Abstract
Background:
Facial fractures are common traumatic injuries with variable outcomes due to variations in etiologies, comorbidities, and anatomical complexity. Effective preoperative risk stratification is crucial for identifying patients at higher risk of complications. This study evaluates the utility of the Modified 5-Item Frailty Index (5-mFI) in predicting postoperative outcomes for patients undergoing surgical repair of facial fractures.
Methods:
A retrospective analysis was conducted using American College of Surgeons National Surgical Quality Improvement Program (ACS-NSQIP) data from 2011 to 2021. The 5-mFI score (0-5) was based on hypertension, diabetes, respiratory disease, heart failure, and functional dependence. Patients were stratified into low-risk (5-mFI < 2) and high-risk (5-mFI ≥ 2) groups. Statistical comparisons and multivariable logistic regression were used to evaluate outcomes.
Results:
Of 7549 patients, 6066 (80.4%) were included in the 5-mFI < 2 group and 1483 (19.6%) in the 5-mFI ≥ 2 group. The 5-mFI < 2 group was more functionally independent (99.36% vs 93.46%; P < .001). The 5-mFI ≥ 2 group had increased all-cause complications (28.46% vs 9.33%), wound complications (3.03% vs 1.07%), and readmissions (5.87% vs 2.26%; P < .001). This group encountered higher rates of bleeding (5.53% vs 0.91%) and wound dehiscence (2.09% vs 0.68%). Operative time (164.2 minutes vs 125.8 minutes) and hospital stay (2.49 days vs 1.31 days) were longer (P < .001). Severe complications (1.89% vs 0.21%) and intubation (0.6% vs 0.1%) were higher in the 5-mFI ≥ 2 group. 5-mFI ≥ 2 was associated with hospital stays over 30 days (P = .024).
Conclusion:
5-mFI ≥ 2 patients experience more complications and delayed recovery. Integrating 5-mFI into preoperative assessments may improve patient communication and guide perioperative management.
Introduction
The incidence of facial fractures worldwide was reported between 6 116 489 and 9 493 113 cases in 2017. 1 Facial fractures can arise through numerous mechanisms, including motor vehicle collisions or interpersonal violence, but are most attributable to falls worldwide. 1 These falls are typically associated with an aging population, where ambulation becomes compromised due to decreased muscle strength and impaired proprioception. However, craniofacial injuries such as facial fractures also occur in younger populations who participate in sports.2,3 Most studies identify the mandible (41%-75%) as the most commonly fractured facial bone, with the orbit or maxilla typically reported as the second most frequent, depending on the population studied.4,5
Over the decades, the management of facial fractures has evolved considerably. In the early to mid-20th century, treatment primarily involved closed reduction techniques and maxillomandibular fixation (MMF), commonly known as jaw wiring, to stabilize fractures. 6 However, these methods often led to prolonged immobilization and complications, including malocclusion and temporomandibular disorders. 7 The late 20th century witnessed a paradigm shift with the advent of open reduction and internal fixation (ORIF) techniques, utilizing plates and screws to achieve rigid fixation.8,9 This approach allowed for immediate postoperative mobilization, improved functional outcomes, and reduced complication rates.
Despite advances in craniofacial trauma management, postoperative complications such as surgical site infections, morbidity, and readmissions remain challenging. 10 Preoperative risk stratification is crucial to identifying high-risk patients and guiding clinical decision-making.11,12 Existing tools in predicting adverse outcomes in facial fracture surgery remain limited, particularly in capturing the interplay of comorbidities and physiologic resilience. Frailty reflects the decreased physiological reserve and vulnerability to stressors and has emerged as a predictor of surgical outcomes across specialties. The Modified 5-Item Frailty Index (5-mFI), derived from the American College of Surgeons National Quality Improvement Program (ACS-NSQIP) database, consolidates five comorbidities, including hypertension, diabetes mellitus, chronic obstructive pulmonary disease (COPD), congestive heart failure, and functional dependence, into a validated scoring system. 13 This study evaluates the predictive value of the 5-mFI in patients undergoing surgical repair of facial fractures by utilizing a national cohort to assess the correlation with postoperative complications, readmissions, and resource utilization. By examining the relationship between frailty and craniofacial trauma, we aim to refine preoperative risk assessment, inform patient clinical decision-making, and optimize perioperative management strategies.
Methods
Database and Patient Selection
We retrospectively reviewed de-identified patient data from the American College of Surgeons National Surgical Quality Improvement Program (ACS-NSQIP) database. The information from this database is deidentified and publicly available, deeming it exempt by the Institutional Review Board (IRB). This study examines all cases of facial fractures between 2011 and 2021. Patients were identified using Current Procedural Terminology (CPT) codes corresponding to mandibular fractures and dislocations (21453, 21454, 21461, 21462, 21465, 21470, 21480, 21485, 21490, 21495, 21497), midface fractures (21355, 21356, 21360, 21365, 21366, 21385, 21386, 21387, 21390, 21395), and complex or panfacial fractures (21338, 21339, 21340, 21343, 21344, 21345, 21346, 21347, 21348, 21400, 21401, 21406, 21407, 21408, 21421, 21422, 21423, 21431, 21432, 21433).
