Abstract
Background:
Healthcare systems have become increasingly institutionalized, distancing death from everyday life and limiting community capacity to support dying and bereavement. Compassionate Communities (CCs) aim to address this gap through a public health approach to palliative care. Evidence on their development and evaluation remains limited, particularly in Southern Europe.
Objectives:
To describe the co-creation process of the first Italian CC and outline an evaluation framework to guide implementation and sustainability.
Design:
Participatory, mixed-methods protocol covering the first two phases of the InVita! project: (I) Discover and assess and (II) Focus and commit.
Methods and analysis:
Phase I will map local needs and resources through semi-structured interviews with interest-holders, focus groups with caregivers, and reflexive field diaries. A descriptive survey of adult residents will assess knowledge of palliative care, attitudes toward death, perceived self-efficacy, and community engagement. The survey adapts an existing instrument and incorporates death literacy dimensions, with cultural adaptation through interest-holder review. Phase II will translate findings into a shared mission and prioritized actions via participatory workshops and a community awareness event. Data will be analyzed using reflexive thematic analysis for qualitative data and descriptive statistics for survey data. Integration will follow GRAMMS guidelines.
Ethics:
The study was reviewed by the Comitato Etico Area Vasta Emilia-Nord, which determined that formal approval was not required due to its noninterventional nature. All participants will provide informed consent, and data will be anonymized in compliance with GDPR.
Discussion:
This protocol introduces a structured, participatory approach to developing Italy’s first CC. By integrating qualitative and quantitative methods and embedding public involvement, the study aims to generate actionable insights for scaling CC initiatives and advancing public health palliative care.
Trial registration:
Not applicable.
Plain language summary
Serious illness, dying, and grief affect everyone, yet these experiences are often hidden from everyday life. This can leave families feeling isolated and unsupported. Compassionate Communities is an approach that brings care back into the community, encouraging people, organizations, and services to collaborate in supporting those at the end of life.
This project, called InVita!, is the first attempt to create a Compassionate Community in Italy. We will collaborate with local residents, volunteers, and health and social care professionals to identify existing support and gaps in services. We will use interviews, group discussions, and a community survey to gather information about individuals’ knowledge, attitudes, and confidence in helping others at the end of life.
The results will guide practical actions, such as awareness campaigns and support networks, to make care more inclusive and sustainable for everyone in the community.
Keywords
Background
Over the past century, healthcare systems in high-income countries have shifted from community-based care to highly professionalized and institutionalized models, profoundly affecting end-of-life care. 1 While this transition has improved access and clinical outcomes, it has also distanced death from everyday life, eroding communities’ capacity to support dying and bereavement.
The Lancet Commission on the Value of Death describes this as a paradox: death and dying have become “unbalanced,” dominated by medical interventions and removed from social and cultural contexts. 2 The report argues that modern societies have lost sight of the value of death itself, not merely the process of dying. Death, the Commission states, is integral to life: “Death and life are bound together: without death there would be no life. Death allows new ideas and new ways. Death also reminds us of our fragility and sameness: we all die” 2 (p. 837). Rediscovering this value, the report suggests, can transform end-of-life care and enrich life itself. To achieve this, the Commission calls for a radical rebalancing of “death systems”—the social, cultural, economic, and political structures that shape how death, dying, and grief are experienced—guided by five principles, including recognizing death as valuable and embedding care within relationships and communities. 2
Palliative care (PC) plays a crucial role in addressing these challenges by providing comprehensive support for individuals with serious illnesses and their families. 3 However, demographic changes, chronic disease trajectories, and evolving family structures have created complex needs that exceed the capacity of health services alone.4,5 Increasingly, families face prolonged caregiving responsibilities, often with limited social support,6,7 resulting in significant emotional and financial strain.8–10
To address these gaps, scholars and practitioners advocate for a public health approach to P, 11 grounded in community engagement, 12 and shared responsibility.13,14 Compassionate Communities (CCs) are grounded in this approach, first theorized by Allan Kellehear 4 and inspired by the WHO’s Ottawa Charter for Health Promotion. 15 They are defined as communities that recognize that “all-natural cycles of sickness and health, birth and death, and love and loss occur every day within the orbits of their institutions and regular activities” (p. 1).13,16 Care in such communities is understood as everyone’s responsibility, not solely that of health services. Unlike the broader notion of Caring Communities, which addresses a wide range of social and health needs, CCs focus specifically on serious illness, dying, death, and grief, fostering collective responses across civic, cultural, and social life. 13
Existing evidence highlights both the promise and the challenges of CC implementation. Librada-Flores et al., 17 in a systematic review, identified diverse models worldwide but noted that most initiatives lack standardized frameworks and robust evaluation strategies. This heterogeneity complicates comparisons and limits the transferability of lessons learned. Similarly, Dumont et al. 18 observed that published evaluations often focus on isolated activities—such as volunteer training or awareness campaigns—rather than the systemic processes underpinning CC development. These gaps underscore the need for comprehensive protocols that document both process and outcomes.
