Abstract
Fournier’s gangrene (FG) is a surgical emergency. The main treatment plan for this disease includes several aggressive debridements, which lead to the development of massive soft-tissue defects in the affected area. Current literature describes various possible reconstructive options for the closure of those defects, yet, there is no evidence on which is the most efficient. Here we describe an unusual case of an otherwise healthy male presenting with a scrotal Fournier’s gangrene. In our case, the reconstruction was performed via anterolateral thigh flap. Due to a postoperative complication the flap was partly lost, however, consequences were managed successfully and a satisfactory result was achieved.
Introduction
Fournier’s gangrene (FG) is a surgical urological emergency. It is a rapidly progressing, potentially fatal, necrotizing fasciitis that affects the external genitalia, perineal or perianal regions. 1 This condition was named after Jean-Alfred Fournier, a venerologist, who described several idiopathic cases in 1883. 2 Eventually, it was observed that distinct causes of FG are associated with immunodeficiency disorders. It is also known that FG occurs predominantly in males rather than females, with a ratio of 10:1. FG develops due to the invasion and infiltration of synergistic polymicrobial agents originating from the colorectal, genitourinary, or dermal infection sites. 3 Frequently, the disease manifests with symptoms of perineal discomfort, fever, local edema, skin necrosis, and erythema with induration. 4 An urgent determination and aggressive surgical debridement of devitalized tissues and broad-spectrum antibiotics are essential to reduce morbidity and mortality associated with FG. 5 After the infection is managed successfully, further guidance requires the coverage of remaining tissue defects. Achieving a proper functional and cosmetic appearance is a substantial reconstructive challenge.
We present a rare case of an otherwise healthy male without any confirmed comorbidities or health predispositions related to FG. Multiple surgical techniques were used in order to reach the most acceptable functional and aesthetic results.
Case Report
A 48-year-old male patient was referred from a regional hospital to our center’s emergency department due to worsening symptoms. He had a high-grade fever of 39°C for a week. However, when the painful swelling of the scrotum occurred, he decided to call emergency services. The patient denied having any concomitant diseases (such as diabetes or HIV), recent traumas, or sexually transmitted infections. The patient also denied being a smoker, any chronic alcohol consumption, and drug abuse.