Data Cohorts and Analysis
A 5-mFI score was calculated for each patient by assigning 1 point for the presence of any of the following preoperative conditions: respiratory disease, heart failure, diabetes mellitus, hypertension requiring medication, and functional health status. Respiratory disease was defined as a documented history of chronic obstructive pulmonary disease (COPD) or pneumonia within the 30 days preceding surgery. Heart failure was identified if a patient had congestive heart failure within the same 30-day preoperative period. Diabetes status included both insulin-dependent and insulin-independent diabetes mellitus. The NSQIP database categorizes functional health status as independent, partially dependent, or completely dependent. In this analysis, patients classified as partially or completely dependent were grouped together as “Dependent,” while those listed as independent were considered “Not dependent.” The 5-mFI score for each patient was calculated by summing the number of these conditions present, resulting in scores ranging from 0 to 5. Patients were then stratified into 2 frailty risk categories: low-risk (5-mFI < 2) and high-risk (5-mFI ≥ 2). This stratification was based on established methodologies from prior research utilizing 5-mFI as a predictor of postoperative outcomes. Comparative analysis was conducted between these frailty groups, evaluating differences in demographic characteristics, preoperative risk factors, comorbidities, and postoperative complications.
Primary and Secondary Outcomes
The primary outcome of this study was the incidence of wound and systemic complications, while secondary outcomes included reoperation rates, length of hospital stay, and readmission rates.
Statistical Analysis
Descriptive analyses were conducted to compare frailty groups in terms of demographics, preoperative risk factors, comorbidities, and postoperative complications. Continuous variables were analyzed using unpaired t-tests, while categorical variables were assessed using chi-square tests. To evaluate the association between frailty and postoperative outcomes and address confounding, multivariable logistic regression was performed, adjusting for age, gender, body mass index (BMI), American Society of Anesthesiologists (ASA) classification, smoking status, steroid use, bleeding disorders, operative time, and length of hospital stay. A separate multivariate analysis was performed with frailty as a continuous variable ranging from 0 to 5. Additionally, logistic regression was used to analyze the relationship between frailty and specific postoperative complications. A 95% confidence interval was applied, and P-values <.05 were considered statistically significant. All statistical analyses were conducted using IBM SPSS Statistics® Version 28.0.1.0.
Bias Control and Reporting Guidelines
To minimize selection bias, this study included all adult patients identified in the ACS-NSQIP database with CPT codes corresponding to facial fracture procedures from 2011 to 2021. Only cases with complete data for all variables required to calculate the 5-item Modified Frailty Index (5-mFI) were included. Misclassification and information bias were reduced by relying on standardized definitions and coding used within NSQIP, which undergoes regular audits for data reliability. The retrospective nature of the study may introduce inherent biases; however, use of a national dataset and standardized data collection protocols help mitigate these risks.
