Abstract
Over the past decade there has been a dramatic increase in the consumption of complementary and alternative medicine. The market for supplements and topical agents has grown, with recent reports estimating its value at 6.63 billion dollars. As more consumers utilize these largely unregulated products, it follows that healthcare providers will encounter new injury patterns related to them. Here we will discuss the evaluation and management of phototoxic reaction injuries sustained in a healthy 25-year-old female as a result of exposure to essential oils in the setting of ultra-violet A radiation.
Introduction
The global essential oils market has recently been valued at over 6.5 billion US dollars, with anticipated growth to over 11 billion US dollars by the year 2022. 1 This rapid growth highlights the growing popularity of alternative or holistic medicine, 2,3 a market which currently accounts for 30 billion US dollars annually. 2 According to the CDC, nearly half of adults seek out some form of alternative or complementary medicine either in place of or in addition to routine medical care. Essential oils have become tightly associated with this holistic approach. With approximately 40% of this market based in North America – both as the primary importer and exporter of oils – healthcare practitioners in the United States are increasingly likely to encounter patients who regularly use these products. 3
Bergamot oil, or orange oil, is a cold pressed essential oil derived from fruit. It is made from the bergamot orange originating in Italy. In 2015 bergamot oil dominated the essential oil market with over 52 kilotons produced. Bergamot oil has a scent of orange peel with floral tones. Given these characteristics it has become pervasive in both the personal care and cleaning product industries, the latter of which has largely contributed to its increased production. An increase in utilization of orange oil for therapeutic applications has been seen in the geriatric population as well. 3
There is some evidence to support the hypothesis that essential oils have a beneficial effect on circulation and soothing effects on the central nervous system, which in turn has fostered adoption of essential oils into aromatherapy and medical sectors. 4 As previously discussed, the high utilization of these products affirms both consumer interest in and awareness of these benefits. There is a slowly amassing body of literature regarding treatment of adverse effects such as phototoxic reactions due to essential oils, but the documentation of such events remains sparse to date. The presented case illustrates such a pattern of injury, in which a healthy 25-year-old female sustained mixed 1st and 2nd degree phototoxic reactions due to topical exposure to essential oils.
Description
Patient is a 25-year-old female with no significant past medical history presenting to the emergency department for burns to her chest. She reports that 2 days prior she underwent acupuncture at which time both lavender and bergamot essential oils were applied to her upper chest. Two hours following acupuncture she presented to a tanning salon and completed a session of tanning in a tanning bed. Upon returning home she showered and noted redness on her upper chest which she described as similar to a sunburn. The following day she had increased redness and tenderness to the involved region. Two days following her initial exposure she developed blistering. The patient denied prior skin sensitivity or allergic reactions, or recent changes in topical agents or household products.
On physical exam, the patient’s skin is Fitzpatrick type II. She is noted to have bilateral upper chest burns with blanching erythema towards the periphery consistent with first degree injury and 2 islands of blistering on either side of her chest, indicative of second-degree injury. Her total body surface area involvement totaled less than 1 percent (see Figure 1). No active drainage, purulence, or evidence of infection was noted. Following non-excisional debridement of loose epidermis, Litmus paper testing was performed and her second-degree burns noted to have a pH of 7 (neutral).
