Abstract
Degloving injuries of the foot pose an important challenge to the reconstructive surgeon. Key features of reconstruction include sensibility, stability, and durability. Preservation of plantar sensibility is considered to be a critical factor in the evaluation of lower extremity trauma, with its absence once being considered an indication for amputation. However, recent studies show that outcomes following limb preservation are not as adversely affected by a lack of plantar sensation than was once thought. With the increasing practice pattern of attempting limb salvage in the face of impaired plantar sensation, methods and devices designed to provide patients with maximal protection for loss of protective sensation (LOPS) in the affected limb are critical. The authors present the innovative use of the SurroSense Rx smart insole system (Orpyx Medical Technologies Inc, Calgary, Canada) in the management of LOPS in a patient with a degloving injury of the foot that was reconstructed with a latissimus dorsi free flap and skin graft. To the authors’ knowledge, this is the first reported case of use of such a system following a traumatic injury to the lower extremity.
Keywords
Introduction
Degloving injuries involving the plantar foot pose significant challenges for surgical management and rehabilitation, given the functional requirement of any reconstruction to withstand the repetitive trauma associated with weight-bearing and ambulation. 1 –6 Injuries to the heel are particularly challenging, as the heel plays a vital role in weight transmission and walking dynamics. 7 Native plantar glabrous skin is thick and durable, allowing it to tolerate significant stress from weight and shear forces, while also making it difficult to reconstruct. 8
Optimal plantar reconstruction provides durable coverage with a favourable aesthetic, while enabling sufficient protective sensation to prevent pressure sores. 9 In the setting of significant tissue loss, especially of the heel, robust coverage is often achieved with skin-grafted muscle flaps, such as serratus, latissimus, and rectus femoris flaps. 10,11 Coverage with microvascular free tissue transfer has the advantage of providing abundant, healthy soft tissue in various thicknesses, depending on the size and location of the defect. In addition, free flaps can be innervated to provide some sensory feedback. Despite their durability, however, the loss of plantar protective sensation (LOPS) that often persists in these patients, even in the presence of nerve coaptation, leads to neuropathic ulceration in upward of 23% of cases involving plantar defect reconstruction. 12,13
Post-operative diligence, patient education, and meticulous foot care are extremely important in maintaining results without ulceration. 14 Although specialized orthotics can help prevent recurrent breakdown, 15 these are no substitute for the dynamic feedback cues provided by sensate plantar skin.
The authors present the innovative use of the SurroSense Rx in the management of LOPS in a patient with a degloving injury of the right heel that was reconstructed with a latissimus dorsi free flap and skin graft. To date, this device has been used and studied exclusively in patients with diabetic peripheral neuropathy at high risk of first and recurrent plantar ulcers. To the authors’ knowledge, this is the first reported use case of such a system following a traumatic injury to the lower extremity.
The SurroSense Rx (Figure 1) is a smart insole intended to prevent plantar ulcers in the context of LOPS. The device compensates for LOPS by providing dynamic smartwatch-based cues for effective, on-demand off-loading. This feedback is based on the identification of critical time/pressure signatures in insole sensor data. When safe pressure and time thresholds are exceeded, the patient is instructed to go through a series of off-loading steps, including walking on the spot, actively taking weight off the affected foot, and/or checking the footwear for fit or the presence of a foreign body (eg, a rock inside the shoe) in an effort to offload the area.

The SurroSense Rx smart insole system (Image used with permission from Orpyx Medical Technologies Inc, Calgary, Alberta).
Case Report
The patient is a 19-year-old male who sustained a degloving injury of the right foot, including the plantar skin on the proximal half of the foot, following a motor vehicle collision (Figure 2). This was resurfaced with microvascular free tissue transfer of the left latissimus dorsi muscle, covered with a split thickness skin graft (Figure 3).