This manuscript was prepared in accordance with the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) guidelines. A completed STROBE checklist is included as Supplemental Material.
Results
A total of 7549 patients with facial fractures were included in the analysis. Of these, 6066 (80.4%) were classified into the lower frailty group (5-mFI < 2), while 1483 (19.6%) met criteria for higher frailty (5-mFI ≥ 2). The higher frailty group was significantly older (mean age 58.8 vs 35.8 years; P < .001), had a higher BMI (28.5 kg/m2 vs 26.1 kg/m2; P < .001), and included a lower proportion of male patients (64.3% vs 78.2%; P < .001). Racial distribution varied as well, with a greater percentage of Caucasian/White patients in the higher frailty group (64.5% vs 55.3%; P < .001), and a higher proportion of patients in the lower frailty group not reporting race (21.3% vs 12.1%; P < .001). Rates of African American, Asian, and Native Hawaiian or Pacific islander patients were comparable between groups. Demographic and baseline characteristics are summarized in Table 1.
Patient Demographics.
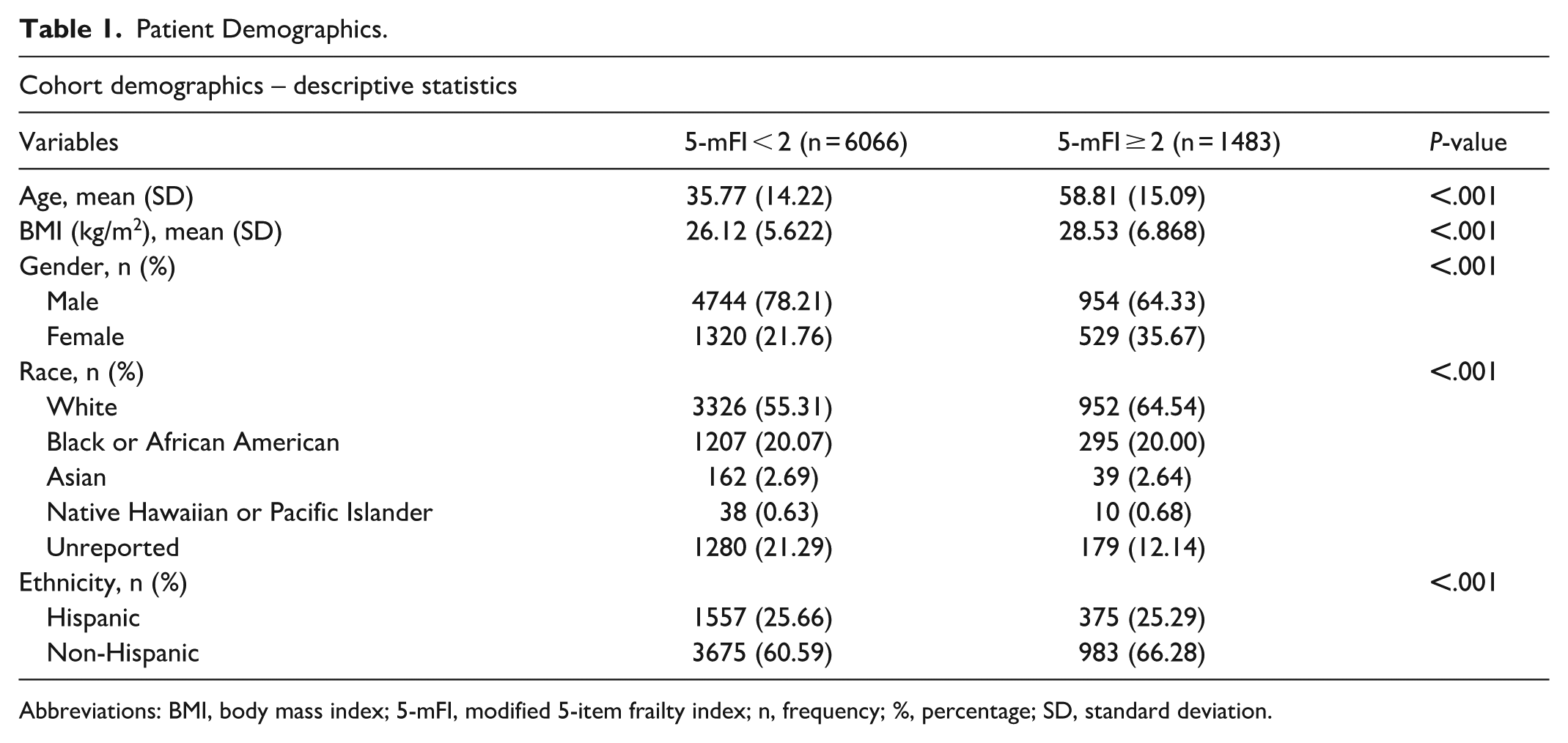
Abbreviations: BMI, body mass index; 5-mFI, modified 5-item frailty index; n, frequency; %, percentage; SD, standard deviation.
Patients with 5-mFI < 2 were significantly more likely to be functionally independent (99.4% vs 93.5%; P < .001), while the 5-mFI ≥ 2 group had greater proportions of partially dependent (4.9%) and totally dependent patients (0.7%). ASA classification differed significantly between groups, with fewer patients in the 5-mFI ≥ 2 group categorized as ASA Class 1 (1.2% vs 27.2%; P < .001) or Class 2 (36.2% vs 59.6%; P < .001), and more classified as ASA Class 3 (57.3% vs 12.7%; P < .001) or Class 4 (5.2% vs 0.4%; P < .001). One patient in the 5-mFI ≥ 2 group was ASA Class 5, compared to none in the 5-mFI < 2 group.
Active smoking was more common in the 5-mFI < 2 group (41.7% vs 31.2%; P < .001). The 5-mFI ≥ 2 group demonstrated significantly higher rates of hypertension (86.7% vs 0%; P < .001), diabetes mellitus (27.6% vs 0%; P < .001), and congestive heart failure (2.1% vs 0%; P < .001). Rates of chronic obstructive pulmonary disease (7.8% vs 0%; P < .001) and ventilator dependence (0.6% vs 0.2%; P = .0065) were also significantly higher in the 5-mFI ≥ 2 group.
Operative and hospitalization metrics differed between groups. Mean operative time was longer in the 5-mFI ≥ 2 group (164.20 ± 180.37 minutes) compared to the 5-mFI < 2 group (125.77 ± 111.83 minutes; P < .001). Mean length of hospital stay was also longer in the 5-mFI ≥ 2 group (2.49 ± 9.43 days) compared to the 5-mFI < 2 group (1.31 ± 4.06 days; P < .001). Preoperative wound infections were more frequent in the 5-mFI ≥ 2 group (1.2% vs 0.7%; P = .028). Group differences in comorbidity status and preoperative risk factors are summarized in Table 2.
Comorbidities and Preoperative Risk Factors.
