Abstract
Introduction:
The clitoris is a vital organ for female sexual arousal, and adequate blood flow is essential for its function. L-citrulline, a precursor to L-arginine, boosts nitric oxide (NO) production, potentially enhancing blood flow. This study aimed to evaluate the effect of a topical gel containing L-citrulline and L-arginine on clitoral blood flow in healthy women.
Methods:
Five female volunteers aged 24-32 participated in this pilot study. The topical gel was applied externally to the vulva. Doppler ultrasound was used to measure clitoral length, clitoral volume, peak systolic velocity (PSV), resistive index (RI), and pulsatility index (PI) before and after gel application.
Results:
Significant increases were observed in clitoral length (20 mm-24 mm, P < .001), volume (0.13 mm³-0.3 mm³, P = .002), and PSV (7.1 cm/s-16.7 cm/s, P = .004) at five minutes post-application. RI and PI decreased from 0.9 to 0.6 (P < .001) and from 2.8 to 1.3 (P = .003), respectively.
Conclusion:
Topical L-citrulline and L-arginine gel significantly improves clitoral blood flow, suggesting its potential as a non-invasive treatment for enhancing sexual function in healthy women. Further research is required to evaluate how clinicians can use these findings to counsel patients about using gels to increase clitoral blood flow.
Introduction
The clitoris is a critical component in female sexual arousal and orgasm, consisting of erectile tissue that becomes engorged with blood during arousal. Adequate blood flow to the clitoris is essential for optimal sexual function, as demonstrated by significant correlations between clitoral tissue perfusion and various aspects of female sexual function, including arousal, lubrication, orgasm, and satisfaction. 1 Enhanced blood flow to the clitoris is linked to increased sensitivity, evidenced by decreased clitoral vibratory sensation thresholds during arousal and following orgasm. 2
L-arginine, an amino acid known for its role in nitric oxide (NO) production, has been widely studied for its potential to enhance sexual function through improved blood flow. Topical application of L-arginine can increase clitoral blood flow and improve sexual arousal in women with sexual dysfunction. 3 L-citrulline, a precursor to L-arginine, also boosts NO production and offers several advantages, including better absorption and a longer-lasting effect on NO levels. 4
Our study aims to assess the effectiveness of a topical gel containing L-arginine and L-citrulline in promoting clitoral blood flow. We hypothesize that topical application of this gel will significantly enhance clitoral vascular perfusion, potentially contributing to improved sexual arousal.
Methods
Study Design and Participants
This cross-sectional pilot study was designed to evaluate the effect of the topical study gel, which contains L-citrulline and L-arginine gel (Enchantment Gel, CERĒ, USATM), on clitoral blood flow. Five healthy female volunteers aged 24-32 were recruited to participate in the study. Participants were fully informed about the study procedures and provided written informed consent before participation. This investigation was conducted in accordance with the Code of Ethics of the World Medical Association (Declaration of Helsinki).
Intervention
Outcome Measures
Ultrasound was selected as the imaging modality for this case due to its efficiency, low cost, and versatility in evaluating the clitoris, making it suitable for use in any clinical setting. Sonographic assessments of the clitoris were performed using a Samsung WS80A ultrasound machine with an L3-12 A linear array transducer. The following parameters were measured at each time point: clitoral length (CL), clitoral volume (CV), peak systolic velocity (PSV), resistive index (RI), and pulsatility index (PI).
These measurements were used to assess clitoral blood flow both qualitatively (via color Doppler images) and quantitatively (using PSV, RI, and PI of the deep artery of the clitoris).
Procedure
Baseline sonographic assessments were conducted prior to study gel application. For baseline images, neutral ultrasound gel (without L-arginine and L-citrulline) was used. Participants then self-applied approximately~4 cc of the study gel topically to the vulva, and sonographic measurements were repeated at 3, 5, and 7 minutes after application. Images of each parameter were captured and stored for analysis. A uniform light pressure was applied with the transducer, as heavier pressure could skew blood flow. All ultrasounds were performed by the same radiologist for consistency. Volunteers were asked to report any adverse effects such as pain, numbness, burning, rash, or itching at all time points.
Statistical Analysis
To assess the impact of gel application on the dependent variables, a two-step analysis approach was employed. A permutational multivariate analysis of variance (PERMANOVA) was conducted to evaluate the overall multivariate effect of the gel application on the dependent variables across the different time points.
