Abstract
Background:
Timely initiation of antenatal care (ANC) is essential for reducing maternal and neonatal mortality and achieving Sustainable Development Goal 3. In Sub-Saharan Africa, and particularly in Somalia, delays remain widespread. The median time for first ANC in Somalia is about 5 months, well beyond the World Health Organization recommendation of the first trimester. Late ANC initiation compromises early detection and management of pregnancy complications. This study examined the timing of first ANC and its predictors among Somali women using survival analysis.
Methods:
This retrospective analysis used data from the 2020 Somalia Demographic and Health Survey, including 7,100 women aged 15–49. Survival analysis defined the event as initiating ANC within the first trimester (≤12 weeks). Kaplan–Meier curves illustrated survival probabilities, log-rank tests compared groups, and a multivariate Cox Proportional Hazards model identified independent predictors, adjusting for sociodemographic and obstetric characteristics.
Results:
Higher maternal education increased the likelihood of timely initiation (primary: AHR = 1.26, 95% confidence interval [CI]: [1.12–1.41]; higher: AHR = 1.35, 95% CI: [1.02–1.78]). Prior delivery in a health facility was strongly predictive (AHR = 2.24, 95% CI: [2.04–2.46]). Delayed initiation was associated with rural (AHR = 0.82, 95% CI: [0.74–0.92]) and nomadic residence (AHR = 0.32, 95% CI: [0.27–0.39]), certain regions (Hiraan: AHR = 0.33, 95% CI: [0.25–0.44]), not watching television (AHR = 0.84, 95% CI: [0.73–0.96]), and husband’s unemployment (AHR = 0.77, 95% CI: [0.70–0.84]). The magnitude of these effects was substantial; for instance, prior delivery in a health facility more than doubled the likelihood of timely ANC initiation, while nomadic residence reduced this likelihood by 68% compared with urban residence. Wealth status was not significant after adjustment.
Conclusion:
Delays in ANC initiation remain widespread in Somalia. Independent predictors include maternal education, prior delivery location, residence type, region, media exposure, and husband’s socioeconomic status. Interventions should focus on rural and nomadic populations, strengthen health education, and leverage facility-based experiences to improve timely ANC uptake.
Introduction
Antenatal care (ANC) represents a health care service provided to pregnant women for early prevention, diagnosis, and treatment of medical- and pregnancy-related complications. 1 Also another study defined ANC as the care provided to pregnant women and teenage girls by trained health care professionals to ensure the greatest possible health for both mother and unborn child throughout pregnancy. 2 Due to the importance of ANC for protecting the health of women and their unborn children, the World Health Organization (WHO) recommended eight or more ANC visits for women with positive pregnancy experiences. Additionally, the WHO has recommended that all pregnant women have at least four ANC visits, with the first visit occurring in the first trimester, to guarantee the best possible care throughout the pregnancy. 3 The main purpose of focused ANC is to help women sustain normal pregnancies through early identification of preexisting conditions, complications that arise during childbirth, and promotion of well-being. 4 ANC programs provide for early detection of risks and complications associated with pregnancy and ensure access to care, including health education, vaccines, medical testing, and therapies. 5
Moreover, ANC services contribute to the enhancement of health care facility delivery, resulting in decreased maternal morbidity and mortality.6,7 This support in achieving Sustainable Development Goal 3 (SDG 3), which emphasizes maternal mortality reduction and improvements in women’s health care, to reduce the global maternal mortality ratio to 70 per 100,000 live births by 2030. 8 In 2020, for instance, 287,000 maternal fatalities occurred globally. In low- and middle-income nations, more than 99% of these fatalities occurred. Around 70% of all maternal deaths reported worldwide in 2020 occurred in Sub-Saharan Africa (SSA), which continues to be the region with the greatest rate of maternal mortality. 9 Western Africa reported the highest maternal deaths due to complications during and following pregnancy and childbirth, followed by Central and Eastern Africa. South Sudan, Chad, and Nigeria recorded the highest maternal deaths during this period. 9
While the utilization of ANC in developing countries has considerably improved, a limited number of pregnant women attend a total of four ANC visits, with 72% initiating the first visit after 12 weeks of gestation10–16. However, the magnitude of timely initiation of ANC visits in SSA was 38.0%, ranging from 14.5% in Mozambique to 68.6% in Liberia. 10 A significant proportion of pregnant women in SSA delay initiating ANC visits, missing out on crucial services that can promote optimal maternal and child health outcomes. 10 For example, a study in Ethiopia found that 62.3% of pregnant women delayed ANC initiation, with participants on average beginning ANC at 4 months’ gestational age. Similarly, in a study conducted in Kenya, 58% of women had at least four ANC visits,11,12 while in Somalia, the utilization rate is even lower, with 33% of pregnant women initiating the first visit during the fourth month of the gestation period.13,14 The 2020 SDHS data showed that the median time to ANC initiation in Somalia was 5 months. 15
Thus, the WHO underlines the vital need to put the focus on mothers who commence fewer visits and initiate the ANC late.12,16 Numerous studies on the determinants of ANC utilization have found an association between the sociodemographic, reproductive, and obstetric variables of the mother with the utilization of ANC. 17 However, not enough studies are done in investigating the determinants and timing of ANC visits in Somalia, and the available pieces of evidence are inconclusive. Delay in the timing of the first visit increases the risk of the development of complications for both mother and child.7,12 Very few studies done in Somalia using both secondary and primary data had not considered the adoption of survival analysis approaches in the data analysis. Therefore, after 12 weeks of pregnancy, delayed ANC attendance is becoming more and more of a public health issue in Somalia. So, the main purpose of the study is to examine the time to initiate ANC and its predictors among pregnant women in Somalia using samples from 2020 SDHS dataset by employing a new analytical survival analysis approach.
