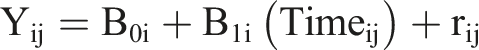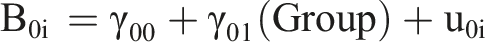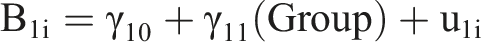Abstract
Infant mortality rates (IMR) and other health disparities (e.g., low provider access; higher obesity rates) exist across rural America, especially in the southeastern United States. These disparities coincide with negative socioeconomic factors such as poverty and low household income. Georgia’s 2020 preterm birth rate was seventh highest among the 50 U.S. states, its rate of low birth weight (LBW) babies was fourth among states.
Methods
This study used a novel, combined spatiotemporal analysis to assess IMR and health trends in Georgia counties (n = 159). We spatially regressed IMR on 14 biopsychosocial health variables and assessed IMR 2012–2022 longitudinal trends, rural versus urban or by Health Professional Shortage Area (HPSA) status, using a two-level hierarchical linear model.
Results
Analyses demonstrated significant associations between IMR and rural counties as well as counties that have high African American populations, high unemployment, and high uninsurance rates. Principal Care Provider Rates showed a negative spatial regression relationship. There was a −0.056 IMR slope for urban counties from 2015 to 2022, whereas the rural county IMR slope was 0.135.
Conclusions
Findings concur with previous research suggesting the need for coordinated county-specific socioeconomic development and corresponding increased health programs. Combined geospatial and multilevel models represent a novel approach to inform public health epidemiology.
Background
In 2020, the leading causes of death among U.S. Georgians were (a) heart disease (183.7 per 100,000 people); (b) cancer (147.6); (c) COVID-19 (138.8); (d) accidents (50.8); (e) Alzheimer’s Disease (45.9); (f) stroke (43); (g) chronic lower respiratory diseases (41.6); and (h) diabetes (23.9).1,2 These rankings closely mirror corresponding 2020 mortality rankings for the United States. 3
Of particular concern are U.S. infant mortality statistics that lag behind many other developed nations. 4 Georgia’s 2020 preterm birth rate was 11.4 per 1000 births, seventh highest among the 50 states, and low birth weight (LBW) was 9.9, fourth among states.2,5 The infant mortality rate (IMR) was 6.28, sixteenth among states.2,4–6
Factors impacting IMR
When looking at disparities in IMR, African American IMR have improved but remain approximately twice that of non-Hispanic Caucasians nationally. 7 Regionally, the Great Lakes states (Illinois, Indiana, Michigan, Ohio, Wisconsin) have the highest regional African-American IMR = 13.77, whereas the New England states were lowest at IMR = 8.78. In this particular study, Kandasamy et al. 7 identified higher African American marriage rates and higher state Maternal and Child Health (MCH) budgets as protective factors against IMR. Furthermore, IMR was significantly higher in counties that are rural and/or experience high poverty. 8
Bhatt and Beck-Sagué 9 demonstrated that 2014–2016 infant mortality rates declined in Affordable Care Act (ACA) Medicaid expansion states but increased in the nineteen non-expansion states. Ten of the nineteen Medicaid non-expansion states, including Georgia, were in the U.S. South, which generally has higher IMR rates. As of November, 2022, 11 states had not participated in Medicaid expansion, including Georgia and seven additional Southern states. 10 In an earlier 2007–2009 study of the Period Linked Birth-Infant Death File, Hirai et al. 11 recommended state-centered health promotion strategies given variations in causes of IMR across Southern states. Current IMRs are being targeted by Healthy People 2030 national objectives, including reductions in fetal, infant, and children deaths. 12
Yang and McManus 13 applied geospatial analyses to examine IMR and other health/social factors in the 159 Georgia counties. They identified hotspot counties of high IMR in varied clusters that generally concentrated across mostly rural counties in the eastern middle portion of the state, extending westward to the Southwestern counties while including a few Atlantic coast counties. These clusters followed the overall Piedmont/coastal plain geographical characteristics of low socioeconomic conditions, IMR, and other poor health outcomes across the Southeastern United States. 14 Clustering of specific variable frequencies has been a characteristic of complex systems, including physical phenomena and biological systems.15,16 Likewise, Arcaya et al. 17 used a two-level geospatial model to a combination of within-state and overall spatial processes that impact U.S. county-level longevity rates.
Ehrenthal, Kuo, and Kirby 18 examined the 2014–2016 NCHS Period Linked Birth-Infant Death Files, demonstrating significantly higher odds ratios for neonatal, post-neonatal, and infant deaths in noncore rural and micropolitan counties compared to fringe and central metropolitan U.S. counties.
