Abstract
Fournier’s gangrene is a necrotizing infection of the soft tissue structures of the perineum that can extend quickly, requiring aggressive and repeated surgical debridement. This can result in extensive tissue loss and functional impairment, creating reconstructive challenges for plastic surgeons. We present a case of Fournier’s gangrene which resulted in complete loss of the pelvic floor musculature and functional loss of the urinary and fecal outlets. Given the extent of the defect and involvement of areas that would traditionally be used as donor site for local and regional flaps, reconstruction was sought with a free latissimus dorsi flap in combination with split-thickness skin grafting following serial debridement and negative pressure wound therapy. The patient survived and made a satisfactory recovery.
Introduction
The pelvic floor has many essential functions. Its muscular and fascial components separate the pelvic contents from the perineum; it allows for increases in intra-abdominal pressure while maintaining domain and preventing herniation, keeps the rectum and vagina closed, and maintains anal rectal angle for defecation and continence. There are several etiologies that can result in complex perineal defects, including hidradenitis suppurativa, pyoderma gangrenosum, necrotizing fasciitis/Fournier’s gangrene (FG), trauma, ulcers, autoimmune disease, congenital defects, and various malignancies. 1
Fournier’s gangrene is a rare and challenging type of necrotizing fasciitis that can involve the scrotum, penis, vagina, perineum, medial thighs, and lower abdomen, often resulting in rapidly progressive soft tissue necrosis and destruction along the perineal and genital fascial planes, resulting in high morbidity and mortality. 1 The disease spreads quickly, requiring repeated surgical debridement along with broad-spectrum antibiotic therapy. 2 Once the active infection is adequately controlled and necrotic tissues debrided, many reconstructive options exist depending on the location and extent of the defect.
The perineal region is a challenging and problematic area to reconstruct, with a number of site-specific obstacles. Goals of reconstruction include stable and durable soft tissue coverage, obliteration of dead space, coverage of internal organs, restoration of fascial integrity, prevention of herniation during changes in intra-abdominal pressure, potential for resuming sexual function, and restoring aesthetic outcomes. The “replace like with like” principle should be followed when possible, recruiting vascularized tissue while avoiding synthetic or bioprosthetic mesh in a contaminated wound bed. Reconstructive options include skin grafting, 3 local fasciocutaneous or myocutaneous flaps, 4 perforator flaps, 5-7 and rarely free flap transfer. Local options include advancement V-Y flaps, rotational or keystone flaps. Perforator-based flaps using the medial 8 and lateral 5-7 circumflex femoral vessels and profunda femoris branches can typically be considered. Anterolateral thigh, 6,7 tensor fascia lata, 8 rectus femoris, and vastus lateralis 9 are reconstructive options from the lateral thigh. Gracilis, 10 Singapore, groin flaps, gluteal flaps, 11,12 and posterior thigh flaps 13,14 are other reconstructive options. Abdomen-based flaps including vertical rectus abdominis myocutaneous 15 and deep inferior epigastric artery perforator (DIEP) flaps 16 are considered. Often, a combination of negative pressure therapy, 17 -19 dressing changes, secondary healing, and skin grafting can accelerate the time to healing. A goal of reconstruction is to minimize the risk of fistulization, infection, wound breakdown, and perineal herniation. The surgeon should choose a method of reconstruction that is suitable to address the defect, considering the patient’s ability to tolerate a long operation. 20
We present a case of extensive perineal defect following FG in a paraplegic patient. As many of the well-described options for perineal reconstruction were within the zone of injury, or were insufficient in size to address the extent of the wound, the defect was reconstructed by combining a free latissimus dorsi (LD) flap with split-thickness skin grafting (STSG). Despite preexisting comorbidities and extensive pelvic muscle and organ involvement, the patient survived and recovered satisfactorily. To our knowledge, this is the first described case of LD flap for repair of such an extensive perineal defect secondary to FG.
Case Presentation
A 71-year-old male presented to a community hospital with a wound in his left perineal area after a fall. The patient had a history of trauma-induced paraplegia since 1999 with a spinal cord injury at the level of T11-12. He was functionally independent at the time of injury. His past medical history was also significant for a previous non-ST segment elevation myocardial infarction (NSTEMI) with PCI, hypertension, dyslipidemia, and type II diabetes. His medications included fondaparinux, aspirin, clopidogrel, lisinopril, hydrochlorothiazide, metoprolol, rosuvastatin, metformin, insulin, and oxybutynin. He was a nonsmoker.