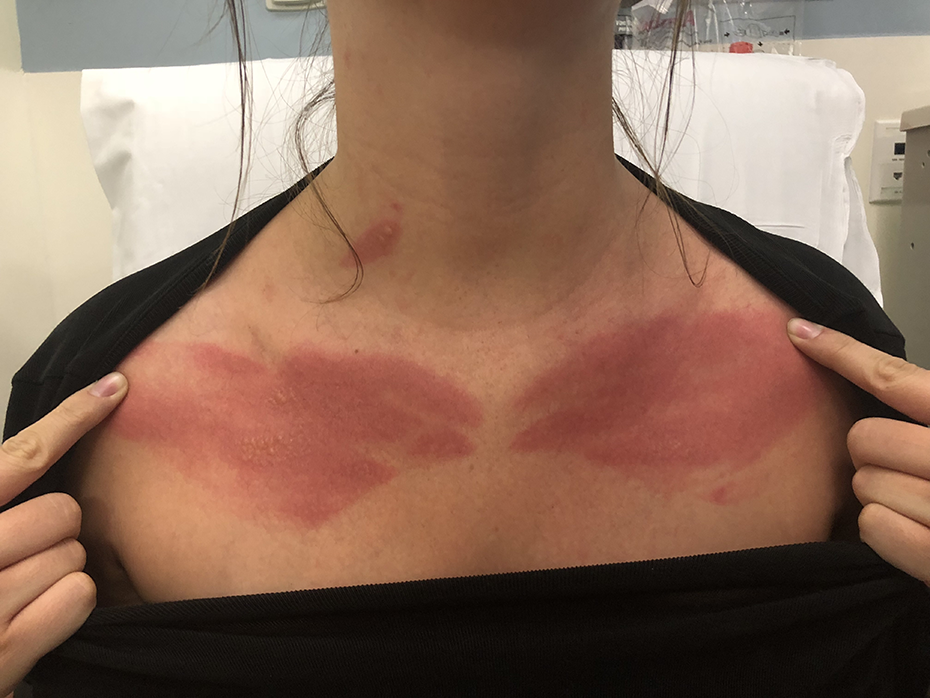
Patient 2 days following exposure to bergamot oil and UV-A rays from tanning bed.
Patient’s wounds were dressed in collagenase ointment and non-adherent silicone based dressings placed over the wounds with additional supplies provided in the emergency department for continued daily wound care. She was discharged home with follow up 4 days after presentation in burn clinic. At her follow up appointment, the patient was noted to be healing well with evidence of early re-epithelialization of her second-degree wounds and no signs of infection. Patient reported adherence to her wound care regimen.
Discussion
Phototoxic effects of Bergamot oil were described in the early 1900’s when it was noted that those who applied cologne water, containing the inciting agent, with subsequent sun exposure developed pigmented macules. 5 Bergamot oil is in the family of furocoumarins with the parent compound psoralen, which is a mutagen that works by intercalating into DNA resulting in cell apoptosis. 6 These photosensitive and melanogenic properties caused by the presence of furocoumarins, primarily bergapten (5-methoxypsoralen [5-MOP]) have led to strict regulation regarding the concentrations of this oil in commercially sold products in Europe. 5,7 Psoralens have been utilized in the medical field specifically for these effects such as in photochemotherapy with high intensity long wavelength UVA irradiation, more commonly known as PUVA therapy. In this treatment, a pharmacologically inactive compound is converted to the active metabolite by exposure to a radiation source such that diseased tissue can be targeted specifically. Therapeutic applications include psoriasis, mycosis fungoides, and various other dermal and epidermal neoplasms. Despite stringent methodology behind these treatments, there are still regular reports of phototoxicity resulting from this process. 8
A few recent reports have demonstrated that similar to PUVA, bergamot essential oils can result in phototoxicity resulting in burns when combined with ultraviolet radiation. In one case report, 2 patients suffered localized and disseminated bullous phototoxic skin reactions following bergamot oil exposure. 7 In both cases topical application of bergamot was followed by UVA exposure. Reports such as this highlight the possible health hazards of using psoralen-containing aromatherapy oils or those with similar composition and chemical properties. 7 Multiple reports cite the utilization of a tanning bed in combination with recent essential oil exposure. Tanning beds often emit UVA only due to purported decreased carcinogenic and oncogenic effects. 9 However, a higher concentration of UVA rays will activate psoralens to a greater degree than environmental UV exposure.
