Abstract
Background:
Cancer patients experience significant changes in their social roles along with various physical and psychological challenges. Despite the growing recognition of the importance of palliative care in Bangladesh, there is a notable gap in research focusing on the psychosocial issues faced by patients with advanced cancer.
Aim:
This study aims to explore the level of social support perceived by Bangladeshi cancer patients and determine how this support relates to their mental health status.
Methods:
This cross-sectional study was conducted among 115 advanced cancer (stages III and IV) patients admitted to the palliative medicine department of a tertiary care hospital in Bangladesh. Perceived social support was measured by the Multidimensional Scale of Perceived Social Support, and the mental health status of the patients was assessed by Depression, Anxiety, and Stress Scale-21. Data collection was done from June to November 2023. Relationships between perceived social support, depression, anxiety, and stress were assessed by the Spearman correlation test. The moderating effect of perceived social support on patients’ mental health variables was determined by multiple linear regression and simple slope analysis.
Result:
The study included an almost equal number of male (49.6%) and female (50.4%) patients, with a mean age of 50.7 ± 14.4 years. Overall, perceived social support was moderate to high for most (74.7%) of the participants. Among the participants, 78.3% experienced anxiety, 77.4% suffered from depression, and 70.5% experienced stress. Depression, anxiety, and stress were all negatively and significantly (
Conclusion:
Perceived social support has a profound and significant effect on the mental health of advanced cancer patients. Integrating psychosocial support early in palliative care can be highly beneficial to the mental health of these patients.
Plain language summary
This cross-sectional study was conducted among 115 patients with advanced cancer (stages III and IV) admitted to the palliative medicine department of a tertiary care hospital in Bangladesh. The majority of the patients with advanced cancer suffer from depression and anxiety and experience high level of stress. Younger patients report more of these psychological issues. High level of perceived social support is associated with lower levels of depression, anxiety, and stress. It acts as a buffer against these negative emotions. Patients who experienced a high level of social support while dealing with physical pain reported less depression.
Background
Health is a multidimensional concept that encompasses not only physical health but also mental, emotional, and social well-being. 1 Cancer and its clinical manifestations, along with its treatment side effects, bring about various changes in the patient’s personal life, daily activities, work, and relationships with their families and friends, as well as in their role in society. 2 These changes often lead to a huge psychological burden, a high level of stress, reduced compliance with treatment, and increased mortality.3,4
Among all the mental health issues encountered by advanced cancer patients, anxiety and depression are the most common problems. 5 Several studies conducted in different countries found that about 16–38% of patients with advanced cancer suffer from clinical depression, 93% report mild- to-moderate levels of anxiety, and 93.6% experience a high level of stress throughout their illness period.6–11 Aside from psychological issues, these patients are also burdened with various physical symptoms. Among them, pain is one of the most common physical symptoms reported by cancer patients. Almost 35–96% of patients with advanced cancer suffer from pain. 12 These physical and mental health issues are interconnected and influenced by psychosocial variables. Researchers suggested that depression, anxiety, and perceptions of social support influence cancer patients’ degrees of pain interference. 13 Currently, about 1.3–1.5 million people in Bangladesh are living with cancer, and most of them suffer from significant physical and psychosocial burdens. Our sociocultural context, cultural norms, and stigmas surrounding cancer also influence the illness experience of these patients.14,15 Studies have demonstrated that social support helps to ease some of the challenges of living with cancer. 16
Perceived social support is a crucial factor that affects the physical and psychological well-being of cancer patients. It also plays a significant role in determining their quality of life during the advanced stage of the disease. 17 Perceived social support refers to ‘how an individual perceives friends, family members, and others as sources available to provide material, psychological, and overall support during times of need’. 18 According to Cohen and Wills’ stress buffer theory, social support protects (i.e. buffers) people from the adverse effects of stress. 19 Another model suggests that patients who perceive high social support have lower levels of depression. 20 One study demonstrated a negative association between perceived social support and anxiety symptoms, which indicates a high level of social support can alleviate anxiety. 21 Although the direct relationship between perceived social support, mental health issues, and pain is not often explored, one study found that a higher level of social support is linked to less pain and depressive symptoms. 22 All of these models are above and beyond the effects of covariates such as age, cancer stage, treatment modalities, performance status, and use of antidepressant and pain medications. However, many studies have also suggested that age is an important factor influencing the mental health status of cancer patients, specifically depression and anxiety. Despite this, there is not enough literature available exploring the direct relationship between age and psychosocial variables.11,23,24
Palliative care services in Bangladesh have evolved over the years but remain limited in availability and accessibility, especially outside urban centers. Furthermore, the challenges faced by cancer patients and their families are compounded by socioeconomic disparities and limited access to healthcare services. Therefore, it is crucial to understand the significance of social support and mental health issues in this context. An observational study found significant physical, psychosocial, and spiritual burdens among Bangladeshi patients with advanced incurable illnesses. Although their families and friends provide some practical support, only a few patients have access to any professional support for these concerns. 15 Despite these challenges, palliative care providers in Bangladesh play a crucial role in addressing the complex needs of patients with advanced cancer, including pain management, symptom control, and psychosocial support. A study conducted in a community-based palliative care center in Bangladesh showed a significant reduction of pain and other symptoms among cancer patients, in addition to a significant improvement in their quality of life. 25
Despite the growing recognition of the importance of palliative care in Bangladesh, there is a notable gap in research focusing on the psychosocial issues faced by advanced cancer patients. In addition, the relationship between perceived social support and physical and psychological issues, which is particularly important for determining the need for further psychosocial aspects of palliative care interventions, remains unexplored. The purpose of this study is to fill the knowledge gap by investigating the level of social support that patients with advanced cancer in Bangladesh perceive. Additionally, the study aims to determine how this support is related to their mental health and physical symptoms like pain.