Recent theoretical contributions have advanced the understanding of CCs as complex interventions. Bakelants et al. 19 argue for the application of implementation science frameworks to capture the dynamic interplay of contextual factors, interest-holder engagement, and adaptive strategies. However, empirical applications of these frameworks remain scarce, particularly in Southern European contexts where health systems and community structures differ significantly from those in Anglo-Saxon countries.
International experiences provide valuable insights into key success factors. 20 Gómez-Batiste et al. 21 describe the Vic (Barcelona) model in Spain, which emphasizes phased development, interest-holder coalitions, and integration with municipal policies. While this model demonstrates feasibility, its replication requires adaptation to local socio-cultural and institutional contexts. Similarly, Quintiens et al. 22 published the first protocol combining process and outcome evaluation for two Compassionate Cities in Belgium, highlighting the importance of mixed-methods designs and co-creation approaches. Yet, such protocols remain rare, limiting opportunities for cross-contextual learning.
Our study addresses these gaps directly. It documents the co-creation of the first Italian CC, applying a structured, phased approach inspired by international models but tailored to the Italian health system and community assets.
Over the years, our hospital-based PC unit has recognized the need to extend its work beyond the hospital setting to change perceptions of PC23,24 and increase public awareness. Stigma surrounding death often contributes to delayed referrals for patients with PC needs. 3 In practice, we also observed that resources outside the formal health system—such as voluntary associations, widely present in the province of Reggio Emilia—were underutilized by patients attending our Cancer Center.
The province of Reggio Emilia (Emilia-Romagna Region, Northern Italy) offers a relevant context for this initiative. In 2021, 5819 people died, 25.5% of whom were oncological patients. Approximately 80% of deaths were associated with PC needs, and 40%–45% required specialist PC due to complex social and clinical conditions such as poverty, isolation, or limited access to services. Despite a specialized and longstanding PC network, only about 30% of deaths in the municipality of Reggio Emilia occurred at home. (https://salute.regione.emilia-romagna.it/normativa-e-documentazione/rapporti/atlante-di-mortalita/atlante-di-mortalita).
This territory also provides favorable conditions for community-based innovation: small to medium-sized municipalities (around 20,000 inhabitants), prior experience with social change projects, and a primary care network integrated with local municipalities and voluntary associations. These features informed the selection of the hilly area of Reggio Emilia as the site for developing the first Italian CC.
To address these challenges, we explored international experiences of citizen participation and public health approaches in PC20,25,26 and initiated dialogue with local charitable organizations serving patients with incurable diseases. Consistent with recommendations in the literature, 17 we adopted an asset-based approach rather than a deficit-based model, focusing on leveraging community resources to complement healthcare services, particularly at the end of life. 27 This perspective calls for reorienting PC toward shared responsibility among health systems, social services, and local communities. 14
Building on this foundation, the hospital PC unit partnered with CSV Emilia—a third-sector organization that coordinates most voluntary associations in the area—to engage local interest-holders and residents in co-creating the first Italian CC. This initiative, named InVita!, is structured into four iterative phases adapted from the Vic model 21 :
– Phase I—Discover and assess: Identify needs, resources, and existing initiatives; engage interest-holders and citizens.