The patient fell and injured the left side of his perineum, subsequently developing a necrotizing infection. After initial debridement at his home hospital, he was transferred to our care and admitted to the intensive care unit (ICU). A computed tomography of the abdomen showed soft tissue loss within the left perineum with gas locules involving the left upper thigh, mons pubis, left gluteal region, and perineum. The ulcerated and necrotic areas were surgically debrided multiple times by general surgery and involved the left buttock, left thigh, left testicle, perineum, groin, rectum, pelvic floor muscles, and ischial tuberosities. Despite multiple serial debridement and prolonged intravenous antibiotic therapy with vancomycin, ceftriaxone, and metronidazole, the necrotizing fasciitis progressed. Due to bowel involvement, the patient had a left mucous fistula and right end colostomy created by general surgery with an open midline laparotomy incision. Due to extensive necrotic penile and prostate tissue, a penectomy and prostatectomy were carried out and the remaining bladder neck was catheterized (Figure 1). Otolaryngology performed a tracheostomy. Multidisciplinary care included otolaryngology, general surgery, urology, anesthesia, ICU, medicine, infectious disease, cardiology, geriatrics, nursing, physiotherapy, and occupational therapy. The patient was left with a complex pelvic floor defect with complete loss of the perineum, buttock, and muscular diaphragm.
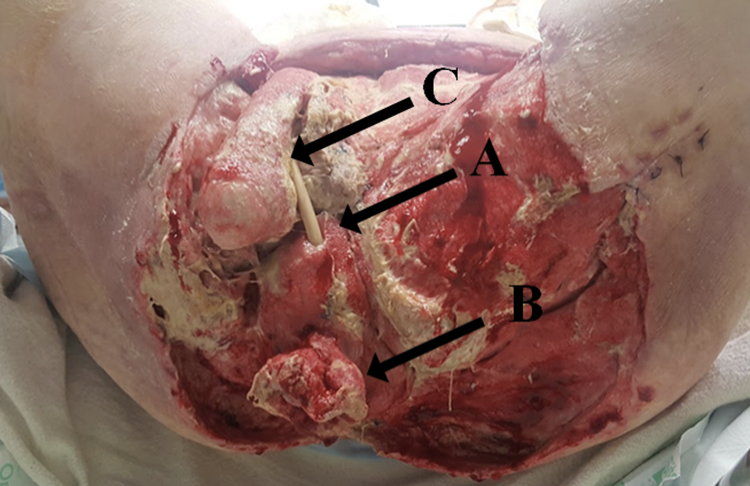
Perineal view with the patient in the lithotomy position. Extensive soft tissue defect of the perineum extending to the buttock posteriorly, bilateral medial thighs, and the lower abdomen. Bladder neck (A) is catheterized and rectal stump (B) and right testicle (C) are exposed.
The exposed rectal stump was partially resected and oversewn by general surgery. It became incorporated into the granulation tissue over the course of several serial negative pressure wound therapy (NPWT) dressing applications. The remaining right testicle was partially buried into the soft tissue of the thigh.
After resolution of the acute infection, plastic surgery assumed management of this patient. The patient received NPWT dressing changes and further serial debridement (Figure 2). Due to the extent of the defect, the bladder was exposed and there was leakage of urine around the catheter in the bladder neck. Urology and interventional radiology were consulted. Nephrostomy tubes were placed in the lower back bilaterally to divert urine and the ureters were clipped. An intravenous pyelogram confirmed that there was no urine flow to the bladder. The remaining bladder was allowed to granulate with NPWT dressing changes.