Methods
Study design and setting
This cross-sectional study was conducted among advanced cancer patients admitted to the Department of Palliative Medicine, Bangabandhu Sheikh Mujib Medical University (BSMMU), Shahbag, Dhaka. Data collection was done from June to November 2023.
Sample criteria
Patients with stage III and IV cancers, above 18 years of age, admitted to the Department of Palliative Medicine, BSMMU, were included in the study. Patients with cognitive impairment (mini mental score <24) were excluded from this study. 26
Sample size
In a Turkish study, the mean perceived social support among cancer patients was reported at 24.6 ± 5.1 on the Multidimensional Scale of Perceived Social Support (MSPSS) scale. 23 We considered this score as a reference to calculate our sample size using a one-sample proportion test with absolute precision.
Formula

Here,
Calculation,
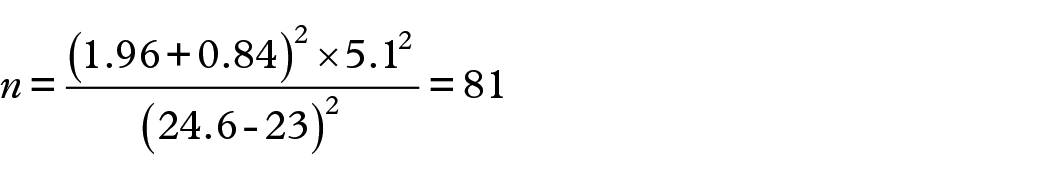
According to this formula, the required minimum sample size was 81. To increase the power of the study, we initially approached 130 patients. Among them, eight patients refused to give informed consent, two withdrew themselves as they were feeling sick, and five were unable to complete the questionnaire. So, our final sample size was 115.
Data collection instruments
Data were collected using a structured questionnaire. It contained questions related to socio-demographic and disease-related information, pain, perceived social support, and mental health-related variables.
Pain was measured by a numerical rating scale. It is a continuous scale ranging from 0 (no pain) to 10 (the worst possible pain experienced). This scale also divides pain into three categories based on intensity: mild (1–3), moderate (4–6), and severe (7–10). 27
The mental health status of the patients was assessed by the validated Bangla version of the Depression, Anxiety, and Stress Scale-21 (DASS 21), developed by Lovibond and Lovibond
28
(α = 0.74) and translated and validated in Bangla by Alim
The perceived social support of the patients was measured by the validated Bangla version of the MSPSS, developed by Zimet
Patient recruitment and data collection procedure
The patients were recruited
At first, the questionnaire was pre-tested among 10 cancer patients. During the pre-testing phase, many participants were confused by the term ‘significant others’ mentioned in the MSPSS questionnaire. To clear up this confusion, we provided an explanation for the term based on a definition used in a study conducted in Thailand. 32 According to this study, ‘significant others’ refers to special persons who provide social support to the patient outside of friends or family. This group includes individuals such as neighbors, co-workers, colleagues, classmates, doctors, nurses, palliative care assistants, or volunteers. We have incorporated this explanation into the final questionnaire to ensure clarity for all participants.
The members of the research team collected data from the patients through in-person interviews. The primary investigator recorded the most appropriate response on the questionnaire. Sensitive questions were asked privately, and patients were encouraged to write them down if they felt uncomfortable discussing them openly. Each interview lasted 30 minutes to an hour, depending on the patient’s condition. Very frail patients required multiple visits to complete an interview.
