Abstract
Blood transfusion services maintain quality practice through adherence to guidelines but are faced with blood component wastage due to multiple factors. One factor, in particular, is poor ordering and utilization practices followed by physicians who may not be familiar with the indications and the optimal conditions for the handling of blood products. This study evaluates whether an educational intervention would help reduce ordering of plasma and improve wastage rates after thawing. The study followed a quasi-experimental pre-test post-test design. A multifaceted educational intervention was introduced at a tertiary hospital-based combining predisposing, enabling, and reinforcing activities, based on the literature of effective continuous professional development. The activities included a brief survey to evaluate participant knowledge about indications of plasma and its storage condition, a lecture, and periodic reports and reminders sent to all department heads in the hospital. Respondents to the survey and lecture attendees included physicians in adult critical care and anesthesia departments. Monthly plasma utilization and wastage rates were compared before and after introducing the intervention. Sixty physicians participated in the survey. The questions were answered correctly by less than half. After introducing the intervention, monthly plasma transfusion rates decreased; however, wastage rates did not improve. There is a knowledge gap among physicians who order plasma. The educational intervention resulted in lower plasma transfusion rates but did not affect wastage rates. Future interventions would benefit from including physicians in other departments as well as nurses.
Introduction
Much needed units of fresh frozen plasma (FFP) are sometimes wasted at high rates owing to suboptimal transfusion practices. 1 In blood banks, plasma (FFP) is stored frozen for 1 to 7 years. FFP units are thawed over 30 min, when requested for transfusion, and then can be kept between 1 °C and 6 °C for 24 h. Units that are not used within those 24 h or not kept at the required temperature (1 °C–10 °C) are discarded. 2
To maintain high standards, blood transfusion services (BTS) rely on quality indicators 3 and collect data regularly for presentation to management and other stakeholders. These quality indicators include wastage as percentage of issue (WAPI), calculated as the percentage of wasted blood units divided by the number of units issued for transfusion (including those wasted after being issued).1,4 Compared with the benchmarking rate of 1.5%, 5 high wastage rates of FFP have been noticed in the past few years in our center, ranging from 6% to 10%, 6 and sometimes as high as 20%.
In an international survey including 30 countries, Yazer et al calculated median WAPI values according to geographical region. For Europe, median WAPI values were as follows: RBCs 1.6%, platelets 3.3%, and plasma 2.7%; for North America: RBCs 1.3%, platelets 2.9%, and plasma 5%; and for the rest of the world: RBCs 2.4%, platelets 7.2%, and plasma 5.7%. They noted that percentages varied among centers; for example, plasma WAPI ranged between 0% and 29.2%. According to their results, most participants (91.8%) implemented strategies to reduce wastage. 7
Several interventions have been suggested in the literature to reduce blood component wastage, and communication was a common recommendation. In one study, follow-up communication with ordering physicians to enquire whether ordered components should continue to be held for their patients was proven to be effective. 8 A center in Houston implemented an educational intervention for health care professionals caring for coronary artery bypass graft patients that included a presentation, information handouts, educating key practitioners, regular sharing of data reports, and communicating with ordering physicians through letters when ordered transfusions do not follow recommended guidelines. As a result, utilization of blood products was reduced by 14% over one year. 9 Stanger et al also recommended communication, including information on inventory levels and anticipated needs. 10
Blood component wastage is multifactorial, and one particular factor is inappropriate ordering of FFP by physicians who may not be familiar with appropriate indications or proper handling and storage. Knowledge gaps in transfusion practices have been documented among students, postgraduate trainees,11,12 as well as practicing physicians.13,14 One underlying cause is that physicians not specializing in transfusion medicine do not receive enough education on the specialty during their academic years or clinical practice. 15
Alamri et al assessed knowledge among surgeons and surgical trainees, at our center, of transfusion practices and regulations. They found highly variable responses; most participants did not recognize serious transfusion adverse effects and many followed ordering practices that did not comply with practice guidelines. The authors recommended providing surgeons with continuing professional development education to raise their awareness in this area. 14 No regular education in transfusion medicine is provided to physicians or trainees at our center, a likely contributing factor to the high rates of in-date FFP wastage observed, which markedly exceed benchmarking levels. Wasting this precious resource, no doubt, brings with it financial losses. 1
In this study, an educational intervention was designed based on principles of effective continuous professional development programs (Table 1). The educational intervention was then introduced targeting practicing physicians involved in ordering FFP as part of their practice, with the aim of decreasing ordering practices that do not follow guidelines and improving FFP in-date wastage rates. 1
Attributes of Effective Continuous Professional Development Activities.

We present the following article in accordance with the SQUIRE 2.0 reporting checklist.
