 years. Nine adult lay listeners judged perceived hypernasality using direct magnitude estimation procedures. These investigators also reported a decrease in perceived hypernasality as a function of age. Limitations of the study included a brief speech sample consisting of counting and inter-listener reliability that was only fair.
The paucity of longitudinal data describing nasal resonance during the early school-age years is especially concerning given this is a time when other changes are occurring in speech production and vocal tract growth. There are well-known changes in temporal aspects of speech production and vocal fundamental frequency (ie, pitch) with increasing age. Speech segment durations – including vowels that are primarily responsible for hyper nasal resonance – and fundamental frequency decrease with age (see Baken and Orlikoff 7 and Hixon et al 8 for reviews). Anatomically, young children have shorter vocal tracts with the larynx positioned relatively high,9,10 close to the nasopharynx. With increasing age, the larynx lowers and the vocal tract lengthens. Although Vorperian et al 10 reported accelerated growth of these structures between birth and 18 months of age, they also noted “considerable growth after age 6 until they reach their adult mature size” (p. 344). In addition, the adenoids start to involute after reaching maximum size in children at roughly 7 to 8 years of age. 11
How age-related changes in speech production and vocal tract growth may influence the perception of nasal resonance is not clear. Indeed, as reviewed by Jones, 12 the research literature regarding the influence of speech and vocal characteristics on hypernasality is scant, focuses on adults, and is somewhat contradictory. Although reduced speaking rate is commonly believed to result in a decrease in perceived nasality, the available evidence is equivocal. Jones et al. 13 experimentally manipulated word production time in 10 children with inconsistent nasality. They reported that 40% of the children were judged to be less nasal when word production time was decreased. As Jones et al. 13 stated, “Words of longer duration may be perceived as more nasal because nasal sound transmission occurs for a longer time period relative to the same word produced with a shorter duration” (p. 465).
There are also conflicting findings regarding the influence of vocal pitch on perceived nasality. While some studies have shown lower pitch is associated with less nasality,14,15 other studies have shown the converse. 16 It must be emphasized that these studies typically involved adults, not children. Clinically, it is our impression that young children who exhibit high vocal pitch are often perceived as more nasal, especially if they also engage in increased loudness. Given the close proximity of the larynx and nasopharynx in young children, a child who engages in hyper-functional vocal behavior may more readily excite acoustic resonance of the nasal cavity compared to an older child with a lower larynx and normal vocal qualities.
Because perceptual assessment is the gold standard and possible secondary speech surgeries may be considered even in young children who exhibit mild hypernasality, it is critical to determine if perceived nasality may change over time along with concomitant changes in other speech and vocal characteristics. The primary purpose of this prospective study was to determine the effect of age on perceived nasal resonance of young children with repaired cleft palate. A secondary purpose was to explore changes in vowel segment duration, speaking rate, and fundamental frequency of the children.
Methods and Materials
Participants
As part of a larger IRB-approved multi-site study, 20 children (12 males, 8 females) with repaired cleft palate were seen at 3 time points (TP) with mean ages of 6.0 (SD = 0.8), 7.0 (SD = 0.8), and 8.0 (SD = 0.9) years. Ten children had unilateral cleft lip and palate (UCLP), 4 had clefts of the hard and soft palate, and 6 had clefts of the soft palate only. All had a single-stage palate repair by 14 months of age; none had known syndromes, oronasal fistulae, sensorineural hearing loss, or secondary speech surgeries. None of the children had non-oral maladaptive articulations, nasal air emission, or nasal turbulence; some had developmental or phonological errors (eg, gliding). Hypernasality of the children at the first time point ranged from none (normal resonance) to severe. This was determined by consensus agreement of 3 of the investigators (all SLPs) using a five-point ordinal scale of none (0), slight (1), mild (2), moderate (3), and severe (4). This scale is essentially the same as recommended by the Americleft group. 3 Table 1 shows demographic information of the children including initial judgments of hypernasality.