Material and Methods
Study setting
This study was conducted in Somalia, a country located in the Horn of Africa with a diverse topography, encompassing plateaus, plains, and hills. Somalia’s total land area is estimated at 637,657 km2, with a 3,333 km coastline along the Gulf of Aden to the north and the Indian Ocean to the east and south. It borders Djibouti along the north-west, Ethiopia to the west, and Kenya to the south-west. Somalia has a tropical hot climate with minimal seasonal variations and daily temperatures ranging from 30°C to 40°C. The country experiences low annual rainfall and four distinct seasons: Gu’ and Deyr (rainy seasons) and Haga and Jilal (dry seasons). Over the years, however, changing and unpredictable climate patterns have resulted in recurrent floods and drought experienced across the country. 15
Study design
The study employed a retrospective cross-sectional design using data from the 2020 Somalia Demographic and Health Survey (SDHS) dataset. This design allowed for the examination of factors associated with the timing of the first ANC visit among pregnant women at a specific point in time.
Data source
The primary data source for this study was the publicly available 2020 SDHS dataset, collected by the Somali National Bureau of Statistics (SNBS) in collaboration with the Ministry of Health and other stakeholders. 18 The data are available from the corresponding author on reasonable request.
Sampling procedure
The SDHS 2020 employed a multistage cluster sampling design to ensure a nationally representative sample across all regions of Somalia. The country was stratified into urban, rural, and nomadic areas, resulting in a total of 55 sampling strata. Due to security concerns, all three strata of Lower Shabelle and Middle Juba regions, along with the rural and nomadic strata of Bay region, were excluded from the survey. The final sampling frame comprised 47 sampling strata. The survey utilized a three-stage stratified cluster sample design with probability proportional to size (PPS) sampling at the first and second stages for primary sampling units (PSUs) and secondary sampling units, respectively. Systematic sampling was used for households at the third stage. 18
A two-stage stratified cluster sample design was applied, with PPS sampling for PSUs at the first stage and systematic sampling for households at the second stage. To ensure comparable precision across regions, PSUs were allocated equally to each region with slight adjustments in two regions. A sample of 35 EAs was selected independently in each stratum, with probability proportional to the number of digitized dwelling structures. A complete listing of households was conducted in the selected EAs, and information on births and deaths was recorded using the maternal mortality questionnaire. A sample of 10 EAs (or Temporary Nomadic Settlements [TNS] for nomadic areas) was selected from each stratum, with probability proportional to the number of households. A systematic sample of 30 households was then selected from each Enumeration Area (or TNS) for the main survey interview. 18
Study population and sample
The target population of this study comprised pregnant women (15–49 years old) residing in Somalia, who had received ANC during their pregnancy prior to the survey collection. The SDHS 2020 interviewed a total of 16,486 women, including 11,876 ever-married women and 4,610 never-married women. To minimize recall bias, this analysis was restricted to the most recent birth for each woman within the 5 years preceding the survey. After data cleaning and preprocessing, the final sample size utilized for this study was 7,100 observations with 16 variables.
Variables of the study
Outcome variable
The dependent variable of the study was the time in months it takes among pregnant women to have their first ANC visit checks. When a pregnant woman receives ANC during her first trimester of pregnancy, it is considered a success (event = 1); otherwise, it is a failure (censored = 0).
Explanatory variables
The availability of 2020 SDHS dataset and existing literature10,19,20 enabled to deduce the independent variables of the study. These were chosen as explanatory variables of the study: region, residence, mothers’ education, frequency of listening to radio, frequency of watching television, wealth quintile, total children ever born, age of respondent at first birth, distance to health facility, age at first marriage, respondent worked in last 12 months, delivery location, husband worked last 12 months, even husband ever attended school.
Methods of data analysis
This study employed a comprehensive data analysis approach utilizing the statistical software package STATA, version 16.0, for all data extraction and analysis. To account for the complex multistage cluster sampling design and to ensure the results remained nationally representative after sample restrictions, all analyses were performed using the survey weights provided in the SDHS dataset. The following steps were undertaken.
Descriptive statistics were calculated for all variables included in the study, including summary statistics (count and percentage) for categorical variables. These descriptive statistics provided an initial overview of the sociodemographic characteristics of the study population and their relationship with the timing of the first ANC visit.