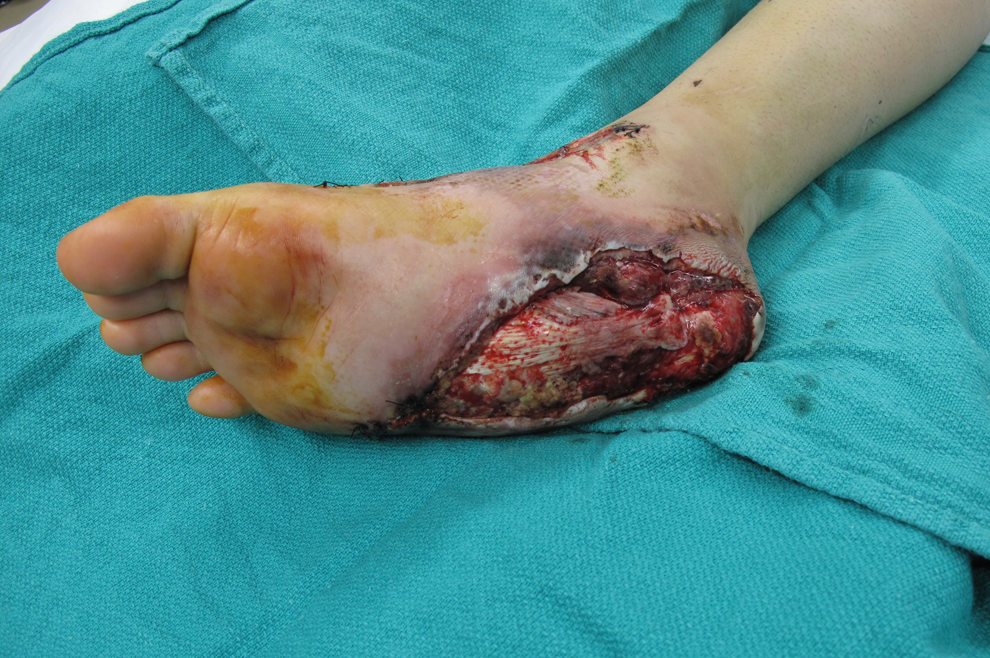
Patient foot post-degloving injury to the right heel.
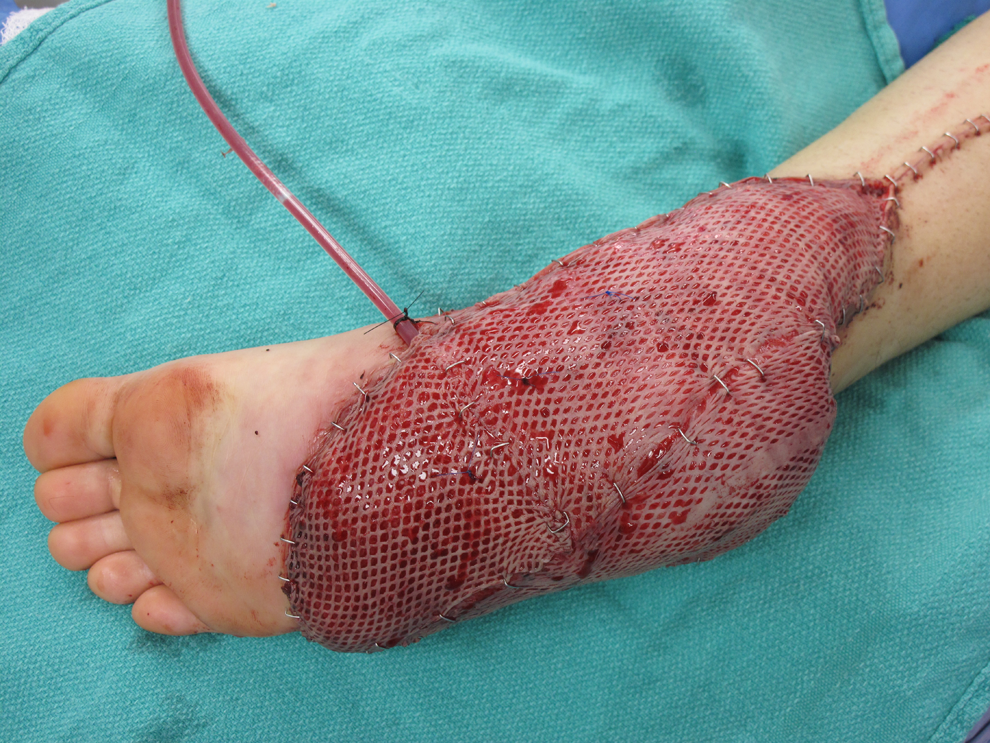
Patient foot post-reconstruction, involving microvascular free tissue transfer of the left latissimus dorsi muscle, covered with a split thickness skin graft.
