Abstract
Background:
Anxiety during pregnancy is a prevalent but underemphasized mental health concern with downstream impacts on the entire family unit. Quality social support is strongly related to mental well-being and provides a promising strategy to prevent and manage prenatal anxiety.
Methods:
This convergent mixed-methods study used a cross-sectional survey and interviews to: (1) Quantitatively investigate what adverse social determinants of health and multi-level sources of social support are most predictive of prenatal anxiety and (2) Qualitatively examine different types of social support that may buffer prenatal anxiety among a sample of pregnant women experiencing socioeconomic disadvantage.
Results:
Hierarchical linear regressions revealed that race and food insecurity were predictive of prenatal anxiety and that social support from friends/peers was most protective against prenatal anxiety. Integration of quantitative survey data and qualitative interview data suggested that emotional support was most protective among this sample of pregnant women.
Discussion:
The results of this study highlight opportunities for adaptations of prenatal peer support programs to include a focus on mitigating food insecurity and promoting emotional support from peers in order to most effectively buffer prenatal anxiety among underresourced pregnant women.
Prenatal anxiety is an often-overlooked public health concern with lasting effects on the health and well-being of families. 1 Approximately 20% of prenatal individuals meet the clinical criteria for anxiety, 2 and the adverse impacts are not isolated to pregnancy. Prenatal anxiety has been associated with increased risk of poor physical and mental health outcomes for the mother and baby (i.e., preeclampsia, hemorrhage, fetal death, preterm birth, or a low birthweight). 3 The multigenerational impacts of prenatal anxiety extend beyond birth experience, negatively affecting the development of the child4,5 and health care costs for the family.6,7 One study on the economic burden of perinatal mood and anxiety disorders (PMADs) from conception to 5 years postpartum estimated that untreated PMADs can cost a mother-child dyad more than $30,000. 7
Because both biological and social determinants of health contribute to the risk and severity of mental health challenges, 8 prenatal anxiety disproportionately impacts women of low socioeconomic status (SES).8,9 Unmet psychological needs and systemic inequities such as insufficient access to quality health care, food insecurity, housing- and transportation-related strain, and discrimination influence this disparity.10,11 Given that individuals of low SES with prenatal anxiety are more likely to deliver preterm and have adverse prenatal health outcomes,8,12 there is a need for effective interventions to buffer associations between adverse social determinants of health (e.g., food insecurity, poverty) and prenatal anxiety in low-income populations. 13 Thus far, literature on the prevalence and treatment of prenatal anxiety is insufficient, with most focusing on prenatal depression or grouping depression and anxiety together as prenatal mood and anxiety disorders.9,13,14 The prevalence and far-reaching effects of prenatal anxiety and the disproportionate impact on vulnerable communities emphasize the critical importance of identifying tailored evidence-based strategies to prevent and treat this mental health disorder.12,15
Social support provides a promising strategy to prevent and manage prenatal anxiety due to its strong connection to improved psychological health. 16 It is well established that appropriate social support is associated with lower anxiety and depression.17–19 In prenatal individuals specifically, perceived social support has been shown to predict prenatal anxiety, possibly due to its ability to mitigate stress.20,21 Similarly, lack of social support is associated with increased risk of prenatal anxiety. 22 In those with low social support, prenatal stress was shown to increase poorer infant temperament, 23 which could further contribute to anxiety risk. In contrast, ample social support and social networks are associated with better labor and infant health outcomes (i.e., babies with higher Apgar scores and birth weight). 24 There is a lack of evidence around the types and sources of social support that are most protective against prenatal anxiety specifically.16,22 To effectively leverage social support as a prevention strategy for prenatal anxiety, more research is needed to understand the specific types and sources of social support that are most protective for low-SES prenatal women.16,20,21
The connection between social support and anxiety in low-income prenatal populations can be explained in part by the stress-buffering model, which posits that social support provides emotional, informational, or tangible resources to help individuals cope with stress and reduce its psychological impacts. 25 Emotional support involves perceptions of empathy and reassurance, fostering a sense of belonging and connection. Informational support provides advice and guidance to inform decision-making and help individuals navigate stressors. Tangible support includes material assistance to alleviate stressors, such as financial resources. 25 Thus far, most of the research with the buffering model has focused on non-prenatal populations, 26 and the evidence on functional aspects of social support and prenatal anxiety is mixed. For instance, informational and emotional support from health professionals have both been shown to protect against prenatal anxiety, 22 but there is also some evidence to support tangible resources, such as financial assistance and help with childcare, as critical for prenatal health outcomes. 24 The application of the stress-buffering model may help to elucidate both the external sources of stress as well as how types and sources of social support may buffer prenatal anxiety among low-SES women.