– Phase II—Focus and commit: Define the project’s mission, purpose, and objectives through participatory workshops.
– Phase III—Build and launch: Implement co-designed activities to activate the CC in the target area.
– Phase IV—Evaluate and sustain: Conduct quantitative and qualitative evaluation and plan for long-term sustainability.
This protocol specifically describes the first two phases—Discover and assess, and Focus and commit—which lay the groundwork for subsequent implementation and evaluation (Table 1).
Overview of InVita! project phases and key actions.

Methods
Study design
This study will adopt a participatory, mixed-methods design to document and evaluate the first two phases of the InVita! project, which aims to co-create the first Italian CC. The design will combine qualitative inquiry (semi-structured interviews, focus groups, and reflexive field diaries) with a descriptive, cross-sectional survey of residents in the target municipalities.
The qualitative strand will explore local resources, needs, and experiences related to serious illness, caregiving, dying, and bereavement, while fostering co-construction of priorities with interest-holders. The survey will provide a population-level descriptive profile of knowledge, attitudes, and community engagement to inform planning and outreach strategies.
Reporting will follow GRAMMS 28 to ensure transparency in describing the rationale for mixing, strand-specific methods, and integration, and GRIPP2-SF 29 to document patient and public involvement (PPI) throughout the research process. The design is informed by mixed-methods principles30,31 and incorporates a process evaluation to assess sociocultural relevance, the identification of health priorities, and community ownership.32,33
Development process
Phase I: Discover and assess
Phase I will aim to build a shared understanding of local needs, resources, and experiences related to end-of-life care. Activities will include:
– Formation of a partnership group comprising health and social services, voluntary associations, municipal actors, and caregivers/experts-by-experience.
– Semi-structured interviews with interest-holders to explore organizational roles, existing supports, gaps, and expectations for the CC. 22
– Focus groups with caregivers to capture lived experiences, barriers, and enablers in providing end-of-life support.
– Reflexive field diaries maintained by researchers and partners to document engagement dynamics and co-construction processes.32,34