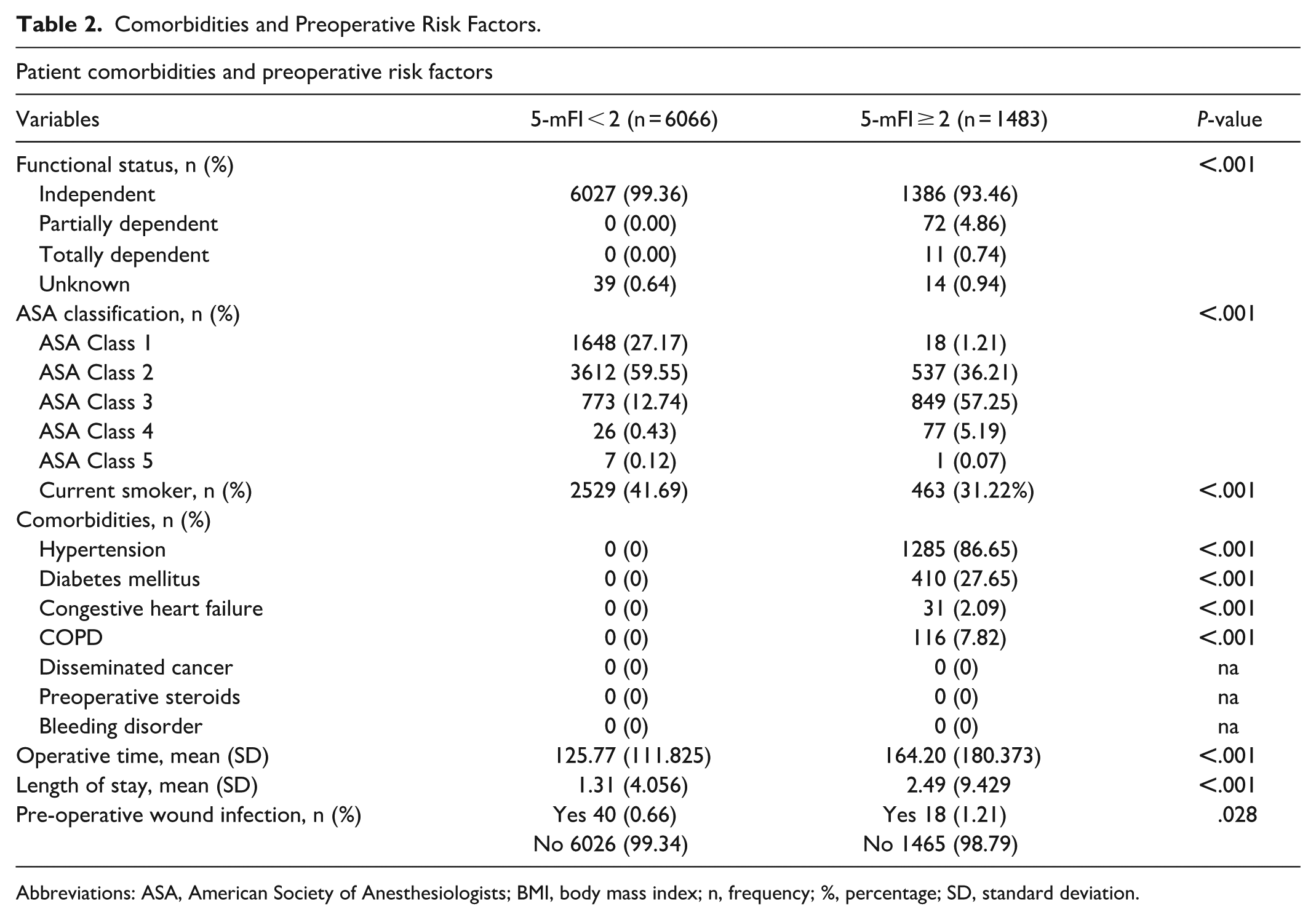
Abbreviations: ASA, American Society of Anesthesiologists; BMI, body mass index; n, frequency; %, percentage; SD, standard deviation.
Postoperative complications were significantly higher in the 5-mFI ≥ 2 group compared to the 5-mFI < 2 group. The overall rate of all-cause complications was higher in the 5-mFI ≥ 2 group (28.46%) than in the 5-mFI < 2 group (9.33%; P < .001). Wound-related complications were also more common in the 5-mFI ≥ 2 group (3.03% vs 1.07%; P < .001), including superficial surgical site infections (0.20% vs 0.03%; P = .023), organ/space infections (0.61% vs 0.25%; P = .027), and wound dehiscence (2.09% vs 0.68%; P < .001). Deep surgical site infections were rare and similar between groups (0.13% vs 0.12%; P = .846).
Mild systemic complications occurred more frequently in patients with 5-mFI ≥ 2 (6.06%) compared to those with 5-mFI < 2 (1.25%; P < .001). Postoperative bleeding was significantly more common in the higher frailty group (5.53% vs 0.91%; P < .001), as was deep vein thrombosis (DVT) requiring therapy (0.40% vs 0.13%; P = .029). Other complications, including pneumonia (0.07% vs 0.03%; P = .551), urinary tract infections (0% vs 0.03%; P = .484), and sepsis (0.07% vs 0.15%; P = .544), were infrequent and not significantly different between groups.
Severe systemic complications were more common in the 5-mFI ≥ 2 group (1.89%) than in the 5-mFI < 2 group (0.21%; P < .001). Unplanned intubation occurred in 0.6% of 5-mFI ≥ 2 patients compared to 0.1% of 5-mFI < 2 patients (P < .001), and prolonged ventilator dependence (>48 hours) occurred in 0.27% of the 5-mFI ≥ 2 group and in none of the 5-mFI < 2 group (P < .001). Pulmonary embolism occurred in 0.27% of the 5-mFI ≥ 2 group and 0.12% of the 5-mFI < 2 group (P = .163). Stroke or cerebrovascular accident occurred only in the 5-mFI ≥ 2 group (0.20%; P < .001). Cardiac complications were also more prevalent among patients with higher frailty. Cardiac arrest occurred in 0.34% of patients with 5-mFI ≥ 2 compared to 0.02% with 5-mFI < 2 (P < .001), and myocardial infarction occurred in 0.20% and 0.02%, respectively (P = .005). No cases of renal failure or septic shock were reported in either group.
Readmission rates were significantly higher in the 5-mFI ≥ 2 group (5.87%) compared to the 5-mFI < 2 group (2.26%; P < .001), as were unplanned readmissions (5.66% vs 1.96%; P < .001). A prolonged hospital stay exceeding 30 days occurred in 0.88% of the 5-mFI ≥ 2 group compared to 0.15% of the 5-mFI < 2 group (P < .001). Return to the operating room was also more frequent among higher frailty patients (5.06% vs 2.42%; P < .001).
