Abstract
Background:
Arthroscopic access to the hip can be challenging. We present a reproducible, safe, and efficient method for arthroscopic access to the hip. This can be especially beneficial for hips that may be predisposed to more difficult access.
Indications:
Hip arthroscopy is indicated in patients with symptomatic femoral acetabular impingement (FAI) who have failed conservative treatment options. FAI surgery aims to address both bony impingement and labral pathology in the hip.
Technique:
In this technique, we describe methodical steps to hip access. These steps include special attention to patient positioning and preoperative radiographs, air arthrogram, bevel control for needle joint entry, careful interpretation of intraoperative fluoroscopy, and adequate capsulotomy for viewing.
Results:
The majority of patients undergoing hip arthroscopy for FAI have improvements in both hip function and pain. Preoperative findings of increased center edge angle and male sex may predispose patients to more difficult hip arthroscopy access. The use of this technique may aid in reproducible access.
Discussion/Conclusion:
Hip arthroscopy is a good option for patients who have failed conservative treatment options and have signs and symptoms of FAI. Reproducible, safe, and efficient access to the hip is critical to starting hip arthroscopy cases.
Patient Consent Disclosure Statement:
The author(s) attests that consent has been obtained from any patient(s) appearing in this publication. If the individual may be identifiable, the author(s) has included a statement of release or other written form of approval from the patient(s) with this submission for publication.
This is a visual representation of the abstract.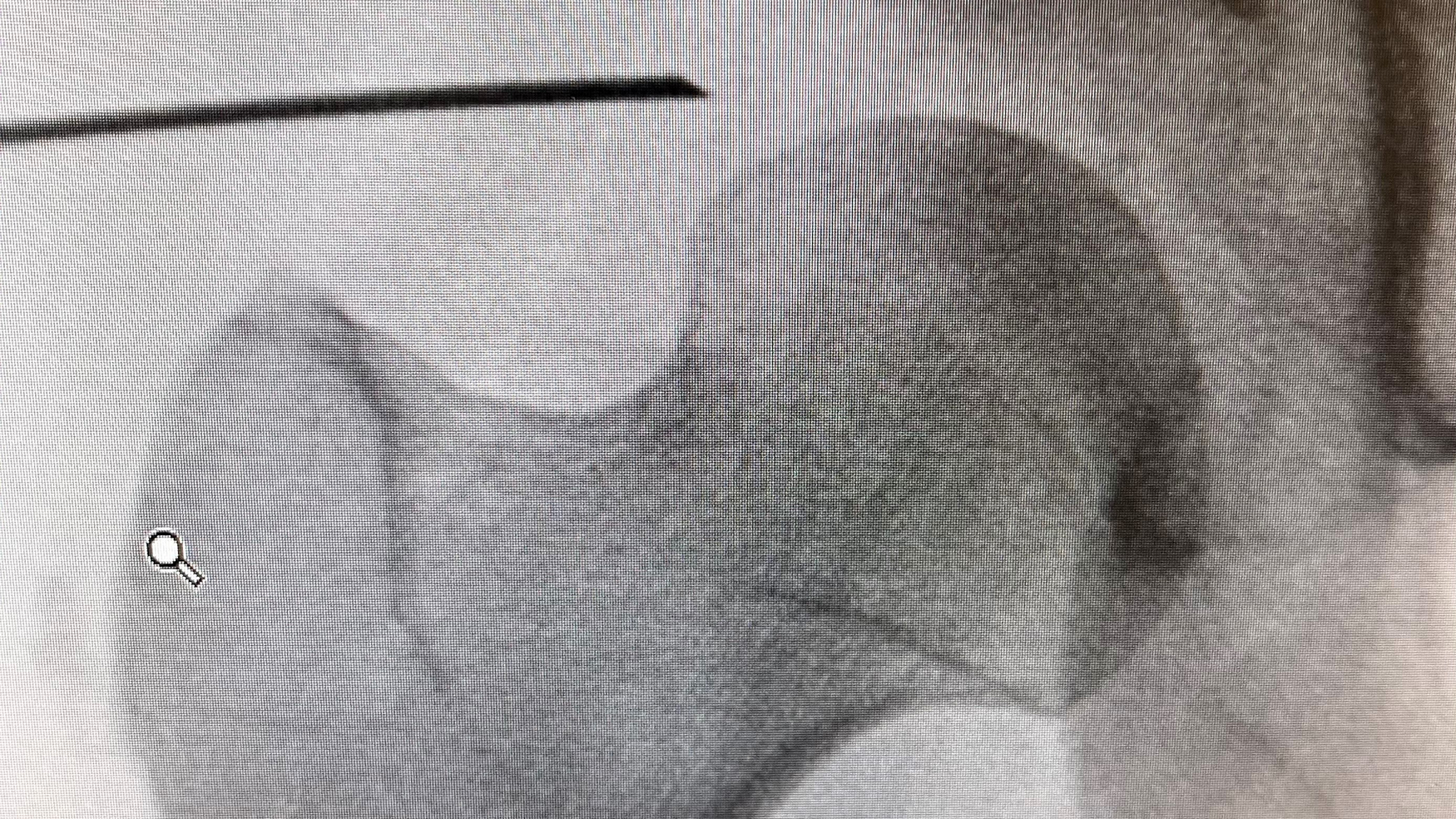
Video Transcript
In this video, we will describe a methodical and reproducible technique for optimizing access in hip arthroscopy.
These are our relevant disclosures.
As an overview, we will discuss general hip arthroscopy access goals, give a patient case presentation, and go over an in-depth description of our hip arthroscopy access technique.
Background
The goals of hip arthroscopy access are to perform a safe entry into the hip joint; to take care to avoid injury to neurovascular structures; to perform efficient access to decrease surgical and traction time on the hip; to have a reproducible reliable technique for access; and to obtain optimal portal placement for arthroscopic instrumentation.
