Abstract
In collaboration with some of the leading headache centres in Germany, Switzerland and Austria, we have established new guidelines for the treatment of migraine attacks and the prevention of migraine. A thorough literature research of the last 10 years has been the basis of the current recommendations. At the beginning, we present therapeutic novelties, followed by a summary of all recommendations. After an introduction, we cover topics like drug therapy and practical experience, non-effective medication, migraine prevention, interventional methods, non-medicational and psychological methods for prevention and therapies without proof of efficacy.
What is new?
- Topiramate and onabotulinumtoxinA are effective in chronic migraine with or without medication overuse. The efficacy of other substances for the prevention of chronic migraine has not been sufficiently demonstrated. - Valproic acid, topiramate and amitriptyline have been tested as migraine prevention in children and adolescents. In light of a very high placebo rate, no therapeutic superiority over placebo could be shown. - Closure of a patent foramen ovale does not lead to freedom from attacks in migraine with aura.
The most important recommendations at a glance
Therapy of migraine attacks
- Analgesics like acetylsalicylic acid and non-steroidal anti-inflammatory drugs (NSAIDs) are effective in the treatment of migraine. Mild and moderate migraine attacks should be treated initially with these substances. They are also effective in some patients with severe migraine attacks. - The serotonin (5-HT)1B/1D-agonists (listed alphabetically) almotriptan, eletriptan, frovatriptan, naratriptan, rizatriptan, sumatriptan and zolmitriptan are the substances with the best efficacy in acute migraine attacks and should be used in migraine attacks which are unresponsive to analgesics or NSAIDs. - Sumatriptan subcutaneous is the most effective therapy of acute migraine attacks. - Eletriptan and rizatriptan are the most effective oral triptans according to results of meta-analyses. - The combination of triptans with naproxen is more effective than the monotherapy. - Ergotamines are effective for migraine attack therapy. However, the efficacy in prospective studies is poorly documented and they have more side effects than triptans and other acute therapeutics. They should therefore no longer be used as the therapy of first choice. - Triptans are superior to ergot alkaloids with respect to efficacy. - The efficacy of medications in therapy of acute migraine attacks is higher if taken early in the attack. - The threshold for the onset of medication-overuse headache according to International classification of headache disorders-3 is ≥10 intake days/month over at least 3 months for triptans, combination drugs, ergots and opioids. - Anti-emetics are effective in the treatment of nausea and vomiting in migraine attacks. - The efficacy of non-medication procedures in the therapy of acute migraine attacks has not been adequately investigated.
Migraine prevention
- In frequent migraine attacks or migraine patients with severe symptoms or persistent aura, migraine prevention should be offered in addition to prevention by education and behavioural therapy. - The choice of a migraine prophylactic drug should be based on the attack frequency (episodic vs. chronic), comorbid diseases and the patient’s individual needs. - The efficacy of the beta blockers metoprolol and propranolol, the calcium antagonist flunarizine, the anticonvulsants topiramate and valproic acid and the antidepressant amitriptyline for migraine prevention has been shown in randomized studies. - Valproic acid should not be used by women of childbearing potential. - Effective, but less well investigated, are bisoprolol, lisinopril and candesartan. - Topiramate and onabotulinumtoxinA are effective in chronic migraine with or without medication overuse. - Drug therapy should be supplemented by non-medication procedures of behaviour therapy (e.g. relaxation procedures). - Regular aerobic endurance sport is recommended. - Procedures of psychological pain therapy (coping with pain, stress management, relaxation procedures) should be used for patients with migraine and reduced quality of life.
Overview and introduction
Introduction
Migraine is a frequent disease with a point prevalence of 20% in women and 8% in men. Therefore, guidelines for the treatment of migraine attacks and the prevention by drug treatment or behavioural therapy have great practical importance.
The purpose of this guideline is to optimize the treatment of acute migraine attacks and the prevention of migraine. The guideline is evidence-based, takes into account the clinical experience of the guideline authors and is a further development of the following guidelines and recommendations.
- Deutsche Gesellschaft für Neurologie (German Society for Neurology; DGN) and Deutsche Migräne- und Kopfschmerzgesellschaft (German Migraine and Headache Society; DMKG) Guideline Therapy of Migraine 2012
1
- DMKG Guideline: Relaxation procedures and behaviour-therapeutic interventions in the treatment of migraine
2
- European Federation of Neurological Societies (EFNS) Guideline 2009
3
- Report of the Quality Standards Subcommittee of the American Academy of Neurology and the American Headache Society 2012
4,5
- Guidelines of the Canadian Headache Society (2012).
6
- Guidelines of the French Headache Society (2014).
7
Definition
In migraine, there are attacks of moderate to severe, frequently one-sided pulsating-throbbing headache which increase in intensity on physical activity. 8 One-third of the patients suffer holocranial headache. The individual attacks are accompanied by lack of appetite (almost always), nausea (80%), vomiting (40–50%), photophobia (60%), sensitivity to noise (50%) and hypersensitivity to certain odours (10%). Signs of activation of the parasympathetic system are observed in up to 82% of the patients, most often mild watering eyes. 9 When the head pains are one-sided, they may change sides during an attack or from one attack to another. The intensity of the attacks may vary markedly from attack to attack. The duration of the attacks, according to the definition of the International Headache Society (IHS), is between 4 and 72 h (https://www.ichd-3.org). In children, the attacks are shorter and may manifest without headache, with only severe nausea, vomiting and dizziness. 10 The localization of the head pain is more often bilateral.
Epidemiology
Migraine is one of the most common forms of headache. The 1-year prevalence of migraine is between 10% and 15%. 11 –15 Prior to puberty, the 1-year prevalence of migraine is 3–7%. 14,16 Boys and girls are about equally often affected. The highest prevalence is observed between the ages of 20 and 50. In this phase of life, women are up to three times more often affected than men. The difference in the prevalence between the sexes is greatest at about age 30. 17
Diagnosis
The diagnosis is based on the prior history and unremarkable neurological examination results (for details, see Guideline ‘Diagnostics and apparative supplementary examinations in headache’). Additional diagnostic procedures, and especially imaging, are necessary in headache with unusual clinical presentation (e.g. to rule out subarachnoid haemorrhage) and for headache with distinctive persistent neurological or psychopathological characteristics.
Drug therapy of acute migraine attacks (Figure 1)
5-HT1B/1D-agonists (triptans)

The serotonin (5-HT)1B/1D-receptor agonists (so-called triptans) almotriptan, eletriptan, frovatriptan, naratriptan, rizatriptan, sumatriptan and zolmitriptan are the therapy of first choice in moderate and severe migraine attacks which are not or only insufficiently responsive to therapy with analgesics or non-steroidal anti-inflammatory drugs (NSAIDs). If headache recurs after initial effectiveness of a triptan, a second dose of the triptan may not be given for at least 2 h.

Acute medication for treatment of migraine attacks. ASA: acetylsalicylic acid; MCP: metoclopramide; NSAID: non-steroidal anti-inflammatory drug.
Triptans are specific migraine medications. However, the response to triptans is not suitable for diagnosing migraine, since triptans may be ineffective in migraine and effective, in secondary headache, for example, subarachnoid hemorrhage. 18
All triptans have proven their effectiveness in large placebo-controlled studies. The data obtained in clinical studies on the efficacy of oral triptans have been summarized in large meta-analyses. The single studies are not referred individually. 19 –24 Cochrane analyses are available for the various non-oral application forms of sumatriptan which also demonstrated efficacy. 25 –28 The efficacy of zolmitriptan as a nasal spray has been shown in placebo-controlled studies 29 –31 ; the efficacy of nasal and oral zolmitriptan was also shown in a Cochrane analysis. 32
In long-lasting migraine attacks, migraine headache may recur after the end of successful pharmacological effect of a migraine medication (‘recurrent headache/headache recurrence’). Recurrent headache is defined as a worsening of headache intensity from no headache or mild headache to moderate or severe headache in a period from 2–24 h after the first effective medication application. 33 This problem is more frequent with triptans than with ergotamine tartrate or acetylsalicylic acid (ASA). Recurrence is experienced in 15–40% of patients after oral doses of triptans, whereby a second administration of the substance is again effective. 34
Triptans with a longer half-life, such as frovatriptan and naratriptan, have a tendency to lower recurrence rates than those with a shorter half-life. 35 However, their initial efficacy is lower. If the first administration of a triptan is ineffective, a second dose is usually also ineffective, unless the first dose was vomited. In these cases, a non-opioid analgesic should be used as a substitute.
Table 1 presents an overview of available triptans.
Therapy of acute migraine attacks with triptans.

OTC: over the counter; TIA: transient ischemic attack; OTD: orally dissolving tablet.
a Available without prescription in Germany (prescription-free, OTC).
b Sumatriptan Supp available in Switzerland.
The triptans in comparison
The shortest time to onset of effect is with the subcutaneous administration of sumatriptan (10 min). 36 Oral sumatriptan, almotriptan and zolmitriptan act after 45–60 min. 21 Rizatriptan and eletriptan oral act the fastest (after 30 min). If the first dose of eletriptan 40 mg is not effective, 2 × 40 mg can also be given (80 mg tablets are available in Switzerland). Naratriptan and frovatriptan require up to 4 h to the onset of effect. 37 Zolmitriptan 5 mg as nasal spray has a more rapid onset of effect than oral zolmitriptan 2.5 mg. 29
The reduction of headache after 2 h, the most important parameter in clinical studies for the efficacy of migraine medications, is greatest following subcutaneous administration of sumatriptan (70–80%). 38 Sumatriptan nasal spray is as effective as sumatriptan tablets. 39,40 Sumatriptan 25 mg oral is less effective than 50 and 100 mg (ca. 50–60%) but also has fewer side effects. Naratriptan and frovatriptan (2.5 mg) are less effective in improving headache after 2 h than sumatriptan, rizatriptan and zolmitriptan 20,41 but also have fewer side effects and a somewhat lower rate of recurrence. The onset of effect of naratriptan and frovatriptan is probably prolonged compared to the other triptans, although no difference could be determined in several studies between frovatriptan and other triptans. 42 After 4 h, the efficacy is comparable to that of sumatriptan. Zolmitriptan 2.5 and 5 mg and almotriptan 12.5 mg are in the middle efficacy range. Rizatriptan 10 mg is somewhat more effective than 100 mg sumatriptan 43 –45 and almotriptan 12.5 mg. 46 Eletriptan in a dose of 80 mg is the most effective oral triptan. 47 In a meta-analysis, eletriptan 40 mg and rizatriptan 10 mg showed the highest rate of freedom from pain after 2 h, eletriptan also showed the highest rate of freedom from pain over 24 h. 19
The frequency of recurrence of the various triptans is between 15% and 40%. In menstrually associated migraine, frovatriptan showed a lower recurrence rate after 2 h than rizatriptan and almotriptan with equal efficacy. 48,49 If a triptan remains ineffective in three consecutively treated attacks, another triptan may still prove effective. 47,50 –52
Comparison of triptans with other medications in the treatment of acute migraine attacks

