Abstract
Background:
Education about palliative care (PC) is needed at all levels of medical professional development. There is limited literature in Latin America to describe medical students’ level of knowledge about PC and attitudes about the end of life. We assessed the impact of medical student participation in a PC elective rotation during their training.
Methods:
In an observational and cross-sectional study, fifth-year medical students from a public university in Peru completed validated tools in Spanish, including the Palliative Care Knowledge Test questionnaire and the Collett–Lester Fear of Death Scale (score range 1–5). Results were summarized using descriptive statistics and bivariate analysis.
Results:
A total of 128 students participated (corresponding to a response rate of 78%); 81 were male (63.3%) and 47 were female (36.7%); 98 (76.6%) were aged 25 or younger; and 29 (22.7%) had participated in the PC rotation. Knowledge levels about PC were high in 110 participants (85.9%) and intermediate in 18 (14.1%). Knowledge levels were higher among those who participated in the PC rotation (p = 0.011). The mean score for fear of death was 3.19 (SD 0.87), and those who participated in the PC rotation had a higher mean of fear of death (3.48) than those who did not (3.10; p = 0.037), especially in the category of their “own dying process” (p = 0.016).
Conclusions:
Knowledge about PC was higher among medical students who participated in a PC rotation. These students also had a higher fear of death. More research is warranted to address different factors affecting students’ attitudes about death and end-of-life care.
Key Message
Latin American medical students who participated in a palliative care rotation were more knowledgeable about palliative care but had a higher fear of death, indicating that more education is needed to address factors affecting students’ attitudes about death and end-of-life care.
Introduction
The primary mission of palliative care is to improve quality of life and alleviate the suffering associated with advanced diseases, in both patients with the disease and their families and caregivers. Many patients living with serious illness have multidimensional needs, and they often do not receive adequate care, partly because of deficiencies in resources and knowledge of how to approach these challenging conditions.1,2 Due to the current state of the world’s health care system and the inequitable distribution of resources, there is a great need for palliative care.3,4 Therefore, knowledge about palliative care is critical for all health care professionals, throughout their professional life.
Attitudes about facing the end of our own life can vary, and for health care professionals, fear of their own death might impact the effectiveness of their training and approach to the care of patients at the end of life. It is therefore important to consider factors related to clinicians’ own perspectives about death and the end-of-life process from the beginning of their training.1,5,6
Until 2020, few Latin American countries had included specific palliative care courses in undergraduate health sciences programs, and deficient levels of knowledge about palliative care have been reported in these students.7,8 However, students showed a favorable attitude toward receiving palliative care education.9–11 In Peru, medical students were reported to have low to intermediate levels of knowledge about palliative care.12,13 In 2022, upon observing the gap in knowledge about palliative care in undergraduate training, a Peruvian public university created an elective rotation in palliative care for fifth-year medical students. 14 This formal integration of palliative care teaching at the undergraduate level led us to determine the level of knowledge about palliative care in medical students and their attitudes about death, comparing those who participated in the elective rotation with those who did not.
Methods
The research complied with the recommendations of the Helsinki declaration, and approval was obtained from the institutional ethics committee (Act No. 0104-2023 CEI-FM-UNMSM). Informed consent was obtained from the participants, and the data were anonymized to preserve their confidentiality.
We conducted an observational, cross-sectional study of 164 fifth-year medical students from a Peruvian public university between July and August 2023. All enrolled students who gave informed consent were included, and we excluded those who declined to participate or had another previous health-related profession.
The palliative care elective was a 16-week rotation structured around both didactic and practical components. The weekly schedule consisted of a one-hour virtual class dedicated to the principles of palliative care and symptom management. The students also had two hours of in-person practical activities, including supervised visits to hospital units and interviews with patients and their families/caregivers. Additionally, students participated in group workshops covering communication techniques and symptom management. The rotation was an official part of the students’ curriculum and featured an evaluation process based on a set of pre-established competencies.
To assess the level of knowledge, we administered the Spanish version of the Palliative Care Knowledge Test (PCKT) questionnaire, which comprises 31 questions spanning five dimensions (generalities, ethics, spirituality, symptoms, and opioid management). Responses showing 13 or fewer correct answers are considered low level of knowledge, 14–21 correct answers are considered intermediate knowledge, and 22–31 correct answers are considered high level of knowledge. This tool was validated in Peru12,13 with acceptable reliability (Kuder Richardson—20: 0.640).