Sex, Cleft Type, Age at First Time Point, and Hypernasality Ratings at First Time Point of the 20 Children.
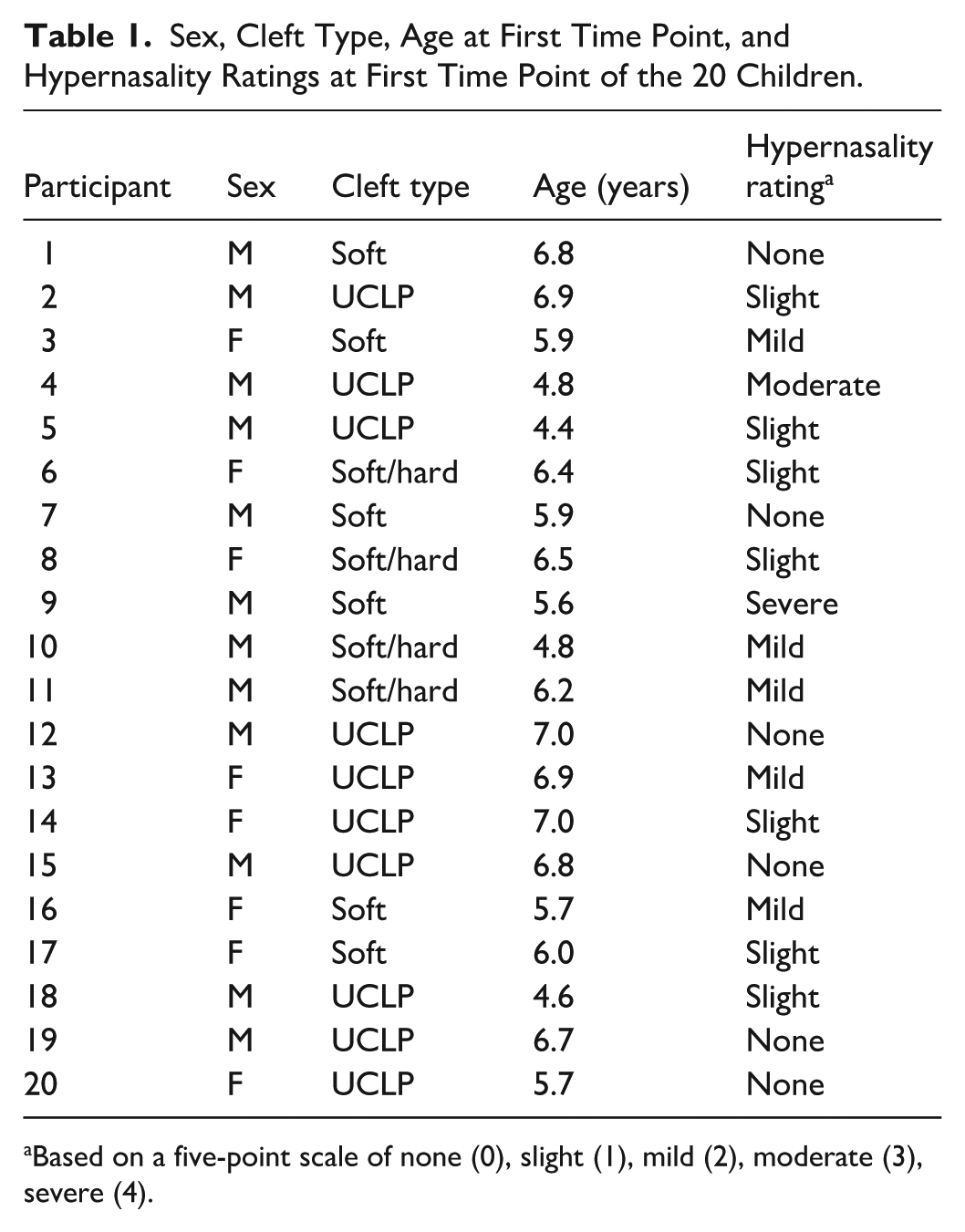
Based on a five-point scale of none (0), slight (1), mild (2), moderate (3), severe (4).