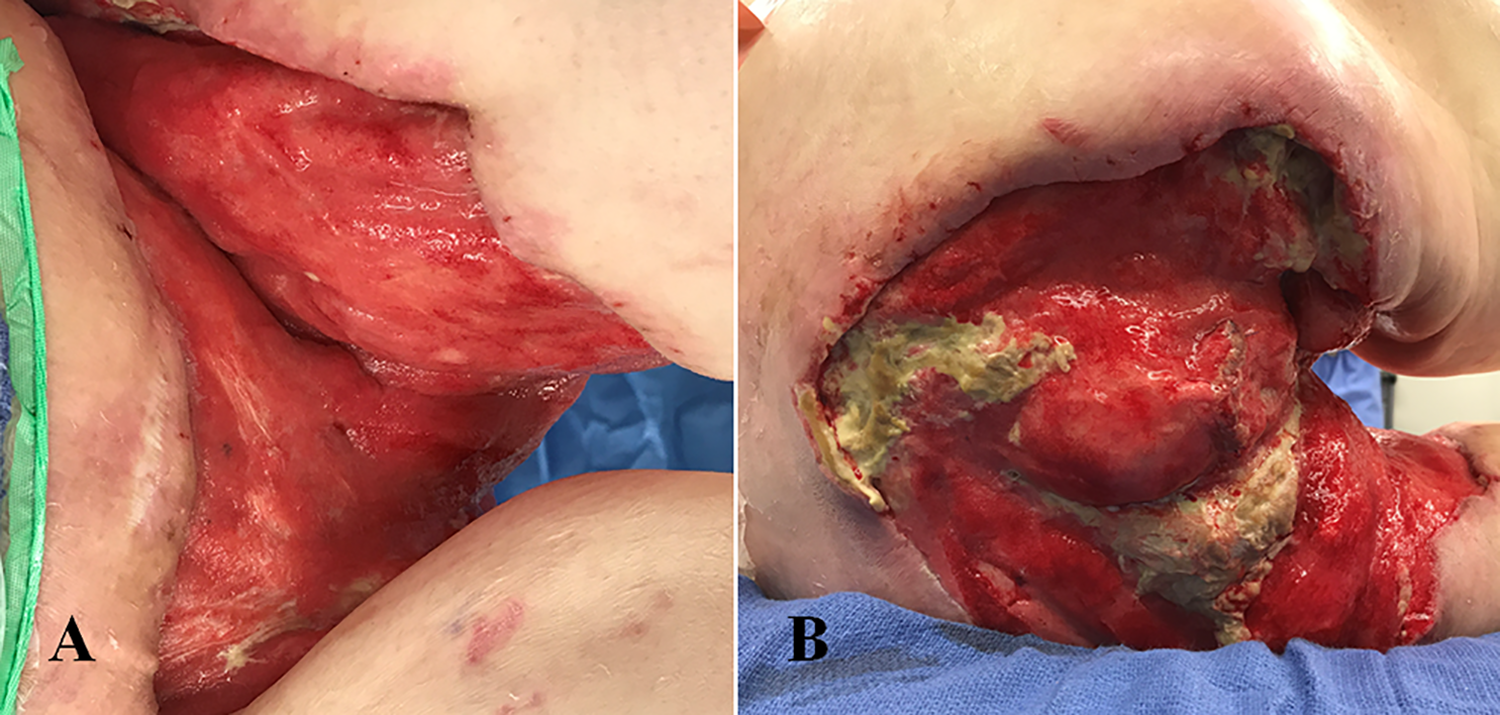
Perineal defect following serial debridement and negative pressure wound therapy application. Anterior perineal view (A) and posterior perineal view (B) with the patient in the lateral position. Granulation tissue is present throughout the wound bed. There is exposed ischial and sacral bone and exposed residual bladder neck and rectal stump.
Abdominal donor sites were not considered given the extent of the FG into the lower abdomen, placement of the right colostomy and left mucous fistula, and partially open midline laparotomy incision. Reconstructive options from the left thigh, groin, and buttocks were not viable given the extent of soft tissue loss and involvement of the musculature. We considered reconstruction using the right thigh, but we were concerned about limited size and reach to cover the exposed ischium and sacral bone. It was also considered that the thigh musculature in a long-term paraplegic patient would provide less substantial coverage given the fatty atrophy of muscle bulk and less predictable harvest. Although we were not keen on sacrificing the latissimus muscle in a paraplegic patient, we decided to proceed given the size of the defect and limited viable reconstructive options in the context of extensive soft tissue loss.
A free LD flap was performed. A skin paddle was raised with the muscle to assist with postoperative monitoring. The LD flap was raised in the usual fashion. The right groin was chosen as the recipient site as the left groin had been more extensively debrided. No satisfactory arterial branches outside the zone of injury were available for anastomosis so the arterial repair was performed end to side to the femoral artery. The flap vein was anastomosed end to end with the saphenous vein using a coupler.
The LD myocutaneous flap provided adequate coverage of the exposed vital structures. Exposed muscle flap was covered with STSG (Figure 3).
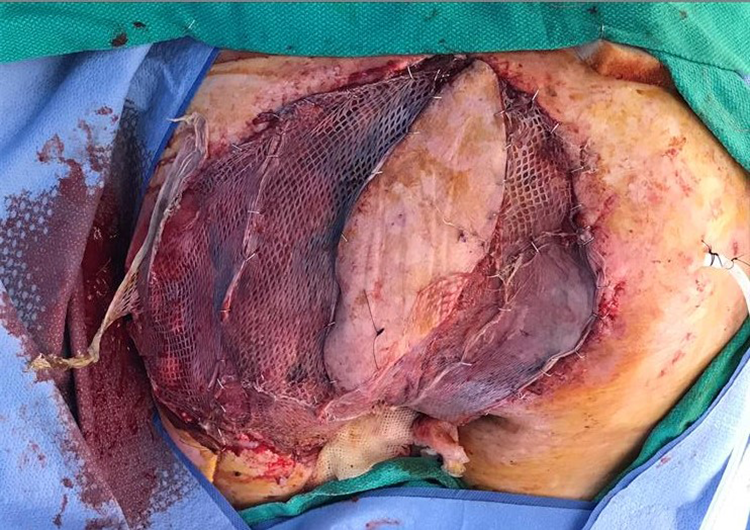
Immediate postoperative view of the reconstructed defect with the latissimus dorsi (LD) flap inset and remaining areas covered with skin grafts from the bilateral thighs.