Time-to-event analysis
The dependent variable was the time in months it took pregnant women to have their first ANC visit. A successful event (event = 1) occurred when a woman received ANC during her first trimester, while a censored event (censored = 0) indicated the woman did not receive ANC during the first trimester.
Kaplan–Meier estimates
Kaplan–Meier survival curves were estimated and presented to visually depict the probability of a woman initiating ANC over time. This allowed for a comparison of survival probabilities across different covariate groups, such as place of residence, education levels, wealth quintiles, women’s employment status, and regional disparities. 21
Log-rank test
Log-rank tests were conducted to statistically compare the survival curves of different covariate groups, assessing whether there were statistically significant differences in the timing of ANC initiation. 22
Multivariate analysis
To identify the predictors of the timing of the first ANC visit, a Cox proportional hazards (PH) model was employed. This model allowed for the assessment of the association between each predictor variable and the risk of initiating ANC, while controlling for the influence of other factors. 23
Variable selection
The Cox PH model included all variables that demonstrated statistical significance at a 5% level in the log-rank test. This approach ensured that the final model included variables with a demonstrable association with the timing of ANC initiation.
PH assumption
The (PH) assumption, which is crucial for the validity of the Cox PH model, was validated using the Schoenfeld residuals global test.
Hazard ratios
The Cox PH model generated hazard ratios (HRs) for each predictor, representing the relative risk of initiating ANC in a specific group compared with the reference group, adjusted for other variables in the model.
The results from the Cox PH model were presented and interpreted in terms of the HRs, their associated p-values, and 95% confidence intervals (CIs). This provided a clear understanding of the magnitude and direction of the association between each predictor and the likelihood of initiating ANC.
The analysis focused on identifying statistically significant predictors of timely ANC initiation and describing the relative risk of initiating ANC for each covariate group.
This multifaceted approach using descriptive statistics, survival analysis, and the Cox PH model enabled a comprehensive investigation of the predictors of timely ANC initiation among pregnant women in Somalia. The findings provided valuable insights for developing effective interventions to improve maternal and child health outcomes in the country.
Ethical considerations
This study utilized publicly available data from the SDHS 2020, which was collected through a rigorous process adhering to ethical standards, including informed consent and data confidentiality. The analysis focused on aggregate data and did not involve any personally identifiable information. All ethical considerations regarding data use and privacy were observed, ensuring responsible and ethical research practices.
Results
Descriptive statistics of the study participants
Analysis of the sociodemographic characteristics in Table 1 revealed variations in the timing of the first ANC visit among pregnant women in Somalia. Geographic location plays a role, with regions such as Banadir (51.8%) and Awdal (50.8%) showing higher rates of timely visits (“Even” category) compared with regions such as Hiraan (15.6%). Residence is also a key factor, with urban women (51.6%) significantly more likely to have timely visits than rural (36.5%) and especially nomadic women (10.9%). Socioeconomic status strongly influences timing: rates increase dramatically with mother’s education level (from 29.1% with no education to 78.1% with higher education), wealth quintile (16.4% lowest to 60.1% highest), and frequency of watching television (30.4% not at all to 69.7% weekly). Delivering in a health facility (68.6%) is strongly associated with timely ANC compared with home delivery (23.6%). Interestingly, women whose husbands had not attended school reported higher timely visits (56.7%) than those whose husbands had (26.4%).
Summary of Sociodemographic Characteristics Among Pregnant Women in Somalia

ANC, antenatal care.
Bivariate analysis using log-rank tests in Table 2 revealed factors significantly associated (p < 0.001) with the timing of the first ANC visit among pregnant women in Somalia. Strong predictors of more timely initiation included higher mother’s education (log-rank = 753.95), higher wealth quintile (log-rank = 1908.76), urban residence (log-rank = 3238.69), frequent media exposure (listening to radio: log-rank = 241.27; watching TV: log-rank = 853.21), delivering in a health facility (log-rank = 1660.37), and employment (respondent worked: log-rank = 14.34; husband worked: log-rank = 851.15). For these groups, the observed number of timely visits significantly exceeded expected values, such as for women in the highest wealth quintile (Observed Events [Obs] = 719 vs. Exp = 299.86) and those delivering in a health facility (Obs = 1144 vs. Exp = 451.76). Significant regional variations were also observed (log-rank = 794.28), with areas like Banadir having far more timely visits than expected. Counterintuitively, women whose husbands had not attended school (log-rank = 902.74; Obs = 1027 vs. Expected Events [Exp] = 497.94) and those reporting distance to a health facility as a “problem” (log-rank = 125.16; Obs = 1034 vs. Exp = 801.11) also had significantly more timely visits than expected (p < 0.001). Conversely, factors such as the total number of children ever born (p = 0.198), age at first birth (p = 0.265), and age at first marriage (p = 0.212) did not show a statistically significant association with the timing of the first ANC visit in this analysis.