The patient was brought intubated under anesthesia with a septic shock and unstable vital signs: pulse rate of 130 bpm, respiratory rate of 26 breaths per minute, blood pressure 135/65 mm/Hg, and a temperature of 40°C.
Local examination revealed scrotal and penile edema and areas with skin discoloration (Figure 1). After examination, the patient was clinically diagnosed with FG. There were no other foci of infection detected.
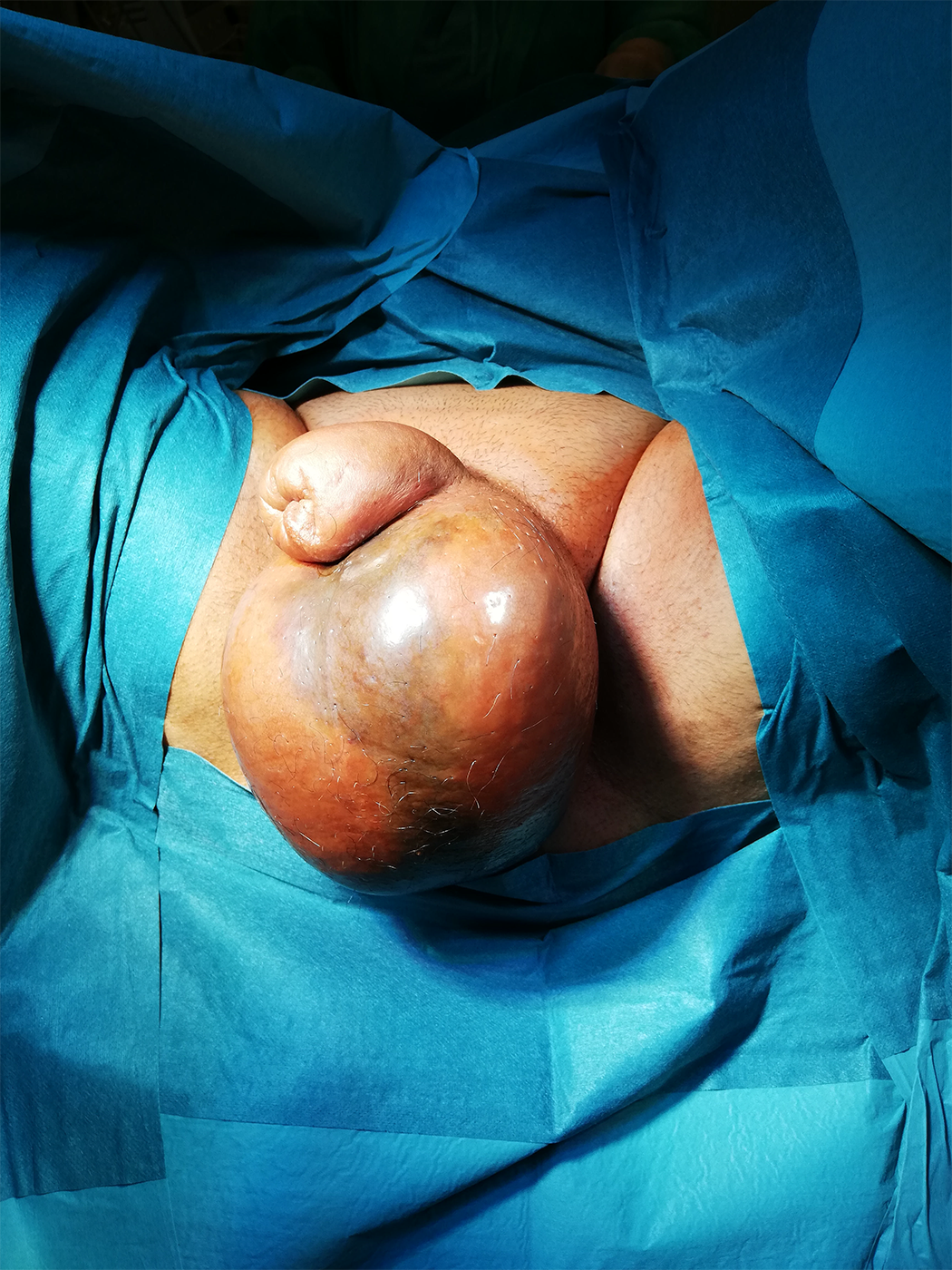
Fournier’s gangrene of scrotucm with edema.
Laboratory indicator analysis showed 25 000 WBC/mm3, CRP of 338 mg/l, Blood Urea Nitrogen 13,4 mmol/l, and Creatinine 120 umol/l.
Immediately after admission, the patient was administered intravenous (IV) antibiotics and fluid resuscitation. An urgent surgery of necrotic tissue debridement was performed under general anesthesia. Devitalized tissues were excised up to the bleeding edges, bilateral incisions in the inguinal area were made, and setons were placed. Discharged purulent material was collected and sent for a bacterial culture test and pathological examination. Due to penile edema, dorsumcision was performed in order to gain access for a 16 Fr Foley catheter insertion (Figure 2).