Comparison studies between triptans and NSAIDs and ASA showed the following results for the primary endpoint: - 50 mg sumatriptan were more effective than 1000 mg ASA, but not more effective than 400 mg ibuprofen.
53
- The combination of ASA, paracetamol and caffeine was more effective than 50 mg sumatriptan.
54
- The efficacy of a combination of 900 mg ASA and metoclopramide was comparable to 100 mg sumatriptan.
55
- The efficacy of a combination of 1000 mg paracetamol and caffeine was comparable to 50 mg sumatriptan.
56
- The efficacy of 100 mg diclofenac was comparable to 100 mg sumatriptan.
57
- Rizatriptan 10 mg was superior to ibuprofen 400 mg.
58
No comparison studies are available for the other triptans. However, triptans were effective in ca. 60% of all non-responders to NSAIDs. 59 Sumatriptan 6 mg subcutaneous (s.c.) was slightly more effective than 1000 mg ASA intravenous (i.v.) but had more side effects. 60
Among the preparations containing ergot alkaloids, ergotamine tartrate was less effective in comparison studies than sumatriptan, 61 rizatriptan, 62 eletriptan 63 and almotriptan. 64
Drug combinations

Combination therapy has been best investigated for the combination of sumatriptan and naproxen, 65 –67 for which efficacy was demonstrated in a Cochrane analysis. 68 Compared to placebo, the numbers needed to treat (NNT) was 4.9, when the initial headache was moderate or severe. As an alternative, the NSAID can also be given with a time delay after the triptan. No placebo-controlled studies are available on this. The combination of naproxen and sumatriptan is also effective in patients with ‘probable’ migraine according to IHS criteria. 69 The combination of rizatriptan and paracetamol, however, was not significantly more effective than rizatriptan alone. 70 Frovatriptan and dexketoprofen in combination are more effective than frovatriptan alone. 71 Administration of metoclopramide not only improves the autonomic secondary symptoms but also leads to better resorption and effect of sumatriptan. 72
Time of administration of the triptans

Triptans may be effective at any time during the attack, which means they must not necessarily be taken immediately after the start of the headache phase. The earlier in the migraine attack the triptans are taken, the better they work. 73 –78 To prevent development of headache due to medication overuse, early administration should only be recommended if attacks are not too frequent (<10 headache days per month) and if patients can clearly identify the headache as a migraine attack.
Side effects and safety of triptans

Life-threatening side effects (myocardial infarction, serious cardiac arrhythmias, stroke) are extremely rare and were observed after administration of sumatriptan in a frequency of 1:1.000.000. 79 Either clear contraindications (such as pre-existing coronary heart disease) were present or the diagnosis of migraine was incorrect in nearly all affected patients. Since the mechanism of action of the various triptans is the same, a similar incidence of life-threatening side effects must be expected. With respect to reported side effects, oral application forms have a lower risk than subcutaneous administration. This is supported by a review article. 80 For safety reasons, patients who suffer migraine with aura should not take a triptan until the aura has abated and the headache started. Moreover, triptans are probably not effective when they are taken during the aura. 81,82 Population-based studies show no elevated risk of vascular events for the use of triptans compared to analgesics. 83,84 This was also found in a retrospective analysis of patients with migraine with brainstem aura and hemiplegic migraine. 85 In Germany, naratriptan and almotriptan over the counter (OTC) are available without prescription. There are only a very few reports of serious adverse events for the two triptans.
Theoretically, all antidepressants that inhibit the reuptake of serotonin could elicit a serotonergic syndrome in combination with a triptan. Rizatriptan and sumatriptan are primarily metabolized via the Monoamine-oxidase (MOA)-A system and in combination with MAO-inhibitors and other serotonergic antidepressants can lead to elevated levels of the active substance and more frequent side effects. Almotriptan and zolmitriptan, in addition to a potent MAO-component, are metabolized via other cytochrome-bound systems. Therefore, fewer adverse events are to be expected if these triptans are combined with serotonin uptake inhibitors. Eletriptan, naratriptan and frovatriptan are not metabolized via the MAO-system. They should be preferred in concurrent serotonergic medication. The choice of an individual triptan should also be based on concurrent medication and to its metabolism. Serotonergic syndromes have, however, only been described in very few cases. 86 –88
Ergot alkaloids

Anti-emetics (Table 2)

Nausea and vomiting are among the characteristic symptoms of migraine. Pharmacokinetic investigations indicate that the absorption of analgesics like paracetamol 90 or ASA 91 may be slowed during migraine attacks. The background is assumed to be disrupted gastric motility during the migraine attack. 92 This is the basis for the combination of analgesics or triptans with prokinetic-effective anti-emetics which is not recommended in generally. Anti-emetics should improve the efficacy of oral analgesics via accelerated and possibly improved absorption. In fact, this hypothesis has only been investigated in few, mostly small studies with conflicting results. In a Cochrane review, a better efficacy in nausea and vomiting could be shown for the combination of ASA and metoclopramide. 93 After i.v. administration, metoclopramide seems to have an analgesic effect of its own in migraine. Domperidone, taken in the prodromal phase of migraine, reduced the onset of a subsequent headache phase of migraine in two studies. 94,95
Anti-emetics in the therapy of acute migraine attacks.
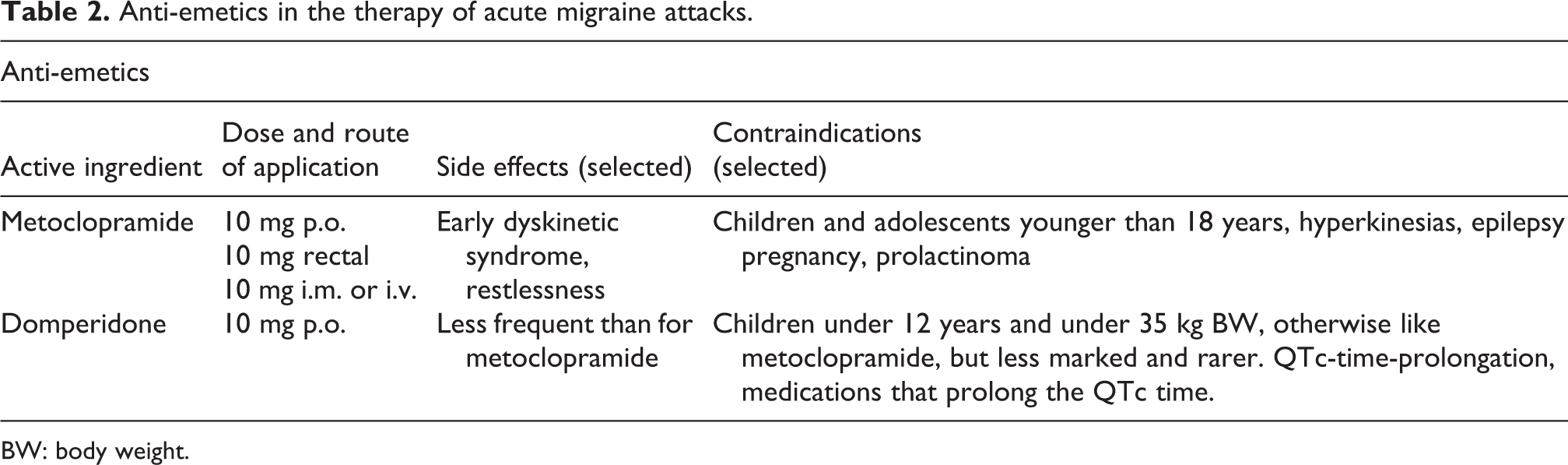
BW: body weight.
In a randomized, open study, a combination of 900 mg ASA in combination with metoclopramide 10 mg oral (n = 7) was more effective than ASA alone (n = 8). 96 In a double-blind crossover study (n = 16), 50 mg sumatriptan plus metoclopramide 10 mg oral were more effective than sumatriptan 50 mg alone. 72 In a larger study (n = 118, crossover design), a soluble fixed combination of 650 mg ASA and metoclopramide 10 mg was superior to placebo but not to ASA as monotherapy with respect to the reduction of headache 97 A similar result was also found for domperidone. In a placebo-controlled study in crossover design (n = 46), the combination of paracetamol with domperidone was not superior to paracetamol as monotherapy with respect to the reduction of headache pain. 98 A Cochrane review published in 2010 concluded that the combination with 10 mg metoclopramide substantially improved the efficacy of ASA on the secondary migraine symptoms nausea and vomiting, but the added administration of metoclopramide has no additional effect on the headache. 99
Numerous case series or comparison studies with other substances without placebo control have been conducted with consistently positive results on the efficacy of metoclopramide 10–20 mg i.v. in the acute therapy of migraine. 100 –104 However, placebo-controlled studies showed conflicting results. 105 In one study (n = 50), metoclopramide 10 mg i.v. was superior to placebo, 106 in another study (n = 40) to both placebo and also ibuprofen 600 mg oral. 107 On the other hand, metoclopramide 10 mg i.v. showed a small superiority in a comparison study (n = 70) versus prochlorperazine and placebo. 108 In another comparison study (n = 113), metoclopramide was superior to magnesium sulphate and placebo. 109 Metoclopramide 10 mg intramuscular (i.m.). in a comparison study versus prochlorperazine and placebo (n = 86) was not more effective than placebo. 110 In a comparison study, metoclopramide up to 4 × 10 mg i.v. was similarly effective in the first 2 h as 6 mg sumatriptan s.c. 101 Nonetheless, a meta-analysis from 2004 concluded that metoclopramide i.v. is a therapeutic option for the treatment of acute migraine attacks in the emergency room. 111 Metoclopramide is approved in Germany for the symptomatic treatment of nausea and vomiting caused by acute migraine. It can be used with oral analgesics to promote absorption in acute migraine attacks.
In a controlled study (n = 330), valproate 1000 mg i.v. versus metoclopramide 10 mg versus ketorolac 30 mg were compared in the treatment of acute migraine attacks in the emergency room. 112 Metoclopramide showed significant superiority over both comparison substances for several endpoints. Valproate was less effective than metoclopramide or ketorolac.
Intravenous rehydration after severe vomiting by administration of fluids is often performed in emergency situations. In a post hoc analysis, the short- (1 h) and long-term effect (24 h) was compared between patients with (n = 112) and without rehydration (n = 458) in administration of metoclopramide. The additional rehydration did not lead to an improvement in headache parameters in patients with acute migraine attacks treated with metoclopramide. 113 Rehydration can, however, be necessary in fluid loss due to repeated vomiting.
Domperidone taken during the prodromal phase of a migraine attack may reduce the onset of headache. 94,95
Small studies are only available for the anti-emetic dimenhydrinate. It is preferred in nausea in connection with dizziness and impaired equilibrium. 114 –118 Dimenhydrinate is a salt of diphenhydramine and 8-chlortheophylline. It was not effective in the treatment of nausea in a controlled study in acute migraine attack. 119
Analgesics (Table 3)

About 80% of all patients treat headache with (mostly prescription-free) analgesics. 120 Table 3 gives an overview of the currently recommended analgesics, NSAIDs and coxibs for the treatment of acute migraine attack.
Analgesics/NSAIDs/COX-2-inhibitors with proven effectiveness in the acute treatment of migraine attacks.a