Bivariate Analyses of Timing to First ANC Visits Among Pregnant Women in Somalia

The adjusted Cox PH Model in Table 3 revealed several key factors independently associated with an earlier initiation of the first ANC visit among pregnant women in Somalia. Notably, mother’s education level demonstrated a significant positive influence; compared with women with no education, those with primary (AHR = 1.258, p < 0.001), secondary (Adjusted Hazard Ratio [AHR] = 1.303, p = 0.005), and higher education (AHR = 1.348, p = 0.037) exhibited a progressively higher likelihood of timely ANC attendance. The strongest predictor for earlier care was the location of previous delivery, with women who delivered in a health facility showing more than double the likelihood of timely ANC initiation compared with those who delivered at home (AHR = 2.238, p < 0.001). This underscores the importance of positive past experiences with the health care system. Intriguingly, the analysis also found that women whose husbands had not attended school had a significantly higher likelihood (AHR = 1.195, p < 0.001) of timely ANC compared with those whose husbands had attended, a counterintuitive finding suggesting complex social dynamics may be at play, which warrant further exploration.
Cox Proportional Hazard Model on the Determinants of Timing to First ANC Among Pregnant Women in Somalia
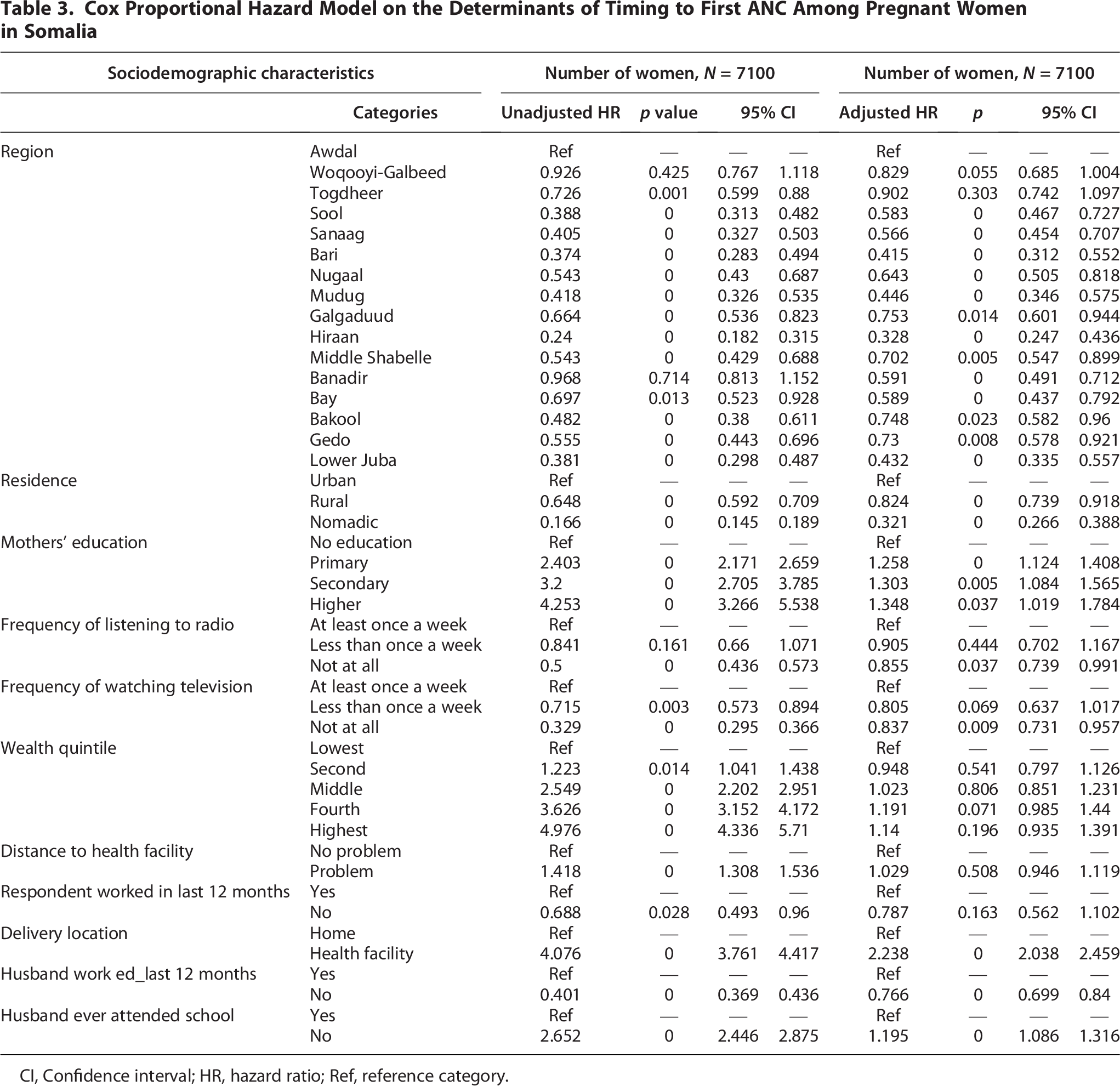
CI, Confidence interval; HR, hazard ratio; Ref, reference category.
