Abstract
Inherited retinal diseases (IRDs) are a genetically and phenotypically heterogeneous group of genetic eye disorders. There are more than 300 disease entities, and together this group of disorders affects millions of people globally and is a frequent cause of blindness or low-vision certification. However, each type is rare or ultra-rare. Characteristically, the impaired vision in IRDs is due to retinal photoreceptor dysfunction and loss resulting from mutation in a gene that codes for a retinal protein. Historically, IRDs have been considered incurable and individuals living with these blinding conditions could be offered only supportive care. However, the treatment landscape for IRDs is beginning to evolve. Progress is being made, driven by improvements in understanding of genotype–phenotype relationships, through advances in molecular genetic testing and retinal imaging. Alongside this expanding knowledge of IRDs, the current era of precision medicine is fueling a growth in targeted therapies. This has resulted in the first treatment for an IRD being approved. Several other therapies are currently in development in the IRD space, including RNA-based therapies, gene-based therapies (such as augmentation therapy and gene editing), cell therapy, visual prosthetics, and optogenetics. RNA-based therapies are a novel approach within precision medicine that have demonstrated success, particularly in rare diseases. Three antisense oligonucleotides (AONs) are currently in development for the treatment of specific IRD subtypes. These RNA-based therapies bring several key advantages in the setting of IRDs, and the potential to bring meaningful vision benefit to individuals living with inherited blinding disorders. This review will examine the increasing breadth and relevance of RNA-based therapies in clinical medicine, explore the key features that make AONs suitable for treating genetic eye diseases, and provide an overview of the three-leading investigational AONs in clinical trials.
Keywords
Introduction
Globally, an estimated 43.4 million people are blind and another 295 million have moderate-to-severe visual impairment. 1 Around one-third of cases of blindness or severe visual impairment have a genetic basis, either as part of a multifactorial etiology, for example, as in age-related macular degeneration, diabetic retinopathy, or glaucoma, or as the direct result of genetic mutations, such as in inherited retinal diseases (IRDs), inherited corneal dystrophies, or optic neuropathies.2,3
IRDs are a genetically and phenotypically heterogeneous group of genetic eye disorders. There are more than 300 disease entities, and together this group of disorders affects at least 1 in 1400 individuals, or around 5.5 million people worldwide.4–9 However, each type is rare or ultra-rare. Despite the lack of global data documenting the overall disease burden of IRDs in terms of loss of sight, studies in the United Kingdom and Australia show that they account for around 6% of blindness or low-vision certifications, 10 12% among children (making it the second most common diagnosis), and 20–23% among individuals of working age (making it the most common diagnosis). Cost of illness (blindness) studies in the Republic of Ireland and in the United Kingdom estimate total costs of £42.6 and £523.3 million, respectively, in 2019. 11 Well-being costs accounted for approximately one-third of these sums, illustrating the significant impact sight loss has on the individual with an IRD.
The impaired vision in IRDs is due to retinal photoreceptor dysfunction or loss resulting from mutation in a gene that codes for a retinal protein.8,12,13 The precise phenotype of each IRD depends on the role of the affected protein, which may include phototransduction, photoreceptor morphogenesis and maintenance, photoreceptor ciliary transport, or the retinoid cycle. 13 Other body systems may also be implicated if the aberrant protein synthesis impacts tissues other than the retina: IRDs that affect other systems, such as hearing, are known as syndromic disorders. 14
Historically, IRDs have been considered incurable and individuals living with these blinding conditions could only be offered supportive care to treat associated complications, such as cataracts and macular edema, or in some cases with nutritional adjustments.15,16 However, the treatment landscape for IRDs is changing. Progress is being made, driven by improvements in understanding of genotype–phenotype relationships, through advances in molecular genetic testing and retinal imaging. 13 Alongside this expanding knowledge of IRDs, the current era of precision medicine is fueling a growth in targeted therapies. This has resulted in the first treatment for an IRD being approved in 2017 in the United States and in 2018 in Europe.17,18 Voretigene neparvovec-rzyl (Luxturna®; Spark Therapeutics Inc.) is a gene therapy for adult and pediatric patients with vision loss due to IRD caused by biallelic mutations in the retinoid isomerohydrolase (RPE65) gene. 18 This approval represents a landmark change for individuals living with an IRD. However, voretigene neparvovec-rzyl is applicable only for patients with RPE65-related IRD, and only in those with sufficient viable retinal cells.17,18 Consequently, there remains a pressing medical need for treatment options for people with a genetic eye disease outside of this small subset of patients. Several other therapies are in development in the IRD space, building on the success of voretigene neparvovec-rzyl, including DNA-based therapies (such as augmentation therapy and gene editing), RNA-based therapies, cell therapy, visual prosthetics, and optogenetics.19,20
RNA-based therapies are a novel approach within precision medicine that have demonstrated success, particularly in rare diseases; 21 and a number of therapies are currently in development for the treatment of IRDs. This review will examine the increasing breadth and relevance of RNA-based therapies in clinical medicine and, more specifically, in ophthalmology, explore the key features that make such therapies suitable for treating genetic eye diseases, and provide an overview of investigational RNA-based therapies for IRDs that have reached clinical trials.