Results
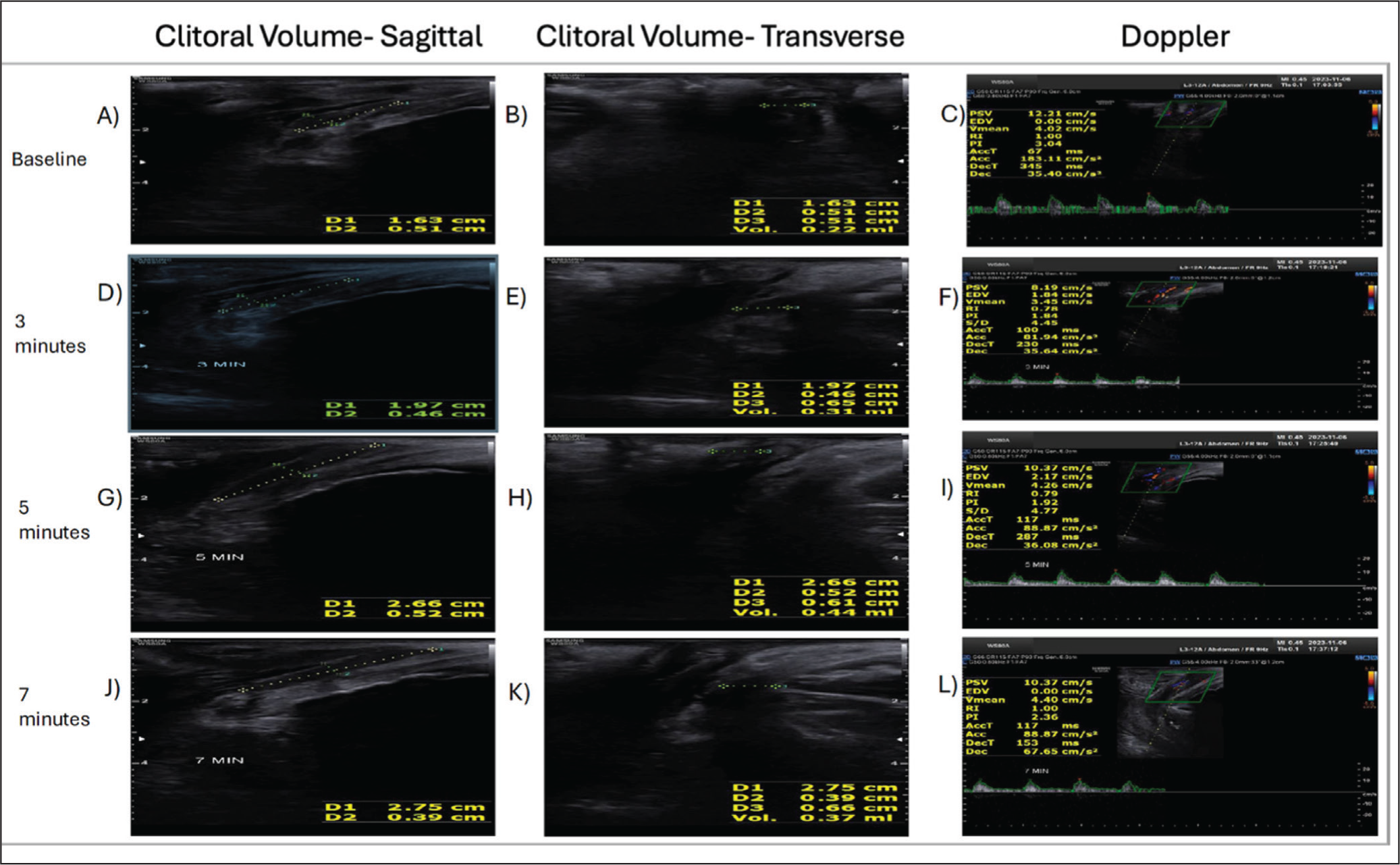
Five healthy female volunteers aged 24-32 years without a history of sexual dysfunction participated in the study. The median baseline CL was 20 mm, CV was 0.13 mm3 and and PSV was 7.11 cm/s, while RI and PI were 0.9 and 2.8, respectively (Table S1). There were statistically significant changes in all parameters at 5 minutes after application of the gel. The median CL increased from 20 mm at baseline to 24 mm at 5 minutes after gel application (P < .001). The median CV increased from 0.13 mm³ at baseline to 0.3 mm³ at 5 minutes post-application (P = .002). PSV increased from a baseline median of 7.1 cm/s-16.7 cm/s at 5 minutes post-application (P = .004). A significant decrease in RI was observed at 5 minutes post-application (P < .001), with the median RI dropping from 0.9 at baseline to 0.60 at 5 minutes. PI also significantly decreased, with a median value of 1.3 at 5 minutes post-application (P = .003), compared to 2.8 at baseline. Representative images for grayscale ultrasound (transverse and sagittal views of the clitoris), as well as qualitative and quantitative (PSV) color Doppler flow, are demonstrated at baseline (Figure 1A-C), 3 minutes (Figure 1D-F), 5 minutes (Figure 1G-I), and 7 minutes (Figure 1J-L).