– Feedback sessions to validate findings and collaboratively identify priorities.
– Descriptive survey among adult residents (⩾18 years) of the same municipalities to map knowledge of PC, attitudes toward death, perceived self-efficacy, and community engagement. The survey instrument will be adapted from the Bruges study 22 and will incorporate dimensions from the Death Literacy Index, 35 which measures knowledge, skills, and experiential understanding related to death and dying. This adaptation will be co-reviewed with interest-holders for cultural relevance (see Figure 1).
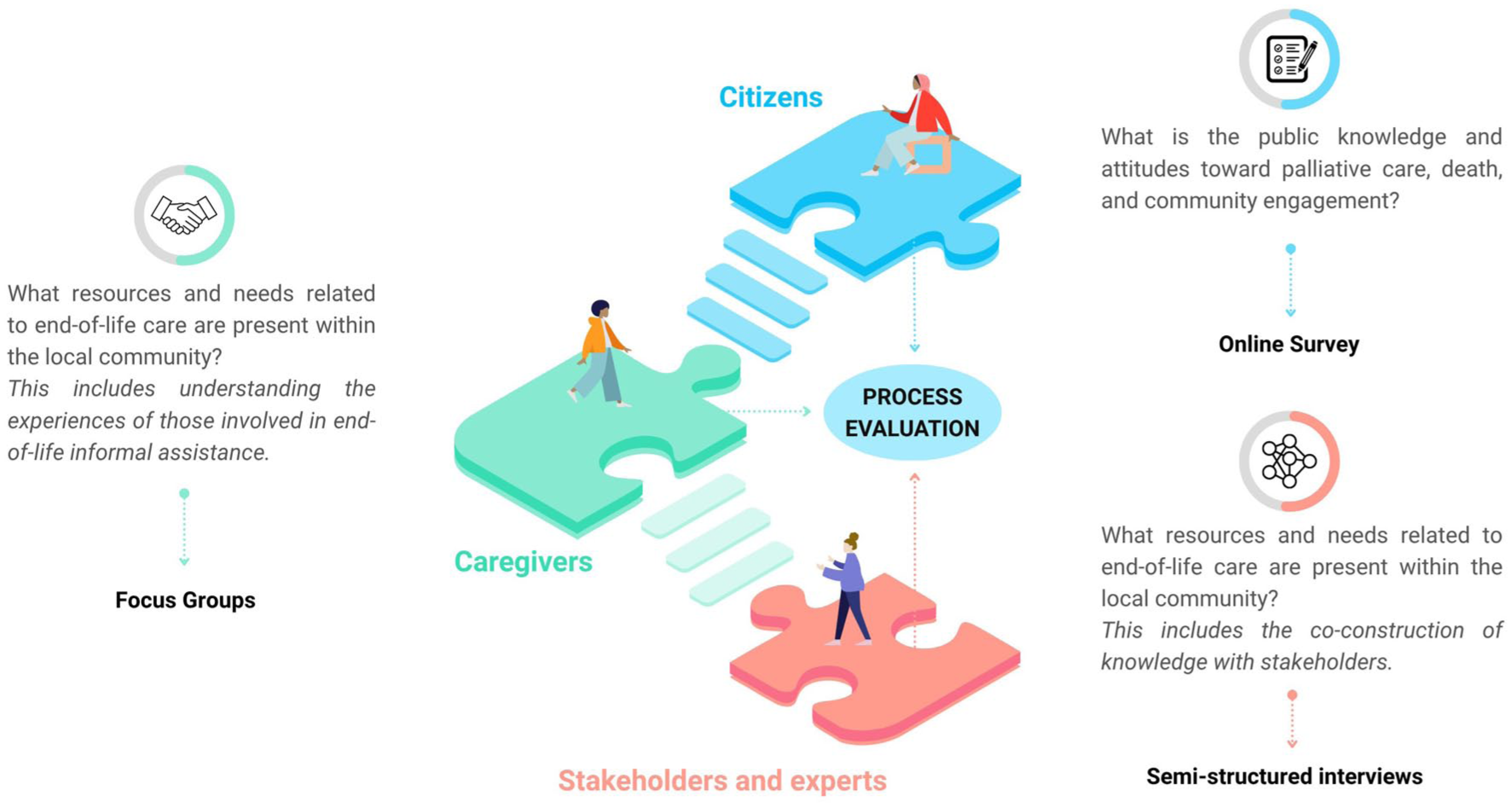
Phase I data sources.
Phase II: Focus and commit
Phase II will translate the insights from phase I into a shared mission and a prioritized set of actions. A start-up assembly will present qualitative themes and survey findings, enabling structured deliberation on feasibility and equity. Partners and citizens will co-define short-, medium-, and long-term priorities (e.g., awareness campaigns, grief support, and volunteer connector networks). A community awareness event will communicate the emerging vision and invite broader participation. All decisions and adaptations will be documented in accordance with GRIPP2 principles to evidence the impact of PPI on the process. 29
Participants and recruitment
Participants will be approached through multiple community-based channels to maximize reach and inclusivity. Specifically, we will disseminate invitations via municipal communication platforms (e.g., official websites and newsletters), health community centers (Case della Comunità), and local voluntary associations. In addition, information will be shared during civic events and through posters in public spaces (e.g., libraries, pharmacies, and community halls). The survey will be accessible both online (via a secure REDCap link) and in paper format at community venues to minimize digital exclusion.
Based on this assumption, a sample of approximately 385 respondents across municipalities will yield a ±5% margin of error at 95% confidence for the combined population. To allow municipality-level reporting, we will aim for 200–250 respondents per municipality, corresponding to a precision of approximately ±6%–7%. Recruitment will be monitored weekly, with booster outreach (e.g., additional paper sessions, targeted reminders) as needed. Because the survey is descriptive, the emphasis will be on precision of estimates, rather than hypothesis testing.