To assess attitudes about the end of life, we evaluated fear of death using the Spanish version of the Collett-Lester Fear of Death Scale. This scale was validated in Mexico, 9 and it consists of four dimensions (one’s own death, one’s own dying process, death of other people, and dying process of other people), assigning values using a Likert scale ranging from 1 (low fear) to 5 (high fear). The Collett–Lester Fear of Death Scale (in Spanish) has shown excellent reliability (Cronbach’s alpha 0.959).
We conducted a virtual survey using an electronic form containing both the PCKT and the Collett–Lester Fear of Death Scale. The data were coded and tabulated in Microsoft Office Excel 2020. Descriptive statistics, including proportions, frequencies, measures of central tendency, and dispersion, were used to summarize results, according to the nature of the variable. The type of distribution was determined using graphical methods and the Kolmogorov–Smirnov test. Parametric and nonparametric tests and 95% confidence intervals were applied to compare scores (overall and subsets of scores, by category of knowledge on PCKT and for each dimension assessed in the Collett-Lester Fear of Death Scale) between those who participated in the palliative care elective rotation and those who did not, and p < 0.05 was considered a statistically significant difference. SPSS version 27 was used for all statistical analyses.
Results
A total of 128 students participated, yielding a response rate of 78.0%. No participants dropped out of the study or had any previous experience in a health profession. Among the 128 participants, 29 (22.7%) had participated in the palliative care elective rotation. Demographically, 81 (63.3%) participants were male and 47 (36.7%) were female. 98 (76.6%) students were 20–25 years old, 28 (21.9%) were 26–30 years old, and 2 (1.6%) were older than 36 years. Responses showed that 39.4% of participants reported a preference for clinical medical areas, 4% had previously taken a palliative care course, and 26.3% had delayed courses since beginning their studies at the university (Table 1).
Characteristics of Fifth-Year Medical Students at a Peruvian Public University According to Their Participation in a Palliative Care Course 2023

PC, palliative care.
Chi square.
The level of palliative care knowledge was high in 110 participants (85.9%) and intermediate in 18 (14.1%), with a median PCKT score of 23 (mean 23.35, SD 2.229, IQR 3), presenting a nonnormal distribution (Kolmogorov–Smirnov test, p < 0.001; Fig. 1). The level of knowledge was higher among those who had participated in the palliative care elective rotation (median PCKT score 24 compared with 23, p = 0.011, Mann–Whitney U test; Fig. 2). PCKT scores indicating knowledge of symptoms in palliative care were significantly higher among those who participated in the rotation (p = 0.005; Fig. 3).

Distribution of Palliative Care Knowledge Test (PCKT) scores showing level of knowledge about palliative care among fifth-year medical students at a Peruvian public university in 2023 (scores can range from 0 to 31; <13 = low knowledge level, 14–21 = intermediate knowledge level, and 22–31 = high knowledge level).
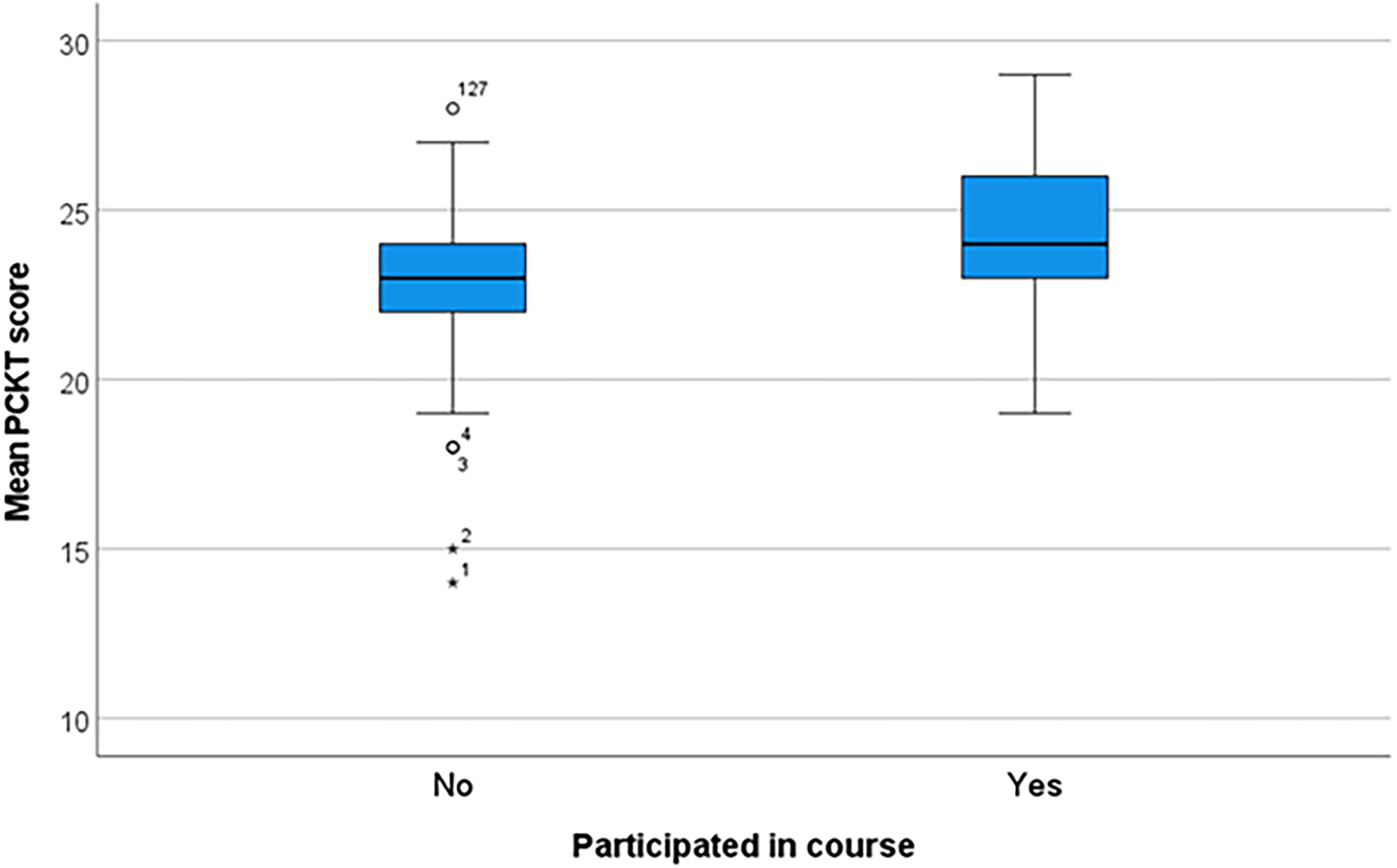
Level of knowledge about palliative care (Palliative Care Knowledge Test [PCKT] scores) in fifth-year medical students at a Peruvian public university in 2023, grouped by participation in the palliative care elective rotation.