There is evidence to suggest bergamot essential oils may be effective in the treatment of hyperlipidemia, psoriasis, and even stress reduction. 10 Unfortunately, while these health benefits may be credible, the sale of essential oils primarily occurs under the label of cosmetics, and therefore has far less rigorous labeling and regulation requirements under the FDA. The MSDS for bergamot oils states that skin exposure can be adequately managed by irrigation with soap and water with application of an emollient recommended for any areas of skin irritation, after which formal medical attention should be sought. 11 While exposures are benign in the majority cases, a beauty product containing bergamot oil may not include warnings of adverse reactions or how to proceed in the case of such a reaction. The patient simultaneously had lavender oil applied that can result in contact dermatitis, but has a distinct chemical structure than bergamot oil and causes dermatitis through oxidation. 12 The patient previously used lavender oil without any irritation and therefore unlikely that it contributed to the burn that she sustained.
Given the potential severity of these adverse events, it is important that consumers be aware of the possible interaction between psoralen derived compounds and UV exposure. Similarly, healthcare providers should be familiar with this interaction so that patients utilizing holistic or alternative products can be educated appropriately. Patient’s sustaining phototoxic injuries from aromatherapy oils should be treated initially with irrigation with normal saline or water. Following removal of all remaining oil, the phototoxic reaction can be triaged according to depth of injury and total body surface area involvement. In this instance, treatment of a partial thickness (second degree) burn with collagenase and a silicone-based dressing to cover the involved area, which is standard practice for burn injuries of this depth at our burn center, yielded a satisfactory outcome with no residual scarring (see Figure 2).
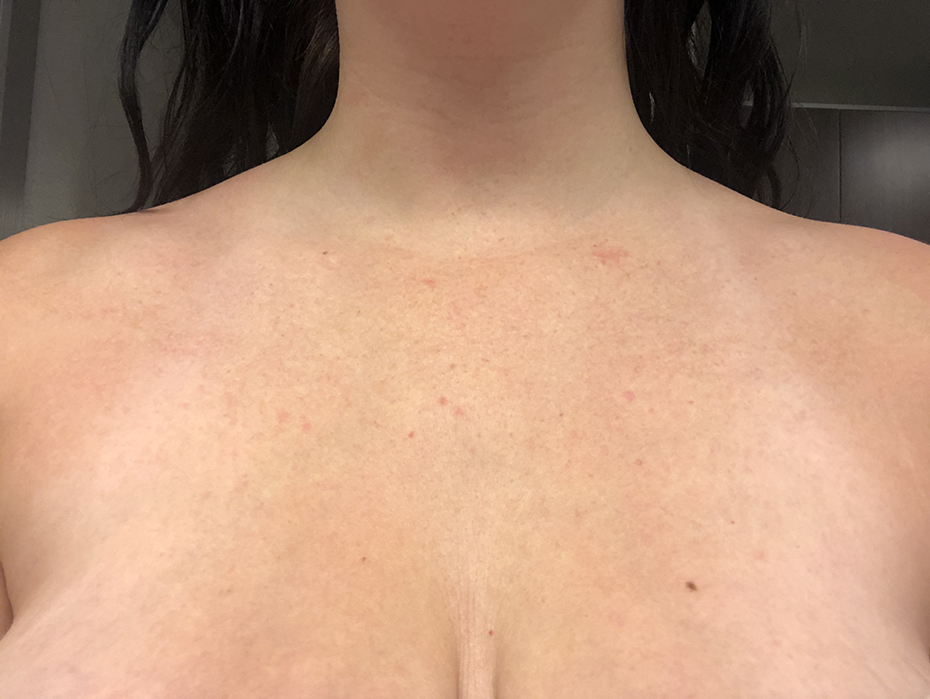
Patient 2 years following exposure to bergamot oil and UV-A rays from tanning bed after adherence of wound care with collagenase and silicone based dressings.
Conclusion
Alternative or holistic medicine has become an increasingly common practice both globally and in the United States. In regard to essential oils, multiple reports now exist in the literature describing chemical burns of varying severity following topical application of psoralen derived compounds such as bergamot oil in combination with UVA exposure. Given the marketing of these products under the branding of “cosmetics” it can be inferred that there will be overlap between the populations utilizing tanning salons and bergamot oil. It is important that providers regularly include a history of any natural products or supplements in their evaluation of patients. We must continue to educate ourselves and our patients in order to avoid such adverse events as described in this case.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