Additionally, consideration of how social support may operate at multiple levels of influence could inform promising preventative strategies to mitigate prenatal mental health disparities. The socio-ecological model is a systems-level framework that describes how health and behavior are shaped by the dynamic interactions across the individual-, interpersonal-, organizational-, community- and policy-levels. 27 When considering prenatal anxiety, a multi-level approach can capture how personal factors (i.e., knowledge, attitudes, self-efficacy) interact with social relationships, organizational settings, and community norms to shape behaviors and outcomes.28,29 Existing literature supports that family and partner social support is especially protective for depression and anxiety.15,17,30 Poor-quality partner relationships are an established risk factor for prenatal anxiety. 31 Outside of familial support, support from other mothers has also been shown to buffer against prenatal anxiety. 22 Additionally, perceived social support from health care providers is a predictor of prenatal depression, but there is a lack of evidence on its relationship to prenatal anxiety. 22 Though existing literature highlights the value of social support for mitigating risk, particularly within socioeconomically disadvantaged communities,9,32 evidence around what specific types and sources of social support are most protective for this population is lacking.
Further investigation is needed to understand how adverse social determinants of health are contributing to the disproportionate prenatal anxiety rates in low-income communities. 33 Identifying protective factors for prenatal anxiety can inform effective prevention and treatment and mitigate the host of associated negative outcomes. 14 To address these gaps, the following convergent parallel mixed-methods study seeks to answer the following questions: (1) What specific social determinants are most predictive of prenatal anxiety? (2) What multilevel sources of social support (family/friend/significant other, community/neighborhood) are most protective against prenatal anxiety? and (3) What types of social support (emotional, informational, and tangible) help to mitigate anxiety among this sample of prenatal individuals?
Methods
Participants
All procedures were approved by the Colorado Multiple Institutional Review Board (IRB #: 22-1725). This study is a part of a larger longitudinal mixed-methods study examining perinatal anxiety, well-being, and biopsychosocial mechanisms to inform a nature-based therapeutic program. Pregnant individuals in the United States were recruited using non-probability purposive sampling techniques between June of 2023 and September of 2024 from two sources: (1) two targeted health care clinics in Colorado and 2) Prolific Academic. Eligibility criteria were: (1) >6 weeks pregnant, (2) at least 18 years of age, (3) english-speaking, and (4) experiencing socioeconomic disadvantage. Participants were classified as experiencing socioeconomic disadvantage if they endorsed low-income status (defined in one of five ways: Medicaid recipient, participation in federal assistance programs, household income <250% Federal Poverty Line, no- or partial-insurance, subjective experience of high financial stress), if they endorsed low educational attainment (less than a college degree), or if they endorsed both factors. There were no exclusion criteria. Prolific Academic is an online research platform that provides the recruitment and management of participants for online research. The platform provides high-quality data collection and is used by researchers globally to recruit diverse and representative samples. Prolific Academic recruited a representative sample of pregnant women across the United States. 34 Of the full sample, 55% were recruited from Colorado clinics, and 45% were recruited from Prolific. Demographic differences between the samples were explored; only education was statistically significant, with the Prolific sample reporting higher education than the Colorado sample.
