Abstract
Background:
Osteochondral allografting is a well-established, durable treatment option for focal patellar cartilage defects, particularly in young, active patients with symptomatic grade 3 and 4 lesions. Clinical outcomes show success rates of 77% to 87% when grafts are accurately placed and properly integrated. Precise cartilage-to-graft congruity is critical, as malalignment may lead to persistent pain, graft failure, or cartilage degeneration. Arthroscope-assisted techniques enhance visual accuracy, improving fit and load distribution while reducing the risk of prominent or unstable grafts.
Indication:
The procedure was indicated in a young female patient with a symptomatic grade 4 osteochondral defect of the patella that had failed nonoperative management. No concomitant realignment or osteotomy was required.
Technique Description:
Through a medial parapatellar approach, the patella was everted, and multiple full-thickness defects were identified on the medial and lateral facets. The degenerated cartilage was debrided, and the recipient sites were precisely measured and prepared (6-8 mm diameter, 8 mm depth). Using arthroscopic assistance, osteochondral plugs were harvested from the flattest portion of the donor condyle with careful axial alignment. Each graft was inserted under direct arthroscopic visualization, ensuring a flush, congruent surface with surrounding native cartilage. Multiple grafts were placed sequentially, guided by enhanced visualization to avoid prominence and optimize contour matching.
Results:
Intraoperative assessment confirmed stable fixation and optimal surface congruence of all grafts. Arthroscopic visualization enabled correction of subtle irregularities that may not be palpable through open techniques. Rehabilitation was initiated early to prevent arthrofibrosis, with partial weightbearing maintained for 4 weeks, followed by a progressive recovery program emphasizing mobility, strength, and endurance.
Discussion/Conclusion:
Arthroscope-assisted patellar osteochondral grafting provides enhanced accuracy in graft placement and alignment, potentially improving integration and long-term outcomes. This technique is particularly valuable for achieving flush, congruent reconstruction in patients with isolated patellar chondral lesions. Early mobilization and structured rehabilitation are essential for optimizing functional recovery and reducing the risk of complications, such as stiffness, pain, or poor graft incorporation.
Patient Consent Disclosure Statement:
The author(s) attests that consent has been obtained from any patient(s) appearing in this publication. If the individual may be identifiable, the author(s) has included a statement of release or other written form of approval from the patient(s) with this submission for publication.
This is a visual representation of the abstract.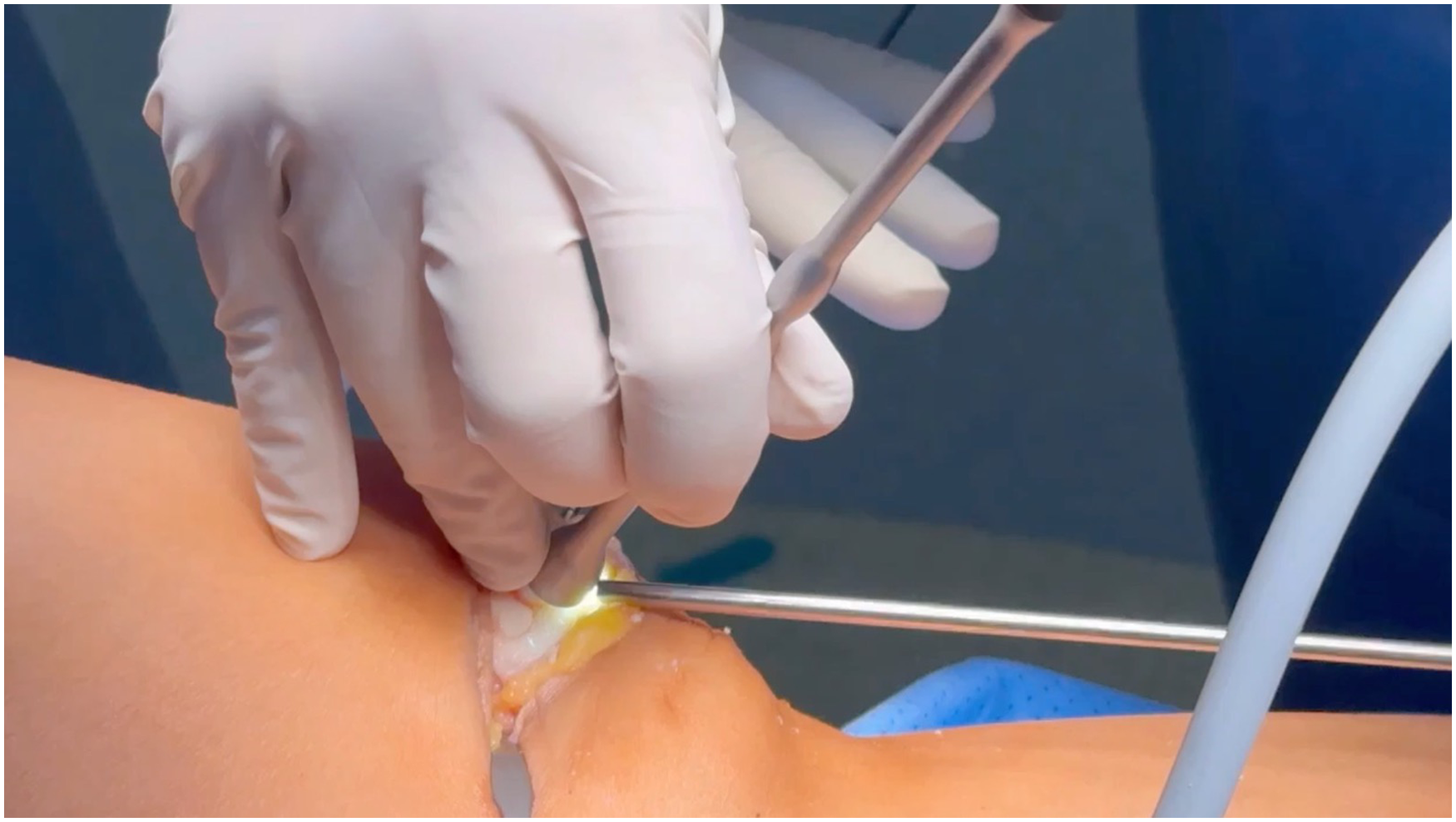
Keywords
Video Transcript
Background
Background Osteochondral grafts are an effective, durable option for patellar defects (1-4 cm2), improving pain, functional scores, and daily activities.3,4,8 Osteochondral grafts restore hyaline cartilage, providing long-term durability and joint preservation. This results in significant pain reduction and functional improvement, as reflected by higher International Knee Documentation Committee and Knee injury and Osteoarthritis Outcome Score scores postoperatively.1,2