RNA-based therapies
Ribonucleic acid (RNA) is produced from deoxyribonucleic acid (DNA) via the transcription process. There are different types of RNAs, some of them called coding RNAs (e.g. mRNAs) are involved in protein synthesis while some others, the non-coding RNAs (ncRNAs), do not code for proteins but may modulate gene expression.22–24 The ncRNAs, such as microRNAs (miRNAs), long non-coding RNAs (lncRNA), silencing RNAs (siRNAs), etc., are involved in a variety of biological functions. For example, they regulate gene expression and translation, RNA processing, and translation levels; they protect genomes from foreign nucleic acids; and they can guide DNA synthesis or genome rearrangement.22–24 Within the context of genetic diseases involving protein disruption, coding RNAs have been considered a potential therapeutic target for more than four decades; the correction at the RNA level of changes induced by a pathogenic variant in the DNA could restore normal protein production or stop pathogenic protein production.22,23 A class of non-coding RNAs regrouped under a competing endogenous RNA (ceRNA) network can target coding and non-coding RNA molecules and indirectly regulate each other by competing for them. Thus, leading to an additional post-transcriptional regulatory layer accomplished by non-coding RNAs. However, ceRNAs are also involved in the pathogenesis of several diseases. 25 Further understanding this ceRNA network may provide a base to identify potential therapeutic targets or new prognostic biomarkers.26,27
There are several categories of RNA-based therapies, including single-stranded antisense oligonucleotides (known as AONs or ASOs), double-stranded small interfering RNAs, mRNAs, and aptamers.21,28,29 RNA-targeting small molecule drugs are not considered RNA-based therapies per se because these are not analogs of nucleic acid polymers. 30 Not including vaccines, 13 RNA-based therapies have already been approved across several therapeutic areas, but none of them for IRDs (Table 1).21,29,31,32 These include one aptamer (pegaptanib; for age-related macular degeneration) and three small interfering RNAs (patisiran, givosiran, and lumasiran; all for hepatic conditions). However, the majority of approvals are among the family of AONs; these comprise fomivirsen (to treat cytomegalovirus-induced retinitis) and eight therapies for hereditary conditions, including familial hypercholesterolemia, Duchenne muscular dystrophy, spinal muscular atrophy, hereditary transthyretin amyloidosis, and familial chylomicronemia syndrome.21,29,32,33 In addition, more than 400 drug development programs for RNA-based therapies are underway across a variety of ocular and non-ocular areas, but predominantly for oncology. 21 Within this pipeline, several RNA-based therapies are being investigated for IRDs, all of which are AONs. Because AONs can target a patient-specific mutation, there is also precedent for ‘N-of-1’ use of patient-specific AONs. 34
Summary of approved RNA-based therapies.a21,29,31,32

Source: EMA and FDA websites.
Approval status as of August 23, 2021.
AON: antisense oligonucleotide; CMV: cytomegalovirus; EMA: European Medicines Agency; FDA: Food and Drug Administration; IV: intravenous; SC: subcutaneous.
Excluding RNA-based vaccines.
Discontinued due to lack of commercial interest.
Withdrawn from use due to reduced clinical need.
AONs are short lengths of chemically stabilized single-stranded RNA or DNA that modify the expression of a given nucleotide sequence by binding to target pre-mRNA or mRNA via base pairing.28,32,33,35 They act on the processing of the mutant RNAs to suppress the defects that result in abnormal synthesis or function of proteins, and thereby slow down or reverse the course of an associated disease.28,36 The precise mechanism of action depends on the AON; for example, they can be engineered for pre-mRNA splicing correction, exon skipping, or mRNA knockdown.28,32,33,35
Under normal circumstances, genes are transcribed into pre-mRNA transcripts, comprising exons holding the genetic code required to synthesize a protein, separated by non-coding introns. Splicing removes the introns from the pre-mRNA to generate the mature mRNA that is then translated into the protein (Figure 1(a)).33,35 Splicing defects can arise, for example, due to deep-intronic mutations that generate a new splice donor or acceptor site in the intron, which leads to retention of a part of that intron during splicing, and thereby its inclusion in the mature mRNA (i.e. insertion of a pseudoexon).33,35 Such is the case in CEP290-associated IRD, as described later in this article. The addition of this pseudoexon leads to either nonsense-mediated mRNA decay and therefore an absence of protein production, or synthesis of an abnormal protein. 33 By binding to the deep-intronic mutant region, AONs can modulate splicing and prevent inclusion of the pseudoexon and the resultant disruption of protein synthesis (Figure 1(b)). 33 AONs can also be designed to bind to splice sites or regulatory elements on a target exon to prevent recruitment of splicing factors, causing skipping of that exon during RNA splicing.28,33 This design stops mutation-containing exons being incorporated into the mature mRNA (Figure 1(c)). This strategy is relevant for USH2A mutations discussed below.