The spatiotemporal analysis of health trends is of extreme importance for better understanding the biopsychosocial forces that impact individual and population health. The study uses 11 consecutive years of county-level population health data, with longitudinal time and spatial autocorrelation/regression along two analytical pathways: (a) geospatial regression19,20; and (b) hierarchical linear models.21,22
Spatial analysis
When examining event data, spatial lattice data, and other geographic data, it is important to examine the effects of neighboring geographic entities in various combinations for a particular observed variable. Correlated geographic effects between neighboring counties can inflate significance and the regression coefficient of determination when Ordinary Least Squares (OLS) regression is used.
Anselin and Bera 19 noted the importance of spatial dependence in economic statistics and modeling because of high/low value regional clustering and neighbor similarities/dissimilarities. Fotheringham and Brunsdon 20 also noted scaling differences in statistical reporting, with the realization of local variations in geographic clusters with finer spatial divisions even when there were similarities in spatial trends.20,23–25
Besides the issues of spatial autocorrelation and heterogeneity, Anselin 26 focused on the importance of proper model specification, including latent variables. Earlier, Anselin 27 had also emphasized the usefulness of Local Indicators of Spatial Association (LISA) for the identification of geographic hotspots that strengthen overall global spatial statistics, including Moran’s I statistic. Furthermore, Wheeler and Tiefelsdorf 28 stressed the importance of proper model weighting and assessments of regression coefficient multicollinearity to avoid biased models.
Temporal analysis
Longitudinally, Bryk and Raudenbush 21 identified several major problems in social science regression models: (a) variability not just within individuals but between individuals across different, nested groups/treatments at multiple levels; (b) variability within individuals over time; and (c) correlation of regression slopes and intercepts as well as errors. The result was the development of multilevel models, including hierarchical linear models that provided improved estimation and prediction. 21
Similarly, Singer and Willett 22 stressed the importance of multilevel models that: (a) adjust for and center time; (b) address longitudinal change within persons and between persons across layers of nested groupings; and (c) address the limited reliability of traditional OLS regression estimates in complex models, like spatial regression.
Therefore the objectives of this study were to: 1. Spatially map and regress the 2022 Georgia IMR on specific health and biopsychosocial variables as described above in the research literature; and 2. Temporally/longitudinally assess 11 year trends (2012–2022) in IMR and these associated health and biopsychosocial variables, comparing within and between 159 counties nested within rural/urban or low/medium/high HPSA (i.e. Health Professions Shortage Areas).
Methods
This study used GeoDa version 1.18.0.16 (spatial.uchicago.edu/software) for geospatial mapping/statistics and SAS Proc Mixed 29 for hierarchical linear models. The data source was the 2012–2022 annual County Health Rankings and Roadmaps (https://countyhealthrankings.org) compiled by the University of Wisconsin Population Health Institute from nationally-representative data sources and from county and state health department reported data. Annual data were merged using county FIPS codes.
Due to some variations in data capture, plus minimizing missing data, across the 11 data collection periods (2012–2022), we used the following county-level variables: (a) Infant Mortality Rate; (b) Percent Low Birth Rate (LBR); (c) Teen Birth Rate (TBR); (d) Percent Adults Obese; (e) Percent Adults Physically Inactive; (f) Percent Adults with Diabetes; (g) Percent Women screened Mammography; (h) Primary Care Physician (PCP) Rate; (i) Percent attended College; (j) Percent Single Parent Households (SPH); (k) Percent Unemployed; (l) Percent Uninsured; (m) Percent Black/African American; (n) Percent Rural; and (o) Violent Crime Rate (VCR). For some variables, missing data in certain years required longitudinal analysis adjustment to shorter time ranges (e.g., 2015–2022). All variables were freely available from the County Health Data and Roadmaps website.
For the outcome variable Infant Mortality Rate, n = 79 rural counties did not report data across the 2012–2022 longitudinal period, thereby limiting geospatial and HLM models in this study to n = 80 Georgia counties, of which n = 37 were urban and n = 43 were rural. Across the reporting counties, IMR ranged between 3.41 and 14.46 infant deaths per 1000 births. All Georgia counties (n = 159) reported the other variables, with the exception of PCP rate (n = 144) and Violent Crime Rate (n = 152).
Statistical models
Geospatial regression
For the single year (2022) geospatial analysis, each variable was mapped by scatterplot onto Infant Mortality Rate, including the Local Moran’s I and EB rates. A multiple regression analysis was conducted:
For the geospatial analyses, spatial regression statistics included spatial R2, Moran’s I for spatial autocorrelation, and Jarque-Bera multicollinearity estimates. Spatial weighting utilized Queen contiguity. Given 14 independent variables, we used a Bonferroni Type 1 adjusted error rate with alpha set at 0.0035.
Hierarchical linear model
For the hierarchical linear model of these variables across the 11 years, 2012–2022, the following analyses were conducted using SAS Proc Mixed.