Materials and Methods
Following a quasi-experimental, pretest post-test design, this study was conducted at a 780-bed hospital considered a reference center for adult and pediatric cardiac surgery. According to transfusion services records, most orders for FFP come from critical care, and anesthesia departments. All physicians from those departments were invited to participate. All non-physician health care specialists and pediatric critical care physicians were excluded. 1
Outcome Variables
The following outcome variables were collected: Number of FFP units ordered, transfused, wasted, and calculated FFP WAPI. WAPI is calculated as the percentage of wasted units divided by the number of units issued for transfusion (including those wasted after being issued). The percentage of physicians who answered questions correctly on the pre-education survey was also collected.
Intervention
The continuing professional development intervention was designed based on the medical education literature describing features of effective continuous professional development activities and included three elements: predisposing, enabling, and reinforcing. 16 For the predisposing element, an email was sent to participants to introduce the problem of FFP wastage, invite them to attend the lecture, and provide them with a link to the survey. The survey was electronic and anonymous and comprised two multiple-choice questions: (Q1) After thawing FFP for transfusion, how long can it be stored in the refrigerator (1 °C–6 °C) before it expires? 4, 6, 24, or 72 h. (Q2) In a patient with disseminated intravascular coagulation, which international normalized ratio (INR) level would prompt you to request FFP transfusion before surgery? ≥1.3, ≥1.5, ≥1.8, or ≥2. Based on local guidelines, the correct answers were 24 h for Q1 and ≥1.5 for Q2. Results of the survey were shared during the lecture to reinforce awareness of the knowledge gap. The lecture (enabling element), a 30-min PowerPoint presentation, summarized results of the survey and presented data from hospital records showing percentages of appropriate orders of FFP as well as the problem of FFP wastage, its causes, and suggested solutions. Participants were given 30 min afterwards for discussion, questions, and to give their feedback. Feedback was also collected using an evaluation form. These activities were repeated on three occasions in 2018 to capture the highest number of participants.
For the reinforcing element, reports were sent every two months to all clinical department heads showing data on numbers of FFP units ordered, transfused, or wasted as well as reminders of FFP storage conditions and shelf-life along with suggested strategies to improve utilization. 1
Only critical care and anesthesia department staff were sent email and invited to participate in the lecture and survey; however, the periodic reports were distributed to all departments. For the study, plasma transfusion and wastage rates were collected from the BTS’ paper records and the Laboratory Information System. 1
Statistical Analysis
Statistical analysis was performed using t-test to compare the mean difference between the 12 months preceding and the 12 months following the intervention.
Results
A total of 60 physicians participated in the lecture and survey. Among them, 18 (30%) answered question 1 correctly and 22 (37%) answered question 2 correctly.
The average number of FFP units transfused per month was 357 units during the 12 months prior to introducing the intervention (March 2017 to February 2018), and 270 units after initiation of the intervention (from March 2018 to February 2019; Tables 2–4, Figure 1). The average number of FFP units transfused per month dropped by 24% (357 to 270 units) in the 12 months following the intervention. For the two 12-month comparison before and after intervention, there is a significant reduction in the mean number of units transfused monthly, a mean monthly reduction of 87 units, P = .010. This reduction reflects a large effect (Cohen's d = 0.89), demonstrating the meaningful impact of the intervention.

Number of transfused FFP units over 12 months before and after introducing the intervention.
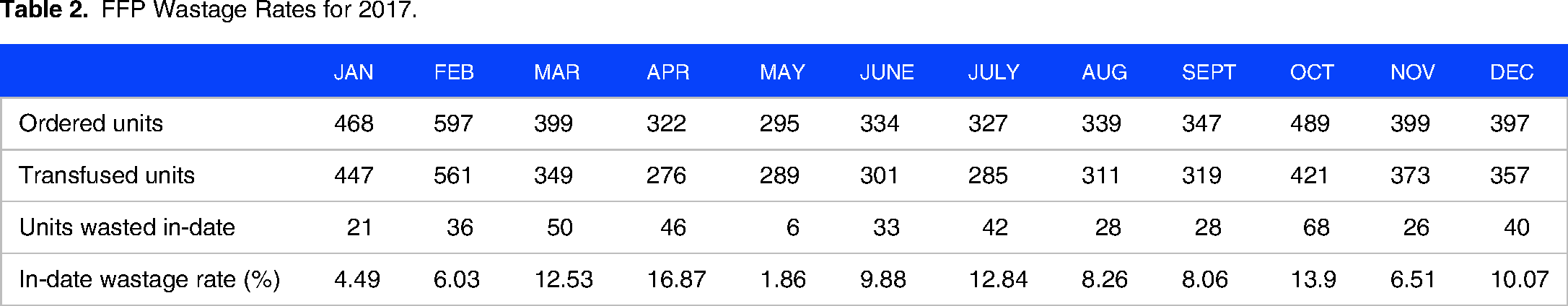
FFP Wastage Rates for 2017.
FFP Wastage Rates for 2018.

FFP Wastage Rates for 2019.

Average monthly ordering rates of red blood cells were also compared for the 12 months before and after the intervention to ensure that the above percentage did not result from a change in patient numbers or a drop in blood product utilization; red blood cell ordering was almost identical (1365 and 1364 units). 1
As shown in Tables 1–3, the average monthly FFP in-date wastage rates were 9.28%, 13.2%, and 13.8% for 2017, 2018, and 2019, respectively.
