Abstract
Background:
Patellar instability, often associated with medial patellofemoral ligament rupture, is prevalent in adolescents. Risk factors include trochlear dysplasia, patella alta, abnormal patellar tilt, and increased tibial tubercle to trochlear groove (TT-TG) distance.
Indication:
A variety of surgical options are available for addressing patellar instability, and the selection of each technique should be tailored to the unique pathoanatomy of each patient. Medial patellofemoral ligament reconstruction (MPFLR) is indicated for patients with patellar instability, and tibial tubercle osteotomy (TTO) is indicated for patients with a TT-TG >20 mm.
Technique Description:
An anterior midline incision is performed to expose the patella, patellar tendon, and tibial tubercle. Diagnostic arthroscopy is performed to assess patellar engagement and cartilage integrity, followed by the TTO. Three guidewires are placed with 15° of obliquity, to guide a 6-cm osteotomy, from medial to lateral and from proximal to distal. A distal cortical hinge must be left intact. A 15-mm medial resection of the tibial tubercle is performed to avoid protrusion against the skin, which is followed by medialization of the tubercle and fixation with K-wires until dynamic testing ensures proper alignment and definitive fixation is achieved with cannulated headless screws. A lateral retinacular lengthening is performed to balance patellar forces. MPFLR is executed using a semitendinosus allograft. The graft is anchored to the patella and drawn through a surgically created plane to the medial femoral condyle. The femoral tunnel is created under fluoroscopy guidance, and the graft is then passed and secured. Graft tension and patellar mobility are adjusted according to dynamic testing. Once patellar stability is achieved and maintained through range of motion, the graft is then fixed.
Results:
Patients can expect improved clinical outcomes with a high return-to-sports rate following both isolated MPFLR and concomitant TTO. The combination of MPFLR + TTO significantly reduces revision rate, compared to isolated MPFLR in patients with increased TT-TG distance, and enhances postoperative patellofemoral tracking.
Discussion/Conclusions:
MPFLR + TTO improves patellofemoral tracking and corrects patellar instability, substantially improving postoperative outcomes compared to MPFLR alone. Patients with patellar instability and an increased TT-TG may be effectively treated with MPFLR + TTO.