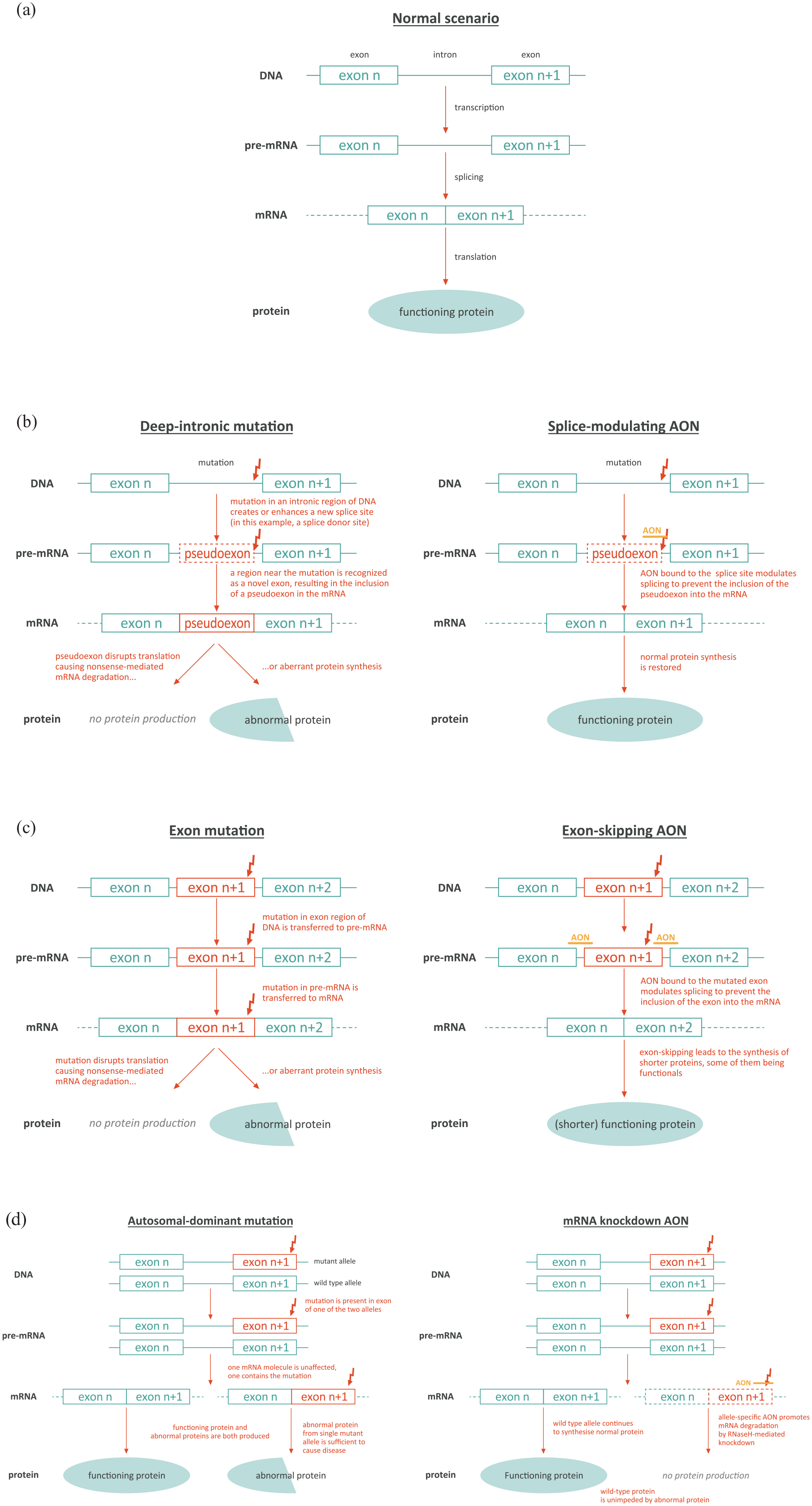
Mechanisms of action of AONs in genetic eye disease. (a) Wild-type scenario. (b) AON correcting deep-intronic mutation. (c) AON inducing exon skipping. (d) AON producing mRNA knockdown (adapted from Collin 2017). 33
In some autosomal-dominant conditions, such as autosomal-dominant retinitis pigmentosa (adRP) detailed below, protein production from a single mutant allele is sufficient to manifest disease (i.e. dominant negative effect), despite the presence of a normal allele that produces normal protein. In these circumstances, AONs can be used to trigger allele-selective degradation or ‘knockdown’ of mutant mRNA transcripts, so that the wild-type allele can continue to produce wild-type protein unhindered. 33 In this approach, the AON is designed to recognize the mutant allele and activate the enzyme RNase H (which is involved in the degradation of transcripts) at the level of the (pre-)mRNA, to reduce the number of mutant mRNA transcripts, and therefore the amount of mutant target protein (Figure 1(d)). 32 Further applications of AONs include base editing of the RNA to directly change individual sites (e.g. to correct G > A mutations) and repeat-targeting to prevent the toxic effects caused by expanded, non-coding trinucleotide sequences in RNA.37,38
Characteristics of AONs in genetic eye diseases
RNA therapies, such as AONs, can be considered a form of genetic therapy as they are highly specific and target the underlying genetic cause of a disease.5,28,32,39 RNA-based therapy and DNA-based therapy (gene therapy), are two different approaches. 32 They differ in several ways including mechanism of action, permanency of effect, and delivery to the target cells.32,39 Table 2 summarizes the key differences between AONs and DNA-based therapy in the setting of genetic eye diseases and these are discussed below.
