Abstract
Background:
Fat transfer for buttock augmentation has become popular in the last quarter century. Increasingly, patients obtain the surgery internationally and return home in the early post-operative period. Complications after procedures performed internationally can be difficult to manage due to a paucity of medical and surgical history as well as challenges in obtaining salient records such as operative reports or communicating with the initial surgical team. In the case of fat grafting, complications including infection, hematoma, and injury to critical structures can occur at both the recipient and donor sites.
Case:
A 28-year-old female underwent large volume buttock fat grafting in the Dominican Republic and received a post-operative course of oral levofloxacin and clindamycin. After her return home, she presented to our institution on post-operative day 9 with buttock pain, tachycardia, and leukocytosis. Imaging of her buttocks showed questionable fluid collections, with no drainable abscess. Drainage of the fat grafted areas by Interventional Radiology recovered a small amount of fluid with negative initial bacterial cultures. Despite antibiotic therapy with vancomycin and meropenem and fluid resuscitation, she did not experience clinical improvement and definitive treatment required bilateral debridement of buttocks with intraoperative findings of large volume fat necrosis. Cultures from the wound grew Peptostreptococcus after a week of incubation, and the patient recovered without further surgical intervention. The case suggests that immediate post-operative antibiotics can select for slow-growing organisms, and diagnosis of large volume fat graft necrosis may be delayed given the absence of a clear abscess cavity on imaging.
Keywords
Introduction
Many US patients seeking more affordable care travel abroad to receive surgery. The Centers for Disease Control and Prevention reports that hundreds of thousands of US residents currently travel outside of the borders for medical care, and it is an industry that is expected to grow. 1 Autologous fat grafting for buttocks augmentation is popular in both the United States and abroad and is commonly known as a “Brazilian butt lift.” 2 The technique for this type of buttock augmentation involves liposuction to sculpt the flank and buttock with transfer of the removed fat to improve or enhance the contour of the buttocks. 2 Large case series have demonstrated the procedure to be safe 3 ; however, significant complications including fat embolism and death have been reported. 4 Life-threatening infections have also been reported. 5 -7 Diagnosis of these complications can be challenging in the context of a surgical procedure performed abroad when available surgical and medical information is limited.
Case
A 28-year-old otherwise healthy female underwent large volume liposuction and fat grafts to the bilateral buttocks in the Dominican Republic 9 days prior to admission to our hospital. The operative report indicated that 3000 cm3 of fat was injected intramuscularly into the bilateral buttocks. Prophylactic oral levofloxacin and clindamycin were initiated immediately post-procedure and were continued for a total of 7 days. On post-operative day 4, while still in the Dominican Republic, the patient developed a fever and complained of buttock pain. No further intervention was undertaken at this time. Prior to travel home, she had a negative duplex Doppler of her lower extremities and she was discharged home to the United States on post-operative day 5 on prophylactic enoxaparin injections. She continued to have bilateral buttock pain and malaise. On post-operative day 8, she presented with shortness of breath, fevers to 38.9°C, tachycardia to 110 seconds, anemia with drop in hemoglobin from 12 to 7.6, and leukocytosis to 19.1. A computed tomography (CT) of the chest did not demonstrate a pulmonary embolus. A CT of the abdomen and pelvis demonstrated heterogeneous collections in the bilateral gluteal muscles (Figure 1) with no clear evidence of a drainable fluid collection. On initial examination, she had mild buttock tenderness with no evidence of erythema, hematoma, or palpable fluid collection (Figure 2). The patient was given intravenous vancomycin and meropenem and appeared to improve with fluid resuscitation. On post-operative days 11 and 12, the patient became increasingly lethargic and febrile with persistent leukocytosis to 14.3 and 16.5, respectively, meeting 2 of the 4 SIRS criteria. A repeat CT of the abdomen and pelvis was performed which again demonstrated heterogeneous fluid collections in the bilateral gluteal muscles. Interventional radiology was consulted to aspirate the left-sided fluid collection which appeared to have a drainable area. Aspiration of the fluid collection returned 13 cc of yellow, turbid fluid, aerobic, and anaerobic cultures of which were initially negative for bacteria. Despite ongoing antibiotic therapy, the patient continued to have fever and leukocytosis. Due to a lack of clinical improvement, a bilateral operative debridement was performed on post-operative day 15. The bilateral buttocks were widely incised and drained. The left gluteus yielded 400 cc of gray fluid from multiple intragluteal pockets. The right gluteus yielded large amounts of oil and fat globules without purulence (Figure 3). Cultures of the bilateral surgical sites were collected before and after washout of the wounds. The wounds were packed open with wet to dry dressings (Figure 4) and the patient was admitted to ICU intubated for further care. Bacterial cultures from the initial interventional radiology procedure grew Peptostreptococcus after 8 days of incubation. Prewashout cultures of the left buttock also grew Peptostreptococcus which required 8 days of incubation for growth. Prewashout cultures of the right buttock were negative for growth. Blood cultures collected daily on post-operative days 9 to 12 and urine cultures were negative. The patient was also found to have bilateral pulmonary emboli requiring oral anticoagulation. Over the course of 5 days following debridement, the patient’s white count improved to 10.2 and fevers resolved. The patient was on hospital day 12 on 2 weeks of Augmentin, oral anticoagulation, and daily dressing changes; she presented to plastic surgery clinic for follow-up 5 days post-discharge and was transitioned to vacuum-assisted wound therapy for her gluteal wounds.