Statistical analysis
All statistical analyses were performed using the Statistical Package for the Social Sciences (SPSS) 26 version (IBM Inc., New York, USA). The subscales of MSPSS and DASS 21 were calculated separately. For the MSPSS scale, scores for each subscale were summated separately and divided by 4 to calculate scores for each subscale. For the total score, scores for all subscales were summated and divided by 12. For DASS 21, all scores were multiplied by 2 to calculate the final score.
Categorical variables, such as gender, educational status, economic class, marital status, educational status, primary diagnosis, time since diagnosis, and patient performance status, were presented in frequency and percentage. Continuous variables such as age, annual household income, pain scale, perceived social support scores, and anxiety, stress, and depression scores were presented as mean, SD, median, and range. To improve data triangulation, scores for perceived social support, pain and depression, anxiety, and stress were presented into categories according to the scoring manual. All the skewed data was standardized before analysis.
The Spearman correlation test was used to determine the relationship between perceived social support, depression, anxiety, and stress scores. Multiple linear regression analysis was performed to identify the factors influencing the mental health status of the patients. We examined the continuous scores of DASS 21 and MSPSS for this part of the analysis. A simple slope analysis was done to see the interaction effects of perceived social support and other influencing factors of the mental health variables. All means were calculated at a 95% confidence interval, and
Result
Among the study participants, 49.6% were male and 50.4% were female, with a mean age of 50.7 ± 14.4 years. The majority (91.2%) belonged to lower to lower-middle income groups according to the World Bank Group classification. 33 Cancers of the gastrointestinal system (21.7%) were most prevalent among the participants of this study, followed by cancers of the genitourinary system (18.3%), hepatobiliary system (18.3%), and breast (12.2%). Sixty percent of these patients presented to palliative care within 10 months of diagnosis. The majority (80%) of these patients complained of pain, and among them 60.9% suffered from moderate to severe pain (Table 1).
Socio-demographic and clinical characteristics of the patients (

According to World Bank Group classification (updated on July 2022).
The level of overall perceived social support was moderate to high for most (74.7%) of the participants, and only 25.3% perceived low level of support. However, 97.4% of the participant perceived moderate-to-high levels of support from their families. The lowest level of support was perceived from friends (53%) (Table 2).
Level of perceived social support among the patients (

The majority of the participants suffered from depression (77.4%), anxiety (78.3%), and stress (70.5%). Among them, 40% of them suffered from severe-to-extremely severe depression, 53.9% of them had severe to extremely severe levels of anxiety, and 45% of them experienced severe to extremely severe levels of stress (Table 3).
Mental health status of the patients (

Depression, anxiety, and stress were all found to be negatively and significantly (
Relationship between of perceived social support and mental health (

Spearman correlation was done. Bold values indicates
Multiple linear regression analysis showed that the perceived level of social support was negatively and significantly related with depression, anxiety, and stress, whereas pain severity was positively and significantly related with the depression level of the patients. Younger patients were found to be more depressed, anxious, and stressed. Low perceived social support was associated with more depression, anxiety, and stress. Increased level of pain was also associated with higher levels of depression. The interaction effects among moderating variables showed that depression among patients with pain was significantly influenced by the social support they perceived. Patients with pain perceiving higher social support were found to be less depressed. Depression and anxiety among the younger patients were significantly buffered by the social support they perceived. However, we did not find any significant interaction effect of social support with patients’ age on the stress level (Table 5).
Moderating effect of perceived social support on mental health status (

Multiple linear regression was done; interaction effects were assessed by simple slope analysis; all variables were analyzed in continuous form.
Discussion
Cancer is a life-changing disease that affects not only the physical condition of patients but also their mental and social well-being. In this study, we investigated the perceived social support of advanced cancer patients in Bangladesh and its relationship with pain and various psychological issues. To the best of our knowledge, this is the first study to explore this relationship.
In this study, most (74.7%) of the participants perceived moderate-to-high levels of social support. Our finding was mostly similar to Iranian and Turkish studies, where the majority (74.5%) of patients reported perceiving moderate-to-high levels of social support.34,35 It might be due to the religious and cultural similarities between our country and Iranian and Turkish populations, where people mostly lived in tightly knit communities, and supporting other community members was deeply ingrained in their values.
The majority of our participants perceived the highest level of support from their families. The findings of our study were in line with those of other studies conducted in different regions of the world, including East Asian countries such as China, Middle Eastern countries such as Turkey and Iran, and Western countries such as the United States and Scotland.36–40 High score on the family support subscale among our patients indicated close familial relationships in Bangladeshi society.