In the immediate post-operative period, the patient experienced minor wound dehiscence over the right heel. Fragility of the reconstructed right heel, coupled with LOPS of the overlying skin, meant that the right heel required daily taping and ongoing diligence to help prevent secondary and tertiary pressure ulceration. In an effort to help manage this condition, the patient was fitted with the SurroSense Rx to enable ongoing plantar pressure feedback from the insensate foot.
Results
The patient was monitored with the device for a total of 181 days, throughout which no recurrent ulcerative events were seen (Figure 4). Adherence over time is shown in Figure 5.
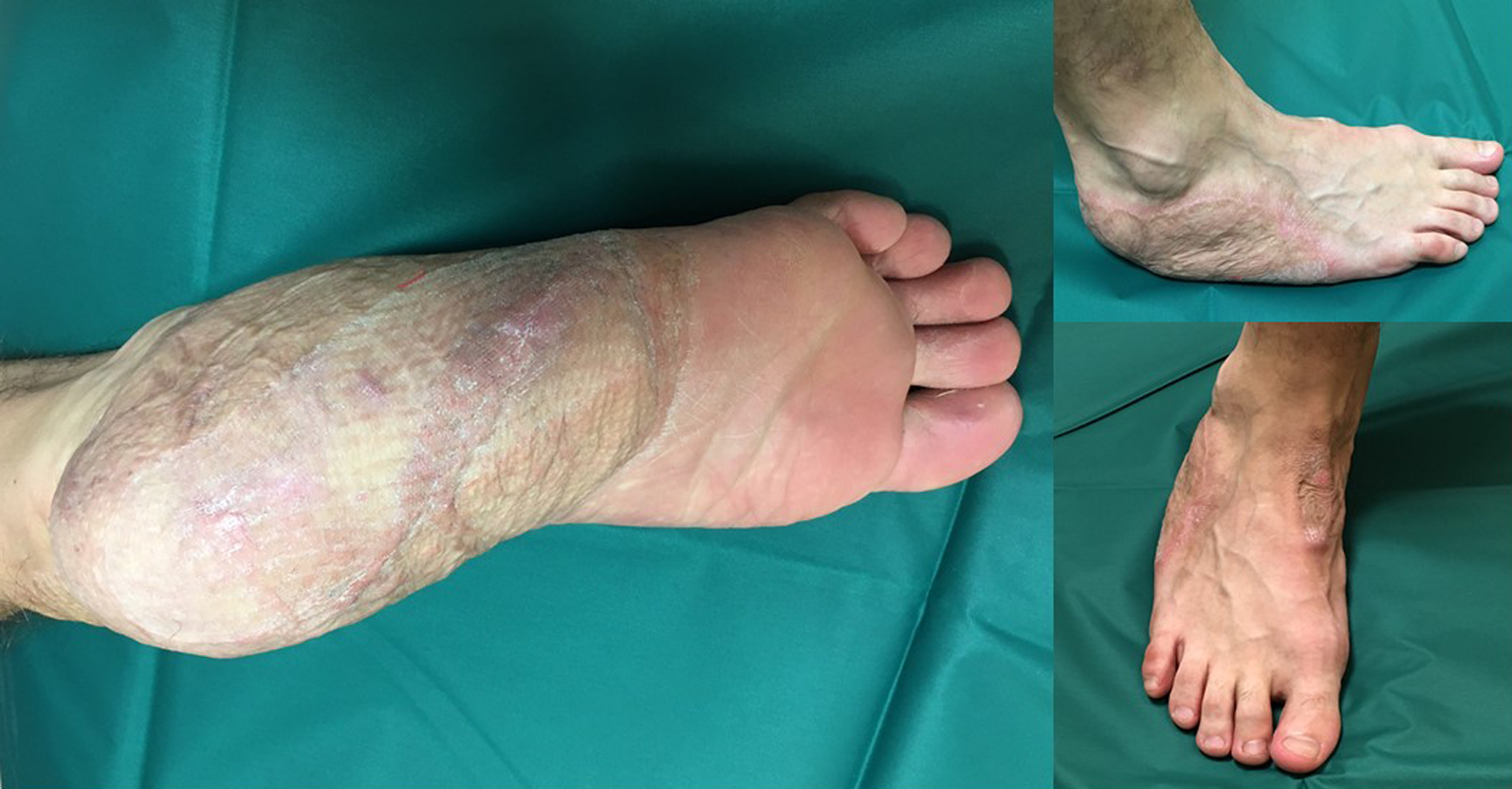
Patient’s healed reconstructed right foot.
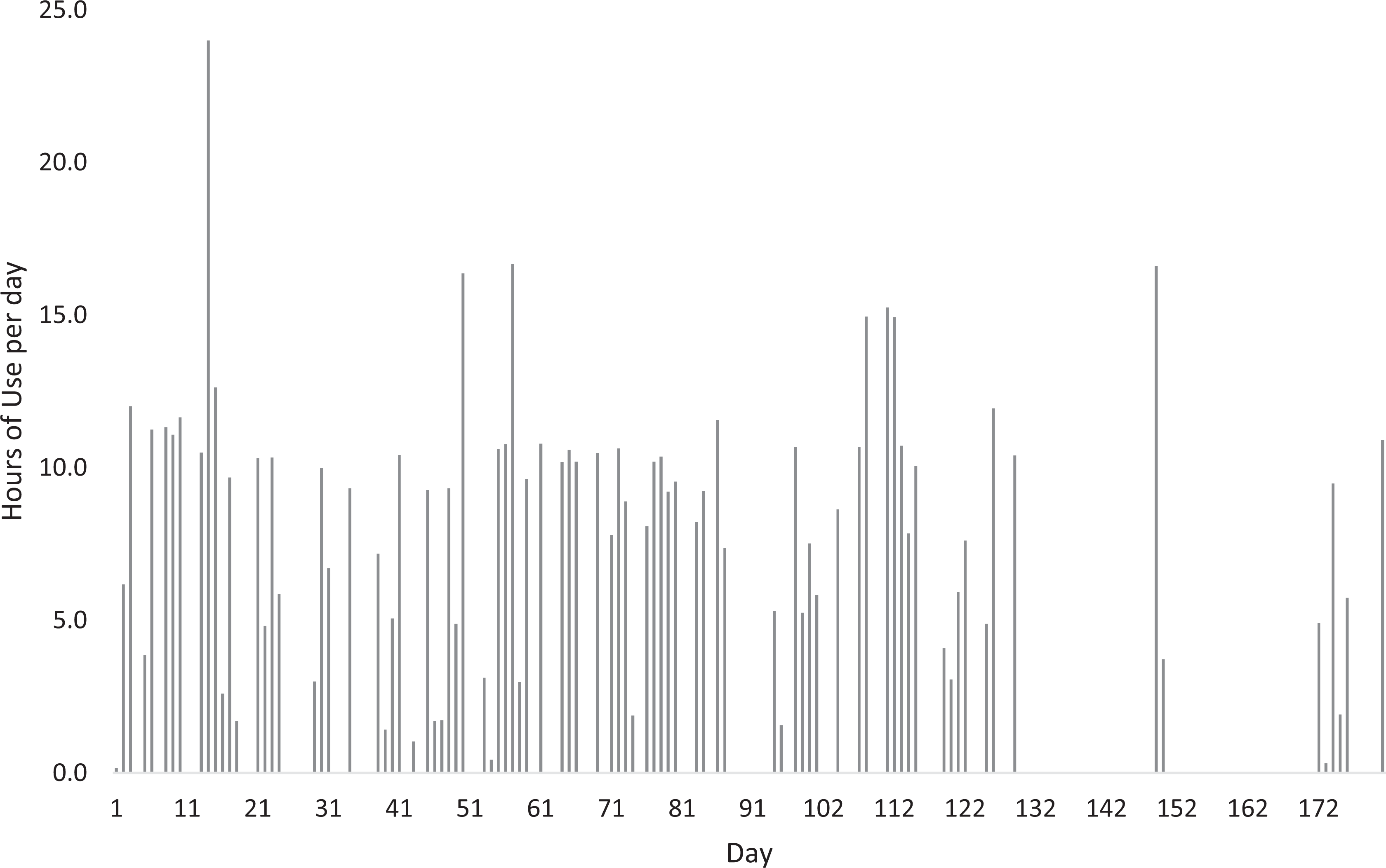
Patient adherence (hours of device use per day) over the period of device use.