Procedures
The study consent and surveys were administered via Research Electronic Data Capture (REDCap). 35 REDCap is a secure, web-based application designed to support data capture for research studies. Individuals were asked to complete up to four surveys across the prenatal period: (1) first or second trimester, (2) third trimester, (3) 6 weeks postpartum, (4) 12 weeks postpartum. Each survey took approximately 20 minutes to complete, and participants received a $20 electronic gift card for each survey completion. The second timepoint for analyses in the present study, as social support in the 3rd trimester has been identified as critical to protect against postpartum mood and anxiety disorders.36,37
The qualitative data were obtained from a subset of survey participants from clinics in Colorado who indicated interest in participating in an interview. Convenience sampling was used to recruit participants via email or phone. Semi-structured interviews were conducted over Zoom or phone based on preference and lasted 30–60 minutes. The qualitative interview guide was based on the self-determination theory framework and included questions about psychological-, social-, and community-level resources that promote mental well-being. Questions explored how these multilevel resources may protect against perinatal anxiety. An example question was: “What types of supports have helped you thus far and how have they helped you in your pregnancy?” Please see the Supplementary Appendix for more details on the interview guide. Participants received a $20 electronic gift card sent via email after the interview was completed.
Instruments
The 125-item survey used at each timepoint assessed sociodemographic factors and social determinants of health (e.g., food insecurity, unmet basic needs), prenatal mental health outcomes (e.g., anxiety), and types and sources of psychosocial resources (i.e., self-efficacy, optimism, social support) using validated instruments. Sociodemographic characteristics were operationalized via the following variables: age (continuous), ethnicity (non-Hispanic vs. Hispanic), race (White, Black or African American, American Indian or Alaskan Native, Asian or Pacific Islander, or other), highest level of education (some high school, completed high school, associate’s degree, some college, completed college, and beyond college), and total household income (continuous). Food insecurity was operationalized via 2 one-item yes(1)/no(0) questions: (1) During the last 12 months, did you ever eat less than you felt you should because there wasn’t enough money to buy food? and (2) Within the past 12 months, the food you bought just didn’t last and you didn’t have money to get more. Unmet basic needs were evaluated via a one-item question with eight response options and a check all that apply option: In the past year, have you or any family members you live with been unable to get any of the following when it was really needed? Example responses include clothing, utilities, childcare, and medicine.
The primary outcome investigated in this study was assessed using the generalized anxiety disorder (GAD)-7 scale, which is a 7-item reliable brief measure of anxiety (α = 0.89) (Spitzer et al., 2006). Anxiety was assessed as a continuous variable for all analyses. Sources of social support were assessed via the Multidimensional Scale of Perceived Social Support (MSPSS). This MSPSS is a 12-item scale that measures three sources of social support (friends/peers, family, significant other) on a 7-point Likert scale (1 = very strongly disagree, 7 = very strongly agree). The tool shows an internal consistency of 0.90–0.94 in a prenatal sample. 38 A sample item is “I get the emotional help & support I need from my family.” 38
Quantitative data analysis
To explore the primary research question, all quantitative variables of interest were examined for missing data and multivariate outliers. Percent missingness ranged from 0% to 14.9%; however, Little’s Missing Completely At Random test 39 provided evidence that data were missing completely at random (X2(214) = 242.65, p = .09), so the full information maximum likelihood estimator was used to account for all available data. First, we exported data from REDCap to SPSS Software Version 29.0 40 and investigated univariate distributions (means, standard deviations, and graphical displays), bivariate associations between all key continuous variables, and assumptions of normality, linearity, and homoskedasticity between all key variables. 41 We conducted hierarchical linear regression modeling to explore our first two research questions. First, sociodemographic characteristics and social determinants of health were added to the model to predict anxiety (continuous). Next, sources of social support (e.g., family, friends/peers, significant other) were added to block 2 and community/neighborhood support was added to block 3. R2 and adjusted R2 values, and corresponding p-values for each block are presented, as well as parameter estimates, standard errors, and p-values for the final model. Alpha (α) was set at 0.05.
Qualitative data analysis
Qualitative data were analyzed using a phenomenological approach to explore pregnant participants’ lived experiences. Thematic analysis was used to systematically group the data and identify key themes and patterns. Inductive and deductive coding strategies were used; inductive coding captured novel themes in the data, and deductive coding captured social support based on the MSPSS and established types of social support (emotional, informational, and tangible). The data were further iteratively explored to shed insight into the types and sources of social support that helped participants cope with stress and anxiety during pregnancy.