The patient had a moderately prolonged hospital stay postoperatively secondary to a transient bout of delirium and marginal dehiscence of the LD flap in 2 or 3 areas. These areas were treated with dressings. The flap survived and healed with supportive management. One month after the procedure, the patient was repatriated to his home hospital in stable condition.
Discussion
Fournier’s gangrene has historically been linked to a high mortality rate. Length of stay in hospital has recently been shown to be associated with advanced age, high serum alkaline phosphatase, low hematocrit, and preexisting comorbidities such as hypertension and diabetes. 21,22 Diabetes is generally implicated among patients with FG, another factor which can impair wound healing. 21 The mortality rate has improved over the years and was recently estimated at about 5%, 23 although there have previously been studies that state it can be as high as 40%. 22 Our patient had a severe case of FG and loss of the pelvic floor which required both urinary and fecal diversion. Suprapubic tube placement and fecal diversion are common necessities in FG patients which play a significant role in impacting length of stay in hospital. 23
Reconstruction of the perineum following necrotizing soft tissue infections remains an ongoing challenge that requires specific case-to-case considerations. Many reconstructive options exist and are described in the literature. The choice of reconstruction ultimately depends on the zone of injury and extent of the pelvic floor defect. In this case, many of the commonly utilized reconstructive options for perineal defects were not sufficient and/or were within the zone of injury.
This case was especially problematic given the patient’s multiple preexisting comorbidities, extent of pelvic muscle involvement, large size of defect, and exposure of bone and pelvic organs. We recognized the importance adequate debridement and temporizing the wound with NPWT dressing changes. It was imperative to establish stable diversion of urine and feces prior to reconstruction to prevent wound breakdown, infection, and fistula formation. We wanted to provide stable and durable coverage of the remaining pelvic organs and exposed bone. Although NPWT combined with STSG is widely used as a treatment for pelvic defects, it may not have provided the durability of coverage necessary for a paraplegic patient who is consistently sitting or lying down. We sought reconstruction that would withstand mechanical shear forces during patient transfer. We wanted to provide durable coverage so that the residual bladder and rectal stumps would not become exposed with time. In addition, we wanted to create a supportive sling to prevent herniation of pelvic contents during movement, coughing, or other Valsalva maneuvers. Although we did not want to sacrifice the LD muscle which is especially important in a paraplegic patient, it was a viable option given its large size, bulk, and reliability.
Abdominal donor site options including a DIEP flap and unilateral rectus abdominis muscle flap were not appropriate options given the extent of the FG into the lower abdomen, recent placement of right-sided colostomy, and violated abdominal wall from a recent and still partially open laparotomy incision. One other consideration would have been to do a thoracodorsal artery perforator flap versus a free LD flap. Ultimately, this was felt not to be an appropriate option. The comparatively thin nature of the perforator flap would not provide robust enough coverage over the exposed ischium and sacrum, creating a higher risk for subsequent breakdown and pressure ulceration in a paraplegic patient. 24 Furthermore, the LD muscle flap was felt to be a better choice in a potentially contaminated wound as the more robust vascularity has enhanced potential for bacterial clearance.
The LD flap, based on the thoracodorsal artery, is often utilized given its size and bulk, relatively long vascular pedicle, and consistent anatomy. 25 The LD flap has been used with good results in cases of abdominoperineal resection for oncologic malignancies, providing well-vascularized coverage for large, sometimes previously irradiated defects unsuitable for reconstruction with the more commonly utilized local and regional flaps. 26 -28
We report a case of complex perineal defect being reconstructed successfully with a free LD flap using an end-to-side femoral artery anastomosis in combination with STSG. To our knowledge, no prior FG reconstruction cases using this method have been reported. Although rarely necessary given the number of regional perforator flap options, free flaps for perineal defects can provide reliable and robust coverage when the defect is too large, the zone of injury extends to involve potential donor sites, or the presence of a stoma excludes the option of abdominally based flaps. Although rarely used in perineal reconstruction, we demonstrate that the LD flap’s versatility can be expanded to postinfectious pelvic reconstruction should other reconstructive options be compromised.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Statement on Human Rights
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2008 (5). Informed consent was obtained from all patients for being included in the study.
Statement of Informed Consent
Informed consent was obtained from all individual participants included in the study.