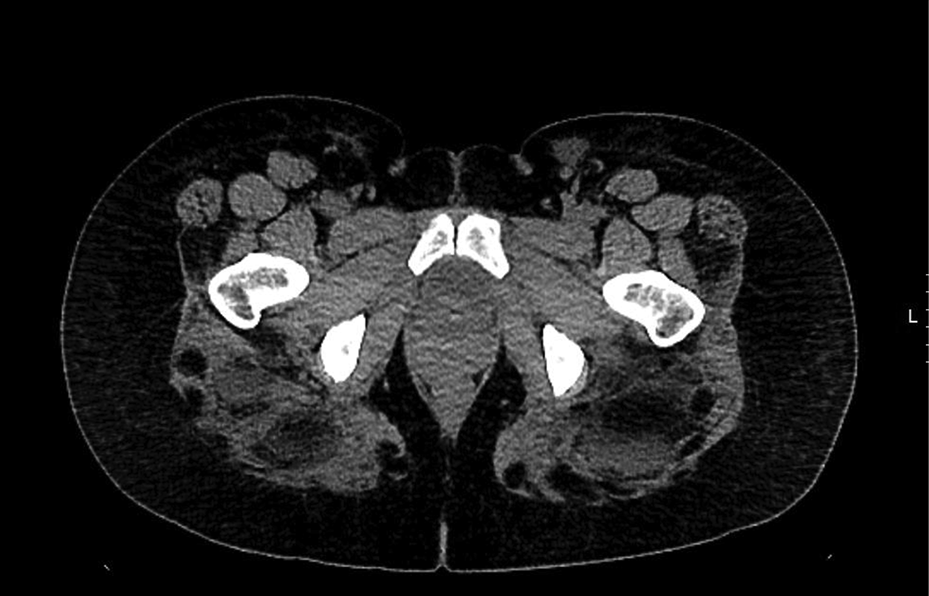
Computed tomography (CT) scan demonstrating large heterogeneous fluid collections but no drainable abscess cavities.
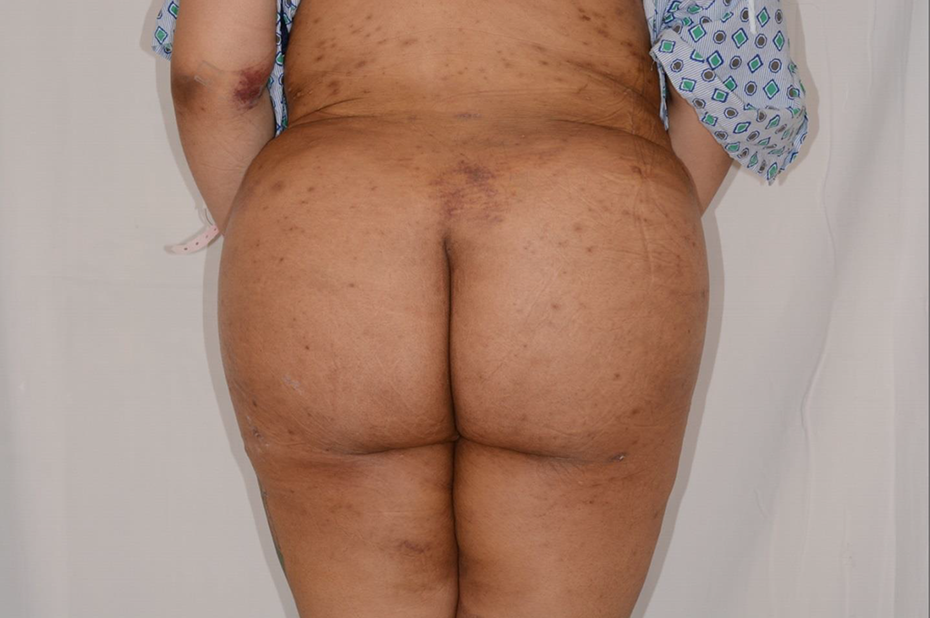
Physical examination demonstrated mild tenderness but no signs of fluid collection.