Audio Recordings
At each age, the children were audio recorded with a head-mounted condenser microphone repeating 4 short sentences – buy baby a bib, daddy did it, we are hanging on, we were away. The sentences primarily targeted voiced oral consonants and vowels, both high and low. One sentence included nasal consonants to account for possible assimilative nasality to adjacent vowels. The children were recorded either in a sound-attenuated booth (2 sites) or in a quiet room within an acoustic sound enclosure (1 site). All sites used identical microphones (AKG, model C520) with the audio signal digitized via Computerized Speech Lab (KayPentax, model 4500) at a sampling rate of 44.1 kHz.
Paired-Comparison Listening Task
A paired-comparison task was used to determine perceived nasal resonance as a function of age. Sixty audio files were created with pairs of the 4 sentences: 20 audios had sentences from TP1 paired with TP2, 20 audios had sentences from TP1 paired with TP3, and 20 audios had sentences from TP2 paired with TP3. The order of the time points was counterbalanced within each set of the 20 audio files and the order of the sentences was randomized within each audio file. Loudness of all audio files was normalized to −1 dB using Adobe Audition (version 26.0.0.56). Five SLPs (all females) completed the listening task using an online Qualtrics survey. All had at least 16 years’ experience as an SLP with 3 reporting extensive experience with the craniofacial population. The SLPs were blind to the specific objectives of the study. They were simply told that the purpose was to examine factors influencing the perception of hypernasality. The SLPs were instructed to listen to the 60 randomly presented audio files and judge whether the first or second recording was more nasal (even if slightly) or if both recordings were the same. Ten randomly selected audios were repeated. A value of “1” was assigned to the recording of a pair selected as more nasal; if both recordings were judged the same, then a value of “0.5” was assigned to both recordings. 17
Acoustic Analyses
The sentences from each time point were analyzed using Praat 18 and TF32 19 software to determine vowel segment duration, speaking rate, and fundamental frequency of the children. Each recording was segmented and aligned using Montreal Forced Aligner 20 ; boundaries were hand-corrected where necessary. Vowel durations were measured automatically in Praat using a custom script. 21 Mean F0 was hand-measured using Praat’s voice report feature. Speaking rate was measured in TF32 by determining the duration of each sentence and calculating syllables per second (SPS).
Results
Paired-Comparison Nasality Judgments
Group means of the assigned paired-comparison values for recordings at TP1, TP2, and TP3 were 27.4 (SD = 3.6), 17.5 (SD = 0.9), and 15.1 (SD = 3.0), respectively (Figure 1). Higher values indicate that the time point was selected as “more nasal” more often by the SLPs. The maximum possible score for a time point was 40 (ie, all SLPs selecting that time point as more nasal across all 40 comparisons). Overall, there was a 45% reduction in the metric from TP1 to TP3. Because 6 children were judged to have normal resonance at TP1 by the investigators, we recalculated the metric with these children omitted. A similar decreasing pattern over time occurred with an even greater reduction from TP1 to TP3 of 59%. Including all children, ANOVA showed a significant main effect of time point (P < .001); Bonferroni post hoc tests showed significant differences between TP1 and TP2 (P < .001) and between TP1 and TP3 (P < .001). There were no statistically significant sex differences at any time point.