Conversely, several factors significantly increased the probability of a delayed first ANC visit. Residence type emerged as a major determinant, with rural women having a lower likelihood (AHR = 0.824, p < 0.001) and nomadic women having a drastically lower likelihood (AHR = 0.321, p < 0.001) of timely visits compared with their urban counterparts, highlighting substantial geographic access barriers. Significant regional disparities also persisted after adjustment; compared with Awdal, residing in regions such as Hiraan (AHR = 0.328, p < 0.001), Bari (AHR = 0.415, p < 0.001), Lower Juba (AHR = 0.432, p < 0.001), and Mudug (AHR = 0.446, p < 0.001) was strongly associated with later ANC initiation. Furthermore, reduced exposure to mass media, specifically not listening to the radio (AHR = 0.855, p = 0.037) or not watching television (AHR = 0.837, p = 0.009) compared with weekly exposure, was linked to delayed care. Last, having a husband who was not employed in the past year also significantly reduced the likelihood of timely ANC (AHR = 0.766, p < 0.001), likely reflecting economic constraints impacting health care access.
It is crucial to note the impact of the multivariate adjustment on certain variables. Factors such as wealth quintile, perceived problems with distance to a health facility, and whether the respondent herself worked in the last 12 months, which showed significant associations in the initial bivariate analyses in Table 3, lost their statistical significance (all p > 0.05) in the final adjusted Cox model. This indicates that their unadjusted associations were likely confounded by other, more influential factors captured in the model, such as education, residence type, or region. Therefore, the independent predictors robustly associated with the timing of the first ANC visit in this Somali context, after controlling for confounding effects, are primarily mother’s education, prior delivery location, husband’s education level (in an unexpected direction), residence type, geographic region, media exposure, and husband’s employment status.
The proportional hazards assumption was assessed using Schoenfeld residuals. The global test indicated no evidence of proportionality violation (χ2 = 21.48, df = 14, p = 0.0899). Although region (p = 0.0322) and maternal employment status (p = 0.0452) showed minor deviations, the overall model satisfied the PH assumption, and the Cox PH model was considered appropriate. Therefore, the global test is nonsignificant, and the Cox model is acceptable (Table 4).
Test of Proportional Hazards Assumption Using Schoenfeld Residuals
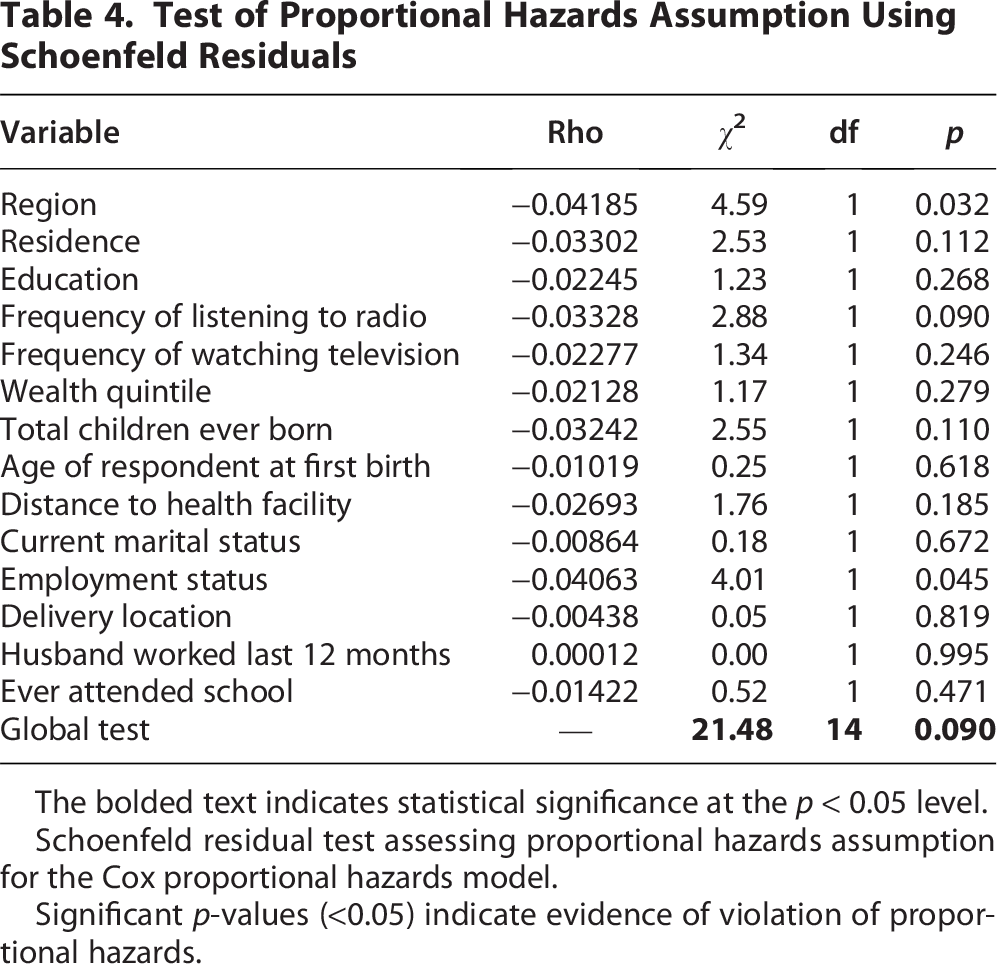
The bolded text indicates statistical significance at the p < 0.05 level.