The patient generated alerts as per Figure 6. An alert was generated when pressure on a single region was inadequately offloaded (ie, pressure over time differed from what one would see in a normal, sensate foot). Alert length was defined as the time from the alert onset to the time of effective off-loading.
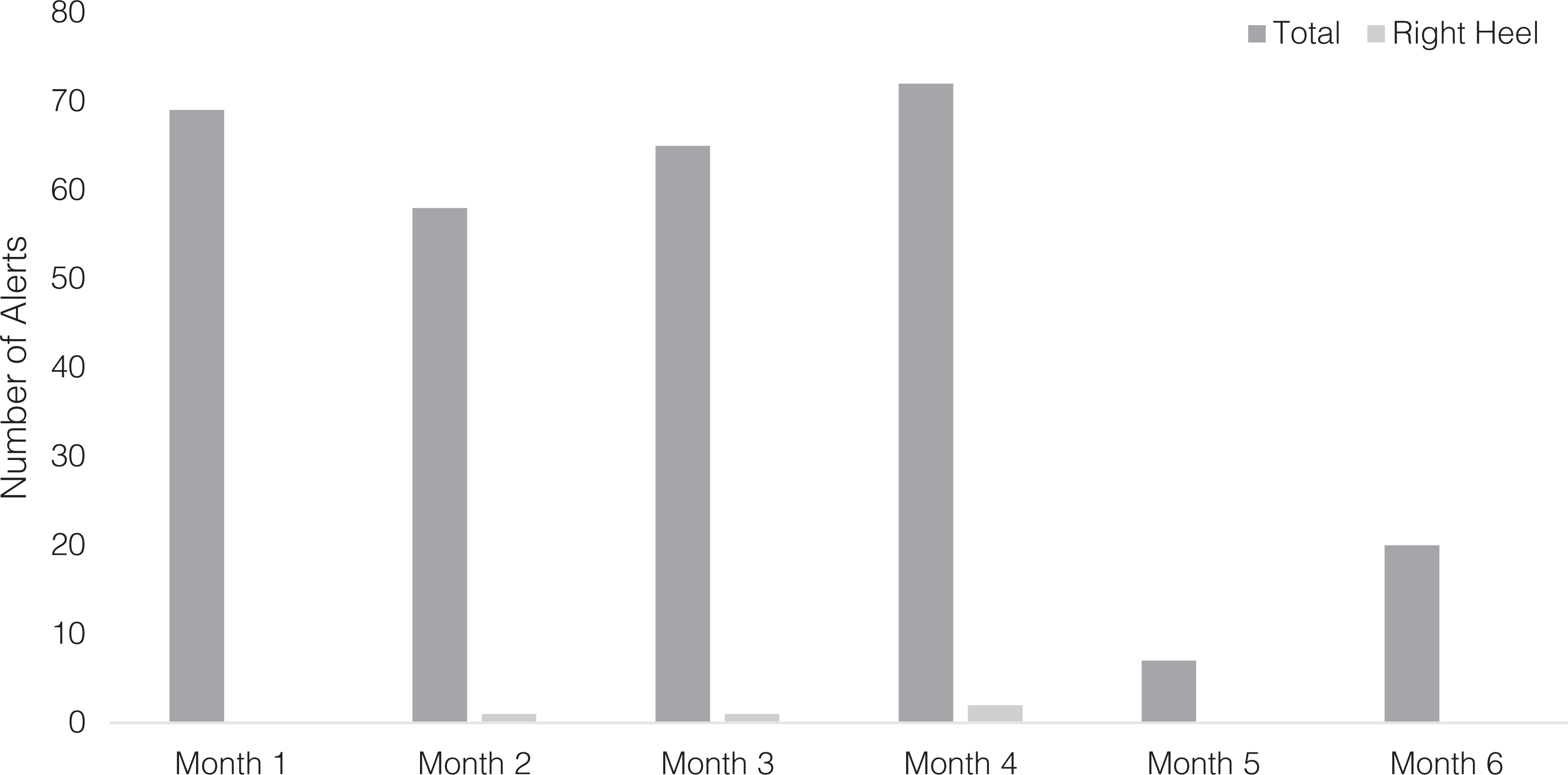
Total number of alerts for the right heel sensor compared to all other sensors (right and left).
The left foot demonstrated a significantly higher alert number than the right (Figure 7). Notably, the affected region (right heel) triggered substantially fewer alerts than any other region.
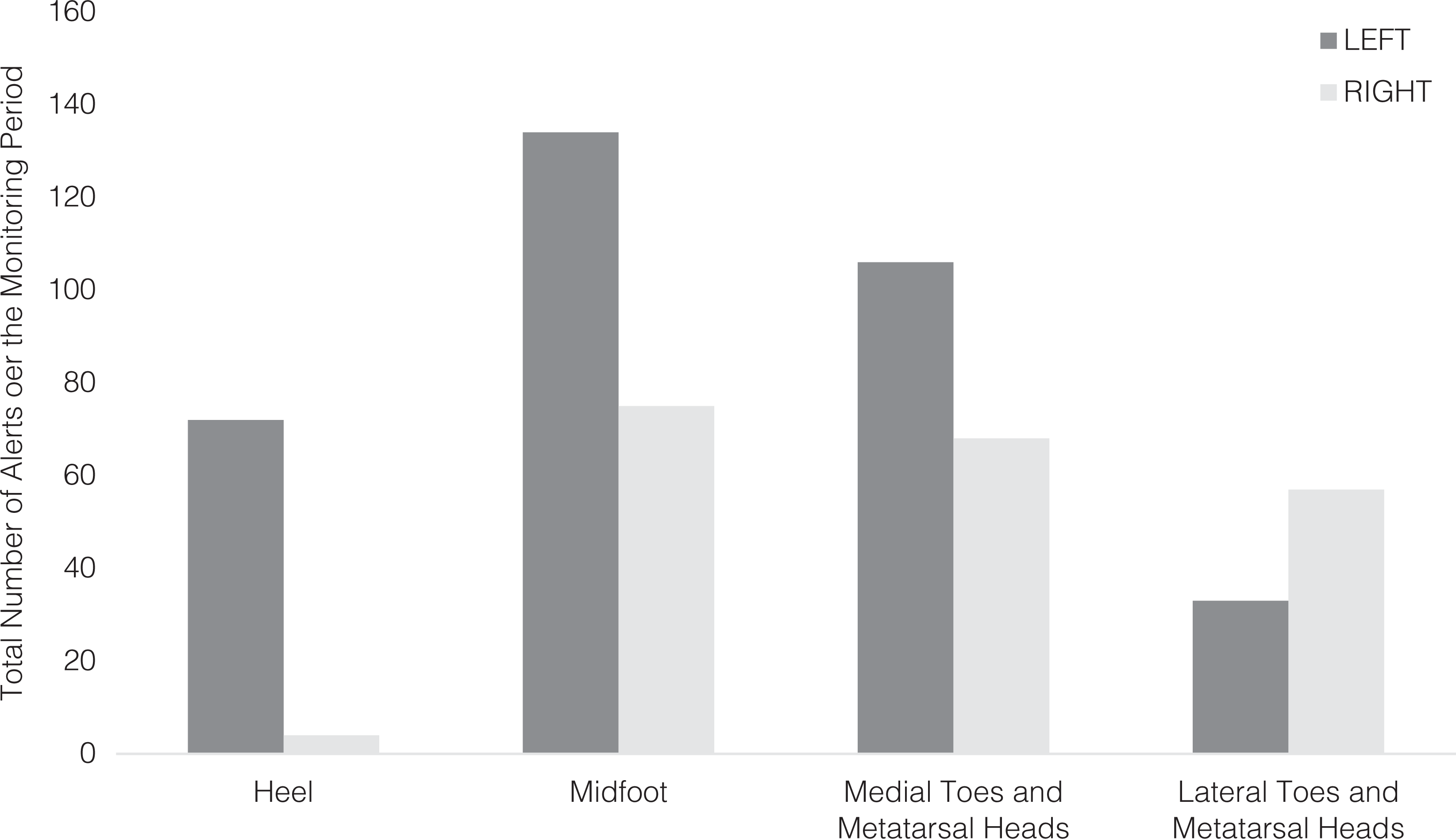
Alert distribution by footmap region for the right and left foot over the monitoring period.
Discussion