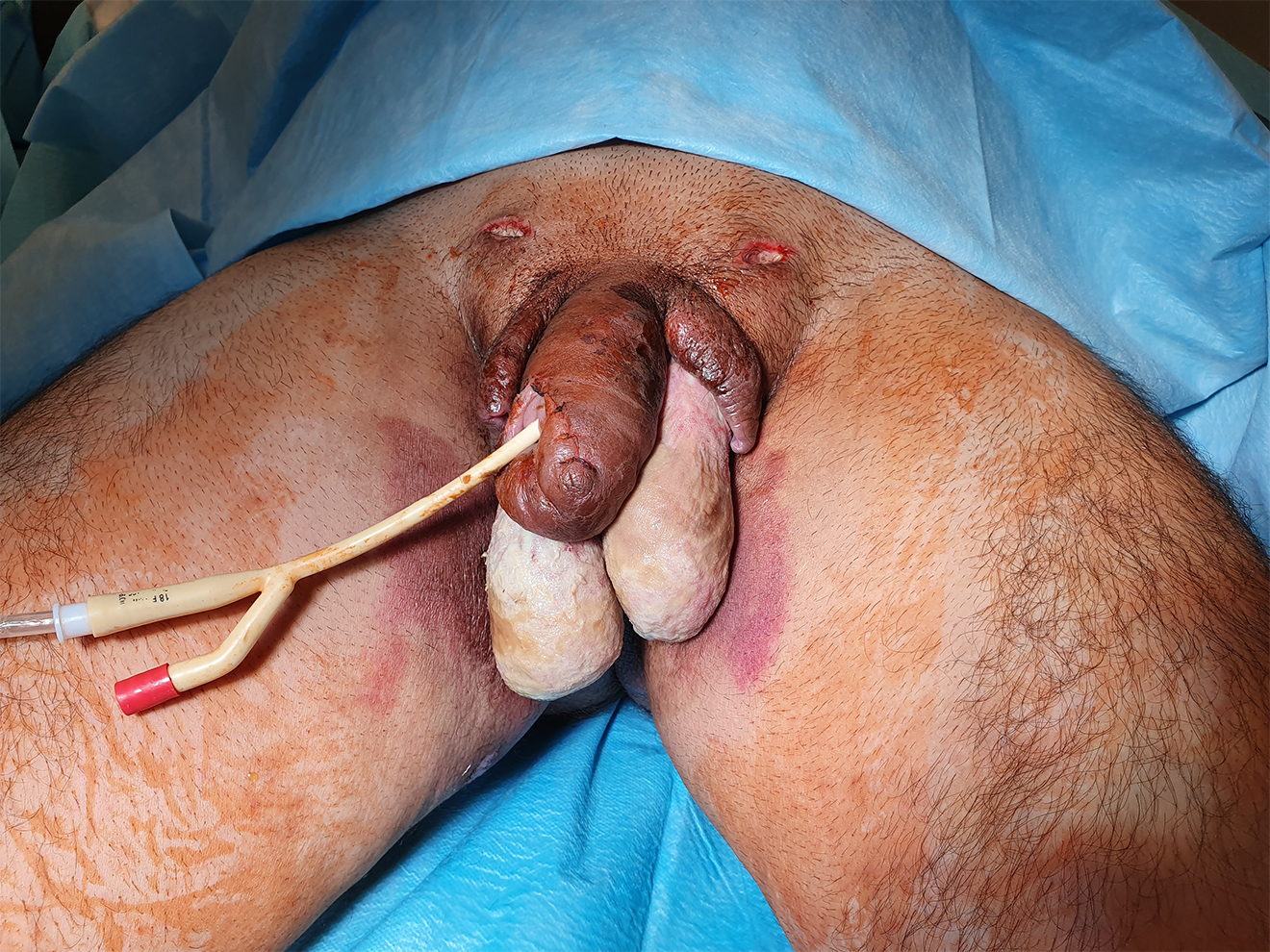
Dorsumcision made to insert a catheter.
The results of the bacterial culture test revealed an anaerobic infection consisting of - Pseudomona aeruginosa, Enterobacter cloacae, Bacteroides fragilis. Pathology reports of removed tissues showed epidermal and subcutaneous necrosis, acute inflammation with neutrophilic infiltrates, microorganisms and edema.
Due to the patient’s penicillin allergy, Sol. Tazocini was chosen for an antimicrobial treatment. After a week in ICU, the patient was transferred to the urological department. During the ensuing three weeks, multiple debridement surgeries were made in conjunction with intravenous a/b therapy until the active infection was under control (Figure 3, 4). When the wound was covered by healthy granulation tissue and secondary healing of the edges was observed, further reconstructive options were discussed. The patient was mostly concerned about the functional and aesthetic outcome of the surgery. Therefore, considering the massive scale of the defect, the surgical team decided to perform a reconstruction surgery using a pedicled flap.
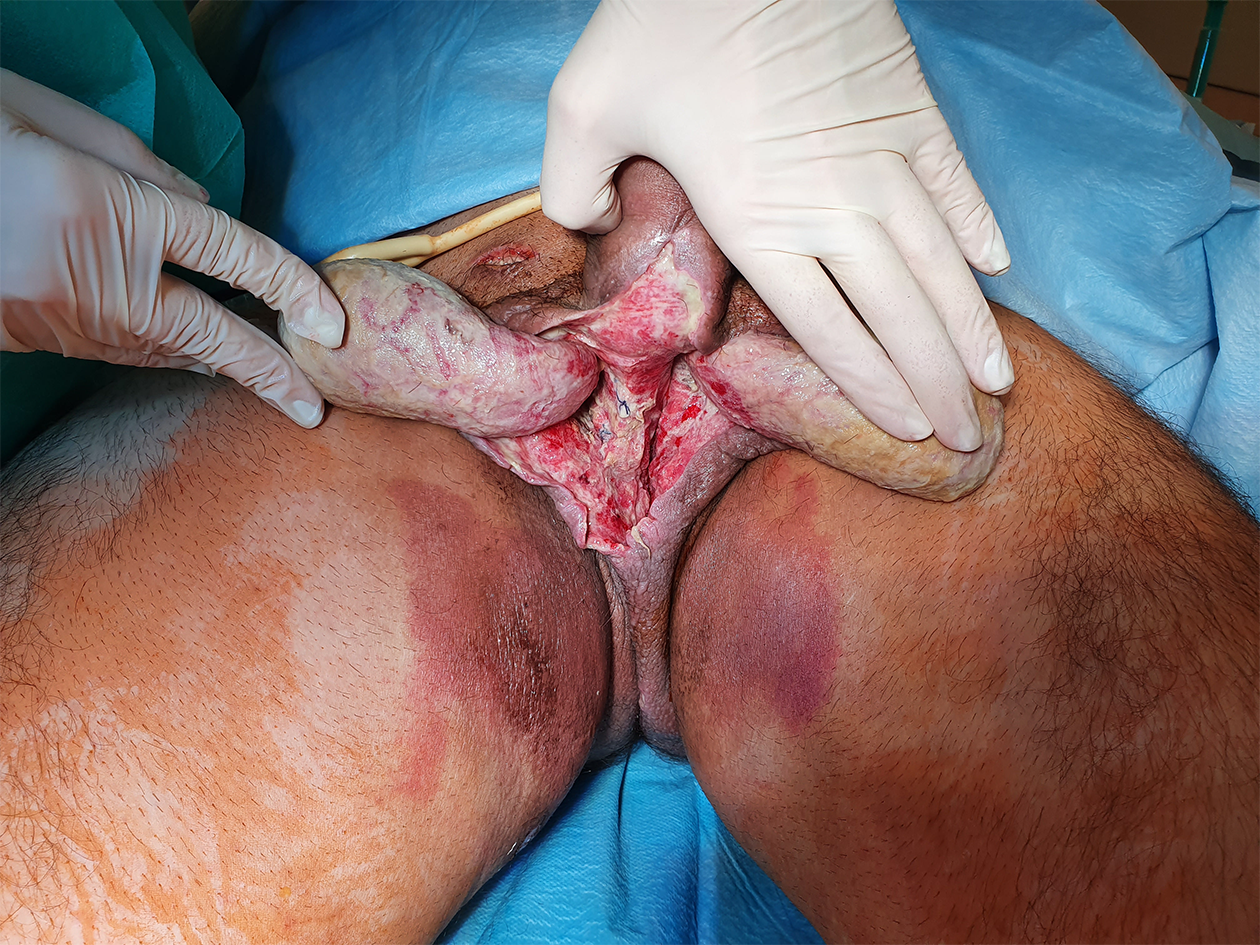
Granulated wound lodge tissue.
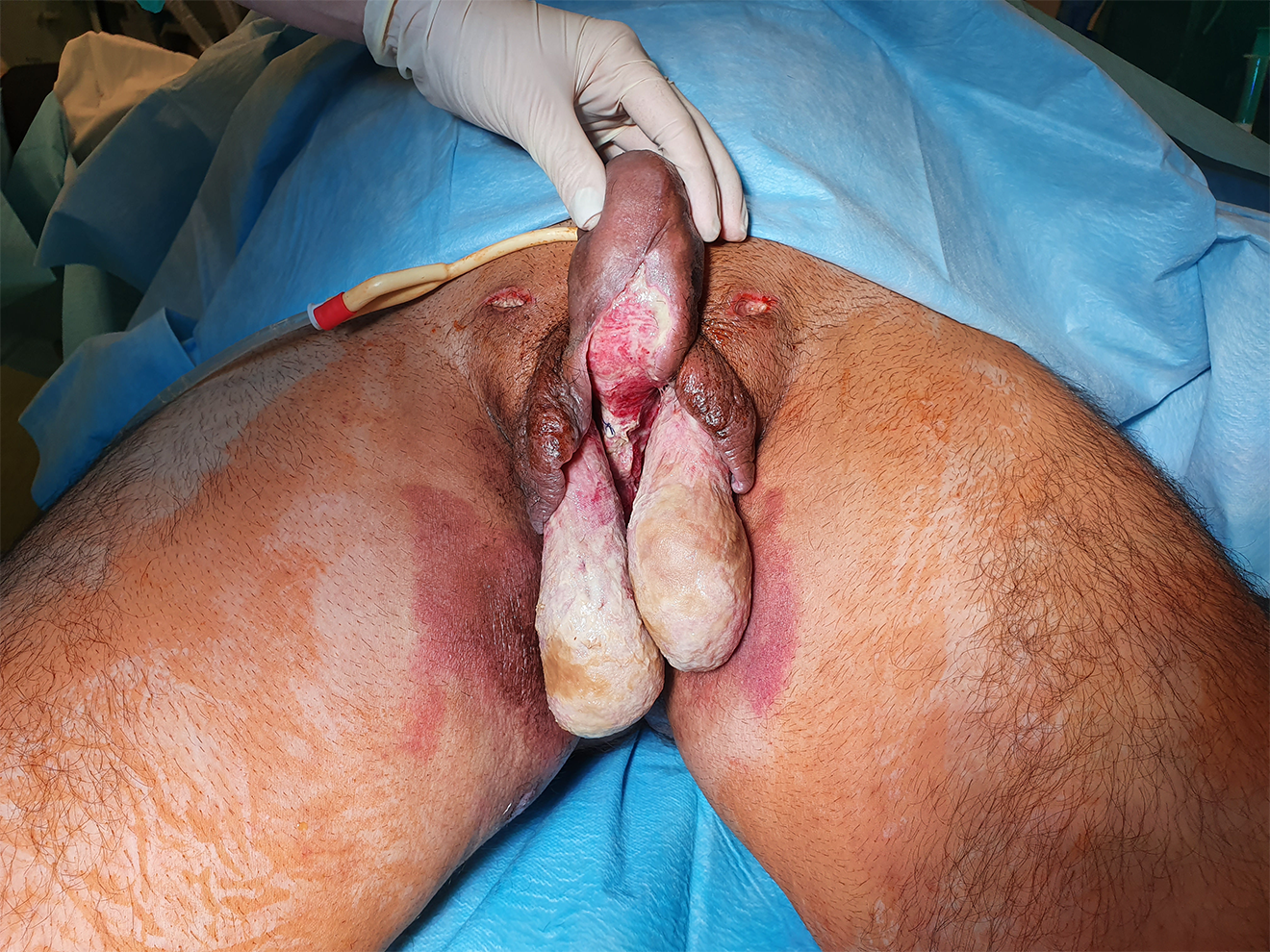
Fibrinoid tissue covering testicles.