Key differentiating features of RNA- and DNA-based therapies.

RNA: ribonucleic acid; DNA: deoxyribonucleic acid; DSB: double-strand breaks; IRD: inherited retinal disease.
Act at the RNA level and do not alter the genome
AONs make transient alterations to the RNA without altering the genome. 32 At a maximum, splice-modulating AONs restore normal levels of target mRNA and do not bring a risk of overexpression of target protein that may cause cellular toxicity.36,50 DNA-based therapies act at gene level and could make changes or additions to the DNA. 32 The principal forms of DNA-based therapy are gene augmentation therapy which uses vectors (such as adeno-associated viruses; AAVs) to insert a normal, non-mutated cDNA copy of the optimized coding sequence of the target gene into the host cells; and gene editing therapy, which corrects defects in the genetic sequence of the mutated gene using clustered regularly interspaced short palindromic repeats (CRISPR) technology.5,39,51 Wild-type AAVs integrate into the host DNA. When recombinant AAV vectors are used, the genomic DNA is not modified and the introduced genetic sequence is very rarely integrated into the host DNA; instead, it typically coexists as a so-called episome in the nucleus of the target cell.5,39,40 This is the case with the gene augmentation therapy voretigene neparvovec-rzyl, which uses AAV serotype 2 (AAV2) to carry a functional cDNA copy of the RPE65 gene into the retinal pigment epithelial cells in individuals who have reduced or absent RPE65 protein due to biallelic RPE65 mutations.5,18 With lentivirus vectors, random integration into the genome can occur, which may be associated with a risk of insertional mutagenesis potentially affecting a tumor suppressor gene, leading to cancer.5,52 However, the risk of malignant transformation is probably low with insertion in non-dividing cells, such as the neurosensory retina. Gene editing, by definition, makes changes directly to the genomic DNA of the mutated gene.5,51,40 The risks associated with this approach have not yet been fully elucidated.
Long-lasting effect but non-permanent nature
AONs are similar to drug therapies in that their duration of effect depends on their half-life and clearance rate. 41 This means that repeated administration is required, and this could have implications for patient safety and convenience and for healthcare resource utilization costs. For AONs used in the eye, repeat treatment is relatively infrequent; currently twice per year. 36 This is because, unlike other target cells, retinal cells are post-mitotic, enabling AONs to have a long-lasting therapeutic effect. 53 Also, the chemical modification of the AONs, such as the inclusion of phosphorothioate (PS) backbone, the attachment of the 2′-O-methoxyethyl or 2′-O-methyl group to the sugar residues of the PS backbone, and the formulation of emulsification drops, ensures a long half-life, preserves the AONs from early degradation, and therefore ensures prolonged response. 33 Conversely, the transient nature of both RNA and AONs means the AON effects are somewhat reversible.36,41 It may, therefore, be possible to adjust the strength of the effects by modifying subsequent dosing (if required), and potential side effects might be transient.41,45
DNA-based therapies are assumed to be a one-time therapy. The durability of DNA-based therapies in ophthalmological settings has not yet been categorically shown; long-term data for voretigene neparvovec-rzyl extend only up to 4 years post-treatment to date. 42 Other DNA-based therapies aimed at RPE65-associated Leber congenital amaurosis (LCA) have shown variable durability of effect, in some cases, reporting subsequent declining visual efficacy alongside persisting degenerative loss of photoreceptors.43,44,54 If these therapies prove to be permanent when targeting non-dividing cells, this could represent an advantage in patient burden in terms of requiring only one-off surgery, albeit with one eye treated at a time. This single intervention will require thorough assessment to identify the appropriate dosing prior to surgery, especially taking into account individual variation, to achieve maximum benefit while avoiding any permanent side effects.
Do not require vectors for delivery
AONs can be administered as naked molecules as the chemical modifications and the optimized formulation ameliorate their cell uptake. As such, vectors are not needed and this approach is not hampered by limitations of vector capacity or vector-associated intraocular inflammation.45,55,56 Their relatively small size means that AONs may provide therapeutic benefit and restore protein function in diseases in which gene sequences are too large to be delivered via AAV2 (e.g. ABCA4 for Stargardt disease and MYO7A or USH2A associated with Usher syndrome) or other acceptable viral vectors used in gene augmentation therapy.52,57 It should be noted that dual-vector strategies with the potential to overcome this limitation are currently in preclinical development. 58 Both approaches offer alternatives and more potential therapeutic options for the patients.