On multivariable analysis, after controlling for age, gender, BMI, race, ASA classification, smoking status, preoperative wound infection, steroid use, and operative time, frailty (5-mFI ≥ 2) was not significantly associated with all-cause complications (OR 1.287, P = .110), wound complications (OR 0.821, P = .452), mild systemic complications (OR 0.925, P = .727), pneumonia (OR 2.677, P = .479), postoperative bleeding (OR 0.779, P = .314), pulmonary embolism (OR 2.499, P = .255), unplanned intubation (OR 0.544, P = .548), cardiac arrest (OR 0.569, P = .660), unplanned readmission (OR 0.428, P = .278), or return to the operating room (OR 1.007, P = .975). However, patients with 5-mFI ≥ 2 had significantly higher odds of experiencing a prolonged hospital stay of more than 30 days (OR 0.277, P = .024). These findings are visualized in Table 3.
Postoperative Outcomes in Facial Fractures Cohort.
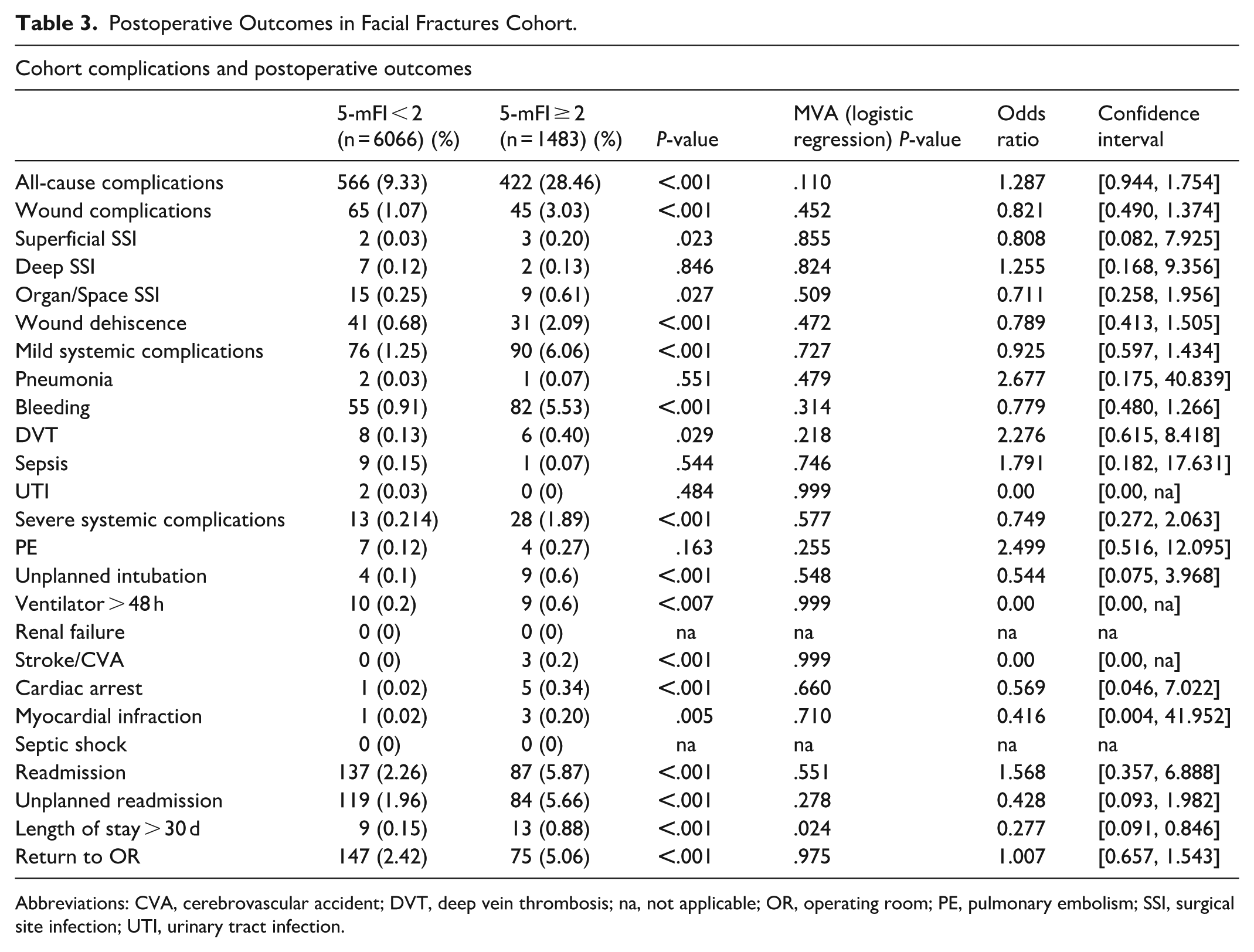
Abbreviations: CVA, cerebrovascular accident; DVT, deep vein thrombosis; na, not applicable; OR, operating room; PE, pulmonary embolism; SSI, surgical site infection; UTI, urinary tract infection.