29
The individual level model for each county is as follows21,22:
The level 2 model across all counties and groups built upon and is incorporated within the B0i and B1i parameters in the level 1 individual model:
IMR and change in IMR were assessed in the level 1 and 2 hierarchical models for n = 159 Georgia counties over 11 years from 2012 to 2022. Given univariate comparisons, we used a Type 1 error rate of 0.05 for the model assessments. One analysis focused on the Group as Rural (1) versus Urban (0), rural counties defined as 40% rural or greater (Variable “Percent Rural”) in the County Health Rankings and Roadmaps. By this criterion, n = 120 of n = 159 Georgia counties meet the rural criterion, consistent with the Georgia Department of Community Health. 30
A separate analysis focused on Group as three levels: Health Professions Shortage Areas HPSA low (0) (i.e., high PCP rate), HPSA medium (1), and high HPSA (2), as defined by the United States Health Resources Services Administration. 31 High HPSA, or high need shortage areas are operationally defined as a Primary Care Physician (PCP) Rate of 3000:1 patients: provider. 31 Given that the mean U.S. county PCP Rate is 1320:1 and based upon variations in county population densities with respect to access, 32 we used a median HPSA range for PCP Rates less than 3000:1 but greater than 1000:1. Low need HPSA was defined as a county PCP Rate <1000:1.
Results
The distribution of Infant Mortality Rates (IMR) across Georgia is shown in Figure 1(a). Whereas 36 counties did not provide information, the higher IMR counties clustered in rural sections of the state, including the east and across the southern portion of the state. One urban area with a high disadvantaged population is included in central Georgia. A few northern counties above the greater Atlanta metropolitan region had higher IMR. (a) Infant Mortality Rates (IMR) across Georgia counties, 2016. Moran’s I = 0.251 for IMR by Rurality. The four circled counties had significantly high rurality and IMR, whereas the two counties shown in black had significantly low rurality and IMR. Lightly shaded counties without highlighted boundaries did not provide IMR data. (b) Spatial Plot IMR by Principal Care Provider (PCP) Rate (R2 = 0.02). (c) Spatial Plot IMR by Pct. African American (R2 = 0.276).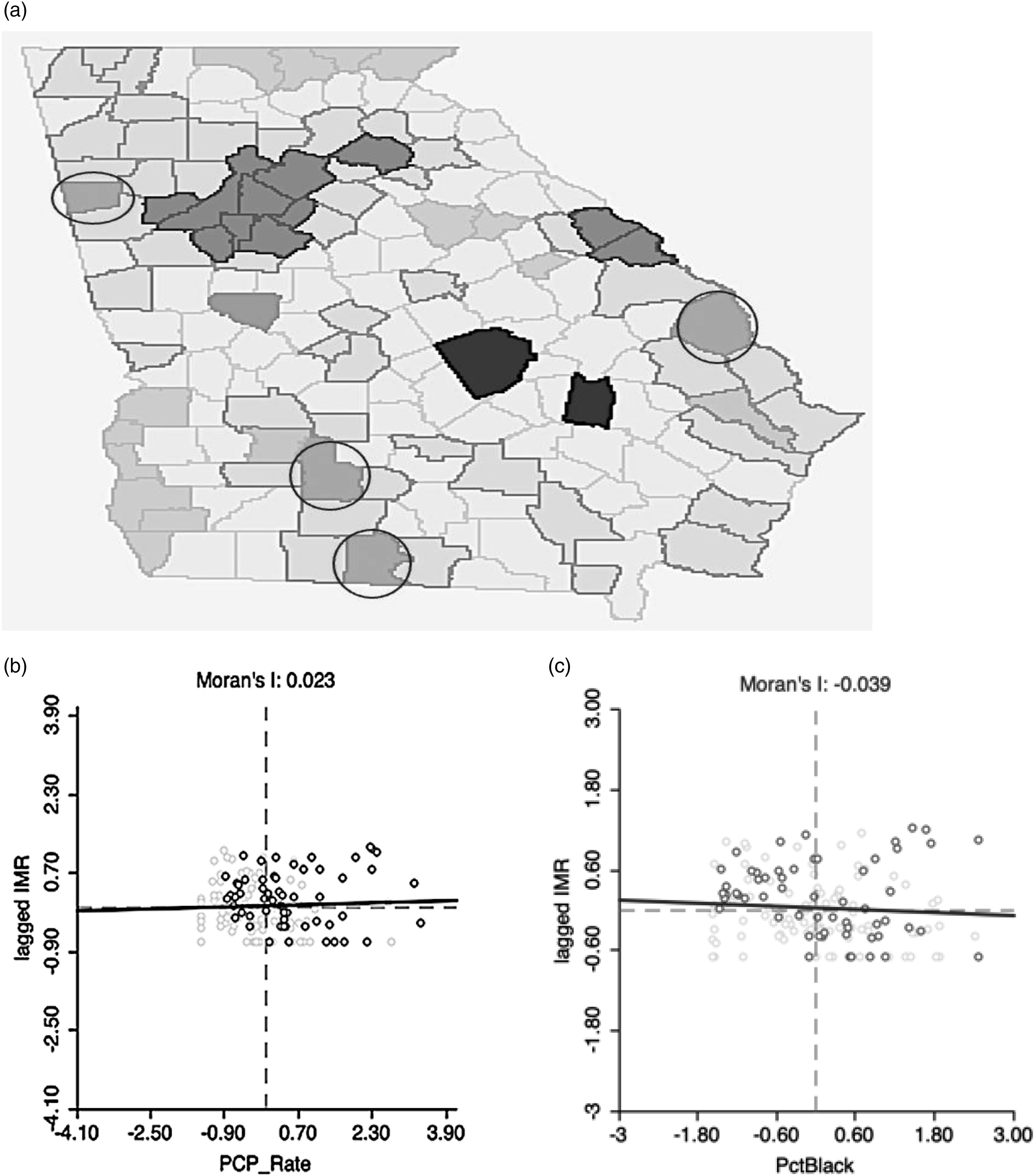
Spatial analysis
Univariate and multivariate spatial regressions of 2022 infant mortality rate on county-level independent variables.