Administered via intravitreal injection
AONs can be administered via an intravitreal injection.28,59 This method is low-risk, fast, and convenient and can be performed in a clinic or office setting with topical anesthesia depending on patient age and acceptance.47,48 Intravitreal administration is known to be less invasive than subretinal delivery which is required for many AAV gene augmentation therapies. It has a low rate of procedural complications, including intraocular inflammation which could represent an advantage for the patients.39,46,49,52,53,60 It must be noted that cataracts occur with intravitreal treatments. 60 Subretinal delivery requires, in most cases, a general anesthetic and is relatively invasive, entailing removal of vitreous via pars plana vitrectomy, retinotomy, temporary retinal/macular detachment, and then injection of the therapy into the subretinal space.18,49 Attempts to deliver AAV gene augmentation through intravitreal route have so far not proven successful and have led to intraocular inflammation. 61 Individuals receiving subretinal voretigene neparvovec-rzyl require the retina to be > 100 microns thick at the posterior pole. 17
Broad distribution within the retina
The optimal mode of delivery for an IRD treatment has not been fully defined. Intravitreal administration of a treatment allows broad distribution within the retina to reach a larger number of retinal cells.45,52 Furthermore, preclinical and early clinical data show that intravitreally administered AONs can be used to target the peripheral and central regions of the retina 50 and can reach all layers of the retina. 36 Therapies delivered to the subretinal space target mainly the macular region of the total retinal area. 45 More research is needed to understand whether there are any potential advantages of targeting the entire retina, and especially the periphery, in terms of whether this confers any potential for early intervention for AONs.
Low risk of systemic side effects
AONs used to treat genetic eye diseases are associated with limited off-target effects.28,36 This low risk of systemic side effects also applies to DNA-based therapies. This is due to several unique features of the eye. First, the small size of the eye means that only small doses are needed.5,19,51 Local delivery also enhances drug bioavailability which supports the use of low doses.5,59 Second, the eye is a closed compartment, so intravitreal and subretinal delivery methods have a lower rate of systemic side effects versus systemic administration, with blood–retinal barriers helping to prevent systemic spread.5,59 Third, the eye is highly compartmentalized, so treatment can be targeted to specific regions (e.g. subretinal space or vitreous cavity), thus reducing off-target exposure.5,19,51 However, despite delivery into the vitreous cavity, there is evidence of exposure of AONs anteriorly, even as far as the cornea. 62 Finally, as certain sub-compartments of the eye are the sites of immune deviation (referred to as immune privileged), treatments can be administered into the eye with reduced risk of provoking inflammation and immune-mediated damage.5,19,51
RNA-based therapies in development for IRDs
There are currently no approved RNA-based therapies for IRDs. Three investigational RNA-based therapies for IRDs are in phase I/II and II/III clinical trials: sepofarsen, ultevursen, and QR-1123 (Tables 3 and 4). All are AONs, developed by ProQR Therapeutics and Ionis Pharmaceuticals [in the case of P23H autosomal dominant retinitis pigmentosa treatment (QR-1123), and which is licensed to ProQR Therapeutics]. The ongoing studies will build on knowledge gained from both animal and preclinical research including studies using retinal organoids 36 and aim to validate results from these translational models within the clinical trial setting for each respective IRD.
Summary of clinical trials of RNA therapies in IRDs. a

adRP: autosomal-dominant retinitis pigmentosa; AON: antisense oligonucleotide; IVT: intravitreal; LCA: Leber congenital amaurosis.
According to planned, completed and ongoing trials listed on www.clinicaltrials.gov as of 29 April 2022.
Sepofarsen (formerly named QR-110)
Sepofarsen is being developed as a treatment for CEP290-associated IRD, also commonly referred to as LCA10. LCA comprises a group of heterogeneous disease subtypes classified according to the associated gene defect. 13 At least 25 genes that code for a diverse range of retinal functions have been linked to 17 phenotypes of LCA9,13 and more than 400 mutations have been implicated in these known phenotypes. 14 Additional subtypes exist but the gene defects are yet to be identified. 13 Typically, CEP290-associated IRD is inherited as an autosomal recessive trait.14,64 CEP290-associated IRD is the most common and severe subtype of LCA; it accounts for 15–30% of cases13,65–67 and has an estimated prevalence of < 1 patient per 100,000 individuals. 55 This subtype is linked to mutations in the centrosomal protein 290 (CEP290) gene, which encodes the CEP290 protein localized in the transition zone of the connecting cilium of photoreceptors68,69 located between the inner and outer segments of rods and cones.69,70 This ciliary transition zone transports proteins to and from the outer segment of the photoreceptor where phototransduction occurs to convert light into electrical signals and vision.69,70 CEP290 is required for normal ciliary function and photoreceptor survival.36,64,69
The most common disease-causing mutation in CEP290-associated IRD is c.2991 + 1655A > G (also known as p.Cys998*).13,67,71,72,73 This is present in at least one allele in 21–77% of individuals with CEP290-associated IRD.65–68,73 The c.2991 + 1655A > G point mutation activates a cryptic splice site in intron 26, resulting in the inclusion of a pseudoexon between exons 26 and 27 in the CEP290 mRNA. Within this aberrant exon is a stop codon that prevents expression of a functional protein, either by resulting in the degradation of the mRNA or in a truncated CEP290 protein.35,65 As a consequence of the absence of functional CEP290 protein, protein transport through the cilium is hampered and the outer segment of the photoreceptor degenerates and shortens in length, 64 the latter manifesting as a reduction in thickness in the outer nuclear layer in the peripheral to perifoveal region of the retina. Retained photoreceptor nuclei in the fovea with abnormal segments are also observed on optical coherence tomography (OCT). 64 Loss of integrity of the retinal layers is correlated with reduced visual function. 70 Electroretinography (ERG) responses are also undetectable, indicative of photoreceptor dysfunction.14,68 Interestingly, the photoreceptor degeneration progresses gradually over several decades; in the first decades of life despite widespread loss of rod photoreceptors, the foveal outer nuclear layer may be preserved.13,68,70 This suggests that a window of opportunity for early treatment may exist during which cone rescue could be possible.5,45,74
Symptoms of CEP290-associated IRD (which are also common to all LCA and EORD/EOSRD subtypes) include severe, congenital or early vision loss, nystagmus, and sluggishly reactive pupils. 14 Sight varies from bare light perception to 20/200 in most of the cases, although there are also subjects with milder progression and less dramatically reduced visual acuity until adulthood.68,71,75 At presentation, 64% of individuals with CEP290-associated IRD have vision classified as counting fingers or worse in the better-seeing eye. 73
Sepofarsen is a 17-mer single-stranded, fully phosphorothioated, and 2′-O-methyl-modified AON that has been designed to modulate RNA splicing by blocking the cryptic splice site, thus restoring normal splicing and normal CEP290 protein synthesis (Figure 2(a)). 36 In preclinical studies, sepofarsen restored normal CEP290 mRNA and protein expression in fibroblasts and retinal organoids derived from individuals with c.2991 + 1655A > G mutation in the CEP290 gene, and in animal models, this AON was able to reach all retinal layers. 36 The positive preclinical data from optic cup studies with sepofarsen have been substantiated by positive early clinical data, confirming these models to be a good predictor of clinical outcomes.