RCT: Randomized-Controlled Trial; NSAID: non-steroidal anti-inflammatory drug; ASA: acetylsalicylic acid; ICHD: International classification of headache disorders.
a Listed in order of decreasing evidence.
Analgesics are available in various formulations. The resulting pharmacokinetic profiles can influence the therapeutic effectiveness. Effervescent tablets, with active substances already dissolved outside the stomach, lead to more rapid absorption, quicker pain reduction and functionality. Since local high concentrations of the active components of the drug on the gastric mucosa are reduced, the tolerability is also higher. Effervescent formulations should therefore be preferred. 121
A Cochrane review investigated the effectiveness of ASA alone or in combination with an anti-emetic in the treatment of acute migraine attacks. 122 No studies are available for a single dose of 500 mg ASA. In 13 studies (n = 4222), ASA 900 mg or ASA 1000 mg alone or in combination with metoclopramide 10 mg were compared to placebo or active comparator substances, for example, sumatriptan 50 mg or 100 mg. The NNT for 2 h freedom from pain was 6.6 for ASA 1000 mg as monotherapy and 6.2 in combination with metoclopramide. Sumatriptan 50 mg showed no superiority. Sumatriptan 100 mg was significantly superior to the combination of ASA with metoclopramide for 2 h freedom from headache. ASA proved effective in migraine acute therapy, similar to sumatriptan 50 mg or 100 mg. The efficacy of the i.v. formulation of 1000 mg lysin-acetylsalicylate 60 respectively of 900 mg in combination with 10 mg metoclopramide 123 in the treatment of severe migraine attacks was proven in placebo-controlled randomized studies.
Ibuprofen was also evaluated in a Cochrane review with respect to effectiveness in acute migraine attack alone or in combination with anti-emetics. 124 Nine studies (n = 4373 attacks) compared ibuprofen with placebo or other active ingredients. The NNT for 2 h headache improvement for ibuprofen 400 mg versus placebo was 7.2. Effervescent solutions of ibuprofen 400 mg had a higher efficacy than standard tablets for the parameter headache improvement after 1 h. Ibuprofen resulted in headache pain reduction in about half of the patients. Complete freedom from headache and secondary symptoms was only achieved in a minority of patients. In a randomized-controlled trial (RCT), no significant difference could be observed between the dosages 200 mg, 400 mg and 600 mg ibuprofen for the primary endpoint headache reduction 2 h after taking the medication. 125 Older studies are available for the dosages of 800 mg and 1200 mg ibuprofen. These studies do not meet the current requirements of an RCT. 126,127 No headache or migraine studies are available for ibuprofen-lysinate, a substance frequently used in self-medication.
In a systematic Cochrane review, the use of paracetamol and ibuprofen was compared in migraine and tension-type headache. Ibuprofen was consistently superior to paracetamol. Since neither medication is effective for every patient, both are needed. The clinical practice of using paracetamol as the first analgesic is not supported by data. The effectiveness of paracetamol has not been sufficiently documented in migraine. 128 In a Cochrane review, the effectiveness of paracetamol alone or in combination with an anti-emetic in the acute therapy of migraine was analysed. 129 Eleven studies (n = 2942) compared paracetamol 1000 mg alone or in combination with an anti-emetic, with placebo or an active comparator. The NNT for 2 h freedom from headache was 12. The NNT of paracetamol is higher than for other analgesics. It should therefore only be considered in the therapy of migraine attacks in case of contraindications or intolerance of ASA or other NSAIDs. In a smaller RCT, 1000 mg paracetamol i.v. was not superior to placebo treatment. 130
According to a study with 1021 participants, there are three subgroups of patients in self-medication 131 : 48.8% of the patients are relatively young, suffer mostly from migraine and have the lowest frequency of medication-overuse headache; 29.5% comprise older patients, mostly without migraine headache; and 21.7% form a subgroup with high disability, additional pains in several parts of the body and a high prevalence medication-overuse headache of 73%. 131 The data show that results of studies in the framework of self-medication cannot be directly transferred to the specific indication migraine as defined by the IHS classification
The fixed combination of 250 mg ASA, 200 or 250 mg paracetamol and 50 or 65 mg caffeine was examined in various studies. 54,132 –134 A study performed in Germany 132 included only patients who had already used self-medication with analgesics and were satisfied with that. No specific headache diagnosis, such as migraine, was applied as inclusion criterion. Headache diagnosis was provided for the treated headache episodes. Patients were excluded who had treated their headache earlier with prescription medications. Some studies describe an increased risk of medication-overuse headache 135 –144 with the use of combination analgesics.
Combination analgesics with fixed doses are supposed to have better analgesic efficacy than the individual active substances. It is unclear whether oral combinations have only additive or also synergistic effects. Moore et al. 128 analysed the available studies. Additive effects could be demonstrated for sumatriptan plus naproxen in the treatment of acute migraine attacks. There was no evidence of synergistic effects of other combinations.
The efficacy in relief of headache pain and in improvement of secondary symptoms such as phonophobia, photophobia, nausea and vomiting and a greater efficacy compared to 400 mg ibuprofen 133 and compared to 50 mg sumatriptan 54 have been proven for the combination of aspirin, acetaminophen and caffeine. The fixed combination of 1000 mg ASA and 1000 mg paracetamol was found superior to a combination of 500 mg ASA and 400 mg paracetamol and to monotherapy with 100 mg caffeine. 132 Two post hoc analyses report efficacy for the fixed triple combination in patients with severe migraine attacks, 145,146 one also in women with menstrually associated migraine. 147
Data for ketoprofen are limited. No RCT is available for oral formulations of 50 mg, 100 mg and 200 mg. Only one older, very small study without placebo control is available for the i.m. formulation of 100 mg. 148 For 25 mg dexketoprofen per os (p.o.). only one open, uncontrolled study has been performed. 149 A more recent RCT shows that a ‘dual release’ formulation with 75 mg and 150 mg ketoprofen is effective in the acute therapy of migraine. This formulation is not available in German-speaking countries. 150
In a placebo-controlled study, metamizole (novaminsulfon) 1000 mg orally was found to be effective in the treatment of acute migraine attack. 151 A Cochrane review based on few clinical studies rated the i. v. formulation of 1000 mg metamizole as effective in migraine and episodic tension-type headache 152 In a controlled study, 1000 mg phenazon were found to be an effective treatment of acute migraine attacks. 153
A Cochrane review of naproxen in doses of 275 mg, 500 mg or 825 mg alone or in combination with anti-emetic showed a statistical superiority of naproxen over placebo. The high NNT of 11 for freedom from headache after 2 h does not indicate a clinically relevant efficacy. There are no RCTs available on the efficacy of the OTC doses of 200–250 mg naproxen.
A Cochrane review analysed the efficacy of diclofenac with or without anti-emetics in the treatment of migraine attacks. 154 New preparations (potassium salt, water-soluble drops) have become available for accelerated absorption. An NNT of 6.2 for freedom from pain after 2 h was calculated for a single dose of 50 mg diclofenac potassium. Only a minority of patients attain freedom from headache over 24 h with the single dose, so repeated administration of diclofenac potassium might be necessary.
Diclofenac potassium is approved for the treatment of the headache phase of migraine attacks with and without aura. The active ingredient is available as drops, which could promote absorption and tolerability. A positive effect has been demonstrated for the oral application of 50 mg in a controlled study. 155 No RCTs have been performed on diclofenac potassium in the doses 12.5 and 25 mg in the treatment of migraine attacks. Diclofenac potassium doses of 50 and 100 mg were found to be effective in two RCTs.
The results for diclofenac sodium in a dose of 100 mg are contradictory. An older study rated diclofenac sodium in doses of 50 and 100 mg as effective. 156 In a more recent RCT, 100 mg diclofenac sodium was only effective in combination with 100 mg caffeine but not as monotherapy. 157 There is only one open 158 and one blinded but not placebo-controlled study 159 available for 75 mg diclofenac sodium in i.m. formulation.
No RCTs on the acute therapy of migraine are available for the following active ingredients or active combinations: ASA + vitamin C, ASA + caffeine, aceclofenac, acemetacin, etoricoxib, ibuprofen-lysine, indometacin, meloxicam, paracetamol + caffeine, piroxicam, propyphenazone and tiaprofenic acid.
The efficacy of the selective COX-2-inhibitors celecoxib, etoricoxib and parecoxib currently available in the German-speaking region has not been investigated in controlled studies. No RCTs have been performed on the therapy of acute migraine attacks with these coxibs.
Other substances for therapy of migraine attacks
Tramadol in combination with paracetamol 160 was found effective in acute migraine attacks. Nonetheless, opioids and tranquilizers should not be used to treat migraine attacks. 161 Opioids have limited efficacy, often lead to vomiting, central-nervous side effects, have a significant potential for dependency and overuse and lead more quickly to medication-overuse headache.
Special situations in acute therapy
Treatment of migraine attacks in children

No Reye Syndrome has yet been observed in children after treatment of migraine with ASA, but the use of ASA is not recommended before the age of 12. If anti-emetics are necessary, domperidone should be used and not metoclopramide, due to the elevated risk of acute extra-pyramidal dystonia with metoclopramide.
Sumatriptan 10 mg and zolmitriptan 5 mg as nasal spray are approved for the treatment of migraine in adolescents age 12 or older. In triptan studies, the high placebo response and the short duration of attacks were methodical problems in showing efficacy of triptans in children under the age of 12 years. Sufficient data are available to justify the use of triptans (sumatriptan 10–20 mg as nasal spray, zolmitriptan 2.5–5 mg tablets, rizatriptan 5–10 mg tablets and almotriptan 12.5 mg tablets) in adolescents in case of inadequate response to acute therapy with analgesics. 162,163
In Germany, only the use of sumatriptan nasal spray 10 mg is approved for the treatment migraine attacks in adolescents 12 years and older. Ergotamine tartrate and oral triptans are not approved for paediatric use. Ergotamine is approved after the age of 16 years.
Emergency treatment of migraine attacks