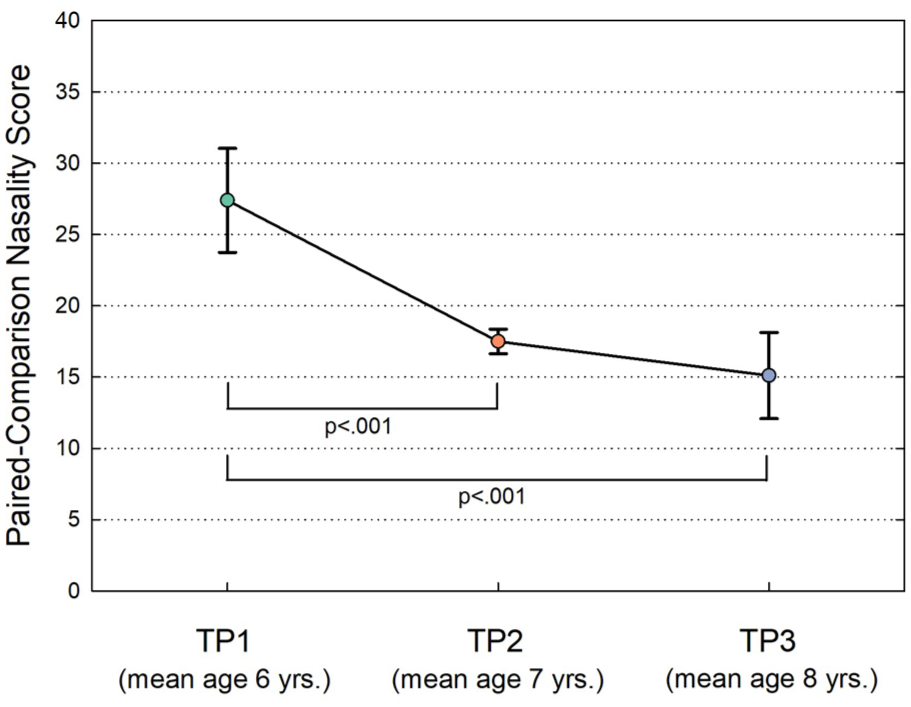
Means and standard deviations (error bars) of paired-comparison nasality judgments of the children at the 3 time points (TP).
Intra-listener reliability was estimated based on the 10 repeated paired comparisons by calculating point-to-point agreements and Kappa statistics for each of the 5 SLPs. Mean agreement was 72%, range 60% to 100%. Mean Kappa was .56, range .32 to 1.00. The range of Kappa values reflects fair to perfect agreement. 22 Inter-listener reliability was estimated by calculating point-to-point agreements and Kappa statistics for each pair of SLPs based on the 60 paired comparisons. Mean agreement was 56%, range 48% to 68%. Mean Kappa was .34, range .23 to .52. This range of Kappa values reflects fair to moderate agreement. 22 The lower inter-listener agreements likely reflect that the SLPs were influenced by different perceptual characteristics such as fundamental frequency as reported below. In addition, the SLPs may have been influenced differently by the developmental articulation errors of some children.
Vowel Segment Duration
Group means of vowel duration for recordings at TP1, TP2, and TP3 were 172 (SD = 20), 166 (SD = 22), and 156 (SD = 19) ms, respectively (Figure 2). The decrease in duration from TP1 to TP3 was 9%. Repeated measures ANOVA showed a significant main effect of time point (P = .021); post hoc Bonferroni tests showed a significant difference between TP1 and TP3 (P = .019). There were no statistically significant sex differences in vowel duration at any time point.