Mechanisms of action of (a) sepofarsen, (b) Ultevursen, and (c) QR-1123 detailing wild-type condition, mutant condition, and mechanism of action of AON.
The first-in-human, 12-month, phase Ib/II dose-escalation study of sepofarsen (PQ-110-001; NCT03140969) assessed the safety and efficacy of two doses of this AON in 11 individuals with CEP290-associated IRD aged ⩾ 6 years in the worse-seeing eye.57,76,77 Six participants received loading/maintenance doses of 160 µg/80 µg and five received 320 µg/160 µg. The final 12-month pooled data reported clinically meaningful improvements from baseline to Month 12 in treated eyes versus untreated eyes in best-corrected visual acuity (BCVA) (p < 0.05), red full-field stimulus test (FST) (p < 0.01), and blue FST (p < 0.02). There were also signals of improvement in functional vision as shown in composite mobility course score.57,77 The most common adverse events were cataracts; all participants who showed visual decline during cataract development regained pre-cataract visual acuity after lens replacement, with no procedural complications. 57 There were two cases of mild cystoid macular edema and two of retinal thinning (all with the 320 µg/160 µg regimen). 57 No study discontinuations occurred, 77 and no inflammation was observed. Based on efficacy observations at the first two dose levels, the 500 µg/270 µg dose was not initiated, and following safety assessment, the 320 µg/160 µg dose was discontinued.57,77
The Insight Study (PQ-110-002/NCT03913130) is an ongoing extension of the above study in which the same participants are receiving treatment of the contralateral eye and continued treatment of the first treated eye with sepofarsen 160 µg/80 µg every 6 months. Initial results from four patients showed the safety profile of sepofarsen dosed in the contralateral eye to be consistent with that observed in the phase Ib/II trial. Improvements in BCVA of ⩾ 0.8 logMAR were observed in two patients which was similar to the efficacy in the first treated eye. All four patients showed similar improvements in FST to those observed in the first treated eye. 78
Additional ongoing clinical trials of sepofarsen in CEP290-associated IRD include the phase II/III Illuminate study (PQ-110-003/NCT03913143) in adults and children aged ⩾ 8 years, and the phase II/III dose-escalation Brighten study (PQ-110-005/NCT04855045) in children aged < 8 years (Table 4). The phase II/III Illuminate study (PQ-110-003/NCT03913143) did not meet the primary endpoint nor notable secondary endpoints – and despite having good responders in the active treatment arms, no additional benefit was observed in either treatment arm versus sham in prespecified analyses. However, post hoc analyses reveal multiple pointers of a beneficial effect when comparing sepofarsen against sham group if the contralateral eyes of each group are adjusted for. 79 Sepofarsen showed to be generally well tolerated with a consistent safety profile as observed in the phase Ib/II trial (PQ-110-001; NCT03140969). Additional analyses are being conducted to understand the conflicting data observed in the sepofarsen trials.