The treatment of first choice is the intravenous administration of 1000 mg ASA with or without metoclopramide. 164 In a dose of 10–40 mg, metoclopramide i.v. was found to provide an independent analgesic effect. 101,111 If there are no contraindications, sumatriptan 6 mg can also be given subcutaneously. If the patient has already taken oral triptans for several days before the consultation, no therapeutic effect can be expected from repeated administration of a triptan, including sumatriptan s.c. Triptans act better at the start of an attack than during its course or with repeated administration within an attack. Sumatriptan s.c. is slightly more effective than ASA i.v., but it has significantly more side effects. The two substances do not differ with respect to the occurrence or onset of recurrent headache. 164 The intravenous administration of 1000 mg metamizole is significantly more effective than placebo but can lead to drop in blood pressure and allergic reactions. 165,166
The intravenous administration of 1000 mg paracetamol was not superior to placebo in acute migraine attacks. 130 There is evidence that the intravenous administration of valproic acid in a dose of 300 mg or 800 mg is also effective in the treatment of acute migraine attacks. 167,168 Valproic acid is not approved for the treatment of migraine attacks. Opioids cannot be recommended for the therapy of acute migraine attacks. They are inferior to other acute medications, 169 have a high side effect potential and lead very frequently to recurrence of headache. 102,158,170 –175
Based on expert consensus, therapy of a status migrainosus is recommended with a single administration of 50–100 mg prednisone or 4–8 mg dexamethasone. This is confirmed by a survey of studies on the therapy of migraine attacks with corticosteroids. 176 The data indicate a reduction in headache intensity and a reduction of recurrent headache.
Treatment of migraine attacks during pregnancy
Migraine attacks can be treated between the first and second trimenon of pregnancy with ASA or ibuprofen. These substances should be avoided in the third trimenon. Paracetamol should only be given if there are contraindications for ASA. 177 Triptans are not approved for use in pregnancy. There is no clinical evidence that triptans lead to malformations or other complications in pregnancy. 177,178 A large pregnancy registry for sumatriptan reported no increased rate of complications in the first trimenon. 179,180 Similar results are also found in smaller registries for naratriptan and rizatriptan. 181,182 No unfavourable effects could be observed for the further motor and intellectual development of the children until the age of 3 years. 183 Sumatriptan should only be taken by pregnant women when the expected benefit for the mother outweighs a possible risk for the child. Ergots are contraindicated during pregnancy.
Treatment of migraine attacks in menstrually associated migraine
By definition, menstrually associated migraine is a migraine in which the attacks occur exclusively in the time from 2 days before up to 3 days after the onset of bleeding in at least 2 or 3 cycles. If attacks also occur independent of menstruation, the term is menstrually associated migraine. Menstrually associated attacks are considered particularly severe and long-lasting with poor response to acute therapy and increased occurrence of recurrent headache. Menstrually associated migraine attacks last longer and, after initially successful therapy, tend more frequently to lead to recurrent headache. 184
The acute therapy does not differ from the general therapy of migraine attacks. Superiority over placebo has been shown for all triptans in acute therapy. This applies also for the combination of sumatriptan and naproxen. 185,186 In comparison studies, within the triptan groups, frovatriptan (2.5 mg) had a lower recurrence rate than 10 mg rizatriptan and 12.5 mg almotriptan with equally good effectiveness. 49,187 A further study showed that the combination of 10 mg rizatriptan with 4 mg dexamethasone was more effective but also associated with more side effects than the administration of rizatriptan alone. 188 Dexamethasone alone was inferior to monotherapy with rizatriptan and can therefore not be recommended. If the response of menstrually associated migraine to the usual acute therapy is inadequate, the indication for short-term prevention should be considered (see below).
Non-pharmaceutical procedures for acute therapy of migraine attacks
Acupuncture
There is some evidence that traditional Chinese acupuncture is effective in the treatment of acute migraine attacks. 189 Two randomized studies investigated the effect of acupuncture on the acute headache of a migraine attack. One study in two German centres for Chinese medicine compared the efficacy of acupuncture with sumatriptan (6 mg s.c.) or placebo in the acute attack. Acupuncture and sumatriptan had a similar efficacy in the prevention of development to a severe attack and both were significantly superior to placebo. Sumatriptan was superior in the treatment of a migraine attack with severe headache. 190
Migraine prevention (Figure 2)
Indication for drug treatment for migraine prevention
The indication for drug treatment for the prevention of migraine is based on the frequency of migraine attacks, reduction in quality of life and the risk of medication overuse. Additional criteria (not evidence-based) are: - Three or more migraine attacks per month with negative impact on quality of life; - Migraine attacks which regularly last longer than 72 h; - Attacks which are unresponsive to acute therapy according to the above-mentioned recommendations (including triptans); - Patients who cannot tolerate the side effects of acute therapy; - Increase in attack frequency and intake of analgesics or migraine drugs on ≥10 days per month; - Complicated migraine attacks with debilitating (e.g. hemiplegic) and/or long-lasting auras; and - Following migrainous brain infarction when other causes of stroke can be excluded.

Drug treatment for the prevention of migraine.
The aim of drug treatment for migraine prevention is a reduction of frequency, severity and duration of the migraine attacks and the prevention of medication overuse and medication-overuse headache. Migraine prevention is considered effective when it achieves a reduction of the migraine attack frequency of 50% or more. Patients should keep a headache diary to document the frequency of attacks and success or failure of the medication taken for the treatment of migraine attacks.
Substances for migraine prevention

Drugs with high evidence
Medications for migraine prevention should be given in slowly increasing doses. The effectiveness, defined as a reduction of migraine days by ≥50%, can be evaluated 2 months after reaching the highest tolerated dose. OnabotulinumtoxinA and topiramate are effective in the prevention of chronic migraine. In controlled studies, combination therapy was not superior to monotherapy. A meta-analysis of 121 placebo-controlled studies showed efficacy in at least three studies for amitriptyline, flunarizin, propranolol, topiramate and valproic acid. In at least two studies, three ACE-inhibitors (enalapril, lisinopril, captopril), two angiotensin receptor blockers (candesartan, telmisartan), two anticonvulsives (lamotrigine, levetiracetam) and the beta blockers atenolol, bisoprolol and timolol 191 were effective.
Substances for migraine prevention with high/good scientific evidence.
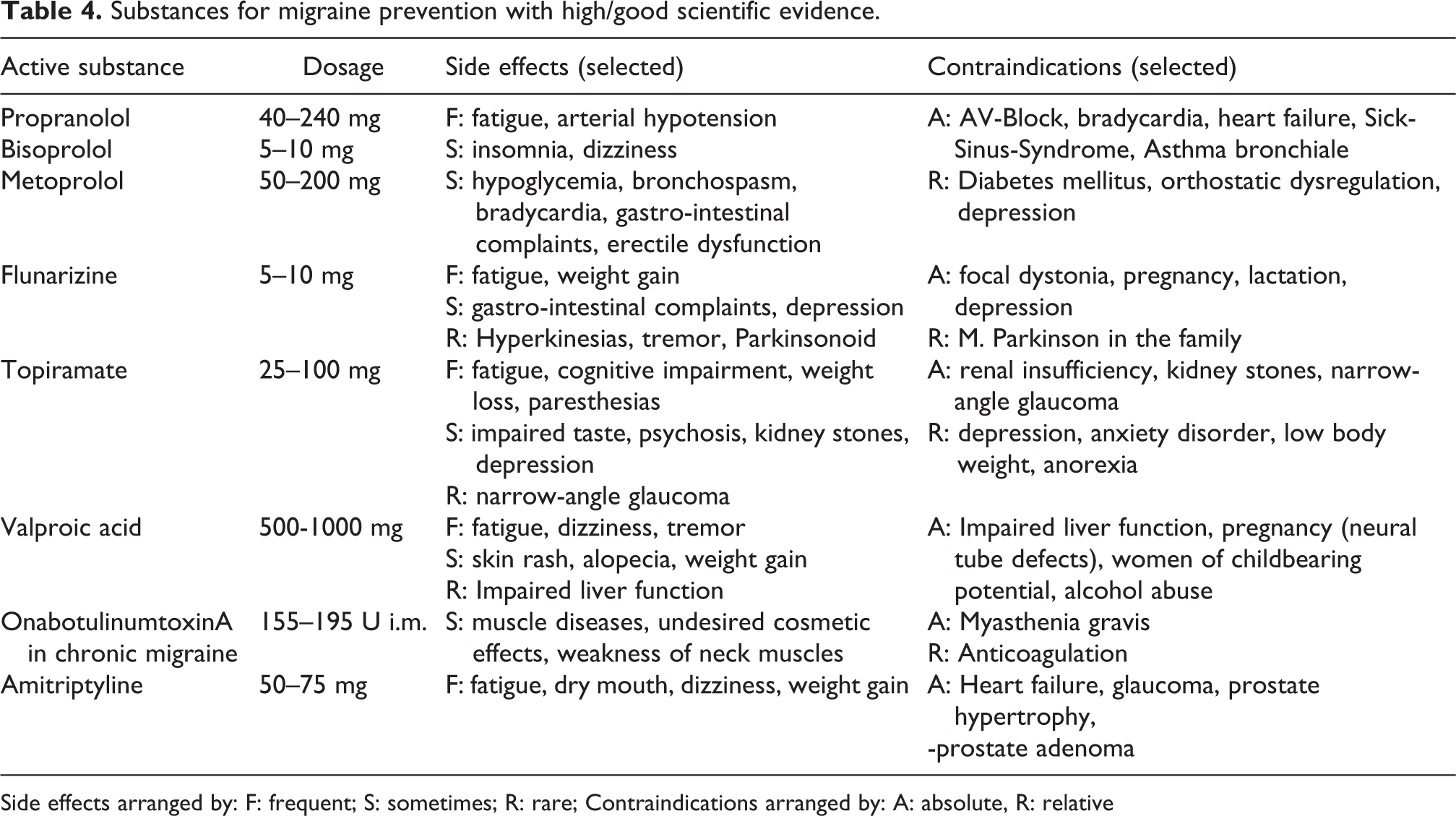
Side effects arranged by: F: frequent; S: sometimes; R: rare; Contraindications arranged by: A: absolute, R: relative
All substances have in common that they are often effective even in low doses in migraine prevention. As far as has yet been investigated, the beta blockers, valproic acid, topiramate and amitriptyline have in common that they reduce with temporal latency the sensibility of cortex cells to generate a ‘cortical spreading depression’ in animal experiments. 192
Beta blockers
Beta blockers are effective substances for prevention of migraine. Most data are available for propranolol and metoprolol with more than 50 studies each. Meta-analyses and reviews also confirm their preventive effect. 193 –195 Holroyd et al. calculated an average 44% reduction of migraine activity for propanolol in a dose of 160 mg. 193 In a Cochrane analysis, the relative risk in the placebo-controlled studies to respond to treatment with propranolol was 1.94 (95% confidence interval 1.61–2.35). 195 Response rates increase dose-dependently, whereby doses between 60 mg and 320 mg/day were investigated. However, the criterion ‘response to treatment’ was not uniformly defined in the studies, which partly explains the heterogeneous results. No significant difference in efficacy was found for propranolol in comparison with other migraine prophylactic substances (other beta blockers, flunarizine). However, this result could also be due to the poor methodology of most trials (small number of cases). The superiority of propranolol over placebo is documented for the 200-mg/day dose in various studies. 196 –198 The effect strength of metoprolol is comparable to that of propranolol. 195
The evidence for the preventive effect of other beta blockers is less-well documented. Bisoprolol was significantly superior to placebo in one study and in a further study just as effective as metoprolol. 199,200 Positive studies are also available for timolol, 201 –203 atenolol 204 –206 and nebivolol. 207 Acebutolol, 208 alprenolol, 209 oxprenolol 210 and pindolol 211 are ineffective in the prevention of migraine.
Flunarizine and calcium channel blockers
Flunarizine is the only calcium channel blocker which showed a significant effect in migraine prevention. 212 –221