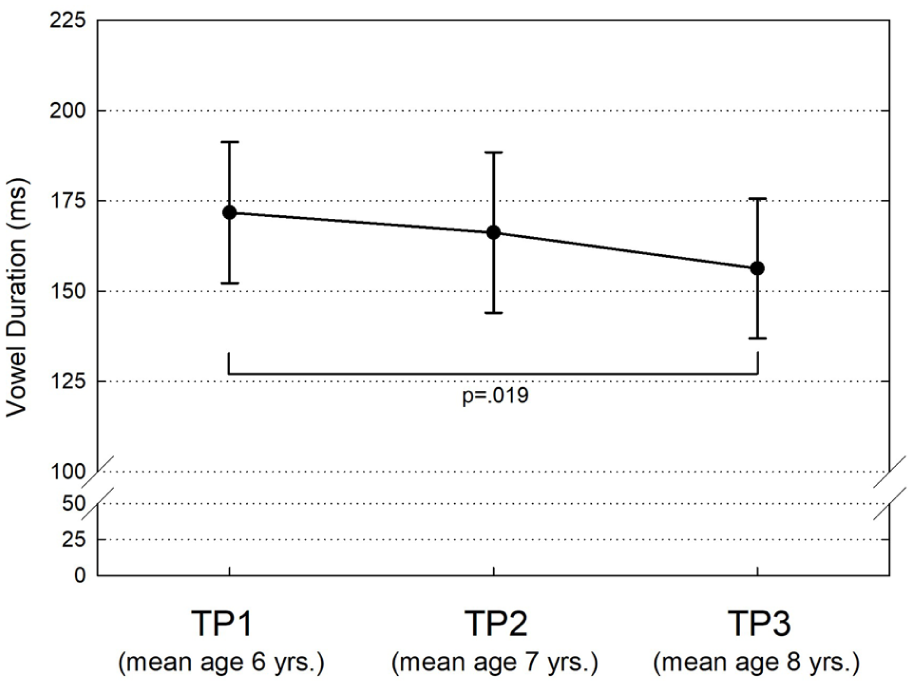
Means and standard deviations (error bars) of vowel segment duration of the children at the 3 time points (TP).
Speaking Rate
Group means of SPS for recordings at TP1, TP2, and TP3 were 3.7 (SD = 0.4), 3.9 (SD = 0.4), and 4.2 (SD = 0.4), respectively (Figure 3). The increase in SPS from TP1 to TP3 was 14%. Repeated measures ANOVA showed a significant main effect of time point (P < .001); post hoc Bonferroni tests showed significant differences between TP1 and TP3 (P < .001) and between TP2 and TP3 (P = .032). There were no statistically significant sex differences in SPS at any time point.
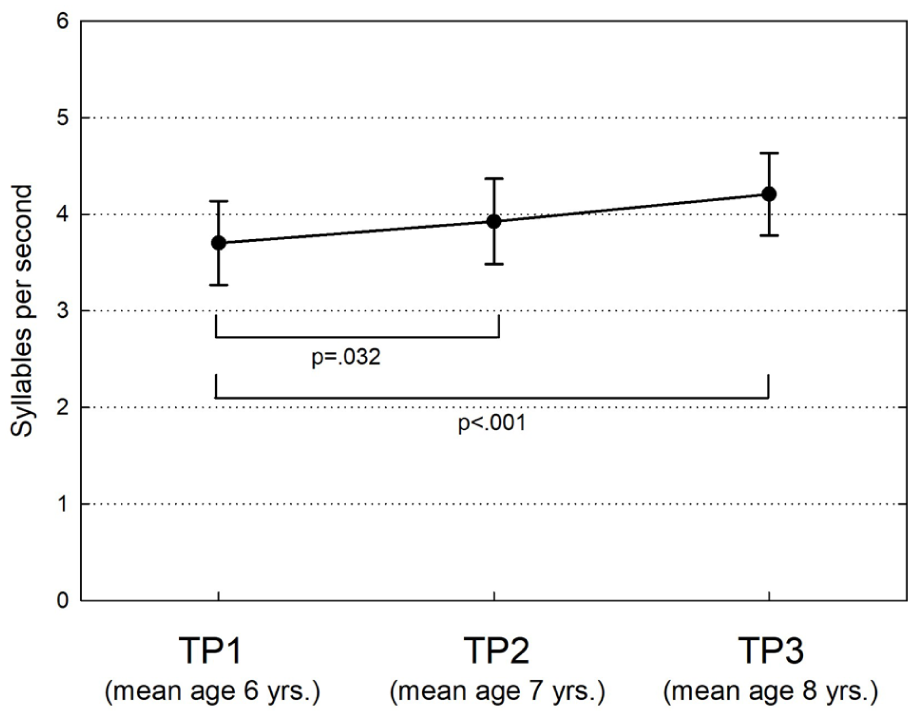
Means and standard deviations (error bars) of speaking rate in syllables per second of the children at the 3 time points.