It is interesting to note that in our study, cancer patients perceived the lowest level of social support from their friends. This difference in perception might be due to cultural differences, where Asian and Middle Eastern countries rely more on families for support, whereas in Western countries, both families and friends are considered the main sources of social support.41,42 Although we did not investigate the reasons behind these differences, our findings suggest that similar to other Asian countries, families are perceived as the main source of social support by Bangladeshi cancer patients.
Perceived social support has a significant impact on psychological issues such as depression, anxiety, and stress, which are commonly experienced by cancer patients. Our research revealed a strong negative correlation between perceived social support and these three psychological issues. Patients who reported higher levels of perceived social support experienced lower levels of depression, anxiety, and stress. Several studies conducted across different countries have also reported similar findings.10,43,44 This phenomenon can be explained by the stress-buffering hypothesis. According to this hypothesis, perceived social support reduces psychological problems by lowering the sense of threat posed by a situation and increasing the accessibility of help. 19 We also observed a notable negative relationship between family support and anxiety, stress, and depression. This means that high level of family support was associated with lower levels of psychological issues among our study participants. Our findings align with previous studies which suggest that family support is a powerful protective factor against such issues, particularly in Asian communities.24,45
Age plays a significant role in determining the psychological well-being of cancer patients. We found that younger age was associated with higher depression, stress, and anxiety scores. This finding is supported by three separate studies that have demonstrated an inverse correlation between age and psychological distress. Younger cancer patients may experience higher levels of stress and anxiety due to worrying about their diagnosis and treatment.11,46,47 However, several studies have reported a higher level of depression among older patients, which contradicts our findings.23,24 Our research has also shown that social support plays a vital role in reducing depression and anxiety levels among young patients. Specifically, perceived social support can act as a buffer against these negative emotions. Studies suggest that young cancer patients tend to receive a high level of social support from their friends and families, which may help alleviate some of their emotional burden. 48
Pain was another factor that was significantly associated with the mental health of cancer patients. We observed a direct relationship between pain and depression. Regression analysis showed that an increased level of pain was associated with higher levels of depression among our patients. Other studies also found a strong relationship between pain level, depression, and the functional capacity of cancer patients.
49
Our study also found a direct buffering effect of perceived social support on pain and depression levels. Patients who perceived a high level of social support while dealing with physical pain had lower levels of depression. Our findings supported the model created by Fisher
Our study findings underscore the significant role of social support in addressing mental health issues among advanced cancer patients. Further research is needed to explore the specific needs for such support in clinical settings and to identify effective methods of implementation. This may include investigating psychosocial interventions, integrating multidisciplinary teams into clinics, and providing support to caregivers.
Limitations
It is important to note that this study has some limitations that need to be considered. First, the research was carried out at only one institute, so the findings may not be generalized. Second, the study was cross-sectional in nature, which means that we were unable to observe any changes in the participants’ perception of social support throughout the course of their illness. In addition, due to this cross-sectional design, temporal relationships between variables could not be determined.
Conclusion
Perceived social support has a profound and significant effect on the mental health of advanced cancer patients. Palliative care professionals can work toward integrating psychosocial support early in their management plan, especially for younger patients with psychological distress. They also need to keep social factors in mind while managing pain and psychological issues among advanced cancer patients.
Supplemental Material
sj-doc-2-pcr-10.1177_26323524241256379 – Supplemental material for Relationship between perceived social support and mental health status of the advanced cancer patients receiving palliative care in Bangladesh
Supplemental material, sj-doc-2-pcr-10.1177_26323524241256379 for Relationship between perceived social support and mental health status of the advanced cancer patients receiving palliative care in Bangladesh by Jheelam Biswas, A. K. M. Motiur Rahman Bhuiyan, Afroja Alam and Mostofa Kamal Chowdhury in Palliative Care and Social Practice
Supplemental Material
sj-docx-1-pcr-10.1177_26323524241256379 – Supplemental material for Relationship between perceived social support and mental health status of the advanced cancer patients receiving palliative care in Bangladesh
Supplemental material, sj-docx-1-pcr-10.1177_26323524241256379 for Relationship between perceived social support and mental health status of the advanced cancer patients receiving palliative care in Bangladesh by Jheelam Biswas, A. K. M. Motiur Rahman Bhuiyan, Afroja Alam and Mostofa Kamal Chowdhury in Palliative Care and Social Practice
Footnotes
Acknowledgements
The authors gratefully acknowledge the contribution of Palash Chandra Banik, Associate Professor, Department of Non-Communicable Diseases, Bangladesh University of Health Sciences, Dhaka for his contribution in data analysis and editing this manuscript.
Declarations
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