The effect strength of flunarizine does not differ from that of metoprolol, but there are more frequently side effects with flunarizine (depression, weight gain). 222 Flunarizine is a calcium antagonist of the ‘calcium overload blocker’ class. 223 Other ‘pure’ calcium channel blockers like nifedipine 224 and nimodipine 225 are ineffective in migraine prevention. Verapamil was only tested in very small studies and is probably also ineffective.
The recommended dose of flunarizine is 10 mg at night. However, 5 mg are equally effective. 220 For this reason, the dose should be reduced to 10 mg every other day to reduce side effects. For patients older than 65, only the 5-mg dose should be used. Flunarizine has also been studied in children. 226 The paediatric dose is 5 mg per day or 5 mg every other day.
Anticonvulsants
The efficacy of topiramate could be documented in numerous randomized studies. 66,227,228 The initial dosage should start slowly with 2 × 12.5 or 2 × 25 mg and a dose of 2 × 50 mg (if necessary up to 2 × 100 mg) per day as final target dose. There is a dose–effect relationship with respect to efficacy and weight loss (191). Limiting factors of topiramate are cognitive side effects, which almost exclusively occur in the titration phase. 229 There is also evidence from smaller studies and subgroup analyses for the efficacy of topiramate in medication-overuse headache and in chronic migraine. 230,231 In combination with nortriptyline, topiramate was effective in patients who did not respond to monotherapy. 232
Valproic acid showed a marked reduction in migraine attack frequency but not intensity, 233,234 Due to its teratogenic properties, valproic acid should not be prescribed for women of childbearing potential or only after instruction concerning reliable contraception. 235 Valproic acid is not effective in migraine prevention in children and adolescents. 236,237 A reduction in the frequency of migraine attacks could be demonstrated for lamotrigine 238 and levetiracetam 239,240 in smaller, not placebo-controlled studies in patients with migraine. Lamotrigine is effective in the reduction of the frequency of migraine attacks in patients with migraine with, but not without aura. 241 Zonisamide showed similar good effectiveness as topiramate in a comparison study. 242
Antidepressives

Amitriptyline is the drug of first choice in the United States, but its efficacy has only been documented in older studies with poor trial design. 243 –248 A meta-analysis, however, confirmed the efficacy of amitriptyline. 191 Amitriptyline has efficacy comparable to that of topiramate. 249 Amitriptyline is also effective in chronic migraine according to the post hoc assessment of an older study. 250 The best effect was achieved after administration for 4 months. Therefore, amitriptyline should be given for a sufficient time period.
Amitriptyline should preferably be used for prevention when a combination with tension-type headache, chronic neuropathic pain or chronic back pain is present or if – as is often the case in chronic pain – there is additional depression.
Opiramole (50–150 mg) proved its efficacy in an older study. 251 Venlafaxine is a serotonin and noradrenalin reuptake inhibitor (SSNRI), for which two smaller controlled positive studies are available. 252,253
Migraine prevention with medications with a lower evidence level
Analgesics and other medications
ASA in a low dose of (Table 5) 100–300 mg/day probably has a moderate migraine-preventive effect. 254,255 Butterbur has been shown to be effective in two placebo-controlled studies. 256,257 In extremely rare cases, serious hepatic function impairment may occur. The substance butterbur extract is no longer available as a medicinal product in Germany and Austria but is available as a nutrient supplement. Feverfew as a CO2 extract was also effective in two studies. 258,259 Feverfew is not sold in Germany in this form. The use of other forms of feverfew has not been investigated and cannot be recommended. Magnesium in a dose of 10 mmol/day was not effective in a study performed in headache centres. 260 A dose of 24 mmol/day magnesium was, however, effective in a population treated in general practices. 261 If magnesium works at all, the reduction in attack frequency is small or the required doses were not attained because of diarrhoea.
Substances for migraine prevention with less scientific evidence.

Side effects are arranged by: F: frequent; S: sometimes; R: rare; Contraindications are arranged by: A: absolute, R: relative; CHD: coronary heart disease; OAD: occlusive arterial diseases; ASA: acetylsalicylic acid; ACE: angiotensin converting enzyme.
a Off-label use.
Other substances
A prophylactic effect of memantine was found in a small placebo-controlled study. 262 The results for gabapentin are inconsistent to contradictory. 263,264 Oxcarbazepine 265 is ineffective. Among the dopamine-agonists, alpha-dihydroergocryptine is possibly effective. 266
Only smaller placebo-controlled studies are available for high-dose vitamin B2 (daily dose 2 × 200 mg). 267,268 An intensive yellow discoloration of the urine is described as a side effect, otherwise there are no serious side effects or contraindications. The efficacy of coenzyme Q10 (daily dose 3 × 100 mg) was shown in a small bicentric placebo-controlled study. 269 On the other hand, no superiority of coenzyme Q10 versus placebo could be demonstrated in a double-blind, placebo-controlled study in children and adolescents. 270 coenzyme Q10 in combination with magnesium and vitamin B2 or combined with omega-3-fatty acids, as well as other berry extracts and vitamins as dietary nutrients is sold in Germany. Compared to placebo, the combination reduces the severity of the migraine attacks, but not the frequency. 271
Botulinumtoxin

Several reviews and two meta-analyses are available on the use of botulinumtoxin in the prevention of episodic migraine. 272,273 Both of the reviews 274,275 on the use of botulinumtoxin summarize three randomized studies. Two small studies with 48 and 30 patients reported efficacy of botulinumtoxinA over placebo. In the study by Silberstein et al., superiority was found for a dose of 25 IE onabotulinumtoxinA, but not for the dose of 75 units. 276 By contrast, there are five randomized studies, some with more than 400 patients, which report no superiority of onabotulinumtoxinA over placebo in episodic migraine. 272,277 In the guidelines of the American Academy of Neurology, 278 two randomized studies were rated as class-I studies and two as class-II studies. The conclusion was that onabotulinumtoxinA is probably not effective in the therapy of episodic migraine. A meta-analysis published in 2009 273 included eight randomized and controlled studies published up to October 2007, with a total of 1601 patients. Considering both the large placebo effect in the studies and the stratification for the various doses of botulinumtoxin, there was no significant effect for the use of botulinumtoxin in the prevention of episodic migraine.
The scientific evidence is better for the use of botulinumtoxin in the prevention of chronic migraine. 279 –284 Two large phase-III studies, PREEMPT 1 and 2, compared botulinumtoxin with placebo. 281,282,285 One study reported the results of a randomized, controlled study in patients with frequent episodic migraine on 12–14 headache days per month, 286 and three studies compared the efficacy of onabotulinumtoxinA compared to an active comparator like valproic acid, 287 topiramate 288 and amitriptyline. 289 In two monocentric studies, a significant reduction of headache days and also the stress caused by headache was found for both onabotulinumtoxinA and for each of the comparator substances (amitriptyline and valproic acid). 287,289 A similar result is also found in comparison of onabotulinumtoxinA with topiramate. 290 None of the comparator substances was superior to onabotulinumtoxinA. The number of enrolled patients (n = 59–72) was small. The pooled analysis of the data from PREEMPT 1 and 2 285 was positive for all endpoints except the intake of medication to treat acute migraine attacks. The majority of the patients in the PREEMPT studies also met the diagnosis criteria of probable headache due to medication overuse. Overall there were more than 1600 patients in these two randomized studies. The results published to date on the use of onabotulinumtoxinA confirm that onabotulinumtoxinA (155–195 units) is effective in the prevention of chronic migraine. This is also confirmed by a pooled analysis with 1115 patients. 291 Adverse events were reported in 62.4% of the verum group and 51.7% of the placebo group. Treatment-related side effects (placebo) were neck pain in 6.7% (2.2%), muscular weakness in 5.5% (0.3%) and ptosis in 3.3% (0.3%). The side effects were mild and transient, and only 3.8% (1.2%) of the patients terminated participation in the study because of these side effects.
OnabotulinumtoxinA must be injected at 3-month intervals in order to achieve a long-lasting and increasing effect. 292 If there is no improvement in chronic migraine after the third cycle, treatment should be discontinued. In about half of the patients, migraine improved to a degree during therapy that no further injection cycles were necessary. 293
ACE-inhibitors and angiotensin-receptor blockers
Lisinopril and telmisartan were investigated in small placebo-controlled studies and showed a significant reduction in attack frequency. 294,295 There are no large dose-finding studies for lisinopril or other ACE-inhibitors or angiotensin-receptor blockers. A small placebo-controlled crossover study investigated candesartan in 60 patients who suffered 2–6 migraine attacks per month. After a 4-week placebo phase, they randomly received either once-daily 16 mg candesartan or placebo for 3 months, thereafter the other corresponding medication. The primary endpoint was the number of headache days. In the 12 weeks of treatment, the patients in the placebo group had headache on 18.5 days, those under verum on 13.6 days. Candesartan was also superior to placebo with respect to duration of migraine and headache, pain intensity and degree of debility. Quality of life could not be favourably influenced. 296
The goal of a second study was comparison of the effectiveness and tolerability of candesartan versus propranolol. The primary endpoint was the number of days with moderate or severe headache which lasted at least 4 h or had to be treated by taking the usual drugs for attack therapy. Secondary study parameters were the number of headache days, duration of headache in hours, the intensity, the dose of analgesics and triptans, the number of workdays lost due to illness and finally the number of responders – defined as patients in whom the number of migraine days was at least reduced by 50% compared to baseline. In the primary endpoint, candesartan and propranolol were almost equally effective and both better than placebo. The baseline value of an average 4.82 migraine days in 4 weeks decreased with candesartan to 2.95 and with propranolol to 2.91 (placebo 3.53). The two medications were also clearly superior to placebo in most of the secondary endpoints, with the exception of the days with headache for propranolol, the number of analgesic doses for candesartan and workdays missed, which neither of the two drugs could significantly reduce. 297
Special situations in migraine prevention
Prevention of migraine and comorbid disorders