The patient is a 41-year-old male who presented to the outpatient office with chronic left hip pain which had begun after a motor vehicle accident. The patient locates his pain to the groin and posterolateral aspect of his left hip and noted that it was worse in the mornings. He had failed conservative management including 6 weeks of physical therapy as well as an intra-articular steroid injection and anti-inflammatory medication. On physical examination, he had markedly limited internal rotation with the hip flexed to 90° and endorsed pain with flexion adduction and internal rotation of the hips.
A preoperative anteroposterior (AP) pelvis and 45° Dunn lateral showed an increased center edge angle of 45° and an alpha angle of 64°, indicating both pincer and cam deformities. Tang et al 5 recently showed that when evaluating preoperative radiographs, male sex and an increased center edge angle have been identified as risk factors for difficult central compartment access.
It is helpful to evaluate the labrum on multiple magnetic resonance imaging (MRI) series as volume averaging can lend itself to missed pathology if only viewed in one plane. Sagittal MRI images allow for evaluation of the anterior labrum. In this patient, he was noted to have an anterior and superior labral tear.
Coronal imaging shows both the anterior and superior labral arch, again confirming in this patient an anterior superior labral tear.
Byrd et al 1 described portal placement and their relationship to extra-articular structures. For this video, we focus on the anterolateral (AL) portal and the mid-anterior (MA) portal. The AL portal is relatively safe as the closest structure at risk is the superior gluteal nerve measuring an average of 4.4 cm from the portal. The MA portal is a nice adjustment from the anterior portal noted on Table 1 as it increases the distance from the lateral femoral cutaneous nerve which on average is only 0.3 cm from the standard anterior portal.
The major neurovascular bundle of the anterior hip is the femoral nerve, artery, and vein. At the start of the case, a line is drawn from the anterior superior iliac spine (ASIS) to the center of the patella. The greater trochanter is outlined and a second perpendicular line is drawn starting at the tip of the greater trochanter. The safe zone for entry is located lateral and distal to the intersection of these lines. Robertson and Kelly 3 assessed the safe zone for hip arthroscopy utilizing cadaveric specimens and found that out of the 11 portals described, only the anterior and MA portals are within 2 cm of a neurovascular structure. The anterior portal was noted on average to be 15.4 mm from the lateral femoral cutaneous nerve and the MA portal was on average 19.2 mm from the ascending branch of the lateral circumflex artery.
