Abstract
The suture anchor method of surgery has some complications. To best of our knowledge, no report on skin ulcer formation apart from the surgical site after tendinous mallet finger injury using suture anchor is available. We present the case of a 73-year-old woman who sustained tendinous mallet finger in an accident. She was treated surgically with a suture anchor. At 12 months after surgery, the string from the surgical site was removed; 28 months after surgery, a skin ulcer was formed 2-cm proximal from the operative scar, and discharge leaked from the dorsal middle phalanx. Because the wound could not heal by conservative treatment, it was treated surgically. At initial surgery, debridement of the skin ulcer, including the suture knot, was performed. At second surgery, the skin defect was reconstructed using a third dorsal metacarpal artery perforator flap. At 1 year postoperatively, she had no symptoms without recurrence.
Introduction
Mallet finger injuries are usually caused by forced flexion of the distal interphalangeal (DIP) joint, which leads to a discontinuity of the extensor mechanism at the distal phalanx, with or without dorsal avulsion fracture. 1,2 A typical symptom is an extensor lag at the DIP joint.
Suture anchors are widely used for the repair or reconstruction of tendons and ligaments and for bone fractures. Complications related to suture anchors have been reported, but, to our best knowledge, skin ulcer formation apart from the surgical site has not been reported in relation to the use of an anchor. 3 -5
We report the case of a skin ulcer that developed at the dorsal middle phalanx of a finger that had been surgically treated 2 years before for tendinous mallet finger with suture anchors. The skin reconstruction entailed the use of the dorsal metacarpal artery in a perforator flap. We also discuss a pathological mechanism for the development of the ulcer.
Case Presentation
A 73-year-old right-handed woman visited our clinic because of a 4-month history of a skin ulcer with accompanying discharge on her left ring finger. She was a homemaker, and her medical history consisted of a gallstone treated by surgery and hypertension treated by medication for several years. She had never smoked.
Two years and 9 months before visiting our hospital, she had a tendinous mallet finger injury when the left ring finger was hooked by a towel. Four days after injury, she was treated surgically with an anchor system. One year after surgery, the suture string was projected from the wound of dorsal skin at the DIP joint, and it was removed. Two years and 4 months after surgery, discharge began leaking from an ulcer of the dorsal skin at the middle phalanx. Because this condition could not heal with oral antibiotics and standard wound care, she sought further treatment at our institution.
Physical examination revealed a skin ulcer with accompanying discharge and surrounding purple skin at the dorsal middle phalanx of the left ring finger (Figure 1). The operative scar on the dorsal skin at the DIP joint had healed, and the skin ulcer was 2 cm proximal from the scar. The grip strength for the right and left hands, measured with a digital dynamometer, were 15.8 and 9.9 kg, respectively. The active extension/flexion ranges of motion in the left ring finger, measured by a standard goniometer, were 5° to 75° for the metacarpophalangeal joint, −10° to 75° for the proximal interphalangeal joint, and −30° to 50° for the DIP joint. Blood testing revealed a C-reactive protein level of 0.03 mg/dL. The discharge was cultured for bacteria, but the result was negative. Plain radiographs of the left ring finger (Figure 2) revealed the suture anchor at the base of the dorsal distal phalanx. Magnetic resonance images of the finger showed that the pathological lesion at the dorsal middle phalanx had low signal intensity on T1-weighted images and high signal intensity on T2-weighted images, and the terminal tendon was not clearly visible distally from the centre of the middle phalanx.
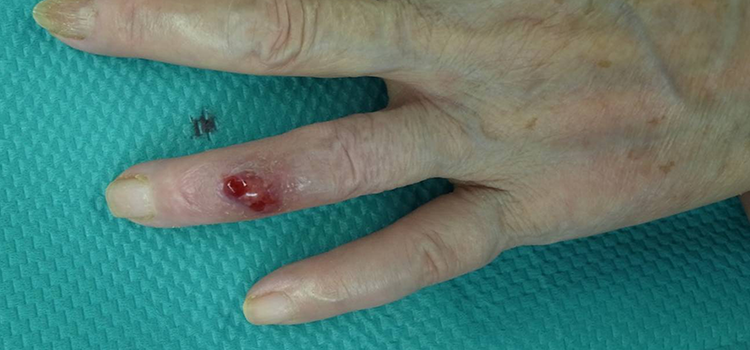
Skin ulcer on the dorsal middle phalanx of the left ring finger.