Psychiatric comorbidities
Population-based studies showed an association of depression and migraine. The odds ratio for the increased risk is 2.0–5.8, 298 –302 whereby this association was greatest for migraine with aura 299 and for women. 303 Comorbid depression is a risk factor for the chronification of migraine 304 and the development of medication-overuse headache. 305 Patients with migraine and depression may possibly be a subgroup with a different pathophysiology. 306 Migraine patients have a nearly fourfold risk of generalized anxiety disorder 307 and an elevated risk of bipolar disorder. 308 Post-traumatic stress disorders are found in patients with chronic migraine about 5 times more often as in controls but also three times as often as in chronic tension headache 309
Amitriptyline is especially suited for migraine prevention in patients with depression, whereby the dose must be within the antidepressive-effective range (75–150 mg/day). There is a relative contraindication for the use of beta blockers flunarizine and topiramate in the presence of depression, patients with an anxiety disorder may be given SSNRIs. For venlafaxine, there is also evidence of a migraine prophylactic effect. 252,253 Beta blockers may suppress the autonomic secondary symptoms in patients with panic attacks such as tachycardia.
Epilepsy
Migraine is weakly but significantly associated with epilepsy. 310 –313 The prevalence of epilepsy is more than three times higher in children with migraine than in children with tension headache. 314 Children, but also adults, with epilepsy also have a significantly higher risk of migraine. 314,315 Idiopathic occipital epilepsy in children is associated with migraine. The attacks are accompanied by a cortical visual disturbances, which are difficult to differentiate from an aura. Topiramate or valproic acid are recommended as migraine prevention for patients with migraine and epilepsy. Lamotrigine is recommended for patients with isolated auras. Ictal or postictal migraine-like headaches react to migraine-specific medications. 316
Vascular diseases
There is no indication for the administration of ASA in women who suffer from migraine with aura but have not suffered any cerebrovascular or cardiovascular event. Women with frequent migraine attacks with aura and vascular risk factors have a slightly higher absolute risk of ischemic stroke, cerebral bleeding and myocardial infarction. Vascular risk factors, for example, hypertension, smoking, hyperlipidaemia must be treated. A large number of epidemiological and case-control studies showed a relationship between migraine with aura in women and vascular events. 317 –321 Contraceptives containing oestrogen 322 are, however, not contraindicated in principle, as long as the other risk factors are under control. Women, who suffer from migraine with aura and have frequent attacks, should use gestagens for contraception. Closure of an open foramen ovale in migraine does not result in freedom from migraine attacks. Patients with metabolic syndrome and migraine should not be treated with valproic acid or amitriptyline as prevention, since these substances may lead to considerable weight gain. Topiramate is recommended in this case. Beta blockers or angiotensin-receptor blockers are recommended for migraine patients with hypertension. Recommendation for regular aerobic endurance sport is especially meaningful in both groups. The combination of simvastatin and vitamin D may be effective in migraine prevention 323 and should thus be discussed in comorbid hyperlipidaemia.
Prevention of migraine aura
Lamotrigine is not effective in the reduction of migraine attack frequency, 241 but it may reduce the frequency of migraine attacks with aura. 238 Flunarizine can result in a reduction in frequency of both auras and migraine attacks. 324 In individual cases, topiramate is also effective. 325 An effect of acetazolamide or lamotrigine, also in combination with valproic acid, has been described for sporadic or familiar hemiplegic migraine. 326,327
Migraine prevention in children and adolescents
The effectiveness of flunarizine (5 mg/day) in children has been proven. 328,329 Topiramate 15–100 mg/day was effective in two studies and has been approved by the Food and Drug Administration for adolescents with migraine. 330 –332 In a large randomized study in children and adolescents, topiramate and amitriptyline were not more effective than placebo 333 In this study, however, there was an extremely high placebo effect. Therefore, the efficacy of the two substances cannot be definitively evaluated. 334 For propranolol, there is some evidence of effectiveness. 328 Valproic acid is not effective in children and adolescents. 335 Case series indicate that effectiveness can be expected of onabotulinumtoxinA in chronic migraine in adolescents. 336 –338 Biofeedback is also effective in children and adolescents, but there is no additive effect when combined with other behavioural therapies. 339
Migraine prevention in pregnancy
There are no controlled studies on this topic. About 50–80% of the patients report a reduction in migraine attacks during pregnancy. 340 In approximately 8% of patients, headaches increase during pregnancy. If migraine occurs for the first time during pregnancy, migraine with aura is more likely. Nursing is assumed to have no effect on postpartum headaches. 341 Metoprolol, 342 propranolol and amitriptyline are considered as possible drug prevention in pregnancy, 343 whereby no controlled studies are available. Magnesium is not recommended, since it could possibly elicit bone damage in the foetus when applied i.v. 343 In addition, non-pharmaceutical measures such as relaxation therapy, biofeedback and acupuncture should be applied. Small case series and individual cases have reported the successful use of onabotulinumtoxinA in chronic migraine and repeated nerve blocks of the greater occipital nerves with lidocain. 343 –345
Prevention of menstrually associated migraine
When menstruation is normal, options for short-term prevention include the administration of naproxen or a triptan with longer half-life, starting 2 days prior to the expected start of migraine for a total of 6 to 7 days. The following substances and dosages were investigated in placebo-controlled studies: frovatriptan 2.5 mg 1×, 2× or 3× daily, zolmitriptan 2.5 mg 2× or 3× daily, naratriptan 2× daily 1 mg or 2.5 mg and naproxen 2× 550 mg per day. 186,346 –354 Among these options, the best evidence is for frovatriptan 2× daily 2.5 mg. 355 Alternatively, naratriptan 2× 1 mg or naproxen 2× 500 mg can be considered. The risk of developing medication-overuse headache due to the short-term prevention is small, if no or only few acute medications are taken in the remaining time intervals.
The strategy of percutaneous oestrogen administration, propagated formerly, can no longer be recommended. This preventive therapy results in shifting the migraine attacks to the time when oestrogen are withdrawn. 356 On the other hand, continuous administration of a combined oral contraceptive (COC) as a preventive measure can be considered. Therapy should be coordinated with the patient’s gynecologist. Continuous administration of COC is considered safe over a period of up to 2 years. 357,358 The effect on the occurrence of migraine headache and not of menstrually associated migraine attacks has, however, only been investigated in open studies thus far. 359,360 The rationale behind this approach is to reduce the number of cycles and the migraine attacks which they trigger. Since COCs significantly increase the risk of stroke, however, and the migraines, especially those with aura, are themselves a risk factor for stroke, the patient’s individual vascular risk profile must be taken into account. 361 –363 This is especially true for migraine with aura. The continuous use of COCs is encouraged in patients with migraine without aura and without cardiovascular risk factors. In other constellations, the indication must be determined on a single-case basis and after the patient has been appropriately instructed. COCs with low oestrogen content should be preferred. 364,365 A highly-active migraine with aura in a patient with a vascular risk profile is a contraindication to the administration of COCs.
Practical aspects of pharmacological migraine prevention and ineffective medications
Practical aspects of pharmacological migraine prevention
The choice of a pharmacological prevention is based on scientific evidence, taking into account the recommendation strength, the anticipated side effects and comorbidities. Prior to starting, the patient’s expectations for effective prevention must be discussed with the patient (in general, reduction of migraine attack frequency by 50%), and the patient must be thoroughly informed of possible adverse drug effects. Necessary steps in the early recognition of relevant side effects should be discussed (like regular control of liver enzymes under therapy with valproate and topiramate). In women of childbearing potential, the possible teratogenic risks must be pointed out and adequate documentation of contraception kept, especially in therapy with valproate. In light of the high teratogenic risk of valproate, we would recommend that women of childbearing potential without reliable contraception should not use valproate.
Medications for migraine prevention should be titrated slowly and taken in the evening if fatigue occurs as a side effect. This does not apply to flunarizine and angiotensin-receptor blockers. Therapeutic success can best be evaluated with headache diaries based on attack frequency or the number of headache days as established criteria, whereby a reduction in pain intensity, attack duration, headache-related disability or distress and the response to acute therapy should be rated as an expression of effective therapy. If no improvement in migraine frequency is achieved within two months after the targeted or tolerated final dose, a switch should be made to a different substance. If migraine prevention is successful, the necessity for continuation of therapy should be considered after 6–12 months. 231 This is achieved either by slow reduction of the dose or by withdrawal of the medication. If the migraine again becomes worse, further treatment cycles may follow. Shorter treatment times of 3 months are associated with a higher rate of deterioration after reduction or withdrawal, as could be shown for flunarizine 217 and valproate. 366 Whether taking the prophylactic drug for more than 6–12 months has not been sufficiently investigated, but it may be necessary in cases with relevant migraine-related impairments.
Behavioural therapy should be used in addition to a medication based migraine prevention (see below).
If there is no or only inadequate response to a monotherapy, combination therapy may be considered. In combination therapy, the potential of drug interactions and comorbidities must be considered. In smaller studies, combinations of beta blockers, 367,368 or flunarizine 368 with topiramate, as well as valproate and beta blockers 369 were effective. A combination of amitriptyline and topiramate did not result in a reduction of headache frequency and intensity but did lead to greater patient satisfaction. 370 For refractory chronic migraine interventional and neuromodulating procedures are available 371 (see below).
Probably ineffective medications in migraine prevention