Fundamental Frequency
Group means of F0 for recordings at TP1, TP2, and TP3 were 246 (SD = 32), 241 (SD = 25), and 226 (SD = 29) Hz, respectively (Figure 4). The decrease in F0 from TP1 to TP3 was 8%. Repeated measures ANOVA showed a significant main effect of time point (P = .006); post hoc Bonferroni tests showed a significant difference between TP1 and TP3 (P = .006). There were no statistically significant sex differences in F0 at any time point.
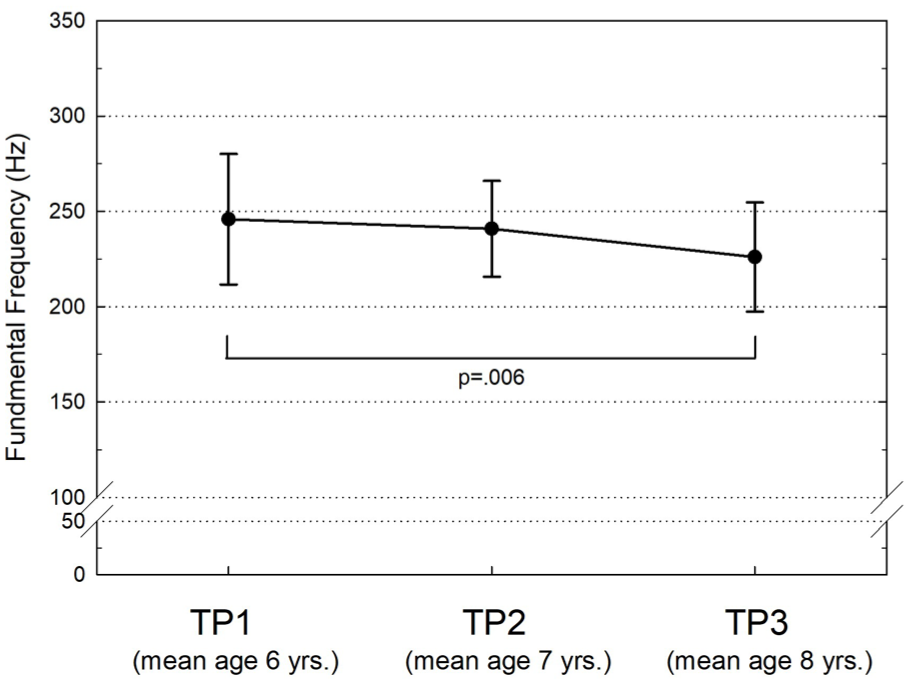
Means and standard deviations (error bars) of fundamental frequency of the children at the 3 time points (TP).
Discussion
The primary purpose of this study was to determine the effects of age on perceived nasal resonance of young children with repaired cleft palate. A secondary purpose was to explore changes in vowel segment duration, speaking rate, and fundamental frequency of the children. Results showed that young children with repaired cleft palate are perceived to be more nasal at younger ages during production of phonetically identical speech samples by experienced SLPs. The findings also showed concomitant changes in speech and voice characteristics as a function of age. Specifically, both vowel segment duration and fundamental frequency decreased with age while speaking rate increased with age. These changes are well known in the literature for typically developing children.7,8 To estimate the degree of influence of the acoustic variables on the findings, we computed Spearman correlation coefficients between perceived hypernasality at the initial time point as judged on an ordinal scale (see Table 1) and the acoustic variables. All correlations were weak, the highest was for fundamental frequency (rs = .254).