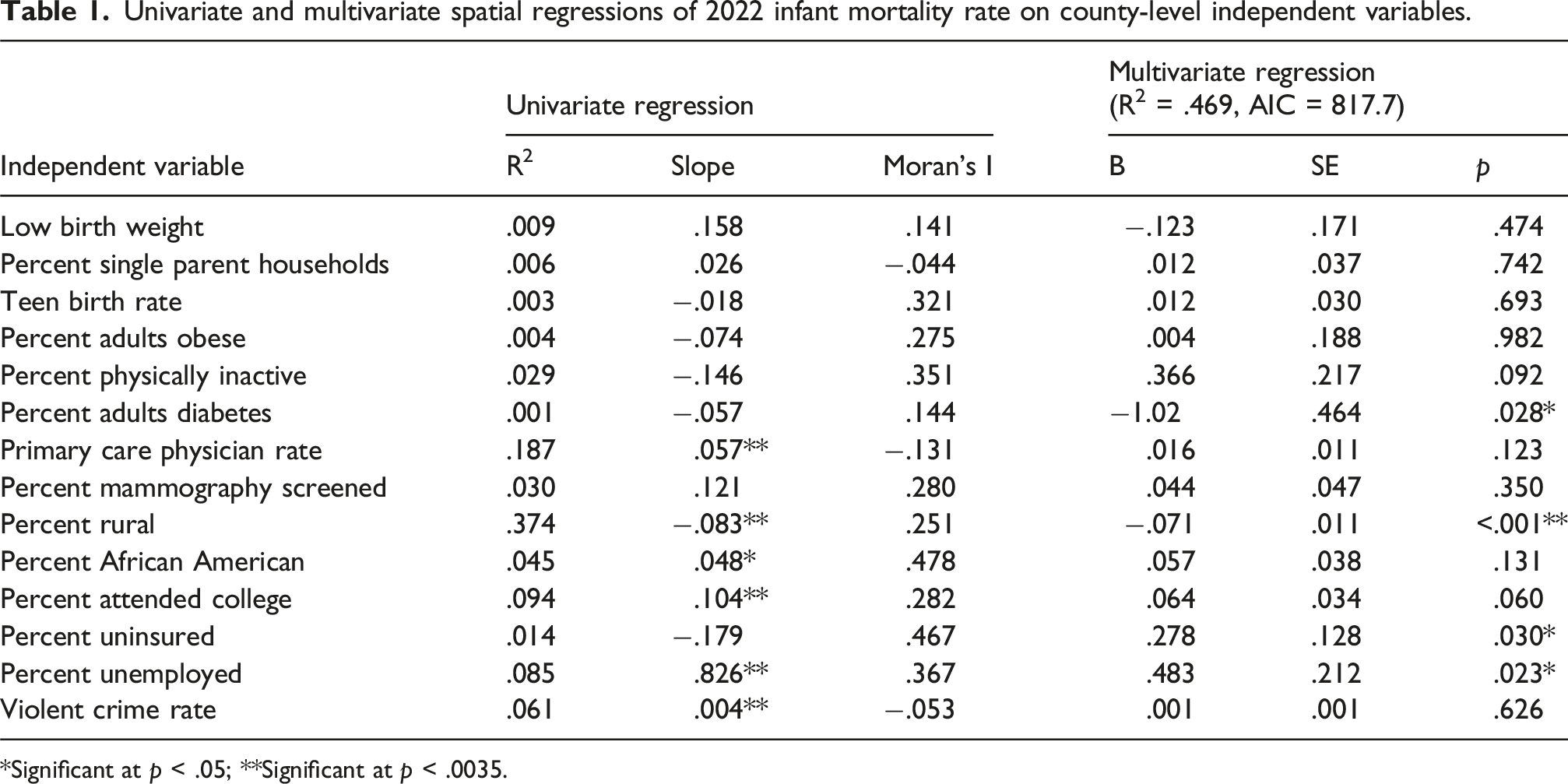
*Significant at p < .05; **Significant at p < .0035.