Discussion
Apart from an introductory lecture given to new house officers (final year of medical school), physicians in our center do not receive systematic mandatory instructions on transfusion medicine. And although nurses receive comprehensive annual training in blood transfusion procedures and competency assessment, the former does not include indications for transfusion or shelf life of blood components. Results indicate that healthcare providers require systematic education on transfusion medicine. This would be helped by the designation of a transfusion medicine staff member to deliver teaching or the hiring of a transfusion safety officer. 17 The institution may also provide access to relevant online resources such as Bloody Easy, 18 Clinical Guide to Transfusion, 19 and Transfusion Medicine for Physicians. 20
Achieving outcome changes can be difficult through continuing professional development 21 ; however, outcome predictors, assessment of knowledge gaps, and utilizing multifaceted elements 22 were used in this study. Despite the drop in FFP utilization, which may have resulted from better compliance with transfusion indications, FFP wastage rates did not show significant improvement. This may be a result of restricting the lecture and prelecture survey to only anesthesia and critical care staff, since wastage rates incorporate results from all hospital departments and not just those targeted in this study. Relying on a multifaceted educational approach is key, and monitoring may prove just as valuable as education in ensuring implementation. 23 Feedback taken from participants in this study showed that FFP is often ordered as a precaution (or “just in case”) and may not be utilized. Process changes that can help to reduce wastage may include thawing only half of the ordered number of units, then thawing the remaining half when the units are picked up for transfusion; and introduction of thawed plasma (stored in the refrigerator for a total of 5 days after thawing). Thawed plasma can be used in place of FFP except in cases requiring factor V or VIII replacement.24–26 Studies have shown reduction in FFP wastage by the utilization of thawed plasma.25,27 Validation studies, to confirm that coagulation factors are maintained during the process, are being performed in our center before implementation. Results from initial studies have been presented at the International Society for Blood Transfusion Congress in 2020. 28
In a cost analysis done in the United States, the acquisition cost for one unit of FFP was $41.9. In our center, the average number of wasted FFP units per month was 43, translating into a loss of $1808 per month. 29 Detailed cost analysis reports for transfusion services are not published in Saudi Arabia. The sharing of such reports with relevant stakeholders (hospital management, department heads, and physicians) may help in affecting change in attitudes and practices to improve how blood products are ordered and utilized. For example, reducing FFP transfusions by an average of 87 units per month, would lead to monthly savings of over $35 000. Furthermore, a major advantage of sharing unit wastage data with ordering physicians would be to establish a greater sense of responsibility when ordering blood and its components. And although periodic communication with departments may prove to be helpful, real-time feedback, within 24 h, with ordering physicians would have greater impact. Sharing of data and reports was accomplished through a hospital transfusion committee, composed of representatives from the different hospital departments involved in ordering or carrying out blood transfusions. Formation of a multidisciplinary subcommittee to be tasked exclusively with finding solutions for the FFP wastage problem would have also been helpful.
Limitations
Perhaps limiting the intervention to physicians in specific departments was the reason wastage rates did not improve, and targeting a wider group of healthcare providers should be considered. This may also highlight the importance of introducing process change to support the educational intervention.
This study did not look into participant level of training; however, only postgraduate trainees and physicians were included. Also, the outcome of the study focused on institutional changes. Changes in participant knowledge, attitude, and behavior were not assessed as part of the investigation but are to be included in future projects. Furthermore, the inclusion of nurses in the intervention may have produced better results, because they are involved in the transfusion process, if not in ordering. We did not assess individual participant knowledge gain or changes in their attitude or behavior after exposure to the intervention. Future projects are planned to include assessment of all Kirkpatrick levels. 30
Our project was limited to improving FFP ordering practices. A single blood component was chosen to provide ordering physicians with succinct, specific, and actionable recommendations. However future projects are planned to focus on other blood components as ordering practices will likely require optimization.
Conclusion and Recommendations
There is a knowledge gap among physicians in transfusion practices. A multifaceted educational intervention was introduced targeting physicians to help reduce FFP utilization and wastage. FFP transfusion rates decreased after implementation of the intervention; however, wastage rates did not improve significantly. Healthcare providers should receive continuing professional development education on transfusion practices regularly, and its completion could be linked to their annual evaluation. This education needs the support of process changes aiming to reduce FFP wastage. The issue of FFP wastage needs further exploration using qualitative and quantitative methods.
Footnotes
Acknowledgments
The authors would like to thank the Department of Medical Education and the Department of Anesthesia and Critical Care in the Faculty of Medicine, King Abdulaziz University. The authors would also like to thank Dr Suzan Alkhodair for editing the manuscript. This work was presented as thesis to King Abdulaziz University to meet the requirement of Master of Medical Education program.
Author contribution
Data Availability
All primary data can be provided by the corresponding author if required.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
Not applicable.
Informed Consent
Not applicable.