Ultevursen (formerly named QR-421a)
Ultevursen is being developed for Usher syndrome and non-syndromic RP (nsRP) associated with biallelic USH2A mutations. USH2A mutations are the most common cause of autosomal recessive RP (implicated in 7–23% of cases), and the two most frequent mutations in USH2A are located in exon 13. 63
There are three main clinical types of Usher syndrome (numbered 1–3) varying in severity of vision and sensorineural hearing loss, age of onset, and involvement of vestibular dysfunction. Usher syndrome has been linked to mutations in 15 genes,8,14 and the pattern of inheritance is autosomal recessive. 14 USH2A mutations are linked to Usher syndrome type 2.63,80–82 In this subtype, hearing impairment is moderate to severe and vision is affected from the second decade of life. 81
Mutations within the USH2A gene disrupt the production of usherin protein which is localized in the connecting cilia of photoreceptors and stereocilia of cochlear hair cells (the sensory cells of the auditory system). 83 This protein is thought to be important for the structural maintenance of photoreceptors and normal development of cochlear hair cells. 84 Disrupted usherin protein production causes progressive photoreceptor degeneration beginning with the rods and eventually also involving the cones.81,84 In USH2A-associated nsRP severe visual impairment occurs by the age of 50 years. 85 Patients with Usher syndrome have an early decline in vision, beginning with night blindness and constricted visual field, followed by the loss of central vision and severe visual impairment.81,85 Congenital hearing impairment is seen in this syndromic form.81,84
Ultevursen is a 21-mer single-stranded, fully phosphorothioated, and 2′-O-(2-methoxyethyl)-modified AON that binds to USH2A pre-mRNA and modulates splicing by exon skipping to exclude exon 13 from the mature mRNA (Figure 2(b)). 63 This mechanism restores synthesis of a shorter but functional usherin protein.63,86
Preclinical proof-of-concept in vitro and in vivo studies have shown that the dose-dependent exon skipping induced by ultevursen is sustained at least 3 months, resulting in the restoration of usherin protein expression and functional ERG responses. 86
The Stellar study (PQ-421a-001/NCT03780257) is a first-in-human phase Ib/II single-dose, dose-escalation trial assessing the safety and efficacy of ultevursen by intravitreal injection in adults with biallelic USH2A pathogenic variants, with at least one mutation occurring in exon 13 (Table 4). 80 Interim data from unilateral treatment in 20 participants showed ultevursen to be well tolerated. 80 There were no serious adverse events or inflammation, one case of worsening of pre-existing cataract, and one case of progression of pre-existing cystoid macula edema. Ultevursen demonstrated encouraging levels of BCVA stabilization (i.e. there was no decline versus baseline), compared with a deterioration in the control eyes, in keeping with the natural history of the disease. 80 Treatment led to clinically significant improvements in retinal sensitivity as measured by the mean change from baseline in the number of loci that improved by ⩾ 7 dB on static perimetry in treated versus untreated eyes. 80 These findings were supported by objective retinal structural optical coherence tomography imaging. 80 The response to ultevursen was similar in all dose cohorts.
Participants from the Stellar study have been given the opportunity to enroll into the Helia extension study (PQ-421a-002/NCT05085964) for continued dosing and follow-up. This study will provide long-term safety, tolerability, and efficacy data of ultevursen. Following reported results in the Stellar study, a double-masked, randomized, sham controlled, 24-month, multiple-dose study, Sirius (PQ-421a-003; NCT05158296) has been initiated to further evaluate efficacy and safety of ultevursen.
QR-1123
QR-1123 is under evaluation as a treatment for adRP associated with the c.68 C > A mutation in RHO leading to a proline-to-histidine (P23 H; p.Pro23His) substitution. Around 15–25% cases of RP are inherited in an autosomal-dominant manner,14,87 and there are several subtypes of adRP. 87 At least 22 genes may be involved in adRP, 9 although the most commonly implicated is the RHO gene, which is responsible for 20–30% of cases of adRP.87,88 RHO codes for the rhodopsin protein, 87 a photosensitive protein when intimately bound to 11-cis-retinal, present in rods and essential for rod-based phototransduction. In turn, the most common mutation in RHO is c.68 C > A; p.Pro23His.88,89 This mutation is seen almost exclusively in the United States, affecting an estimated 2500–3000 individuals 89 and results in a P23H substitution in rhodopsin protein. 87 The mutated protein is misfolded, leading to progressive photoreceptor degeneration. 89 Like other forms of RP, adRP is characterized by rod–cone dystrophy with characteristic photoreceptor degeneration and intraretinal pigment migration predominantly in the mid-peripheral retina. 90 Retinal degeneration progresses from the mid-periphery to the macula and fovea, manifesting as night blindness, followed by progressive, concentric constriction of the visual fields, leading to tunnel vision and eventually blindness. 91
QR-1123 is an allele-specific, RNase H1-activating AON designed to treat P23H adRP by suppressing the formation of the toxic, mutant protein through knockdown of P23H rhodopsin mRNA. This selective inhibition of the mutant protein with dominant negative effect, while retaining the expression of the normal variant, 92 enables the restoration of photoreceptor function (Figure 2(c)). 89
Preclinical proof-of-concept studies of QR-1123 have demonstrated selective reduction of P23H rhodopsin expression and prevention of retinal degeneration in adRP animal and human cell models. 89 The first-in-human phase I/II single-dose, dose-escalation study, Aurora (PQ-1123-001; NCT04123626), is ongoing (Table 4). This study will examine the safety and target engagement of QR-1123 intravitreal injection in adults with adRP due to P23H mutation in RHO.
Discussion
Genetic eye diseases are a leading cause of blindness and moderate-to-severe visual impairment that have, to date, been considered untreatable. However, there has been a surge in research interest in IRDs driven by advanced technologies and precision medicine capabilities, bringing new hope for improved outcomes for individuals living with IRD. This follows the approval of the first interventional therapy for an IRD, and a growing number of innovative, investigational therapies following behind. Among these pipeline products, three AONs targeting specific subtypes of LCA, Usher syndrome, nsRP, and adRP are leading the way.