Data collection
Data analysis and integration
Patient and public involvement
PPI will be embedded throughout. Partners, caregivers, and residents will contribute to instrument design, recruitment strategies, and interpretation of findings. We will report who was involved, how, at which stages, and what changed as a result of involvement (e.g., rewording survey items and prioritizing grief support). Challenges and lessons learned will also be documented. 29
Ethics and data management
The study has been submitted to the Comitato Etico Area Vasta Emilia-Nord (AVEN) for review. In accordance with current Italian regulations governing noninterventional research, the committee determined that the project is exempt from formal ethical approval. This decision is based on the nature of the study, which does not involve clinical interventions, randomization, or the collection of sensitive health data beyond participants’ voluntary narratives and anonymized survey responses.
All procedures will nonetheless adhere to the principles of the Declaration of Helsinki and relevant European data protection regulations (GDPR). Participants will provide informed consent prior to participation, and data will be anonymized or pseudonymized at the point of collection. The exemption from formal approval reflects the minimal risk posed to participants and the public health orientation of the project, which focuses on community engagement and descriptive evaluation rather than experimental treatment or diagnostic procedures.
Finally, data will be stored on secure servers in compliance with GDPR. Facilitators will be trained to monitor distress and provide signposting to support services. Ethical approval will be obtained from the relevant institutional committee.
Discussion
The impetus for our hospital-based specialist PC service to engage in the development of a CC stems from a dual recognition: the persistent stigma surrounding PC and the societal discomfort with death, which often leads to delayed referrals and inadequate support for patients and families.2,3 Inspired by the Lancet Commission’s call to “bring death back into life,” 2 we felt compelled to move beyond the institutional boundaries of healthcare and initiate dialogue with voluntary associations and local municipalities.
Our engagement aligns with the broader literature that identifies both systemic gaps in healthcare and societal challenges—such as the need to normalize PC and strengthen community action—as key drivers for CC initiatives.20,22 By embracing a community-based approach,17,32 we aim to foster a more responsive and sustainable model of care that addresses the increasingly complex needs of individuals at the end of life, which traditional health systems often struggle to meet.
The protocol presented here represents a pioneering effort in our region, marking the first time that a coordinated, methodologically rigorous initiative has been undertaken to support individuals and families facing end-of-life experiences—from cancer to neurodegenerative diseases and age-related frailty. This initiative is rooted in the longstanding presence of voluntary associations, which have been active in end-of-life care for over three decades, mirroring similar grassroots movements in Soweto, Spain, Latin America, Scotland, and India.18,20
Given the relatively nascent state of CC research, our project seeks to contribute to the literature by documenting the early stages of development, including planning, process description, and mixed-methods evaluation.18,22 Publishing this protocol is a deliberate choice to ensure transparency and to allow for iterative updates based on ongoing findings and adaptations, consistent with co-construction methodologies. 19
Importantly, this initiative represents the first CC developed within the cultural context of northern Italy—a region with distinct socio-cultural characteristics that have not yet been explored in existing CC literature. As Bakelants et al. 19 emphasize, flexible integration of diverse models and disciplines is essential. Our steering committee embodies this interdisciplinary ethos, bringing together representatives from health and social services, third-sector organizations, and researchers from diverse fields, including community psychology, anthropology, statistics, and qualitative research.
A cornerstone of our approach is the co-construction of each phase of the protocol, with active involvement from local interest-holders, service providers, caregivers, and the broader community. This participatory process ensures that future actions are grounded in grassroots data and insights, enhancing their relevance, sustainability, and cultural resonance. As Voltz et al. 39 and D’Eer et al. 12 argue, bottom-up initiatives are more likely to be embraced and maintained over time, fostering meaningful cultural change in how death and dying are approached.
Qualitative data from interviews and focus groups will illuminate existing care practices and community perceptions, 40 enabling reflective dialogue with interest-holders to deepen collective awareness of end-of-life needs and resources. The iterative evaluation of the process will allow real-time adjustments based on participant feedback, ensuring the project remains responsive and inclusive.