However, Moran’s I showed large positive clustering of counties with respect to IMR. This means that these counties tended to be nonrandomly located together. Moran’s I represents the slope of the spatial regression and corrects for correlation overestimates that occur when geographic variations are not addressed in ordinary least squares regression.33,34 For example, PCP Rate showed an unexpected positive but significant association with IMR on the OLS scatterplot slope, but the Moran’s I showed the expected negative association between clustering of counties with IMR (Table 1).
Besides PCP Rate, Percent Rural (negative), Percent Attended College, Percent Unemployed, and Violent Crime Rate had significant slopes/associations with IMR at p < .0035. Percent African American had a significant positive slope at p = .007. The negative associations for IMR with Primary Care Provider Rate and positive associations with Percent African American population were consistent with previous findings (Figure 1(b) and (c)).
Percent Rural, Percent African American, Percent Uninsured, Percent Unemployed, Percent Physically Inactive, Percent Adults Obese, Teen Birth Rate, Low Birth Rate, Percent Attended College, and Percent Adults with Diabetes each had strong, positive Moran’s I county clustering with IMR (Table 1, Figure 2). The multiple regression results for IMR on all 14 independent variables are shown in Table 1. The model R2 = .469 was strong, and additional statistics supported a robust model. Only one independent variable was significant at the Bonferroni-adjusted p < .0035: Percent Rural, but slope was negative. Three variables were significant at p < .03: Adults with