Schoenfeld residual test assessing proportional hazards assumption for the Cox proportional hazards model.
Significant p-values (<0.05) indicate evidence of violation of proportional hazards.
The Kaplan–Meier survival curves visually depict significant disparities in the timing of the first ANC visit across various sociodemographic groups, and these visual differences are confirmed as statistically significant by log-rank tests (all p < 0.001). The curves for place of residence show urban women initiating ANC earliest, followed by rural, and then nomadic women initiating latest; the log-rank test confirms a highly significant difference between these groups (Log-rank = 3238.69, p < 0.001). The adjusted Cox model further quantified this, showing nomadic women had a significantly lower hazard of timely ANC compared with urban women (AHR = 0.321). A pronounced gradient is also evident for Wealth Quintile, with the highest quintile curve dropping fastest (earliest ANC) and the lowest quintile curve dropping slowest (latest ANC). This visually clear and graded difference is statistically significant (log-rank = 1908.76, p < 0.001), although wealth lost significance after adjusting for other factors in the Cox model. Similarly, women’s education level demonstrates a strong, statistically significant gradient (log-rank = 753.95, p < 0.001), where higher education corresponds to markedly earlier ANC initiation (fastest curve drop), while no education corresponds to the latest initiation (slowest curve drop). This effect remained significant after adjustment, with higher education showing a higher hazard for timely ANC (higher ed. AHR = 1.348). Finally, while the visual difference for women’s employment status appears less dramatic, employed women show a trend toward earlier ANC initiation compared with unemployed women; this difference was also statistically significant in the unadjusted bivariate analysis (log-rank = 14.34, p < 0.001, though using “Yes” as reference here differs from the table’s “No” as reference, the significance holds), but it lost statistical significance in the adjusted Cox model (p = 0.163) (Fig. 1).
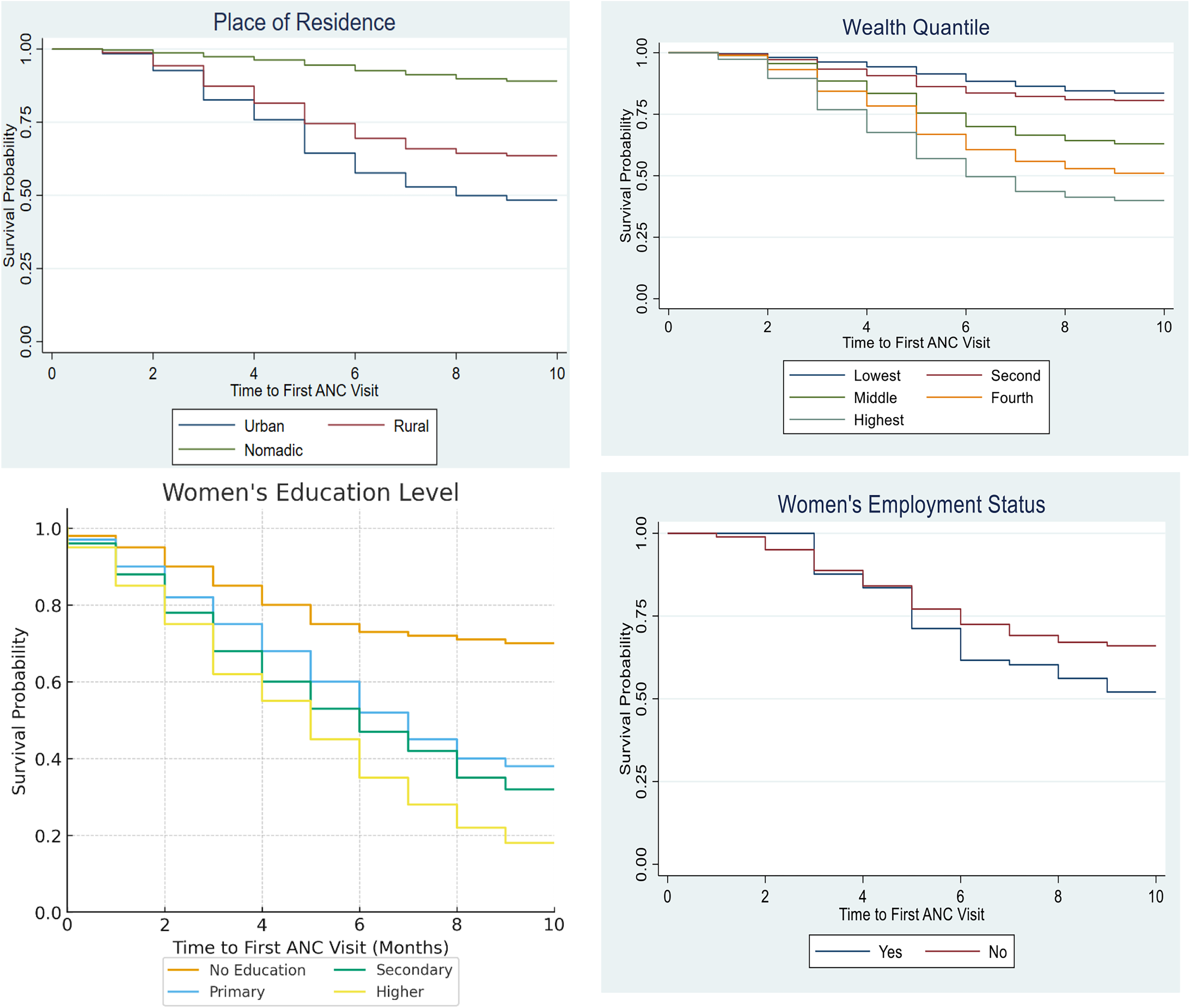
Kaplan–Meier survival curve of timing at first ANC by selected respondents’ characteristics. ANC, antenatal care.