Technique Description
As part of our technique, we recommend performing an air arthrogram at the beginning of the case to aid in traction and distraction of the hip. We find that this allows for easier and less traumatic distraction. In a study by Zhang et al, 2 the added benefit of lower pain scores and decreased opioid dosages were seen during post-anesthesia care unit (PACU) stays in patients who had undergone air arthrogram.
Bevel control throughout access to the hip is imperative. As the hip joint is entered, if the bevel is facing cephalad, the labrum is less likely to be injured and there is less chance of the needle skiving on the capsule. On the contrary, if the bevel is pointed caudad, there is risk of skiving and puncturing the labral tissue. There is also a risk of penetrating the cartilage of the femoral head with this technique. If firm resistance is met while the spinal needle is cephalad, the needle should be repositioned to assure that the femoral head cartilage is not punctured.
When creating the AL portal, there is a tendency for the initial trajectory to drift too far anterior. As you can see on this fluoroscopic image, the needle has passed over the shadow of the capsule. If a guidewire is placed in this position, the wire will be stopped by the anterior wall of the acetabulum.
Prior to placing the entry needle, one should try to identify the outline of the labrum, the femoral head, the capsule, and the sourcil. The optimal entry point for the AL viewing portal is at the inferior 1/3 to 2/3 junction between the acetabulum and the femoral head. This allows space for the needle to clear the labral tissue and is also proximal enough to protect the femoral head cartilage. The needle tip should appear to “float” on the capsule prior to entering the joint. This places the portal in the optimal position in the anterior/posterior plane so that when the guidewire is inserted, it travels across the joint and ends in the cotyloid fossa.
Optimal arthroscopic access to the hip joint begins with patient positioning. The patient is placed in the supine position on a post-less traction pad. The operative hip should be positioned as close to the edge of the bed as safely possible and care should be taken to assure fluoroscopic images can be obtained with an unobstructed view. The ipsilateral arm is placed across the chest resting on a pillow with gel pads around the elbow to pad bony prominences.
Fluoroscopic baseline views of the hip are obtained. These views include AP, AP with 15° internal rotation, 45° Dunn lateral, 90° Dunn lateral, frog lateral, and a flexion adduction internal rotation view. 4 The hip is then placed in full extension with slight internal rotation to allow for the longest view of the femoral neck possible and one should note a “clean” view of the greater trochanter without overlap. Always utilizing this position to start the case allows the surgeon the consistency of knowing that the femoral neck is parallel with the floor. The patient is then placed in 3° to 5° of Trendelenburg and gross traction is applied until moderate resistance is met (this is generally about 50 lbs for women and 75 lbs for men).
The hip is prepped and draped in sterile fashion. A line from the ASIS to the center of the patella is drawn. The greater trochanter borders are traced and a line perpendicular to the tip of the greater trochanter is drawn from the previous longitudinal ASIS line. Staying distal and lateral to these lines delineates the “safe zone” for portal placement.
An air arthrogram is performed to aid in hip access. A 17-gauge long spinal needle is placed across the skin and a fluoroscopy image is used to mark the trajectory of the needle along the femoral neck. The needle is pierced through the skin in the region of the distal AL portal, and following the previously noted trajectory, the needle is advanced until contact with the femoral neck within the capsule. A 30-cc syringe of air is inserted into the joint while an assistant pulls fine traction. A second syringe of air is often needed.