Operative debridement of the right buttock recovered oil and fat globules but no purulence.
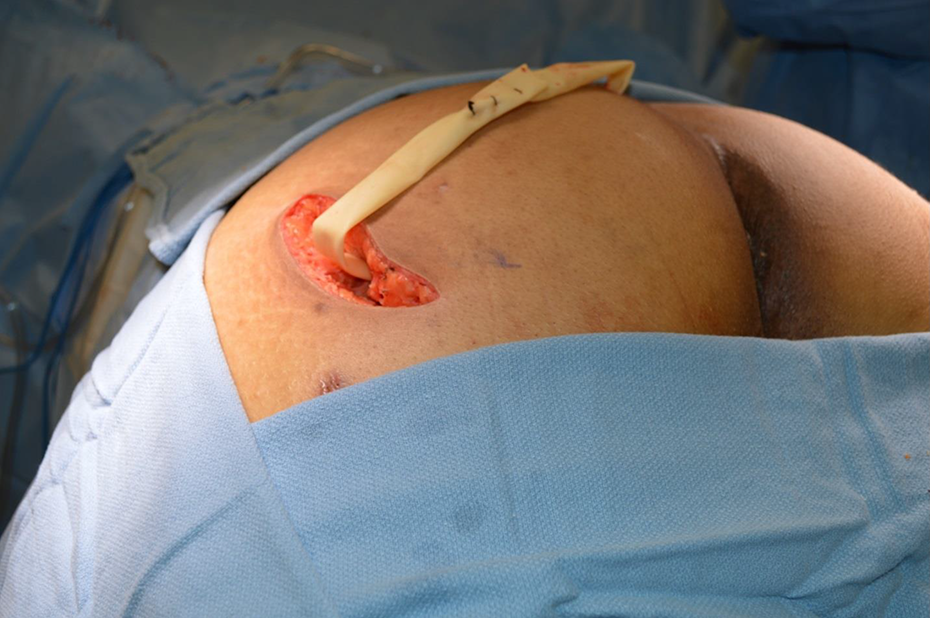
Operative sites were left open and packed.
Discussion
We present a case of sepsis (2 SIRS criteria in the presence of positive tissue cultures) following autologous fat transfer. We believe this patient had large volume fat necrosis and eventually developed a superinfection of the necrotic fat with Peptostreptococcus despite post-operative antibiotic prophylaxis, albeit with questionable fat penetration. Previous reports have described similar presentations of infection following large volume fat necrosis in both the buttock and breast. 5 -7 In our case, obscure imaging characteristics and negative initial cultures confounded the initial diagnosis and treatment. The definitive therapy was surgical debridement.
Fat transfer for cosmetic purposes has been used safely for contouring of the buttocks and breast. 8 Fat necrosis following large volume fat transfer in the breast has been described and is proposed to be more likely when the volume of transferred fat is large. 9 Fat necrosis creates a nidus for bacteria to grow and the potential for infection to develop. It is important for the evaluating clinician to maintain a high suspicion for fat necrosis in the setting of clinical and radiologic uncertainty, as early surgical intervention may prevent development of a complex and life-threatening infection.
This case also demonstrates the challenges associated with culturing the culpable organism. Our patient received broad spectrum antibiotics for a 7-day period post-operatively. The prophylactic antibiotics have the potential to select for resistant and slow-growing organisms or poorly penetrate the target tissues. As was the case in our patient, early cultures of necrotic fat may be culture negative if grown in suboptimal conditions. This reiterates the importance of maintaining a low threshold for surgical intervention.
Finally, the case also highlights the diagnostic challenges faced when a patient has surgery internationally and presents with a complication. The specifics of procedures, including intraoperative anesthesia flow sheets and post-anesthesia care unit records, are often difficult to obtain. The travel to tropical destinations can confound the diagnosis as many of the infectious symptoms these patients present with are also characteristic of tropical diseases which many clinicians are unfamiliar. It is imperative specifically to elucidate not only procedures performed but also post-operative course including medications received, post-operative care, and travel via communication with the patient and initial surgical team. It is also important to gather as many records as possible from the performing surgeon regardless of language or communication barriers, as the information they offer may be invaluable to proper treatment of the complication.
This case highlights several important points. It is important to recognize the imaging characteristics of transferred fat and understand the clinical presentation and radiologic appearance of transferred fat that does incorporate. It is important when a patient has travelled internationally for surgery to gather as much clinical information as possible from both the patient and performing surgeon. Finally, early removal of the inflammatory source regardless of cultures is the definitive treatment if there is concern for large volume fat necrosis.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Statement of Human and Animal Rights
This article does not contain any experimental studies with human or animal subjects.
Statement of Informed Consent
The case report was reviewed by the Institutional Review Board and determined to be exempt. Consent was obtained for photograph use.