Results
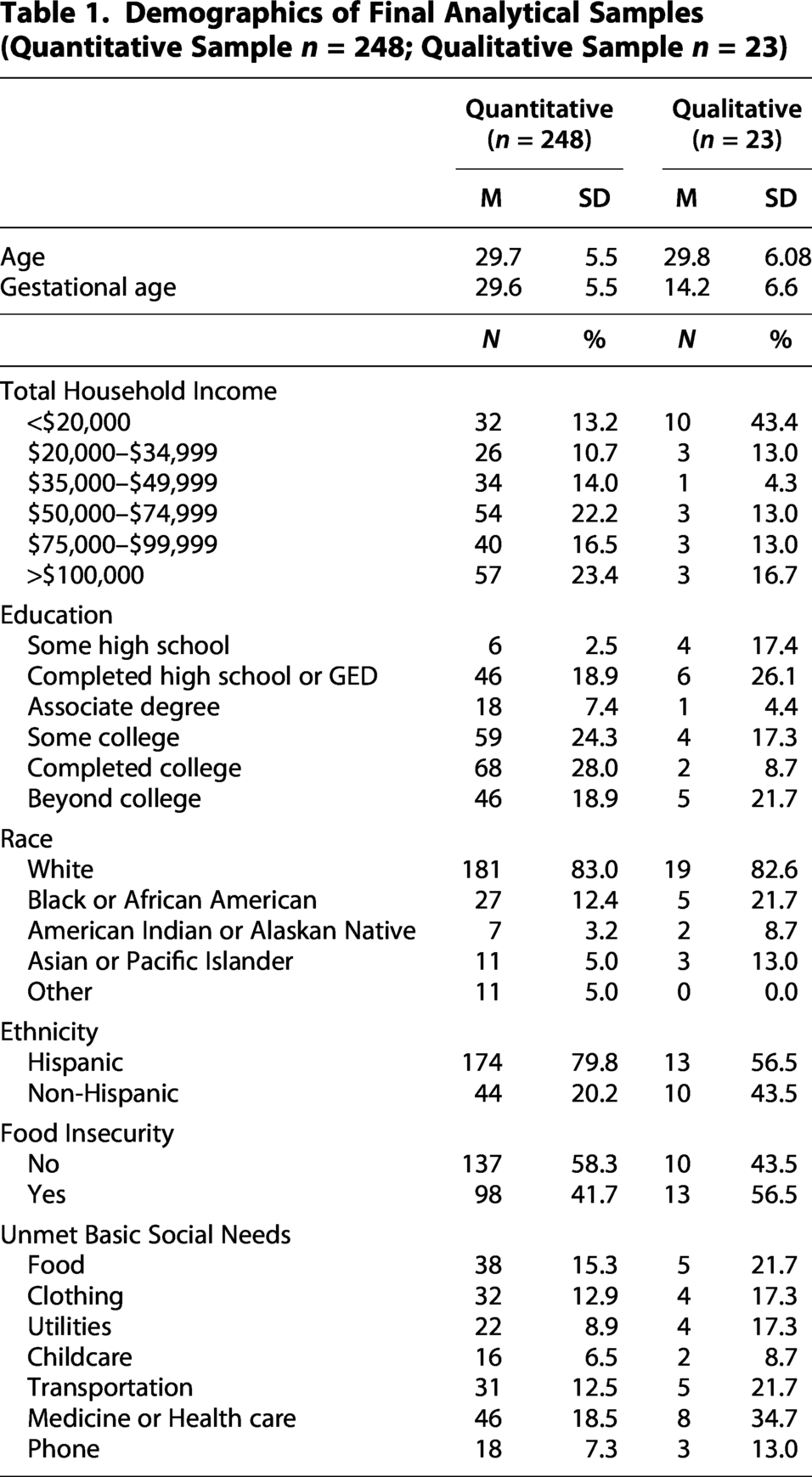
The demographics of the final quantitative and qualitative samples (n = 248 and n = 23, respectively) can be seen in Table 1. Approximately 24% of the quantitative sample reported a total household income level that was below the federal poverty level, while about half made between $35,000 and $99,999 per year. Note that participants only had to endorse one indicator of low-SES to be included in the study. About half of the sample (52%) did not have a college degree; 23% had completed college, and 19% had gone on to additional education after college. Most of the sample (83%) were White, 12% were Black or African American, 5% were Asian or Pacific Islander, 3% were American Indian or Alaskan Native, and 5% reported “other.” The majority of participants were Hispanic (80%), and the food insecurity rate across the sample was about 42%. The most prevalent unmet social need was health care, with nearly 20% of the sample reporting inadequate access to health care.