The significant regional variations highlighted in Table 1 are further illustrated in the Kaplan–Meier survival curves presented in Figure 2, which visually depict the disparities in the timing of ANC initiation across Somalia’s regions. Figure 2 reveals significant regional disparities in the timing of the first ANC visit in Somalia. Notably, regions such as Awdal and Woqooyi-Galbeed show the slowest uptake, with approximately 85% and 83% of women, respectively, still not initiating ANC by 10 months. In contrast, Lower Juba and Banadir demonstrate comparatively earlier initiation, with their survival probabilities dropping to around 50% by 10 months. This wide range, from nearly 85% to 50% not initiating ANC by 10 months, underscores a critical and spatially uneven challenge in accessing timely maternal health care across the country.

Kaplan–Meier curves of time to first ANC visit by region.
Discussion
This study utilized a survival analysis approach on the 2020 SDHS data to investigate the timing of the first ANC visit and identify its predictors among pregnant women in Somalia. The findings confirm that delayed initiation of ANC remains a significant public health challenge in Somalia, consistent with previous reports indicating a median initiation time of 5 months 15 and low overall utilization rates.13,14 This delay starkly contrasts with the WHO recommendation for the first visit to occur within the first trimester (12 weeks), 3 placing Somali women and their unborn children at increased risk, counteracting the goals of reducing maternal mortality, as outlined in SDG 3. 8
Our application of survival analysis provides a nuanced understanding of when women initiate care and the factors influencing this timing, moving beyond simple prevalence estimates often found in earlier studies. Several findings from our multivariate Cox PH model align well with the existing literature on ANC utilization in developing countries and SSA. The strong positive association between higher maternal education (primary, secondary, and higher) and earlier ANC initiation (AHRs 1.258, 1.303, 1.348, respectively, p < 0.05) corroborates the widely established link between female education and improved health-seeking behaviors. 17
Educated women are likely more aware of the benefits of early ANC, 5 possess greater autonomy in decision-making, and may navigate the health care system more effectively. This aligns with findings from broader studies in developing countries11,17 and specifically echoes similar results from Ethiopia 10 and potentially Kenya, 14 although the specific impact magnitude might differ. The significantly lower likelihood of timely ANC initiation among rural (AHR = 0.824, p < 0.001) and especially nomadic women (AHR = 0.321, p < 0.001) compared with urban women confirms findings from other SSA contexts, 10 where geographic access and availability of services heavily influence utilization.
Urban areas typically offer better access to health facilities, information, and potentially more educated populations, contributing to earlier ANC uptake. The extreme disadvantage faced by nomadic populations highlighted in our study underscores the severe access barriers they encounter in Somalia’s specific context. 15 The finding that lack of exposure to radio (AHR = 0.855, p = 0.037) and television (AHR = 0.837, p = 0.009) is associated with delayed ANC initiation supports the role of mass media in disseminating health information and promoting positive health practices. 5 This concords with the general understanding that health education is a key component of ANC promotion.5,7
Furthermore, the finding that women whose husbands were not employed in the last 12 months were less likely to initiate ANC timely (AHR = 0.766, p < 0.001) aligns with socioeconomic determinants influencing health care access. 17 Financial constraints can significantly impede a family’s ability to afford transport, service fees (if any), and time off work for ANC visits. Additionally, the powerful association between having previously delivered in a health facility and timely ANC initiation in the current pregnancy (AHR = 2.238, p < 0.001) is a significant finding. This strongly suggests that positive past experiences with the formal health care system encourage future engagement. It aligns with studies showing ANC attendance enhances facility delivery,6,7 potentially indicating a virtuous cycle where satisfactory facility-based care encourages subsequent timely ANC utilization.