A number of other substances have been tested for efficacy in migraine prevention. 372 Often, single substances initially show effectiveness in published case series or open studies which could not be confirmed in subsequent randomized, placebo-controlled studies. In this guideline, we only recommend medications for which effectiveness has been proven in randomized-controlled studies.
Interventional procedures for migraine therapy
The effectiveness of the transection of the corrugator muscle or other pericranial muscles for the prevention of migraine is not scientifically confirmed and should therefore not be used in prevention of migraine. 373
Many retrospective case series and case-control studies showed and association of migraine with aura and patent foramen ovale (PFO). 374 this association was not observed in the general population in two population-based studies. 375,376 The extent, to which a pathophysiological relationship exists between migraine and PFO, or whether this is only an ontogenetic phenomenon, has not been elucidated. Numerous open studies showed therapeutic effects of PFO closure on migraine, although the quality of these studies is usually poor. 374 The prospective randomized MIST study (Migraine Intervention with STARFlex Technology) could not confirm the effectiveness of this procedure for the endpoint freedom from migraine attacks. 377 In the PRIMA-Study, in which the effectiveness of PFO-closure in patients with migraine with aura was investigated, the patients received clopidogrel 75 mg over 3 months and aspirin 100 mg over 6 months. 378 After 12 months, there were no statistically significant changes with respect to the primary endpoint (number of days with migraine with and without aura) and most of the secondary endpoints (number of migraine attacks per month, number of days on which pain relievers were taken, headache-specific disability). Only the rate of patients with at least 50% reduction in migraine days/month was higher in the group with PFO closure. The third randomized-controlled study on PFO closure (PREMIUM-Study) did also not achieve its primary endpoint. 379
The effectiveness of occipital nerve blocks in patients with migraine was investigated in numerous case series and other open studies. 380 Only one randomized-controlled study tested the effectiveness of an injection of 2.5 ml bupivacaine 0.5% (= 12.5 mg) plus 0.5 ml methylprednisolone (= 20 mg) versus placebo in a mixed collective of episodic and chronic migraine according to ICHD-2. In each of the two groups, there was a reduction of the moderate-to-severe headache days by at least 50% in 30% of the patients. In conclusion no relevant effect of occipital nerve block was found. 381
In a small, monocentric randomized study, patients with chronic migraine (according to ICHD3-beta) received 2 ml bupivacaine 0.5% (= 10 mg) or NaCl injected near the major occipital nerve. In the week following the injection, there was a significant reduction in the number of moderate-to-severe headache days, likewise a significant decrease in attack frequency and a significantly raised periorbital pressure pain threshold. 382 In another randomised controlled study, patients with migraine according to ICHD-2 received 1×/week 1.5 ml bupivacaine 0.5% (= 7.5 mg) or NaCl injected near the occipital nerve over 4 weeks. After 4 weeks, the number of headache days decreased significantly in the treatment group from 18.1 ± 5.3 to 8.8 ± 4.8 headache days compared to placebo (16.9 ± 5.7 to 13.2 ± 6.7 headache days), as well as the pain intensity decreased significantly more in the bupivacaine group (visual analogue scale (VAS) score in placeb group: 8.1 ± 0.9 to 6.7 ± 1.6; VAS score in bupivacaine group: 8.4 ± 1.5 to 5.3 ± 2.1). 383
In a small case series (n = 18) in patients with visual and/or sensory auras, sometimes prolonged over 2 h to 1 week, the occipital injection of bupivacaine resulted in a marked improvement within 30 min in 85% of the cases and complete remission in 60% of the cases, with concomitant improvement in headache in 80% of the cases. 384 In summary, the role of occipital nerve blocks in episodic migraine remains unclear; there is evidence of a possible prophylactic efficacy in chronic migraine. There are no controlled studies on the acute effectiveness of occipital nerve blockades in migraine. The variability of study methods with respect to the site of injection and the medication used (local anaesthetics, corticoids or a combination) making the comparability of the studies difficult.
Interventional and neuromodulating procedures in migraine therapy
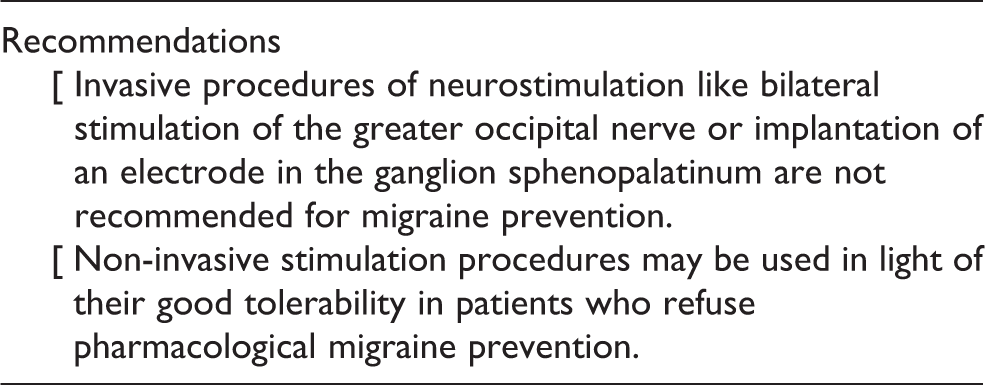
Invasive neurostimulation
Invasive neuromodulating procedure should only be considered in migraine therapy when the criteria of chronic migraine with additional resistance to drug therapy are met. Moreover, these procedures should only be applied within prospective studies by established interdisciplinary and specialized headache centers. The post-operative care and subsequent treatment must be guaranteed. Prior to invasive interventions, a structured catalogue of established diagnostic measures, including psychiatric evaluation, should be used. 385 In case of pathological findings, the indication for the intervention should be reviewed very critically.
Limited effectiveness for chronic stimulation of the major occipitalis nerves (ONS) in chronic migraine with or without additional medication overuse could be demonstrated in two controlled studies 386,387 and further smaller uncontrolled studies and case collections. 388 Due to the only limited study quality and the frequent complications and side effects, 389 ONS can presently not be recommended for therapy of chronic migraine. 390 Initially neurostimulator was authorized for the stimulation of the major occipitalis nerves for the indication ‘chronic migraine’ in 2011 in Germany. The authorization was withdrawn in 2014 due to the unfavourable effect-side effect profile of the procedure. There are currently neither large studies nor long-term experience for other invasive stimulation procedures like cervical spinal cord stimulation, stimulation of the sphenopalatineganglion and combined occipital and frontal (supra- or infraorbital) nerve stimulation. Therefore, the use of these procedures cannot be recommended at this time for the prevention of chronic migraine. 391
Non-invasive neurostimulation
Non-invasive neurostimulations are procedures which can be administered transcutaneously without perforation of the skin, such as transdermal stimulation of the vagus nerve, transdermal stimulation of the supraorbitalis nerves, transcranial direct-current stimulation (tDCS), repetitive transcranial magnetic stimulation (rTMS) and transcutaneous electrical nerve stimulation (TENS). 392
In a double-blind study, a positive effect was demonstrated for the transdermal stimulation of the vagus nerve in cluster-headache. 393 In a pilot study, the method was effective in the treatment of acute migraine attacks. 394 There are no further studies which confirm efficacy and investigate the long-term course. The method is currently being investigated for prevention in migraine patients. A small study investigated the efficacy and tolerabilityof stimulation of the auricular branch of the vagus nerve. Stimulation was applied over 4 h/day. Patients who were stimulated with 1 Hz had a significantly greater reduction in the number of headache days/28 days than patients who were stimulated with 25 Hz (7.0 ± 4.6 vs. −3.3 ± 5.4 days, p = 0.035). 395 The stimulation unit is, however, no longer available in Germany. A single double-blind study indicates the effectiveness of percutaneous mastoid stimulation in migraine, 396 however, the numbers are low and further studies are needed.
Bilateral transcutaneous stimulation of the supraorbitalis nerveshad a good safety and side effects profile but limited nerves had efficacy. 397 –400 Sixty-seven patients were enrolled in a sham-controlled study. 399 After 3 months, the number of migraine attacks was significantly reduced under verum stimulation (6.94 vs. 4.88; p = 0.023), compared to sham-stimulation (6.54 vs. 6.22; p = 0.608). The 50% responder rate of 38.1% was higher than in the group with sham stimulation (12.1%). In an open study on patients with chronic migraine, 50% of the patients attained a significant reduction of days on which acute medication was taken. 401
By means of TMS, influencing the cortical excitability and thus the aura is expected to prevent the subsequent onset of headache. Two studies could demonstrate good efficacy of single-pulse TMS in the acute therapy of migraine with aura. 402,403 However, methodical problems of these studies, in particular with sham control, do not allow a final conclusion on the efficacy of TMS in the acute therapy of migraine with aura. Moreover, the single-pulse TMS has thus far only been shown in migraine patients with aura and thus applies only to a minority (about 10–30%) of all migraine patients. Whether the TMS is also effective in migraine attacks with out aura is unclear, since the theoretically possible ‘silent CSD’ without aura phenomena is controversial. Treatment of acute migraine attacks with single-pulse TMS is currently only of scientific interest. TMS at present is not approved and available in Germany. Studies on the preventive application of repetitive TMS offer only weak evidence at present for a lasting effect of this method. 404 –406 Application can thus not be recommended at the present time.
Small controlled studies are available on tDCS or on TENS which confirm a certain efficacy in migraine. Their use in migraine therapy must presently be viewed critically. 407
Non-pharmaceutical procedures for prevention and psychological procedures
Non-pharmaceutical procedures in migraine prevention

Acupuncture
Acupuncture according to the principles of traditional Chinese medicine is effective in the prevention of migraine. In a current Cochrane analysis, 408 an effect compared to sham-acupuncture was demonstrated in patients with episodic migraine; but the effect was small.
This article included 22 randomized-controlled studies (total 4985 patients) with a minimum observation period of 8 weeks. In five studies, acupuncture treatment (following the principles of traditional Chinese medicine) was compared to no acupuncture (only acute treatment/not regulated routine treatment), in 15 other studies with sham acupuncture and in five studies with an established pharmaceutical prevention. The authors of the Cochrane analysis reach the following conclusion:
There is minor evidence that acupuncture provides additional benefit in the prevention of episodic migraine. In addition, there is evidence that classical acupuncture is marginally superior to sham acupuncture. This could not be confirmed in the original Cochrane analysis. 409 Acupuncture can be considered as at least as effective as pharmaceutical prevention.
No studies are available on the use of acupuncture in patients with chronic migraine with one exception. 410 Compared to topiramate (mean maintenance dose 84 mg/day), a significantly higher mean reduction in the monthly days with moderate to severe headache (10.4 vs. 7.8) with fewer side effects (6% vs. 66%) could be demonstrated. Otherwise only studies with the inclusion criterion chronic daily headache have been published. These, however, investigated chronic tension-type headache and probably also headache in medication overuse in addition to chronic migraine, so that no clear statement can be made on chronic migraine alone. 411,412
In an overview article on the effect of sham acupuncture (acupuncture at non-classical acupuncture points or only surface needle placement without additional stimulation), the authors concluded that the pronounced unspecific effect which can be observed in sham-acupuncture studies, makes it difficult to recognize a relatively small specific additional effect in classical acupuncture. 413
Piercing
Nowadays there are numerous links in the Internet (for example in Facebook) in which so-called Daith Piercings are recommended for the therapy of migraine. Piercing is set in the auricular cartilage, which is comparable to an acupuncture point used in migraine treatment. The procedure not based on pathophysiological concepts and no randomized-controlled studies are currently available. Due to possible risks to health, the application of ear piercings in the treatment of migraine is discouraged.

Homoeopathy
In randomized placebo-controlled studies, there were even some negative results for homoeopathy over placebo. 414 –417

Endurance sports
Regular endurance sport is frequently recommended in the prevention of migraine and is part of most multimodal therapy programs for headache patients. It is unclear whether endurance sports likely produces unspecific effects as ‘an alternative relaxation procedure’, or whether the effects are really specific, achieved by improvement of the physical performance capacity. Other effects could be produced by the weight loss associated with sport, since obesity is associated with increased headache frequency. 418 These questions are of importance in enabling statements on the recommended training frequency, training duration and training intensity for migraine prevention. A survey of the studies published up to 2008 concluded that there are several studies which indicate a possible effectiveness of sports in migraine prevention, but none of the studies is sufficiently powered to allow statistical confirmation of effectiveness. 419 A more recent review article reaches similar results: the results are promising, but the individual specific contribution has not yet been investigated. 420 A pilot study showed positive effects of endurance sport on migraine frequency. 421 In a pre-post–study on 33 patients, Overath et al. 422 could show that aerobic endurance training over a period of 10 weeks improved or normalized both the clinical symptoms (number of migraine days per month) and the area of executive functions as well as amplitudes and habituation of the contingent negative variation (CNV). Regular endurance sport was compared in a three-armed study on the effect of topiramate up to the individually highest tolerated dose and relaxation training. No significant difference was observed between the therapy arms, but the number of headache attacks in all 3 arms was reduced by less than one attack per month. Side effects were only reported in the treatment arm with topiramate. 423