Facial fractures were further stratified into subtypes by anatomic location and complexity. Among midface fractures, all-cause complications were significantly more common in the 5-mFI ≥ 2 group (5.18% vs 2.73%; P < .01). This disparity was even greater in mandibular fractures, where complication rates nearly tripled (12.05% vs 4.25%; P < .01). Patients with complex/panfacial fractures also showed significantly higher rates of complications (4.60% vs 2.25%; P = .015). Wound-related complications followed a similar pattern. Both midface (0.58% vs 0.11%; P = .033) and mandibular fractures (3.29% vs 1.72%; P = .046) demonstrated higher wound complication rates in patients with 5-mFI ≥ 2. Rates were low overall for panfacial fractures, with no significant difference between 5-mFI < 2 and 5-mFI ≥ 2 groups (0.57% vs 0.35%; P = .342).
Mild systemic complications were notably higher for patients with 5-mFI ≥ 2 undergoing mandibular repair (3.56% vs 0.80%; P < .01). These events were rare in midface and complex fracture groups and occurred only in 5-mFI ≥ 2 patients. Severe systemic complications occurred more frequently in patients with midface fracture repairs in the 5-mFI ≥ 2 group (0.43% vs 0.08%; P = .012). No significant differences were observed for mandibular or panfacial fractures.
Readmissions were higher for patients with 5-mFI ≥ 2 undergoing both midface (8.49% vs 1.63%; P = .011) and mandibular fracture repair (3.17% vs 2.76%; P < .01). Unplanned readmissions demonstrated an even stronger association with frailty in midface (3.02% vs 1.36%; P = .003) and mandibular fractures (8.49% vs 2.44%; P < .01). Rates were higher but not statistically significant in the panfacial fracture repair population. Prolonged length of stay (>30 days) was rare overall, but significantly higher in the mandibular 5-mFI ≥ 2 subgroup (1.10% vs 0.20%; P = .011). Return to the operating room was also more frequent among patients with 5-mFI ≥ 2 undergoing mandibular repair (6.30% vs 2.64%; P < .01), while midface and panfacial repairs did not show significant differences. These findings are visualized below in Table 4.
Postoperative Complications by Anatomic Location and Complexity.
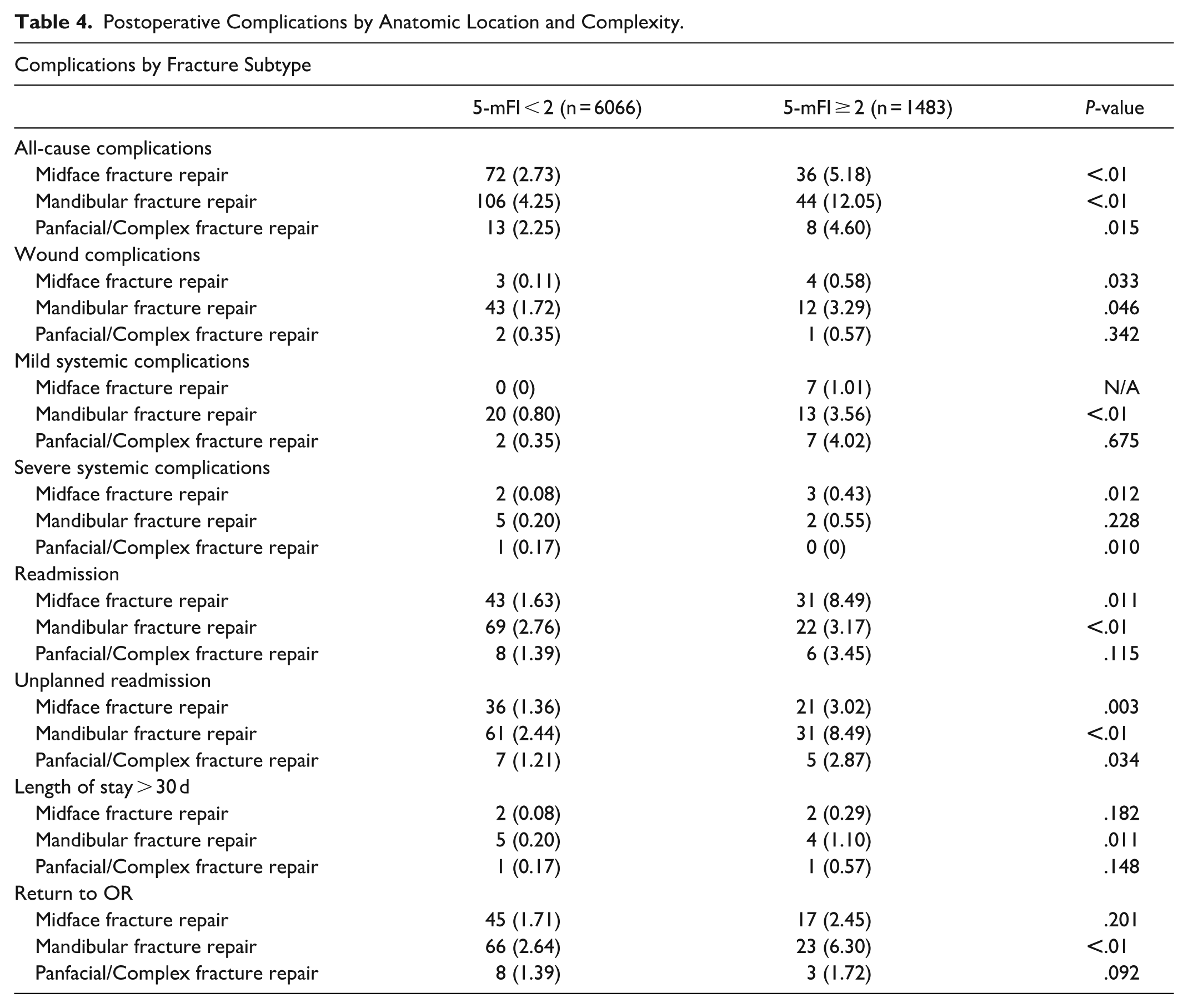
Frailty was evaluated on a continuous scale as well. Multivariate analysis showed that frailty was not independently associated with all-cause complications (P = .214), wound complications (P = .244), mild systemic complications (P = .138), severe systemic complications (P = .703), or return to the operating room (P = .457). However, increased frailty was significantly associated with higher rates of readmission (P = .016), unplanned readmission (P = .008), and prolonged hospital length of stay greater than 30 days (P = .024).