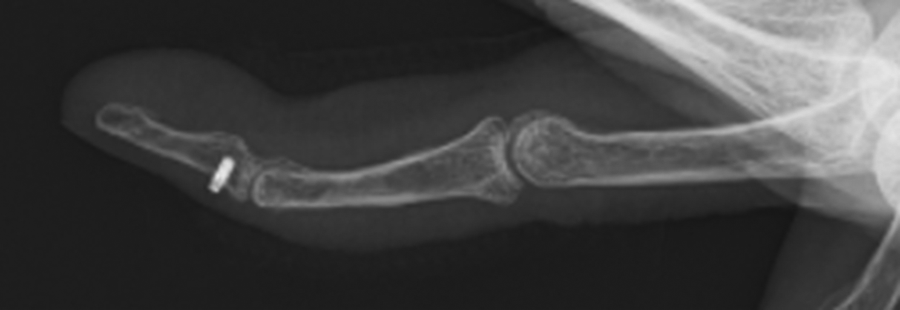
Preoperative lateral plain radiograph.
The diagnosis was of a skin ulcer after surgery for the tendinous mallet finger, and the possibility of a skin tumour was noted. Because the extension lag of the finger did not cause a disability, we planned 2-staged surgery for reconstruction involving the skin ulcer.
Initial surgery was performed with the area under regional anaesthesia and tourniquet control, aiming to obtain a definitive diagnosis. The intraoperative findings were that skin ulcer was formed around a suture knot that should have originated from the suture anchor (Figure 3). The skin ulcer, including the surrounding abnormal skin and suture material, was resected. The anchor system at the distal phalanx was also removed. Histological examination of skin ulcer revealed findings of stitch abscess, with a dense infiltration of neutrophils, lymphocytes, plasma cells, and foreign body giant cells, but no malignancy (Figure 4). The definitive diagnosis was skin ulcer caused by stitch abscess originating from the anchor system.
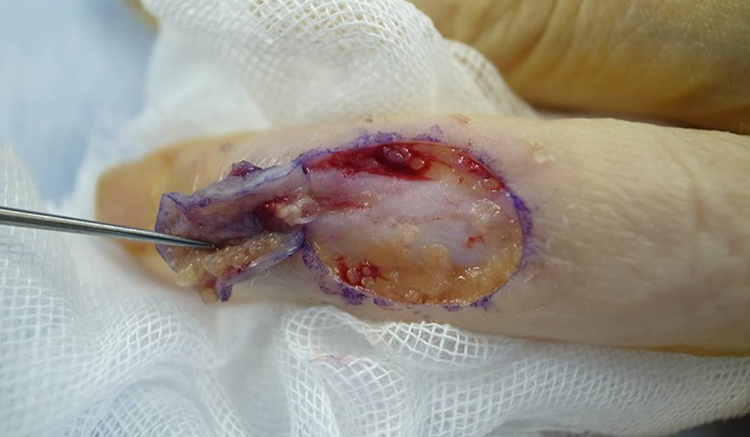
During the first procedure, the suture knot was found under the skin ulcer.
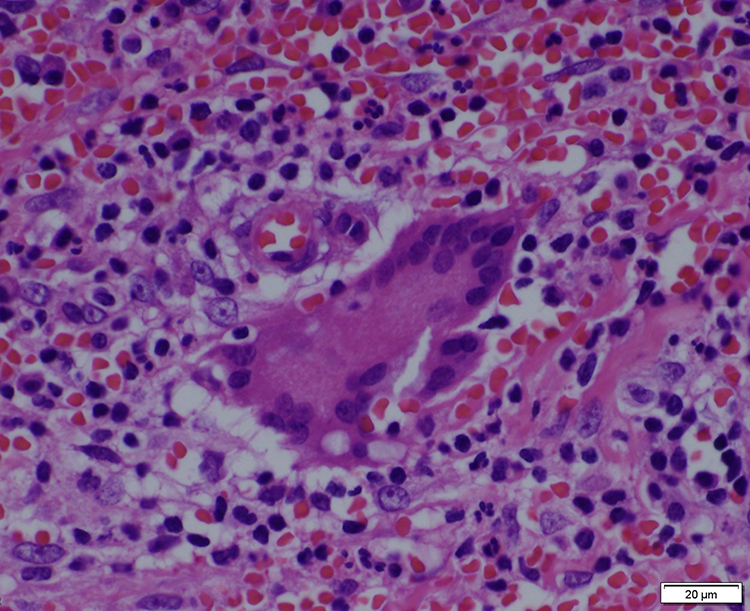
Histological section (magnifications; ×400) stained with haematoxylin and eosin shows dense infiltration of neutrophils, lymphocytes, plasma cells, and foreign body giant cells.