The SurroSense Rx provided provider- and patient-level utility with respect to the management of LOPS on the reconstructed right heel.
From a provider’s perspective, the device was able to monitor and quantify compliance with the prescribed foot care regimen. Data patterns emerged enabling one to deduce behaviour with respect to plantar pressure distribution over time. Initially, very few alerts were triggered on the right heel, while the right forefoot demonstrated a very high alert frequency, suggesting favouring of the affected foot and region.
For the patient, the device provided feedback to guide dynamic off-loading of the plantar surface. The patient indicated that this feedback allowed him to think less about avoiding pressure on his right heel at all times. Similarly, the patient indicated that the use of the system seemed to educate him on what “safe” and “unsafe” pressure-time thresholds were and, in this way, felt that there was some degree of learning that occurred in using the device. Toward the end of the monitoring period, the patient reported decreased use of the device on account of this training effect.
The compensatory behaviour (favouring the right forefoot and the contralateral [left] foot) seen in the early period of device wearing has potential broad implications with respect to the management of impaired plantar sensation, whether the underlying etiology be injury-related or not. The tendency to avoid weight-bearing on an injured region led to overloading of other plantar regions. While this patient’s plantar sensation was intact in those regions, one can imagine that patients with symmetric plantar neuropathy may incur injury to other tissues on account of LOPS in those highly loaded regions. This suggests that the device utilized herein may have utility in the monitoring of unaffected plantar regions in the immediate post-operative or post-ulcerative period in patients with plantar reconstruction or plantar pressure ulceration, respectively.
The lack of recurrence of any ulcerative events over the monitoring period was highly encouraging, suggesting that the system assisted in the secondary prevention of pressure-related injury to the affected foot. Further study with this device in this unique patient population is merited.
Footnotes
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Dr Breanne Everett is a co-founder of, and serves as the CEO for, Orpyx Medical Technologies Inc. Dr A. Robertson Harrop and Emily Bray are shareholders in Orpyx Medical Technologies Inc.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