Achieving graft survival rates ranging from about 87% at 5 years to 77% at 10 years.3,7 While bone marrow grafts may further enhance graft incorporation. Current recommendations highlight the importance of precise cartilage-to-graft matching, as poor alignment can lead to persistent pain, graft failure, and cartilage degeneration. Therefore, accurate implantation and peripheral alignment should be prioritized to ensure symmetric loading and optimal graft integration.5,6
Indications
This case involves a female patient with a grade 4 chondral defect of the patella that failed conservative management. A fresh osteochondral allograft was used.
Technique Description
A medial parapatellar incision was made to access the joint. Two 2.8-mm pins were inserted to evert the patella and expose the articular surface. Grade 4 defects with unstable cartilage were identified on both the medial and lateral facets. The defects were measured, and the degenerated cartilage was debrided. An initial recipient site is prepared with a diameter and depth of 8 mm. Under arthroscopic visualization, a parallel tunnel was created.
The osteochondral graft is harvested from the flattest possible area of the condyle, maintaining a parallel orientation to the graft axis and using the highest precision during harvesting. This technique ensures optimal congruence and a more stable fit of the plug into the previously prepared recipient tunnel.
The graft was inserted under arthroscopic guidance and carefully positioned to achieve the best possible adaptation to the recipient's site without any prominent areas. It is important to know that the graft is gently impacted. Adjacent to this lesion, a new graft was prepared. The recipient's site measured 6 mm in diameter and 8 mm in depth using enhanced arthroscopic visualization.
The graft was implanted flush with the surrounding cartilage to ensure proper alignment with the underlying cartilage surface. The use of the arthroscope enhanced precision, allowing for the visualization of minor surface irregularities imperceptible to palpation. An additional defect was identified on the medial facet, which was treated with a 6-mm diameter osteochondral graft.
Results and Discussion
This surgical technique allows us to be more precise in the placement of osteochondral grafts. Here, we can observe that the grafts are congruent and flush with the cartilage surface. Rehabilitation begins with early mobilization, which is key to preventing arthrofibrosis. 2
Patients should remain partial weightbearing with crutches for 4 weeks unless an osteotomy is performed, followed by a progressive staged rehabilitation program focusing on mobility, endurance, and strength to ensure optimal recovery. 2
Possible complications of osteochondral grafting in the knee include poor graft alignment, damage to surrounding cartilage, persistent pain, intra-articular bleeding that may require drainage, infection, compromised graft integration, and postoperative joint stiffness.2,3,7,8 These are the key bibliographic references cited in this publication.
Footnotes
Submitted August 5, 2025; accepted November 19, 2025.
One or more of the authors has declared the following potential conflict of interest or source of funding: G.A.J.Q. is a consultant for Johnson & Johnson and Stryker. P.A.S.R. is a consultant for Arthrex. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