Demographics of Final Analytical Samples (Quantitative Sample n = 248; Qualitative Sample n = 23)
Results from the hierarchical linear regression models examined the relationship between sources of social support and prenatal anxiety after controlling for sociodemographic factors and social determinants of health (Table 2). The final model presents the results of a hierarchical linear regression model of sociodemographic factors (Block 1: r2 = .13, F(8, 187) = 4.71, p < .001), social determinants of health (Block 2: r2 = .19, F(11, 184) = 5.19, p < .001), and sources of social support (Block 3: r2 = .19, F(12, 183) = 4.70, p < .001) predicting prenatal anxiety. In the final model (see Block 3), race and friend support were significant, with food insecurity approaching significance (p = .07). Being White was associated with higher levels of anxiety (p < .01). After controlling for sociodemographic factors and social determinants of health, social support from friends was significantly and negatively associated with anxiety (β = −.66, p < .01).
Hierarchical Linear Regression Models of Social Determinants of Health and Sources of Social Support Predicting Anxiety among a Sample of Pregnant Women (n = 248)

p < 05.
Ref, reference category.
Qualitative results
The qualitative data provided in-depth insights into how social support empowered participants to successfully navigate the stressors of pregnancy. Pregnant women identified emotional, informational, and tangible resources that help them navigate stressors and anxiety during pregnancy (see Table 3).
Types of Social Support Experienced by Pregnant Women Based on the Stress-Buffering Model (Cohen and Wills, 1985) (n = 23)

Emotional support
Emotional support was the most salient type of support based on both frequency and pertinence in the data. Quality time with partners, family, and friends/peers helped to mitigate stressors and support participant well-being. Individuals in this sample reported that knowing someone was there for them was valuable to prevent emotional distress. One participant described it this way: “My support system like my whole family has been amazing and it makes me so happy to feel so loved like that. It has been one of my really big things.”
Emotional support from spouses and families emerged most often, though friend/peer support was instrumental in fostering an active social life, a sense of social connectedness, mitigating loneliness, and encouraging participants to get out of the house: “I have a friend. we go out to eat here and there and that’s fun too because like it gets lonely. so it’s nice having somebody else to talk to other than your mom and your sibling.”
The insights from this sample demonstrated how emotional support served to validate, encourage, and comfort pregnant participants and could translate to reduced risk of anxiety: “I’d say on the easier side, mainly because of the support that I have, so I have a really good community of women around me and encourage me and tell me I’m gonna be okay and say you’re enough.”
Informational support
Participants were less likely to reference informational support, such as advice or guidance, as a type of support that mitigated anxiety. That does not diminish the importance of education and accurate information related to the prenatal experience among this sample of pregnant women; many participants expressed a need for more informational support outside of what they currently had access to: “Apps like, like pregnancy apps. They were talking about like gestational diabetes. And so I was like reading into that and it’s like, you know, what helped me because like the doctors, they just told me like, oh, you gotta come in and do this. They didn’t really explain to me like what it was or why it was caused.”
For mothers who had already had a baby, this need extended to a desire for information around what to expect during pregnancy and postpartum: “When I felt a little down, I was like, it must be the baby blues. But when you’re sleep deprived, you’re not remembering how long those are supposed to last or not last or any of that information. I feel like more conversation around that or even discussing like is there a program available through the hospital or somewhere else to have those conversations.”
Common resources for informational support were therapists and social media. Those who had met with a therapist felt it was critically protective to their mental health. Outside of therapy, social media emerged as an easily accessible avenue for pregnant women to feel seen in their experiences and help to mitigate stress: “I know this is going to sound really weird, but I think social media actually…like hearing other moms and some of their struggles and how they overcame those struggles… like you understand there are other people going through the same thing as you and helps you feel better.”