Patient Consent Disclosure Statement:
The author(s) attests that consent has been obtained from any patient(s) appearing in this publication. If the individual may be identifiable, the author(s) has included a statement of release or other written form of approval from the patient(s) with this submission for publication.
This is a visual representation of the abstract.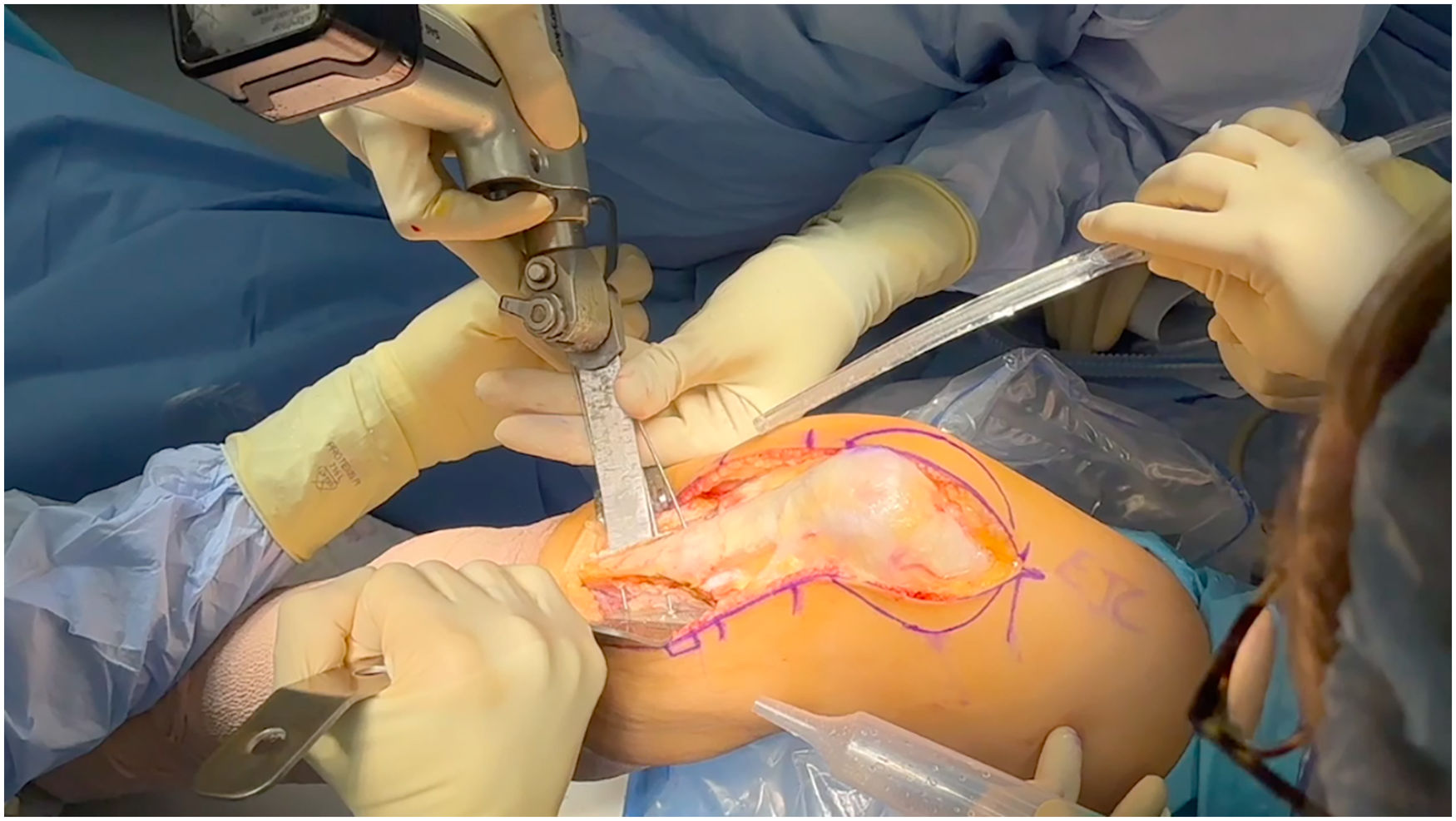
Keywords
Video Transcript
The following is a video on medial patellofemoral ligament reconstruction (MPFLR) with concomitant tibial tubercle osteotomy (TTO).
The following are the authors’ disclosures.
Background
Patellar instability is a prevalent condition with a devastating impact, especially among younger individuals. It has an incidence of 5 to 7 per 100,000 in the general population and 29 to 40 per 100,000 in adolescent patients,1,15 and it is often associated with medial patellofemoral ligament (MPFL) rupture.
Risk factors include trochlear dysplasia, patella alta, abnormal patellar tilt, limb malalignment, and increased tibial tubercle to trochlear groove (TT-TG) distance. 2 Nonoperative treatment has a 43.1% redislocation rate, with increased risk with younger age, contralateral instability, and trochlear dysplasia. 19
A variety of surgical options are available for addressing patellar instability, and the selection of each technique should be tailored to the unique pathoanatomy of each patient. MPFLR; tibial tubercle medialization, distalization, or both; trochleoplasty; and tibial or femoral osteotomies for correction of rotational or coronal plane malalignment may all be used either individually or in combination. 15
The following is a case involving a 22-year-old woman presenting with left knee pain and patellar instability.
The patient reports recurrent dislocations of her left patella, with at least 1 episode per month since childhood. Previously, these episodes were typically benign and painless. However, in recent years, these dislocations have become increasingly painful and imposed limitations on her activities of daily living. She presents with pain rated as 5 out of 10. She has attempted and failed conservative treatment, including physical therapy, bracing, and nonmsteroidal anti-inflammatory drugs, with no significant improvement.