Categories of knowledge about palliative care (Palliative Care Knowledge Test [PCKT] scores, by topic) in fifth-year medical students at a Peruvian public university in 2023, grouped by participation in the palliative care elective rotation.
Scores obtained from the Fear of Death Scale had a normal distribution in our cohort (p = 0.200; Fig. 4). The mean score was 3.19 (SD 0.87), with a higher score observed in the group that took the palliative care elective rotation (3.48 vs. 3.10, p = 0.037, Student t test; Fig. 5). Scores within the dimension of one’s own dying process were significantly higher among those who participated in the palliative care elective rotation (p = 0.016; Fig. 6).

Distribution of Collett–Lester Fear of Death Scale scores in fifth-year medical students at a Peruvian public university in 2023.

Collett–Lester Fear of Death Scale scores in fifth-year medical students at a Peruvian public university in 2023, grouped by participation in the palliative care elective rotation. Circle indicates mild outliers.

Dimensions of fear of death (Collett–Lester Fear of Death Scale scores, by dimension) in fifth-year medical students at a Peruvian public university in 2023, grouped by participation in the palliative care elective rotation.
Discussion
The present study highlights the impact of incorporating palliative care training into the undergraduate medical education of students at a Peruvian public university, showing that students’ theoretical knowledge was improved and their awareness of challenging situations related to end-of-life care was enhanced.
Previous research in Latin America showed that undergraduate students believe palliative care should be a mandatory part of their medical training. 11 The present study showed a high level of basic knowledge about general palliative care in medical students who received formal training, as evaluated by a validated tool, and the level of knowledge in this group was higher than that reported in previous studies conducted at the local and regional level.6,13,15,16 This is likely related to increased training in palliative care in educational and clinical environments or outside of the university environment in the region. 17 More research is needed to evaluate the impact of various factors influencing knowledge about palliative care, including the use of various tools to assess this knowledge 18 and prior implementation of palliative care in different settings.
In our evaluation of specific categories of knowledge about palliative care, we found that students who participated in the palliative care elective rotation had better knowledge of distressing symptoms than did those who did not participate in the rotation. This is most likely due to the curative approach of conventional medical training, which often overlooks distressing symptoms, especially those other than pain that can contribute substantially to the suffering of the patient and their family. Students who did not participate in the palliative care elective rotation also might not have had clinical experience with the complexity of symptoms at the end of life. Our findings also highlight a greater knowledge of opioid use in our cohort than that reported in previous cohorts. 19 Palliative care training addresses end-of-life issues in more detail than other medical training, and students who did not participate in the palliative care elective rotation were not exposed to this information.