Psychological therapy of migraine

Migraine is no longer considered a psychosomatic illness, and the model of a migraine personality could not be demonstrated in carefully designed studies. 424 Today’s valid multidimensional etiopathogenesis model is based on the assumption that there are genetic, psychosocial, physiological and biochemical predispositions which develop in connection with a dysfunctional habitual way of dealing with stress in migraine and can influence its course. 425 In particular, the single migraine attack appears to be elicited by a rapid and intensive shift of excitation states in the affected person (e.g. sleep, meals, tension, too-rapid relaxation) and a ‘balanced lifestyle’ to have a positive effect on attack frequency. 2,426 According to this model, the migraine can be influenced by psychological strategies for lifestyle modification.
Among the psychotherapeutic procedures, behavioural therapy (BT) is best-suited to fulfil the task and to be combined with medical measures (so-called multimodal/multidisciplinary approach.
2,427
Psychodynamic and other schools have not yet brought proof of procedure-specific efficacy in the prevention of migraine. BT interventions emphasize strategies for the prevention of migraine in terms of reduction of attack frequency and headache-related affective and behavioural impairments. BT-interventions teach the patient the ability and skills to influence the course of migraine via modification of personal environmental factors. The most important BT interventions
2,428
can be divided into four categories: - Relaxation training; - Biofeedback therapy; - Cognitive-behavioural therapy more specifically or stress management; and - Combination of medical and CBT strategies.
The indication for psychological treatment is similar to the indication for pharmacological prevention. 429 Patients with frequent migraine (ca. 3–4% of the German population) are candidates for psychological treatment.
Formally, psychological procedures can be divided into simple (biofeedback, relaxation) or combined (cognitive-behavioural-therapeutic) procedures. Cognitive-behavioural therapeutic procedures (CBT) are particularly indicated for patients with chronic headache, since these usually suffer from relevant comorbidities. The following arguments support the application of non-drug procedures (e.g. Andrasik
430
): - Non-pharmacological treatment is preferred; - Pharmacological treatment is poorly tolerated; - Medical contraindications for pharmacological treatment; - Inadequate or no response to pharmacological treatment; - Pregnancy or lactation; and - High-frequency use of analgesics or migraine drugs. - Considerable exposure to stress and inability to cope with stress.
CBT-procedures are available for migraine patients in well-designed standardized programs and can be performed both time- and cost-economically. They can be performed in groups or individually with equal efficacy.
2,431
They usually also contain a module with a relaxation technique (biofeedback is usually not offered in combination). The most common CBT treatment formats are: - In-patient multimodal pain therapy according to the criteria and structure terms of the OPS-Code 8-918 (interdisciplinary diagnostics and therapy psychological procedures are obligatory). - In-patient treatment in special hospitals (usually 6–12 weekly sessions; 60–120 min).
432
- Minimal contact (usually 4–6 weekly sessions; 60–120 min; life-style-modification).
433
- Day-clinic treatment (like ‘minimal contact’, only compact usually in one week; see also migraine treatment in integrated care).
434
–436
- Individual treatment at home (usually lasts ca. 8 weeks; regular supervision by telephone; audio- and other work materials or computer-supported self-treatment).
437,438
- Internet-based treatment (usually ca. 6 weeks relaxation and problem-solving; email supported).
2,439
–441
Behavioural-therapeutic procedures (relaxation, biofeedback, cognitive behavioural therapy) hardly differ from one another in effectiveness. 442,443 More recent reviews indicate a broad heterogeneity of the studies and small effect strength and cite methodical limitations (e.g. small groups, lack of randomization). 444
Biofeedback
Biofeedback is a therapeutic psychological intervention for the conditioning of physiological, particularly autonomic functions. The control of physiological functions (specific) and the conviction of symptom control (unspecific) are mechanisms of biofeedback action. About 100 clinical studies were included in a meta-analysis. The weighted mean effect sizes in the prevention of migraine attack is between 0.4 and 0.6 (for the application of EEG-biofeedback, skin temperature biofeedback, electromyography (EMG)-biofeedback or a combination of temperature and EMG-biofeedback) and in the acute treatment via blood-volume pulse biofeedback (‘vasoconstriction training’) at 0.7. 445,446 Meta-analyses conclude that both relaxation procedures (usually progressive muscle relaxation by the Jacobson method) and also various biofeedback procedures achieve on average a reduction of migraine frequency of 35–45%. 442,445,447 The effect strength of these procedures is in the range reported for propranolol. 2, 193

Relaxation therapy

Relaxation procedures are intended to reduce the general activation level. The assumption is that, in addition to a general relaxing effect, a central suppression of information processing is achieved. 448 Relaxation not only leads to a reduction of hypervigilance and attention, however. Anxiety states are also reduced by relaxation, which in turn increases pain tolerance and reduces at least the subjective pain report. A preventive function in preventing pain is often attributed to relaxation procedures; however, patients also report on abortive properties of relaxation in acute pain states. The procedure of progressive muscle relaxation (PMR) consists of an incremental tensing and relaxing of various muscle groups. Care must be taken that the exercises are performed regularly and not only contingent on pain and that a transfer to everyday living is made. Hypnosis appears to be comparable in its effect to other relaxation procedures. 449
Among the relaxation procedures, PMR is superior to autogenic training for inexperienced people, since success is more rapid and motivation thus remains high. There are as yet only few studies in which the use of PMR in migraine was explicitly investigated. Trautmann and Kröner-Herwig used PMR for the treatment of headache in children. 441 They found significant effects, which increased still further in the follow-up period. However, no differentiation was made between various types of headache, which limits the results. Similar to biofeedback (see above), relaxation procedures (usually PMR) achieve on average a reduction of migraine frequency by 35–45% 450,451 and thus fall in that range cited for propranolol. The therapeutic procedures are applied in the treatment of migraine both pain-specific (e.g. in PMR) and also pain-unspecific. In addition to the clinical efficacy, a shift in the cortical attention support can be proven in the measurement of the contingent negative variation (CNV). The previously elevated CNV returns to normal in regular application of PMR in migraine patients. 452
Cognitive behavioural therapy

Cognitive behavioural therapy (CBT) comprises cognitive-behavioural treatment strategies intended essentially to improve the patient’s self-reliance and control conviction. 453 Behavioural-therapeutic strategies provide the patient with techniques for the analysis and improvement of his own dealing with stress events and can alter expectation patterns. 454 CBT procedures are available for migraine patients in well-designed standardized programs and can be economically performed both as individual and as group therapy with equal effectiveness. 431,436 The CBT comprises essentially the following building blocks: psychoeducation, improvement of self-perception, modification of pain-related cognitions, modification of social impairments, modification of migraine-specific dysfunctional lifestyles (detailed description of the treatment modules in Fritsche et al. 455 ). Improvements are maintained for up to 5 years. Information on the differential effectiveness of individual behavioural-therapeutic procedures – especially CBT – is given in Table 6.
PMR: progressive muscle relaxation; tBFB: thermal finger biofeedback; EMG: electromyography; CBT: cognitive behavioural therapy.
The effectiveness of psychological therapy in migraine has been confirmed in several overview articles. 448 Studies after 2000 are mostly observational studies on psychological treatment of headache in overuse of migraine drugs in migraine, 457 examination of additive effects in the combination of behavioural therapy and pharmacotherapy, 458 treatment of comorbidities, 459 search for success predictorsm, 460 examination of cost-effective applications using new media, 461 self-help for migraine patients, 462 behavioural therapy in children with migraine 463 and especially on multidisciplinary treatment. 434
Combined pharmacological and psychological therapy

Grazzi et al. combined behavioural-therapeutic strategies in eight sessions (of which four sessions were PMR by the Jacobson method, after the 5th session with additional EMG-biofeedback) with pharmacological prevention in patients with transformed migraine of medication overuse during in-patient medication pause. 464 The most recent and only placebo-controlled combination study on migraine prevention compared the effect of the beta blocker propranolol with a behavioural-therapeutic program (PMR, trigger identification and management, stress management, sometimes also temperature feedback) and with a combination of the two therapies in a total of 232 migraine patients with at least three migraine days per month. 458 At the same time, pharmacological acute therapy was optimized in all participating patients. Only the combination therapy led to improvement compared to optimization of the acute therapy alone.

Internet-based offers and smartphone applications
Internet-based methods, email supported treatment, telemedicine and smartphone applications are interesting and promising therapy offers, some have in part already found a niche in psychotherapy (see above 2,437 –441 ). A range of various headache-relevant offers is currently available (e.g. headache diaries, relaxation-apps). In many applications, a lack of quality assurance is deplored (missing standards and regulation) and a lack of headache experts and patients involved in the development. There are several research projects which are currently working on qualitatively improved therapeutic offers, so that conclusive evaluation studies will probably be available in the near future. We refer the interested reader to current overview articles on the topic. 465 –471
Procedures without evidence of effectiveness (thus far)
Numerous procedures are offered and advertised also and especially for non-pharmaceutical preventive migraine therapy, for which no controlled studies have been performed. More than 80% of all migraine patients have experience with complementary or alternative therapy procedures. Mainly, the patients are motivated to use such procedures by the desire to leave nothing untried and to take action themselves against their disease, and the desire for therapy with few or no side effects. 472 No statement on effectiveness can be made for many of the procedures, since there are no studies which enable such an evaluation. Other procedures are ineffective according to currently-available data. There are open studies on some methods, but proof of effectiveness in controlled studies is (as yet) missing. One article examined the influence of dietary measures on migraine in a crossover study after first determining individual food allergies and could find no significant effects of an elimination diet. 473 Scientific study approaches deal increasingly with physiotherapy. The current data do not, however, confirm the effectiveness of manual therapeutic procedures in migraine therapy. 474 The relationship between myoarthropathy of masticatory muscles (synonym: craniomandibular dysfunction) and migraine or headache frequency in migraine patients has been demonstrated several times. Proof that treatment with a biteplate in the therapy of migraine is in fact still missing. 475 We also advise against corrugator surgery.
Procedures with currently lacking proof of effectiveness (incomplete list): - Corrugator surgery - Colon hydrotherapy - Removal of amalgam fillings - Fresh cell therapy - Reflexological massage - Dentition correction - Hyperbar oxygen therapy - Hysterectomy - Magnetic field treatment - Neural therapy - Ozone therapy - Piercings - Psychoanalysis - Psychophony - Sanitation of a presumed mycotic intestinal infection - Tonsillectomy
Methods applied
The German Society of Neurology and the German Migraine and Headache Societies nominated authors for the guideline. Each author team consisting of a neurologist and a psychologist formatted the first draft of a designated section of the guideline. Authors were selected in way to avoid possible conflicts of interest. The authors performed a systematic literature search from the last 10 years.
The draft guideline was modified in four rounds of a Delphi procedure. The final version was approved at a final meeting of authors in November 2017 in Berlin.
An independent committee evaluated possible conflicts of interest. In conclusion >50% of authors had no conflict of interest and the remaining authors had only minor conflicts of interest.
Footnotes
Authors’ note
Hans-Christoph Diener, Charly Gaul, Peter Kropp are the lead authors; Hans-Christoph Diener, Steffen Nägel, and Charly Gaul are the coordinating authors; Andreas Straube, Katharina Kamm, Stephanie Förderreuther, Andreas Gantenbein, Jens Petersen, and Peter Sandor contributed for data collection in Swizterland; Christian Lampl contributed for data collection in Austria. This article is translated from ‘Diener H.-C. et al. S1-Leitlinie Therapie der Migräneattacke und Prophylaxe der Migräne. 2018. In: Deutsche Gesellschaft für Neurologie, Hrsg. Leitlinien für Diagnostik und Therapie in der Neurologie. Online: ![]() ’. This guideline is approved and endorsed by the German Society of Neurology and the German Migraine and Headache Society. Guideline Development Level: S1.
’. This guideline is approved and endorsed by the German Society of Neurology and the German Migraine and Headache Society. Guideline Development Level: S1.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.