On physical examination, her range of motion was from 2° of hyperextension to 140° of flexion. She exhibited a jumping J-sign and no retropatellar crepitus. She had 5 out of 5 strength in both quadriceps and hamstrings and showed no other signs of knee instability or gait abnormalities.
Preoperative plain anteroposterior, lateral, and sunrise view radiographs revealed no evidence of fractures or osteoarthritis. Imaging findings included a Caton-Deschamps index of 1.3 and mild trochlear dysplasia, along with a slight valgus alignment of the lower limbs.
Computed tomography (CT) scans confirmed a TT-TG distance of 26 mm and lateral patellar subluxation, along with an increased patellar tilt of 43° and femoral anteversion of 12°. No loose osteochondral fragments were observed.
In terms of surgical decision-making, the MPFLR is performed in cases of recurrent patellar subluxations or dislocations, to restore the medial stabilizing structure and reduce the risk of recurrent instability.
The indication for TTO encompasses malalignment concerns, in this case specifically, indicated by a TT-TG distance exceeding 20 mm.
Regarding lateral lengthening, an increased patellar tilt observed on CT imaging may indicate the need for the procedure. However, if persistent lateral retinacular tightness is observed after patellar relocation within the TT-TG at a 30° knee flexion angle, a lateral lengthening is recommended. This can be assessed through an intraoperative patellar tilt test.
Our surgical plan was for a knee arthroscopy and MPFLR with semitendinosus allograft, TTO, and possible lateral lengthening.
Technique Description
The patient was positioned supine. A bilateral examination was performed under anesthesia, including heel height, knee range of motion, and patellar tracking, confirming the presence of a jumping J-sign and patellar subluxation.
An anterior midline incision was marked from beyond the superior pole of the patella down the anterior tibial tubercle. The skin and subcutaneous tissue were incised. Subcutaneous flaps were elevated to expose the medial and lateral borders of the patellar tendon and to identify its insertion on the tibial tubercle.
A high anterolateral parapatellar portal was created and a diagnostic arthroscopy was performed. The patella demonstrated significant subluxation, and there was no significant chondral damage in any compartment. The notch demonstrated intact cruciate ligaments. The scope was also employed later, to ensure the precise positioning of anchor drilling, making sure that it remained extra-articular.
We then proceeded with the open TTO. Medial and lateral flaps were elevated, and the medial border of the anterior compartment was incised, with the musculature being gently mobilized laterally with a Cobb elevator.
The tibial tubercule was cleared by removing the periosteum from the medial and lateral aspects of the tubercule in a proximal-to-distal fashion.
Three 2.4-mm osteotomy guide pins were placed colinearly in a medial to lateral direction with a 15° obliquity, to avoid excessive anteriorization. A 6-cm TTO was then performed in a medial to lateral fashion and was completed after guide pin removal. A combination of different sizes of saws and osteotomes was used to free up the tibial tubercle. A 15-mm translation was performed at this point. Distally, the periosteum was left intact, allowing for a distal cortical hinge.
Medialization of the tibial tubercle was performed, and after the desired tubercule position was achieved, it was secured with 3 K-wires. Dynamic testing was performed and patellofemoral tracking was evaluated to ensure correct alignment and elimination of the J-sign.
Definitive fixation of the translated tubercle was then accomplished with three 5-mm cannulated self-tapping headless screws, placed from proximal to distal.
Intraoperative radiograph confirmed proper placement of screws for the definitive fixation of the translated tubercle.
Lateral lengthening was then performed by incising the most superficial lateral layer, as well as the lateral patellofemoral ligament (LPFL). The LPFL was then sutured to the superficial layer, achieving a lengthening of around 1 cm.
Next, a 2-cm incision was made in the superomedial aspect of the patella, and the medial patellar surface was carefully prepared using rongeurs until healthy bleeding bone was exposed. This preparation was essential to facilitate proper graft healing. We proceeded by placing 1 suture anchor at the 50-yard line and a second one at the superior aspect of the patella. After, a previously prepared semitendinosus allograft was placed centered in between the anchors. The graft was then tied with the sutures from the anchors.