Reconstruction was performed via bilateral pedicled anterolateral thigh (ALT) flaps, 9x20 cm each (Figure 5, 6, 7). Arterial perforators of the lateral circumflex femoral system were detached. Bilateral tunnels beneath m.rectus femoris, m.sartorius, and the medial skin of the thigh were made, connecting the donor site with the defect. After passing each flap through the tunnel, excess areas of the flaps were resisted. The flaps were consolidated in the midline to imitate the scrotal raphe. The scrotal defect was fully covered (Figure 8). Careful monitoring of hemostasis and wound washes were performed, edges were sutured in layers, drains were left.
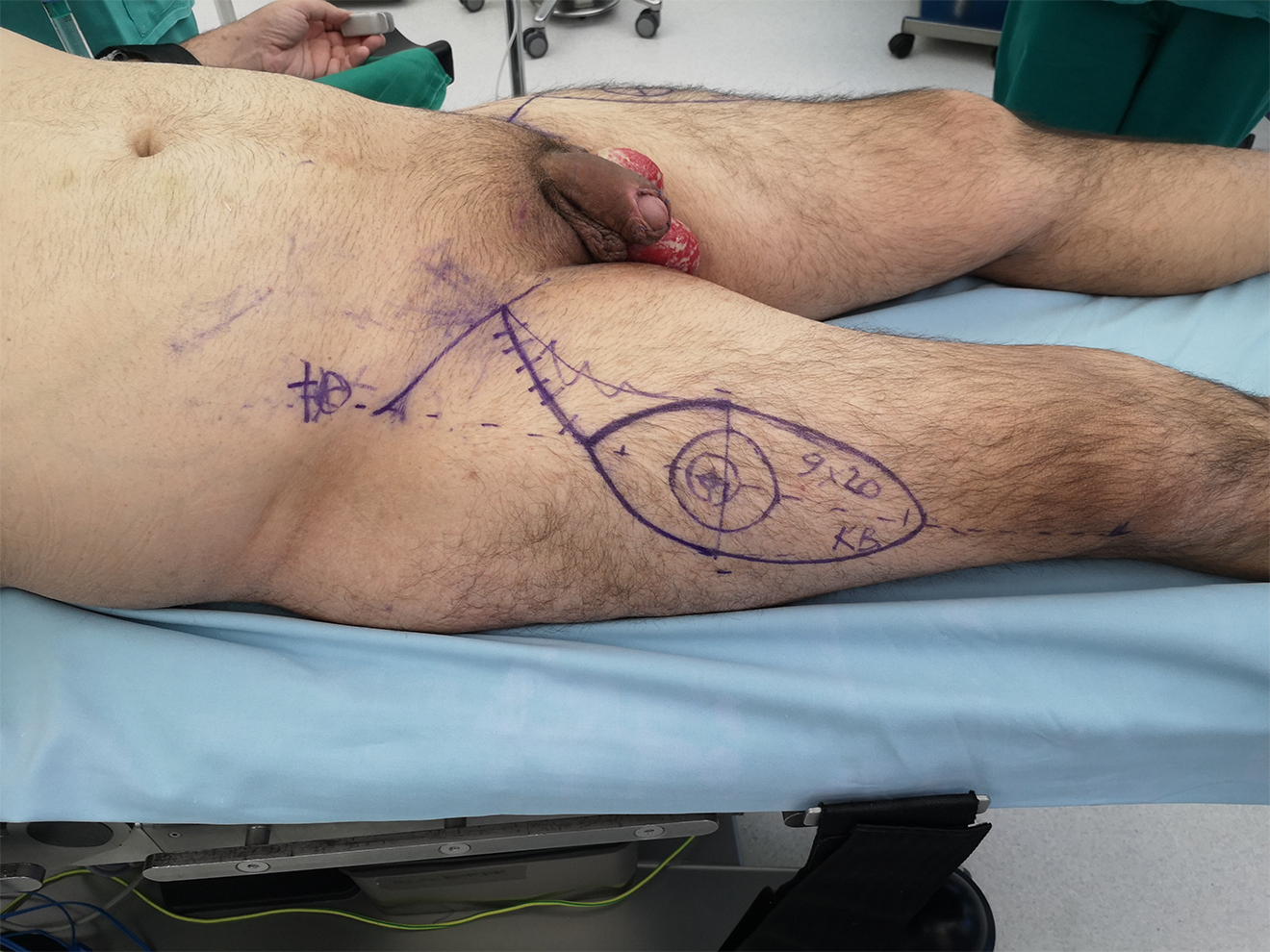
Right side: preoperative markings of ALT flap.