Diabetes, Percent Uninsured, Percent Unemployed (Table 1). GIS Moran’s I and EB rate of IMR on each of six predictor variables. (a) PCP rate (b) Percent rural (c) Percent African American (d) Percent attended college (e) Percent unemployed (f) Violent crime rate.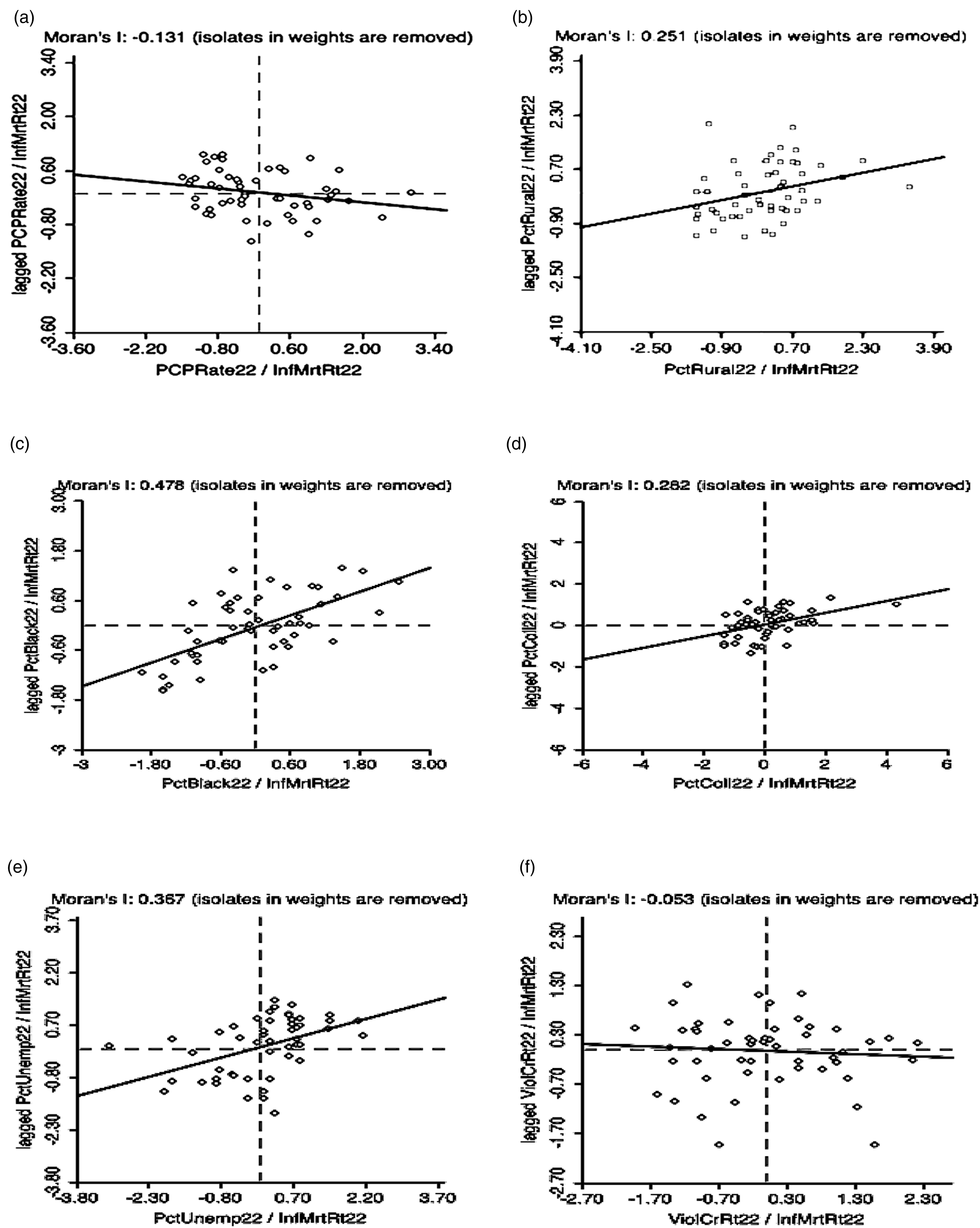
Hierarchical linear models
Hierarchical linear model trends for IMR are shown in Figure 3. Rural versus Urban IMR, 2015-2022, is shown in Figure 3(a). Individual county trajectories are shown, some increasing, some decreasing for both county categories. The smoothed mean county trajectories are shown, with the Urban mean slope starting at a lower level than Rural in 2015 and decreasing through 2022. In contrast, the Rural mean slope increased through 2022. (a) Infant mortality rates by urban (left) versus rural (right) counties, 2015–2022. Smoothed average county trajectories are shown by the darkened slope lines. (b) Infant mortality rates by low HPSA/High PCP counties (left), between adequate and shortage (middle), and high HPSA/low PCP shortage counties (right), 2015–2022. Smoothed average county trajectories are shown by the darkened slope lines.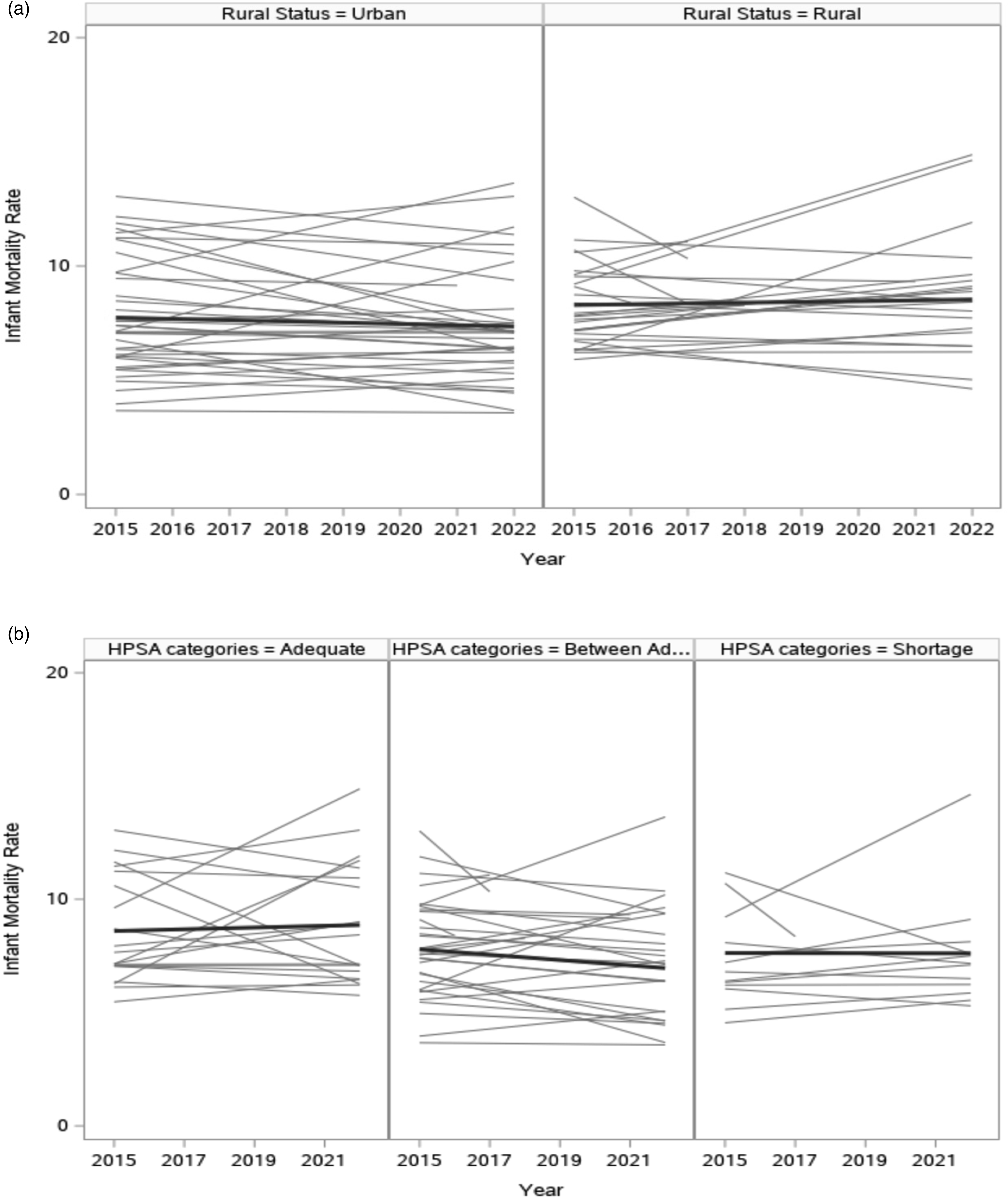
Likewise, three categories of HPSA counties are shown in Figure 3(b), with individual county and mean category trajectories shown. Interestingly, the low HPSA (i.e., Adequate PCP Rate <1000:1) counties showed slightly higher IMR with a gradual increase from 2015 to 2022. The Medium and High HPSA counties had lower IMR from 2015 to 2022, relatively flat for high HPSA although there was a steep negative slope for the Medium HPSA counties where the PCP Rate is between 1000 and 3000:1.