A plane was then developed between the retinacular layer and the joint capsule, extending toward the insertion point of the MPFL on the femur. Both graft limbs were then pulled through this plane, from the medial border of the patella to the anatomic attachment of the MPFL.
Under fluoroscopic guidance, Schottle's point was identified and a guide pin was inserted.
The passing suture from the graft was loaded into the beath pin and pulled through a previously reamed femoral tunnel, docking the graft.
At this point, our graft was passed through the femoral tunnel and the holding sutures were gently tightened and secured from the lateral thigh.
The knee was then cycled through full range of motion while directly visualizing the graft. Motion around the graft was evaluated and, in case of an isometry, graft tension could be modified as needed.
Patellar mobility was examined in extension, aiming for 1 quadrant of lateral translation.
The graft was fixed at 30° of flexion, using a 7-mm peek screw, and a final patellar mobility check was performed.
Results and Discussion
Regarding complications, MPFLR with TTO has a complication incidence ranging from 4% to 13%, which is similar to that of isolated TTO.4,10 Complications include tibial fracture, patellar fracture, infection, nonunion, stiffness, instability, medial patellar subluxation, hardware removal, and arthrofibrosis.4-6,10,11,14,17
Tips and tricks for TTO include the use of 2 or 3 headless or cortical screws angled at 90° to the osteotomy plane for enhanced compression and union. 16 Avoid thermal necrosis, periosteal stripping, and creating an osteotomy shingle that is too thin (<8 mm). 12 Finally, preserve a distal cortical hinge. 7
For MPFLR, fix the graft in 30° to 45° of knee flexion to avoid graft tightness or laxity. 13 Ensure anatomic femoral graft placement with fluoroscopic guidance. 13 Use suture anchor fixation of the graft to the patella, which has been shown to have significantly lower complication rates than transosseous tunnels. 18
Patients can expect favorable outcomes, with up to 84% of patients being shown to achieve minimal clinically important difference for the Kujala score. 9
Combined MPFLR with TTO shows improved postoperative patellofemoral tracking and better patient-reported outcome measures compared to MPFLR in isolation in cases where bony morphology was altered. 3
There is a high return-to-sport rate, up to 92%, following both isolated MPFLR and with concomitant TTO, with an average return-to-sport time of 6.7 months. 8
Patients under 21 have lower rates of knee stiffness and complications. 10
Recurrence of instability postoperatively ranges from 0% to 13.5%.4,10,14
MPFLR with TTO shows lower revision rates at the 2-year follow up. 10
Regarding the postoperative rehabilitation protocol, during the first 6 weeks, the patient is advised to follow a strict touch-down weightbearing regimen with the assistance of crutches and a knee brace locked in the extension.
Between weeks 6 and 12, the patient can gradually advance to partial weightbearing, transitioning to weightbearing as tolerated at week 8. The knee brace can be unlocked, and crutches can be discontinued.
Between weeks 12 and 16, the patient aims to achieve a normal gait pattern with complete range of motion.
By week 16, the rehabilitation program should progress to closed-chain exercises, with an emphasis on enhancing dynamic and static balance on a single leg.
The following are our references.
Thank you for your time and attention.
Footnotes
One or more of the authors has declared the following potential conflict of interest or source of funding: A.B.Y. received research support from Arthrex and Organogenesis; has stock or stock options in Icarus Medical, Patient IQ, and Sparta Biomedical; was a paid consultant for AlloSource, JRF Ortho, and Stryker; was an unpaid consultant for Patient IQ and Sparta Biomedical; and was a paid presenter or speaker for Stryker. J.C. was a board or committee member for AOSSM, Arthroscopy Association of North America, and International Society of Arthroscopy, Knee Surgery, and Orthopaedic Sports Medicine; was a paid consultant for Arthrex, CONMED Linvatec, Ossur, and Smith & Nephew; and was a paid presenter or speaker for Smith & Nephew. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