Tangible support
Tangible support, commonly in the form of financial assistance or help with childcare, was less prevalent in the data. When asked about financial support, some participants emphasized the emotional comfort of knowing their family was there to provide emotional support as opposed to describing the unique benefits of receiving financial support: “And like my mom is like let me know if you need to borrow money or whatever so they are there just in case.”
Participants did acknowledge and appreciate nonmonetary tangible support such as family helping with childcare and partners helping with tasks around the house: “And just the support from my husband. he has really, really stepped up and is very attentive to me. And so that’s really helped. A lot of my emotional and physical load has been lifted a little bit, so where I’m not all alone in it.”
As seen in the quote above, there was significant overlap between tangible support and emotional support. For example, another participant said: “Definitely my family. tce. if I feel like I’m like slipping and going into like a negative mindset, they definitely help me out.”
Overall, it was evident that social support can be protective against mental health challenges. As one participant said, “Having a village and like that support is huge.”
Mixed methods
The mixed methods analysis of types and sources of social support displayed concordance across both quantitative and qualitative findings around the importance of social support for well-being in this sample of low-SES pregnant women (see Fig. 1). The quantitative data identified support from friends and peers as a significant predictor of prenatal anxiety, which was echoed in more detail in the qualitative data. The shared lived experiences provided by friends/peers uniquely support the emotional well-being of participants in ways that a partner or family could not:

Heat map depicting the quantitative and qualitative relationships between types of support and sources of social support among a sample of pregnant women experiencing socioeconomic disadvantage.
“And then a friend who had a baby in August, kind of people who I could also talk to about the experience and kind of what they’re going through. that’s been very helpful.” That said, there was discordance between the quantitative and qualitative data, because the qualitative data suggested that support from partners, family members, and health care providers protected the well-being of participants during pregnancy while the quantitative did not. To further triangulate the data and better understand these relationships, Pearsons correlations (r) between types of support (qualitative) and sources of support (quantitative) were explored. The strongest associations were seen between partner support and emotional (−.66) and informational support (−.61). Family support was also moderately correlated with emotional, informational, and tangible support (>.50). Friend support was also significantly correlated with each type of support, but the correlations were not as strong. This mixed-methods analysis highlighted that emotional and instrumental support from numerous sources, including friends, peers, partners, and family members, may be the most important resource for this sample of pregnant women. Overall, the integration of both data types emphasizes the complex nature of social support and the need for multilevel sources of social support to holistically care for the mental wellbeing needs of pregnant women.
Discussion
This mixed-methods study investigated unique social determinants of health that may be associated with anxiety among low-SES pregnant individuals and emphasized the value of social support, particularly emotional support, for buffering prenatal anxiety. Social support from friends and peers emerged as significantly predictive of anxiety, aligning with existing literature around social support moderating the relationship between stress and psychological health. 20 The findings of this study are supported by the stress-buffering model, as emotional support was shown to help prenatal participants navigate life stressors and reduce the negative psychological impacts. 25 The results of this study provide practical insights to inform policies, programs, and research efforts to reduce the burden of and disparities in prenatal anxiety.