Left side: preoperative markings of ALT flap.

Preoperative markings of a bilateral ALT flap.
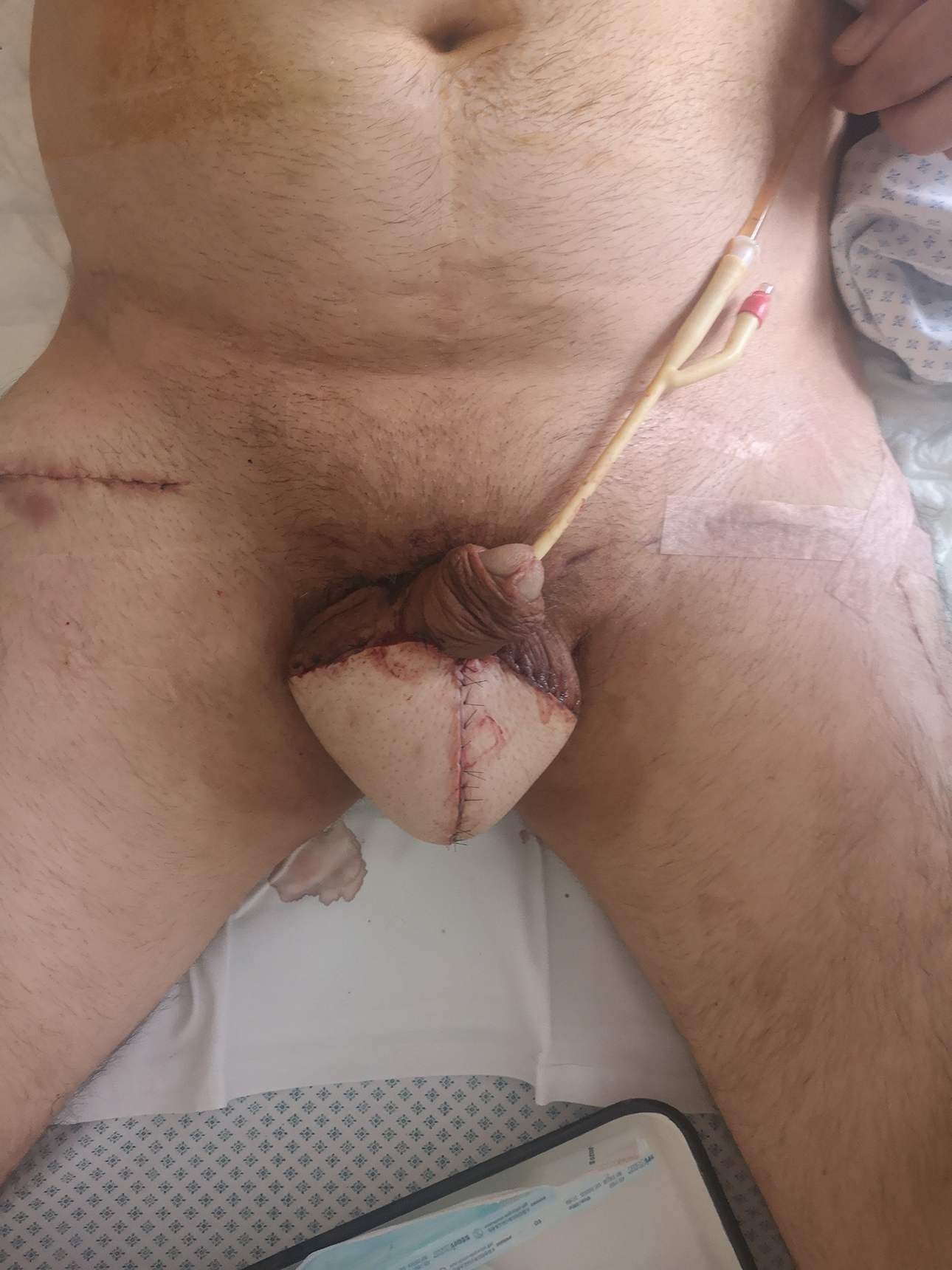
Postoperative result following first reconstructive surgery.
Postoperatively the vascularisation of both flaps was active, the drainage system was functioning, and gauzes were dry. It was decided to continue the appointed a/b treatment, and perform regular dressing of the wound once a day.
Seven days after the surgery, the patient reported a sudden pain in his right thigh. Additionally, the CRP levels increased up to 240 mg/l. Wet gauzes with purulent hemorrhagic exudate were noticed during the routine wound dressing. Consequently, the surgical team decided it was necessary to perform a flap revision surgery.