The second surgery for reconstruction of the skin defect was performed 3 days after the initial procedure. Regional anaesthesia and tourniquet control were used in this procedure as well. Before surgery, the site of a perforator of the third dorsal metacarpal artery was confirmed by ultrasonography. The size of the flap was 18 × 20 mm2, and the proximal site was the dorsal wrist crease. The skin defect on the dorsal middle phalanx could be covered by the dorsal metacarpal artery perforator (DMAP) flap (Figures 5 and 6). For 1 week after surgery, the involved side of the hand was elevated and rested. Afterwards, finger exercises were started. The postoperative course was uneventful, and the flap was survived without congestion and necrosis.
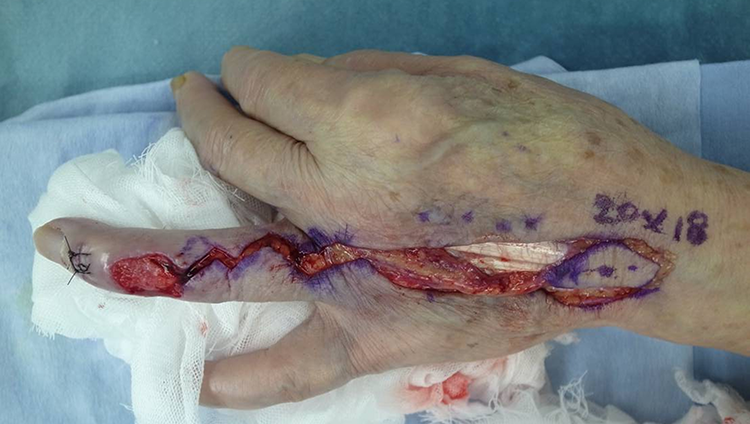
During the second procedure, a third dorsal metacarpal artery perforator flap was elevated.
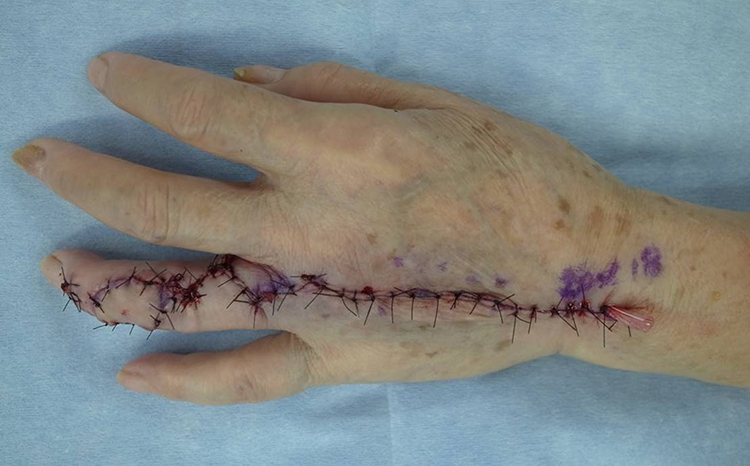
The skin ulcer was reconstructed with a third dorsal metacarpal artery perforator flap.
At the final follow-up 1 year postoperatively, the patient had no symptoms or recurrence of the ulcer (Figures 7 and 8). Her grip strength was 16.2 kg for the right hand and 12.8 kg for the left hand. The active extension/flexion ranges of motion of the left ring finger were 10° to 80° for the metacarpophalangeal joint, 0° to 100° for the proximal interphalangeal joint, and −25° to 60° for the DIP joint. The patient provided written consent for publication of this case report.
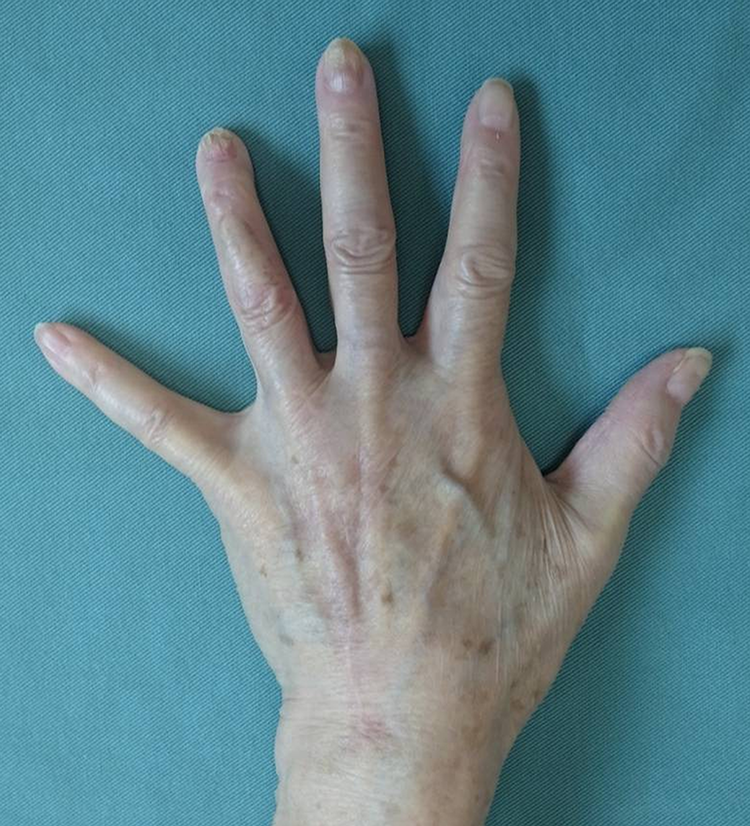
Macroscopic photograph of dorsal view at the last follow-up.