We investigated associations between sociodemographic factors and social determinants of health (i.e., income, education, housing security, food security) and found that race and food security were the only indicators that were predictive of prenatal anxiety among this underresourced sample (associations between food insecurity and anxiety were approaching significance, p = .08). The finding that White women reported higher anxiety is not surprising, as GAD is typically more prevalent in White women.42,43 In prenatal populations specifically, the risk of anxiety is higher in those with a past history of (GAD), low education, and low levels of social support.44,45 Furthermore, though not statistically significant, the finding that food insecurity may be a critical social determinant for prenatal anxiety aligns with a recent scoping review that found prenatal women experiencing food insecurity are at higher risk for depression and anxiety. 46 Food insecurity during pregnancy contributes to poorer maternal and child outcomes, such as preterm labor, gestational diabetes, and neonatal mortality. 47 Though the heterogeneity in methodology and inadequate number of studies limits the strength of evidence, the established relationship between food insecurity and prenatal mental health warrants improved policies to connect pregnant women with resources (e.g., produce prescriptions, subsidies for purchasing nutritious foods, community outreach programs) that reduce food insecurity. 48
Next, we examined multi-level sources of social support that may buffer prenatal anxiety. In the quantitative sample, support from friends and peers was the only source of social support significantly associated with anxiety. This aligns with existing literature, which found that support from friends reduced prenatal anxiety and depression more than family support.22,49 However, in the qualitative data, individuals shared that support from partners, parents, friends, and peers also helped to mitigate poor mental health and promote well-being. The integration of these data suggests that peer relationships may confer resilience; having support from others who understood what they were going through (i.e., moms on social media, mom friend groups, formal support groups) was informational. Nonfamilial relationships, specifically from others who have been or were pregnant, provided a critical avenue for connection, peer support, and learning. Participants valued being around others who knew what they were experiencing and could share insights in a safe space. The benefits of friendships and peer support networks for underresourced pregnant populations provide promising clinical strategies to protect against prenatal anxiety. Peer support programs are an accessible and promising strategy for preventing and treating prenatal mood disorders.50–52 However, more work is needed to assess clinical peer support interventions for prenatal anxiety.51,53 Given the shortage of mental health providers and limited access care for low-income populations, the effectiveness of peer support interventions for prenatal anxiety should be explored further.53,54
We investigated unique sources of social support (i.e., informational, tangible, emotional) based on the stress-buffering hypothesis and found that emotional support was most strongly correlated with anxiety. This finding aligned with qualitative data, where emotional support was most salient (based on relevance and frequency) when participants discussed sources of support in their life. The importance of emotional support is echoed within existing literature, as emotional closeness promotes prenatal mental health 55 and sufficient emotional support from partners, family, and friends/peers can protect against prenatal anxiety. 22 Outside of the prenatal population, emotional support has been seen to be more powerful than tangible support for well-being.56,57 The importance of emotional support highlighted in this study is especially compelling considering the sample was from a low-resourced population. Even though emotional support emerged as more important to participants in our sample than tangible resources, these findings do not dimmish the need for improved access to prenatal health care in underresourced communities.10,12 Future work should consider the interplay between tangible (e.g., financial assistance) and emotional support to better support low-income perinatal populations.
Limitations
This study has several limitations that should be considered when interpreting the results. First, the cross-sectional design prevents any causal understanding of the impact of social support on prenatal anxiety. Furthermore, since the data were only collected at one timepoint, it cannot account for fluctuations and contextual changes across the prenatal period. Therefore, it cannot be generalized across pregnancy. Next, this study used purposive sampling of women in the United States, which limits generalizability to broader populations. Future research should assess a more diverse sample longitudinally to strengthen causal inferences and better understand changes over time and across cultural contexts.
Conclusions
Despite the limitations, the mixed-methods design of this study adds uniquely to the literature by integrating lived experiences and contextualization of supports to more comprehensively elucidate the role of social support in mitigating prenatal anxiety among low-SES women. Fostering group-based emotional social support (e.g., community-based peer networks, digital peer platforms) should be considered a key part of preventing and managing prenatal anxiety. Evidence-based peer support programs present an accessible and effective approach to promote prenatal mental health, but more work needs to be done to understand how to best implement and assess interventions for prenatal anxiety.50–52 Furthermore, this study found that food insecurity may be one of the most important unmet social needs that contributes to prenatal anxiety, highlighting the importance of enhancing clinical screening processes, referral programs, and policies. This study emphasizes the benefit of strengthening social support networks and group-based clinical practices to mitigate the broad-reaching adverse impacts of prenatal anxiety.
Ethics Approval
All procedures were approved by the Colorado Multiple Institutional Review Board.
Consent to Participate
All individuals consented to participate in this study.
Data Availability Statement
Data is available from the authors upon request.
Footnotes
Author Disclosure Statement
No competing financial interests exist.
Funding Information
This Work Was Supported by the National Institute on Minority Health and Health Disparities (5K01MD016928-02) And (NIH/NCATS Colorado CTSA Grant Number Ul1 TR002535).