We believe that a co-constructed evaluation framework will strengthen the partnership between researchers and community interest-holders, aligning the research process with local values and priorities. Participatory training sessions will enhance the capacity of interest-holders in qualitative research, promoting collaborative knowledge production. Co-analysis of focus group data will ensure that diverse perspectives inform the interpretation of caregiver experiences, guiding the development of a community-informed survey that captures broader societal attitudes.
Ultimately, the insights gathered will inform the design of short-, medium-, and long-term interventions, identifying potential benefactors and sustaining the momentum of the CC initiative. Through this protocol, we hope to offer a replicable model for other regions and contribute to the evolving field of public health PC.
Conclusion
This protocol marks a significant milestone in the evolution of public health PC in Italy, laying the foundation for the country’s first CC developed through a rigorously co-constructed, participatory process. By integrating qualitative and quantitative methodologies, and actively involving interest-holders, caregivers, and citizens, the InVita! project aims not only to respond to unmet end-of-life care needs but also to catalyze a cultural shift in how death, dying, and grief are understood and supported within communities.
Rather than offering a static blueprint, this protocol fosters flexibility and responsiveness, enabling iterative adaptation based on community feedback and emerging insights. This dynamic approach is essential for fostering genuine ownership, sustainability, and relevance in a socio-cultural context that has not previously been explored in CC literature.
The project’s interdisciplinary structure—uniting healthcare professionals, social services, voluntary associations, and researchers—reflects the complexity of the challenge and the richness of the response. It positions the InVita! initiative not only as a local innovation but as a potential model for other regions seeking to embed care within relationships and civic life, as advocated by the Lancet Commission on the Value of Death. 2
Future publications will detail the outcomes of each phase, contributing to the global discourse on CCs and offering actionable insights for replication and scaling. Ultimately, this protocol is a call to reimagine care at the end of life—not as a clinical task confined to institutions, but as a shared societal responsibility rooted in compassion, solidarity, and community resilience.
Supplemental Material
sj-doc-1-pcr-10.1177_26323524251397425 – Supplemental material for Initial steps toward the first Compassionate Community in Italy: A study protocol
Supplemental material, sj-doc-1-pcr-10.1177_26323524251397425 for Initial steps toward the first Compassionate Community in Italy: A study protocol by Silvia Tanzi, Elisabetta Bertocchi, Silvia Bertolotti, Ludovica De Panfilis, Luca Ghirotto, Giulietta Luul Balestra, Silvio Cavuto, Martina Fiaccadori, Cinzia Cavalli, Marta Perin and Irene Barbieri in Palliative Care and Social Practice
Footnotes
ORCID iDs
Ethical considerations
The study will be conducted in compliance with the protocol following the principles of the Helsinki Declaration. The Provincial Ethics Committee (EC) of Reggio Emilia, which examined the protocol, the information sheets, and the informed consents relating to the study, did not consider any approval necessary (“the project goes beyond the strictly ‘health’ context and involves various actors: associations, patients, their families, and citizens invited to take part in cognitive surveys”). It was deemed that this part of the project could also be carried out without the EC’s opinion, provided that the information collection is guaranteed to be completely anonymous (See EC note in ![]() ).
).
Consent to participate
All citizens/patients/family members, after receiving the necessary information to clarify the nature and purpose of the project, must state their adherence to the project by signing a specific consent form for the study and data processing. Each person may withdraw their consent at any time without having to justify their choice. The data will be processed and analyzed, ensuring compliance with all applicable privacy criteria under the law. All data collected that could lead to the identification of persons involved will be pseudonymized in external communications, including publications. The researchers will seek participants’ consent before collecting qualitative data. All data collected will be stored securely and accessible only to research team members. All paper surveys will be stored in a locked cabinet. According to good clinical practice guidelines, electronic (raw) data (including privacy-sensitive information and any other information that may lead to the identification of individuals) should be retained for 15 years. Audio files will be deleted as soon as they are transcribed.
Author contributions
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The project won funding provided by the Manodori Foundation Grant for “
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
Not applicable.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