The right side of the flap exhibited a pale coloration relative to the adjacent areas of the skin, lacking any active blood circulation due to pedicle thrombosis. The following observations lead us to conclude that the right side of the flap had to be removed. The surgical team reopened the donor site wound to which a vacuum-assisted closure system (VAC) was applied.
Further management consisted of multiple debridements, a/b therapy and a VAC dressing change until wound healing potential was observed by the presence of healthy, pink-colored granulation tissue.
The scrotal defect was covered with a left-sided flap, however it was not enough for full coverage. 2x2,5 cm defects were left. Hence, Reverdin pinch grafts were used to close it.The grafts healed successfully (Figure 9).
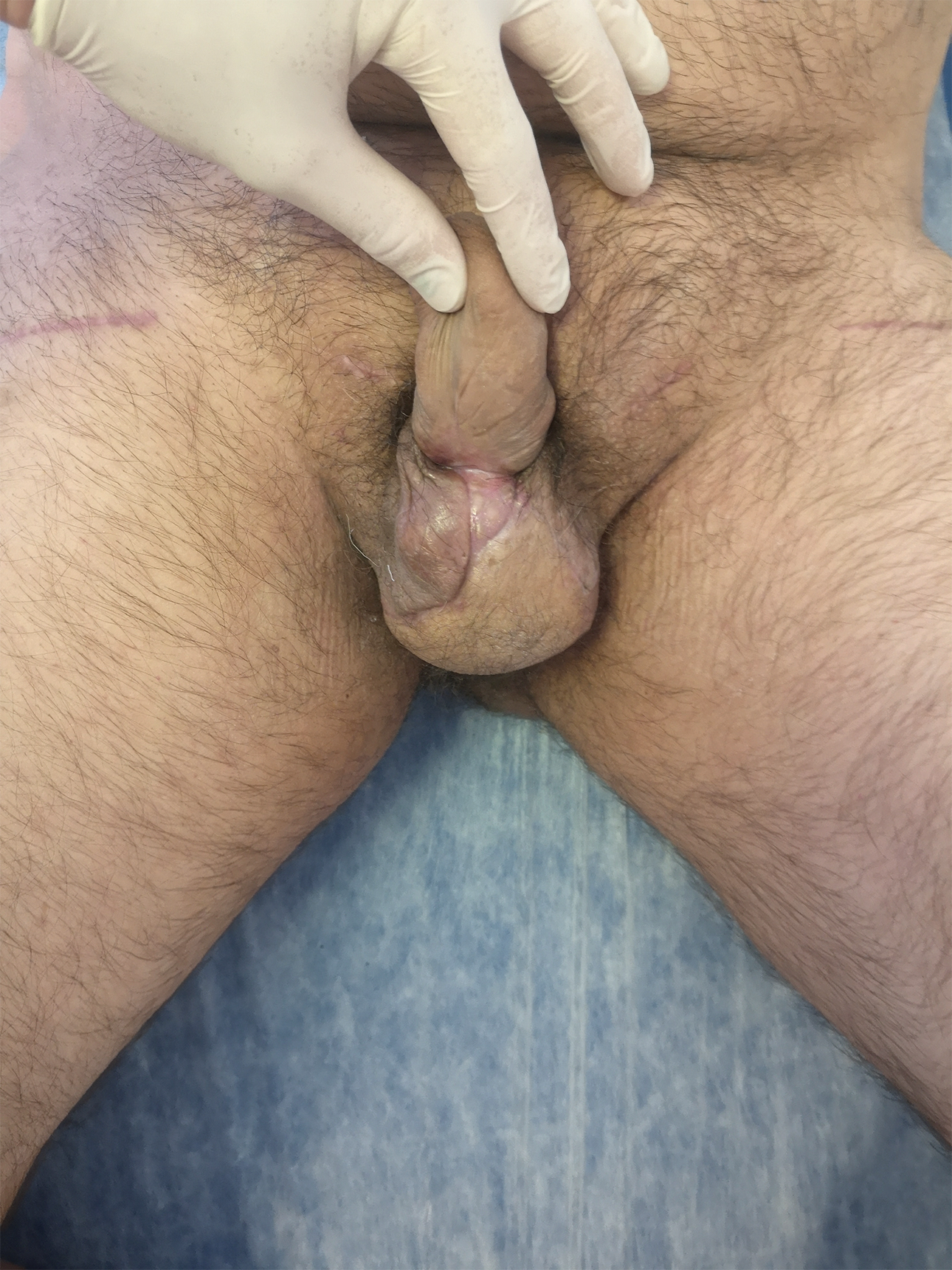
Postoperative result 3 months after surgery.