Discussion
In this study, patients with 5-mFI ≥ 2 undergoing surgical repair for facial fractures experienced significantly higher rates of all-cause complications, wound complications, and severe systemic events such as cardiac arrest and unplanned intubation. Additionally, frail patients had longer operative times, extended hospital stays and nearly triple the rate of readmissions. Higher frailty was significantly associated with prolonged hospitalization > 30 days, underscoring its value in anticipating recovery burden and guiding perioperative planning.
The frailty index has been extensively utilized across various medical specialties to assess patients’ vulnerability to adverse post-operative outcomes. In spine surgery, both orthopedic and neurosurgical studies have shown frailty to be a strong predictor of postoperative complications, mortality, and reoperation in patients with traumatic injuries or spinal deformities.14,15 Moreover, frailty assessments have been applied to specific procedures in other fields, such as traumatic brain injury where the 5-mFI demonstrated greater area under the curve (AUC) and had better predictive utility for all outcomes compared to the Charlson Comorbidity Index (CCI). 16 5-mFI has been shown to predict short-term mortality and severe postoperative complications more precisely than the CCI.17,18 5-mFI strongly predicted prolonged hospital stay, nonroutine discharge, and postoperative complications in patients undergoing spinal metastasis surgery, while the CCI specifically predicted postoperative complications only. 19 Studies also suggest that the 5-mFI and mFI-11 have similar prognostic values, indicating that the choice between these indices may depend on specific clinical contexts.18,20
Wound complications are a significant concern following surgical repair of facial fractures. In trauma patients, particularly those with facial fractures, postoperative follow-up rates are often low, and complication rates are disproportionately high. This makes accurate risk stratification especially critical for anticipating adverse outcomes. Patients with 5-mFI ≥ 2 experienced significantly higher rates of superficial SSIs (0.20% vs 0.03%, P = .023), organ/space SSIs (0.61% vs 0.25%, P = .027), and wound dehiscence (2.09% vs 0.68%, P < .001) compared to their 5-mFI < 2 counterparts. Elsayed et al identified a 21.2% complication rate in mandible fracture treatments, with wound dehiscence or SSIs occurring in 12.4% of cases. Factors such as delayed treatment, tobacco use, and dental extractions were associated with increased complications. 21 However, a frailty index was not applied to this patient population. Another study comparing rates of wound complications in obese women undergoing gynecologic surgery reported significantly higher wound complication rates (50% vs 22.4%; RR 2.23, 95% CI 1.29–3.85) in the high frailty group. Frailty remained an independent predictor even after adjustment (aRR 1.88, 95% CI 1.04–3.40). 22 Collectively, these studies demonstrate the importance of patient-specific risk factors, such as frailty in mitigating wound complications following surgery.
Patients with a 5-mFI ≥ 2 demonstrated significantly higher rates of severe systemic complications (1.89% vs 0.21%, P < .001), including unplanned intubation (0.6% vs 0.1%, P < .001), prolonged ventilator dependence (0.27% vs 0%, P < .001), cardiac arrest (0.34% vs 0.02%, P < .001), and myocardial infarction (0.20% vs 0.02%, P = .005), when compared to their less frail counterparts. In general, craniofacial trauma is rarely associated with systemic complications, which occurred less frequently than wound or mild systemic complications. However, studies have previously reported that these complications may arise from delayed surgical intervention and a delayed diagnosis. 23 While frailty has not been previously used in facial fractures, the 5-mFI index has been associated with increased severe systemic complications in upper extremity replantation and revascularization procedures and lower extremity amputations.24,25 The 5-mFI as a predictor of prolonged intubation is particularly insightful as it adds to previous findings that airway edema, blood in the airway, and loss of teeth resulted in difficult airway intubation. Delayed extubation poses significant perioperative risks in these patients, including prolonged ICU stays and ventilator-associated complications. If frailty indices can reliably identify individuals at higher risk for difficult or prolonged intubation, these tools may become instrumental in preoperative counseling and planning—prompting early airway consultation, staged surgical timing, or the use of awake fiberoptic techniques. This suggests that frailty, as a proxy for comorbidity status, impacts success rates in intubating patients as well. 26 These findings suggest that frailty may serve as a valuable early marker for systemic vulnerability, even in surgical domains not traditionally linked to high systemic risk, such as facial trauma.
