Abstract
Dental implants are increasingly being used to replace missing or lost teeth. Despite significant advances in materials, techniques, and implant design, implant failure remains a major concern for both the dentist and the patient. The most common causes of implant failure are peri-implantitis and a lack of osseointegration. Other causes of implant failure include occlusal overloading, compromised or poor medical status of the patient, habits that harm oral tissues, and implant selection. The most pressing issue that all implantologists face today is the occurrence of complications and failures in implants. To further improve treatment outcomes, the etiologies and factors associated with implant failures should be identified. Osseointegrated dental implants have long been regarded as the closest substitute for missing teeth.
Introduction
Dental implants are frequently used in clinical settings to replace natural teeth. Despite significant advances in materials, techniques, and implant design, implant failure remains a major concern for both the dentist and the patient. The most common causes of implant failure are peri-implantitis and a lack of osseointegration. Other causes of implant failure include occlusal overloading, a patient’s poor or compromised medical status, habits that harm oral tissues, and implant characteristics. 1
An implant is defined as “a graft or insert that is set firmly or deeply into an alveolar process that has been prepared for its insertion.” Implants are used to replace single teeth, partially edentulous arches, and completely edentulous arches. They are inert, alloplastic materials that are typically made of titanium, titanium alloys, or vitalinium. An implant is made up of an implant body that is placed within the bone and an implant screw that is placed on the superior surface of the body and to which the healing cap is attached. Abutments are placed over the implant body to keep the prosthesis in place. Implants are inserted into the bone during stage 1 or stage 2 surgery. 1
Dental implants have become a popular method of replacing missing teeth. The goal of implant-supported tooth replacement is to restore adequate function and aesthetics without affecting adjacent hard and soft tissue structures. Since clinical studies with dental implant treatment have revealed successful outcomes, the use of dental implants in oral rehabilitation has been increasing. The success of any implant procedure is determined by a number of patient-related and procedure-dependent parameters, such as the patient’s general health, the biocompatibility of the implant material, the design of the implant surface, the surgical procedure, and the quality and quantity of bone. 2
The possibility of implant failure is a major source of concern for implantologists. Failure of a dental implant is frequently associated with the implant’s failure to osseointegrate with the bone. Implant dentistry is currently being practiced in an upbeat and optimistic environment, owing to our increased knowledge and ability to provide such services to our patients in such a short period of time. Implant dentistry does have complications. 3
These are more frequently caused by ageing, changing health conditions, long-term wear and tear, poor home care, and insufficient professional maintenance. It is impossible to guarantee success. “Unfortunately, failure is the best teacher most of the time.” 3
Classification of Implant Failure 3
According to Askary et al
Ailing implant: Implants that only have soft tissue problems are classified as ailing and have a better prognosis.
Failing implant: A failing implant is one that is gradually losing bone anchorage but is still clinically stable.
Failed implant: An implant with mobility and excessive bone loss (>70%) that is not treatable is considered a failed implant.
According to Etiology
Medical status (uncontrolled diabetes), habits (parafunctional habits), and oral status are examples of host factors (poor oral hygiene maintenance).
Surgical factor, such as off-axis placement (severe angulation) • Inadequate initial stabilization • Impaired healing and infection due to improper flap design or others • Excess heat generated during bone drills • Inadequate irrigation • Placing the implant in immature bone-grafted sites • Contamination of the fixture prior to placement.
Implant selection factor—for example, bone quality and quantity, improper implant type in improper bone type. • Implant length (too short, crown-implant ratio unfavorable).
Excessive cantilever, pier abutments, no passive fit, improper abutment fit, improper prosthetic design, and improper occlusal scheme, bending moments, connecting implants to natural dentition, premature loading, and excessive torquing are examples of restorative factors.
According to Condition
Ailing implant—for example, the mildest of 3 categories inflammation redness, or mild bone loss may indicate that the implant is not completely healthy.
Failing implant—if check-up X-rays reveal increased bone loss around the top of the implant, the cause must be identified and corrected. Poor oral hygiene, a bad bite, or any number of other factors could be to blame. After the problem has been resolved, the resorbed bone should be grafted.
Failed implant—for example, if the implant has any mobility, the only acceptable treatment is removal.
According to Timing of Failure
Prior to stage II (after stage II).
Stage II—insertion of a healing head and/or an abutment. Following restoration. Poor soft tissue management and poor oral hygiene maintenance.
According to Failure Mode
Lack of osseointegration—for example, contamination of the implant surface.
Unacceptable aesthetics—for example, poor soft tissue management.
Functional problems—for example, difficulty in chewing and biting.
Psychological problems—for example, I have worries with my teeth.
Depending on the Type of Supporting Tissue
Loss of soft tissue—for example, systemic disease and conditions of the patient.
Bone loss—for example, trauma to orofacial structures.
Combination—for example, local disease affecting the teeth, the periodontium, the bone, and the mucosa.
According to Source
Peri-implantitis, for example, infectious process and bacterial origin, peri-implantitis can be caused by a traumatic occlusion, a noninfectious force off the long axis, or premature or excessive loading.
According to the Failure Condition
Clinical and radiographic findings.
Working Classification 4
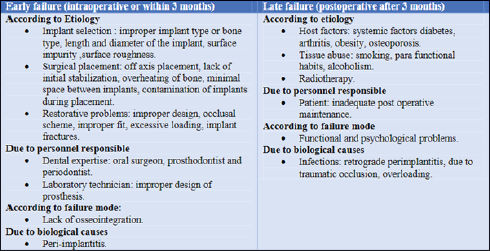
Complications
Oversized osteotomy.
Cortical plate perforation.
Buccal and lingual cortical plate perforation.
Antral perforations.
Inadequate soft tissue flap coverage for the implant.
Hemorrhage.
Inadequate angulations.
Tissue Abuse and Parafunctional Habits
Implant success is harmed by tissue abuse habits, parafunctional habits, and psychiatric illness. Smoking has been linked to a considerable increase in bone loss. It decreases bone density, interfering with osseointegration, and increasing the failure ratio. Baig and Rajan 5 discovered that smokers had more implant failures, while Bain and Moy 6 discovered that smokers had a much higher percentage of implant failures (11.3%) than nonsmokers (4.8%). 1
According to the research conducted by Dror Twito and Paul Sade 7 in Israel between 1999 and 2008, 4.2% of implants, or 321 out of 7,680, failed owing to smoking, which included passive smoking, Bruxism, and other dysfunctional habits which are on the rise. 1
Conclusion
The pathogenesis of implant failure is multifaceted. Several factors have been identified as contributing to implant failure. To cure a current alignment, the practitioner must first identify the main root cause. A thorough history, patient feedback, regular follow-up sessions, and accurate diagnostic instruments will aid in determining the cause of failure. If there are regular follow-ups and check-ups, an early intervention can help with a better prognosis. The early detection of failing implants is critical to the treatment strategy for complications and failing implants.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Statement of Informed Consent and Ethical Approval
Necessary ethical clearances and informed consent was received and obtained respectively before initiating the study from all participants.