Discussion
FG is known to be a fulminant form of infective, polymicrobial, necrotizing fasciitis of the perineal, genital, and perianal regions. 6 Initially, it was defined as an idiopathic disease. However, it is currently believed that FG is caused both by aerobic and anaerobic organisms that invade through perineal and genital abrasions caused by various injuries, traumas, or interventions. The most common microorganisms found in wound cultures of patients with FG are Escherichia coli, Pseudomonas aeruginosa, Staphylococcus aureus, and Enterobacter cloacae. 7 FG has multiple predisposing factors, of which diabetes mellitus, chronic alcoholism, lymphoproliferative diseases, malnutrition, cytotoxic drugs, and HIV infection are the most common. 20-70% of patients with FG suffer from diabetes mellitus, 8 and 25-50% are presented with or have chronic alcoholism. 9 Our case is unusual because no portals of infection entry were detected and the patient was at low risk for both FG and surgical interventions. He hadn’t any particular comorbidities confirmed, which makes this case idiopathic.
Through the years, the mortality of FG remains high, averaging about 20%, 10 frequently due to delayed diagnosis and management. Thus, successful management of FG includes aggressive debridement, antibiotic therapy, fluid resuscitation, and quick diagnosis. 11 Due to the necessary treatments leading to the development of major soft tissue defects, this treatment poses a considerable reconstructive challenge as well.
Reconstruction of the defects left after multiple debridements is necessary both for acceptable aesthetic, psychological and functional results, one of them being the regulation of temperature required for normal spermatogenesis and hormone production in the testes.
There are several options known for the coverage of the defects - delayed primary closure, secondary intention or reconstructive options with flaps or skin grafts. Flap reconstruction is recommended for defects that are larger than half the surface area of the scrotum. In the present case, we used flaps, skin grafts, and secondary intention healing as methods to achieve the best results. Our choice for the reconstruction was the bilateral pedicled ALT flap. Although this flap is rarely associated with infectious postoperative complications (2,2%), the postoperative infection could not be avoided in our case. We can presume that the microorganisms that caused the primary infection were not fully eliminated, despite the normal inflammatory markers prior to the reconstructive surgery.
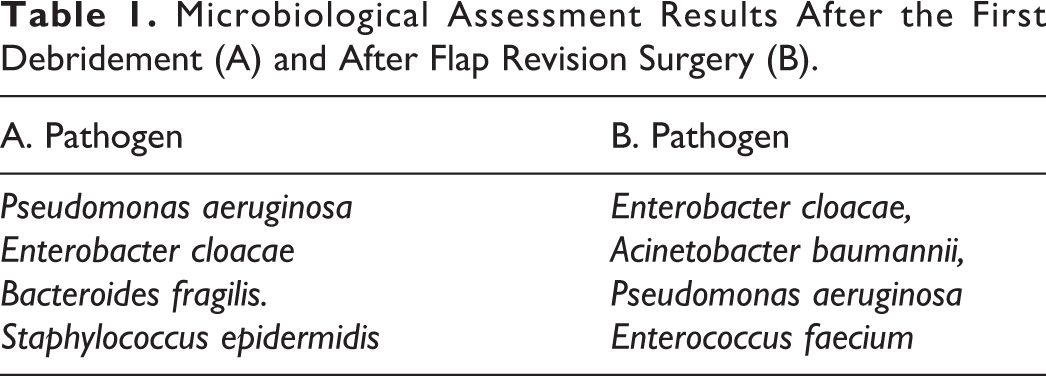
This is supported by the fact that some of the bacteria found in the microbiological examination of purulent material were the same. We compared microorganisms that were found at the time of the first debridement and during the flap revision surgery (Table 1).
Microbiological Assessment Results After the First Debridement (A) and After Flap Revision Surgery (B).
It is believed that the occurrence of wound infection depends on the closure time - the longer it takes, the more likely it is to get infected. 12 In our case the wound was open for approximately a month. We can presume that due to the long exposure of the defect microorganisms had appropriate conditions to persist, despite the antibiotic therapy and other preventative methods.
The difficulties associated with FG treatment is that we cannot predict how long it will take for a patient to recover before considering reconstructive options. There is a known technique for implanting testicles into subcutaneous thigh pouches. This method is temporary, however, it enhances recovery and provides a shorter hospitalization time, until conclusive scrotal reconstruction can be undertaken. 13,14 There is a chance that this technique would have reduced the number of surgical procedures performed for our patient.
Conclusion
FG is both a urological and a surgical emergency. Aggressive debridements that are mandatory for the successful management of the disease require thorough reconstructive surgery. The choice of the reconstructive technique mostly depends on the size of the defect that needs to be covered. A pedicled ALT flap provides reliable defect coverage, resulting in satisfactory functional and aesthetic results, even though, in the present case, it was partly lost.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
Written informed consent was obtained from a legally authorized representative(s) for anonymized patient information to be published in this article.