AONs are well suited for treating the eye, which is a relatively immune-privileged closed compartment and have limited off-target effects. The most common adverse events of sepofarsen are cataracts.57,77–79 Instances were manageable and vision restored to pre-cataract levels after lens replacement surgery. 57 The mechanism behind these cataract events is as yet unknown, but cataracts are reported with intravitreal treatments. 60 They also feature in the natural course of CEP290-associated IRD, occurring spontaneously in 18–63% of cases in natural history studies, and such instances have been managed successfully with lens removal or replacement.65,73,75
The AON platform shares a common technology that encompasses a variety of mechanisms, potentially extending its use across multiple IRDs with different mechanisms (e.g. splice correction, exon skipping, repeat-targeting, exon inclusion, and allele-specific knockdown). These AONs could be useful in both peripheral and central IRDs, and may have the potential to treat a disease at its early stages, which may be particularly beneficial in diseases, such as CEP290-associated IRD. 45 There is also a potential to broaden the application of this RNA platform technology to a range of genetic eye disorders including macular dystrophies (e.g. Stargardt disease) and beyond IRDs (e.g. Fuchs endothelial corneal dystrophy), and possibly other therapeutic areas, in the future.
Generally, AONs are developed to be specific to one mutation in one gene or a defined genetic sequence (such as the exon 13 of the USH2A gene). Therefore, the complex array of genetic mutations within each type and subtype of IRD brings an inherent challenge to the development of RNA-based therapies for genetic eye diseases. 20 There are more than 270 different genes known to cause IRDs, 9 and a large number of mutations may be involved within these genes. 20 On this backdrop of broad genetic heterogeneity, identification and subsequent clinical development of AONs suitable for every individual with an IRD is a time and resource intensive process. The future success of AONs will require more work to understand the presence and significance of retinal-specific splice variants and alternative transcripts for all IRD genes in the humans, which may differ from animal models and non-retinal tissues. Observing clear signs of efficacy in preclinical testing does not always translate to efficacy in human trials, for a variety of reasons. 93 The temporary nature of the therapeutic effect of AONs should also be considered as an important factor for development, potentially bringing an additional therapeutic burden versus a one-administration treatment but also conferring additional flexibility in terms of adjusting the treatment effects. Finally, as a novel therapy, the long-term efficacy and safety of AONs remain to be fully understood, although this will be addressed through the planned clinical research programs for these therapies.
Our understanding of the role of RNA-based therapies in relation to emerging DNA-based therapies will need to be defined. Alongside the pipeline AONs, at least 12 investigational gene augmentation therapies are in development for IRDs and other ophthalmic conditions, which currently include subtypes of LCA, RP, Bietti crystalline dystrophy, and Leber hereditary optic neuropathy. In addition, gene editing therapy is also being evaluated in the IRD space. EDIT-101 (AGN-151587; Editas Medicine) is an in vivo gene editing therapy based on CRISPR. An early-stage trial of this strategy is ongoing with preliminary data from the initial cohorts showing a favorable safety profile, transient EDIT-101 shedding in body fluids with low levels of detection, and signs suggesting biologic activity in some participants.94,95 As our knowledge of DNA- and RNA-based therapy approaches and their side effects grows, we may better understand at which stages of disease each may be applied. We anticipate that the future could bring a multimodal therapeutic strategy to treating certain individuals with IRDs. For instance, definitive DNA-based therapy risk reward may be appropriate for advanced stages of an IRD, whereas RNA-based therapy may offer a better trade-off in early-stage disease due to widespread accessibility to the peripheral retina and lower procedural risks. Therefore, in early disease, as DNA-based therapy would typically not be applicable, there may be a rationale for trialing RNA-based therapy soon after diagnosis. In end-stage disease, combination of DNA-based and RNA-based therapies might be applicable. However, more research is needed to better understand the roles of these targeted therapies across the family of IRDs.
Overall, RNA-based therapies have the potential to become a standard of care for genetic eye conditions. The close structure of oligonucleotides and the several categories of RNA-based therapies targeting different type of mutations could help accelerate the development of new therapies addressing unmet medical needs with urgency. Furthermore, the inclusion of new chemical modifications could further improve stability, half-life, biodisponibility and ultimately the efficacy, safety, and patient comfort.
Of critical importance, to take full advantage of advances in therapy in genetic eye diseases, it is important to improve genetic identification of eligible patients and streamline patient referral pathways to ensure access to treatments or clinical trials, as appropriate. This involves raising awareness of IRDs at every stage of the care pathway with general ophthalmologists, healthcare professionals, genetic counselors, and family practitioners. Improving access to, and use of, genetic testing is fundamental to these objectives as more than one-third of individuals with IRDs currently do not receive these critical investigations. 96
Conclusion
In summary, the treatment paradigm for genetic eye diseases is in the midst of great change, driven by advances in knowledge of the diseases and innovations in therapeutic technologies. RNA-based therapies are an innovative approach within precision medicine that offers several key advantages in the setting of IRDs, and the potential to bring meaningful vision benefit to individuals living with these inherited blinding disorders. Three leading AONs are in clinical trials in specific subtypes of IRDs. Early data from ongoing trials of these therapies are promising and full results are eagerly awaited.