While many findings align with broader literature, some results present contradictions or offer unique contextual insights specific to Somalia. The finding that women whose husbands had not attended school were more likely to initiate ANC timely (AHR = 1.195, p < 0.001) contradicts the common expectation that higher spousal education facilitates better health care utilization, often observed in studies examining determinants of ANC. 17 This counterintuitive result is a key contextual contribution of our study. It may reflect complex sociocultural dynamics within Somali households regarding decision-making power, perceived needs, or perhaps the nature of education received (e.g., traditional vs. formal) and its influence on health beliefs. It could also be confounded by unmeasured factors or specific regional/cultural variations within Somalia. This finding warrants further qualitative investigation to understand the underlying reasons. In the bivariate analysis (log-rank tests), higher wealth quintile and reporting “no problem” with distance were strongly associated with earlier ANC, consistent with general expectations. 17
However, these factors lost statistical significance in the adjusted Cox model. This does not necessarily contradict their importance but suggests their influence on the timing of ANC initiation in Somalia might be largely mediated or confounded by other factors such as maternal education, residence type (which inherently captures access/distance issues for rural/nomadic groups), and husband’s employment status. Our study’s contribution here is demonstrating, through robust multivariate modeling, that factors such as education, residence, and prior health care experience appear to be stronger independent drivers of ANC timing in this specific context than wealth or perceived distance alone, once other variables are controlled. While regional variations are common, 10 our study specifically quantifies the significant disparities in ANC timing within Somalia using survival analysis. Regions such as Hiraan, Bari, Lower Juba, and Mudug showed a significantly lower hazard of timely initiation compared with Awdal, even after adjusting for individual-level factors. This highlights deep-rooted geographical inequities in service availability, accessibility, security, or sociocultural norms impacting ANC timing, contributing context-specific evidence crucial for targeted interventions within Somalia.
Strengths and limitations
The primary strength of this study lies in its use of survival analysis (Kaplan–Meier and Cox PH models) on a large, nationally representative dataset (SDHS 2020). This allowed for a more sophisticated analysis of the timing of ANC initiation and its predictors, identifying not just if but when women access care and the factors influencing this duration, which is a novel approach for this specific research question in Somalia, according to our background review. The multivariate Cox model helps control for confounding factors, providing more robust estimates of independent predictors.
However, the study shares limitations inherent in the data source and design, as noted. Reliance on self-reported data introduces potential recall bias regarding the timing of the first ANC visit and gestational age. Social desirability bias might also influence responses. The cross-sectional nature of the SDHS data prevents the establishment of causal relationships; we can only identify associations. While the SDHS aims for national representation, security issues excluded certain regions, 18 potentially limiting the generalizability of findings to those specific inaccessible areas. Furthermore, the survey may not capture all potentially relevant cultural, social, or health system factors influencing ANC timing.
Implications for policy and practice
The findings underscore the urgent need for targeted interventions to improve timely ANC initiation in Somalia.
Conclusion
This study confirms significant delays in ANC initiation among pregnant women in Somalia, falling short of WHO recommendations. Utilizing a survival analysis approach, we identified key independent predictors influencing the timing of the first ANC visit. Higher maternal education, prior delivery in a health facility, and, paradoxically, having a husband with no schooling were associated with earlier initiation. Conversely, rural/nomadic residence, residing in specific regions, lack of media exposure, and husband’s unemployment were associated with significant delays. While wealth and perceived distance were significant in unadjusted analyses, their effects were attenuated after controlling for other factors. These findings provide crucial, context-specific evidence for developing targeted strategies to improve timely ANC uptake, enhance maternal and child health outcomes, and contribute toward achieving SDG 3 in Somalia. Further research, particularly qualitative studies, is needed to explore unexpected findings and the complex interplay of factors influencing ANC timing in this setting.
Authors’ Contributions
Conceptualization: M.A.H., A.N.A., and A.M.Y.; methodology: A.M.Y. and M.A.H.; data curation: A.M.Y., M.A.H., and A.A.I.; analysis: M.A.H., A.M.Y., and A.A.I.; visualization: M.A.H. and A.M.Y.; writing—original draft preparation: A.N.A., M.A.H., A.M.Y., and A.A.I.; writing—intellectual content, review, and editing: O.S. and A.H.M; and supervision: O.S. and A.H.M. All authors reviewed and approved the final version of the article.
Footnotes
Acknowledgments
The authors are thankful for the assistance and cooperation of the SNBS in making the existing data available for this study. Furthermore, the authors express their appreciation to the families and participants for their volunteer engagement, as their insights have played a vital role in improving our understanding of the timing of the first ANC visit among pregnant women in Somalia.
Author Disclosure Statement
The authors declared that there was no conflict of interest regarding the publication of this article. All authors have disclosed any affiliations, financial or otherwise, that might be perceived as conflicts of interest in connection with this article.
Funding Information
This study received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors. All research activities were self-funded by the authors.
Ethics Approval and Consent to Participate
This study was conducted while maintaining ethical standards to the highest possible extent. This study was conducted in accordance with the requirements of the Helsinki Declaration of the Human Participant Research Association. No human body samples were used in this investigation, and personally identifiable information were gathered.