Infant mortality rate by rural county status (A) and HPSA county status (B) multilevel models for change statistics.
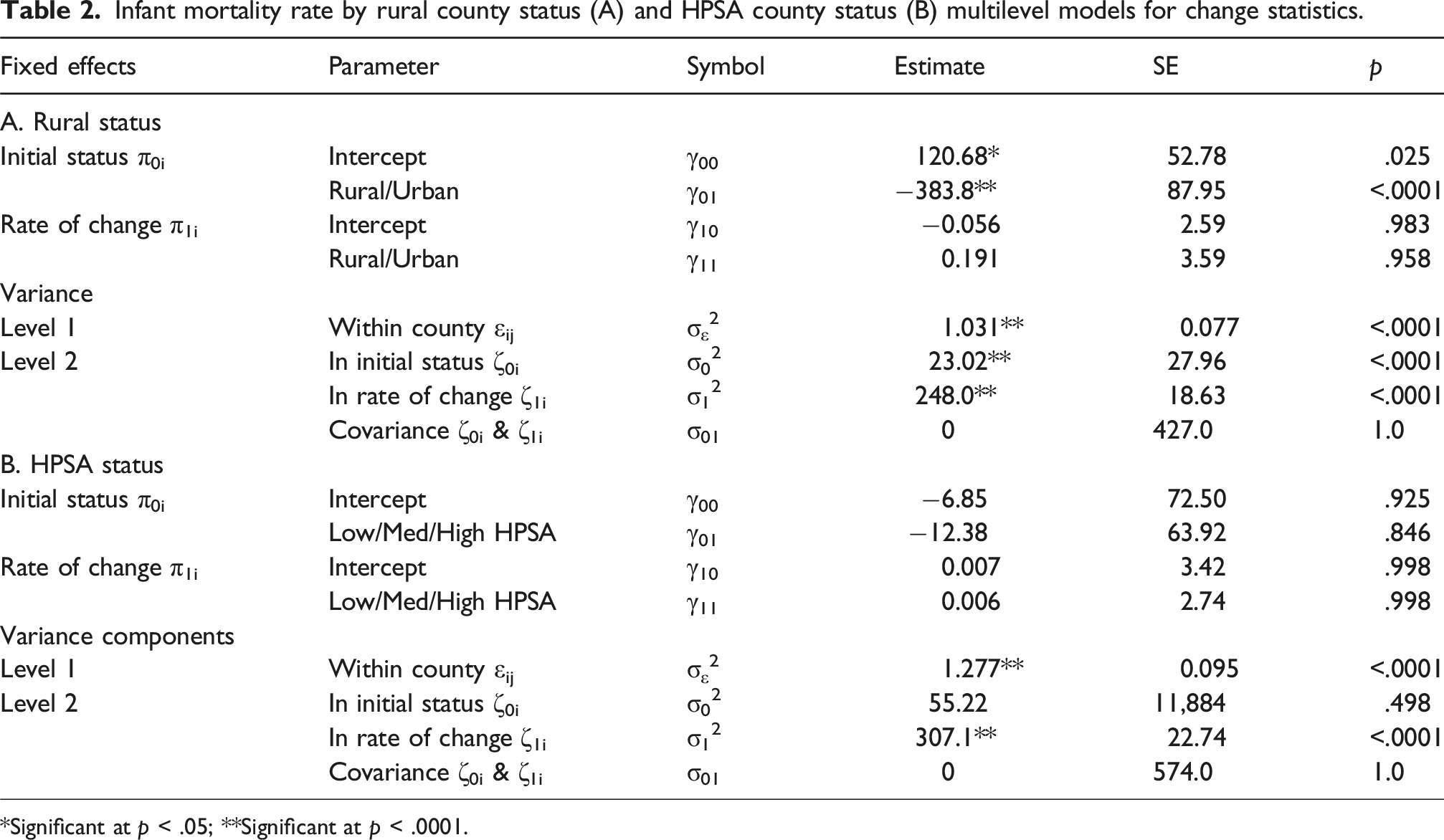
*Significant at p < .05; **Significant at p < .0001.