Do younger children simply have poorer velopharyngeal closure that may account for the present findings? As part of our larger longitudinal study, we also obtained aerodynamic estimates of velopharyngeal closure during the/p/segment of the word “hamper.” Mean velopharyngeal areas and 95% confidence intervals (in parentheses) were 3.2 (1.4, 5.1), 2.7 (0.9, 4.6), and 2.2 (0.6, 3.7) square mm, respectively, across the 3 time points. Although there was a slight trend of larger areas at the younger ages, a repeated measures ANOVA showed no statistically significant differences. Indeed, at the youngest age, 15 of the 20 children had velopharyngeal areas less than 5 square mm, typically considered adequate; 13 children had areas less than 3 square mm.
Clinical Implications. Normal speech and resonance are goals for the child with repaired cleft palate as he/she begins school. If a child is hyper nasal at this time, parents often pursue additional surgery to improve velopharyngeal function and reduce perceptual stigma. The present findings suggest that a reduction in perceived hypernasality may occur for some young children with repaired cleft palate in as little as 1 year without surgical intervention. Craniofacial clinicians, therefore, need to be cognizant of age-related changes in speech and voice production that may influence perceptual judgments of nasality in young children, especially in cases of mild to moderate hypernasality where a child has higher than expected fundamental frequency. Indeed, it has been our experience that clinicians tend to attribute significant hypernasality to some young children who have high vocal pitch when objective measures (eg, aerodynamics) show adequate or even complete velopharyngeal closure. In such cases, it may be that high vocal pitch in conjunction with a shorter vocal tract acoustically excites nasal resonance and contributes to increased perception of hypernasality.
The present findings suggest a “wait and see” approach may be justified for some young children with repaired cleft palate who exhibit only mild (or even moderate) hypernasality before considering imaging and/or surgical intervention. It must be stressed that a reduction in judgments of hypernasality occurred within a year from the youngest ages of the children (4 -7 years of age) when decisions for additional surgery are typically made. During a “wait and see” period, clinicians can emphasize to parents the need to continue (or begin) speech therapy to address any articulation errors that may be impacting speech intelligibility or acceptability. Finally, the present findings suggest that surgical outcome studies that rely solely on perceptual changes in resonance may conflate surgical improvements with other speech and vocal tract maturational effects, especially at 1-year follow-up times of young children.
Limitations. This study included a relatively small number of children with repaired cleft palate and a small number of SLPs as perceptual judges, with relatively low inter-listener reliability. Because of the longitudinal nature of the study, resonance of some children may have changed over time due to factors such as seasonal allergies. Although none of the children exhibited hypo nasal resonance at TP1, 1 child was judged to be slightly hypo nasal at TP3. This child, however, was omitted when we recalculated the nasality metric as he had normal resonance at TP1. The influence of the acoustic variables on perceived nasality also appears weak. Obviously, additional research is needed to confirm the findings with larger numbers of children and listeners, including listeners with various backgrounds (eg, lay listeners, parents).
Conclusions. This study used a paired-comparison listening task to show that children with repaired cleft palate are judged to be more nasal at younger versus older ages when saying identical speech samples. This happened within a year of the baseline ages of 4 to 7 of the children. In addition, there were commitment changes in vowel segment duration, speaking rate, and fundamental frequency of the children as a function of increasing age. These findings suggest that perceptual judgments of nasal resonance in young children with repaired cleft palate may be influenced by maturational changes in speech and voice characteristics. Future studies should consider comparing children before and after major changes in vocal tract structure (eg, pre-post pubertal growth spurts) and/or through the time course of adenoid involution to examine potential improvements or worsening of nasal resonance at later ages.
Footnotes
Ethical Considerations
Research approved by UNC-CH IRB, Study Number 19-1004.
Consent to Participate
Written parental consent was obtained for all child participants. Online consent was obtained for all adult listeners.
Consent for Publication
All participants consented to be in the study.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Research supported by NIH/NIDCR Grant Number R01DE022566.
Declaration of Conflicting Interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Author David J. Zajac is a member of the Editorial Board of FACE and did not take part in the peer review or decision-making process for this submission.
Data Availability Statement
Data is not available for sharing.