Fear of death is an important factor in health care professionals’ approach to palliative care. Death is a natural part of the human life cycle, and historically, end-of-life care preceding death occurred in private settings. However, in recent decades, scientific advances in medicine have led to most deaths occurring in hospitals, where clinicians are focused on preventing or delaying death. 4 The COVID-19 pandemic had high mortality rates that could not be prevented by medical practice, and this resulted in fear and distress in those who interacted with the health care system, especially among health care personnel. 20 Fear is a natural reaction to the unknown that enhances alertness and prepares people to respond, but when left unchecked, fear can become detrimental. Moderate and progressive anxiety has been reported in medical students as they pursue their professional careers, with no variation by gender, and a high level of anxiety about death was associated with a higher rate of depression and distress in this population. 21
In the context of a palliative care course integrated into professional training, the level of fear of death identified in the present study was similar to that reported in a previous study in Mexico,22,23 showing higher fear of death among students who participated in a palliative care course. A high level of fear of death was also reported in nursing students in Chile 5 and health sciences students in Spain. 24 More research is needed to evaluate different cultural aspects influencing the fear of death in clinicians. Measures should also be taken to work on attitudes and skills in medical students to allow adequate adaptation and learn to better manage their own attitudes, resulting in better treatment and a better experience for patients and their caregivers. 25
In our analysis of the different dimensions of fear of death assessed in the Collett–Lester Fear of Death scale, we observed a significantly higher fear of one’s own dying process among those who participated in the palliative care elective rotation, but no difference in the other dimensions (one’s own death or the death or dying process of others). These findings differ from those reported in nursing students in Chile, who expressed a greater fear of the death of others than of their own death.5,24 Fear of the dying process involves fear of pain, suffering, physical dependence, cognitive impairment, and uncertainty. Due to the limitations of our study, we cannot determine the probable causes or related factors associated with the fear of the dying process among students participating in the palliative care rotation. Further research is needed to explore the complex emotions, as well as the spiritual and existential aspects related to this fear. Additionally, future studies should investigate how various elements learned during the rotation might impact a student’s emotional and spiritual well-being and their perspectives on death. These reported variations in the different dimensions of fear of death suggest that educational strategies should focus on mitigating the fear of the dying process that comes with learning about it.
Limitations
The present study provides an overview of the knowledge and attitudes of a group of medical students in the intermediate stage of professional training. This study has several limitations, including its cross-sectional design, which prevents the inference of causality between students’ emotions and perceptions. The design also limits the ability to report on the longitudinal experiences of students during their palliative care rotation and after medical school. Additionally, the students may have had personal or uncontrolled biases when electing the rotation, which could have influenced their perspectives on the experience and their personal views on death. Further studies are needed to evaluate the influence of Palliative Care rotation on the different students’ emotions, perspectives, knowledge, and other aspects of their lives. Participants provided voluntary anonymous responses focused on specific aspects of their level of knowledge as evaluated by an instrument with low demand, but that has been validated at both the local and international level. Fear of death was assessed using a validated Likert-scale instrument, which requires further in-depth analysis. Although these results cannot be generalized to all populations of medical students, they highlight aspects of palliative care training that have not been extensively investigated in this population and can serve as a basis for more targeted future research.
Conclusions
We found that medical students who participated in an elective rotation on palliative care had a high level of knowledge on the subject, and exposure to the topic affected their attitudes about the end of life, specifically, a higher fear of death. These findings indicate that education in palliative care is needed and that future educational offerings should include a focus on attitudes about death and the dying process.
Authors’ Contributions
J.A.T. made conception and design of the work, analysis, interpretation of data, and wrote the main article text. J.P.S. contribute to conception of the work and interpretation of data. K.E.C. contribute to conception of the work and interpretation of data. R.V.A. contribute to conception of the work and interpretation of data. C.P.A. contribute to conception of the work and interpretation of data. R.A.D.C. contribute to conception of the work and interpretation of data; V.G.C. contribute to conception of the work and interpretation of data; T.O.E. contribute to conception of the work and interpretation of data; M.D.G. contribute to conception of the work and supervised data interpretation. All authors reviewed, approved, and accept responsibility for this article.
Footnotes
Acknowledgments
The authors thank Erica Goodoff, Senior Scientific Editor in the Research Medical Library at The University of Texas MD Anderson Cancer Center, for editing this article.
Funding Information
This research was funded by the Universidad Nacional Mayor de San Marcos (RR No. 006081–2023-R/UNMSM with project code A23010411).
Disclosure Statement
The authors have no potential conflicts of interest to disclose.