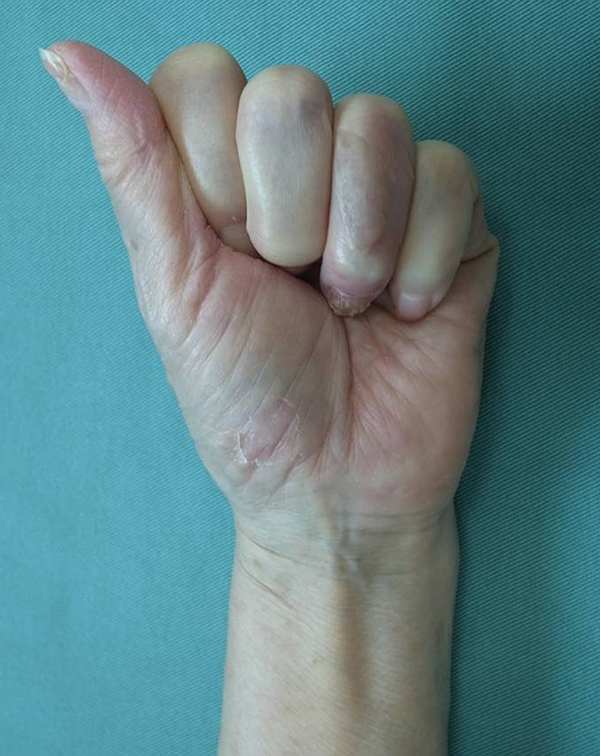
Macroscopic photograph of grip view at the last follow-up.
Discussion
Our patient had a skin ulcer on 1 finger after the finger was surgically treated for tendinous mallet finger with a suture anchor. The ulcer was successfully treated by a DMAP flap after incisional biopsy.
Acute closed tendinous mallet finger is conservatively treated using a splint with the DIP joint in a neutral position to hyperextension, worn full time for 6 to 8 weeks. 6 In some cases, surgery involving a wire for maintaining the DIP joint in extended position might be indicated for patients who cannot perform their jobs with an external splint. 2
Suture anchor systems are widely used for the repair or reconstruction of tendons (including mallet finger) and ligaments and for bone fractures. 7 Complications related to suture anchors have been reported: anchor migration, anchor dislodgment, synovitis caused by absorbable material, osteolysis, and skin ulcer caused by foreign body reaction to the anchor. 3 -5
In our case, we suspected a multistep mechanism of pathology: First, the tendinous mallet finger was treated by a suture anchor; second, the string of suture anchor protruded from the dorsal skin at the DIP joint and was removed; third, after removal of the string, the terminal tendon accompanying the suture knot migrated proximally; and fourth, the remaining suture knot caused the formation of a stitch abscess and skin ulcer. It was a specific point that the skin ulcer was at a site different from the original operative site.
For reconstruction of the dorsal skin defect of middle phalanx, some other flaps and skin graft are applicable, depending on the size of the defect: local flap, digital artery perforator flap, reverse cross-finger flap, and distant flap. 8 For our patient, DMAP flap was selected as a soft tissue reconstruction because of its advantages: similarity of the skin of the dorsal aspect of the hand to that of the finger, thinness of the flap, easy elevation of flap, no need for skin graft, and ability to start range-of-motion exercises relatively early in the postoperative period. 9,10 Other methods entail some disadvantages: for example, with local flaps and digital artery perforator flaps, a skin graft is necessary; with digital artery perforator flaps, the digital artery perforator can be damaged; and with the reverse cross-finger flap, contractures can occur in the recipient finger.
Conclusion
Postoperative complications can occur at sites distant from the original operative site because of the nature of the anchor system for tendon injury. In this case, the skin ulcer was a postoperative complication after surgery for a tendinous mallet finger with a suture anchor, and it was treated successfully by DMAP flap.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Statements and Informed Consent
Ethical approval was obtained from institutional review board.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Statement of Human and Animal Rights
This article does not contain any experimental studies with human or animal subjects.
Statement of Informed Consent
Written, informed consent was obtained from the patient included in this case report.