Readmission rates, length of hospital stay, and return to the operating room (OR) were analyzed as secondary outcomes in this study. Our findings indicate that patients with a 5-mFI ≥ 2 exhibited significantly higher rates of unplanned readmissions (5.66% vs 1.96%, P < .001) and return to the OR (5.06% vs 2.42%, P < .001) compared to their 5-mFI < 2 counterparts. Additionally, prolonged hospital stays beyond 30 days were more frequent in the frail group (0.88% vs 0.15%, P < .001). The 5-mFI has previously shown frailty to be associated with higher readmission and length of stay rates in other surgeries such as resection of NSCLC tumors. 17 These findings may be attributable to the variables measured in the 5-mFI, including impaired cardiopulmonary function, reduced immune responsiveness, and functional dependence, which collectively contribute to delayed wound healing, poor systemic recovery, and increased risk for perioperative complications such as bleeding, infection, and respiratory failure. In turn, postoperative bleeding and infection are important causes of unplanned admissions and returns to the operating room, alongside complications specific to facial fracture hardware such as malunion, nonunion, osteomyelitis, plate exposure, and the need for re-operation. In the context of mandibular fractures, patient comorbidities have previously been identified as independent predictors of higher reoperation and readmission rates. 27 However, a standardized and reliable frailty index has yet to be widely implemented for predicting patient outcomes following facial fractures, highlighting a critical gap in risk assessment and perioperative management.
Of note, the high-risk group exhibited a nearly threefold increase in all-cause complications (28.46% vs 9.33%), demonstrating the holistic impact of diminished physiological reserve on postoperative recovery. This parallels findings in geriatric trauma populations, where frailty indices have been linked to higher morbidity and mortality, independent of injury severity. 28 Interestingly, the multivariable analyses in our study showed that frailty was not predictive of certain complications, such as wound dehiscence or systemic infections, when controlling for age, gender, body mass index (BMI), American Society of Anesthesiologists (ASA) classification, smoking status, steroid use, bleeding disorders, operative time, and length of hospital stay suggesting that confounding variables may mediate these relationships. This contrasts with studies in abdominal and cardiovascular surgery, where frailty indices consistently predicted complications across adjusted multivariate models.29,30 This discrepancy may reflect unique challenges in facial fracture management, such as the interplay between soft tissue injury and comorbid conditions like diabetes or hypertension, which disproportionately impair wound healing in frail patients.
The clinical implications of these findings are twofold. First, integrating the 5-mFI into preoperative workflows could enhance risk communication and informed decision-making, particularly for elderly or comorbid patients. Patients presenting with facial fractures are often polytrauma cases requiring coordination with multiple surgical teams, where prioritization of injuries becomes a clinical necessity. In such complex scenarios, frailty indices like the 5-mFI may serve as valuable tools to guide triage and stratify surgical risk. Second, targeted interventions such as preoperative optimization of glycemic control, smoking cessation, and multidisciplinary rehabilitation may attenuate frailty-associated risks, as demonstrated in elective orthopedic and oncologic surgeries. 14
This study has several limitations. The dataset captures complications and readmissions only within a 30-day postoperative period, limiting insights into long-term complications, functional recovery, and delayed readmissions—key factors in facial fracture management. Additionally, the dataset lacks critical surgical details, including surgeon experience, fracture severity, and specific operative techniques, all of which significantly influence outcomes. Because facial fractures were identified using CPT codes, anatomically and clinically distinct fractures, such as nasal, zygomaticomaxillary complex (ZMC), and mandibular, were bundled together. This could potentially obscure differences in operative complexity, infection risk, and postoperative course. Given that craniofacial trauma often requires complex reconstructive procedures, the absence of granular data on intraoperative variables, such as plating techniques or intraoperative complications, presents a notable limitation. The 5-mFI, while a validated frailty measure, does not encompass other significant predictors of surgical risk, such as nutritional status, cognitive function, and sarcopenia, which may play a critical role in recovery. Furthermore, social determinants of health, including access to specialized care, socioeconomic disparities, and rehabilitation services are not accounted for in the dataset, yet these factors can profoundly impact postoperative outcomes. Future studies should incorporate patient-reported outcomes, extended follow-up data, and more comprehensive frailty assessments to provide a nuanced understanding of long-term recovery and optimize perioperative risk stratification for patients with facial fractures. Despite these limitations, the findings underscore the utility of frailty indices in surgical decision-making, emphasizing the need for multidisciplinary preoperative optimization to improve outcomes in high-risk patients.
Conclusion
The 5-mFI is effective in stratifying risk for patients undergoing facial fracture repair. Patients with higher frailty demonstrated significantly higher rates of systemic complications, wound complications, longer operative times, and extended hospital stays. These findings support the integration of frailty assessments into preoperative planning to enhance risk communication and guide perioperative management.
Supplemental Material
sj-pdf-1-fac-10.1177_27325016261430814 – Supplemental material for Utilizing the Modified Frailty Index to Stratify Risk in Facial Fracture Management
Supplemental material, sj-pdf-1-fac-10.1177_27325016261430814 for Utilizing the Modified Frailty Index to Stratify Risk in Facial Fracture Management by Rohan Mangal, Anshumi Desai, Soumil Prasad, Angela Luo, Kashyap K. Tadisina, Paulo G. Coelho and Lauren M. Yarholar in FACE
Footnotes
Author Note
This work has not been presented at any academic meeting.
Ethical Considerations
Ethical review was waived for this study, as it involved the analysis of fully anonymized and publicly available data.
Consent to Participate
The requirement for informed consent was waived by the Institutional Review Board because this study used the de-identified ACS NSQIP database. The dataset contains no direct patient identifiers, and individual patient consent was not required.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The datasets generated and/or analyzed during the current study are available from the corresponding author on reasonable request.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