Attention is then turned to the AL portal located 2 cm anterior and proximal to the tip of the greater trochanter. The spinal needle should be laid across the skin and fluoroscopy used to trace the path of the needle into the joint. The spinal needle should be parallel to the acetabular sourcil. The bevel of the needle prior to capsular penetration should face cephalad. Fluoroscopic views should be obtained and needle position should be scrutinized until the tip of the needle appears to be “floating” on the capsule and is entering at the inferior 1/3 to 2/3 of the space between the sourcil and the femoral head. After piercing through the capsule, the needle should be turned 180°. A 30 cc of sterile saline is injected into the joint and the needle is pulled back from the capsule so that the fluid stays intra-articular. Repeat fluoroscopic imaging should show that the air-filled intracapsular space is now radio-dense with fluid. The process of capsule entry with the spinal needle should be repeated with fluoroscopic guidance. When the stylet is removed after joint entry, pressurized saline should extravasate, and then a nitinol wire is inserted. Fluoroscopy should show the nitinol wire passes easily into the joint and sits deep in the cotyloid fossa. If the surgeon finds that the position of the wire is not bottomed out in the cotyloid fossa, then the spinal needle should be removed and repositioned. Once appropriate nitinol wire position is confirmed, the skin should be incised along the wire and a cannulated viewing cannula is inserted. A co-linear twisting motion with large turns of the cannula is used to enter the joint (as opposed to simple forward pressure) and a gentle giving way can be felt after passing through the capsule. Care should be taken to make sure that the nitinol wire glides easily during this portion as it can easily bend during the entry process. The inner trocar of the viewing cannula should be removed with the nitinol wire simultaneously and the end of the wire is checked to make sure it is intact.
A 70° arthroscope is inserted into the AL viewing portal in a dry fashion and attention is turned to creating the MA portal. The arthroscope should be focused on the triangle created by the femoral head, labrum, and anterior capsule. The MA portal is located slightly distal and about a hand breadth medial to the AL portal. The spinal needle bevel is oriented toward the ceiling and is aimed about 10° proximal and toward the patient's sacral region. The spinal needle should enter the triangle under direct arthroscopic visualization. The stylet is removed and a nitinol wire is placed. The skin is incised along the nitinol wire. Another cannulated viewing cannula is placed over the guidewire. The wire should be checked frequently. Once the viewing portal enters the joint, the wire can be removed and the trocar advanced.
Once the MA viewing cannula is in position, the camera should be removed from the AL viewing portal and immediately placed in the MA portal. The camera light cord should be turned so that that the viewer is looking straight down on the AL cannula. The labrum is assessed to assure no injury occurred during placement of the AL portal (portal position should be adjusted prior to starting the capsulotomy if labral injury has occurred). A capsulotomy knife is inserted into the AL portal and the viewing cannula is removed for greater excursion of the knife. The capsulotomy is started by incising the capsule toward the camera in the MA portal until the surgeon touches the MA cannula. The AL cannula is then placed on top of the capsulotomy knife to re-establish access, and the arthroscope is placed back into the AL portal. The light cord should then be spun so that the view is looking directly up at the MA cannula. The capsulotomy knife is inserted and MA cannula removed. The capsulotomy is finished by cutting toward the AL cannula and meeting the previously incised capsule edge. An arthroscopic cautery device is used through the MA portal to tidy the edges of the capsulotomy for better definition and later repair. The arthroscopic cautery device can then be used to assure complete capsulotomy and to clear soft tissue adhesions from the extra-articular side of the capsule to allow for better viewing and excursion during the case.
Results and Discussion
Here are postoperative AP and 45° Dunn lateral views showing the successful correction of bony impingement.
In summary, consistent and reproducible arthroscopic access to the hip starts with patient positioning. We recommend internally rotating the hip so that the longest view of the femoral neck is seen and there is a clean view of the greater trochanter. Air arthrogram is helpful for distraction. Entering the joint with the needle bevel cephalad and then after entry turning the bevel 180° caudad is helpful to avoid labral and chondral injuries. Finally, accurate interpretation of fluoroscopic views is essential.
Thank you for viewing this video.
Footnotes
Submitted September 20, 2023; accepted February 28, 2024.
One or more of the authors has declared the following potential conflict of interest or source of funding: F.W.G. is a pain consultant for Allosource and Stryker Sports Medicine; is a paid presenter/speaker for Arthrex Inc; is a board or committee member for AOSSM; and receives publishing royalties from Saunders/Mosby-Elsevier. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