PERMANOVA analysis demonstrated significant multivariate effects between the baseline and 5-minute post-application time points (P = .036). No significant changes were found in comparisons between other time points.
Ultrasound Images of Clitoral Volume and Doppler Measurements at (A) Baseline, (B) 3 mins, (C) 5 mins, and (D) 7 mins.
Discussion
Our study finds that topical application of the study gel containing L-arginine and L-citrulline leads to a measurable increase in clitoral blood flow at 5 minutes, which returns to baseline at 7 minutes. The results demonstrated significant increases in CL, CV, and PSV, alongside significant decreases in RI and PI at five minutes post-application. These findings suggest that topical application of the study gel on the clitoral area led to an increase in blood flow. These findings could suggest a role in potentially improving sexual function.
We build on previous research investigating the use of NO in clitoral blood flow. Lovie et al described a case report in a single volunteer where a gel containing both L-citrulline and L-arginine was evaluated. They demonstrated a significant increase in clitoral blood and PSV at 5-15 minutes after application, thus supporting the efficacy of NO donors in increasing clitoral vascularization. 5 Another study by Souto et al showed that a topical S-nitrosoglutathione (GSNO) gel significantly increased clitoral blood flow, with notable improvements in both systolic and diastolic speeds, as well as resistance in the clitoral arteries. This study also highlighted the safety of NO-based treatments, with no adverse effects reported. 6 Another study explored the neurovascular mechanisms underlying clitoral erection, identifying that NO-mediated relaxation of clitoral smooth muscle is facilitated by cyclic guanosine monophosphate-dependent protein kinase and large-conductance, calcium-activated potassium channels. This pathway mirrors penile erection and emphasizes the physiological rationale for using NO donors such as L-citrulline and L-arginine to enhance clitoral blood flow. 7 Additionally, Oliver et al focused on the regulation of endothelial NO synthase (eNOS) activity in the clitoris. They revealed that eNOS activation is critical for increasing clitoral blood flow during sexual arousal. Their research also highlighted the role of GSNO reductase (GSNO-R) in modulating NO availability, suggesting that disruptions in this pathway could contribute to sexual dysfunction. 8
The improvements in clitoral blood flow observed in our study can be attributed to the role of L-arginine and L-citrulline in enhancing NO production. Nitric acid, as a potent vasodilator, facilitates the relaxation of smooth muscle cells in vascular walls, increasing blood flow to erectile tissues, including the clitoris. The reduction in RI and PI values supports the vasodilatory effects of the study gel, indicating improved perfusion and reduced vascular resistance.
Clinically, these findings suggest that L-citrulline and L-arginine-containing gel helps increase clitoral blood flow. Further studies are needed to determine the impact of this on overall sexual function. Our pilot study is not without its limitations. The small sample size of five participants limits the generalizability of the findings. Additionally, the open-label design introduces potential bias, as participants were aware of the treatment they were receiving. Lack of blinding for the radiologist performing the scans can further cause bias. Future studies should include larger cohorts, potentially employ randomized, double-blind designs, and subjective outcomes to validate these findings.
Conclusion
In conclusion, this pilot study suggests that the topical study gel containing L-citrulline and L-arginine is effective in enhancing clitoral blood flow, with potential implications for improving sexual arousal in women. However, further research is needed to confirm these findings, explore the long-term effects, and investigate the gel’s efficacy in a broader population.
Supplemental Material
Supplemental material for this article available online.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
Our study was conducted in accordance with the Code of Ethics of the World Medical Association (Declaration of Helsinki).
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
All participants signed written informed consent.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