For the three group HPSA Multilevel Model statistics, the rate of change γ10 = 0.007 showed the relatively flat, slight positive slope for the high HPSA counties, as illustrated in Figure 2(b). The difference in county IMR slopes across the three groups was γ11 = 0.006, roughly flat when all three groups were considered together. Likewise, the initial statuses of the three groups are not significantly different. For the variance components of the level 1 and level 2 models, two variance components (σε2 and σ12) representing within county and rate of change residual variation were significant, indicating that there was substantial residual variation that remained in the true values of these two components after controlling for HPSA level. As before, an additional variable(s) might contribute with HPSA level to the multilevel time model of IMR, especially given the large variance component for rate of change.
Discussion
The 2022 spatial regression results showed significant IMR disparities between rural and urban Georgia counties, consistent with previous research findings and trends along the southeastern coastal plain for IMR and other health disparities. There were significant associations between IMR and rural counties as well as counties that have high African American populations, high unemployment, and high uninsurance rates. Principal Care Provider Rates showed a negative spatial regression relationship, as expected. The findings support previous studies that indicate a strong need for county-specific social capital interventions, health programs, improved housing, etc.11,13,14
From a temporal perspective, the Rural/Urban hierarchical linear model reiterates this rural/urban dichotomy from 2012 to 2022. The IMR slope for 120 rural Georgia counties is increasing, whereas the urban IMR slope is decreasing. The HPSA model is less clear, although the medium need counties (PCP Rates between 1000 and 3000:1) demonstrate a period IMR decline. It is possible that the higher IMR rates for low need counties (PCP Rates <1000:1) that are increasing might be due to the presence of high disadvantaged populations within urban counties: a population density effect.
The complementary geospatial and longitudinal, temporal analyses used in this study support previous findings5–14,17,18 that show regional socioeconomic risk factors that associate with higher infant mortality rates. These trends persist over time, and they show worsening outcomes in many rural counties. Maternal and child health outcomes in rural Georgia and across the southeastern United States are further complicated by the prevalence of health professional shortage areas (HPSAs), with the concentration of pediatric, mental health, and other medical specialists in urban areas. Many rural counties have no such specialists and rely heavily on a few general practitioners.
The study demonstrates the advantages of using both spatial and temporal analyses to assess population health trends. These approaches are straightforward to implement, and they can be valuable to clinicians, policymakers, and researchers to improve the health of rural communities. The spatial approach improves upon OLS regression methodologies to show regional clusters in measured variables. The temporal approach using hierarchical linear models not only displays time trends but also statistically evaluates both within county variation as well as between county variation, coupled with nesting effects within larger groupings (e.g., Rural vs Urban). Such hierarchical linear models have rarely been applied in public health research, and never with county-level data. Such approaches have been extensively used in educational and economic research and planning.21,35
The high association rates between IMR, rurality, high minority, and low socioeconomic conditions mirror other chronic health problems confronting communities. Health disparities and overall poor health ratings in communities strongly correlate with poor socioeconomic conditions. Public health approaches could benefit from stronger partnerships with business/industry, economic planners, and state and local governments to target rural county infrastructure and opportunities for citizens.
Limitations of this study include: (a) Missing data such that some IMR comparisons were for 2015–2022 instead of all 11 years data 2012–2022; (b) data source limitations in the County Health Rankings and Roadmaps, which vary from nationally-representative data to public health departments, the latter of which might be biased towards certain population groups in varied counties; (c) variations in choice of Queen contiguity levels and alternative methods of weighting that are available for geospatial regression analyses; and (d) nonreporting from 36 or more Georgia counties on IMR or other variables, particularly in rural areas that were strategic to the assessed models.
Future research directions should examine the possibility of truly merging spatial and longitudinal methodologies to better assess spatiotemporal clusters. Applications from this research include state and local government, business, education, and health department partnerships to improve health programs for expectant families to provide resources and supports to reduce IMR and other health risks. Most importantly, there is a need for county-level investments to lift residents out of cycles of poverty and disadvantaged conditions that lead to poor health.
Conclusion
In summary, research indicates that infant mortality and other negative health outcomes cluster in geographic areas both at the state and county level, and they are strongly impacted by geographic-specific socioeconomic factors. Besides geospatial regression of infant mortality factors in static time, the study originally adds a longitudinal component across 11 years of data and tests these temporal trends within potential group nesting effects. Major contributors to Georgia infant mortality rates included high percentage unemployed, high rurality, percentage African American population, and violent crime rates. The study findings strongly indicate the need for public health infrastructure and socioeconomic supports in rural counties to reduce infant mortality.
Footnotes
Ethics approval
This study used secondary analysis of data that is publicly available online.
Author contributions
DH contributed all study and manuscript components, including conceptualization, methodology, analysis, investigation, and writing.
Funding
The author received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The author declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
All data is available upon request.